The Endocrine System
1/74
Earn XP
Description and Tags
These flashcards cover essential concepts related to the Endocrine System and hormonal functions.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
75 Terms
Endocrine System
A system composed of unicellular and multicellular glands that secrete hormones into the bloodstream.
Hormones
Signaling molecules synthesized by specific cells, tissues, or glands, carried in the blood to target cells.
Negative Feedback Loop
A regulatory mechanism where an increase in a product or response inhibits further hormone release or synthesis.
Amines
Small molecules derived from amino acids, including catecholamines such as epinephrine and norepinephrine.
Peptide and Protein Hormones
Large, complex molecules derived from peptide subunits, such as adrenocorticotropic hormone and antidiuretic hormone.
Steroid Hormones
Hormones derived from cholesterol characterized by cyclic hydrocarbon structures, including testosterone and estrogen.
Eicosanoids
Biologically active lipids synthesized from arachidonic acid; may not be classified as true hormones by some, but rather, signaling molecules
Lipid-Soluble Hormones
Hormones that can cross cell membranes and bind to cytoplasmic receptors, affecting gene transcription.
Will be bound to carrier proteins while in circulation that ensure the hormone gets to the target cell
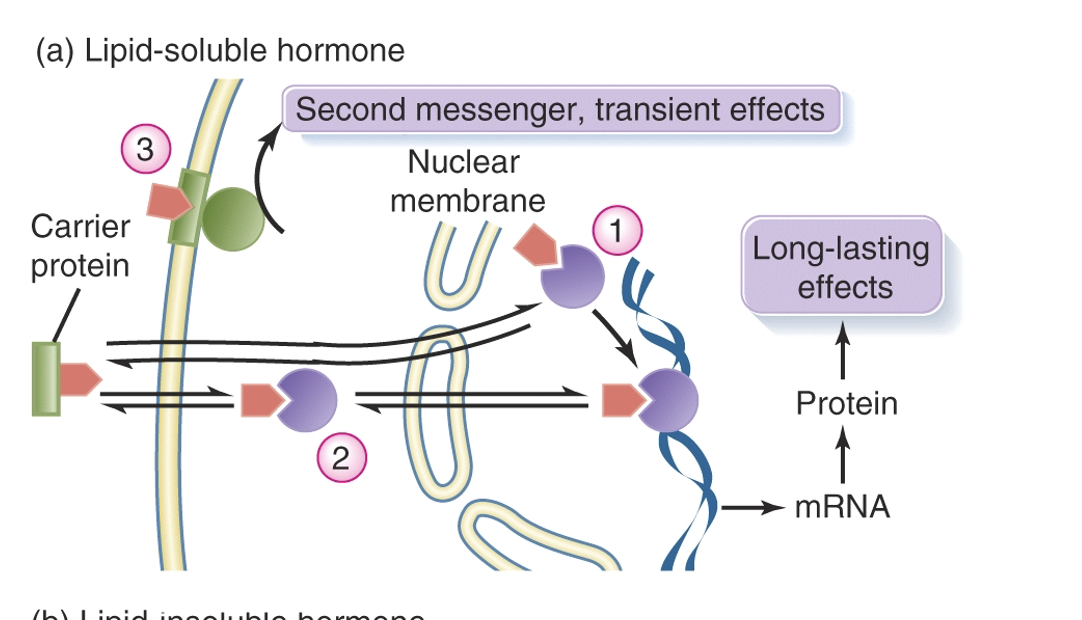
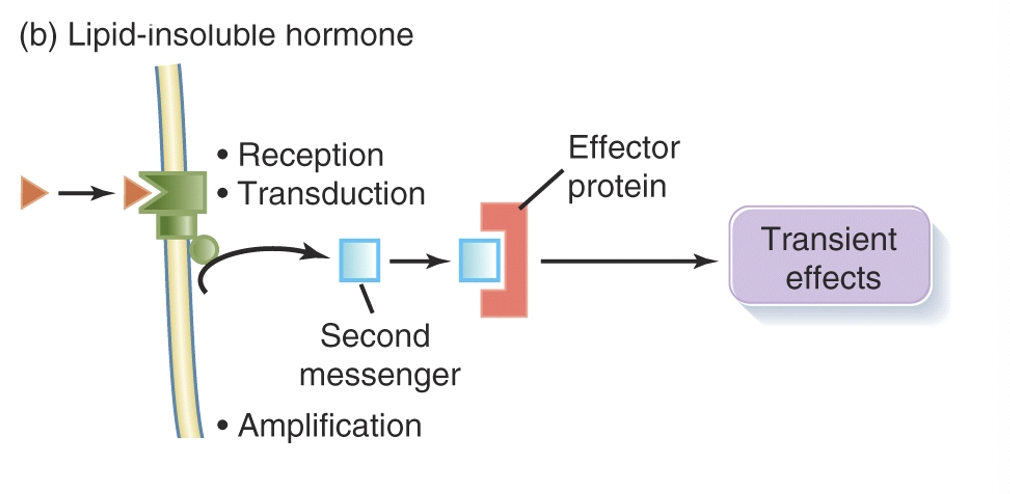
Lipid-Insoluble Hormones
Hormones that bind to surface receptors, generating secondary messengers that mediate quick cellular responses.
