ASCI 438
1/21
Earn XP
Description and Tags
CHAPTER 9, MIDTERM II
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
22 Terms
Anatomy of the heart
1st organ to become fully functional
Circulatory system
Heart: Pump! pressure gradient for blood to travel to all tissues
Blood vessels: Passageways that blood uses to travel to all parts of the body
Blood: Transport medium for O2, nutrients, wastes, long distances
Travels in 2 loops! (Continuously, both from the heart)
Pulmonary Circulation
Closed loop, carries blood between the heart and the lungs
Systematic Circulation:
Carries blood between the heart and all body systems (except lungs)
The heart is positioned in the middle of the thoracic cavity
Heart composition: Hollow, muscular, the size of a closed fist
Positioned at an angle, lies mostly on the right side, apex thumbs to the left
We listen to it on the left bc on the right, there are bones surrounding it
Location: Thoracic cavity, midline between the sternum anteriorly and verebrae
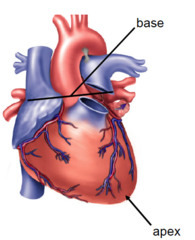
The heart is a dual pump
The left and right side of the heart functions as 2 separate pumps!
Heart division: L and R, top and bottom= 4 chambers
Atria= Receive blood via veins (vessels that return blood to heart), transfer it to ventricles
Ventricles=Pump blood out the heart, via arteries(out of heart)
Septum= L and R sides are separated by this
The complete circuit of blood flow
Blood returns from the systemic circulation (right side) via 2 large veins: VENAE CAVAE- 1 returns from above heart level, and one from below
Blood entering the RA is returning from body tissues where O2 has been taken out, and CO2 has been added
From RA, the blood goes to RV passing through the tricuspid valve, and gets pumped out through the pulmonary artery-it has 2 branches 1 to ea
ch lung.
Then the blood leaves the lungs via 2 veins, pulmonary veins 1 coming from each lung into the LA, passing through the mitral valve(bicuspid valve) into the LV
Then blood gets carried out by a single artery- AORTA the aorta then branches out into major arteries into the systemic circulation
*The R side receives deoxygenated blood from systemic circulation and pumps it into the pulmonary circulation*
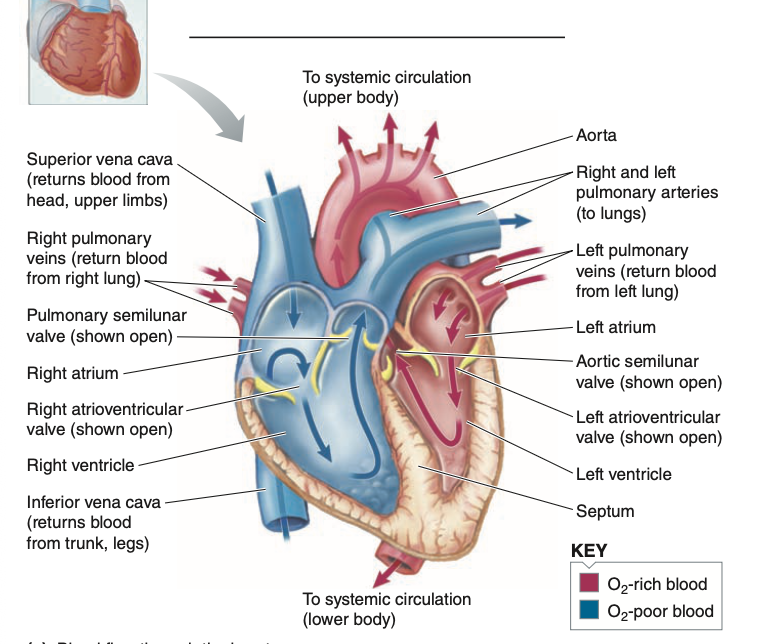
Comparison of the right and left pumps
LEFT PUMP
Systemic circulation
high pressure
high-resistance system
works harder bc it pumps out the same volume of blood as the right side with higher pressure/resistance
longer system
thicker muscle
RIGHT PUMP
Pulmonary circulation
low pressure, low resistance
Things in common
Pumps out an equal amount of blood
same volume
Pressure: force exerted on the vessel walls by the blood pumped into them by the heart
Resistance: Opposition to blood flow, caused by friction between the flowing blood and the vessel wall.
