bones study guide
1/98
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
99 Terms
What are the functions of bone?
Support, protection, movement, mineral storage, blood cell formation, triglyceride storage.
What is hematopoiesis?
Blood cell production in red bone marrow.
If given or shown a bone, be able to determine what classification it belongs to.
Long, short, flat, irregular, sesamoid.
What two types of bone texture do we find in bones?
Compact bone and spongy bone.
Describe the structure of flat bones.
Compact bone on outside, spongy bone (diploë) inside.
What types of bone would we find in flat bones?
Outer compact bone, inner spongy bone.
What type of bone marrow would we find in flat bones?
Red bone marrow.
What is the diaphysis?
-Tubular shaft that forms the axis of long bones
Composed of compact bone surrounding a medullary cavity (medulla = innermost)
The medullary cavity contains either red bone marrow and/or yellow bone marrow (fat)
What type of bone is predominantly found in the diaphysis? Why that kind of bone?
Compact bone, Resists bending and provides strength.
What is the medullary cavity? What would we find here?
Central cavity of diaphysis. Red bone marrow and/or yellow bone marrow.
Where would we find the epiphyses?
Ends of long bones.
Describe the types of bone found at the epiphyses.
Outer compact bone, inner spongy bone.
What type of cartilage is found at articular surfaces?
Hyaline cartilage.
What are the metaphyses? What important structure is found here?
Regions between diaphysis and epiphysis.
in growing bones, includes the epiphyseal plate
in mature bone, includes the epiphyseal line
Difference between epiphyseal plate and epiphyseal line?
Plate = cartilage (growing); line = bone (growth complete).
What is periosteum?
double-layered outer membrane
Where would you find periosteum?
External bone surface except joints.
Would you find periosteum on articular surfaces? What would you find instead?
No. Articular cartilage.
Describe the two layers of periosteum.
1. Dense fibrous outer layer – dense irregular connective tissue proper
2. Cellular inner layer – contains osteogenic cells and osteoblast
What tissue makes up the outer fibrous layer?
Dense irregular connective tissue.
What specialized cells are in the cellular layer? What role do they play? What type of growth are they responsible for?
Osteoblasts, osteoclasts, osteoprogenitor cells.
Bone growth and remodeling.
Appositional growth
What are nociceptors?
Pain receptors.
Is it easy to detach a muscle from a bone?
No, because collagen fibers of tendons blend with periosteum.
What is endosteum?
Delicate cellular layer covering internal surfaces of bone
Where would you find endosteum?
Medullary cavity and trabeculae surfaces.
Covers the trabeculae of spongy bone and the canals (passageways for blood vessels) that pass through compact bone
What specialized cells are found in endosteum? What roles do they play?
• Contains osteogenic cells, osteoblasts, and osteoclasts
• Bone growth, repair, and remodeling occur here
What type of extracellular matrix does bone have?
Solid, mineralized matrix.
What mineral is bone predominantly composed of?
Calcium phosphate
What type of fiber do we find in bone?
Collagen.
What is the function of collagen fiber?
Provide a framework for calcium crystals
Allows for some flexibility
What would bone be like without collagen?
Brittle and easily fractured.
What are the specialized cells in bone?
Osteogenic cells, osteoblasts, osteocytes, osteoclasts.
Function of osteogenic cells?
Stem cells that produce osteoblasts.
Function of osteoblasts?
Build bone matrix.
Secrete osteoid – unmineralized bone matrix
Function of osteocytes?
Maintain bone matrix.
Function of osteoclasts?
Break down bone matrix.
What is osteoid?
Unmineralized bone matrix.
What fiber is found in osteoid?
Collagen.
When do osteoblasts differentiate into osteocytes?
When osteoblasts become surrounded by bone matrix
Where would we find osteocytes?
In lacunae within bone matrix.
What is the functional unit of compact bone?
Osteon.
How are osteons oriented relative to stress?
The medial side of the diaphysis experiences compression.
The lateral side of the diaphysis experiences tension.
Why is the diaphysis mostly compact bone?
To withstand compression and bending forces.
Why is spongy bone found in areas with little stress?
Lighter and reduces weight.
What advantage does spongy bone have over compact bone?
Reduces bone weight, easier movement.
Are trabeculae arranged randomly?
No.
Open network of branching trabeculae (”beams”) – reduces weight
• Cross-braced trabeculae oriented long lines of stress
What determines trabeculae organization?
Lines of stress.
What two types of forces do bones experience?
Compression and tension.
Are trabeculae organized into osteons?
No.
How do osteocytes in spongy bone get nutrients?
Diffusion from blood in marrow spaces.
Describe microscopic structure of compact bone.
Osteons with central canal, lamellae, lacunae, canaliculi.
