topic 14: digestive system
1/78
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
79 Terms
what does the structure of the body and its physiological processes rely on?
nutrients absorbed by the digestive system
glucose for ATP
proteins found in skeletal muscle
lipids found in cell membrane
steroid hormones that surround and protect organs
calcium in bones
Na+/K+ for neural signaling
why is digestion important for human physiology?
proper digestion impacts nearly every system in the body, making it an important part of maintain health and homeostasis
what does the digestive system involve?
digestive tract (opening to external environment)
mouth to anus
accessory organs
e.g. teeth, tongue, salivary glands, liver, gallbladder, pancreas
what are the 4 basic processes of digestion?
digestion
absorption
motility
secretion
what is digestion?
breakdown of large food pieces into small molecules
mechanical - motility (chewing, breaking things down, stomach churning, food moving through tract)
chemical - enzymes with acid
what is absorption?
nutrients in lumen are transported into enterocytes (cells of the small intestine) line the villi of the small intestine → then are transported from the enterocytes into the blood or lymph
lots of surface area to maximize absoprtion
what is motility?
smooth muscle contracts in tract (no conscious thoughts)
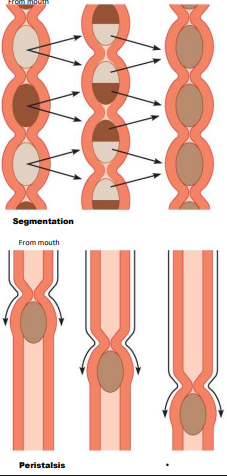
mixes food/chyme (segmentation, back and forth, and churning) helps with mechanical break down
move food/chyme (peristalsis) moves in right direction
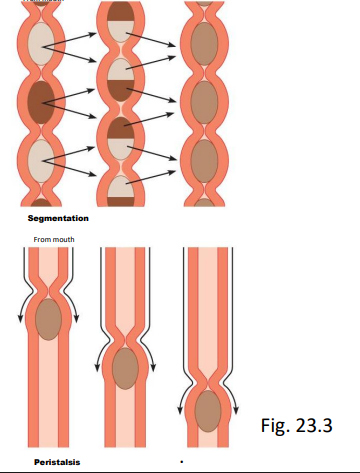
what is secretion?
digestive juice into lumen
acidic components with various enzymes
glands (endocrine)
where does digestion start?
in the mouth by mechanically breaking down food through chewing and chemically processing foods with enzymes in saliva
what do the salivary glands do?
secrete saliva that moistens (taste, speech, food manipulation) + prevents caries (contains lysozyme, antibodies)
PSNS in salivary glands?
stimulates secretion of thin, enzyme rich saliva (salivary amylase)
SNS in salivary glands?
mucus rich saliva
what are the processes occurring in the mouth?
digestion
mechanical - chewing (breaks food into smaller pieces and mixes it with saliva)
↑ surface area so that saliva will come in contact for chemical digestion
chemical digestion
absorption
what is chemical digestion in the mouth digestion of?
carbohydrates (starch/glycogen) —(salivary amylase, pH 7)—→ disaccharides + oligosaccharides
triglycerides ——(lipid lipase)—→ fatty acids + monoglycerides
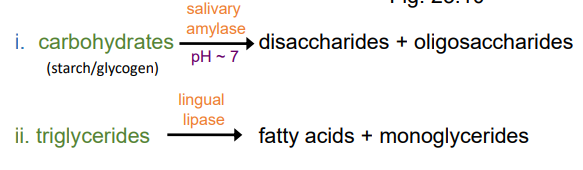
absorption in the mouth?
no foods
some drugs (e.g. nitroglycerin for angina = vasodilator)
what is the role of the pharynx and esophagus in digestion?
transport food from mouth to stomach via swallowing and peristalsis (contraction of smooth muscle)
swallowing (deglutition)
what are the 3 phases of swallowing (deglutition)?
