Type 1 DM
1/55
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
56 Terms
What is the primary pathophysiology of Type 1 Diabetes Mellitus?
The destruction of pancreatic beta cells, leading to a functional absence of insulin.
In what ways is DM1 a catabolic disorder?
Circulating insulin is very low or absent, plasma glucagon is elevated, and pancreatic beta cells fail to respond to all insulin-secretory stimuli.
What is the main autoimmune mechanism in Type 1a DM?
Lymphocytic infiltration and destruction of the insulin-secreting cells of the islets of Langerhans.
Which specific antibody is most commonly associated with Type 1a DM?
Glutamic acid decarboxylase (GAD) antibodies.
What environmental factors are hypothesized to trigger Type 1 DM in susceptible individuals?
Viral infections (e.g., mumps, rubella, Coxsackie B4), toxic chemicals, exposure to cow's milk in infancy, and cytotoxins.
What role does Vitamin D play in the context of Type 1 DM?
Evidence suggests higher levels of Vitamin D may result in lower autoimmunity of pancreatic islet cells.
What is the most common metabolic disease?
Type 1 Diabetes Mellitus
What is the peak age of onset for Type 1 DM?
11 to 13 years old.
What is type 1 diabetic at an increased risk of developing?
Ischemic heart disease, cerebral vascular disease, chronic renal disease and reduced visual acuity and blindness.
What are the classic clinical symptoms of Type 1 DM?
Polyuria, polydipsia, polyphagia, fatigue, nausea, and blurred vision.
What causes the weight loss seen in Type 1 DM despite normal or increased appetite?
A catabolic state resulting in the depletion of glycogen, proteins, and triglycerides.
Why do Type 1 DM patients experience blurred vision?
The hyperosmolar state causes glucose and its metabolites to cause dilation of the lens, which alters its focal length.
What is the cause of peripheral neuropathy in Type 1 DM?
Sustained hyperglycemia leads to the accumulation of sorbitol in peripheral sensory nerves, presents as numbness and tingling in a glove and stocking pattern.
What is the clinical significance of nocturnal enuresis (bed wetting) in children regarding diabetes?
It can be an early indicator of the onset of diabetes due to polyuria.
What are the classic clinical signs of Diabetic Ketoacidosis (DKA)?
Kussmaul respiration, dehydration, hypotension, and altered mental status.
What are the four ADA diagnostic criteria for diabetes?
A1C ≥6.5%; Fasting Plasma Glucose ≥126 mg/dl; 2-h plasma glucose ≥200 mg/dl during an OGTT; or Random plasma glucose ≥200 mg/dl in a patient with classic hyperglycemia symptoms.
Which specific marker is considered a reliable indicator for diagnosing or monitoring DKA?
Plasma acetone, specifically the beta-hydroxybutyrate level.
What is the expected C-peptide level in established Type 1 Diabetes Mellitus?
Low or low-normal.
Which antibody titer suggests Type 1a Diabetes Mellitus?
A high positive titer of glutamic acid decarboxylase (GAD) antibodies.
How long before clinical presentation does beta cell destruction typically begin in T1DM?
Months or even years before the onset of clinical symptoms.
How does the presentation of Type 1 DM in adults (late 30s/40s) differ from children?
It tends to present in a less aggressive manner.
What are the primary goals of exogenous insulin therapy in Type 1 DM?
To reverse the catabolic condition, prevent ketosis, decrease hyperglucagonemia, and normalize lipid and protein metabolism.
What is the first-line therapy for Type 1 Diabetes Mellitus?
Subcutaneous insulin therapy.
What are the target preprandial and postprandial glucose levels for T1DM patients?
80-130 mg/dL before meals and <180 mg/dL peak postprandial.
