Lecture 18 A + P 2
1/34
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
35 Terms
ADAPTIVE IMMUNE SYSTEM: Humoral Immunity
HUMORAL Immunity
B-Cells
Recognize soluble or cell surface Antigens and differentiate into Antibody secreting cells.
These guys go in and bind the whole pathogen or whole area
B cells recognize native (whole) antigens, whereas T cells
recognize processed antigens presented on MHC
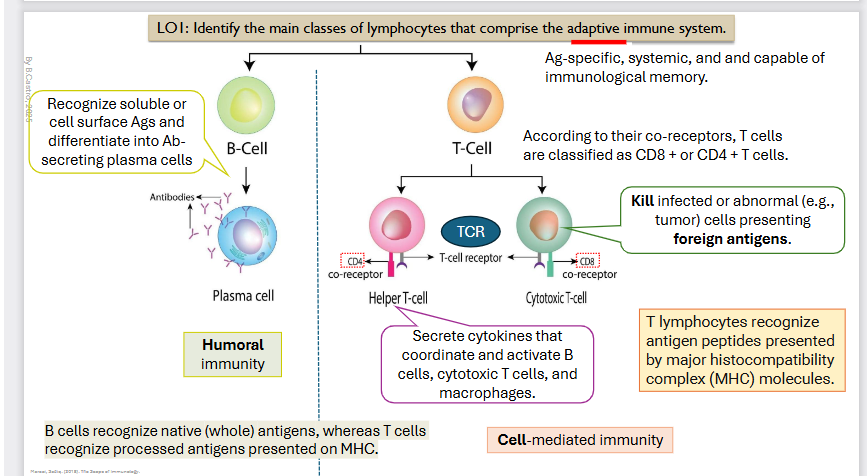
ADAPTIVE IMMUNE SYSTEM: Cell - Mediated Immunity
T-cells
Coreceptor is CD4 → Helper T-Cell
Secrete cytokines that coordinate and activate cells, cytotoxic T cells, and macrophages
CD8 Coreceptor → Cytotoxic T-Cell
Kill infected or abnormal (e.g., tumor) cells presenting foreign antigens.
T lymphocytes recognize antigen peptides presented by major histocompatibility complex (MHC)
Antigen-specific, systemic, and and capable of
immunological memory.
Innate immune recognition vs Antigens
Innate immune recognition (neutrophils)
Recognized by:
PRRs (like TLRs, NOD-like receptors)
They detect
PAMPs (Pathogen - associated molecular patterns)
EX: lps, flagelln
DAMPS (Damage - associated molecular patterns) (signals from damaged cells)
Antigens
Recognized by
Antibodies (B - Cells)
T - cell receptors (T cells)
Recognition is Highly Specific (unique epitopes)
Examples
A specific viral protein
A bacterial toxin
What is an antigen/antigenic
“derived from “antibody generating”
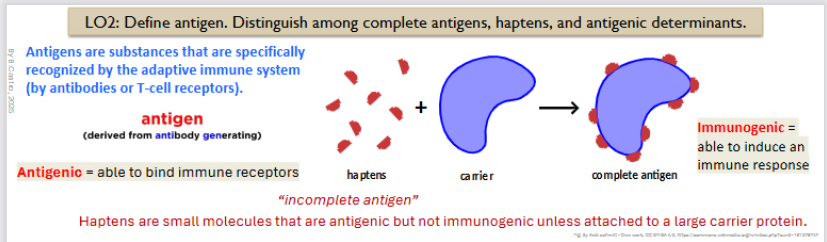
They are substances that are specifically recognized by the adaptive immune system (by antibodies or T-cell receptors)
Antigenic: Meaning to be able to bind to immune receptors
What is a hapten and what can it interact with
“Incomplete antigen”
They are small molecules that are antigenic but not immunogenic unless attatched to a large carrier protein.
Immunogenic =able to induce an immune response
What is an epitope
Antigenic Determinants (also known as Epitopes)
Specific regions of an antigen that are recognized by antibodies orT-cell receptors
A single antigen can have multiple epitopes
This means that there can be different immune cells to recognize different parts of the same molecule.

Explain MHC (major histocompatibility complex) in adaptive immunity
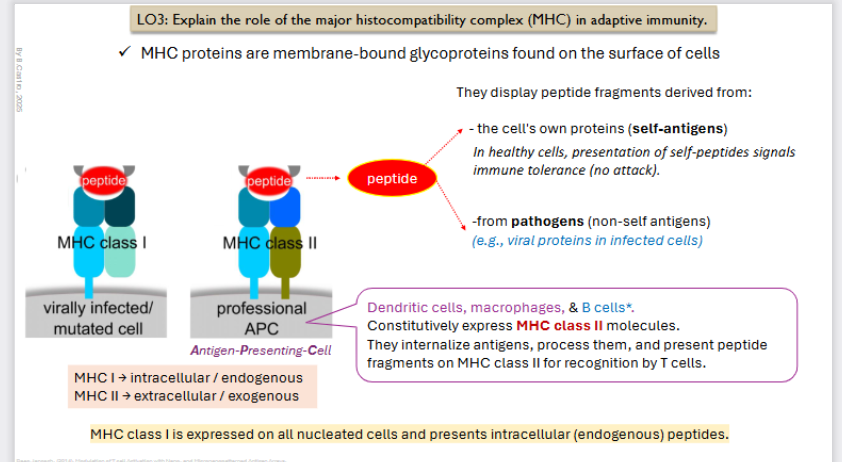
MHC proteins are membrane bound glycoproteins found on the surface of cells
They display peptide fragments derived from
The cell’s own proteins (self antigens)
In healthy cells, presentation of SELF peptides signals immune tolerance (no attack)
from pathogens (non-self antigens)
EX: Viral proteins in infected self.