buccal phase (voluntary)
pharyngeal phase (involuntary form here)
esophageal phase
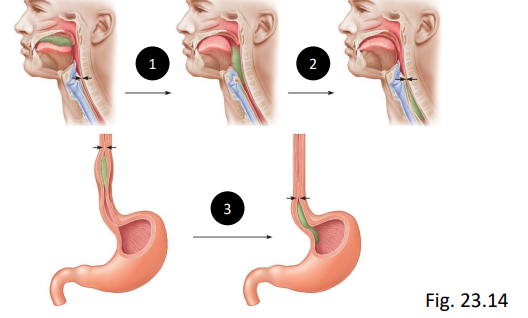
what happens during the buccal phase of swallowing?
food is compacted by the tongue into a “bolus” - moves to pharynx by tongue pressing on hard plate
voluntary
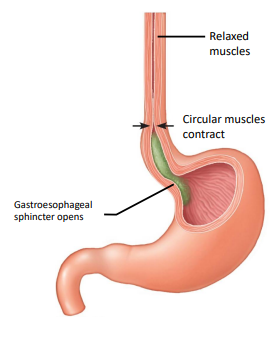
what happens during the pharyngeal phase of swallowing?
swallowing center (medulla) initiates swallowing reflex
skeletal to smooth muscle (involuntary from here)
what happens during the esophageal phase of swallowing?
food moves down esophagus via peristalsis (wave-like contractions of smooth muscle)
somatic motor neurons to skeletal muscle → upper 1/3
PSNS (via vagus nerve) to smooth muscle → lower 1/3
middle 1/3 = mix of both
during swallowing, why cant food enter (or re-enter) the mouth?
because tongue is pressed up against the hard palate
directional flow
during swallowing, why cant food enter (or re-enter) the nasopharynx?
because the uvula and soft palate are elevated, closing off the nasopharynx
during swallowing, why cant food enter (or re-enter) the trachea?
because the glottis and epiglottis (covers glottis) are closed during swallowing (as a result breathing temporarily stops when we swallow)
what does the stomach do in digestion?
mechanically churns food
chemically breaks down proteins with gastric acids and enzymes
regulates controlled release of partially digestion food (chyme) into the small intestine for further processing and absorption
↑ SA that chemicals can react to
what is protein chemically broken down by?
gastric acids and enzymes
how does digestion occur in the stomach?
mechanical - churning (motility) mixes food with gastric acid and enzymes
chemical digestion of the stomach consists of?
carbohydrates - salivary amylase remains active in the stomach until pH < 7
lipids - lingual lipase (tongue), gastric lipase (chief cells) are active until pH < 5-6
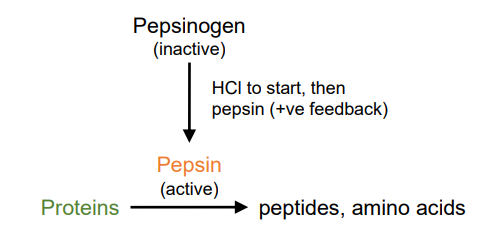
proteins - HCl (from parietal cells) denatures proteins and acts on pepsinogen (an inactive enzyme secreted by chief cells) to create the active enzyme pepsin. pepsin then breaks proteins into peptides and amino acids
low pH turns pepsinogen into active form
what digestions carbohydrates?
salivary amylase (active until pH < 7)
what digests lipids?
lingual lipase (tongue)
gastric lipase (chief cells)
active until pH < 5-6
what digests proteins?
