KIN 360 - Chapter 28 Study Guide
1/28
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
29 Terms
Discuss the structure and list the functions of the reproductive system.
Production of gametes
-specialized organs of the reproductive system produce gametes: sperm cells in males and oocytes (eggs) in females
Fertilization
-enables fertilization of the oocyte by the sperm
-duct system in males nourishes sperm cells until they are mature and deposited in the female reproductive tract
-female reproductive system receives the sperm cells from the male and transports them to the fertilization sit
Development and nourishment of a new individual
-female reproductive system nurtures a new individual and provides nourishment (milk) after birth
Production of reproductive hormones
-hormones produced control its development and the development of the gender-specific body form
-essential for the normal function of the reproductive system and for reproductive behavior
Distinguish among the functions that occur in males, females, and both.
male:
-production of sperm cells
sustenance and transfer of sperm cells to the female
production of testosterone
females:
production of ova (femal sex cells)
reception of sperm cells
nuturing the developemnt of and providing nourishment for developing fetus
production estrogen and pregesterone
Functions in both
-sexual arousal
-make reproductive cells (sperm or eggs)
-go through puberty
-produce sex hormones (different types)
-pass on genes to offspring
Describe the gonads (primary sex organs) of the male and female reproductive system and indicate their functions.
Gonads (testes)
-produce sex hormones and sperm
-sperm are delivered through the epididymis, ductus deferens, the ejaculatory duct, and the urethra
-accessory sex glands: empty their secretions into the ducts during ejaculation
--> seminal vesicles, prostate gland, and bulbourethral glands
Gonads (ovaries)
-produce sex hormones and ova
-accessory ducts: uterine tubes, uterus, vagina, and mammary glands
Describe the components of the scrotum (and spermatic cord) and their role in regulating the temperature of the testes.
scrotum
-two two-chambered sac containing the testes
-separated by raphe
-intrascrotal temperature is kept constant
Dartos
-smooth muscle that wrinkles scrotal skin
spermatic cord
-ductus deferens
-blood and lymphatic vessels
-nerves
-cremaster muscle is a covering of the spermatic cord
Cremaster
-bands of skeletal muscle that elevate the testes
-keep the testes 3 degrees C lower than core body temp, necessary for sperm production (spermatogensis)
when its cold, testes will be elevated to keep warm, when it's warm, tested will be lowered to remain cool
Describe the descent of the testes (when, why, what if it doesn't happen).
(during fetal development) pass from abdominal cavity through the inguinal canal to the scrotum
a tunica vaginalis covers each testis, protecting agaisnt friction
guided by the gubernaculum
pass through inguinal rings (oblique passageways in the anterior abdominal wall)
The testes move into the scrotum because sperm production requires a temperature slightly lower than normal body temperature.
cryptorchidism: failure of one or both of testes to descend into scrotum, prevents normal sperm development
Describe the structure of the testes, the specialized cells of the testes.
-located outside of the body cavity so that sperm production can take place at a lower-than-body temperature
-serve as both endocrine and exocrine glands
Endocrine
-testosterone
Exocrine
-sperm cells are secreted through a duct system
specailized cells:
seminiferous tubules: produce sperm cells, coverge to form the tubulus rectus which carried sperm to the rete testis, from rete testis the sperm leaves the testis via effeerent ductules and enter the epidiymis
interstital cells: surround the seminiferous tubules and produce testosterone
sustentacular cells: nourish the sperm cells, produce hormones, contain tight junctions that form a blood-testis barrier
Describe the process of spermatogenesis (all divisions and products).
