Chapter 25 Digestive System Outline
1/64
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
65 Terms
5 stages of digestion
Ingestion: intake of food
Digestion: mechanical and chemical breakdown of food into usable form
Absorption: uptake of nutrients by digestive tract, then blood and lymph
Compaction: absorbing water and consolidating indigestible residue into feces
Defecation: elimination of feces
Mechanical digestion occurs…
in the mouth (physical breakdown of food into smaller particles)
teeth cut and grind while stomach and small intestines churn
Chemical digestion
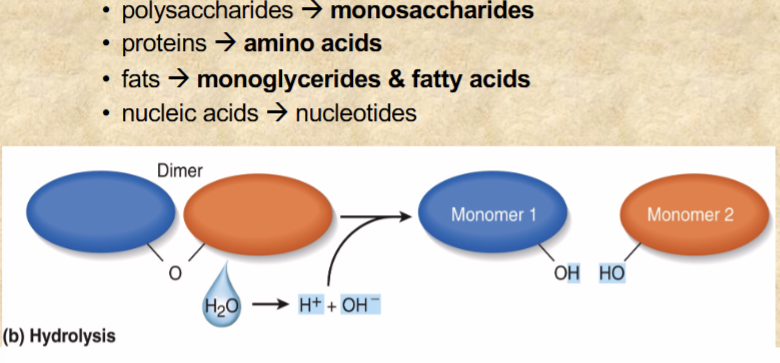
HYDROLYSIS reactions that break dietary macromolecules into monomers
by digestive enzymes from salivary glands, stomach, pancreas, and small intestine
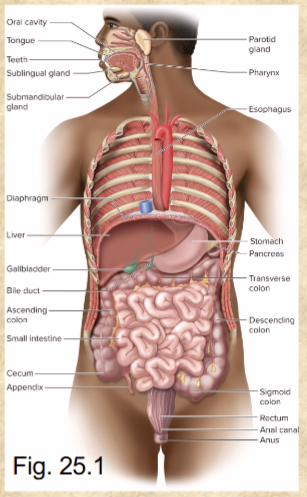
Digestive tract or alimentary canal consists of
mouth, pharynx, esophagus, stomach, small & large intestines
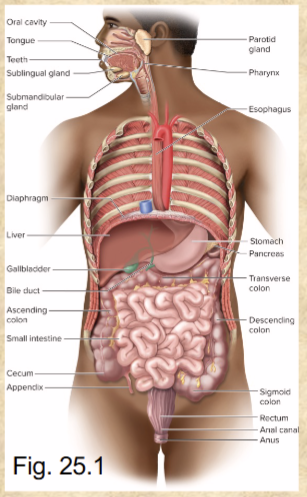
Accessory organs consist of
