Cardiovascular System
1/76
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
77 Terms
What is haemotology?
Haematology is the science of blood, blood forming tissues and disorders of the blood
What is the average volume of blood?
Male = 5-6 litres
Female = 4-5 litres
(Plasma volume increases during pregnancy)
What is the temperature of blood?
37 degrees Celsius
How is blood transported
Connective tissue
What is the pH of blood?
pH - slightly alkaline
7.35-7.45
How is blood made to be protective?
Clotting protects against excessive blood loss
Phagocytic white blood cells and antibodies protect against infection and disease
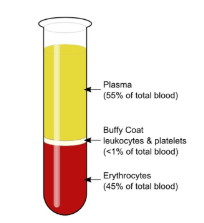
What are the constituents of blood?
Plasma
White blood cells (leucocytes)
Platelets (thrombocytes)
Red blood cells (erythrocytes)
Describe RBC?
Small
Biconcave
No nucleus (mature RBCs)
Flexible
Life cycle = 120 days
Damaged erythrocytes are removed from the circulation and destroyed by phagocytic macrophages in the liver & spleen
Main function – transport of gases
Describe haemoglobin?
Oxygen binds to haem group = Oxyhaemoglobin
Carbon dioxide binds to globin = Carbaminohaemoglobin
What is a full blood count?
Full Blood Count (FBC) Commonly ordered blood test that analyses the number of red blood cells, white blood cells and platelets in a sample.
For example, to investigate anaemia.
What is erythropoiesis?
The process of erythrocyte production
How does erythropoiesis work?
Erythropoietin (EPO) – hormone that controls erythrocyte production
↓ O2 in circulation is detected by kidneys, causing EPO secretion
EPO can be used to treat anaemia caused by chronic kidney disease and cancer treatment
Describe WBC?
Largest blood cells, contain nucleus
All leucocytes can migrate out of blood vessels into the surrounding tissues
Main function is the defence against infectious disease and invasion
Phagocytosis
Describe Platelets?
Approx 150,000 - 400,000 platelets per μL of blood
Fragments of cells (megakaryocytes) from the red bone marrow
2-4μm in diameter
no nucleus
Function - ‘clotting’ or homeostasis - sequence of events initiated to stop bleeding
What are the stages of platelet formation?
vascular spasm, platelet plug formation, coagulation
Describe blood plasma?
Pale straw colour
Approx. 91.5% water
Approx. 8.5% solutes
solutes include proteins (albumins, globulins, fibronogen), nutrients, vitamins, hormones, respitory gases, electrolytes, and waste products
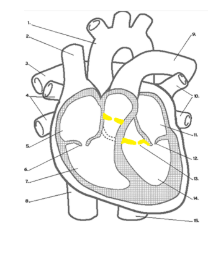
Describe the heart structure and surface landmarks?
Cone shape
Mediastinum
Anatomical Relations:
Superior vena cave
Inferior vena cava
Ascending aorta
Descending (thoracic) aorta
What is the pericardium?
Pericardium - 2 layers, fibrous and serous (double layer - parietal and visceral), pericardial space with small volume of pericardial fluid
What are two pathologies affecting the pericardium?