HCl (from parietal cells) denatures
acts on pepsinogen (inactive) to create active enzyme pepsin (activated by low pH)
pepsin breaks down proteins into peptides and amino acids (+ve feedback)
absorption in the stomach?
food = very little (if any)
not happening at stomach because of thick mucus membrane
some drugs - alcohol, aspirin (penetrate mucous)
ulcers (H. pylori)
what does the small intestine do in digestion?
primary site for digestion and absorption of nutrients
digestion in the small intestine?
mechanical - segmentation and peristalsis
chemical - involves secretion from
pancreas
gall bladder (release bile into intestine)
intestinal wall
(accessory organs)
steps in chemical digestion in the small intestine
neutralize acid (so pancreatic enzymes can work)
pancreatic enzymes
intestinal wall enzymes
what happens during step 1: neutralize acid (so pancreatic enzymes can work)
chyme from stomach as a low pH that would damage the intestinal wall
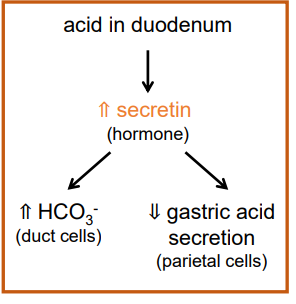
when acidic chyme is released into the duodenum, it triggers the secretion of the hormone secretin from cells in the intestinal wall
(low pH) secretin stimulates duct cells of the pancreas and gall bladder to secrete alkaline fluid (contains bicarbonate = HCO3-) that will neutralize the acid in chyme
can act as a buffer ↑pH and bind H+ removing from system
secretin also acts on the parietal cells of the gastric glands (stomach) to reduce acid secretion
regulation:
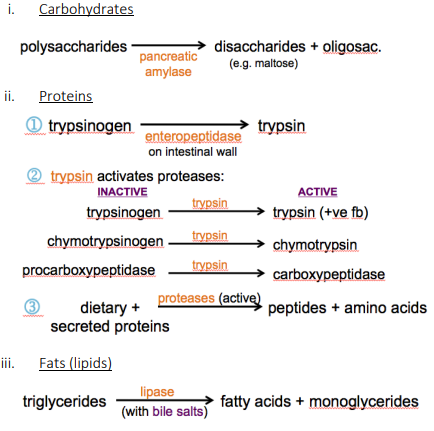
what happens during step 2: pancreatic enzymes (secreted into intestinal lumen from pancreatic acinar cells) continue chemical digestion
carbohydrates
polysaccharides —(pancreatic amylase)→ disaccharides + oligosacs. (e.g. maltose)
proteins
trypsinogen —(enteropeptidase on intestinal wall)→ trypsin
trypsin activates proteases:
inactive active
trypsinogen —(trypsin)→ trypsin (+ve fb)
chymotrypsinogen —(trypsin)→ chymotrypsin
procarboxypeptidase —(trypsin)→ carboxypeptidase
dietary + secreted proteins —(proteases (active))→ peptides + amino acids
fats (lipids)
triglycerides —(lipase w/ bile salts)→ fatty acids + monoglycerides
regulation of pancreatic enzymes secretion in step 2?
presence of fatty acids and amino acids in the duodenum stimulates the secretion of the hormones cholecystokinin (CCK) from enteroendocrine cells of the small intestine (cells in the guts secrete hormones)
what are the effects of CCK?
simulates (increases) pancreatic enzyme secretion
stimulates gallbladder contractions - releases bile into duodenum
decreases gastric motility (slows emptying of stomach) and decreases gastric secretions
what happens during step 3?
enzymes on the surface of microvilli of enterocytes further breakdown nutrients do that they are small enough to be absorbed
carbohydrates
di + oligosaccharides —-(disaccharidases + oligosaccharidases)→ monosaccharides
e.g. 1: sucrose —(sucrase)→ glucose + fructose
e.g. 2: maltose —(maltase)→ glucose + fructose
e.g. 3: lactose —(lactase)→ glucose + glucose
proteins
peptides —(aminopeptidases + dipeptidases)→ smaller peptides + amino acids
lipids
no longer further digestion (no lipase on microvilli of enterocytes(
what is a lactase deficiency?
causes lactose intolerance
lactose remains undigested and passes into the large intestine where bacteria will ferment it, resulting in symptoms like gas and diarrhea
absorption in the small intestine
transport of nutrients from lumen of small intestine into enterocytes, and from enterocytes into the blood or lymph
small intestine is the main site of absorption due to?
large surface area (folds, villi, microvilli)
nutrients are digested into molecules that are small enough to be absorbed
absorption of H2O in the small intestine?
