Chapter 18: Practical Applications of immunology
1/43
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
44 Terms
vaccine
contains proteins from the organism to be targeted
nucleic acids encoding those proteins (DNA or mRNA vaccines)
disabled forms of the organism itself = body’s immune defenses against pathogen
types of vaccines
attenuated vaccines
inactivated vaccines
subunit vaccines
recombinant
toxoids
VLP
polysaccharide vaccines
conjugated vaccine
DNA
mRNA
essential elements of diagnostic tests
sensitivity
specificity
sensitivity
probability that test is reactive if the specimen is a true positive (catch disease when its there)
specificity
probability that test will NOT be reactive if a specimen is a true negative (rule out disease when its not there)
precipitation reactions
involve the reaction of soluble antigens with IgG or IgM antibodies
occurs in 2 stages / steps…
antigens and antibodies rapidly form small antigen-antibody complexes (tiny clumps)
antigen-antibody complexes form larger interlocking molecular aggregates (molecules stick together) called lattices that precipitate from the solution
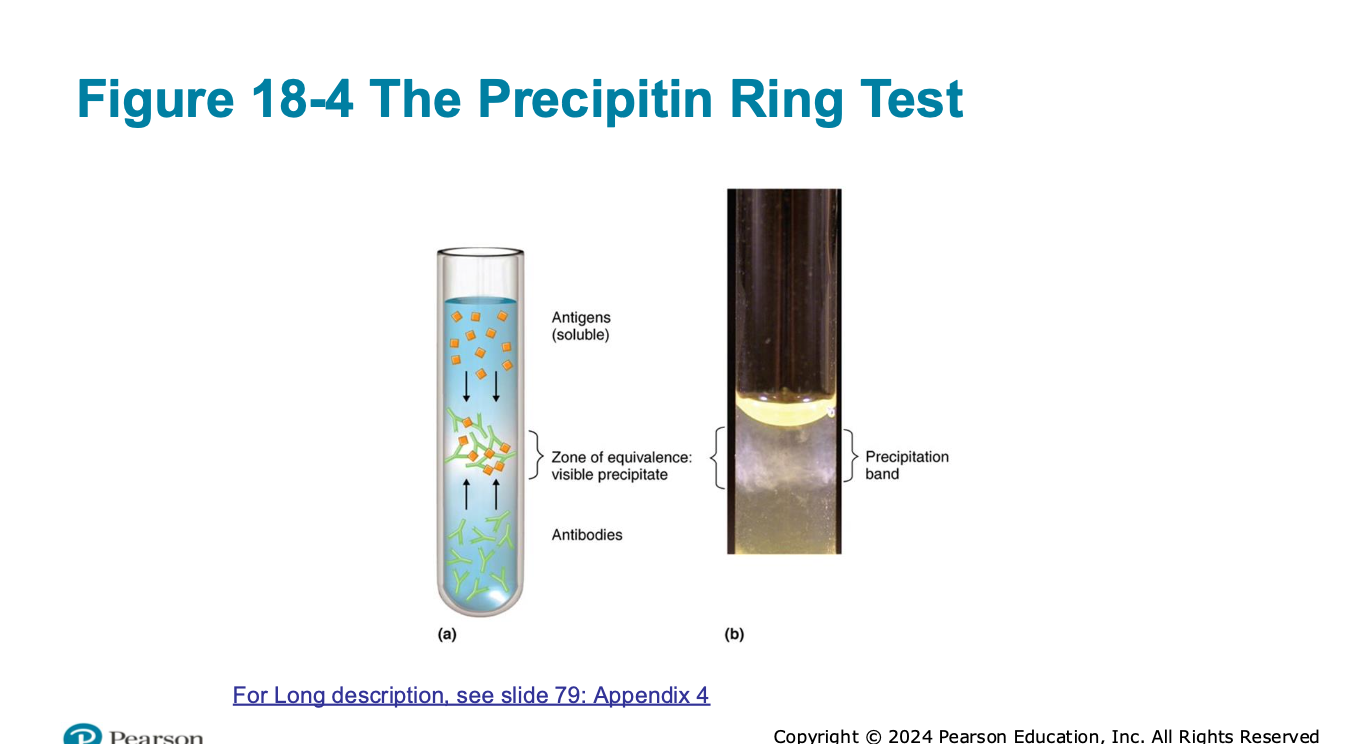
forms the zone of equivalence (precipitin ring test)
involves soluble antigens
zone of equivalence (precipitin ring test)
cloudy line of precipitation will appear in the area in which the optimal ratio has been reached
agglutination reactions
involves either particulate antigens (particles such as cells that carry antigenic molecules) or soluble antigens adhering to particles
agglutination antibodies bind to antigens on particles and cross link them into visible clumps
(particulate antigens + antibodies = visible clumps)
IgM = most efficient antibody, IgG = less efficient
direct and indirect tests
particulate antigens
antigens that are already on cells
direct agglutination test
detect antibodies against naturally occurring cell bound antigens, detect antibodies against relatively large cellular antigens on RBC, bacteria, fungi
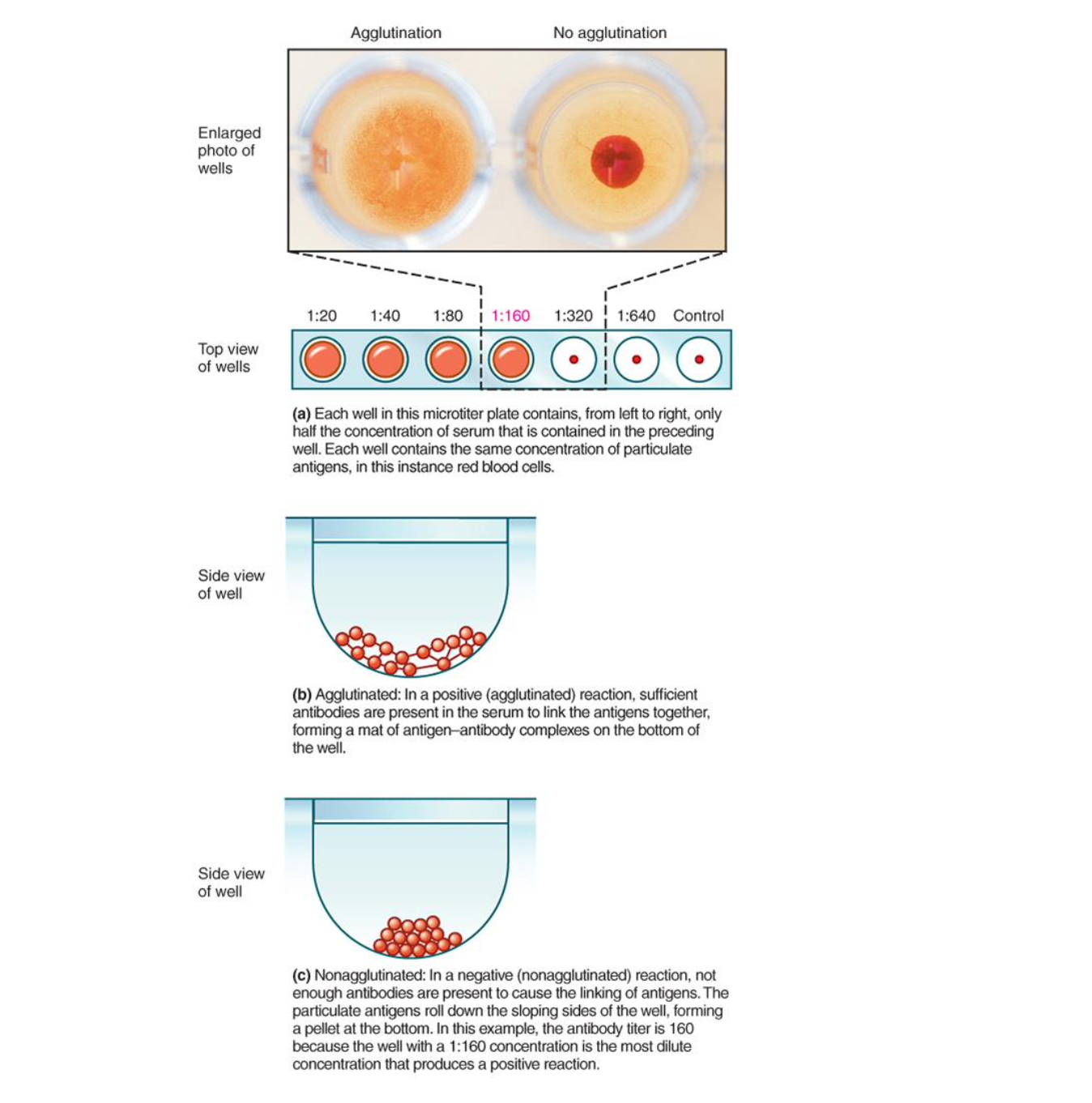
direct agglutination process
add antigen (bacteria) to wells
add diluted patient serum (contains antibodies)
look for clumping
titer - highest dilution of serum that still causes agglutination