MHC class I
Where does it take the peptide from
What T-cell does it interact with
What cell type is it in
What do they secrete for immune response
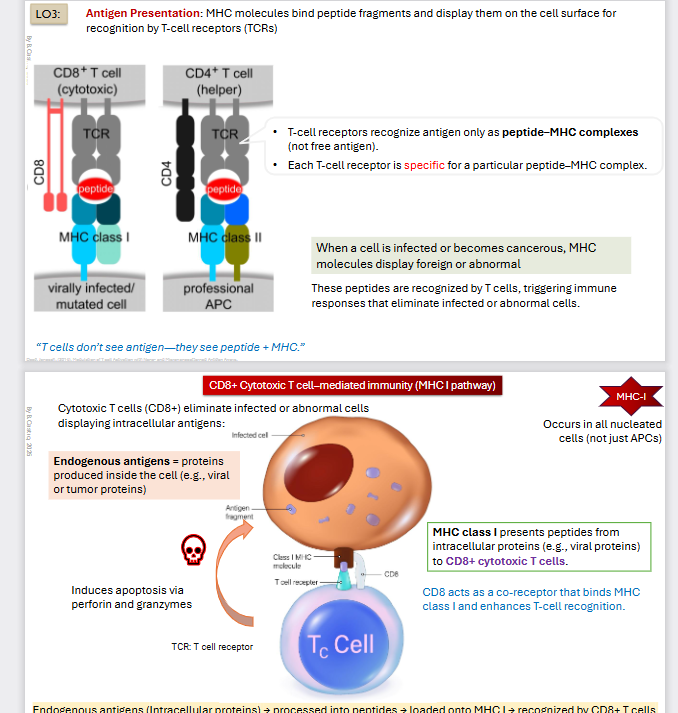
MHC Class I
Virally Infected/mutated cell
MHC I → Intracellular / endogenous
MHC Class I is expressed on all nucleated cells and presents intracellular (endogenous) peptides.
Once the T cells interact they multiply to get rid of the intruder.
Include endogenous antigens
Proteins produced inside the cell (viral or tumor proteins)
All nucleated cells not just APCs
MHC class I presents peptides from intracellular Proteins to CD8+ cytotoxic t-cells
CD8 acts as a co-receptor that binds MHC class I and enhances T-cell recognition
Once they are recognized, T-cells Induces apoptosis via perforin and granzyme to the targets.
Endogenous antigens (Intracellular proteins) → processed into peptides → loaded onto MHC I → recognized by CD8+ T cells → Induce apoptosis via perforin and granzyme
MHC class II
Where does it take the peptide from
What T-cell does it interact with
What cell type is it in
What do they secrete for immune response
MHC Class II
Professional APC (antigen presenting cell)
Extracellular / exogenous
Dendritic Cells, macrophages, and B cells (only present after activation). Constitutively express MHC class II molecules. They internalize antigens (that came from the outside), process them, and present peptide fragments on MHC class II for recognition by T cells
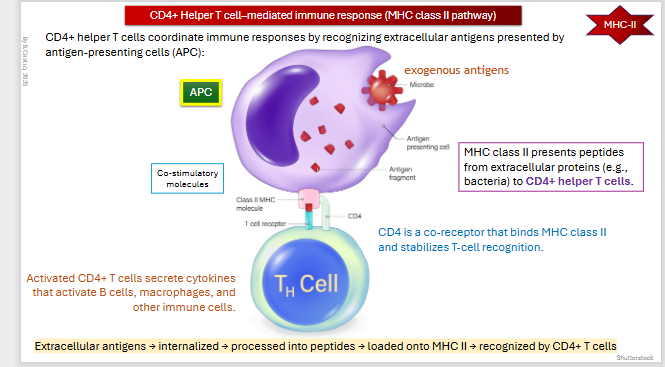
CD4+ helper T cells coordinate immune responses by recognizing extracellular antigens presented by antigen-presenting cells (APC)
MHC class II presents peptides from extracellular proteins (e.g., bacteria) to CD4+ helper T cells
CD4 is a co-receptor that binds MHC class II and stabilizes T-cell recognition
Activated CD4+ T cells secrete cytokines that activate B cells, macrophages, and other immune cells
Extracellular antigens → internalized → processed into peptides → loaded onto MHC II → recognized by CD4+ T cells
Primary Lymphoid organs
What cell types come from these
What locations are they from in particular
What is the cell maturation of cell type considered here
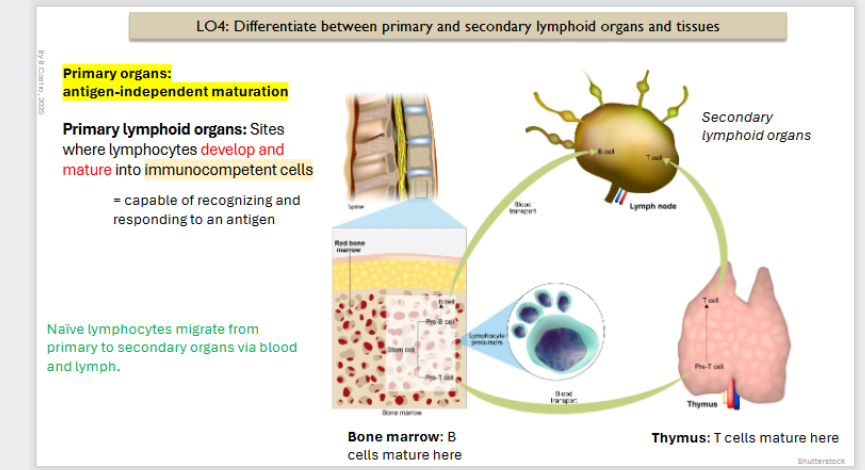
Primary Organs: Antigen independent maturation (origin of B and T cells)
Primary Lymphoid organs: Sites where lymphocytes develop and mature into immunocompetent (capable of recognizing and responding to an antigen) cells.
Naive lymphocytes migrate from primary to secondary organs via blood and lymph.
B cells mature from the bone marrow
T cells mature from the thymus
Naive lymphocytes (recently mature B/T cells that do not have their antigen yet.) migrate from primary to secondary organs via blood and lymph.
Secondary organs and tissue:
Where are the secondary organs and tissues
What do they do to cells
Breakdown of one of the types of secondary categories.
Antigen dependent activation
Sites where mature lymphocytes encounter antigen and become activated, and proliferate.