~8500ml/day absorbed assuming
H2O ingested in food/drink = ~2000 ml/day
H20 from secretions = ~7000 ml/day
so ~9000 ml/day taken in, 500 ml/day lost due to large intestine (eliminate ½ liter of H2O a day; some mixed with fecal material and exit that way)
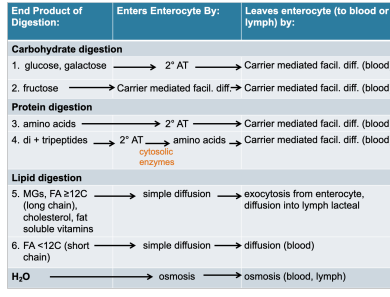
absorption table
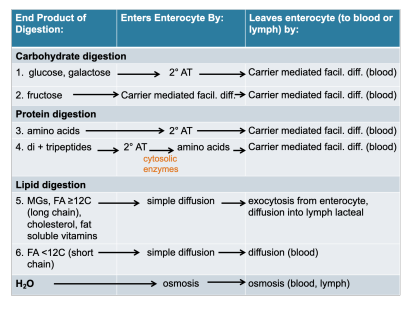
absorbed nutrients go?
to the liver via hepatic portal vein (blood)
into lacteals (lymph), and are carried through the lymphatic circulation (including the thoracic duct) to the left subclavian vein where they enter the blood
(lacteal → thoracic duct → left subclavian vein → blood)
fat digestion and absorption in the small intestine
required bile from:
liver (synthesizes)
gall bladder (stores)
can produce bile without gall bladder (lesser amount)
what does bile consist of?
water (H2O secretion)
bile salts (derived from cholesterol)
pile pigments (bilirubin from RBC breakdown) urine yellow
ions (HCO3-) (neutralize anything acidic)
detoxified/inactivated drugs. toxin, hormones, etc.
what is the function of bile salts?
emulsification
micelle formation
bile salt: emulsification
breaks up larger globules of fat into many droplets
↑SA to aid digestion
split fat molecules to smaller and smaller components
bile salts: micelle formation
keeps products of fat digestion in solution
what is a micelle?
= a vesicle-like structure formed from bile salts and phospholipids that is filled with monoglycerides and fatty acids
interior = hydrophobic
exterior = hydrophilic
keep it separate in solution so the fats don’t rejoin
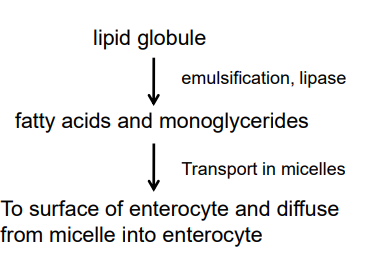
fat digestion and absorption: what happens in the lumen of the small intestine?
a lipid globule is emulsified by bile salts and chemically broken down by the enzyme lipase to form fatty acids and monoglycerides
fatty acids and monoglycerides are packaged in micelles
micelles transport fat digestion products to the surface of the epithelial cells (enterocytes) that line the lumen of the small intestine
the fatty acid and monoglyceride contents of the micelle are then able to diffuse into the enterocyte
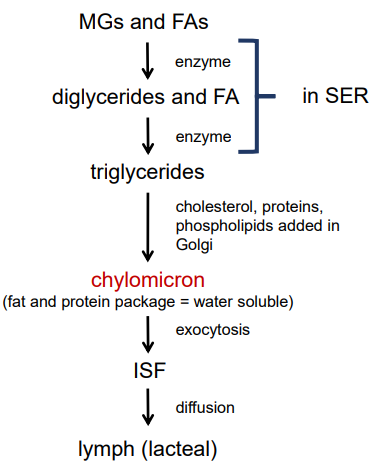
fat digestion and absorption in enterocytes (small intestine)
the products of fat digestion (fatty acids and monoglycerides) undergo reassembly into triglycerides and packaging to make them water soluble for transport in the lymph/blood
what are the steps in fat digestion and absorption in the enterocyte?