teeth, tongue, salivary glands, liver, gallbladder, and pancreas
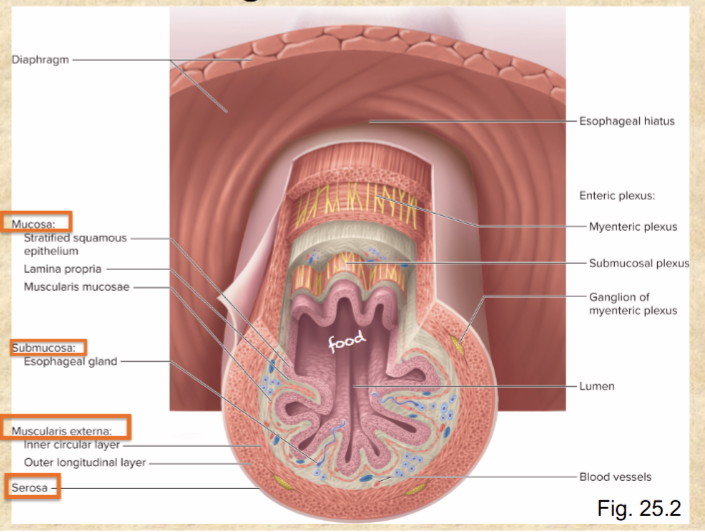
4 layers of the digestive tract wall inner to outer
mucosa, submucosa, muscularis externa, serosa
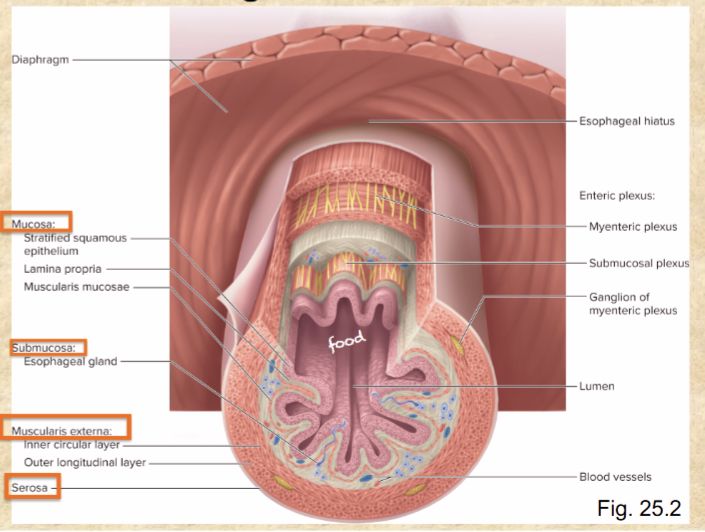
Layers of mucosa
stratified squamous epithelium
lamina propria
muscularis mucosae
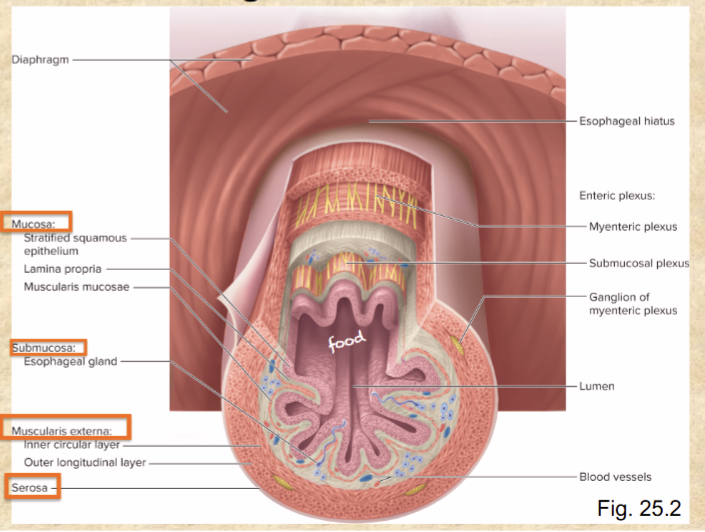
Layers of muscularis externa
inner circular layer
outer longitudinal layer
Enteric nervous system
network in esophagus, stomach, and intestines
senses tension in gut wall, conditions in lumen
regulates motility, secretion, and blood flow
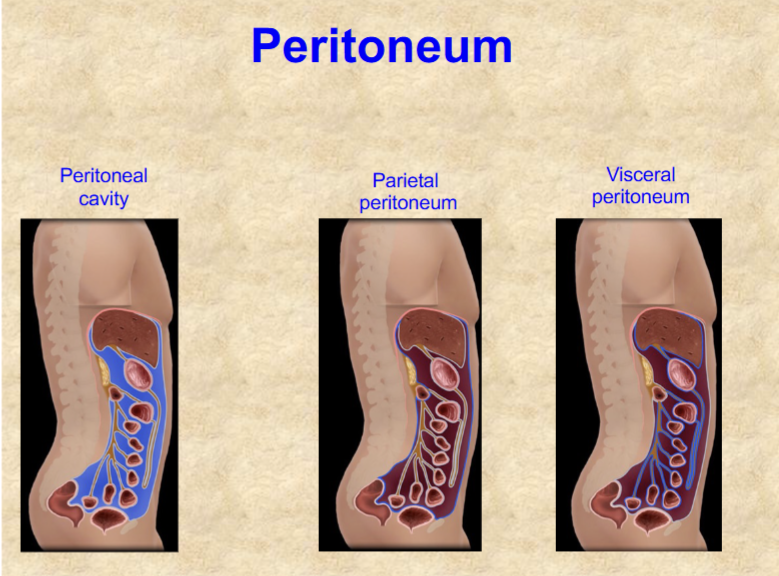
Mesenteries relationship to peritoneum
connective tissue, suspend stomach and intestines from abdominal wall
hold viscera in proper place
prevent intestinal twisting
provide passage of blood vessels and nerves
hold lymph nodes & lymphatic vessels
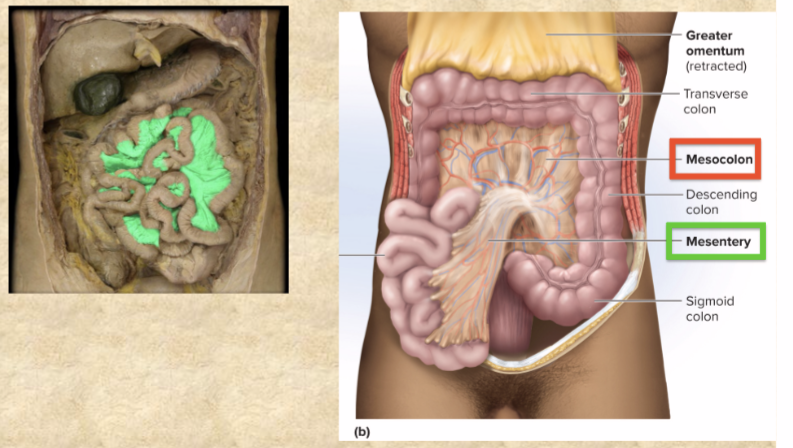
Mesocolon
anchors colon to posterior abdominal wall
Motility and secretion controlled by what 3 mechanisms?