Pressure-operated heart valves ensure that blood flows in the right direction through the heart
Blood flow- one fixed direction
Veins→Atria→Ventricles→Arteries
How is it possible?There’s 4 one way valves, they can open and close passively due to pressure differences
Forward pressure gradient: more pressure behind valve, forces the valve open
Backward pressure gradient:more pressure in from of valve, forces the valve closed
Can force the door closed but cannot force it to swing open
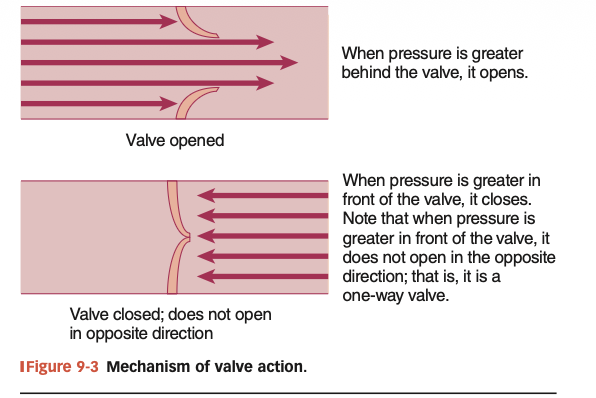
Atrioventricular valves between the atria and the ventricles
Right and left atrioventricular (AV) valves are positioned between the atrium and ventricle
Tricuspid valve: the right AV valve
Bicuspid valve (mitral valve): the left AV valve
The edges of the AV valve leaflets are fastened by tough, thin cords= Chordea tendinae- prevent the valve from everting, the cords extend from the edges of each cusp and attach to a small nipple-shaped structure= Papillary muscles
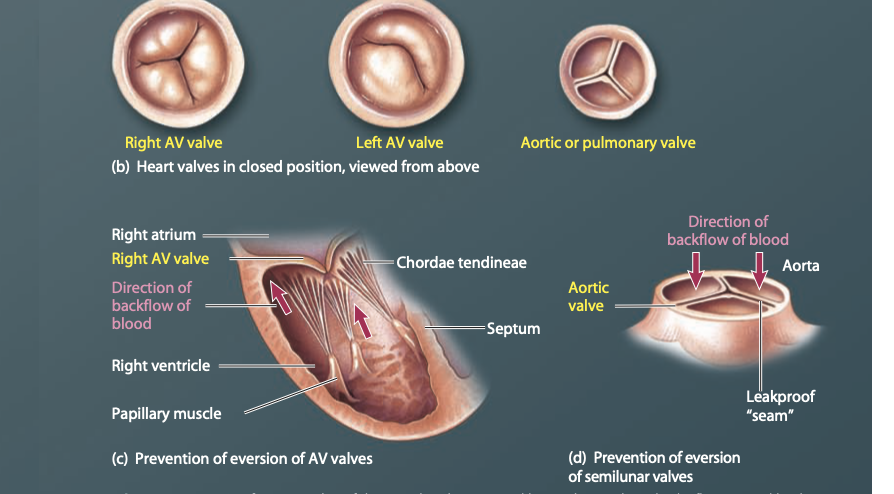
Semilunar valves between the ventricular and major arteries
The AORTIC AND PULMONARY ARTERIES-lie at the junction where the major arteries leave the ventricles= semilunar valves
They have 3 cusps resembling a shallow half-moon shape
The valves are forced to open when the L and R ventricular pressures exceed the pressure in the aorta and pulmonary artery
Closure results when the ventricles relax, and closed valves prevent blood from flowing from the arteries back into the ventricles
Prevented from everting by the structure and positioning of the cusp
No valves between atria and veins
There are no valves between the atria and veins but backflow of blood from the atria into the veins is not a problem
Why?
