Pain
1/74
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
75 Terms
less
pain is ___ discrete than other tactile senses
threshold
first pain
tolerance
maximum intensity of pain a person is capable of enduring
second pain
longer lasting, diffuse pain after "first pain" subsides
hyperalgesia
increased response to noxious stimuli
primary hyperalgesia
increased sensitivity at the site of injury
secondary hyperalgesia
Increased sensitivity outside the site of injury
allodynia
painful response to a non-noxious stimulus
acute pain
associated with actual/potential tissue damage
- severity of injury not necessarily related to intensity of pain
protective mechanism
chemical, mechanical, and thermal
what types of nociceptors are activated by noxious stimuli in acute pain?
protective mechanism of acute pain
withdrawal from harm to prevent further damage
healing behaviors (not weight bearing after hurting ankle)
A delta and C
what fiber types transmit pain?
A delta fibers
tissue damage- mechanical stimulus
- may also respond to chemical
cooling temperature
coarse touch (perceive touch but can't localize)
C fibers
tissue damage: mechanical, chemical, and thermal
heating temperature
itch
tickle
cutaneous pain
discriminative pain
usually sharp
rarely refers to other areas
muscle pain
diffuse
dull/aching/cramping
often refers to superficial structures
neuropathic pain
damage to nerves themselves
burning/shooting/tingling
visceral pain
from visceral organs
diffuse
dull/stabbing/cramping
often refers!!!
amygdala and hypothalamus
what two structures involve an emotional aspect of pain?
periaqueductal gray
the ____ ____ is involved in descending pain inhibition
reticular formation
the ____ ____ is why pain can interfere with sleep?
DCML
visceral pain is carried through the ____ pathway
wide dynamic range neurons
in lamina V
receive non-noxious and noxious information
also receive visceral sensory info
likely a mechanism for referred pain (may fire spontaneously)
peripheral sensitization
triggered by inflammatory response to tissue damage
- nociceptor threshold is lower
- firing rate of pain neurons is increased
- dorsal horn of SC: increased excitatory NTs (glutamate, aspartate, and substance P)
Pain signal is larger compared to before tissue damage!!
central sensitization
hyper-excitability of CNS neurons associated with pain perception
can occur in the absence of tissue injury
happens when there is prolonged peripheral sensitization
peripheral sensitization nociceptors
release substance P, calcitonin gene-related peptide, and ATP
facilitate inflammatory response
- vasodilation
- edema
- release of histamine from mast cells
histamine
non-neural cells like mast cells, macrophages, and neutrophils release bradykinin, ____, serotonin, prostaglandins, and cytokines
increase the response of nociceptors
glutamate; increased