-sperm cells are produced in the seminiferous tubules
-spermatogenic cells make up the walls of the seminiferous tubules and are in various stages of cell division
-spermatogenic cells give rise to sperm in a series of events:
Mitosis
-spermatogonia form spermatocytes
Meiosis
-spermatocytes form spermatids
Spermiogenesis
-spermatids form sperm
-maturation process
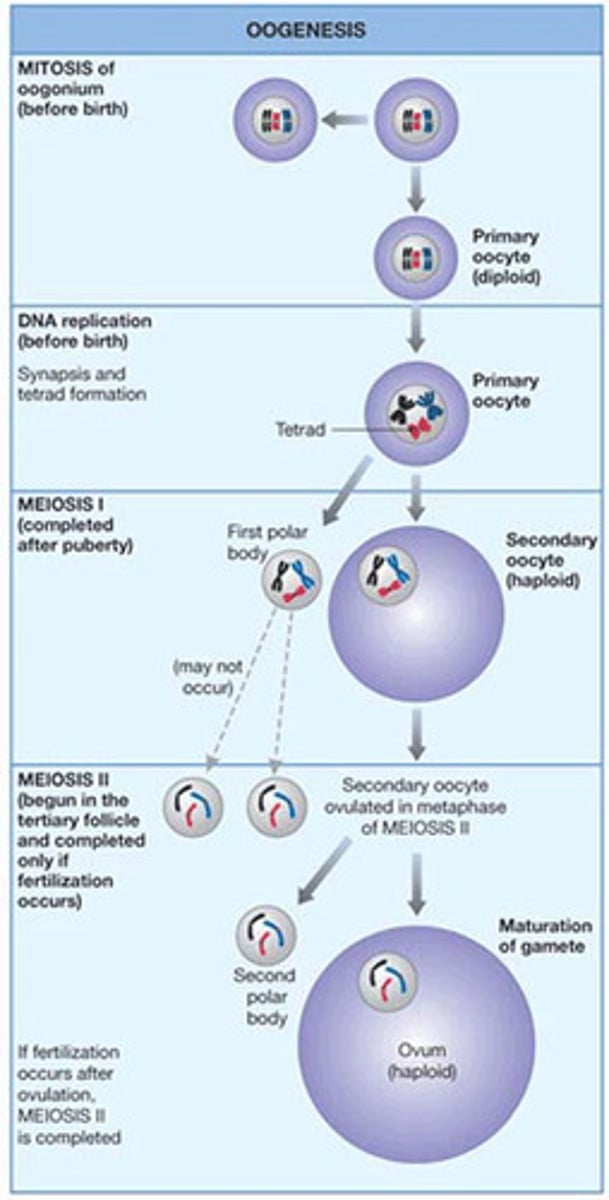
spermatogenesis in detail
spermatogonia are the cells that give rise to sperm cells. The spermatogonia divide by mitosis. One daughter cell remains a spermatogonium that can divide again by mitosis. The other daughter cell becomes a primary spermatocyte
the primary spermatocyte divides by meiosis to form secondary spermatocytes
the secondary spermatocytes divide by meiosis to form spermatids
the spermatids differentiate to form sperm cells
sustentacular cells, in which the spermatogonia and developing sperm cells are embedded, maintain the blood- testis barrier
List the ducts of the male reproductive system (epididymis through urethra) and explain their function of each part.
duct system → efferent ductules extend from testes into the duct of epidiymis
1. Epididymis
-stores sperm
-site of sperm cell maturation → ability to fertilize an oocyte develops, flagella become capable of movement
2. Vas Deferens
-carries sperm from the epididymis through inguinal canal into the abdominal cavity
-its terminus expands to form the ampulla and then joins the duct of the seminal veiscle to form the ejaculatory duct
3. Ejaculatory Duct
--sperm and seminal fluid mix in the ejaculatory duct and enter the prostatic urethra during ejaculation
4. Urethra
-carries semen out of the body
-also carries urine (but not at the same time)
Describe the structure of the penis, seminal vesicles, prostate gland, and bulbourethral glands and explain their functions/secretions.
Penis
-copulatory organ designed to deliver sperm into the female reproductive tract
-consists of an attached root and a free shaft that ends in the enlarged glans penis
-prepuce (foreskin) →covers gland penis, circumcision is the surgical removal of the prepuce after birth
-bulb and crura form root of the penis that attatches the penis to the coxal bones
-consists of corpus cavernosum and spongiosum
-erection: spongy erectile tissue fills with blood
Seminal vesicles
-lie on the posterior wall of the bladder
-joins the ductus deferens to form the ejaculatory duct
Prostate gland
-a doughnut shaped gland that encircles part of the urethra inferior to the bladder, empties into prostatic urethra
Bulbourethral glands
-pea-sized glands inferior to the prostate
-a mucous gland that empties into the spongy urethra
Differentiate the components of the ejaculate (%, composition, glands).