indirect (passive) test
used when antigens are soluble (not naturally on cells); the antibody reacts with the attached antigen or in reverse by using particles coated with antibodies to detect the antigens against which they are specific for
(use coated particles to detect soluble antigens or antibodies)
two formats
detect antibodies (use antigens)
detect antigens (use antibodies)
indirect agglutination process
attach antigen or antibody to particles like latex beads
add patient sample
if target is present = beads clump

neutralization reactions
is an antigen-antibody reaction in which antibodies block the harmful effects of a bacterial exotoxin or block viruses from infecting cells
uses antitoxin
antitoxin
antibodies to toxin, binds to the exotoxin and blocks its toxic effect before damaging cell
hemagglutination
specific type of agglutination reaction involving RBCs (clumping of RBCs caused by antibodies binding to antigens on RBCs)
ELISA
“Enzyme linked immunosorbent assay”
is a doble antigen test
theres 2 basic methods (direct and indirect)
variolation
small prevention procedure involving inoculation of material from dried small pox scabs into the respiratory tract or skin (1400s in china-1700s)
herd immunity
immunity in most of the population
outbreaks are sporadic due to the lack of susceptible individuals
attenuated vaccines
Weakened live pathogen, reduced virulence
Closely mimic an actual infection
Vaccine organisms replicate in the body, magnifying the effect
Confers lifelong immunity (both humoral and cellular)
Not given to immunocompromised patients
Risk of mutating back to virulent form
Problem with the oral polio vaccine
inactivated vaccines
Whole microbes are killed or inactivated
Safer than attenuated vaccines
Require repeated booster doses
Induce mostly humoral immunity
subunit vaccines
use antigenic fragments to best stimulate an immune response (avoids dangers associated with use of live or killed pathogenic organisms)
recombinant vaccines
subunit vaccines produced by genetic modification of yeast or insects (non pathogentic microbes) to produce desired antigenic fraction
is a product of recombinant DNAs
ex. hepatitis B vaccine, the capsid grown in recombinant yeast
toxoids