neural, hormonal, and paracrine mechanisms
Neural control of motility and secretion (short vs long reflexes)
short: stretch or chemical stimulation acts through myenteric plexus
stimulates peristalsis (wave-like muscle contractions)
long: parasympathetic stimulation of digestive motility and secretion
Hormonal control of motility and secretion
via blood, stimulate DISTANT parts of digestive tract
gastrin & secretin
Paracrine secretions
diffuse through tissue fluids to stimulate NEARBY target cells
mouth=
buccal cavity
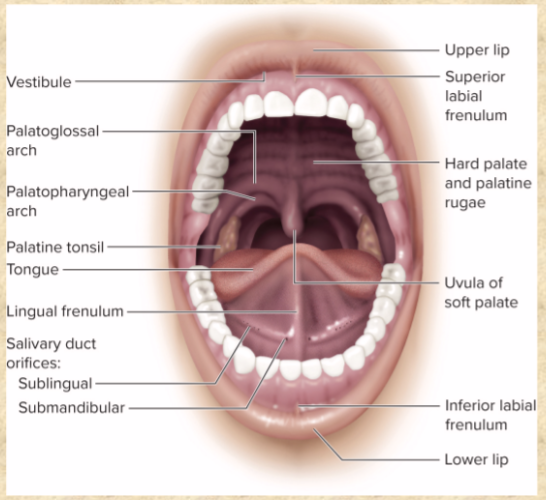
tongue functions
agile and sensitive organ
manipulates food between teeth while avoids being bitten
sensitive enough to feel stray hair in bite of food
tastes
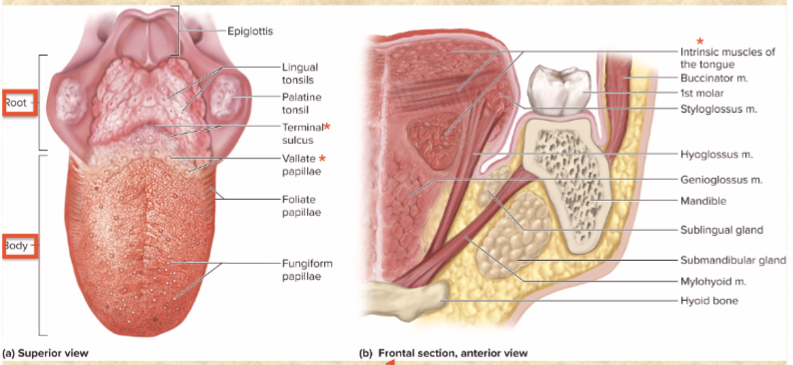
lingual papillae
tiny projections—sites of taste buds
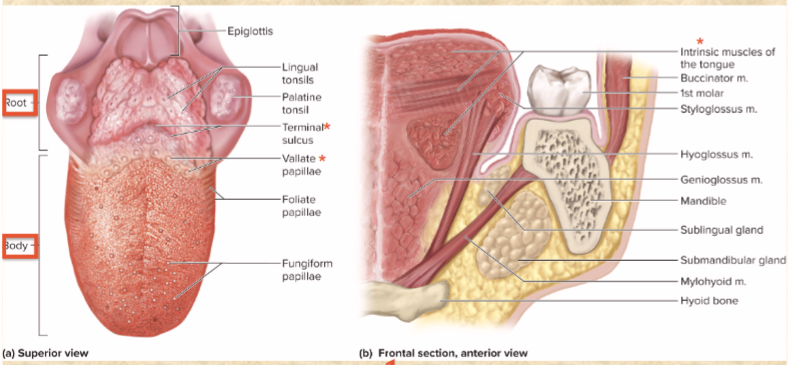
vallate papillae
v-shaped row—boundary between body and root
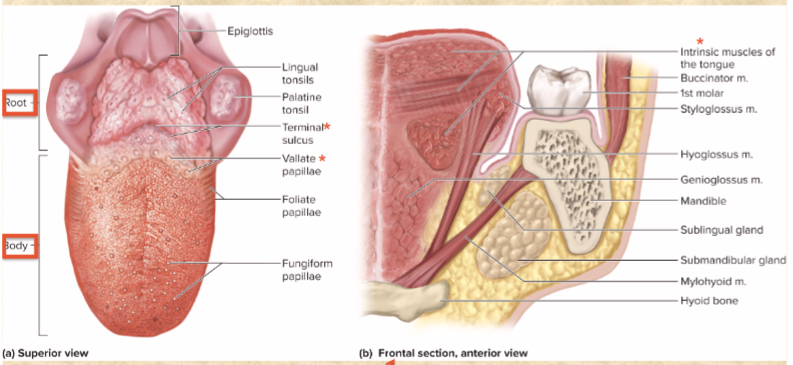
terminal sulcus
groove behind vallate papillae
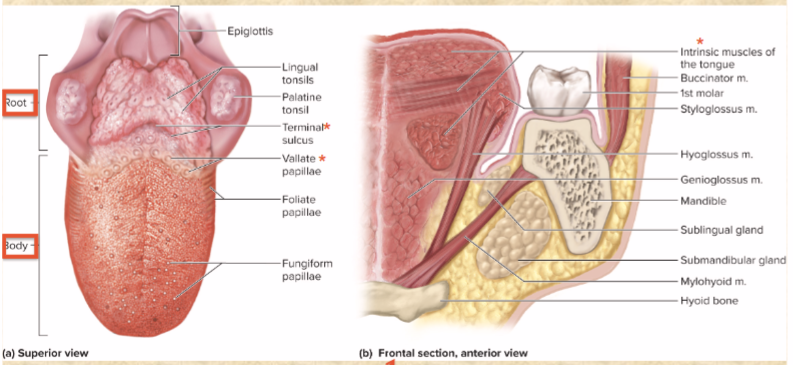
lingual frenulum
median fold— attaches body to floor
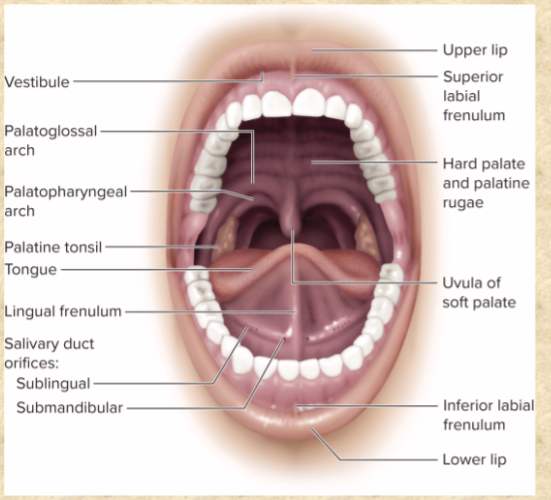
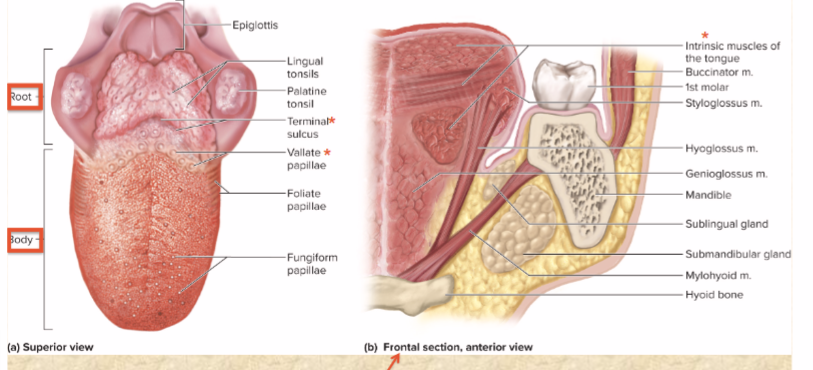
intrinsic muscles
contained entirely within tongue
subtle movements of speech
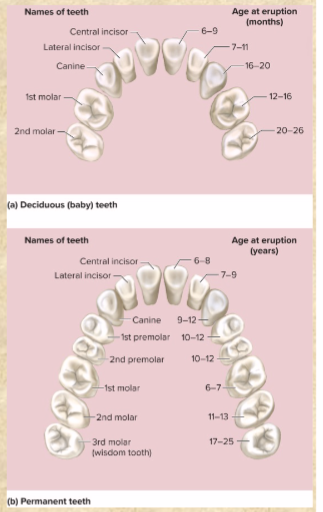
32 adult teeth, 20 baby teeth from midline to rear type of teeth
2 incisors—chisel-like; cut/bite
1 canine—pointed; puncture & shred
2 premolars—broad surface; crush & grind
3 molars—even broader surface! crush & grind