-testicular secretions contain sperm cells (1-5% of total volume)
-seminal vesicle fluid contains fructose, clotting proteins, and prostaglandins (60% of total volume)
-prostate secretions make the seminal fluid more pH neutral, proteolytic enzymes break down clotting proteins (30% total volume)
-bulbourethral glands produce mucus, which neutralizes the acidic pH in the female vagina (less than 5% total vagina)
List the hormones that influence the male reproductive system and describe their functions.
-Gonadotropin-releasing hormone (GnRH) from hypothalamus stimulates the release of LH and FSH from the anterior pituitary
LH
-stimulates the interstitial cells to produce testosterone
FSH
-stimulates sperm cell formation, stimulates sustentacular cells of seminiferous tubules to increase spermatogenesis and to secrete inhibin
Inhibin
-produced by sustentacular cells
-has a negative feedback effect and inhibits FSH secretion
testosterone has a stimulatory effect on the sustentacular cells and a negative feedback effect on the hypothalamus and pituitary to reduce LH and FSH secretion
Demonstrate an understanding of the changes that occur in males during puberty.
Puberty
-age at which individuals become a capable of sexual production
before puberty
before birth: placenta secretes hCG hormone which stimulates secretion of testosterone by fetal testes, from birth to puberty- minimal stimulation/secretion of testosterone
During puberty
-pituitary becomes less sensitive to testosterone
-testosterone does not completely suppress GnRH release, resulting in increased production of FSH, LH, and testosterone
Name the organs of the female reproductive system.
-ovaries
-uterine tubes
-uterus
-vagina
-external genitalia
-mammary glands
Describe the anatomy and histology of the ovaries.
-paired organs on each side of the uterus held in place by several ligaments
--> suspensory ligaments: anchor the ovary to the lateral body wall