Three groups:
Cyclic Nucleotide Monophosphates (cNMP)
cAMP (adenosine 3’,5’-cyclic monophosphate)
cGMP (guanine 3’,5’-cyclic monophosphate)
Inositol Phospholipids
1,4,5-triphosphate (IP3)
1,2-diacyglycerol (DAG)
Ca+2
cAMP hormonal pathway
A lipid-insoluble hormone binds to a receptor protein on the target cell membrane
The binding of the receptor and hormone causes GTP to bind to the G protein
The activated G protein will activate adenylate cyclase, which will catalyze the conversion of ATP to cAMP
cAMP will then bind to Protein Kinase A
The catalytic subunit is now free to phosphorylate effector proteins using ATP for the high-energy phosphate group
In the case of hormones, the phosphorylated proteins will display an increase in activity
G proteins
Molecular switches that transmit signals from receptors to other intracellular proteins, involved in cAMP pathways.
Inositol Phospholipid Signaling Pathway
A lipid-insoluble hormone binds to a receptor protein on the target cell membrane
The binding of the hormones to the receptor-Gp protein activates Gp which, in turn, induces the activation of Phosphoinositide-Specific Phospholipase C (PLC)
PLC hydrolyzes Phosphatidyl Inositol Biphosphate (PIP2) into two major secondary messengers
When IP3 is the secondary messenger: IP3 detaches from the cell membrane and diffuses into the cytoplasm. IP3 then acts on calcium stores within the cell, especially in the ER
When DAG is the secondary messenger, it has two signaling roles:
It can be cleaved to release arachidonic acid
DAG can activate Protein Kinase C (PKC)
Growth Hormone (GH)
A peptide hormone secreted by acidophils that stimulates growth and metabolism in various tissues.
Oxytocin
Milk ejection, uterine contraction, arteriole vasoconstriction
Antidiuretic Hormone
Increases tubular reabsorption and water conservation
Somatotropin
Promotes growth
Prolactin (PR)
A hormone produced by acidophils that stimulates milk production and various metabolic processes in mammals.
Adrenocorticotropic Hormone (ACTH)
A polypeptide hormone that stimulates the adrenal glands to secrete glucocorticoids and other hormones. (mineralocorticoids, gonadocorticoids)
Thyroid Stimulating Hormone (TSH)
A tropic hormone that stimulates the thyroid gland to produce thyroid hormones like Thyroxine and Triiodothyronine
Melanocyte Stimulating Hormone
Promotes melanogenesis
Luteinizing Hormone
Promotes sex hormone production
Follicle Stimulating Hormone
Promotes the development of the reproductive system and gametogenesis
Calcitonin
A polypeptide hormone produced by parafollicular cells that decreases blood calcium levels by inhibiting osteoclast activity.
Parathyroid Hormone (PTH)
A hormone that increases blood calcium levels by stimulating bone resorption and renal reabsorption of calcium.
Catecholamines
Hormones produced by the adrenal medulla that include epinephrine and norepinephrine, affecting body metabolism and stress responses.
