Unit 3: CV System 2
1/51
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
52 Terms
what is cardiac output?
the volume of blood pumped each minute by each ventricle
what is stroke volume?
the amount of blood pumped by the LV in 1 contraction
what is the average HR, SV, and CO?
average HR is 70 bpm, average SV is 70-80 ml/beat, and average CO is 5600 ml/minute
what is the equation to find CO?
CO = HR x SV
how is cardiac rate regulated?
Cardiac rate is regulated by the autonomic nervous system, hormones, and intrinsic factors such as the pacemaker cells in the sinoatrial node. It goes all the way down to the cellular level, where adequate APs are needed to depolarize the different nodes in the heart.
how does the sympathetic nervous system affect the heart?
increases the rate of diastolic depolarization, increase cardiac rate, increased conduction rate, increased strength of contraction
how does the parasympathetic nervous system affect the heart?
decreased rate of diastolic depolarization, decreased cardiac rate, decreased conduction rate
how does the autonomic nervous system play a role in cardiac regulation?
strongly affect the SA and the AV nodes and the rate of depolarization and conduction rate, and sympathetic nerve effects control the strength of atrial muscle and ventricular contraction
what 3 variables affect SV?
EDV/preload, ESV/afterload, and contractility
what is the end diastolic volume?
the amount of blood in the ventricles at the end of diastole, just before the heart contracts. It is affected by preload which is the amount of stretch of load on the myocardial wall pre-contraction
what is end systolic volume?
the volume of blood in the ventricles at the end of systole, just before the heart begins to fill again during diastole. is affected by afterload, or the resistance faced by the heart to pump blood in to the aorta
what is contractility?