reassembly of triglycerides
in the smooth endoplasmic reticulum, monoglycerides and fatty acids are acted on by enzymes that convert them back into triglycerides
chylomicron formation
in the Golgi apparatus, the triglycerides are packaged with cholesterol, phospholipid, and proteins to form a water soluble package called a chylomicron
exocytosis of chylomicrons
chylomicrons are packaged into vesicles and released into the interstitial fluid (travel down top side where picked up by lymphatic vessels)
transport into the lacteal
chylomicrons diffuse into the lymph lacteal (they are too large to enter the blood capillaries)
gastric motility/secretion
3 regulatory phases
cephalic phase
gastric phase
intestinal phase
cephalic phase of gastric motility/secretion
prepares stomach for goof (start at level of nervous system)
triggers = thought, sight, smell, taste of food
PSNS (vagus nerve) and enteric nervous system coordinate secretions and motor responses of the stomach
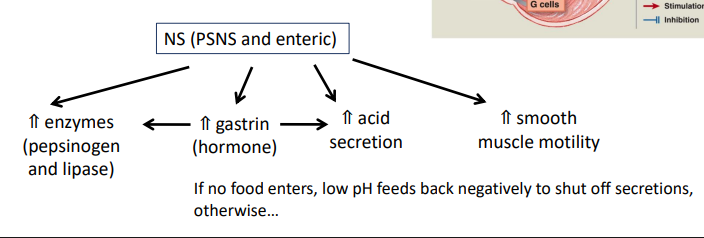
gastric phase of gastric motility/secretion
food = buffer - ⇓pH slowly; reaches 3 when stomach nearly empty (trigger for stomach)
when pH is less than 3
shuts down NS (enteric) which ⇓ acid
⇓ gastrin therefore ⇓ acid
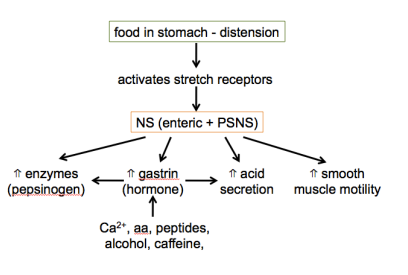
intestinal phase of gastric motility/secretion
controls rate of chyme (=food + gastric juice) entry into duodenum
gastric emptying is regulated so that:
acid can be neutralized in small intestine
tonicity does not overwhelm small intestine
time for digestion/absorption in small intestine (as slow down motility)
intestine is for absorption so can’t have mucus layer
what happens during the intestinal phase?
initially (for a short time) get ⇑ gastric secretion (getting chyme into intestine) - duodenal gastrin release (due to duodenal stretch)
then inhibitory signals
what goes inhibitory signals cause?