--> ovarian ligament: attaches the ovary to the superior margin of the uterus; ovarian arteries, veins, and nerves enter the ovary through this ligament
--> broad ligament: supports the uterus
Visceral peritoneum
-covers the surface of the ovaries
Tunica albuginea
-outer capsule of the ovary that is divided internally into:
--> cortex: dense outer region that contains follicles
--> medulla: loose inner region that receives blood and lymphatic vessels and nerves
--> stroma: connective tissue of ovaries
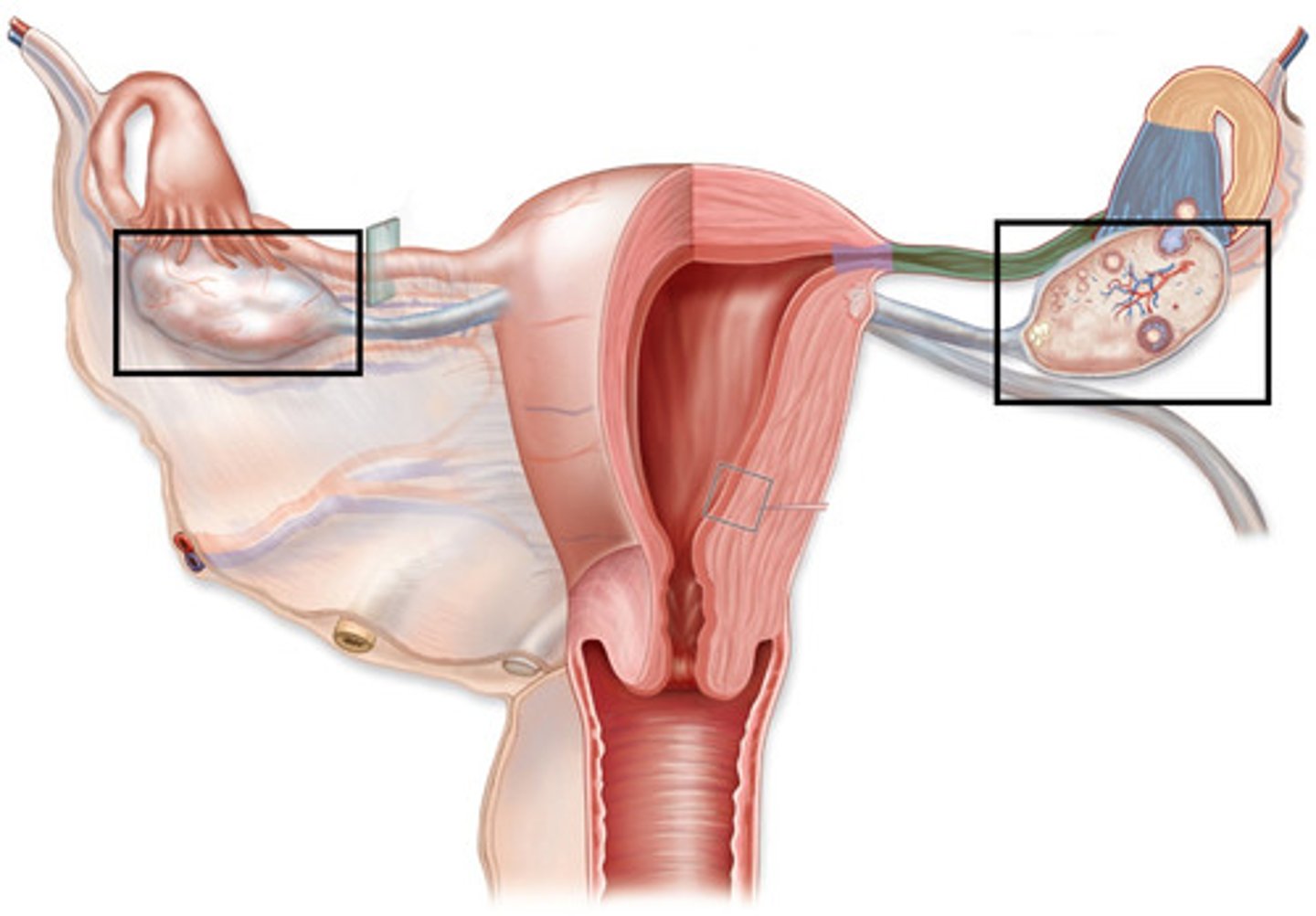
Discuss the simultaneous development of the oocyte and the follicle.
Oogenesis
-production of a secondary oocyte in the ovaries
Oogonia
-divide by mitosis to produce other oogonia and primary oocytes
-primary oocytes are surrounded by granulosa cells and called a primordial follicle
-primordial follicle becomes a primary follicle when oocyte and granular cells enlarge
-primary follicle becomes a secondary follicle and enlarges to form graafian follicle
primordial follicle --> primary follicle --> Graafian follicle
--> these follicles are maturing and enlarging, until it ruptures which is ovulation
oogenesis and fertilaztion of oocyte
oogonia are the cells from which oocytes arise. divide by mitosis to produce other oogonia and primary oocytes
primary oocytes begin first meiotic division but stop at prophase I. all of the primary oocytes remain in this state until puberty
first meiotic division completed in a single mature follicle just before ovulation durin each cycle. a secondary oocyte and the first polar body result from unequal division of cytoplasm
secondary oocyte begins the second meiotic divison but stops at metaphase II
second meiotic divison is completed after ovulation and after a sperm cell unites with a secondary oocyte. secondary oocyte and a second polar body formed
fertilization completed after the nuclei of the secondary oocyte and the sperm cell unite → resulting in a cell called a zygote
Describe ovulation, fertilization, embryo, and fetus.