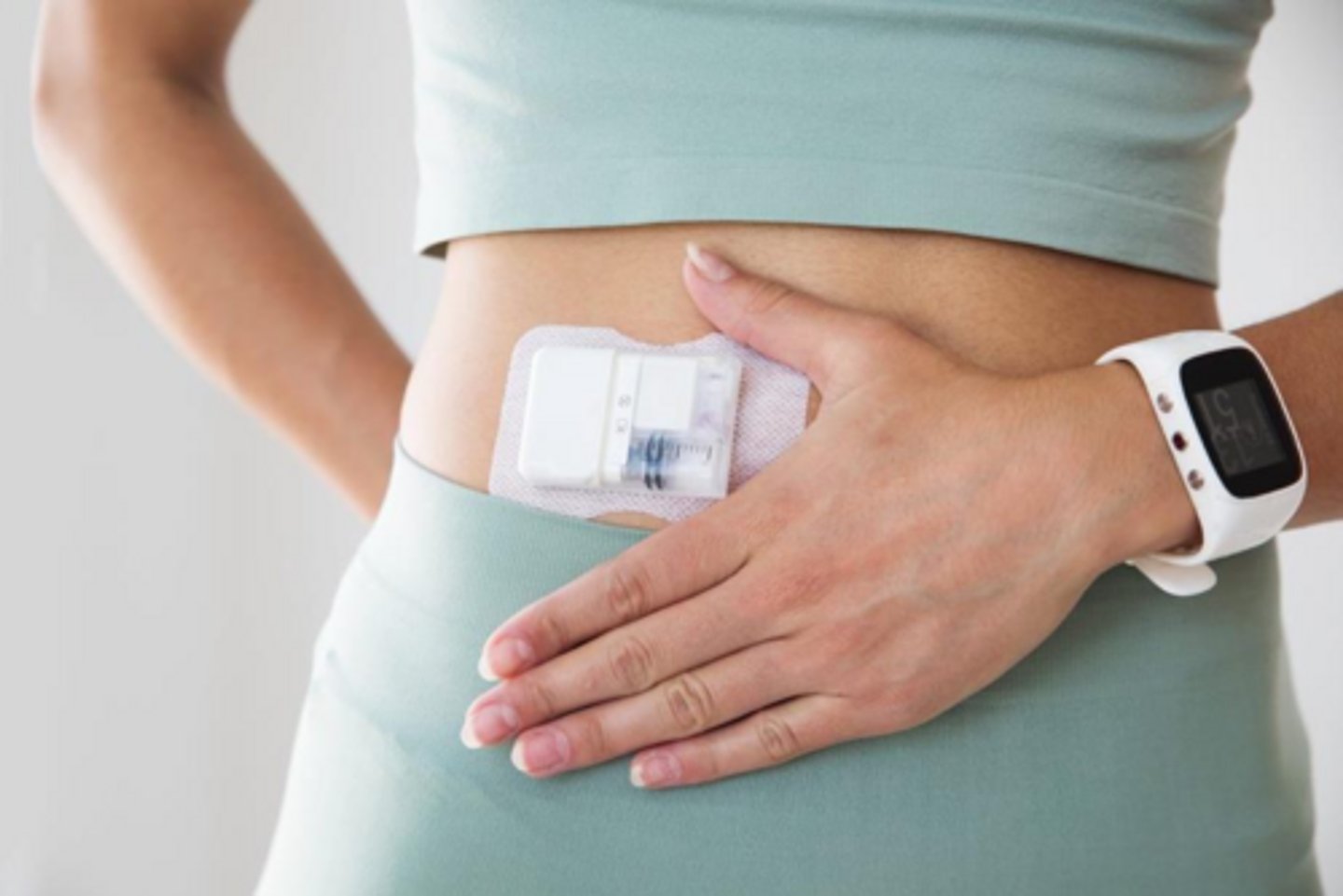
What is the preferred insulin delivery system for children and adults with T1DM?
Automated insulin delivery (AID) systems.
When should rapid- or short-acting insulins be utilized?
Whenever quick glucose utilization is needed, such as before meals or when blood glucose is >250 mg/dL.
Name three examples of basal (long-acting) insulin options.
