CMS Final: Derm E2
1/183
Earn XP
Description and Tags
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
184 Terms
which type of urticaria is IgE dependent?
acute (<6 weeks)
which type of urticaria results from stroking/scratching skin?
dermographism
which condition is a malar rash/butterfly rash associated with?
cutaneous lupus erythematosus
how long does a butterfly rash last and what makes it worse?
lasts hours-weeks;
exacerbated by sun exposure
does a butterfly rash include the nasolabial folds?
no they are spared
what vascular manifestations are seen in cutaneous lupus erythematosus?
periungal erythema
livedo reticularis
raynauds
vasculitis
what sign/sx is seen in ACUTE cutaneous lupus?
butterfly rash
what sign/sx is seen in SUBACUTE cutaneous lupus?
small, erythematous, slightly scaly papules that evolve into psoriasiform plaques or annular plaques→seen on shoulders, forearms, neck and upper torso
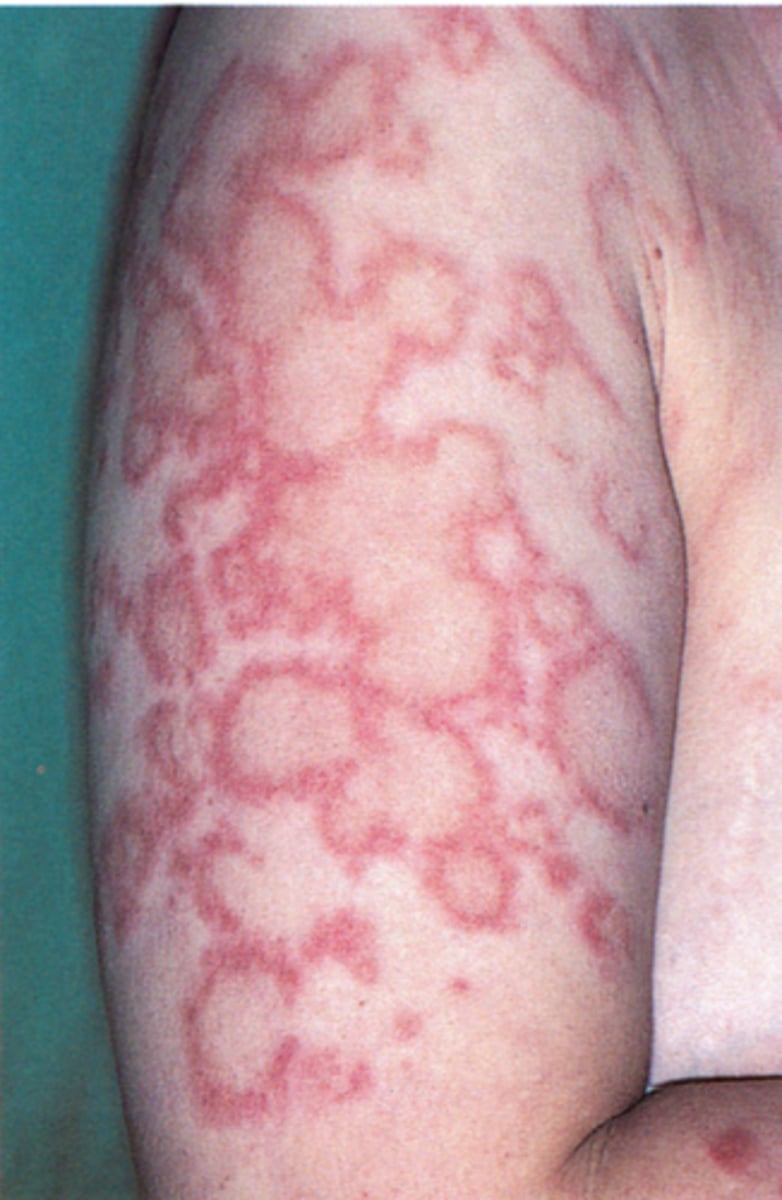
what is the most common type of chronic cutaneous lupus?
discoid
what skin manifestation is seen in chronic cutaneous lupus?