crown, root, neck, and gingival sulcus of tooth
above gum
below gum
where crown, root, and gum meet
space between tooth and gum
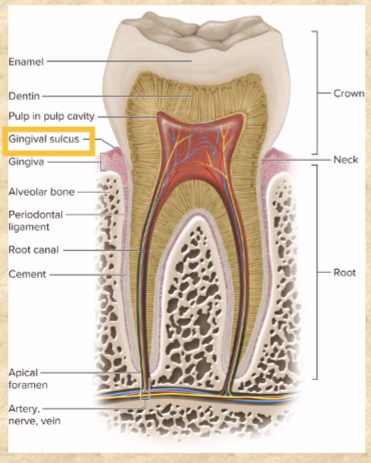
Cement, Dentin, and Enamel of tooth
covers root—living
makes up most inside of tooth—living
covers crown and neck—non-living
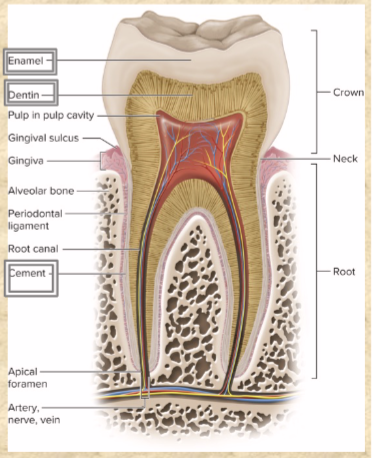
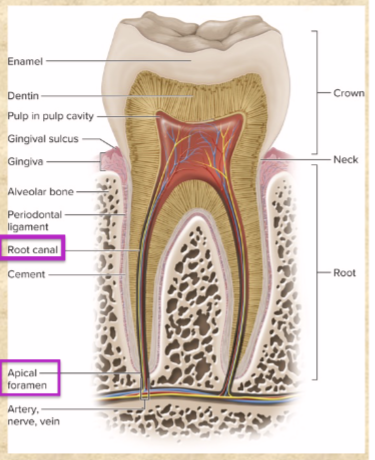
Root canal and apical foramen of tooth
nerves and blood vessels
pore at basal end of canal
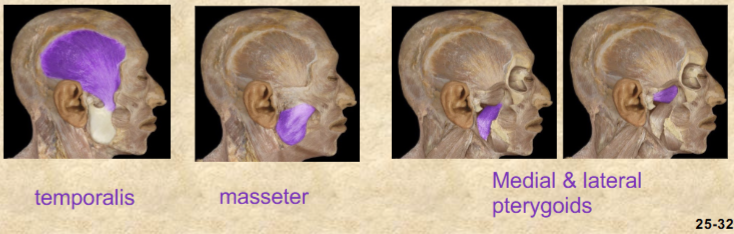
Mastication is first step in…
mechanical digestion (breaks down food into smaller particles)
temporalis, masseter, medial and lateral pterygoids are key muscles involved in mastication
Saliva functions
moisten mouth
– begin starch & fat digestion
– cleanse teeth
– inhibit bacterial growth
– dissolve molecules for taste
buds
– moistens food, binds into
bolus for swallowing
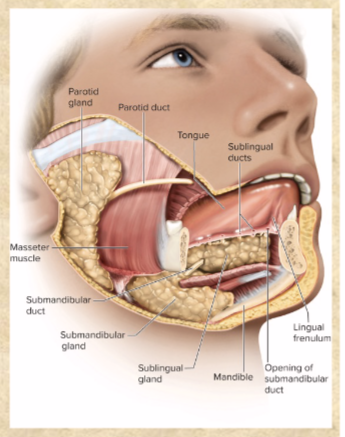
Saliva is hypotonic solution of 97-99.5% water plus…
salivary amylase: begins STARCH digestion in mouth
lingual lipase: activated by stomach acid; digests FAT after food swallowed
mucus: aids swallowing
lysozyme: kills bacteria
immunoglobulin A (IgA)
electrolytes: sodium, potassium, chloride, phosphate, bicarbonate
pH of saliva range
6.8-7
Bolus
mass of food swallowed
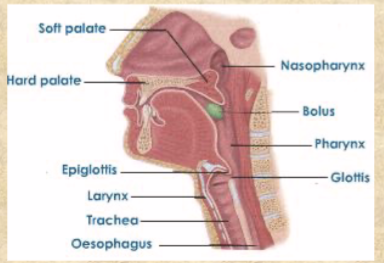
Salivation regulated by
facial and glossopharyngeal nerves to glands (parasympathetic)
Pharynx
connects oral cavity to esophagus
digestive and respiratory tracts intersect