inactivated toxins produced by a pathogen and elicit an antibody response against that particular toxin
diphtheria, tetanus
virus like particle (VLP) vaccines
resemble intact viruses but do not contain viral genetic material
ex. HPV
polysaccharide vaccines
made from molecules in pathogen’s capsule; not very immunogenic
ex. pneumococcal vaccine
conjugated vaccines
polysaccharide antigen is attached to a protein (made to deal with children’s poor immune response to vaccines based on capsular polysaccharides)
Children < 2 years old, do not respond to T- independent antigens like capsular polysaccharides
Attaching polysaccharide to a protein carrier (conjugate): makes the vaccine immunogenic in babies as young as 2 months
ex. diphtheria or tetanus toxoid
DNA vaccines
Injected naked or encapsulated DNA into muscle (that encodes specific protein antigens)
DNA directs the synthesis of mRNA (transcription, translation) and produces the protein antigen encoded in the DNA
Stimulates humoral and cellular immunity
mRNA vaccines
mRNA enclosed in a lipid nanoparticle is injected into muscle where it directs the synthesis of the encoded antigen
COVID-19 vaccines direct synthesis of spike protein antigen
vaccine production
produced by growing pathogen in animals, embryonated eggs or cell cultures
adjuvants
Additives to a vaccine that improve its effectiveness
Alum (aluminum salts)
Monophosphoryl lipid A (derivative of LPS)
Improve the innate immune response, activation through Toll-like receptors
vaccine administration
Oral vaccines: favored due to ease of administration and effectiveness against pathogens that enter through the GI tract
Vaccines for rotavirus, adenovirus, cholera, typhoid
Nasal vaccine: attenuated influenza vaccine
Skin patch vaccines: (NanopatchTM) - administers a dry formulation of a vaccine
Multiple-combination vaccines
Immunologic-based diagnostic tests
interactions of humoral antibodies with antigens
Known antibody can identify an unknown pathogen
Known pathogen can determine the presence of an unknown antibody
hybridoma
“immortal” cancerous B cell (myeloma) combined with an antibody-producing normal B cell that when grown in culture produces the type of antibody characteristic of the ancestral b cell indefinitely
