medicine osce
1/66
Earn XP
Description and Tags
potentially malignant and fungal
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
67 Terms
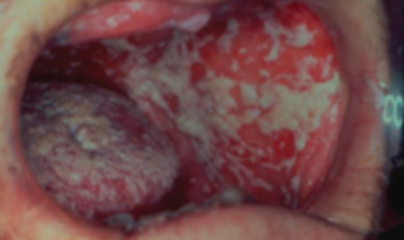
what is this condition
acute pseudomembranous candidiasis (thrush)
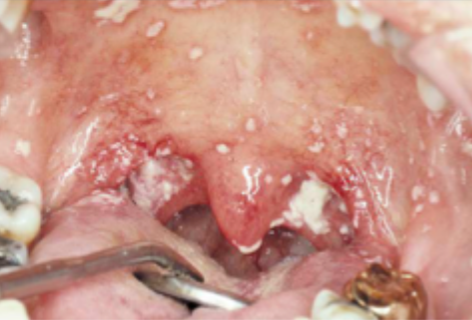
what is this condition
pseudomembranous candidiasis
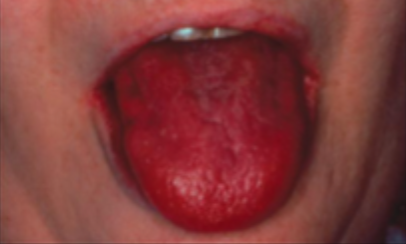
what is this condition
acute atrophic candidiasis
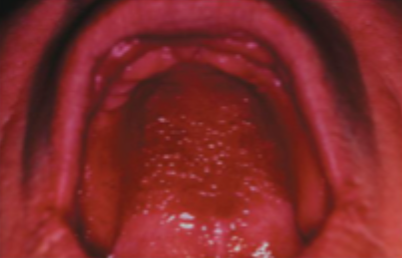
what is this condition
chronic atrophic candidiasis
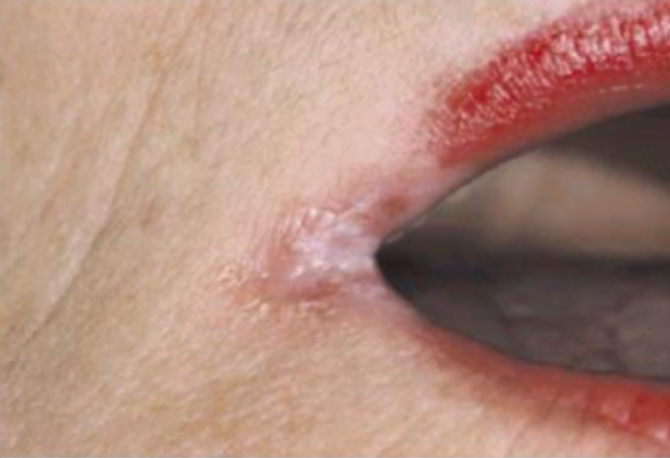
what is this condition
angular chelitis
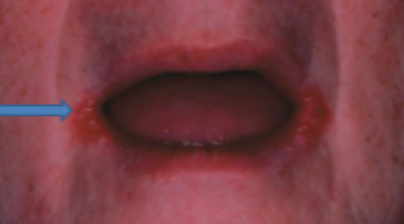
what is this condition
angular chelitis
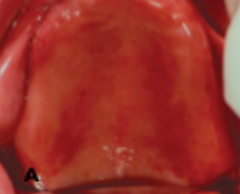
what is this condition
angular stomatitis (perieche) stage 1
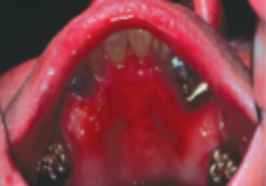
what is this condition
denture stomatitis (stage 2)
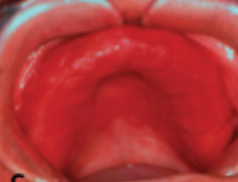
what is this condition
denture stomatitis (stage 2)
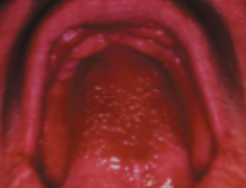
what is this condition
denture stomatitis (stage 3)
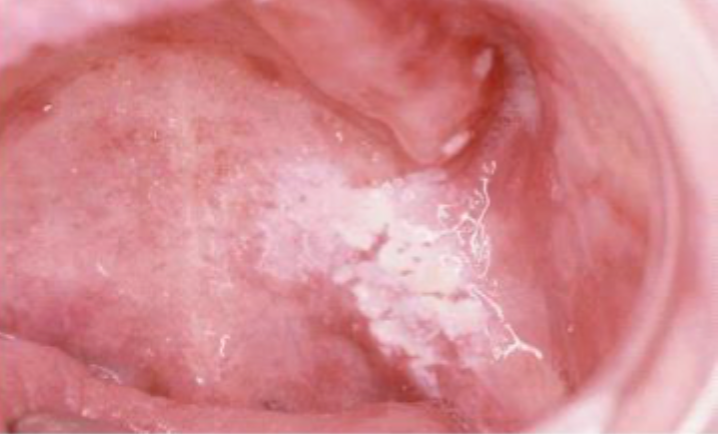
what is this condition
chronic hyperplastic candidiasis
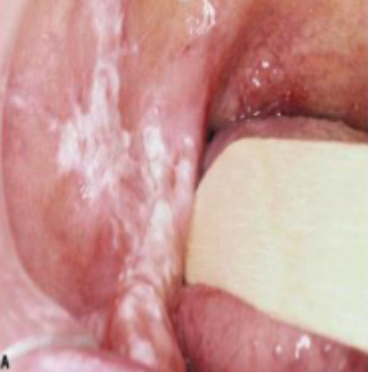
what is this condition
chronic hyperplastic candidiasis
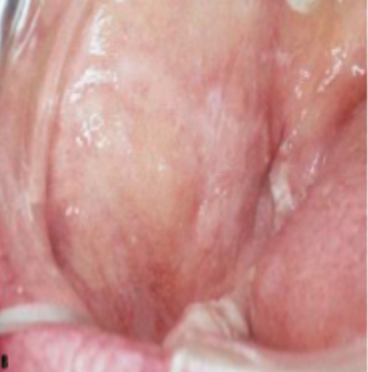
what is this condition
chronic hyperplastic candidiasis
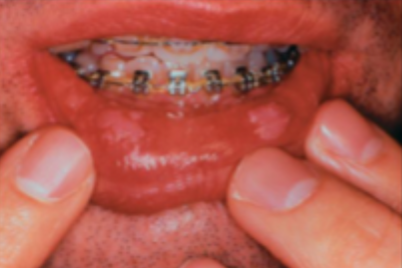
what is this condition
chronic hyperplastic candidiasis
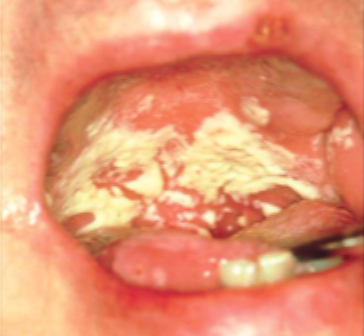