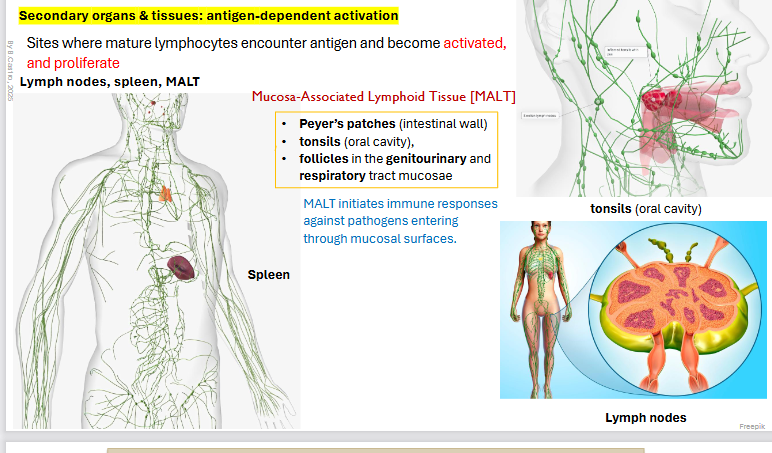
Sites include: Lymph nodes, spleen, MALT
Mucosa Associated Lymphoid tissue: MALT
Peyer’s patches (intestinal wall)
tonsils (oral cavity),
follicles in the genitourinary and respiratory tract mucosae
MALT initiates immune responses against pathogens entering through mucosal surfaces
Primary Follicles of Secondary Lymphoid organs
plus some general bg info
general bg info
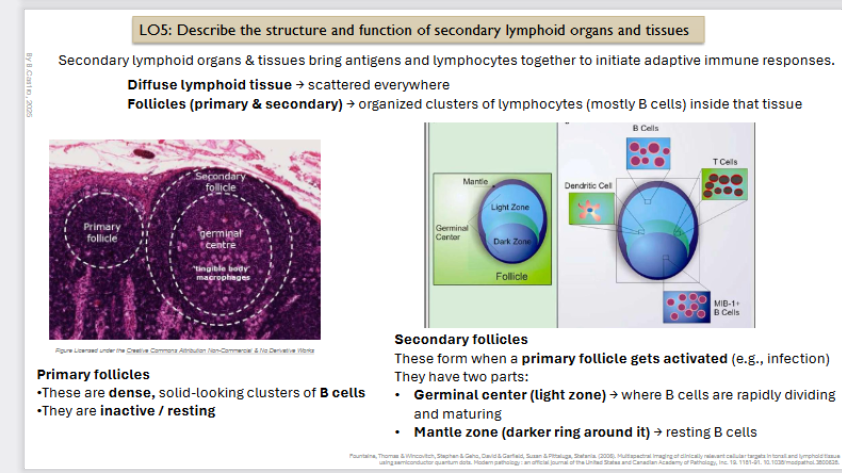
Secondary lymphoid organs & tissues bring antigens and lymphocytes together to initiate adaptive immune responses
Follicles (primary and secondary) → organized clusters of lymphocytes (mostly B cells) inside that tissue.
Lymphoid tissue may be diffuse or packaged into quiescent (primary) follicles [resovoirs for naive B cells]
Primary follicles
•These are dense, solid-looking clusters of B cells
•They are inactive / resting
ECM is made of Lymphocytes with a meshwork of reticular cells.
Reticular Cells are a type of fibroblast that produce and maintain the thin network of fibers (reticular fibers) that form the framework of most lymphoid organs.
There is Diffuse Lymphoid tissue scattered everywhere
![<p>general bg info<br></p><p>Secondary lymphoid organs & tissues bring antigens and lymphocytes together to initiate adaptive immune responses</p><p><strong>Follicles (primary and secondary) → </strong>organized clusters of lymphocytes (mostly B cells) inside that tissue. </p><div data-type="horizontalRule"><hr></div><p>Lymphoid tissue may be diffuse or packaged into <strong>quiescent (primary) follicles [resovoirs for naive B cells]</strong></p><p></p><p><strong>Primary follicles</strong></p><p>•These are dense, solid-looking clusters of B cells</p><p>•They are inactive / resting</p><p></p><p><strong>ECM </strong>is made of <strong>Lymphocytes </strong>with <strong>a </strong>meshwork of reticular <strong>cells.</strong></p><ul><li><p><strong>Reticular Cells </strong>are a type of <strong>fibroblast </strong>that produce and maintain the <strong>thin </strong>network of <strong>fibers </strong>(<strong>reticular fibers</strong>) that form the <strong>framework </strong>of most lymphoid organs. </p></li></ul><p></p><p>There is <strong>Diffuse Lymphoid tissue </strong>scattered everywhere</p><p></p>](https://assets.knowt.com/user-attachments/74cb20af-2ac3-4b45-b1f9-92cac3737c7d.png)
Secondary Follciles
Secondary Follicles
These form when a primary follicle gets activated (e.g., infection)
They have two parts:
Germinal center (light zone) → where B cells are rapidly dividing and maturing
Mantle zone (darker ring around it) → resting B cells Diffuse lymphoid tissue → scattered everywhere
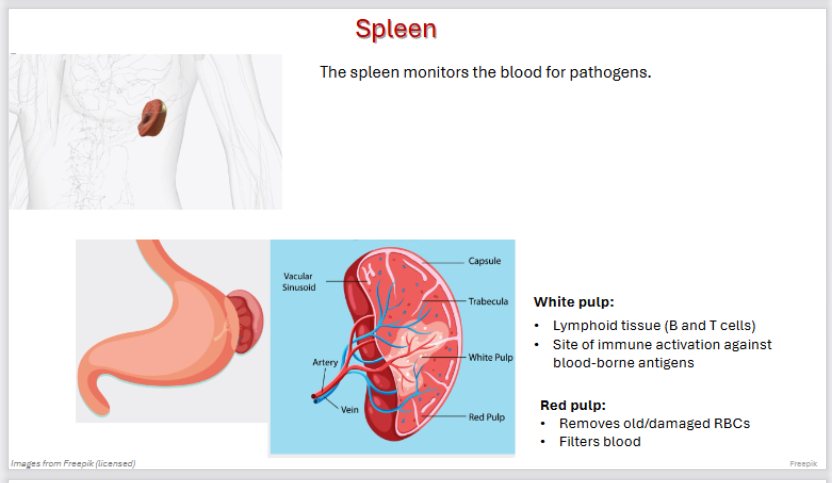
Spleen as a secondary lymphoid organ
The spleen monitors the blood for pathogens.
