Interpreting Lab Values
1/48
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
49 Terms
5,000-10,000 mm3
<2,500 or >30,000 mm3
Reference range for WBCs
Possible critical values for WBCs
WBCs High & Low
-Causes: Infection, inflammation, immune system disorder, severe stress/pain
-Presentation: Fever, fatigue, bleeding/bruising, frequent infections
-Causes: Chemotherapy/radiation, dietary deficiency, autoimmune disease
-Presentation: Frequent/persistent infections, headache/stiff neck, sore throat, fever/chills/night sweats
Clinical implications for High WBCs
Clinical implications for low WBCs
Consider timing of PT session: these tend to be lowest during the early morning and highest during the late afternoon
-Consider timing of PT session
-Monitor for signs/symptoms of infection
-Monitor fatigue, assess RPE, educate regarding energy conservation
-Consider increased risk of infection with dry needling
neutropenia
-ANC <1000/mm3
-Very low immunity --> very high infection risk
150,000-400,000 mm3
<50,000 or >1 million mm3
Reference range for platelets
Possible critical values for platelets
High platelets
Low platelets
-Causes: Cancer, acute/chronic inflammation, strenuous exercise, iron-deficiency anemia
-Presentation: Headache/dizziness, weakness, chest pain, tingling in hands and feet
-Causes: Hemorrhage/blood loss, cancer/chemotherapy/radiation
-Presentation: Petechiae, bruising, bleeding of nose or mouth, hematuria (blood in urine)
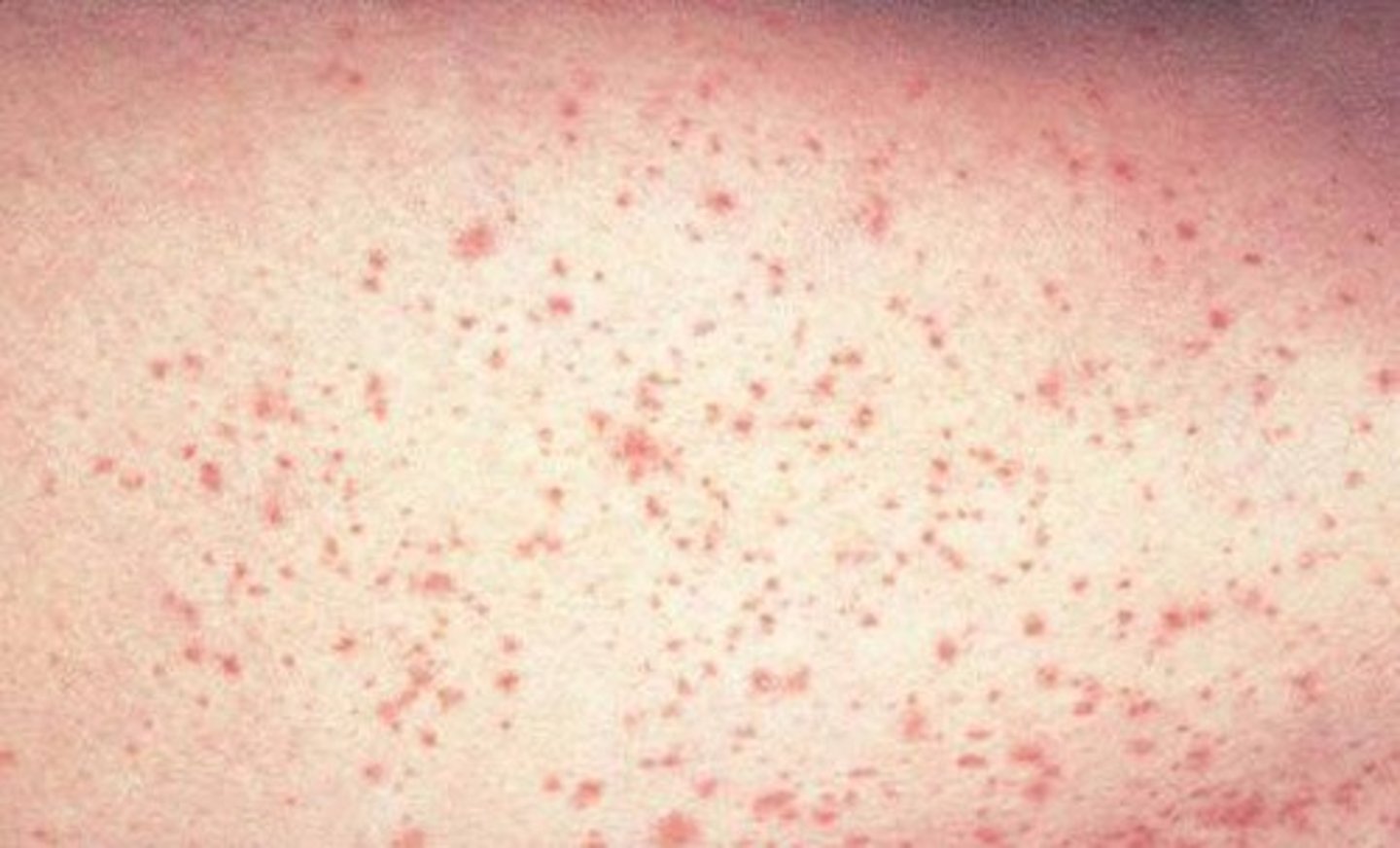
petechiae
a small red or purple spot caused by bleeding into the skin.