Pericarditatis → inflammation of the pericardium, painful
Pericardial effusion → excess fluid in the pericardial space
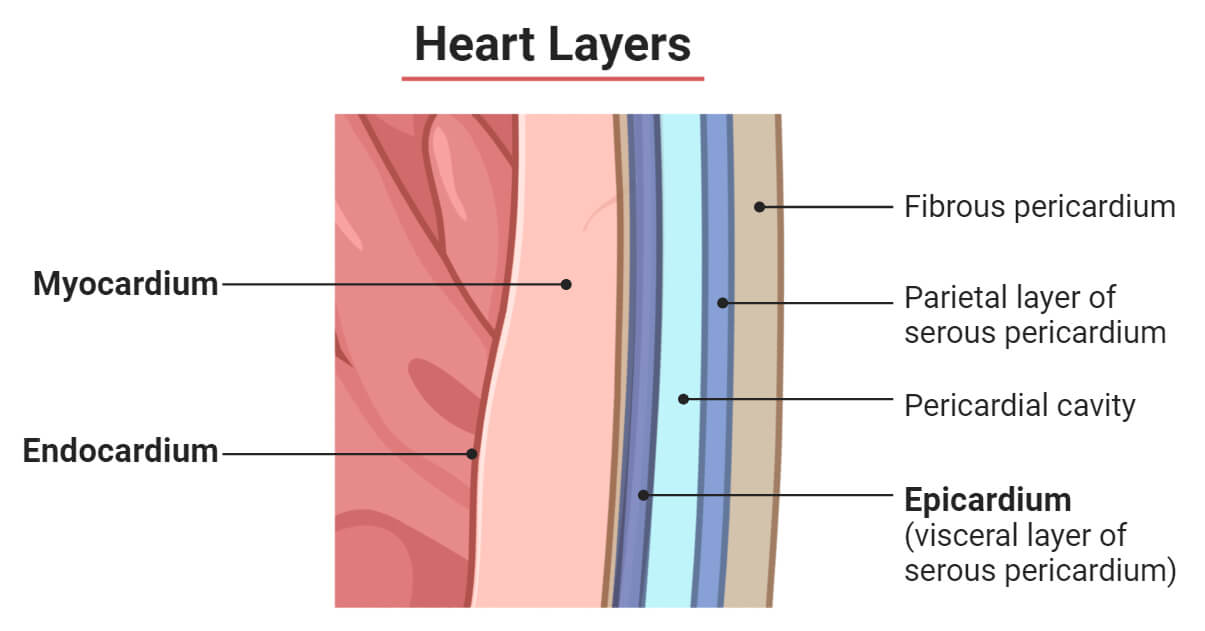
What are the layers of the heart from outermost layer to innermost layer?
Epicardium - inner layer of the serous pericardium
Myocardium - cardiac muscle tissue, thickest layer, rich blood supply
Endocardium - Smooth layer of endothelial cells, lines chambers and valves
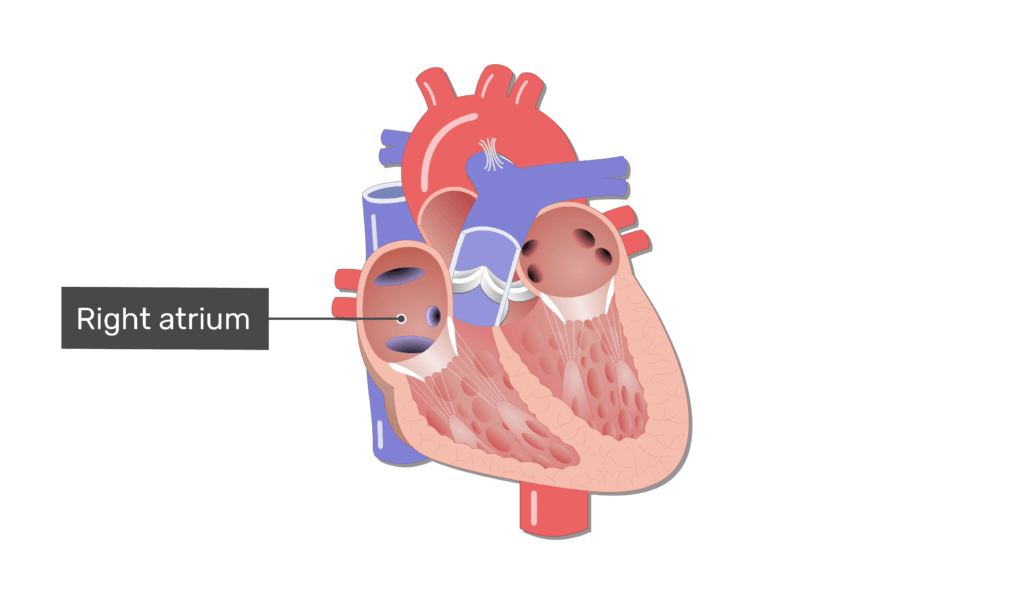
Describe the right atrium?