what is this condition
hyperplastic candidiasis
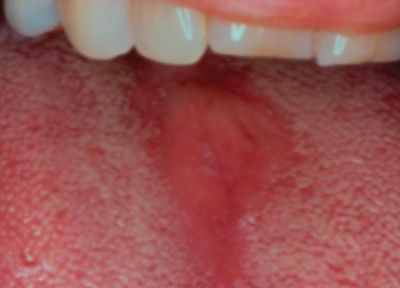
what is this condition
median rhomboid glossitis
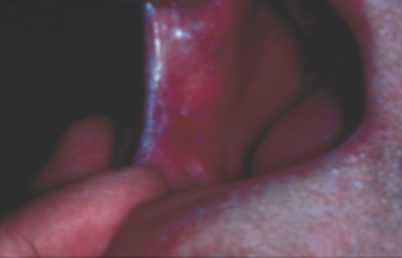
what is this condition
candidal leukoplakia
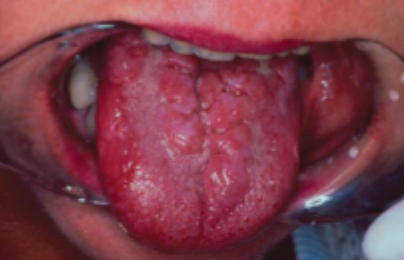
what is this condition
chronic mucocutaneous candidiasis
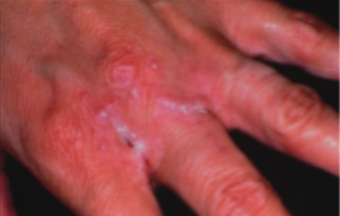
what is this condition
chronic mucocutaneous candidiasis
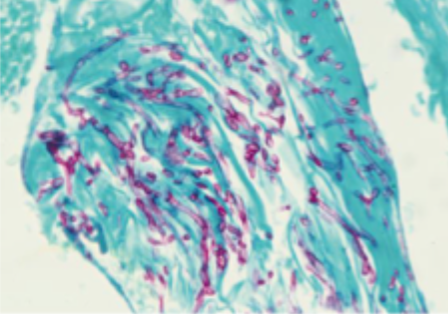
what is this test, and what is it used for
pas stain » used to diagnose candida
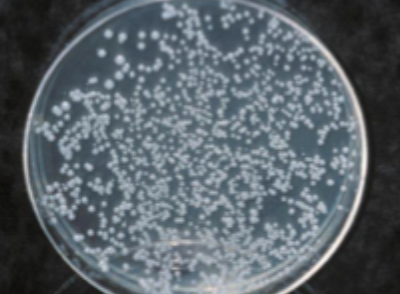
what is this test called, and what is it used for
corn meal agar candidate growth » used to diagnose candida
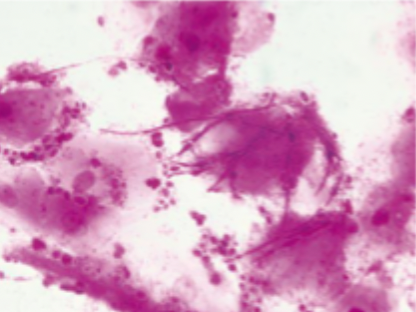
what is this test called, and what is it used for
gram stain with hyphae and myceliae » used to diagnose candida
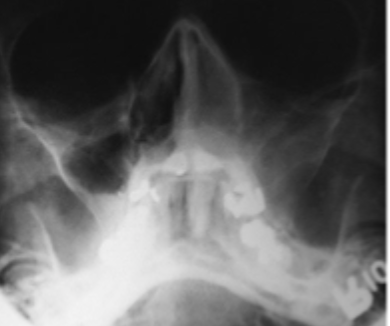
what is this condition
mucormycosis
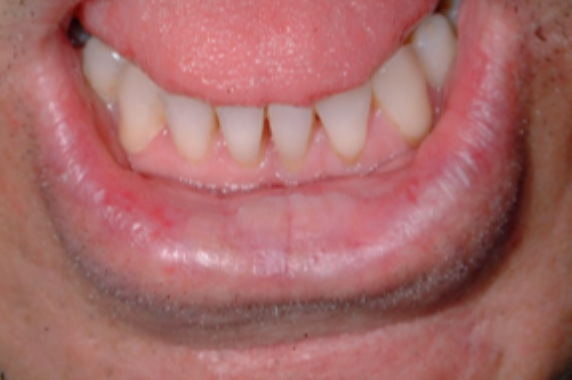
what is this condition
actinic chelitis
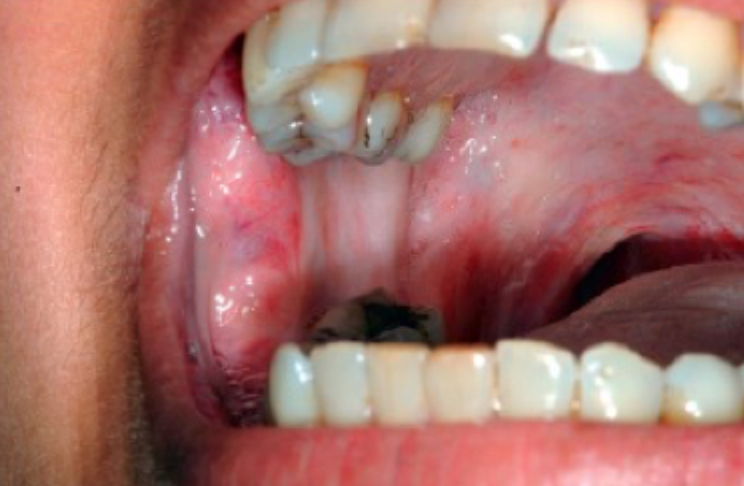
what is this condition
oral submucous fibrosis
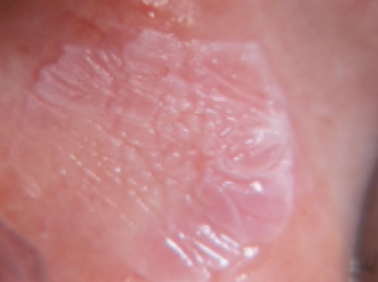
what is this condition
homogenous leukoplakia
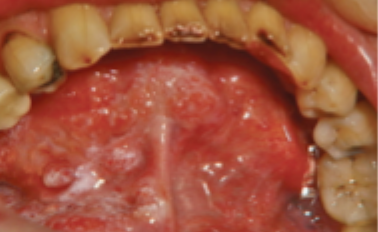
what is this condition
non-homogenous oral leukoplakia
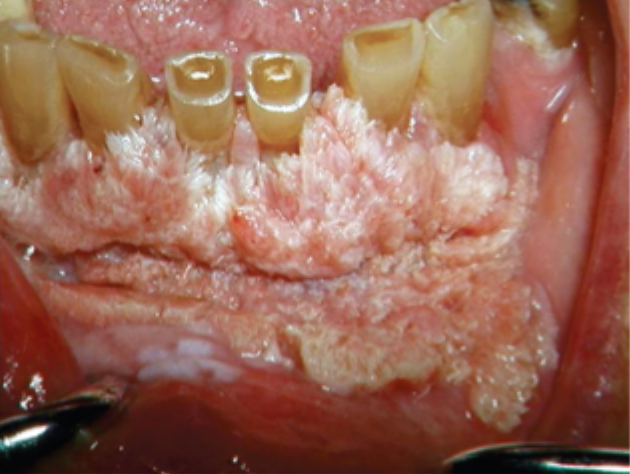
what is this condition
verrucous oral leukoplakia
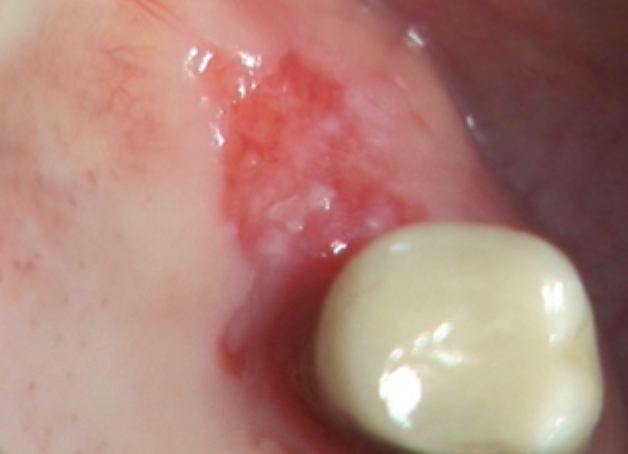
what is this condition
erythroplakia
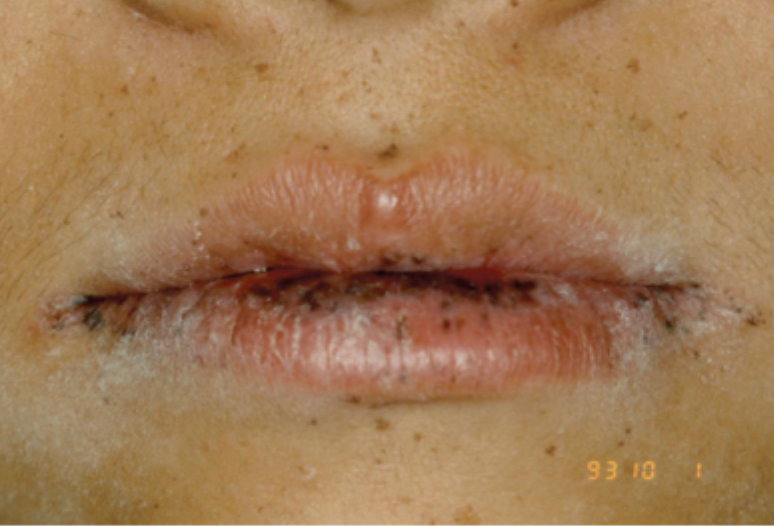
what is this condition