the strength of ventricular contraction
what is the ejection fraction (EF)?
the percentage of blood that is ejected from the ventricles during each contraction compared to the total blood volume in the ventricles at the end of diastole. It is a key indicator of heart function. Normally it is approximately 60% of the EDV
what is the Frank-Starling Law of the Heart?
states that the strength of the heart's contraction is directly related to the initial length of the cardiac muscle fibers. This means that an increase in the volume of blood filling the heart (preload or EDV) leads to a stronger contraction and greater stroke volume. (see image for direct visualization). Increased contractility also increases SV
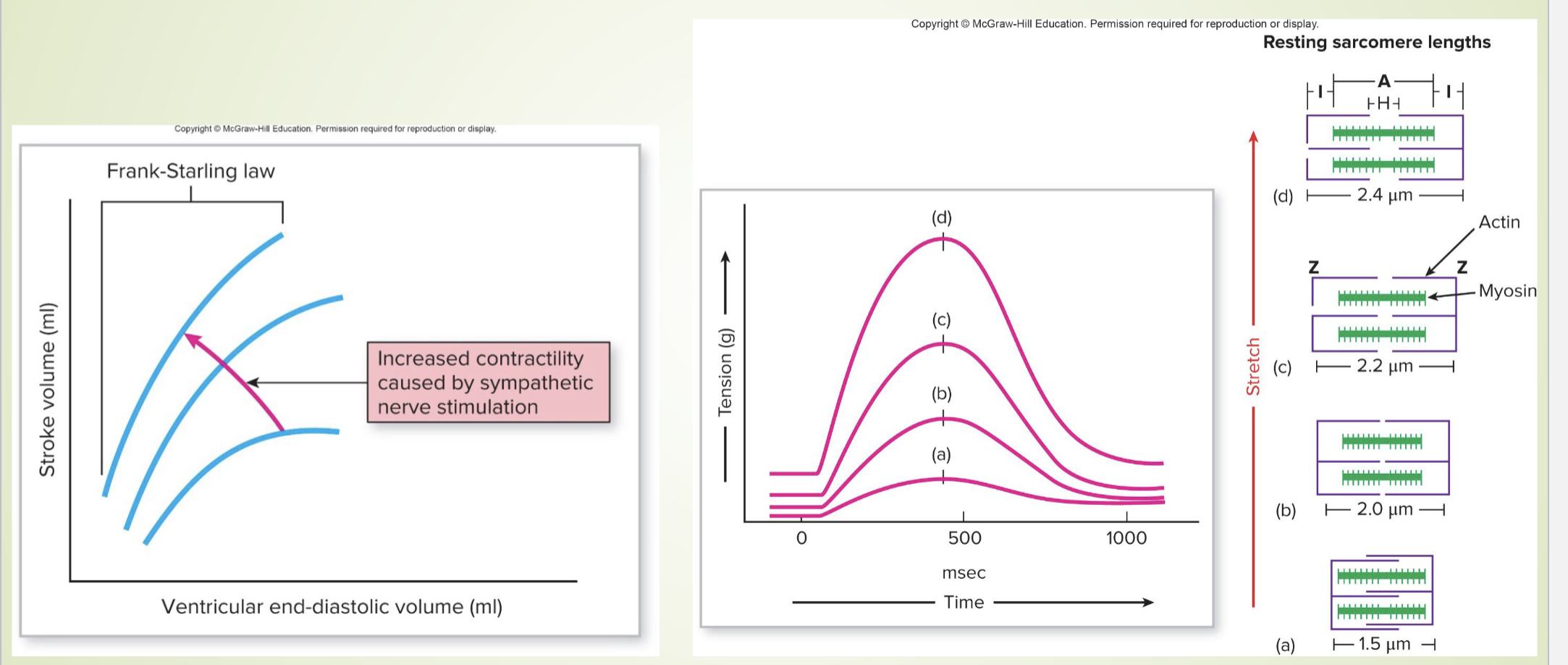
what is preload?
the degree of muscle fiber stretch at the beginning of contraction
what is afterload?
the resistance faced by the heart to pump blood into aorta
how does an increase in afterload affect SV?
it decreases the SV
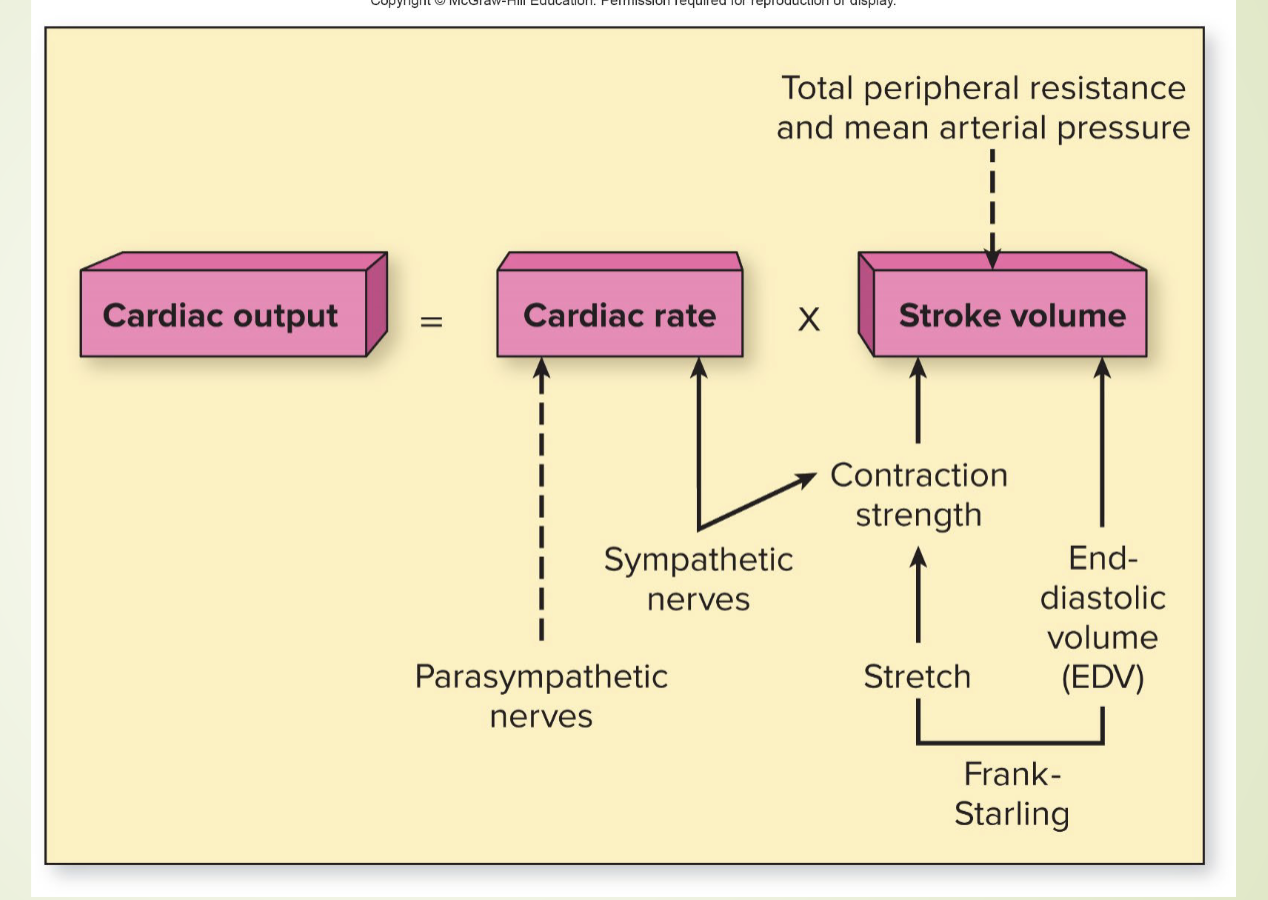
explain the attached graphic
cardiac output is affected by the factors that affect the cardiac rate and the stroke volume. Things that affect the cardiac rate are parasympathetic and sympathetic nerve (to decrease or increase), and things that affect SV are the contraction, stretch, and EDV, which are respectively affected by the sympathetic nerves and the frank-starling law
how does venous return affect CO?
venous return directly affects the EDV, which affects the magnitude of CO (when increasing the venous return this increases the end-diastolic volume, leading to a higher stroke volume due to the Frank-Starling mechanism. This ultimately increases cardiac output)
what is the pressure in the veins like compared to arteries?
due to the high compliance of veins, their pressure is lower than that of the arteries
what factors affect the venous return?