Clinical implications for high platelets
Clinical implications for low platelets
-Screen for and monitor for signs/symptoms of VTE
-Pulmonary Embolism (PE) and DVT
-Wells Clinical Prediction rules
-Fall prevention
-Monitor fatigue, assess RPE, educate regarding energy conservation
-Consider increased risk of bleeding with dry needling
-Male: 14-18 g/dL3
-Female: 12-16 g/dL3
<5 or >20 g/dL3
Reference range for Hemoglobin
Possible critical values for hemoglobin
Yes
Are hemoglobin values slightly decreased in older adults?
High hemoglobin
Low hemoglobin
-Causes: Severe dehydration, smoking, congenital heart disease & heart failure, chronic pulmonary diseases
-Presentation: Fatigue, headache/dizziness/visual changes, transient ischemic attack (TIA), dysrhythmias, bleeding/bruising
-Blood is thick and not bruising well
-Causes: Hemorrhage/blood loss, Vitamin B12 & iron deficiency, cancer, metabolic disorders, medications
-Presentation: Pallor, tachycardia, orthostatic hypotension, dysrhythmias, impaired endurance/activity tolerance
Clinical implications for high hemoglobin
Clinical implications for low hemoglobin
-Monitor vitals
-Monitor cardiac rhythm
-Activity pacing
-Monitor SpO2 closely
-Monitor cardiac rhythm & signs of decreased activity tolerance
-Monitor for signs of impaired tissue perfusion (discoloration, weak/absent peripheral pulses, decreased temperature, angina)
-Monitor for orthostatic hypotension, prevent falls, & provide patient education
-Male: 42-52%
-Female: 37-47%
<15% or >60%
Reference ranges for hematocrit
Possible critical values for hematocrit
Yes
Are hematocrit values slightly decreased in older adults?
-Causes: Severe dehydration, congenital heart disease, chronic pulmonary disorders, burns
-Presentation: Fatigue, headache/dizziness/visual changes, transient ischemic attack (TIA), dysrhythmias, bleeding/bruising
-Causes: Hemorrhage, cancer, dietary deficiency, rheumatoid arthritis, liver or kidney disease
-Presentation: Orthostatic hypotension, headache/dizziness, pallor, angina, dysrhythmia, dyspnea
High hematocrit
Low hematocrit
Clinical implications for high hematocrit
Clinical implications for low hematocrit
-Screen for and monitor for signs/symptoms of venous thromboembolism (VTE)
-Pulmonary embolism (PE) and DVT
-Wells Clinical Prediction Rules
-Monitor SpO2 closely
-Monitor for signs of impaired tissue perfusion (discoloration, weak/absent peripheral pulses, decreased temperature, angina)
-Monitor for orthostatic hypotension, prevent falls, & provide patient education
-Monitor fatigue, assess RPE, educate regarding energy conservation
136-145 mEq/L
<120 or >160 mEq/L
Reference range for Sodium
Possible critical values for sodium
True
T/F There can be a high concentration of sodium and relatively low concentration of fluid
-Causes: Hypovolemia, sodium overload, endocrine disorders
-Presentation: Thirst, low urine production, confusion/irritability, hyperreflexia, seizure, tachycardia, hypotension
-Causes: Hypervolemia AND hypovolemia, dehydration, diuretics, liver or kidney disease, GI disorders
-Presentation: lethargy/weakness/confusion, hyporeflexia, seizure, orthostatic hypotension, pitting edema
High sodium
Low sodium
hypervolemia
sodium concentration is low in comparison to concentration of fluid
hypovolemia
sodium concentration is low because there is low is low blood supply overall
-Monitor vitals and cardiac rhythm closely--may have decreased activity tolerance
-Assess/monitor for cognitive and neurologic impairment
-Collaborate with interprofessional team regarding fluid intake
-Consider seizure precautions
-Assess/monitor for cognitive impairment
-Monitor for orthostatic hypotension, prevent falls, & provide patient education
-Consider seizure precautions
Clinical implications for high sodium
Clinical implications for low sodium
3.5-5.0 mEq/L
<2.5 or >6.5 mEq/L
Reference range for potassium
Possible critical values for potassium
-Causes: Excess potassium supplementation, renal failure, metabolic/diabetic acidosis, blood transfusion
-Presentation: Muscle weakness/paralysis & tenderness, paresthesia, dysrhythmia, bradycardia
-Causes: Fluid overload, kidney or GI dysfunction, diuretics, alcohol use disorder