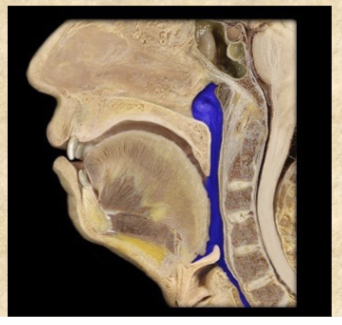
Esophagus
straight muscular tube 25-30 cm long
connects pharynx to cardiac orifice of stomach
stratified squamous epithelium
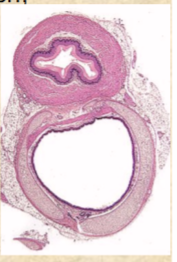
lower esophageal sphincter prevents
stomach contents from regurgitating in esophagus
protects esophagus from stomach acid
heartburn—burning sensation from acid reflux
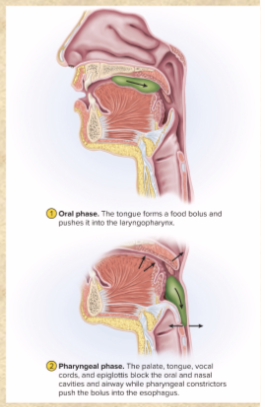
2 phases of swallowing
Buccal phase (voluntary)
Pharyngoesophageal phase (involuntary)
Buccal phase of swallowing
voluntary
TONGUE presses bolus against palate, pushes posteriorly
epiglottis tips posteriorly, bolus slides by
bolus enters laryngopharynx; stimulates tactile receptors to activate next phase
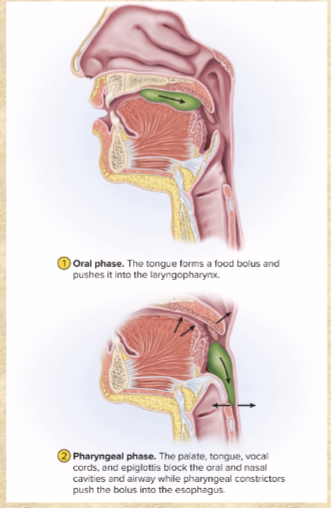
Pharyngoesophageal phase of swallowing
involuntary
prevent food/drink going back to mouth
tongue root blocks oral cavity
– soft palate rises, blocks nasopharynx
– larynx moves up to meet epiglottis,
vestibular folds close airway
– epiglottis covers airway
• bolus driven downward by constriction
of pharyngeal constrictors
• bolus enters esophagus, stimulates
peristalsis
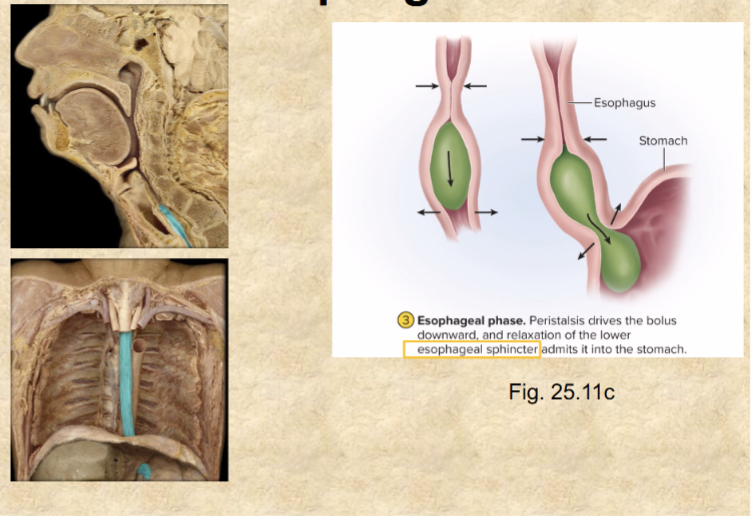
Esophageal phase of swallowing
peristalsis—wave of muscular contraction that pushes bolus ahead—involuntary
(liquid reaches stomach in 1-2 sec, bolus 4-8 sec)
at end of esophagus, lower esophageal sphincter relaxes—food enters stomach
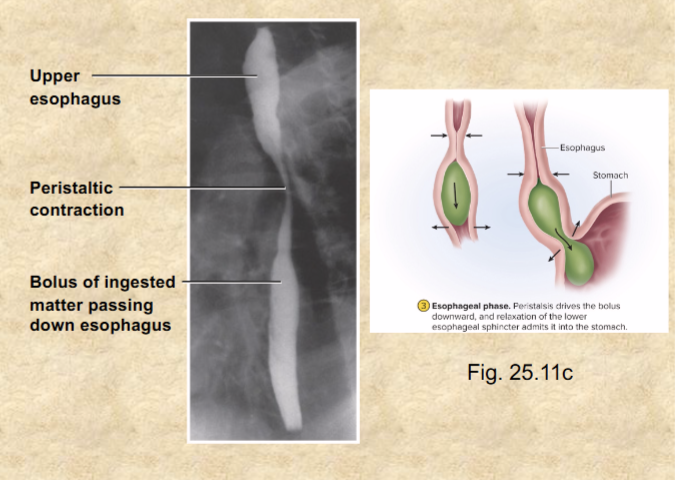
What constricts and contracts during peristalsis?