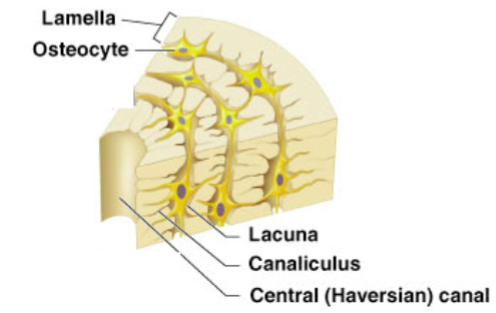
Describe microscopic structure of spongy bone.
Trabeculae with marrow-filled spaces.
What would we find in open spaces of spongy bone?
Red or yellow marrow.
Are bones vascular or avascular?
Vascular.
Identify blood vessels supplying bone.
Perforating canals, central canals, metaphyseal vessels, and periosteal vessels.
What is yellow bone marrow composed of? What is its function?
Adipose tissue. Fat storage.
Where is yellow marrow found?
Medullary cavity of long bones.
What is the function of red bone marrow?
Hematopoiesis.
Where is red marrow found?
Flat bones, epiphyses of long bones.
What is hematopoiesis?
Blood cell formation.
Difference between calcification and ossification?
Calcification = mineral deposition; ossification = bone formation.
What are the two types of ossification?
Endochondral and intramembranous.
Where does endochondral ossification occur?
Hyaline cartilage models.
bone replaces a hyaline cartilage bone model
Forms all the bones of the skeleton below the base of the skull (except the clavicles)
Where does intramembranous ossification occur?
Fibrous connective tissue membranes.
bone develops directly from embryonic fibrous connective tissue
Forms most of the flat bones of the skull, mandible, and clavicle
Describe endochondral ossification.
on other quizlet
Cartilage model → calcification → primary ossification center → medullary cavity → secondary centers → epiphyseal plate.
What is appositional growth? What cells are involved? How does it occur?
increase in Bone Thickness. Osteoblasts and osteoclasts. Osteoblasts add bone to outer surface; osteoclasts remove inner bone.
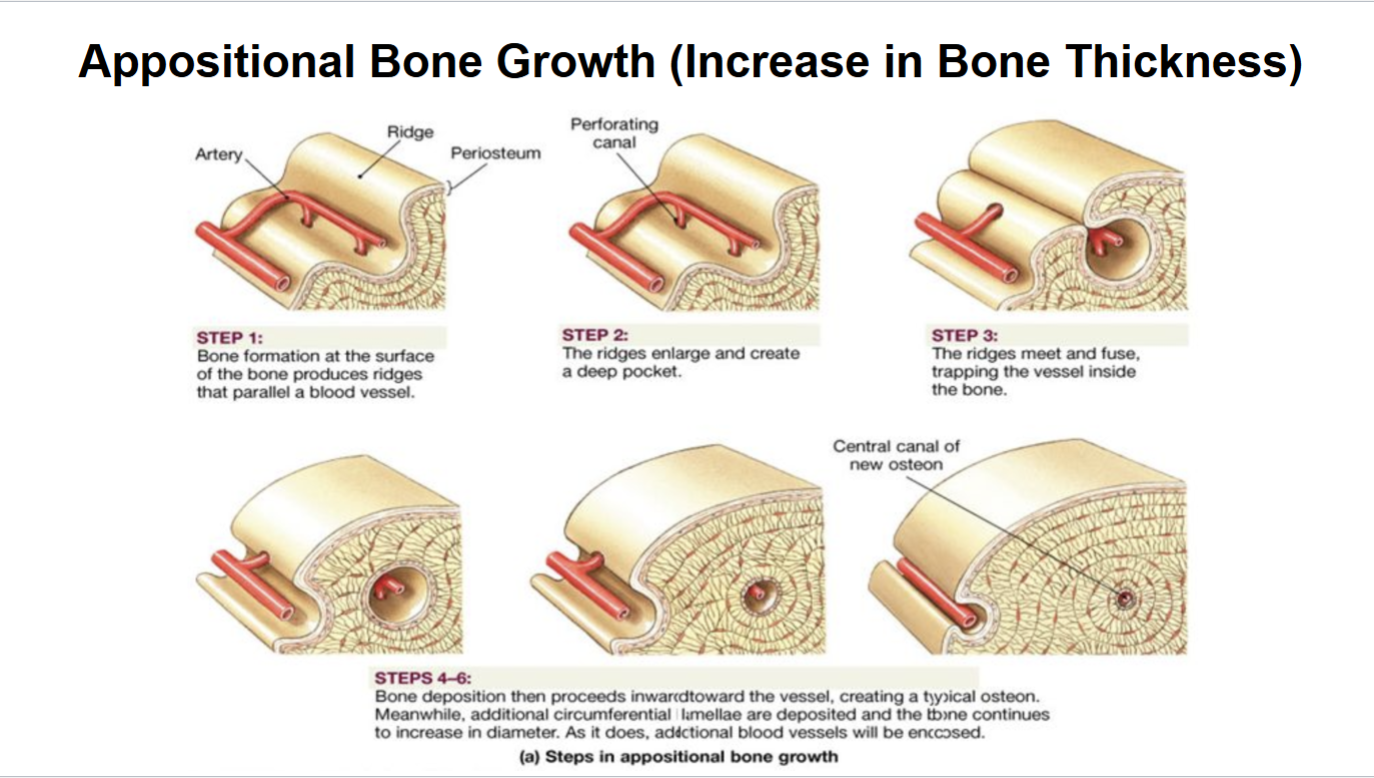
How do long bones increase in length?