Receives blood from:
Superior vena cava
Inferior vena cava
Coronary sinus
Has:
Separated by the interatrial septum
Separated from the right ventricle by the tricuspid (right atrioventricular) valve
Right auricale slightly increases the capacity of the right atrium
Fossa ovalis - remanant of foramen volae (between left and right atria), which closes after birth
Foramen ovale is present in the fetus - blood bypasses fetal lungs
Describe the blood flow of the right atrium?
Superior vena cava received deoxygenated blood from the head + neck)
Inferior vena cava receives deoxygenated blood from the body
Coronary sinus → deoxygenated blood from the coronary circulation
Describe the right ventricle?
Separated from the left ventricle by the interventricular septum
Separated from the pulmonary trunk by the pulmonary (semi lunar) valve
Pulmonary trunk arises from the right ventricle, dividing into left and right pulmonary arteries and takes deoxygenated blood to the lungs
Chrodae tendineae - attached to the cusps of the tricuspid valve
has papillary muscles
Describe the left atrium?
Receives deoxygenated blood from the pulmonary veins
Left auricle
Biscuspid valve (or Mitral valve)
Describe the blood pathway in the left atrium?
Left atrium receives blood from the pulmonary veins that is oxygenated from the lungs
This is separated from the left ventricle by the bicuspid valve (mitral valve)
Left auricle - slightly increases capacity of left atrium
Describe the left ventricle?
Thick muscular wall - thicker than the right ventricle, because the left ventricle has to pump blood further (and at higher pressure) than the right ventricle
Separated from the aorta by the aortic (semilunar) valve
Ascending aorta arises from the left ventricle, taking oxygenated blood to the body
Has papillary muscles and chordae tendineae
Separated from the right ventricle by the interventricular septum
Describe the heart valves?
Open and close according to pressure changes as the heart contracts (systole) and relaxes (diastole)
Ensures one way flow of blood through the heart
prevents backflow of blood
Describe the 2 atrioventricular valves?
Between the atrium and ventricle
Tricuspid (or Right Atrioventricular)
2 cusps, or leaflets
Mitral (Bicuspid) (or Left Atrioventricular)
2 cusps, or leaflets
Open when the atria contracts
Closed when the ventricles contract
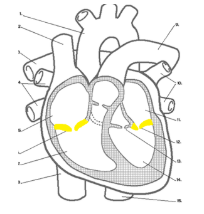
Describe the semilunar valve?
Semilunar (semi = half, lunar = moon-shaped)
Each valve is made up of 3 moon-shaped cusps
Aortic valve
Pulmonary valve
Open when the ventricles contract
Aortic valve: between the ……..ventricle and the …….. …………
Pulmonary valve: between the ………… ventricle and ………… ………….
Aortic valve: between the left ventricle and the ascending aorta
Pulmonary valve: between the right ventricle and pulmonary trunk
Describe blood pressure in the heart?
Blood pressure is the force of blood pushing against the walls of your arteries
Systolic pressure: pumps out blood
Diastolic pressure: rest between beats
Normal blood pressure is typically considered to be around 120/80 mmHg.
Blood pressure can vary throughout the day and can be influenced by factors such as stress, physical activity and diet
Describe the aorta?
Arises the from the left ventricle
Includes:
Ascending aorta
Arch of aorta
Descending (thoracic) aorta
Passes through the diaphragm
Abdominal aorta
Coeliac trunk
Superior mesenteric artery
Left and right renal arteries
Divides into left and right common iliac arteries
Describe the blood vessels?
Tunica intima (interna) → the innermost layer
Tunica media
Tunica adventitia (externa) → the outermost layer
Describe the atrial supply to the brain?
Approx. 2% of body weight
Receives approx. 15-20% of cardiac output
High oxygen and glucose requirements
Thus, requires constant blood flow
What does a decrease in cerebral flow result in?
Brief decrease in cerebral flow results in unconsciousness
1-2 minutes = impairment of neuronal function
>4 minutes = permanent injury
What is cardiac output?