White pulp:
Lymphoid tissue (B and T cells)
Site of immune activation against blood-borne antigens
Red pulp:
Removes old/damaged RBCs
Filters blood
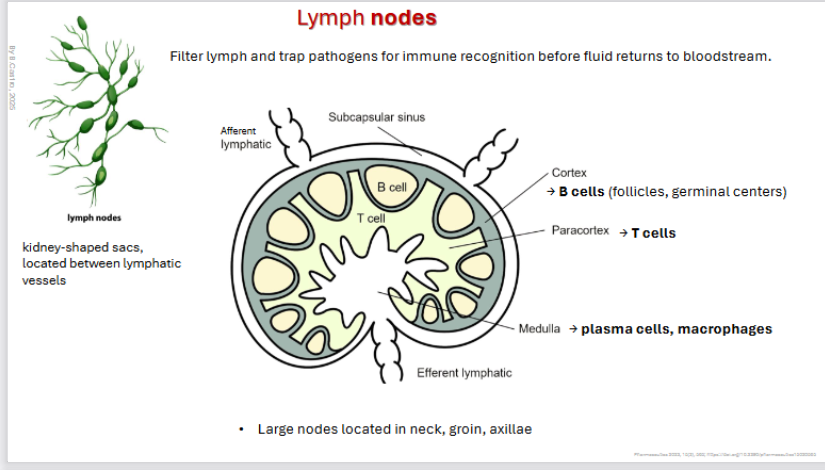
Lymph Nodes
Filter lymph and trap pathogens for immune recognition before fluid returns to bloodstream.
• Large nodes located in neck, groin, axillae
kidney-shaped sacs,
located between lymphatic vessels
→ B cells (follicles, germinal centers)
→ Paracortex: T cells
→ Medulla: plasma cells, macrophages
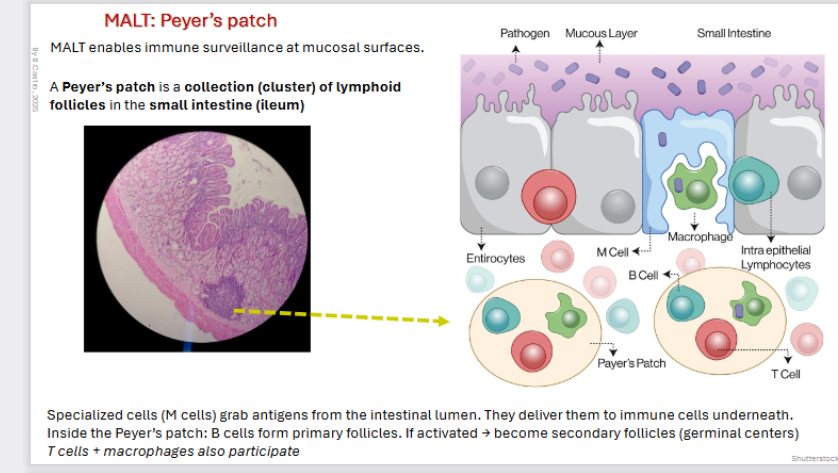
MALT: Peyer’s Patch
MALT enables immune surveillance at mucosal surfaces.
A Peyer’s patch is a collection (cluster) of lymphoid follicles in the small intestine (ileum)
Specialized cells (M cells) grab antigens from the intestinal lumen. They deliver them to immune cells underneath.
Inside the Peyer’s patch: B cells form primary follicles. If activated → become secondary follicles (germinal centers)
T cells + macrophages also participate
Maturation of B - cells
1) Origin: They start in the red bone marrow and stick there until they are done
2) Maturation: they develop immunocompetence & self-tolerance
Maturation of T-cells
Where do they start
Where do the go for maturation
What selection does it undergo
Where does selection take place
1) Origin: They start in the red bone marrow
2) Then it undergoes maturation inside the thymus
Produces thymosin’s → Thymosin’s help the t cell development and the thymus shrinks with age (involution)
During maturation they develop immunocompetence and self - tolerance [not attack our own bodies]
Maturation: Positive Selection
Takes place in the cortical region (cortical thymic epithelial cells)
cTECs present self-peptides bound to MHC molecules to immature T cell
T cells must recognize self-MHC, failure to recognize it: apoptosis
Survivors proceed to negative selection
Maturation: Negative Selection
Takes place in the Medullary TEC’s
Completes their maturation, commit to specific functional lineages (CD4+ or CD 8+) and exit exit the thymus.
3) Seeding secondary organs and circulation
Naive lymphocytes leave primary organs
Immunocompetent = can recognize antigen
Naive = has not yet encountered antigen
They seed (colonize) the secondary lymphoid organs and circulate through blood and lymph.