discrete, erythematous, indurated plaques covered by a well-formed adherent scale that extends into dilated hair follicles → healed plaques leave depressed central scars, atrophy, telangiectasia, and hyper/hypopigmentation
which form of lupus presents as painful indurated plaques or firm subcutaneous nodules?
lupus panniculitis (profundus)
→ upon resolution they are left with subcutaneous atrophy and scarring
what is the first line of treatment for cutaneous lupus?
sunscreen + topical/intralesional/oral corticosteroids
what treatment is used for refractory lupus?
antimalarials (-quin)
what is a hallmark of scleroderma?
widespread vascular dysfunction and progressive fibrosis of skin and internal organs
what are some clinical features of scleroderma?
edema, skin thickening/hardening, Raynaud's, painful ulcerations at DIP and PIP, sclerodactyly
what is the first line of treatment for scleroderma?
methotrexate
scleroderma, lupus, sjrogans, dermatomyositis, polymyocitis, hypothyroidism
rule out raynauds?? idk what she said about these dx in class
what is a big risk factor for raynaud's?
smoking
what are some scleroderma associated syndromes?
CREST!
C = calcinosis cutis
R = raynaud's
E = esophageal dysfunction
S = scerlodactyly
T = telangiectasia
which subtype of raynaud's is due to underlying disease?
secondary
what is defined as an exaggerated vascular response to cold temperature or emotional distress?
Raynaud's phenomenon
what is the first line treatment for Raynaud's?