total blood volume, venous pressure (which is the driving force for blood return), and the compliance of the veins (in general veins have high compliance), as well as respiration since it exerts some pressure that will affect the venous return (these all then affect EDV)
When a person donates a pint of blood, which would be increased compared to pre-donation values?
the heart rate and the total peripheral resistance (since blood becomes more viscous due to loss of fluid)
what is osmotic pressure responsible for?
responsible for the movement of water across semi-permeable membranes, helping to maintain fluid balance between blood vessels and surrounding tissues.
what is required for fluid exchange?
there needs to be a difference in pressure between the tissues, or a net filtration pressure in which the hydrostatic pressure of blood in the capillaries minus the hydrostatic pressure of the fluid outside of the capillaries is a positive value
what is colloid osmotic pressure?
osmotic pressure that is due to proteins dissolved in fluid, blood plasma has higher colloid osmotic pressure than interstial fluid, this difference is called oncotic pressure, (normally is 25 mmHg which favors movement into capillaries)
what are starling forces?
combination of hydrostatic pressure and oncotic pressure that predicts movement of fluid across capillary membranes
what is edema?
there is excessive accumulations of interstitial fluids in tissues spaces, too much water leaves the blood capillaries or the water is not being reabsorbed efficiently back into the blood, interferes with capillary transport
what can cause edema?
since edema is a symptoms and not a disease, can be caused by other diseases or things such as CHF, chronic venous insufficiency, or result of immobility, pregnancy, pressure from garments/jewelry/bandages
what is the function of the lymphatic vessels?