peripheral sensitization the amount of ___ released by the presynaptic neuron in the dorsal horn is _____, causing a greater pain signal transmitted by the post-synaptic neuron
silent nociceptors
not normally responsive to mechanical stimuli but become responsive under inflammatory conditions (peripheral sensitization)
chronic pain
pain that is present beyond the normal time frame of healing
- not associated with tissue damage
non-protective: no adaptive purpose
"faulty" neuroplasticity
pain response is greater than what would be expected based on clinical exam
3
chronic pain is characterized as pain that lasts ___ months or longer
characteristics of chronic pain
1. increase receptive field size
2. increased response to noxious stimuli (hyperalgesia)
3. increased response to non-noxious stimuli (allodynia)
4. increase in spontaneous neuronal firing (flares of pain w/o sensory input)
5. decrease in activation threshold of spinal neurons
hyper-excitable
CNS pain-related neurons/structures are _____ in central sensitization of chronic pain
injury/damage
chronic pain can occurs with or without actual tissue ____/____
wind-up
happens with highly sensitized nervous system
firing of APs after a stimulus stops
spinal; supraspinal
descending pain inhibition is influenced by ____ and _____ influences
NE; serotonin
neurotransmitters involved in descending pain inhibition are opioids, _____, and _____
PAG
in the midbrain
pain suppression signal
- antinociception via activation of pons/medulla
- enkephalins, endorphins, dynorphins (opioids)
NE
in the pons, the locus coeruleus releases the NT ____
serotonin
in the medulla the NT that is released is ____
level I
inflammatory mediators
- NSAIDs, RICE principle
- minimize sensitization, directly target inflammation
level II
spinal cord level in dorsal horn
- gate control theory
- enkephalins at lamina II suppress impulses in spinothalamic tract
level III
brainstem level
- conditioned pain modulation
level IV
pituitary level
- pain causes release of endorphins into blood stream
- "runner's high"
level V
cortical
- motivation, placebo, expectations, distractions, stress
gate-control theory
activation of large diameter sensory fibers inhibits pain signal from small diameter sensory fibers
- rubbing something that hurts causes some suppression of the signal
inhibitory
in the gate control theory, large diameter sensory neurons activate _____ interneurons found in lamina II of the dorsal horn
segmental inhibition
occurs in the gate control theory
happens at a specific spinal cord level where the sensory neurons are activated to produce pain signals
conditioned pain modulation
pain inhibits pain
reduced in patients with chronic pain (may still be intact but pain may/ may not decrease)
- ice water bath and finger pressure pain
threshold; tolerance