The amount of blood ejected per minute by the left ventricle into the aorta or by the right ventricle into the pulmonary trunk
What does the venous drainage of the GI tract mean in terms of metastasis?
Many GI tract malignancies are known to metastasis to the liver
Malignant cells from most of the GI tract are transported to the hepatic portal circulation and deposited in the liver
What are the 3 forms of circulation?
Pulmonary
Systematic
Coronary
What is pulmonary circulation?
the circulation of blood through the lungs
the right side of the heart is the pump for pulmonary circulation
Describe the pathway for pulmonary circulation
Right atrium receives deoxygenated blood from the systemic veins (via the inferior vena cava and superior vena cava)
Right ventricle ejects deoxygenated blood into the pulmonary trunk which divided into left and right pulmonary arteries
Blood is oxygenated in the lungs
Oxygenated blood is delivered to the left atrium, by the pulmonary veins
Outline the pathway for pulmonary circulation?
Right Atrium → Right Ventricle → Pulmonary Artery → {Blood Oxygenated} → Pulmonary Veins
What is systematic circulation?
The circulation of blood throughout the body except the air sacs of the lungs
The left side of the heart is the pump for systematic circulation
Describe the pathway for systematic circulation?
Left atrium receives oxygenated blood from pulmonary veins
Left ventricle pumps oxygenated blood (via the aorta) to all of the body’s tissue
Deoxygenated blood is delivered to the right atrium by the systematic veins (inferior and superior vena cava)
Outline the pathway for systematic circulation?
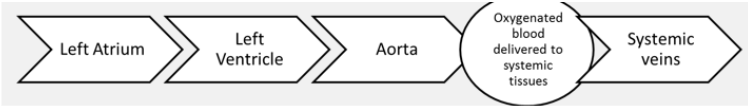
left atrium → left ventricle → aorta → (deoxygenated blood delivered to the systematic tissues) → systematic veins

Describe the coronary vessels?
provides blood flow to the myocardium
main arteries are the left and right coronary arteries
main veins are the cardiac veins and coronary sinus
Outline the coronary circulation?
Ascending Aorta → coronary arteries → capillaries → coronary veins → coronary sinus → right atrium
How are the coronary vessels positioned of the heart?
Coronary arteries branch from the ascending aorta and encircle the heart
During diastole (relaxation), oxygenated blood is propelled into the coronary arteries
Describe the conduction system?
Specialised muscle tissues generate and distribute impulses which cause the cardiac muscle fibres to contract
Components:
Sinoatrial (SA) node
Atrioventricular (AV) node
Atrioventricular bundle (bundle of His)
Bundle branch
Purkinje Fibres
What are sinoatrial nodes?
Specialised cells within the right atrium
Initiates cardiac cycle – the ‘pacemaker’
Rate and strength effected by autonomic nervous system & blood borne chemicals e.g. epinephrine
Cause atria to contract
What are atrioventricular nodes?
Found within interatrial septum
Action potentials conducted along atrial muscle fibres to the AV node
Initiates the impulse in the atrioventricular bundle bundle
What is the atrioventricular bundle/ bundle of his?
Specialised fibres running down the interventricular septum
Transmit impulse through ventricular system
Divide into left and right branches
Extend through interventricular septum towards the apex of the heart
What are Purkyne fibres?
Terminal fibres
Conduct the action potential from the apex up through the ventricular myocardium
Ventricles contract
What is an ECG?
Converts the heart’s lectrical activity → waveform
Used for diagnosis (12 lead ECG) & monitoring (3 or 5 lead ECG)
Can detect numerous abnormalities
Outline the electrical activity of the heart?
Impulse passes Purkinje Fibres
Impulse passes bundle of branches
Impulse passes bundle bundle of His
Impulse arrives in the AV node
The sinoatrial node depolarises
Describe the cardiac cycle?
