Complement system
1/32
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
33 Terms
What is the function of complement
Recognises pathogen or danger signals and triggers a response
What responses does the complement system trigger
Directly lyse pathogen to rupture target cell membranes
Opsonise pathogens to enhance phagocytosis
Act as chemoattractant to attract immune cells
Trigger degranulation of mast cells
How does the complement system work
Through recruitment and activation of zymogen-like proteins
Happens on the cell surface
Zymogen splits into two
Larger enzyme is retained at surface
Smaller part acts as chemoattractant or cell activator
Is complement potent
Extremely potent so tight regulation of complement activation is required
What are the modes of action
Direct inhibitors and blockade
Decay accelerator factors
Found on many WBC surfaces speeds up the decay of convertases
CD59 inhibits the formation of the membrane attack complex on host cell surfaces to protect host cells from being destroyed by the complement system
What does complement being non-specific mean
It must possess very broad activation mechanisms
The pathways to activation also give rise to differing effectors and lend their name to the 3 complement systems
What are the different effectors
The classical pathway
The alternative pathway
The lectin pathway
What are the features of the classical pathway
Activating signal - antigen antibody complex
Effectors - cell phagocytosis, cell lysis, WBC recruitment and activation
Targets - bacteria, viruses, parasites, fungi
Differences - inherently longer due to need for Abs
What are the features of the MB-lectin pathway
Activating signal - host mannose binding lectins
Effectors - cell phagocytosis, cell lysis, WBC recruitment and activation
Targets - bacteria, viruses, parasites, fungi
Differences - binds surface via soluble protein
What are the features of the alternative pathway
Activating signal - C3 binding to pathogen carbohydrates or proteins
Effectors - cell phagocytosis, cell lysis, WBC recruitment and activation
Targets - bacteria, viruses, parasites, fungi
Differences - binds directly to pathogen surface
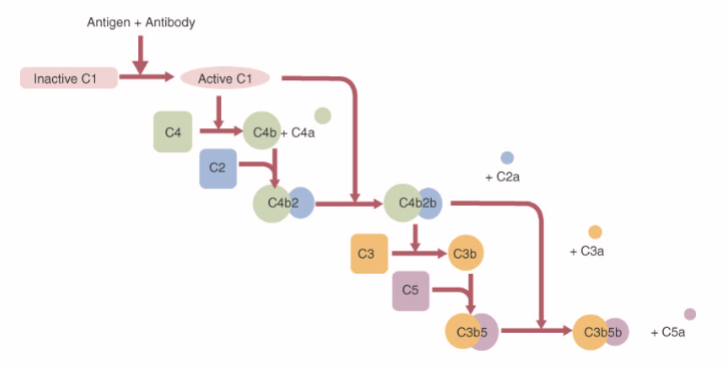
What happens in the classical pathway
Must have lots of antibodies to activate C1
Successive levels of activation
One activated it becomes 2 products
C4b2b also known as C3 convertase and is important part of pathway
C3b5 is first stage of membrane attack complex
Anaphlatoxin as biproduct causing inflammation and vasodilation
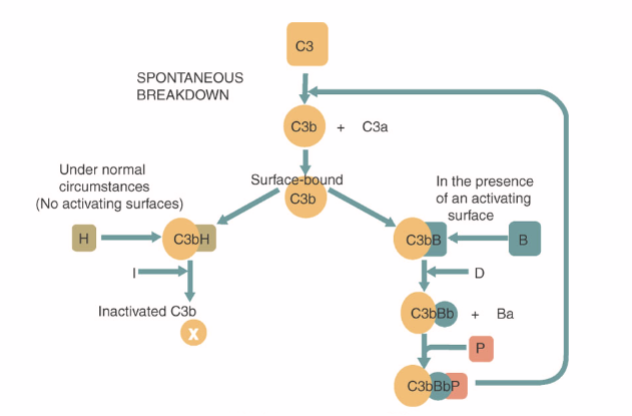
What happens in the alternative pathway
C3 spontaneously coverts without C3 convertase
Becomes activated if binding on a microbial surface
If on host surface it isn’t activated
Factor H binds in the blood to inactivate it
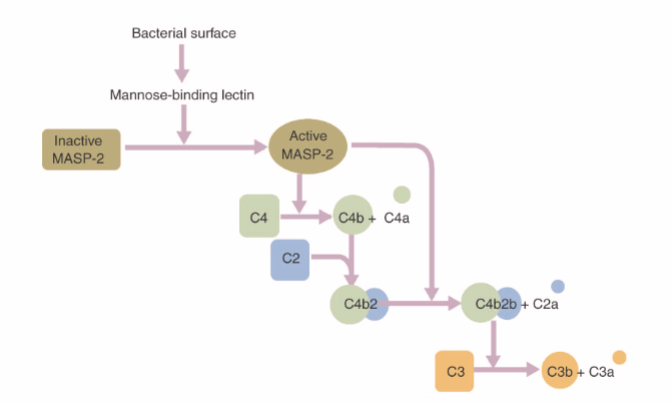
What happens in the MB-lectin pathway
What is C3 made by
Macrophages in the liver
What does C3 break down naturally into
C3a and C3b
What can C3b bind to
Microbe surfaces via carbohydrates
Factor H on host cells taking C3b out of circulation
What does C3a do
Acts as an anaphylatoxin or a chemoattractant
Where do all three pathways converge
On C3
How do MB- lectin and classical pathways converge
C4b + C2b → C3 convertase
How does the alternative pathway converge
C3b + Bb → C3 convertase
Why is there more C3b then C4b
Due to concentration effect as large amounts of C3 are cleaved to C3b then C4 cleaved to C4b
What are the anaphylatoxins
C3a
C4a
C5a
What do the anaphylatoxins do
Change smooth muscle
Increases vasodilation
Activates mast cells or neutrophils
Increases fluid in the tissue and speeds up lymph flow
What is the membrane attack complex
A central effector mechanism of the complement system and innate immune response
It is an endpoint of all 3 activation pathways
Can be referred to MAC or terminal complement complex
Composed of C5b, C6, C7, C8 and multiple copies on C9
What happens in the membrane attack complex
C5 → C5a and C5b
C5b binds to C6
C5b6 is bound by C7
C5b:C6:C7 complex allows the insertion of C7 into the phospholipid bilayer as a hydrophobic site is exposed on the C7 protein once in a complex
Complex is bound by C8
C8ß binds C5b and joins the surface
C8α and C8γ inserts into the cell membrane
This causes 10-16 copies of C9 to polymerise on the cell surface
What does the membrane attack complex do
Opens the bacterial cell cytosol
Dramatic loss of cellular homeostasis
Disrupts proton gradient
Penetration of host lysozome and other proteases
What is canine C3 deficiency
An inhereted disoder
Homozygote dogs have no serum C3
They have trouble making antibodies against certain pathogens
Increased pyometra, pneumonia and sepsis
What is the normal level of C3
126 mg/mL
What is porcine factor H deficiency
Inherited recessive autosomal disease
Carriers born normal up to a few weeks so production problems
DIe of anaemia and renal failure
Factor H stops C3b activation
In animals C3 accumulates on surface and basal membranes on kidneys
What does C3a and C5a do
Peptide mediators of inflammation and phagocyte recruitment
What does C3b do
Bind to complement receptors on phagocytes
Opsonization of pathogens
Removal of immune complexes
What do C5b, C6, C7, C8 and C9 do
Membrane attack complex
Lysis of certain pathogens and cells
What does MAC punching holes in membranes cause
Dramatic loss of cellular homeostasis
Disrupts proton gradient
Penetration of host lysozyme and other proteases