to measure conditioned pain modulation, the pressure pain ____ and pain ____ are used
gate control theory
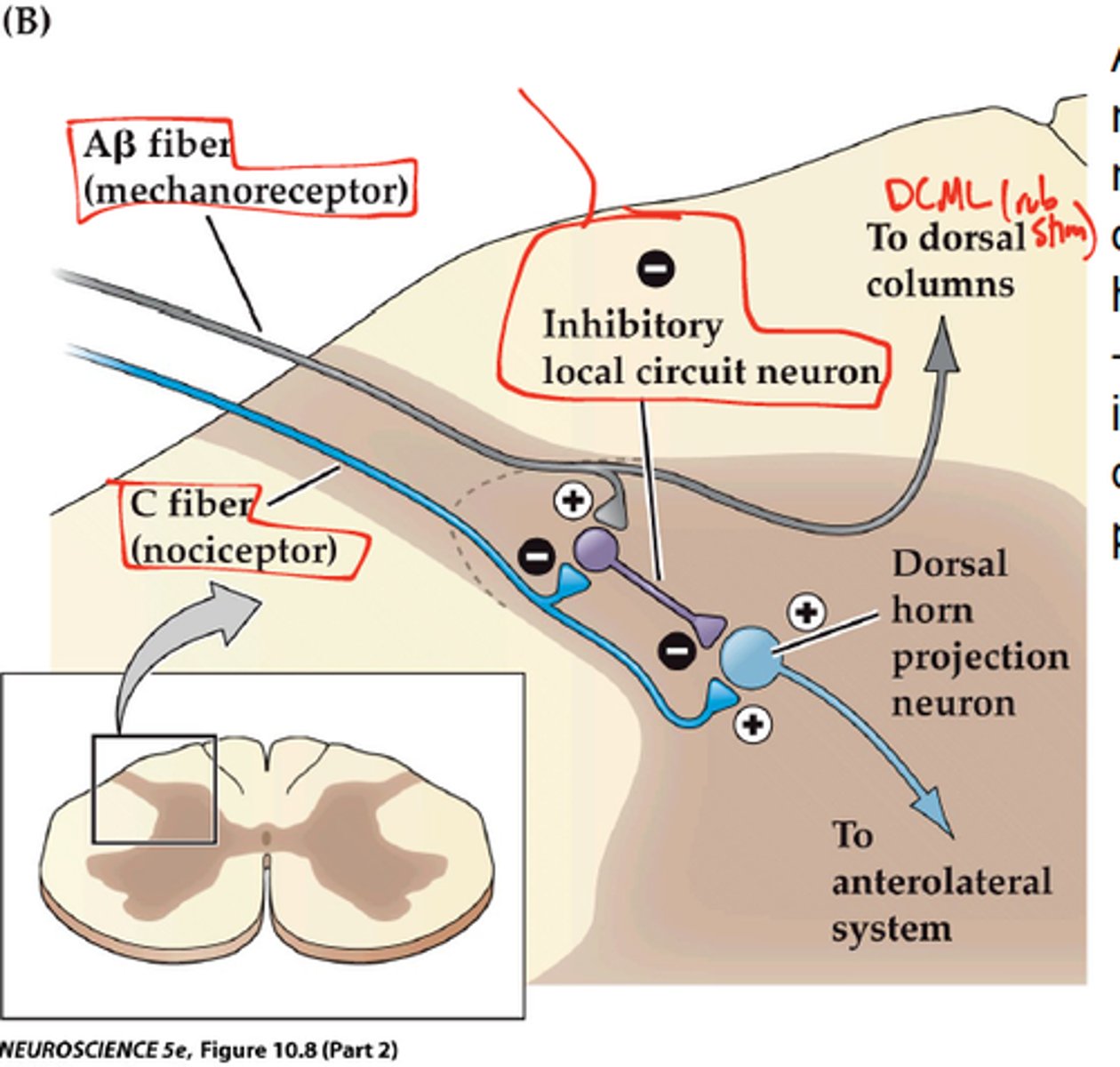
threshold; less
in CPM, the descending inputs make it harder for the 2nd order neuron to reach ____ and also inhibit the 1st order neuron to release ____ NT
opioids
in the PAG the NTs that are secreted are enkephalins, endorphins, and dynorphins, also known as ____
dynorphins
in the RVM and dorsal horn the NTs that are released are enkephalins and ____
decreases
in the dorsal horn, the endogenous opioids are released on the presynaptic sensory neuron which ____ the amount of NT released
inflammatory
opioids receptors are more likely to bind in _____ states
hyperpolarize
endogenous opioids decrease the amount of NT released and ____ the postsynaptic neuron
endorphins
released into blood stream by pituitary gland
released into PAG by hypothalamic neurons
locations of EO
peripheral terminals of small diameter nociceptic afferents
spinal cord (upregulated in inflammatory states)
RVM
PAG
Pons
Amygdala
Bowel muscles and anal sphincter
Brainstem
constipation
a side effect of EOs is ____ because EOs slow down gut motility
suppress
since EOs are found in the brainstem they can ____ CV and respiratory systems to an extreme
placebo effect
the phenomenon in which the expectations of the participants in a study can influence their behavior
limbic system
the placebo effect likely activates the EO system in cortical and subcortical areas like the ____ _____ which is why emotion is involved
narcan
the placebo effect can be blocked by the administration of ____ because it blocks endogenous opioids
catastrophizing
psychological aspect of pain
pain response is increased by patient thinking the pain will be significant/disabling/intractable
"spiraling"
heightened pain perception
kinesiophobia
fear of movement
believe moving will make pain worse
phantom limb
cortical reorganization is a possible mechanism
peripheral neurons another possible mechanism (turns on sensory nerves)
- can use cortical mechanisms as treatment
different
every person experiences ___ phantom limb pain
- no two people are the same
a box with a mirror inside is a common treatment for phantom limb pain
- the mirror allows the brain to ____ perceive the phantom limb is not clenched/cramped etc.
brain
pain is always an output of the ____, 100% of the time
damage
pain does not equal the amount of tissue ____
stress
pain is influenced by multiple factors such as thoughts, activity, sleep, mood, and ____
- influenced by emotions
injury
acute pain serves a useful protection function to warn of danger or ____
hypersensitive
chronic pain results from a ____ nervous system and usually no longer warns of danger
pain
many treatments can help "turn down" a hypersensitive nervous system, reduce ____, and improve quality of life