4) Proliferation and Differentiation
Encounter antigen → activation (with co-stimulation)
Undergo clonal expansion (form a clone, identical cells, same antigen specificity)
Differentiate into: Effector cells & Memory cells
Circulate or reside in tissues to fight infection
![<p>1) <strong>Origin</strong>: They start in the red bone marrow</p><p>2) Then it undergoes maturation inside the <strong>thymus </strong></p><ul><li><p>Produces <strong>thymosin’s → </strong>Thymosin’s help the t cell development and the thymus shrinks with age (involution)</p></li></ul><ul><li><p>During maturation they develop <strong>immunocompetence </strong>and <strong>self - tolerance </strong>[not attack our own bodies]</p></li></ul><p></p><p><strong>Maturation: Positive Selection</strong></p><ul><li><p><strong>Takes place in the cortical region </strong>(cortical thymic epithelial cells)</p></li><li><p><strong>cTECs </strong>present <strong>self</strong>-<strong>peptides </strong>bound to MHC molecules to immature T cell</p></li><li><p>T cells must recognize self-MHC, failure to recognize it: <strong>apoptosis</strong></p></li><li><p>Survivors proceed to negative selection</p></li></ul><p></p><p><strong>Maturation: Negative Selection</strong></p><ul><li><p>Takes place in the Medullary TEC’s</p></li></ul><ul><li><p>Completes their maturation, commit to specific functional lineages (CD4+ or CD 8+) and exit exit the thymus.</p></li></ul><p></p><p><strong>3) Seeding secondary organs and circulation</strong></p><ul><li><p><strong>Naive lymphocytes leave primary organs</strong></p></li></ul><ul><li><p>Immunocompetent = can recognize antigen</p></li><li><p>Naive = has not yet encountered antigen</p></li></ul><p></p><p>They seed (colonize) the secondary lymphoid organs and circulate through blood and lymph.</p><p></p><p><strong>4) Proliferation and Differentiation</strong></p><ul><li><p>Encounter <strong>antigen </strong>→ <strong>activation </strong>(with co-stimulation)</p></li></ul><ul><li><p>Undergo <strong>clonal expansion </strong>(form a clone, identical cells, same antigen specificity)</p></li><li><p><strong>Differentiate </strong>into: <strong>Effector </strong>cells & <strong>Memory </strong>cells</p></li><li><p>Circulate or reside in tissues to fight infection</p></li></ul><p></p><p></p>](https://assets.knowt.com/user-attachments/0a33824f-bf0f-4030-b257-e6fcb68b655d.png)
What are the ways B cells can be primarily activated
Two different ways to be activated
T-cell dependent pathway
T-cell independent Pathway
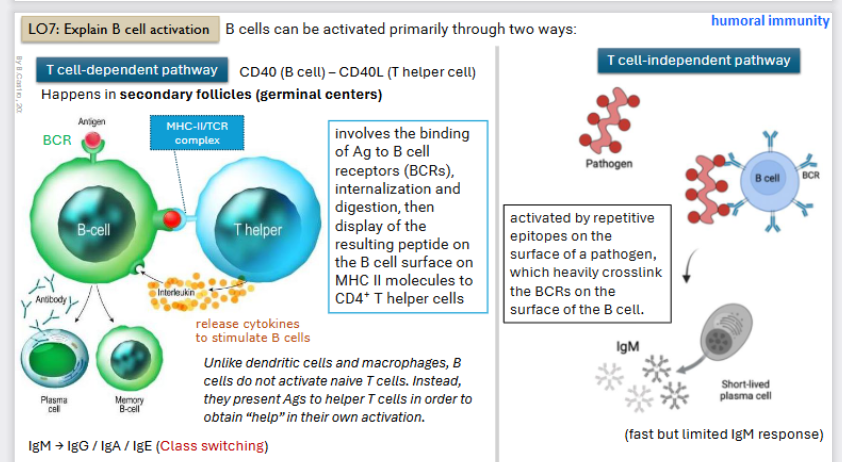
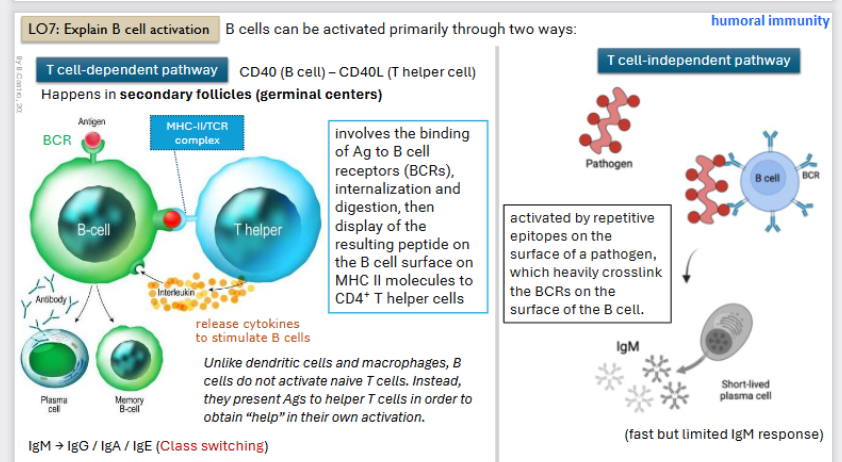
B-cell activation: T-cell dependent pathway
What
When active they can act as professional antigen presenters.
CD 40 (B-cell) to the CD 40L (t-helper cell)
Occurs in the secondary follicles (germ layer)
Binding of the Antigen to B-cells
Then the B - cell forms a complex (MHC - II / TCR complex) with the T - helper cell
T helper cells will release cytokines (interleukins) that make B -cell active (proliferate and differentiate into plasma cells (antibody secretion) or a memory cell (waits in body)
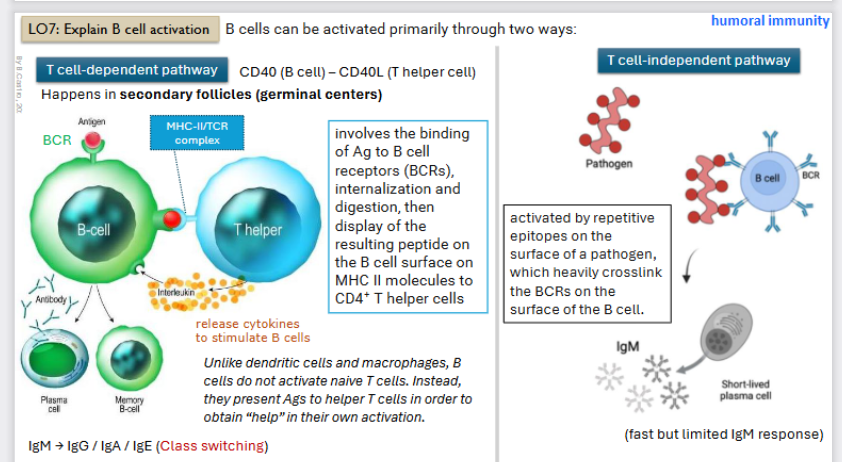
B-cell activation: T-cell independent pathway
Activated by repetitive epitopes on the surface of a pathogen, which heavily crosslink the BCRs (receptor) on the surface of the b - cell.