CCB (amlodipine or nifedipine)
2nd line = PDE5i
what is the first line of treament for dermatomyositis?
hydroxychloroquine
2nd line = add methotrexate
for pruritis → topical steroids/calcineurin inhibitors
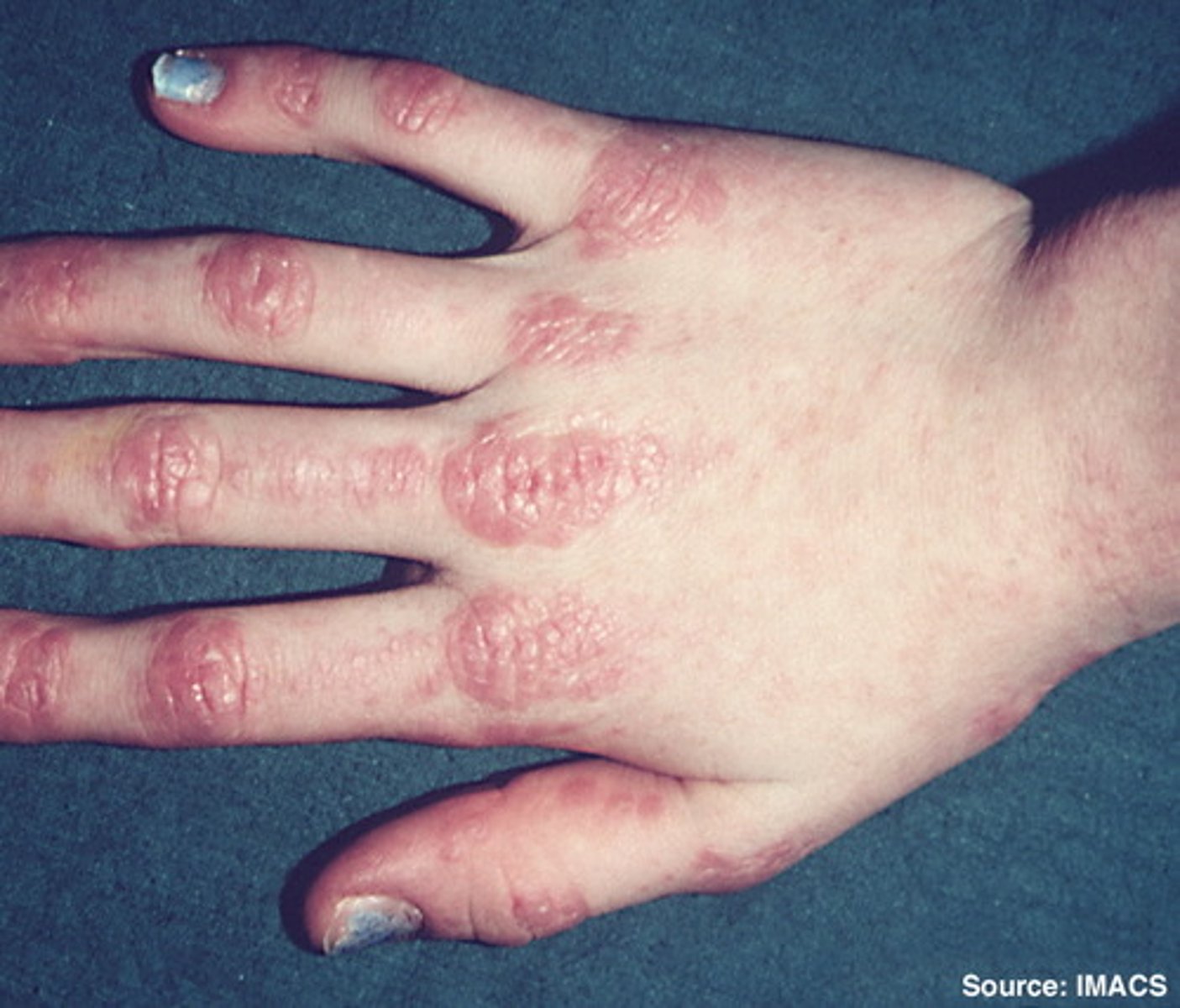
how does dermatomyositis commonly present?
progressive, symmetric, proximal muscle weakness and cutaneous findings
what cutaneous findings are associated with dermatomyositis?
Gottron's papules (fingers), Heliotrope eruption (eyelids), Shawl sign (back)
How is Behcet's diagnosed?
Recurrent Oral Ulceraction + 2 of following:
-recurrent apthae-like genital ulcers
-uveitis
-skin lesions
-+pathergy test
what is the first line of treatment for Behcet's?
topical glucocorticoids for aphthous ulcers
systemic → prednisone
what severe complication is associated with Behcet's?
ocular disease → uveitis → blindness
which subtype of angioedema affects face/extremities, laryngeal edema, angioedema of bowel wall?
hereditary angioedema
what is a pathognomonic finding for IgA vaculitis?
leukocytoclastic vasculitis in postcapillary venules with IgA deposition on bx
what are risk factors for IgA vaculitis?
age 4-7 &
S. pyogenes infection
which condition is defined as "systemic necrotizing vasculitis that typically affects medium-sized muscular arteries with additional involvement of small arteries"?
polyarteritis nodosa
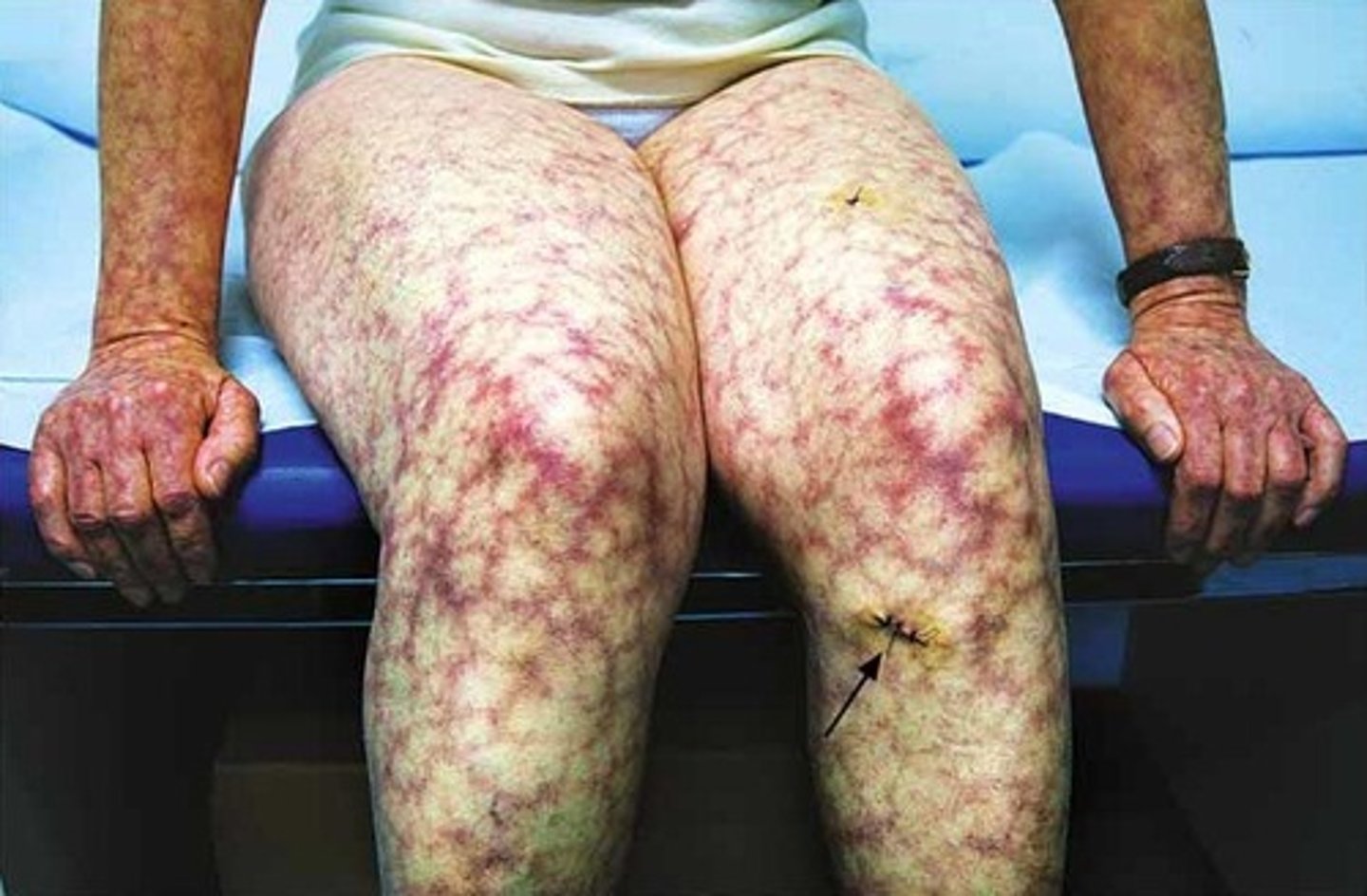
what is a hallmark feature of neurofibromatosis?
cafe au lait spots