-the release of a secondary oocyte from an ovary
-occurs in the ovary
-Usually occurs around day 14 of a 28-day menstrual cycle
-Before ovulation: FSH stimulates follicle development, it triggers a sudden LH surge, LH causes ovulation, follicle ruptures, oocyte is released
-After ovulation, remaining follicle becomes the corpus luteum
-if penetrated by sperm, the secondary oocyte completes the second meiotic division, yielding:
1. one large ovum (gamete)
2. a tiny second polar body
Fertilization
-the joining of a sperm cell and a secondary oocyte to form a zygote
-Usually occurs within about 24 hours after ovulation
-most common location is ampulla of uterine tube
Embryo
-the developing human between fetilization and 8 weeks of development
Fetus
-the developing human from 8 weeks to birth
follicle devleopment
-ovulation occurs when the follicle swells and ruptures and the secondary occyte is released from the ovary
fate of the follicle:
the mature follicle becomes the corpus luteum
if preganacy occurs the corpus luteum persists
if no pregnancy occurs, it degenerates to the corpus albicans
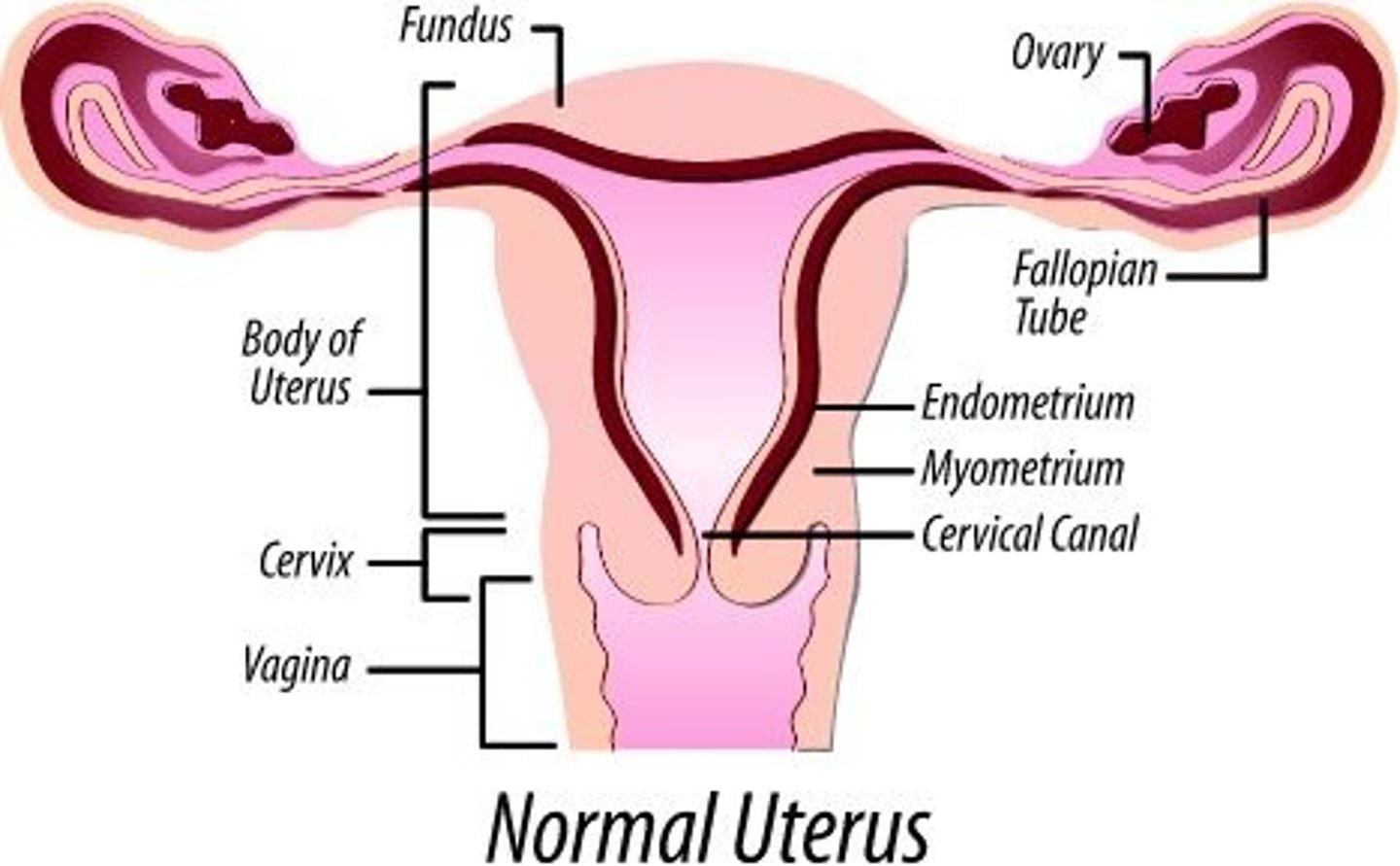
Describe the structure and functions of the uterus (cervix, permetrium, endometrium, myometrium).