Insulin
A peptide hormone secreted by the pancreas that reduces blood glucose levels by promoting glucose uptake and storage.
Glucagon
A peptide hormone produced by the pancreas that raises blood glucose levels by stimulating glucogenolysis.
Follicular Phase
Begins with the release of FSH and stimulates the activation of several primordical follicles to enter into follicular maturation
Luteal Phase
The phase begins with ovulation, and the remaining cells from the follicle become the corpus luteum
Parturition
Oxytocin will stimulate uterine contractions to expel the offspring and placenta
Anestrus
A quiescent period when the animal is not receptive to breeding
Proestrus
The beginning stage when follicles are stimulated to go into the maturation cycle, the uterus swells, and the vagina
Estrus
Period of sexual receptivity of the female
Metestrus
If fertilization occurs: the corpus leteum will continue the thickening of the placenta and the embryos will go through gestation
If fertilization does not occur: the uterine lining will not be maintained and will be reabsorbed
Buriscon
Promotes cuticle development, induces tanning of cuticle
Ecdysone
Promoted the secretion of a new cuticle
Eclosion Hormone
Induces the emergence of the adult form from the chrysalis
Juvenile Hormone
Promotes synthesis of larval structures and inhibits metamorphosis in the larva
Prothoracicotropin
Stimulates the release of ecdysone
Corticotropin Release Factor
a peptide that stimulates ACTH release (Adrenocorticotropic hormone)
Gonadotropin Release Factor
A peptide that stimulates the release of FSH and LH
TSH Release Factor
A peptide that stimulates the release of TSH and PR
Somatostatin Inhibiting Factor
A peptide that inhibits the release of primarily GH and secondarily other hormones, including TSH, insulin, and glucagon
Neurosecretory cells in the hypothalamus
Located in two hypothalamic nuclei:
paraventricular
supraoptic nuclei
Stored in Hering Bodies
Neurohormones
Antidiuretic Hormone (ADH)/Vasopressin: a peptide that increases renal tubular reabsorption for increased water conservation
Oxytocin:
Causes vasoconstriction in arterioles in many animals
In mammals, oxytocin causes ejection of milk from the mammaries
Oxytocin may play a role in the orgasm and seems to promote pair bonding in many different species
Oxytocin causes uterine constrictions in mammals
Hormones of the Adenohypophysis
Acidophils:
GH (aka somatotropin)
targets many tissues including the liver and adipose tissue
promotes growth and lipid and carbohydrate metabolism
antagonist to insulin, stimulates gluconeogenesis
PR
targets the ovaries
promotes secretion of estrogen and progesterone
Basophils: ACTH, TSH, MSH, LH and FSH
ACTH
Targets the steroidogenic tissues associated with the adrenal gland
Stimulates the secretion of glucocorticoids, mineralocorticoids, and gonadocorticoids
TSH
Targets the thyroid gland
Two subunits: alpha and beta
Alpha is considered to be the effector region responsible for stimulating adenylate cyclase
Beta is an amino acid sequence UNIQUE TO TSH
MSH
Targets the pigment cells
LH
Glycoprotein that targets the gonads and promotes sex hormone production
FSH
Glycoproteine that targets the gonads and promotes development of hte reproductive system and gametogenesis
Antidiuretic Hormone (ADH), or Vasopressin
Regulation of water, glucose, and salts in the blood
Retains water, constricts blood vessels
Effect of ADH on the Mammalian Kidney
Raises water permeability in distal tubule and collecting duct cells, mainly through inserting Aquaporin-2 water channels into their membranes via V2 receptors
The G-protein coupled receptors activate adenylyl cyclase, converting ATP to cAMP, which triggers aquaporin-2 exocytosis and gene transcription, thus enhancing water absorption and urine concentration.
Boosts calcium by releasing Ca+2 from stores and increases urea reabsorption through urea transporter regulation, further concentrating urea.