which type of NF is most associated with complication of acoustic neuroma?
NF2 → associated with Schwannomatosis
which condition is associated with cutaneous and mucosal erythema and edema with subsequent desquamation?
Kawasaki disease
does Kawasaki disease include the palms and soles?
yes → erythema
how is Kawasaki disease diagnosed?
presence of fever last 5+ days with no explanation PLUS 4/5 of the following:
1. bilateral bulbar conjunctival injection
2. oral mucous membrane changes (strawb tongue)
3. peripheral extremity changes
4. polymorphous rash
5. cervical LAD
what is the treatment for Kawasaki disease?
IVIG and aspirin
what is a complication of Kawasaki disease?
coronary artery aneurysm (was on exam)
which subtype of sarcoidosis is associated with diffuse, violaceous, soft doughy infiltrations on the nose, cheeks or earlobes?
lupus pernio
which subtype of sarcoidosis is associated with papules and translucent yellow/red with apple jelly appearance on diascopy?
papular
what is seen on diascopy in sarcoidosis?
"apple jelly" semitranslucent yellowish/brown color
what is a hallmark of sarcoidosis?
noncaseating granulomas
what is the triad associated with granulomatosis with polyangiitis (GPA) (Wegners)?
1. necrotizing granuloma in upper resp tract and lungs
2. vasculitis involving both arteries and veins
3. glomerulitis
which condition shows necrotizing vasculitis of small arteries/veins with intra or extravascular granuloma formation on histo?