transport from interstitial spaces back to circulation, collect lymphatic fluid from organs and prevent accumulation of excess fluid, and immunologic effects
how can blood flow be described?
the change in pressure/ resistance
what is resistance dependent on?
the length of the vessel, the viscosity of the blood (which would both increase resistance when increased), and the radius of the blood vessel (which would decrease the resistance when increased)
what is vasoconstriction?
decrease in blood vessel diameter, increases SVR (systemic vascular resistance)
what is vasodilation?
increase in diameter of blood vessels, decrease SVR
what affects blood pressure?
cardiac output, systemic vascular resistance, blood volume, and blood viscosity will cause increases when increased
what is the equation for arterial BP?
CO x TPP (total peripheral resistnace/vasoconstriction)
what is the role of the baroreceptors in BP?
specialized sensors located in the walls of blood vessels that detect changes in arterial blood pressure. They send signals to the central nervous system to help regulate blood pressure by adjusting heart rate and vascular resistance.
how can we measure BP?
sphygmomanometry
how can discrepancies be caused with sphygmomanometry?
incorrect cuff size selection, placement of cuff, technique, age, race/ethnicity, gender, diet, body weight
what is a more invasive way to measure BP ?
a direct measurement via a needle cannula into an artery, saline filled tubing, pressure bag, transducer/infusion flushing system, and the cannula connected ot an electronic pressure monitor
what is pulse pressure?
the difference between BP at systole and at diastole, is a reflection of stroke volume
what is mean arterial pressure (MAP)?
the average pressure in the arteries in one cardiac cycle, is significant bc the difference between MAP and venous pressure drives blood into capillaries
what are the AHA criteria for blood pressure categories?
see image
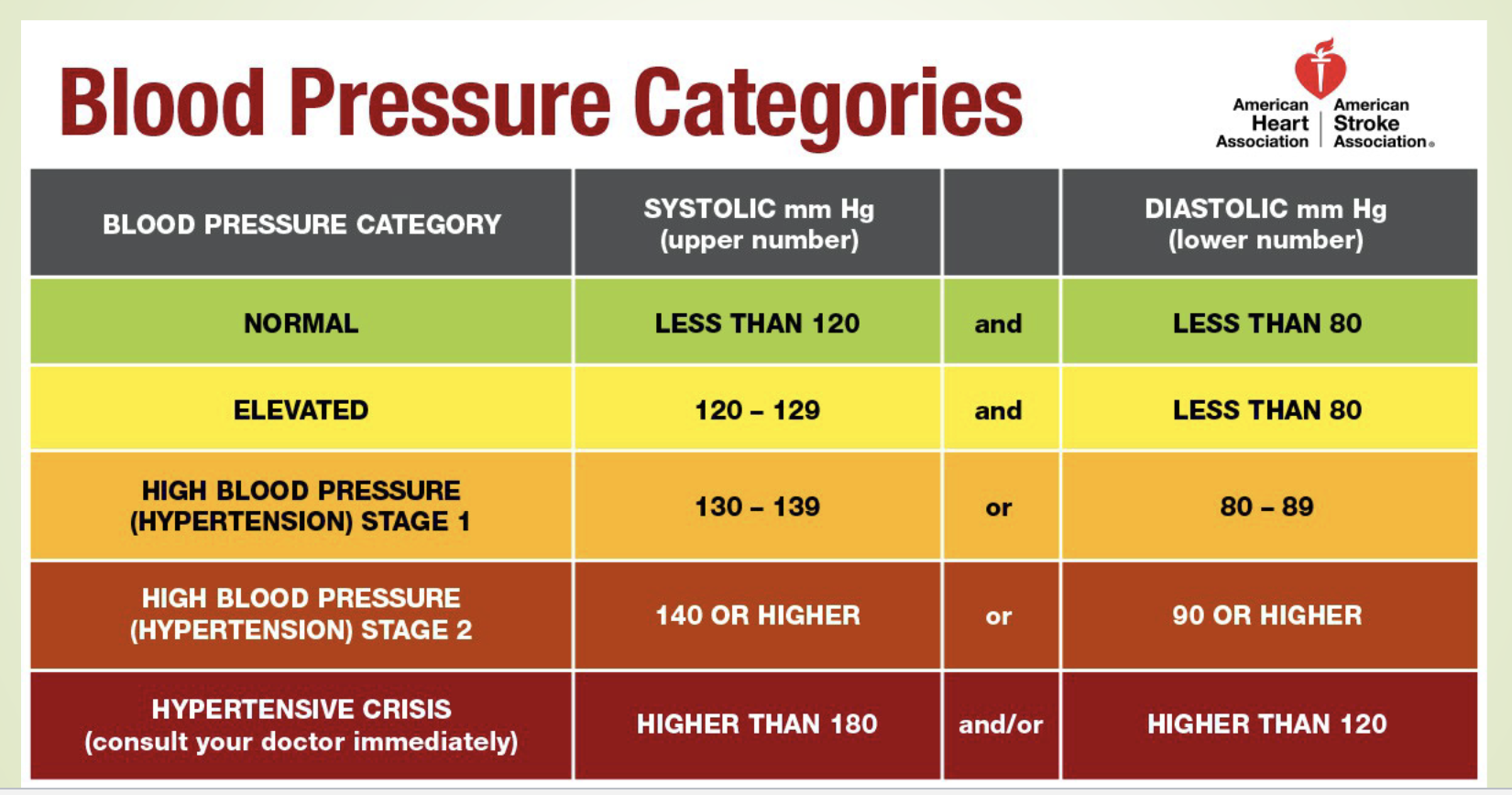
why do we need to treat HTN?
untreated can lead to stroke, vascular damage, arrythmias, cardiac arrest, artherosclerosis
what are treatments for HTN?
lifestyle modifications, movement/exercise, K+/Ca+ supplements, diuretics, beta blockers, ACE inhibitors