Effect of ADH on the Blood Vessels
Increases resistance in the peripheral vasculature by stimulating the smooth muscles of the arterial walls to constrict, utilizing inositol phospholipids as the secondary messenger
Increases arterial blood pressure
Vasotosin
Similar to oxytocin and ADH - peptide hormone
Stimulates the recovery of water from kidneys
Plays a role in sexual behavior
Thyronines
Cells that produce the thyroid hormones
Arranged into hollow spheres called follicles (Follicular Cells)
Stimulated by TSH to produce the hormones THyroxine (T4) and 3,5,3’-Triiodothyronine (T3)
Iodine is required
Lipid-soluble, can cross the cell membrane and bind to recpetors within the cytoplasm
Parafollicular Cells (C cells)
Arranged into small clusters between thyroid follicle
Produce the hormone Calcitonin (Thyrocalcitonin)
Calcium and phosphorous metabolism
Nonmammalian vertebrates produce calcitonin via the Ultumiobranchial Gland
Parathyroid
Parathyroid Hormone (PTH)
Polypeptide hormone that acts as an antagonist to calcitonin
Enhances the release of calcium
By increasing production of activated vitamin D
Adrenal Gland
Adrenal medulla (aminogenic tissue): produces catecholamines, derived from ectoderm
Adrenal cortex (steroidogenic tissue): produces steroid hormones, derived from mesoderm
Vertebrate Variation
Mammals: distinct adrenal gland with cortex and medulla
Fishes: aminogenic and steroidogenic tissues are scattered cell clusters
Adrenal Medulla Function
Considered similar to a sympathetic ganglion
Innervated by sympathetic preganglionic neurons
Releases hormones into blood instead of synapses: acts like modified postganglionic neurons
Chromaffin Cells
Acetylcholine → Increased Ca+2 permability → increased intracellular Ca+2 → exocytosis
Catecholamines
Produced by the adrenal medulla: epinephrine and norepinephrine, causes fight-or-flight response
Catecholamine Synthetsis
Tyrosine → DOPA → Dopamine - Norepinephrine → Epinephrine
Adrenoreceptors
Alpha receptors:
IP3 → increased Ca+2 → smooth muscle contraction
Beta receptors:
cAMP → cardiac contraction, bronchodilation, lipolysis
Adrenal Cortex Layers
Zona glomerulosa: mineralocorticoids (aldosterone)
Zona fasciculata: glucocorticoids (cortisol)
Zona reticularis: androgens
Aldosterone Function
primary regulator of blood pressure, fluid balance, and electrolytes
increases sodium reabsorption and water retention while promoting potassium excretion, thus raising blood volume and pressure.
LONG TERM BLOOD PRESSURE REGULATION
Cortisol Function
Increased glucose (gluconeogenesis)
Increased fat and protein breakdown
Anti-inflammatory
Stress response hormone
What hormones are produced by the Zona Reticularis?
Androgens (testosterone, DHT, androstenedione, DHEA)
How to steroid hormones like cortisol and aldosterone act?
They cross cell memrbanes, bind to intracellular receptors, and affect gene transcription
DHEA
Steroid hormone that serves as a metabolic intermediate for the production of other androgens and estorgenF
Follicular phase
Begins with the release of FSH by the adenohypophysis
During follicular maturation, primordial follicles will go through developmental changes, resulting in a mature follicle called a Graafian Follicle
LH will also be released from the adenohypophysis
FSH will stimualte the productionof the enzyme aramotase which will convert androgens into estrogens
Surge in estrogen levels stimualtes the hypothalamus, triggers the adenohypophysis to increase FSH and LH
Insect Development
Holometabolous: complete metamorphosis
Hemimetabolous: incomplete metamorphosis
PTTH (Prothoracicotropic Hormone)
Produced in brain neurosecretory cells
Stored/released via corpora allata
Stimulates prothoracic gland, releasing ecdysone
Ecdysone
Steroid hormone
alpha-ecdysone: prohormone
beta-ecdysone: active form (molting and new cuticle formation)
Juvenile Hormone (JH)
Maintains juvenile characteristics
How do ecdysone and juvenile hormones work together?
Ecdysone triggers molting, juvenile hormone determine what stage comes next
Bursicon
Protein hormone, causes hardening and darkening (tanning) of new cuticle
Corporal allata
Stores/releases hormoensPr
Prothoracic gland
Produces ecdysone