peri-oral melanosis
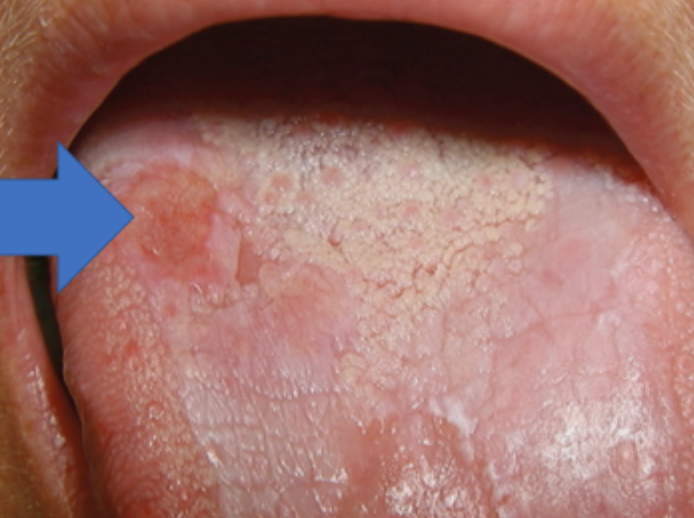
what is this condition
OSCC developed in plaque-like oral lichen plants
actinic chelitis features
sun overexposed individuals
smooth or scaly friable patch OR may involve entire lip
palpably thick with small grey-white plaques
develops into warty nodules » OSCC
management of actinic chelitis
PREVENTION » esp for high risk (photosensitive, xeroderma pigmentosum, transplant)
wearing broad brimmed hats
use UV sunscreen
oral submucous fibrosis features
betel quid chewers
tightening of buccal, palatal and lingual mucosa
trismuis
grade 1 oral submucous fibrosis
oral opening >35mm
grade 2 oral submucous fibrosis
oral opening 20-35mm
grade 3 oral submucous fibrosis
oral opening <20mm
grade 4 oral submucous fibrosis
oral opening <20mm + premalignant disease
grade 5 oral submucous fibrosis
oral opening <20mm + oral squamous cell carcinoma
which grades of OSMF should be sent for biopsy
grade 4 and 5
management of oral submucous fibrosis
physiotherapy (jaw opening exercises) + correcting nutritional deficiencies (iron and vitamin B)
cox-2 inhibitors » hyaluronidase, intralesional corticosteroids
ineffective but may be used: surgery, placenta, interferon gamma

what is this device and what is it used for
physic device for grade 1 and 2 OSMF
features of homogenous leukoplakia
white
well demarcated plaque
identical pattern throughout entire lesion
features of non-homogenous leukoplakia
white patches or plaques
intermingled with red