Antibody will be Immunoglobin M only
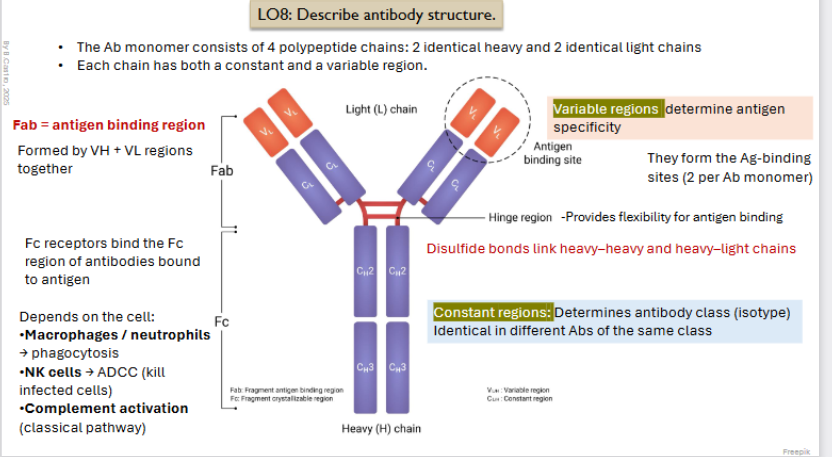
Antibody Structure
What chains are there
What is FC
What is Fab
How do regions affect what the outcome of the antibody will be
The Ab monomer consists of 4 polypeptide chains: 2 identical heavy and 2 identical light chains
Each chain has both a constant and a variable region
Variable region:
Determine antigen specificity
Form antigen binding sites
Constant Regions:
Determines antibody class (isotype) identical in different Abs of the same class)
Fab: Antigen binding region
Formed by VH + VL regions together
Fc receptors bind the Fc region of antibodies bound to antigen
FC is connected with Fab through disulfide link heavy - heavy and heavy light chains.
Depends on the cell:
Macrophages / neutrophils → phagocytosis
NK cells → ADCC (kill infected cells)
Complement activation (classical pathway)
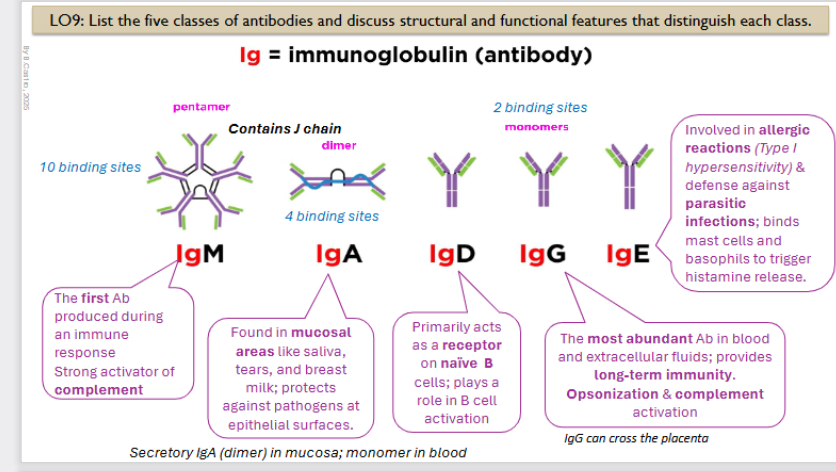
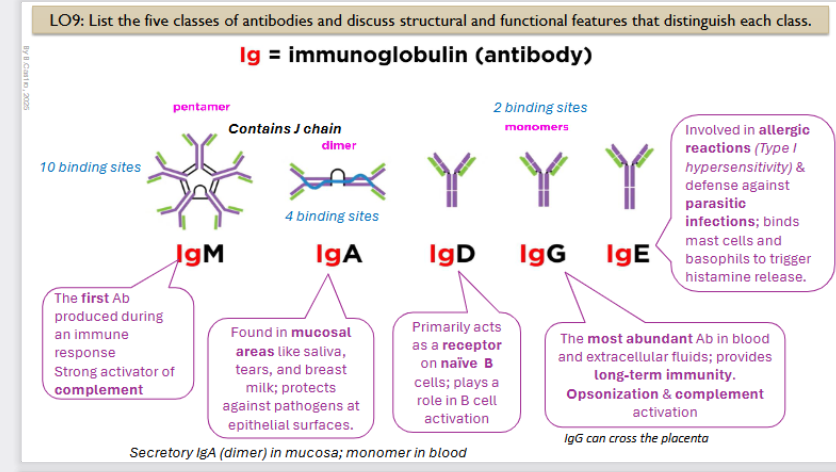
List the five classes of antibodies
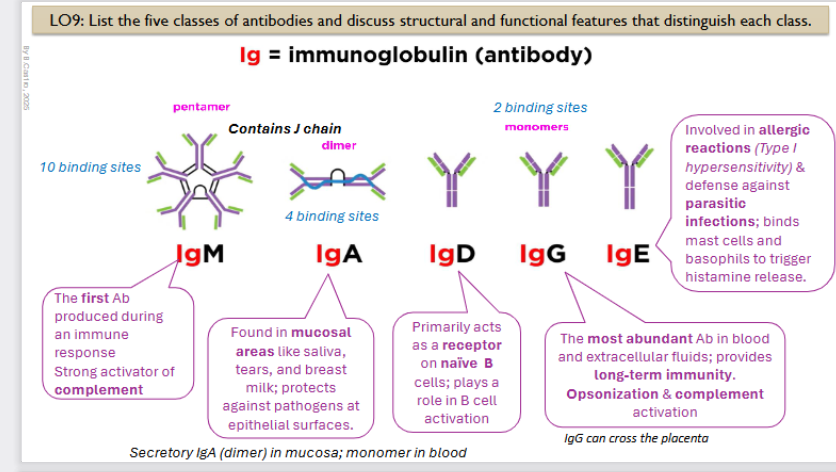
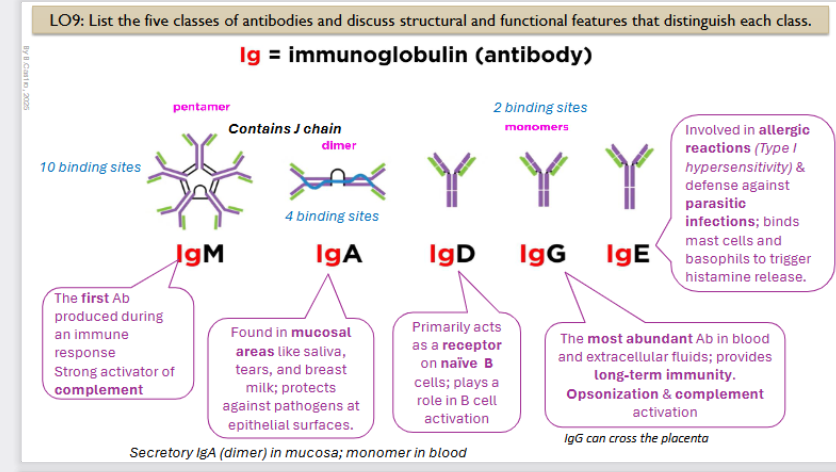
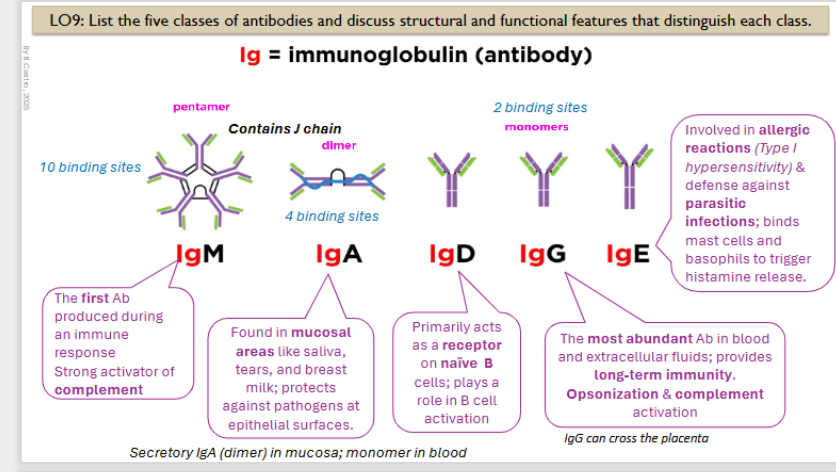
Ig: Immunoglobulin (antibody)
Immunoglobin M
Immunoglobin A
Immunoglobin D
Immunoglobin G
Immunoglobin E
Immunoglobin M structure and function
The first Ab produced during an immune response. Strong activator of complement
It is a pentamer with 10 binding sites
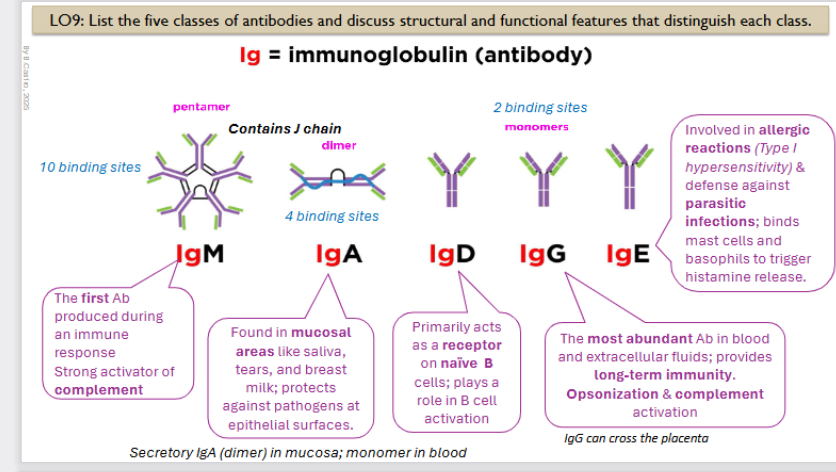
Immunoglobin A structure and function
Found in mucosal areas like saliva, tears, and breast milk; protects against pathogens at epithelial surfaces.
It is a dimer, contains 4 binding sites
it is a secretory IgA (dimer) in mucosa; monomer in blood
Immunoglobin D structure and function