GPA
which drug is used for prevention of opportunistic infections in GPA?
bactrim
what is the treatment for induction of GPA?
cyclophosphamide or Rituximab PLUS prednisone
what is the treatment for maintenance of GPA?
methotrexate or Rituximab or azathioprine
which autoimmune condition is characterized by chronic inflammatory subepidermal blistering?
bullous pemphigoid
what is seen in the prodromal phase of bullous pemphigoid?
weeks/months of pruritic eczematous papular or urticaria-like skin lesions
what is the initial therapy for bullous pemphigoid?
high potency topical steroid (clobetasol) OR oral glucocorticoids OR doxy
which diagnosis should be suspected in a patient >60 y/o with blistering skin disease, desquamative gingivitis/mucositis, and unexplained pruritic urticarial plaques?
bullous pemphigoid
which disease has a prodrome of fever, fatigue, malaise, arthralgias that may precede nodules 1-3 weeks?
erythema nodosum
Where is erythema nodosum most commonly found?
shins
where is a neurofibroma most commonly found?
trunk
what is the diagnostic criteria for neurofibromatosis?
2 of the following:
- > 6 cafe au lait lesions >5mm prepuberty or 15> mm postpuberty
- multiple freckles in axillary+inguinal areas
- >2 neurofibromas or one plexiform neurofibroma
- bone legions
- bilateral optic nerve glioma
- >2 Lisch nodules
- 1st degree relative with NF1
what drug is used to treat pruritis of neurofibromas?
gabapentin
which inherited disorder is characterized by benign hamartomas of the brain, eyes, heart, lungs, liver, kidneys, and skin?
tuberous sclerosis
which blood test should always be checked in patients with xanthomas?
lipid panel
what is the most common xanthoma?
Xanthelasma
what is the cause of scurvy?
Vitamin C deficiency
what are common clinical features of scurvy?
petechiae, extensive ecchymoses, bleeding gums, loss of teeth, hemorrhage into long bones and intracerebral hemorrhage (Severe)
what disease of zinc deficiency is seen in infants?
Acrodermatitis Enteropathica → d/t genetic disorder of zinc absorption
what is the triad of Acrodermatitis Enteropathica?
1. erythematous, dry, scaly plaques of face/anogenital area
2. alopecia
3. diarrhea
which disease is caused by Niacin deficiency?
Pellagra
what is a chemically induced skin irritation that is exacerbated by direct sunlight?
phototoxicity
what is an abnormal cutaneous response that occurs after exposure to UV or visible light?
photosensitivity
how long does UVA damage take to develop?
4-16 hours, fades in 48-72 hrs
how long does UVB damage take to develop?
6-24 hours, fades in 72-120 hrs (more harmful)
what is the criteria to refer to burn center?
- suspected inhalation injury
- moderate-severe burns
- circumferential partial or full thickness burns
- burns to hands, feet, face, and perineum
- chemical burns
- carbon monoxide poisoning
- inadequate family support of abuse
- severe co-morbidities (COPD, CAD, DM, renal insuff)
what is a delayed-type hypersensitivity reaction to an allergen whose antigenicity changes after exposure to UV?
photoallergic
what is chronic photodamage also known as?
Dermatoheliosis (photoaging)
what is characterized by wrinkled, leathery, premature aged, cigarette-paper skin?
dermatoheliosis
what is characterized by circumscribed flat, brown macules with uniform color in a scattered distribution?
solar lentigo
what deadly condition does solar lentigo mimic?
melanoma (solar lentigo is UNIFORM in color)
what is appears as an exaggerated sunburn secondary to phototoxic agent that has been applied/ingested?
phototoxic dermatitis
which fitzpatrick type is most affected by phototoxic dermatitis?
ALL
what is the most common idiopathic photodermatosis?
polymorphous light eruption (PMLE)
what is the cause of PMLE?
genetic susceptibility or delayed-type hypersensitivity
what is skin hardening associated with?
PMLE → treated with PUVA
what type of hypersensitivity is solar urticaria?
immediate type 1 → sunlight induced wheals
what is the etiology of porphyria cutanea tarda?
deficiency of uroporphyrinogen decarboxylase enzyme (UROD)
which disease is characterized by fragile skin, superficial erosions, chronic scarring and alopecia?
porphyria cutanea tarda (vampire disease) (liver skin condition)
which condition shows pink fluorescence under a woods lamp?
porphyria cutanea tarda (vampire disease)****
How are burns classified?
classified according to their depth
which degree of burn involves destruction of the epidermis and varying depths of dermis?
2nd → partial thickness
which degree of burn involves only the epidermis?
1st → superficial
which degree of burn involves destruction of epidermis, dermis, and subq tissue?