Through epiphyseal plate activity.
What are the four zones of the epiphyseal plate?
Resting, proliferation, hypertrophy, calcification.
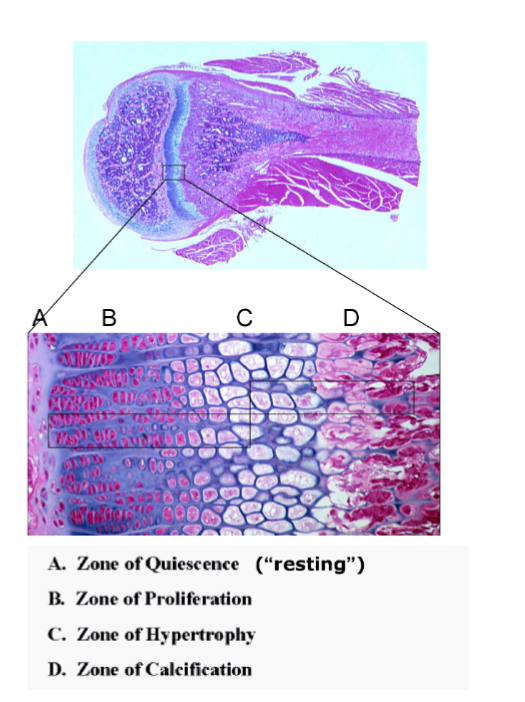
Difference between gigantism and acromegaly?
Gigantism = childhood GH excess; acromegaly = adult GH excess.
What is Marfan syndrome? What causes increased stature?
Connective tissue disorder causing tall stature and long limbs. Increased cartilage formation at epiphyseal plate and affects other connective tissues in the body.
What is achondroplasia? What causes decreased stature? Why are head and trunk normal size?
Genetic disorder causing short limbs. Inhibits chondrocyte proliferation at epiphyseal plate. They grow via intramembranous ossification.
Do bones have nerves?
Yes.
Where are nerves found?
Periosteum, endosteum, marrow cavity.
Which bones form via intramembranous ossification?
Flat bones of skull, mandible, clavicles.
Describe intramembranous ossification.
Mesenchymal cells → osteoblasts → osteoid → calcification → trabeculae → compact bone.
Which cells are responsible for bone resorption? How do they accomplish this?
Osteoclasts. Secrete acids and enzymes.
What is bone remodeling? Why does it occur?
An active and continuous process in which bone is resorbed and deposited. Maintain strength, mineral homeostasis.
Can bone shape be altered after formation?
Yes.
What effect does mechanical stress have?
Strengthens bone (Wolff’s law).
What minerals are needed for mineralization?
Calcium and phosphate
Importance of vitamin D3 and vitamin D?
Needed for Ca2+ and phosphate absorption in digestive tract
How do we get vitamin D3?
Skin + sunlight.
Where does vitamin D come from?
Activation in liver and kidneys.
What role does vitamin C play?
Collagen synthesis.
Effect of growth hormone, thyroxine, and sex hormones on bone?
Stimulate osteoblast activity (bone growth).
What stimulates calcitonin secretion? What gland secretes calcitonin?
High blood calcium. Thyroid gland.
How does calcitonin decrease blood calcium? Is this positive or negative feedback?
Inhibits osteoclasts. Negative.
What stimulates parathyroid hormone secretion?
Low blood calcium.
What gland secretes PTH?
Parathyroid glands.
How does PTH increase blood calcium?
Stimulates osteoclasts, increases absorption, reduces excretion.
Is maintaining Ca²⁺ levels important?
Yes.
What processes depend on Ca²⁺?
Muscle contraction, nerve function, blood clotting.
What is hypocalcemia?
Low blood calcium.
What is hypercalcemia?
High blood calcium.
What are fractures?
Breaks in bone.
Difference between compound and simple fracture?
Compound breaks skin; simple does not.
Steps in fracture repair?
1. Fracture hematoma formation (blood clot)
2. Callus formation
3. Spongy bone formation
4. Compact bone formation
Difference between osteopenia and osteoporosis?
Osteopenia = mild bone loss; osteoporosis = severe bone loss.
Why does bone density decrease after menopause?
Reduced estrogen.