Atrial pressure usually are not much higher than venous pressures
sites where the veanea cavae enter the atria are partially compressed during atrial contraction
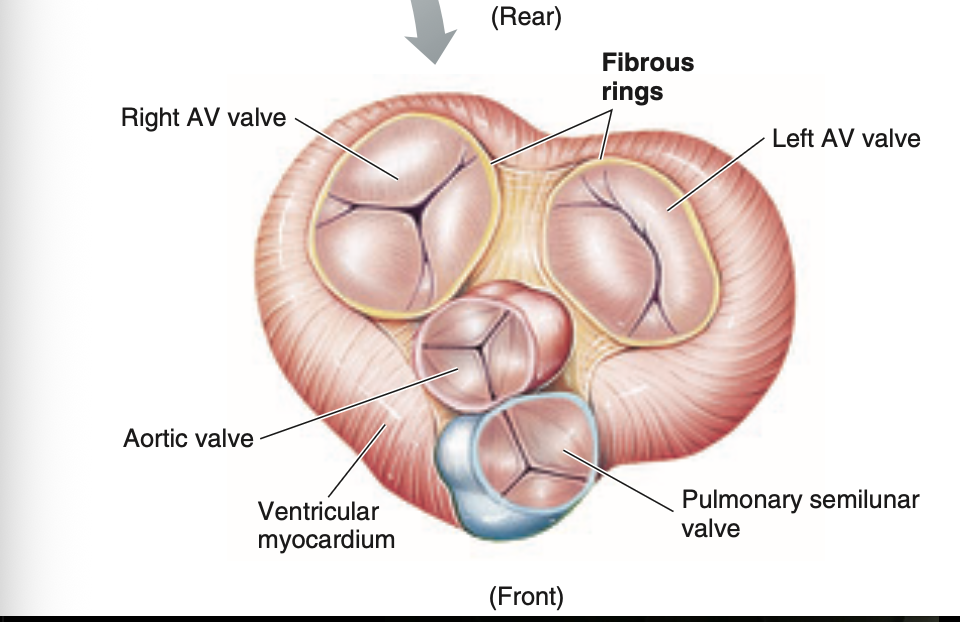
Fibrous skeleton surrounding the valves
Fibrous skeleton= 4 interconnecting rings of dense connective tissue sorround and support the 4 heart valves
Also separates the atria from the ventricles and provides a rigid structure
The atrial muscle is anchored above the rings, and the ventricular muscle is attached to the bottom of the rings.
The heart walls are composed primarily of spirally arranged cardiac muscle fibers
The heart has 3 layers
Endothelium =A thin, inner layer, unique type of epithelium tissue that lines the entire circulatory system
Myocardium =A middle layer, composed of cardiac muscle and constitutes the bulk of the heart wall
Epicardium =A thin, external layer, that covers the heart
The myocardium- interlacing bundles of cardiac muscle fibers, spirally around the heart. when the ventricular muscle contracts and shortens the diameter of the ventricular chambers is reduced and the apex is pulled toward the base of the heart.
Cardiac muscle cells- have an abundance of energy-generating mitochondria, rich blood supply delivered by one capillary for each myocardial fiber
Cardiac muscle fibers are interconnected by intercalated discs from functional syncytia
Intercalated discs: Where individual cardiac muscle cells are interconnected ro form branching fibers, w/ adjacent end to end specialized structures
Membrane junctions:
Desmosomes: type of adhering junction that mechanically holds cells together, abundant in tissues such as the heart, that are subject to mechanical stress
Gap Junctions: Areas of low electrical resistance that allow AP’s to spread from one cardiac cell to adjacent cells
Heart muscle besides pumping blood it secretes a hormone associated with the regulation of blood pressure
The heart is enclosed by the pericardial sac
The heart is enclosed in the double-walled membranous pericardial sac.
2 layers
Fibrous covering: attaches to the connective tissue partition that separates the lungs, and anchors the heart so it remains properly positioned in the chest
secretory lining: secretes pericardial fluid- provides lubrication to prevent friction between the pericardial layers as they glide over each other every beat of the heart
PERICARDITIS: inflammation of the pericardial sac = painful friction between the 2 pericardial layers, viral and bacterial infection
Electrical activity of the heart
AUTORHYTMICITY/AUTOMATICITY: contraction of cardiac muscle cells to eject blood, triggered by APs sweeping across the muscle cell membranes, contraction/beats rhythmically as a result of APs
There are 2 specialized types of cardiac muscle cells:
contractile cells: which are 99% of the cardiac muscle cells these working cells normally do not initiate their action potentials
autorrhythmic cells: small but extremely important remainder of the cardiac cells, do not contract! but initiate and conduct AP’s responsible for the contraction of the working cells
Cardiac autorhythmic cells display pacemaker activity
Cardiac autorhythmic cells do not have a resting potential!
They have a pacemaker activity!- their membrane potential slowly depolarizes, drifts, between ap’s until the threshold is reached.
Pacemaker Potential: autorhythmic cell membranes slow drift to thrrshold
Pacemaker potential in autorhytmic cells