Uterus
-held in place by ligaments
-consists of fundus, body, and cervix
Cervix
-opening between the vagina and uterus
uterine walls:
Perimetrium
-visceral peritoneum
Myometrium
-smooth muscle
Endometrium
-mucous membrane (inner lining) → replaced monthly during menstrual cycle
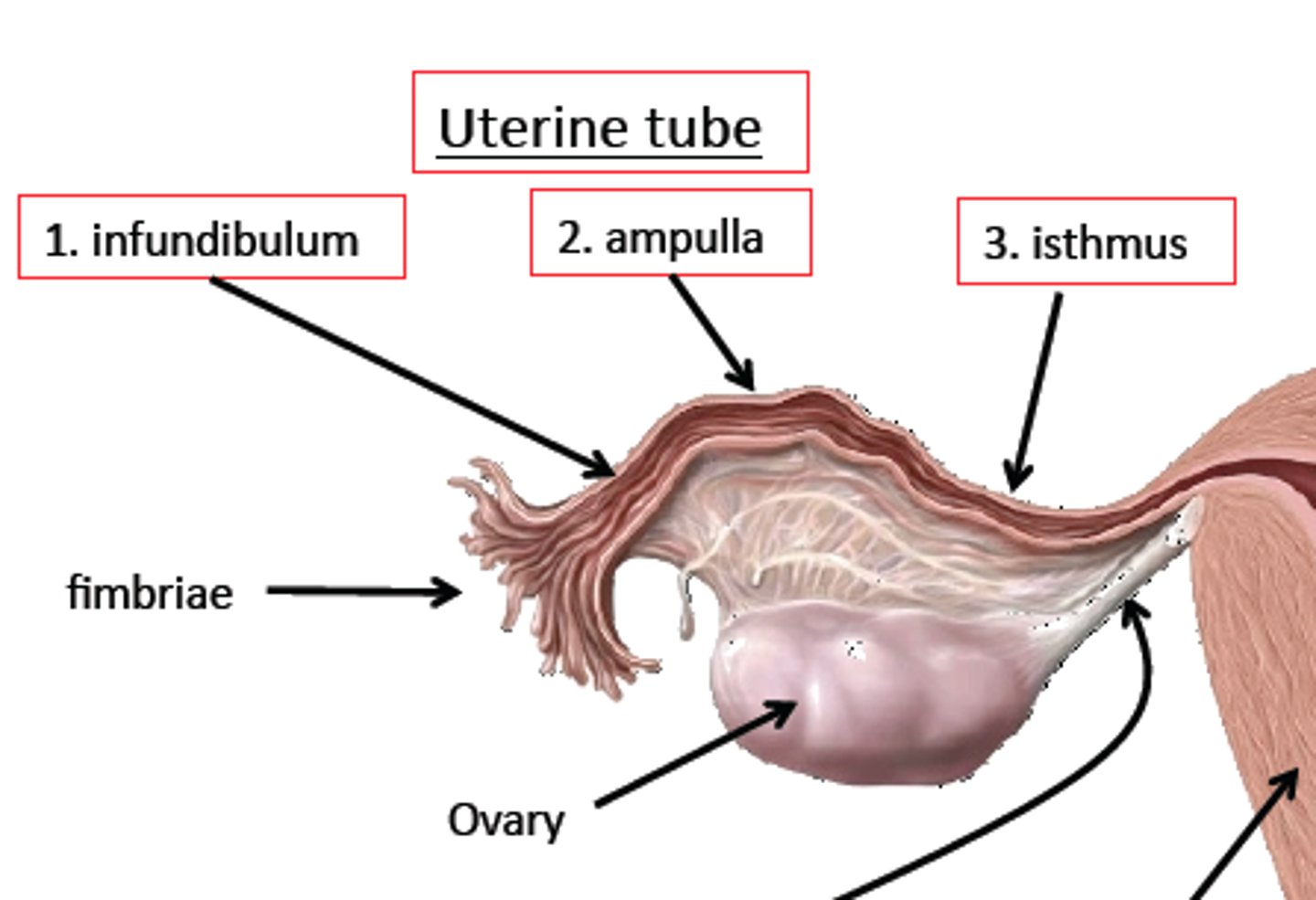
Describe the functions of the uterine tube (location, ampulla, fimbriae, infundibulum).