constricting of inner circle and contracting of outer longitudinal
Primary function of stomach
food storage (upper left abdominal cavity)
1-1.5 L after typical meal
4 L extremely full
chyme
soupy/pasty mixture of semi-digested food in stomach
Stomach….breaks up food particles
MECHANICALLY, liquefies food, and begins chemical digestion of PROTEIN and fat
most digestion occurs after chyme passes on to small intestine
cardiac region of stomach
small area within 3 cm of cardiac orifice
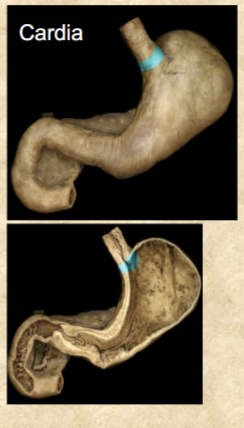
Fundic region of stomach
dome-shaped superior portion
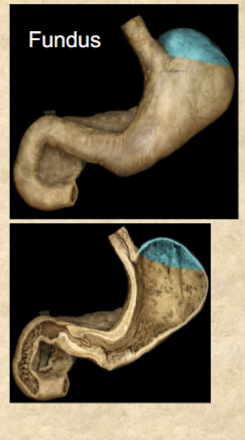
Body (corpus) of stomach
greatest part of stomach
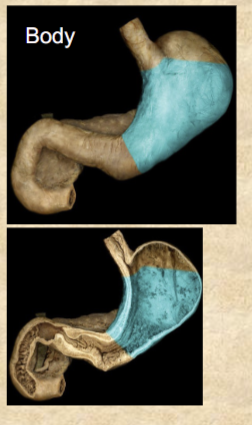
3 parts of pyloric region of stomach
pyloric region is the inferior end
pyloric canal: terminates at pylorus
pylorus: narrow passage to duodenum
pyloric sphincter: regulates passage of chyme into duodenum
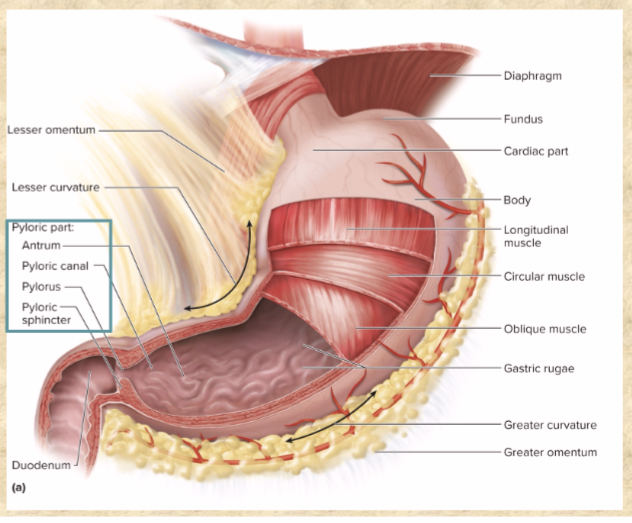
Rugae
longitudinal wrinkles inside stomach
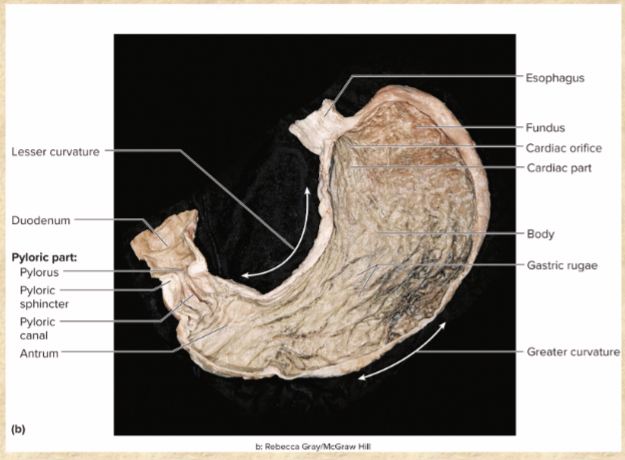
parts of stomach mucosa, submucosa, and muscularis externa
simple columnar epithelium covers mucosa
mucosa and submucosa form rugae when empty, flatten when full
muscularis externa (has 3 layers NOT 2)—outer longitudinal, middle circular, inner oblique layers