1 cardiac cycle = 1 heart beat
Consists of systole (contraction) and diastole (relaxation) of both atria and ventricles
The phases are atrial systole, ventricular systole and relaxation period
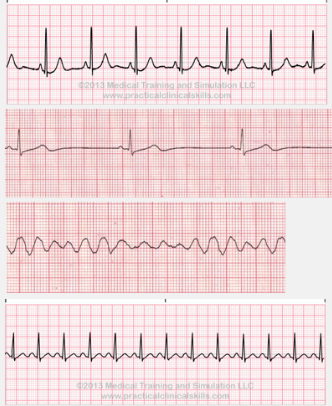

normal sinus rhythm
bradycardia
ventricular fibrillation
tachycardia
Name the different types of heart diseases?
valve disease
aneurysm
cardiac arrhythmia
pericarditis
heart failure
coronary artery disease
cardiomyopathy
Describe DVT?
Most commonly of the lower limb
Symptoms include unilateral swelling of the affected limb, pain, erythema
What are risk factors for DVT?
POOSH SIC
Pregnancy
Obesity
Oral Contraceptives
Smoking
Hormone replacement therapy
Surgery
Immoblity
Cancer
What is imaging for DVT?
Compression ultrasound
Veins containing thrombus do not compress
What are the pulmonary embolism risk factors?
DVT
Immobility including prolonged bed rest, long distance travel
Recent surgery
Pregnancy and the puerperium
Smoking
Oral contraceptives
Hormone Replacement Therapy (HRT)
Obesity
Increasing age
Cancer
What is Pulmonary Embolism?
Known collectively with DVT as Venous Thromboembolism (VTE)
3rd most common vascular disease, after Myocardial Infarction and stroke
Symptoms of Pulmonary Embolism?
Pleuritic chest pain, usually
worse on inspiration
Dyspnoea
Low oxygen saturations
Syncope
Haemoptysis
DVT
Tests for Pulmonary Embolism?
Arterial Blood Gas (ABG)
D-Dimer blood test
Wells score
Treatments of DVT and/or PE
Anticoagulation drugs
IVC Filters
Mechanical thrombectomy
Describe IVC filters?
Small metal devices placed in the inferior vena cava to trap blood clots and prevent them from travelling to the lungs, helping prevent pulmonary embolism.
What is atherosclerosis?
Chronic disease of the arteries characterised by a build up of fat, cholesterol and calcium
Major cause of coronary artery disease and stroke
Endothelial damage
Artery is narrowed
What are the risk factors for atherosclerosis?
SSHHEED POF → CAD, Atherosclerosis
Sedentary Lifestyle
Smoking
Hypercholesterolemia
Hypertension
Excess alcohol consumption
Ethnicity
Diabetes
Poor diet
Obesity
Family history
Describe Abnormal Aortic Aneurysm?
Abnormal dilation of the aorta
May be asymptomatic, may present with referred back or
abdomen pain, mass in the abdomen which may pulsate
Risk factors of Abnormal Aortic Aneurysm?
(MAATHH)
Men
Atherosclerosis
Age
Tobacco
Hypercholesterolemia
Hypertension
Outline the public health screening for AAA?
65 year old males in England
Aim to reduce AAA related mortality in men aged 65-74
Early detection, monitoring and treatment is crucial in order to reduce mortality rates from ruptured AAA
What is coronary artery disease?
Atherosclerosis of the coronary arteries
What are the risk factors of Coronary Artery Disease (CAD)?
SSHHEED POF → CAD
Sedentary Lifestyle
Smoking
Hypercholesterolemia
Hypertension
Excess alcohol consumption
Ethnicity
Diabetes
Poor diet
Obesity
Family history
What are the signs and symptoms of CAD?
Chest pain (angina pectoris)
Pain that radiates to the arm, neck, jaw, back or stomach
May be described as heaviness or tightness, or indigestion
Dizziness
Nausea
Dyspnoea
Fatigue (in chronic CAD)
What imaging is used for CAD?
Cardiac CT
Cardiac MRI
Myocardial Perfusion Imaging (MPI)
Coronary Angiography
(Echocardiography)
PET/CT
What is pericardial effusion?
Abnormal accumulation of fluid between pericardial layers
What are some patholgies of the heart?
Stroke and Transient Ischaemic Attack (TIA)
Peripheral vascular disease
Heart failure