Uterine tubes
-transport oocyte or zygote from the ovaries to the uterus
Infundibulum
-expanded ovarian end of the uterine tube
Fimbriae
-thin processes that surround the openings of the infundibulum into the ovaries
Ampulla
-widest, longest segment of the uterine tube where fertilization takes place
muscular contraction and cilia propel the oocyte through the uterine tube
Describe the structure and function of the vagina, external genitalia, and mammary glands.
Vagina
-female organ of copulation
-allows menstrual flow and childbirth
-has smooth muscle and an inner lining of stratified squamous epithelium
-the hymen covers the vaginal orifice
External genitalia
-consists of the vestibule and its surrounding structures
Mammary glands
-modified sweat glands located in the breasts
-consist of glandular lobes and adipose tissue
-lobules have milk-producing alveoli
-lobes connect to nipple through lactiferous ducts
-areola: surrounds the nipple
-suspensory ligaments: support the breasts
Describe the structures in the external genitalia of women.
Vestibule
-space into which the vagina and urethra open
Labia minora/minus
-folds that cover the vestibule and form the prepuce
Labia majora/majus
-cover the labia minora, unite to form the mons pubis
Mons pubis
-elevated fat deposit anterior to the symphysis pubis
Pudendal cleft
-space between the labia majora
Clinical perineum
-region between the vagina and the anus
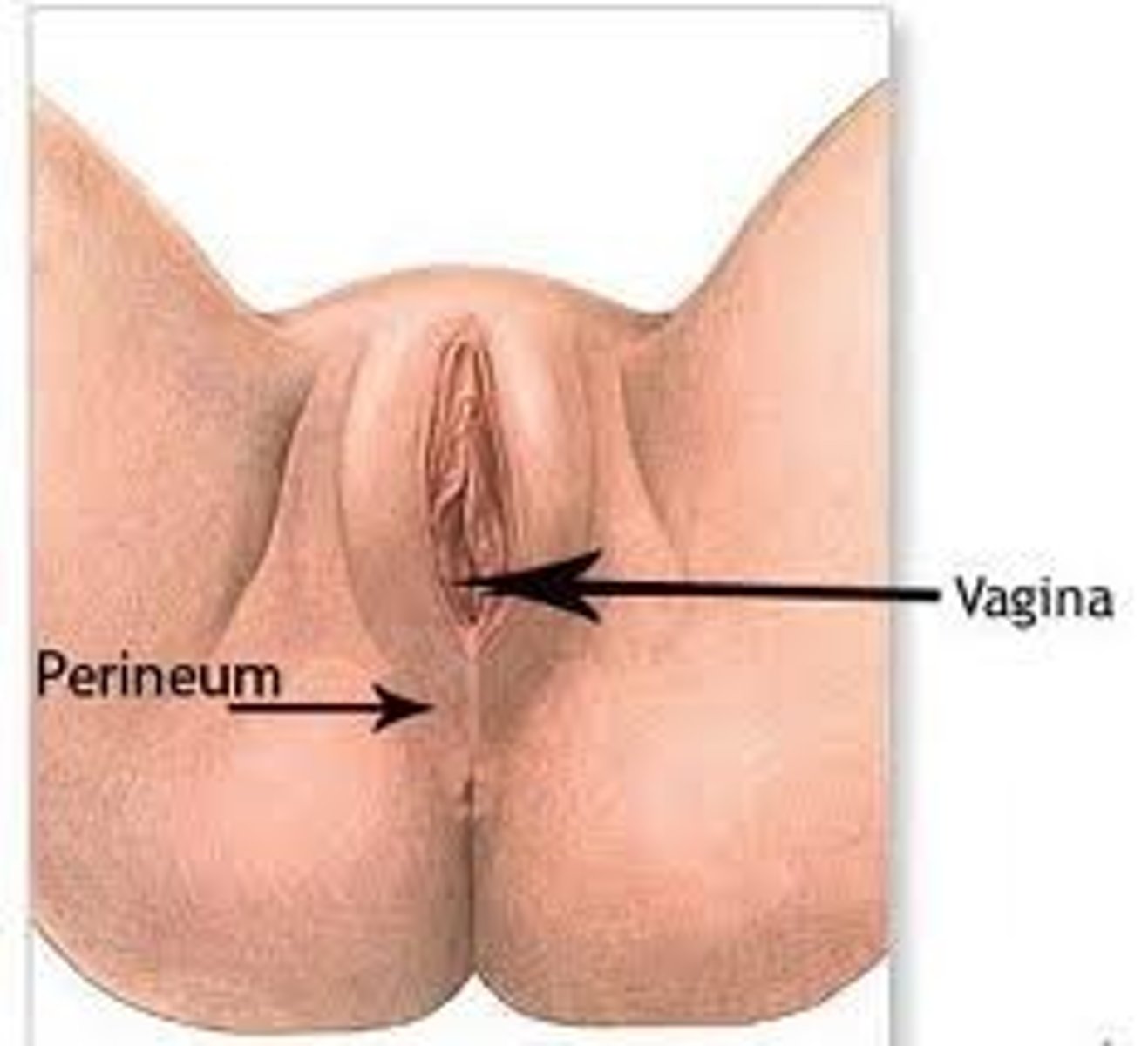
Describe the changes that occur in females during puberty (menarche).
-puberty begins with menarche
-menarche is the first menstrual bleeding
-this is triggered by increased levels of GnRH
-increased production and release of estrogen and progesterone promote the development of the female primary and secondary sexual characteristics
explain the menstrual cycle and the two functions of menstruation and the changes in the ovary and uterus during the three phases.
menstrual cycle:
begins due to a decrease in progesterone and estrogen from the previous cycle
consists of the periodic changes occurring in the ovaries and uterus of a sexually mature, non-pregnant female that result in:
1. the production of a secondary oocyte