what is preeclampsia?
a condition that affects about 8% of the women who are pregnant beyond their 20th week, a new onset of HTN in which thrombocytopenia and proteinuria may be present, this lowers the plasma protein concentration and oncotic pressure, producing edema and swelling of the feet, legs, and hands, believed to stem from dysfunction of the placenta, and if becomes severe, HTN can cause seizures and stroke, only cure is delivery of the baby
what is circulatory shock?
occurs when there is inadequate blood flow to match oxygen usage in the tissues, leading to cellular dysfunction and potential organ failure. there are various types including hypovolemic shock and septic shock
what are the early symptoms of circulatory shock?
decrease pulse pressure, and increase diastolic pressure, decreased Na+ concentration, increased osmolality, increased pH (alkalosis) due to hyperventilation, slight restlessness, occasionally warm, dry skin
what are the late symptoms of circulatory shock?
decreased systolic pressure, decreased volume, and decreased pH (acidosis) due to metabolic acids, cold and clammy skin, cloudy senses
what is hypovolumemic shock
a type of ciruclatory chock, due to low blood volume from an injury, dehydration, or burns. Characterized by decreased CO, and decreased BP, blood is diverted to the heart and brain at the expense of other organs, compensations includes baroreceoptor reflex
what is septic shock?
type of circulatory shock in which there is dangerously low BP due to an infection, bacterial toxins induce NO production, causing widespread vasodilation, and mortality rate is high 50-70%, this is a MEDICAL EMERGENCY
what is congestive heart failure?
occurs when CO is not sufficient to maintain blood flow required by the body, caused by MI, congenital defects, HTN, aortic valve stenosis, or disturbances to electrolyte levels, present similar to hypovolemic shock in symptoms and response
what are the types of CHF?
left side failure which raises left atrial pressure and produces pulmonary congestion and edema causing shortness of breath and right side failure in which right atrial pressure increases and produces systemic congestion and edema