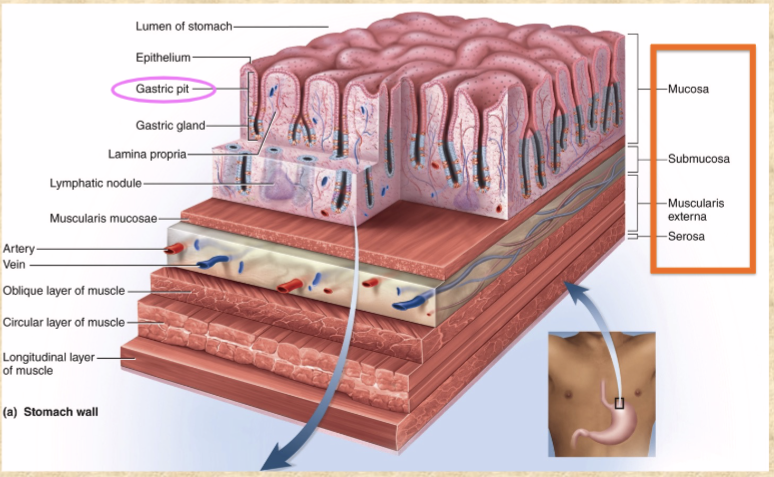
gastric pits
depressions in gastric mucosa
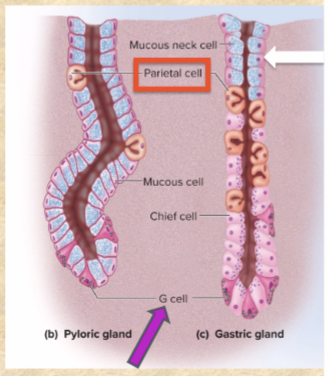
pyloric glands in pyloric region
gastric glands in rest of stomach
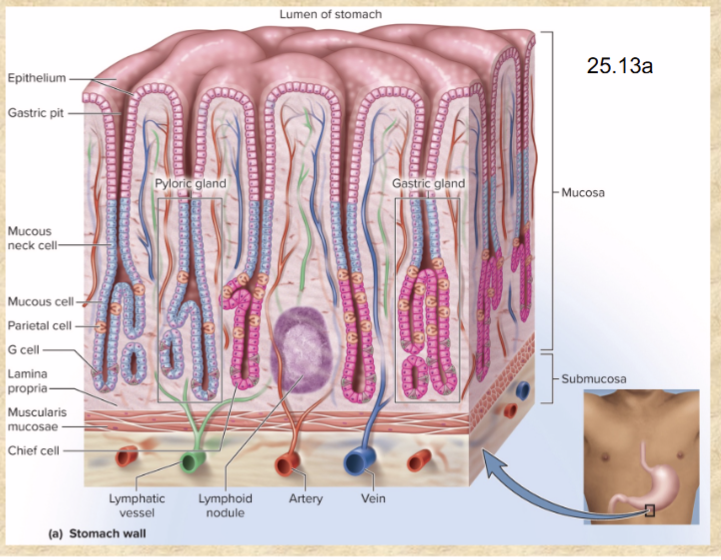
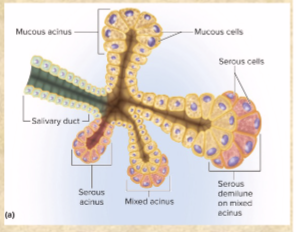
Mucous cells secrete
(blue) mucus
includes mucous neck cells
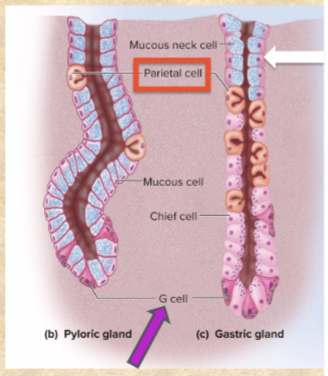
Parietal cells secrete
(orange) HYDROCHLORIC ACID (HCl), intrinsic factor, and ghrelin
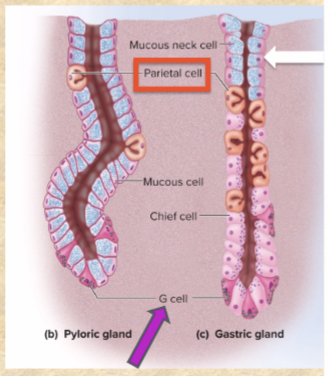
G cells secrete
(dark pink) gastrin
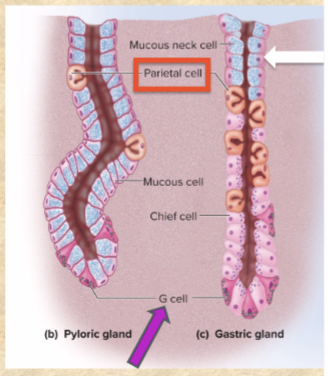
Chief cells secrete
(most numerous, light pink) gastric lipase and pepsinogen (pepsin—DIGESTS PROTEIN)
ONLY IN GASTRIC GLANDS
Gastric secretions
gastric juice— 2-3 L/day produced by gastric glands (water, HCl, and pepsin)
gastric lipase—produced by chief cells
gastric lipase and lingual lipase—minor role in fat digestion but remainder digested in small intestine
Cephalic phase
brain—vagus nerve—enteric NS—lots of secretion
food is coming GET READY
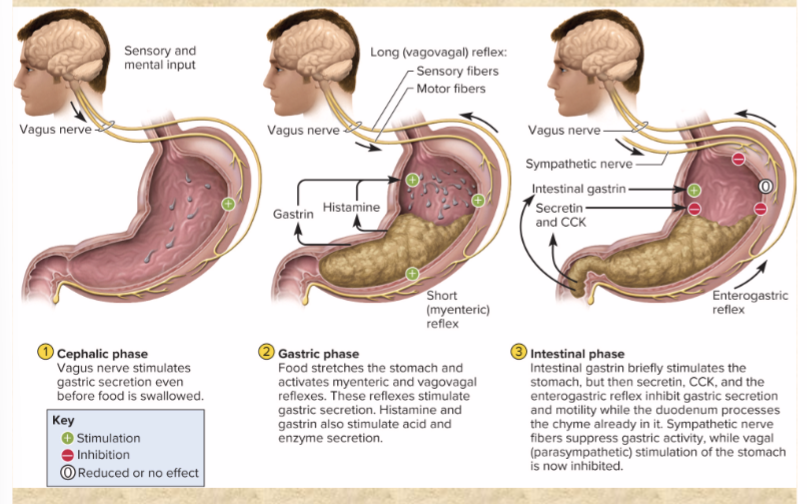
Gastric phase
food stretches stomach and stimulates secretion of ACh, histamine, gastrin prompts acid, pepsin, and mucus
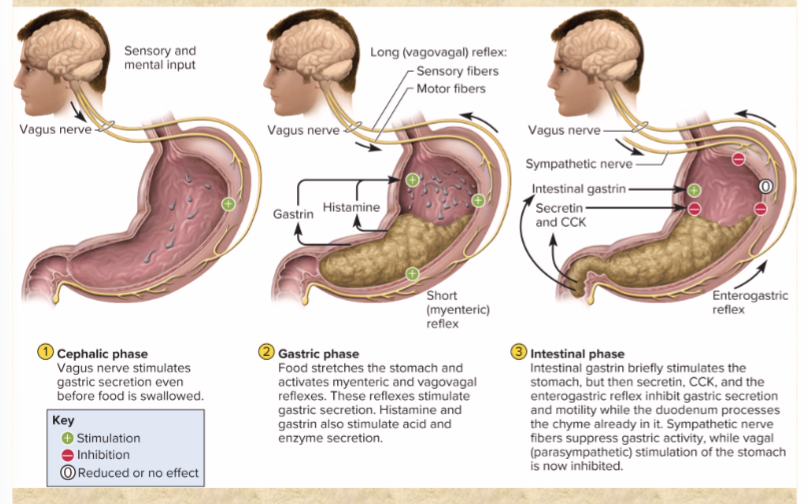
Intestinal phase
enterogastric reflex