Glargine, detemir, and degludec.
Name three examples of prandial (short-acting) insulin options.
Lispro, aspart, and glulisine.
What are the primary characteristics of Insulin Glargine (Lantus)?
It has no peak, a relatively flat profile, and a duration of action lasting more than 24 hours.
What causes the prolonged action of Insulin Detemir (Levemir)?
Slow systemic absorption of detemir molecules from the injection site.
How is Lispro insulin (Humalog) genetically engineered?
By reversing the amino acids lysine and proline in the B chain.
What is the typical onset, peak, and duration of rapid-acting insulins like Lispro, Aspart, and Glulisine?
Onset: 5-10 min; Peak: 1 h; Duration: 4 h.
What is the standard concentration for routine insulin preparations?
100 U/mL.
How is the total daily insulin (TDI) dose typically divided between basal and prandial insulin?
40% to 50% as basal insulin and 50% to 60% as prandial insulin.
What factors necessitate a higher total daily insulin (TDI) dose?
Obesity, sedentary lifestyles, and puberty.
What is the recommended standard of care for glucose monitoring in most people with T1DM?
Continuous Glucose Monitoring (CGM).
What is the recommended Time in Range (TIR) goal for patients using CGM?
>70% of time spent between 70-180 mg/dL.
What are the recommended thresholds for Time Below Range in CGM monitoring?
<4% below 70 mg/dL and <1% below 54 mg/dL.
What are three primary limitations of Continuous Glucose Monitors (CGM)?
They measure interstitial rather than blood glucose, have a lag time of 5-10 minutes, and may require calibration.
What type of insulin is used in insulin pumps?
Rapid-acting insulin only.
How is the bolus insulin dose calculated based on carbohydrates?
Bolus insulin = (Carbs eaten ÷ Insulin-to-Carb Ratio).
What does a patient enter to use the bolus calculator on their insulin pump?
Carbs eaten and current glucose.
What does the insulin pump automatically calculate?
Carb dose, correction dose and total insulin needed.
What are the primary advantages of using an insulin pump?
Better glycemic control, more precise dosing, adjustable basal rates, flexibility for exercise/illness, and fewer injections.