-Presentation: Extremity weakness, leg cramps, hyporeflexia, paresthesia, dysrhymias, hypotension
High potassium
Low potassium
-Monitor vitals & cardiac rhythm closely in patients with potassium >5 mEq/L
-Assess/monitor for sudden loss of muscle strength in ascending pattern
-Monitor vitals & cardiac rhythm closely in patients with potassium <2.5 mEq/L
-Assess/monitor for sudden loss of muscle strength in ascending pattern
Clinical implications for high potassium
Clinical implications for low potassium
74-106 mg/dL
<50 or >400 mg/dL
Reference range for glucose
Possible critical values for glucose
-Causes: diabetes mellitus, acute stress response, chronic kidney disease, medications
-Causes: Excess insulin, malnutrition, alcohol use disorder
high glucose
Low glucose
acute hyperglycemia
-Polyuria, polydipsia, polyphagia (excessive urine, thirst, and unger)
-Dizziness/blurred vision
-Weakness/gatigue
asymptomatic
Acute hyperglycemia in Type 2 DM may be ________ and only suspected due to recurrent infections or non-healing woulds
chronic hyperglycemia
-Chronic kidney disease
-Peripheral neuropathy
-Retinopathy
-Cardiovascular & peripheral vascular disease
-Non-traumatic amputations
diabetic ketoacidosis
-This is an emergency
-Nausea/vomiting
-Fruity breath
-Confusion
-Weak, rapid pulse
-Kussmaul respiration (rapid deep breathing)
acute hypoglycemia
-Insulin rxn (shock); d/t insulin excess or lack of eating, slow pulse, cool, clammy skin, hungry, weak, shakiness, sweating
-Perspiration, shaking
-Weakness/lethargy
-Pallor
-Nervousness/irritability/altered mental status
-Tachycardia/palpitation
-Hunger
-Headache/blurred vision
-Loss of consciousness
-Assess integumentary system for edema, skin lesions, wounds
-Assess for loss of protective sensation
-Educate regarding appropriate footwear & foot self-care
-Educate regarding lifestyle modifications: exercise, glucose control, glucose monitoring
-Collaborate with the interprofessional team if blood glucose is >250 mg/dL
-Monitor blood glucose prior to activity
-Collaborate with the interprofessional team if blood glucose is <100 mg/dL before PT
-Educate on glucose monitoring before, during, and after exercise
-Prevent falls
-Assess/monitor for cognitive impairment
Clinical implications for high glucose
Clinical implications for low glucose
7.35-7.45
<7.25 or >7.55
pH reference range
Possible critical values for pH
21-28 mEq/L
<15 or >40 mEq/L
Reference range for HCO3
Possible critical values for HCO3
35-45 mmHg
<20 or >60 mmHg
Reference range for PaCO2
Possible critical values for PaCO2
80-100 mmHg
<40mmHg
Reference range for PaO2
Possible critical values for PaO2
respiratory alkalosis
-pH increases
-PaCO2 decreases
-Cause: hyperventilation
Respiratory acidosis
-pH decreases
-PaCO2 increases
-Causes: Respiratory depression, pulmonary disease
Metabolic alkalosis
-pH increases
-HCO3 increases
-Causes: Sodium bicarbonate overdose, prolonged vomiting
Metabolic Acidosis
-pH decreases
-HCO3 decreases
-Causes: diabetes, shock, renal failure
anti-factor Xa assay
measure of anticoagulation monitoring for patients on unfractionated/standard heparin (UPH) and low molecular weight heparin (LMWH)
0.2-0.5 IU/mL
0.5-1.2 IU mL
Anti-factor Xa range for preventing VTE
Anti-factor Xa range for treating VTE
INR
international standard for coagulation and monitoring for patients on Coumadin/warfarin
1.5-2.0
2.0-3.0
INR for preventing DVT
INR for treating DVT
>5.5
Possible critical values for INR
High anticoagulation measures
-Increased risk for bleeding (including internal bleeding)
-Prevent falls
-Check for bruising/blood in urine
-Monitor for changes in neurological condition suggestive of intracranial bleeding
-If external bleeding occurs, apply prolonged pressure
-Educate patient on risk posed by falls and contact sports
-Collaborate with the interprofessional team to determine safe exercise/activity levels
If anticoagulation therapy is for preventing VTE/DVT and values are low
Likely not a reason to hold PT - remember, exercise/movement are also good for helping to prevent VTE/DVT
If anticoagulation therapy is for treating a known VTE/DVT and values are low
Consult with the interprofessional team. It MAY be appropriate to wait until the recommended range is achieved