⇓ gastric motility (slows emptying) due to
CCK
enterogastric reflex (enteric NS)
⇓ gastric secretion (acid, enzymes)
inhibitory signals cause ⇓ gastric motility (slows emptying) due to CCK
released due to presence of fatty acids and amino acids
hormones inhibit gastric motility
sensory stretch → chemoreceptors
inhibitory signals cause ⇓ gastric motility (slows emptying) due to enterogastric reflex (enteric NS)
neural reflex that inhibits gastric motility to allow time for digestion and absorption in the small intestine
triggered by presence of amino acids/peptides or acid in duodenum; duodenal stretch, hypertonicity
sensory receptors (stretch receptors, chemoreceptors) are activated
signals are sent directly by the enteric nervous system and to the central nervous system to decrease PSNS activity and increase SS activity
increased SNS signaling decreases motility
inhibitory signals cause ⇓ gastric secretion (acid, enzymes) due to
secretin release due to acid (responds to ⇓pH in small intestine; -ve)
CCK released in response to presence of amino acids and fatty acids in duodenum
enterogastric reflex (increases SNS signaling decreases secretion)
motility in the large intestine
haustral contractions
slow, weak - move material down tube - allow mixing, absorption of salts, H2O (no more urgency)
mass movement
due to food in stomach, via gastrocolic reflex = powerful waves of contraction from transverse colon to rectum
move to fecal mass to rectum - initiates urge to defecate (pushing food already in large intestine further down)
rectal (defecation) reflex
stimulus = feces in rectum (stretch receptors in rectal wall)
CNS integration = in sacral segment of spinal cord (PSNS) closest to where rectum is
effector = smooth muscle (ANS) of rectum contracts, internal anal sphincter relaxes (force fecal out)
external anal sphincter (skeletal muscle) = under voluntary control i.e. not part of reflex
have control: constriction so you don’t poop yourself
digestion in large intestine
none, but bacterial fermentation of indigestion nutrients
bacterial synthesize some vitamins (B6, B5, K, folate, biotin)
not capable of making on your own → bacteria synthesis
any undigested material can be used by bacteria
slow → majority of absorption has already happened
absorption in the large intestine
H2O ~400 ml/day via osmosis (~100 ml/day lost in feces)
depends on how much water you drink or sweat
some fermentation products - gases, vitamins
reuptake of sodium (actively)
more bacteria = increase fermentation activity
drugs (rectally) - e.g. anesthetics
large intestine secretion
K+, HCO3- (neutralize HCl)
actively dumped out
fate of absorbed nutrients: glucose
from blood into body cells (carrier mediated facilitated diffusion) → insulin ⇑ uptake into skeletal muscles, liver cells, fat cells (adipocytes)
what is glucose used for in cells?
catabolism by cells → ATP production
anabolism → stored glucose as glycogen (75% in skeletal muscles, 25% in liver) - represents 1% of body’s energy stores
activation of SNS breaks it down back to glucose
fate of absorbed nutrients: lipids
cholesterol is used to make steroid hormones, bile salts, cell membranes (builds parts i.e. phospholipids and proteins)
triglycerides in blood are delivered to tissues
lipase on the endothelial cells of organs breaks down triglycerides into 3 fatty acids and glycerol
fatty acids and glycerol are transported into tissues cells, where thy can be
used for ATP production (except by neurons)
stored as triglycerides in adipose tissue (represents 99% of body’s energy stores)
used to synthesize cell parts e.g. membrane, myelin (extension of cell membrane; insulation)
fate of absorbed nutrients: amino acids
enter cells by secondary active transport or facilitated diffusion
GH ⇑ entry into most cells → synthesize protein
insulin ⇑ entry into skeletal muscle cells (not exclusive to glucose)
in cells, amino acids are used mainly for protein synthesis (bind to tRNA)
can be used for energy (ATP synthesis) when glucose is low e.g. starvation)
what is metabolic rate?
body’s rate of energy use - sum of all chemical reactions and mechanical work
breaking down and building up
what are the factors of metabolic rate?
SNS, ⇑ metabolic rate
hormones e.g. epinephrine, thyroid hormone, ⇑metabolic rate
body temp - 1°C rise ⇒ 10% ⇑ in metabolic rate
exercise, ⇑ metabolic rate (activates SNS, loose weight when using energy)
food ingestion, ⇑ metabolic rate (need energy to eat)
sleep, ⇓ metabolic rate (less anabolic)
what is basal metabolic rate (BMR)
energy body needs for essential activities e.g. HR, kidney function, breathing etc.
when sleeping you have metabolic rate to keep you alive
digestion hormone summary from stomach and duodenum
gastrin
secretin
CCK
gastrin
⇑ acid, gastric enzyme secretion (lipase and pepsinogen)
secretin
⇑ alkaline fluid secretion (duct cells of pancreas, gallbladder)
⇓ gastric secretion
CCK
⇑ pancreatic enzyme secretion
⇑ contraction of gallbladder
⇓ gastric motility, secretion