Why is there a high risk of Diabetic Ketoacidosis (DKA) with insulin pump use?
Because there is no long-acting insulin onboard; if the pump fails, insulin delivery stops immediately.
What components make up an Automated Insulin Delivery (AID) system?
A CGM, an insulin pump, and an algorithm that automatically adjusts basal insulin.
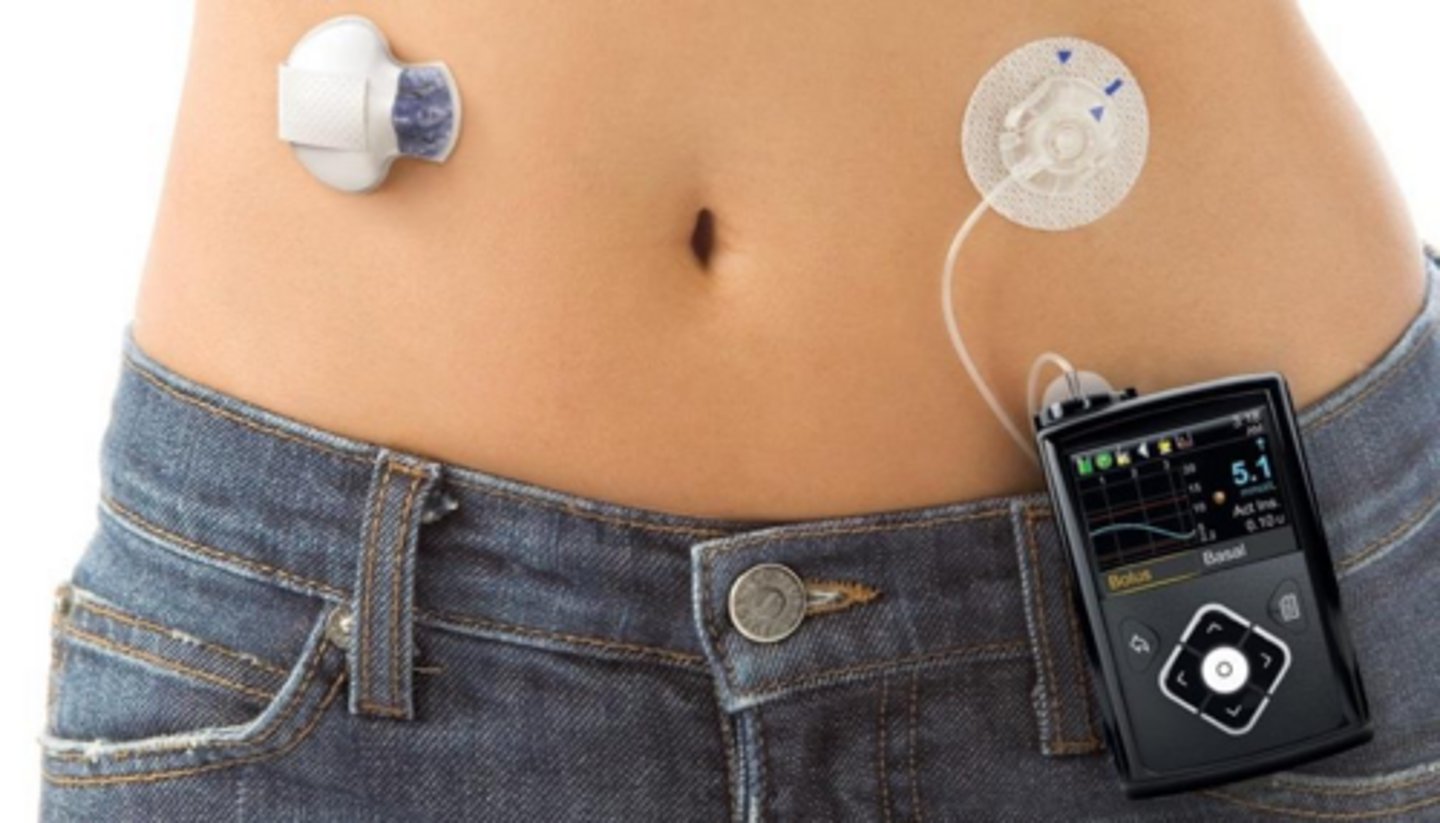
Why is an AID system considered a 'hybrid' closed-loop?
Because the patient must still manually enter carb counts and administer mealtime boluses.
What are the primary benefits of AID systems compared to standard pumps?
Increased time in range, decreased hypoglycemia (especially overnight), reduced glycemic variability, and less decision-making burden.
How does Pramlintide (Symlin) assist in diabetes management?
It slows gastric emptying, suppresses postprandial glucagon, and regulates food intake, helping to lower post-meal glucose fluctuations.
What surgery is possible for DM1 treatment?
Pancreatic transplantation and is most commonly performed simultaneously with kidney transplantation for end stage renal disease.
What is the greatest limitation of pancreatic transplantation?
The requirement for lifelong immunosuppression.
What is the 'Dawn phenomenon' in diabetes?
The natural tendency of blood glucose to rise in the early morning, often due to nocturnal growth hormone spikes and hepatic gluconeogenesis.
What advice should be given to patients regarding exercise and hypoglycemia?
If exercising for more than 30 minutes, patients may need an extra snack to prevent hypoglycemia and must maintain hydration.
What is the main difference between MDI and insulin pumps regarding insulin types?
MDI uses both basal (long-acting) and bolus (rapid-acting) insulin, whereas pumps use only rapid-acting insulin for both basal and bolus needs.
What are the common site issues associated with insulin pumps?
Infection, occlusion, and dislodgement.
What does the 'basal' setting on an insulin pump provide?
Continuous infusion of insulin throughout the day to mimic normal pancreatic function.