2. preparation of the uterus for implantation
Describe the general time course for the three phases of the menstrual cycle.
menstrual phase (days 1-5): uterus sheds all but deepest part of the endometrium
proliferation phase (days 6-14): endometrium rebuild itself
secretory phase (days 14-28)- endometrium prepares for implantation of the embryo
List the hormones of the female reproductive system and explain their functions and how their secretion is regulated.
before ovulation, FSH secretion increases, which stimulates follicles to develop and secrete estrogen
estrogen causes the endometrium, to proliferate and the hypothalamus to increase LH secretion, which results in the LH and FSH surges prior to ovulation
the LH surge causes a foliclle to mature and ovulate. the corpus luteum develops and secretes progesterone and some estrogen
the progesterone causes hypertrophy of the endometrium and has a negative feedback effect on LH and FSH secretion. THe corpus luteum continues to secrete progesterone for approx 12 days after ovulation
Discuss menopause, including the changes that result from it.
-the cessation or stoppage of a menstrual cycle
-perimenopause: the time between the beginning of irregular menstrual cycles and menopause
-occurs at about 40-50 years old
-menstrual periods become less regular, ovulation stops
-LH and FSH is elevated but the few remaining follicles become insensitive to LH and FSH
-ovaries stop producing estrogen and progesterone
-symptoms: hot flashes, irritability, night sweats, fatigue, etc.
Describe the major age-related changes in the male and female reproductive systems.
In males:
-testes decrease in size
-decrease in the number of interstitial cells
-thinning of walls of the seminiferous tubules
-impotence/decrease in sexual performance or activity
-the prostate with have a decrease in blood flow, increased cancer risk, possibly benign prostatic hypertrophy
In females:
-menopause occurs
-uterine position changes
-uterus decreases 50% in size within 15 years after menopause
-vaginal wall become thinner and drier
-sexual excitement lessens
-increased risk of breast, endometrial, cervical, and ovarian cancer