3rd → full thickness
which degree of burn involves subq tissue, muscle, fascia, and bone?
4th → full thickness and can involve muscle and/or bone
which degree of burns can destroy nerve endings?
3rd and 4th
what is the Lund-Browder Chart?
A detailed version of the rule of nines chart that takes into consideration the changes in body surface area brought on by growth. → most accurate
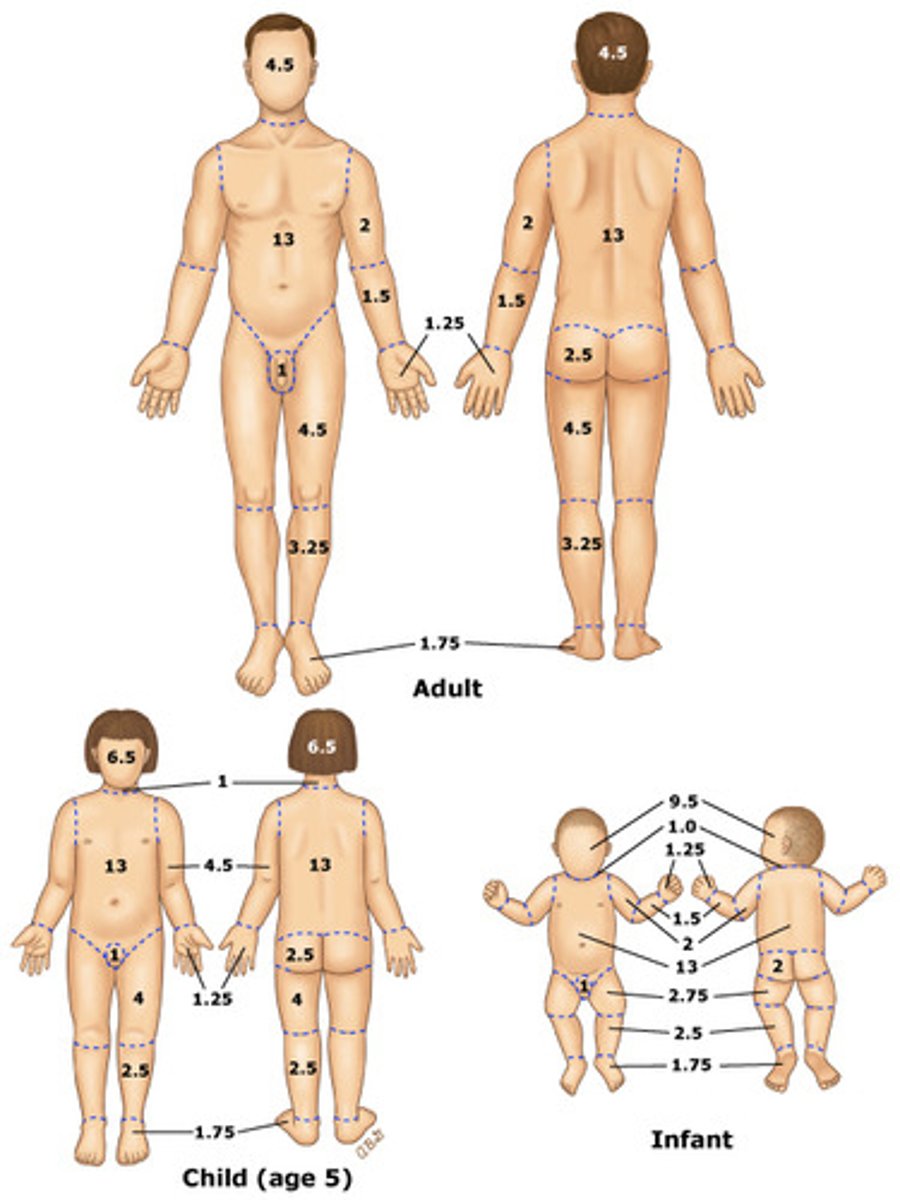
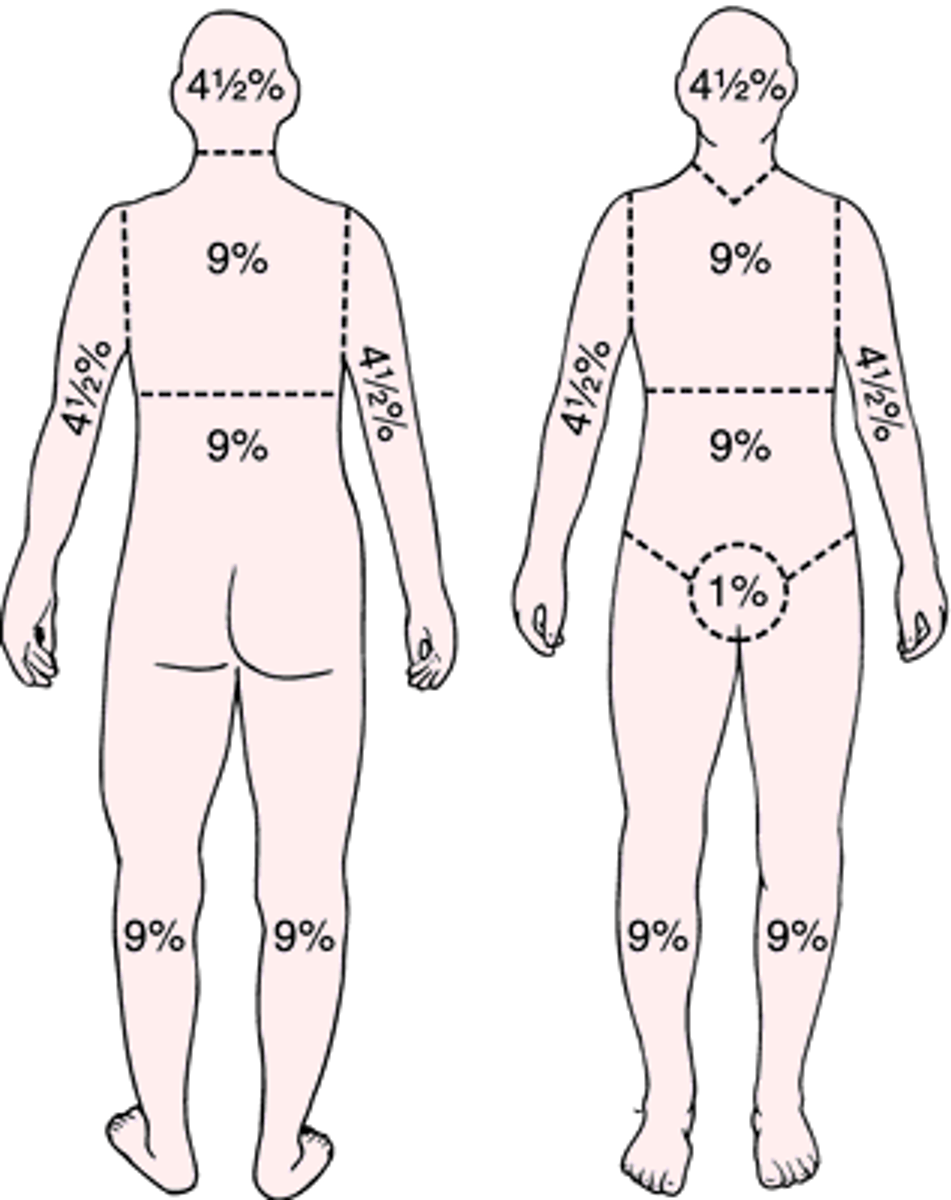
What is the rule of nines used for?
divides the body into 11 sections each accounting for 9%; mainly used to determine the amount of fluids lost in a burn → fastest
what is the treatment for superficial burns?
topical mupirocin or bacitracin
what is the treatment for partial thickness burns?
silvadene
which type of burn appears waxy, white, and leathery gray?
3rd degree
what burn injuries are most common in young children?
scald injuries → evaluate for child abuse
what is the leading cause of death with burns?
systemic infection
Burn Center Referral Criteria
on exam!

which skin condition starts with a "Herald patch"?
pityriasis Rosea → single round or oval, sharply demarcated lesion on chest, neck or back
which condition is characterized by pink/hyperpigmented, scaly, oval, papulosquamous lesions?
pityriasis rosea