features of verrucous leukoplakia
white papillary projections
management of oral leukoplakia
excision
cessation of tobacco, betel, alcohol
ineffective: physio, retinoids (temporary effect, only used if difficult to access), radio/chemo (because it isn’t malignant)
when to excise vs wait+watch oral leukoplakia
no dysplasia » wait and watch
mild dysplasia (buccal, hard palate, dorsal tongue) » wait or remove
mild dysplasia (anywhere else) » remove
moderate/severe dysplasia » remove
features of erythroplakia
red lesion
asymptomatic; sometimes burning sensation when eating
reverse smoking chutta
peutz-jeghers syndrome features
multiple small pigmented macule of lips + perineal skin, hands, feet
oral lichen plants features
risk of malignant transformation in oral mucosa, not necessary with lesion
local predisposing factors for candidiasis
dentures
smoking
atrophic constitution
inhalation steroids
topical steroids hyperkeratosis
oral microflora imbalance
quality and quantity of saliva
general predisposing factors for candidiasis
immunosuppressive diseases + drugs
chemotherapy
endocrine disorders
hematinic deficiencies
features of acute pseudomembraneous candidiasis
patchy white plaque/flecks
scrapable
rapid onset on bad taste + burning sensation
features of acute atrophic candidiasis
red patch » atrophic or erythematous, painful
minimal pseudomembrane
patient likely to have iron deficiency anemia
stage 1 denture stomatitis // chronic atrophic candidiasis
numerous palatal petichae