Primarily acts as a receptor on naïve B cells; plays a role in B cell activation
Monomer, has 2 binding sites
Immunoglobin G structure and function
The most abundant Ab in blood and extracellular fluids; provides long-term immunity. Opsonization & complement activation
Monomer, has 2 binding sites
LgG can cross the placenta
Immunoglobin E structure and function
Involved in allergic reactions (Type I hypersensitivity) & defense against parasitic infections; binds mast cells and basophils to trigger histamine release
Monomer, has 2 binding sites
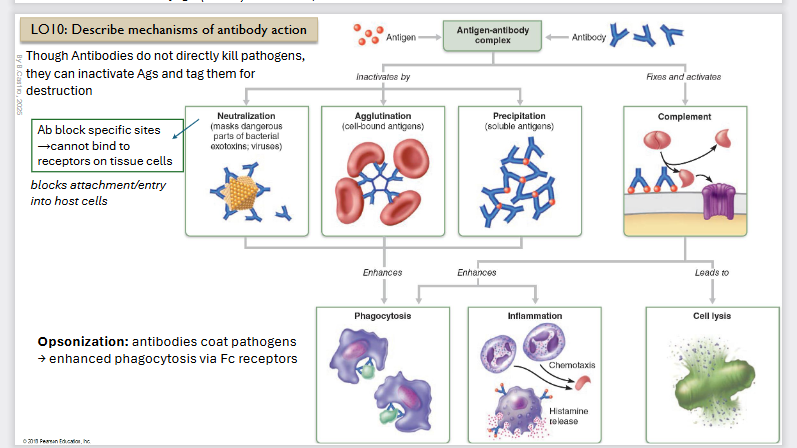
Mechanisms of antibody action
Inactivation
Activation
They are going to not diretly kill pathogens but they can inactivate Antigens and tag them for destruction
Initation:
Antigen + antibody complex:
then it can go two ways, inactivation or fixing and activation
Inactivation Steps
Neutralization:
Masks dangerous parts of bacterial exotoxins, viruses
Antibodies block specific sites → cannot bind to receptors on tissue cells
Agglutination
Cell bound antigens (they are bound to our cells)
Precipitation
Soluble antigens (3x)
Then it enhances
Through phagocytosis
Activation steps:
Complement (classical pathways which leads to lysis.
This leads to cell lysis
It enhances phagocytosis and inflammation
Opsonization: antibodies coat pathogens→ enhanced phagocytosis via Fc receptors blocks attachment/entry into host cells
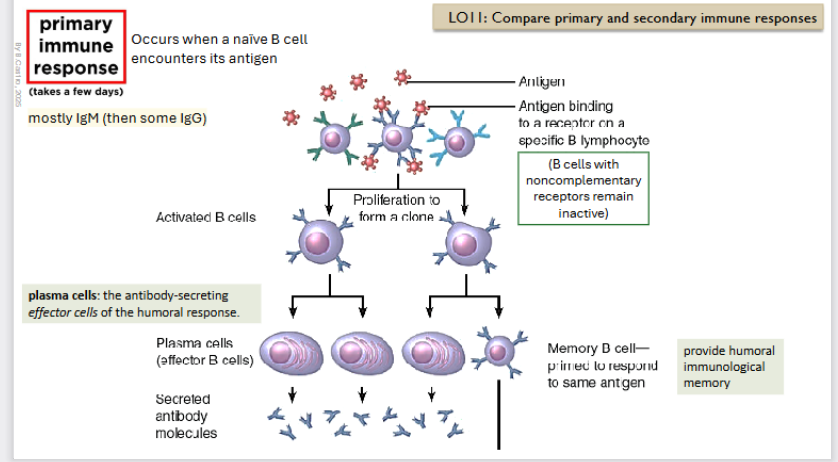
Primary immune response
Occurs when a naive B - cell encounters its antigen (in a secondary organ ofc)
Antigen binds to a receptor on a specific B lymphocyte. (B cells with non complementary receptors reamain inactive).
