ALL clinical skills
1/26
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
27 Terms
What are the critical points of hand hygiene?
Before each episode of direct care
Clean/aseptic procedures
Afteer each episode of direct care
After cpmtact with bolidy fluids
After cpmtact with objects in the patient environment
After removal of gloves
Hands must be decontaminated by soap instead of hand sanitiser when
You have applied sanitiser several times
Your hands are visibly soiled
Your hands are potentially contamited with bodily fluids
You are caring for a patient who has vomiting or diarrhoea
You went to the toilet
You are handling food
What can you not use when washing hands?
Bars of soap
Nail brushes
What is most frequently missed when washing hands?
Thumbs and fingertips
What is respiration split into?
External respiration= drawing air into the lungs
Internal respiration= process of gas exchange between lungs, blood and tissue
How do you assess external respiration
Observe respiratory rate
Observe depth, pattern and effort of breathing
eg. are the struggling to speak? are they using accessory muscles in their neck for regular breathing?
How do you assess internal respiration?
Consider skin pallor/ cyanosis (bluish discoloration)- for ppt w darker skin check inner lower lip and palms
Restlessness and confusion (hypoxemia- low O2 in blood)
What is a pulse oximeter?
Estimates the oxygen saturation of haemoglobin delivered to tissue
94-98% on patients that are acutely ill
or 88-92% where the patient is at risk of hypercapnic respiratory disorder- abnormally high CO2 lvls (eg. COPD)
A patient should rest at least 5 mins before assessment
What are the normal resting rates of patients
Age Rate
Newborn 30-50
2-12years 20-30
Teen 12-20
Adult 12-20
Abnormalities in a patients chest or spine can cause difficulties breathing
What is stridor?
High-pitched wheezing sound caused by distrupted airflow in the larynx or lower bronchiol tree
It can indicate airway obstruction by foreign bodies or tumors
It’s a noisy inspiration (like snoring in deep sleep)
What are the Patterns of respiration
Bradypnoea= slow, regular respiration below 12- can cause oxygen deprivation. Associated w alcohol consuption, over-sedation, metabolic and cws disorder
Tachypnoea= rapid, regular respiration above average. Associated w pneumonia, respiratory insufficiency, lesions in the respiratory centre of the brain, fever or panic attack
Prolonged expiration= COPD (chronic obstructive pulmunary disorder)
Cheyne-strokes respiration= slow, shallow breaths which gradually become rapid and deep, and then slowly subside to 12-20 seconds of apnea. Cycles of 45s-3mins. Due to raised intracranial pressure, celebral anoxia, drug overdose, meningitis, congestive heart failure, end stage renal disease or terminal stage cancer
Dyspnoea= difficult breathing. Associated w pulmunary embolism, pneumothorax, advanced cancer, pericarditis, angina and general, severe chest pain
Orthopnea= SOB because of lying flat. Can be fixed by sitting up
What is the order of examinaion for the respiratory system
Inspection
Palpitation
Percussion (tapping on chest to mobalise lung secretion)
Ausculation (listening to internal sounds of the body)
What is pulse oximetry
Measures the saturation of haemoglobin in the arterial blood
They measure saturation and pulse, and are placed on the fingers and areas
What is silent hypoxia
All vital signs are good but spO2 is low
What is hypoxoemia
low level of oxygen in the blood`
In what patients are pulse oximeter readings less accurate
Patients w black or brown skin
Patients w bad blood flow to capillaries
Why are pulse oximeters not precise
They don’t show how hard the cardiovascular and respiratory system worked to get the oxygen in the blood
The adequacy of ventilation, or the level of haemoglobin in the blood
What is the mechanism behind oxymeters
Red light detects oxygenated and deoxygenated haemoglobin
If the ppt is cold, has peripheral vasoconstriction or painted/dirty nails an ear probe is more reliable
What is the aim of assessing a pulse
To see the pulse rate, rhythm and strenght
Its important to determine a ppt’s normal pulse rate so you can monitor changes due to the disease or medication
How do you determine ventricular rate
Place stetoscope on the 5th intercostal muscle
This is known as monitoring the apex beat ( a pulse deficit)= the ventricles are too weak to create a pulse rate
What happens if a ppt has a low pulse
Can cause inaccuracy in the pulse oximeter and blood pressure monitors
ECGs w low pulse may be read as low cardiac output instead
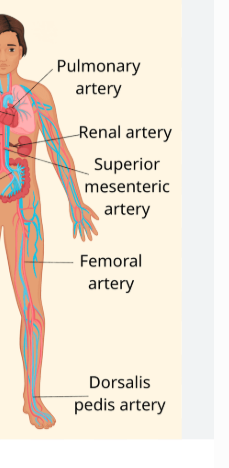
Where do you usally take pulse
Radial artery
Cartoid, femoral and brachial pulses are also used
How is core temperature taken
Can only be done invasevly by putting a probe down the oesophagus or bladder
What is pyrexia
Increase in body temperature (up to 38.9C could be mild to moderate)
Severe pyrexia does not correlate to severe infection
When do you have to closely monitor temperature
Post-operation or critically ill
Receiving blood transfusions
Have conditions that impact metabolic rate (hyporthyroidism)
Have infections
Are in an increased risk of infection
What are the diff ways to measure temp
Disposable thermometers= inaccurate but single use so not risk of hygiene
Electronic temperatures (mouth/auxillary/rectum), easy and provde quick results, expensive and require probe covers
Tympanic= fast, most accurate, non-invasive, however its at risk of poor technique