stage 2 denture stomatitis // chronic atrophic candidiasis
diffuse erythema
stage 3 denture stomatitis // chronic atrophic candidiasis
tissue granulation or nodularity
management of denture stomatitis
avoid dentures for some time
soak denture in boric acid or house bleach
apply nystatin anti fungal cream on fitting surface of denture
features of angular stomatitis (perleche) // angular chelitis
red-fissured scales in angle of mouth
older patient with reduce VDO
chronic hyperplastic candidiasis
firm white leathery plaques
cheeks, lips, palate, tongue
stained with PAS
features of median rhomboid glossitis
erythematous patch of atrophic papillae in central area of dorsum of tongue
features of chronic multifocal candidiasis
ill fitting dentures
dorsum of tongue, midline of palate, angular chelitis, denture bearing areas
features of chronic mucocutaneous candidiasis
localized + diffuse » nails + skin
syndrome associated » endocrine syndromes
treatment of candidiasis in infants
nystatin syrup 100k IU » 1mL 4×day 7-10 days
treatment of candidiasis in adults
nystatin 1 tab 4xday 7 days (sucking) » if resistant extend for 21 days
amphotericin B 100mg/mL 4x day
itraconazole oral suspension » 100-200mg 1xday 2 weeks
ketaconazole 200mg 1xday 2 weeks
fluconazole 100mg 1xday 2 weeks
management of hiv associated candidiasis
flucoconazole
if resistant » itraconazole
features of mucormycosis
maxillary sinus fills with microbial colonies + necrotic tissue
destruction of osseous antral walls
diabetes or immunocompromised