There is a proliferation to form a clone.
Creation of an Activated B cell
Creation of a Memory B cell → primed to respond to the same antigen (stays in the body)
Creation of plasma cells: these guys secrete antibody molecules (mostly IgM)
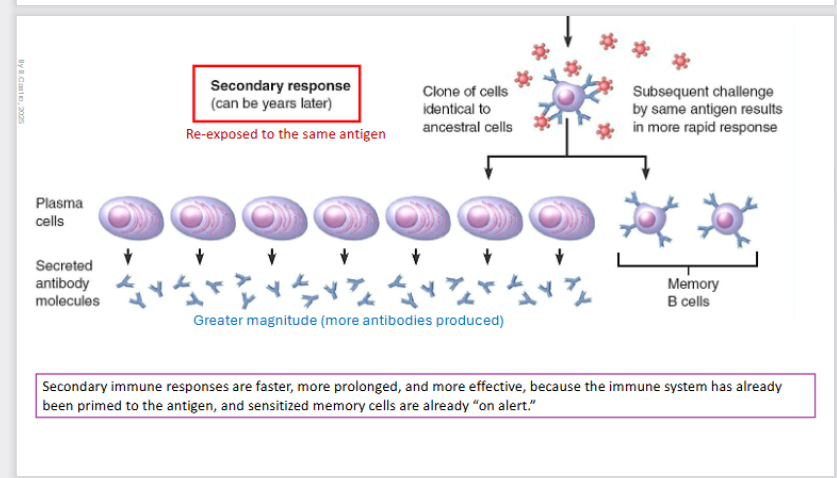
Secondary Immune response
Can happen YEARS later
There is reexposure to the antigen once more.
There is a clone of cells identical to the ancestral cells and the subsequent challenging by the same antigen results in a much quicker response.
Plasma cell creation once more and memory B cells.
There is a greater magnitude (more antibodies produced).
Secondary immune responses are faster, more prolonged, and more effective, because the immune system has already been primed to the antigen, and sensitized memory cells are already “on alert”
Primary immune response on a graph, relative concentrations of different classes of antibodies over time. Primary
Low concentration of plamsa cells generally
Immunoglobin M will be faster acting, then IgG acts.
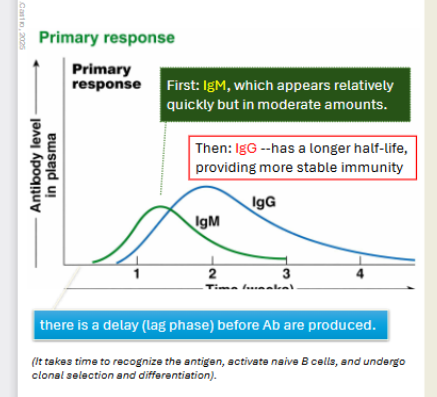
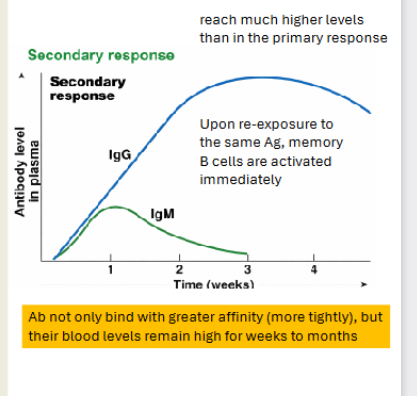
Secondary immune response on a graph, relative concentrations of different classes of antibodies over time. Secondary
Higher responses
Immunoglobin M will be faster acting but low again
However when IgG acts it will be significantly higher
Active Immunity (in humoral)
The body's immune system is directly stimulated to produce antibodies.
It provides an immunological memory.
Can be naturally aquired:
Infection (contact with pathogen)
Can be artificially aquired:
Vaccine (dead or attenuated pathogen)
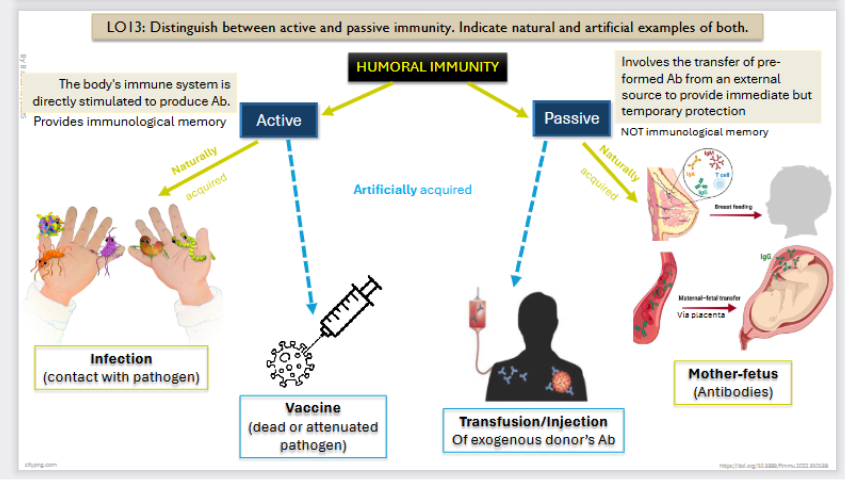
Passive Immunity (in humoral)
Involves the transfer of pre formed Ab from an external source to provide immediate but temporary protection
NOT immunological memory
Can be naturally aquired:
Mother - fetus (antibodies)
Can be artificially acquired:
Transfusion / injection (Of exogenous donor’s Ab)