secretin and CCK from duodenum suppress gastric activity
vomiting
forceful ejection of stomach contents (chyme) from mouth
emetic center in medulla oblongata integrates multiple muscle actions
Projectile vomiting vs chronic vomiting
no prior nausea or retching vs causes dangerous fluid, electrolyte, and acid-base imbalances
Most digestion and nearly all absorption occur in
small intestine
gastric enzymes digest what?
mainly protein (and a little fat)
PROTEIN DIGESTION BEGINS IN STOMACH (PEPSINOGEN)
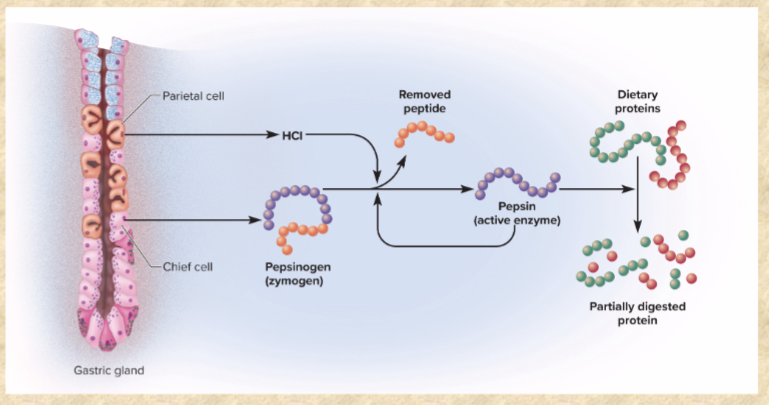
What are the 3 ways the stomach is protected?
mucous coat (thick, alkaline mucus resists action of acid/enzymes), tight junctions (between epithelial cells, prevent gastric juice from seeping through to underlying CT), epithelial cell replacement (stomach epithelial cells live only 3-6 days)
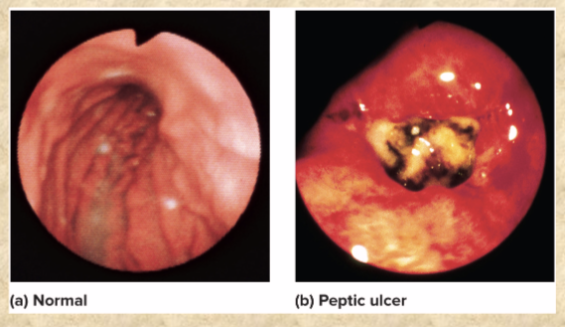
breakdown of the 3 ways stomach is protected can result in inflammation or…
peptic ulcer (mucous coat, tight junctions, epithelial cell replacement)
1.) What are two locations where mechanical digestion takes place? Compare and contrast mechanical and chemical digestion.
Mouth and stomach. Mechanical digestion involves physical breakdown of food into smaller pieces while chemical digestion involves molecular breakdown of food molecules.