produces monoclonal antibodies (MABS)
Nearly unlimited quantities of identical antibody, same specificity as the ancestral normal B cell
No contamination by other antibodies
Highly specific
monoclonal antibodies
Mabs are uniform, highly specific, and produced in large quantities
Used in diagnostic tools
Used in human therapy
Treatments for multiple sclerosis, Crohn’s disease, psoriasis, cancer asthma, arthritis, COVID-19
Often derived from mouse B cells, leading to side effects
viral hemagglutination
occurs when viruses agglutinate RBCs without an antigen-antibody reaction
Viral hemagglutination inhibition test
is used for subtyping viruses (to detect antibodies to a virus)
– Viruses and RBCs are mixed with the patient's serum, If the serum contains antibodies to a virus, they neutralize the virus and inhibit hemagglutination
(red blood cells + antiviral antibodies serum + virus = virs neutralized and hemagglutination inhibited)
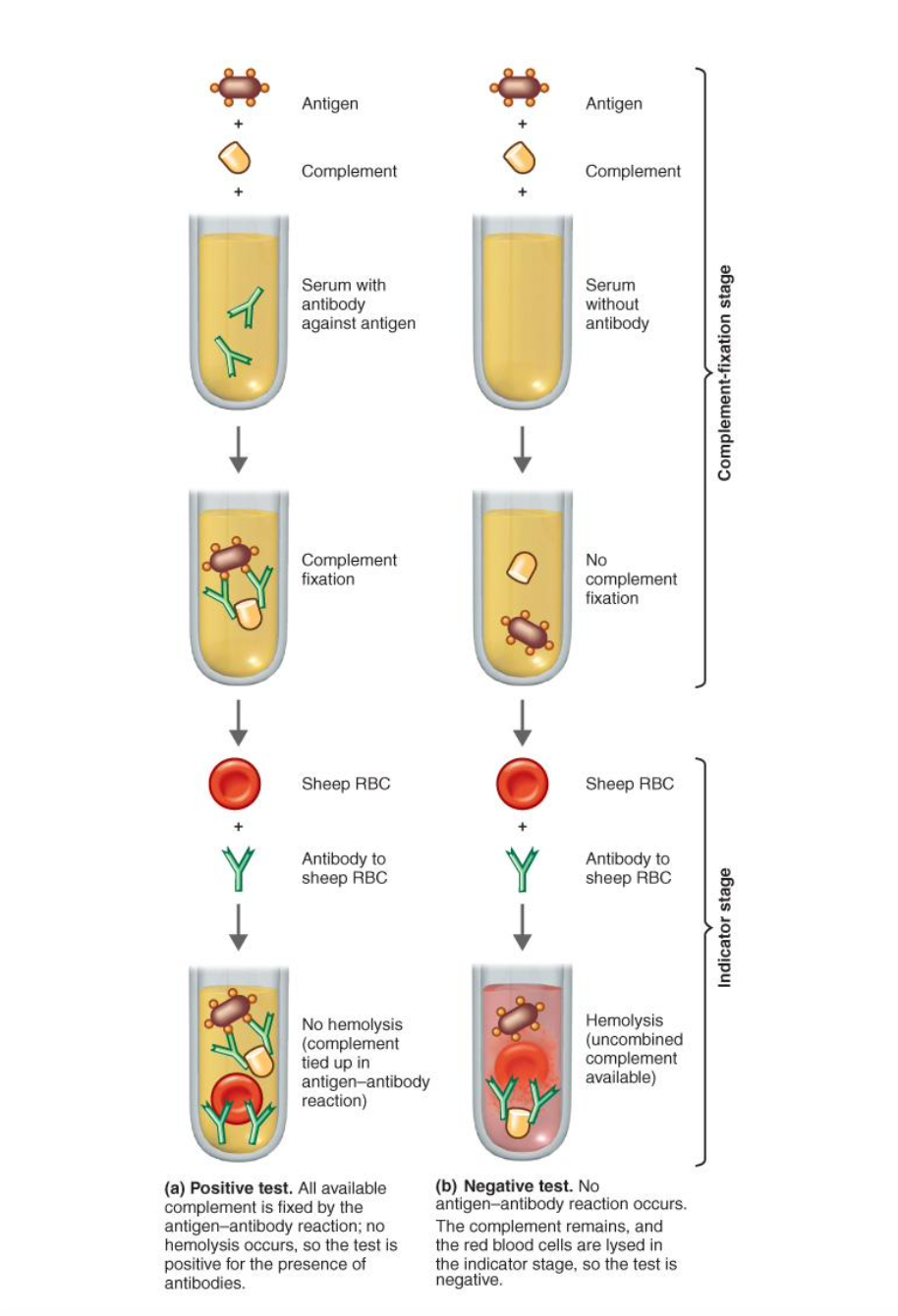
Complement fixation
complement serum protein binds to and is fixed to the antigen–antibody complex (The test checks whether a patient’s serum contains antibodies to a particular pathogen)
Detects small amount of antibody
Works for antibodies that do not work with precipitation or agglutination reactions
Use to diagnose certain viral, fungal, and rickettsial diseases
direct ELISA
detects antigens
have well filled with antibodies for antigens
sample containing target antigens is mixed with antibody
enzyme linked antibodies is mixed in and reacts with antigen bounded to original antibody
substrate attaches to the enzyme detecting antibody and a color is produced (positive test)
indirect ELISA
detects antibodies
have well filled with antigens
patient serum is added, complementary antibody binds to antigen
enzyme linked anti-HISG is added and binds to antibody bound to original antigen
substrate is added to enzyme linked anti HISG and reaction produces a color change (positive test)
rapid antigen test
(similar to ELISA, uses dye molecles instead of enzymes); is a double antigen test and type of lateral flow immmuno assay
Nasal swab sample which may contain SARS-CoV-2 antigens is applied to a paper strip
If SARS-CoV-2 antigens are present, as they flow through the strip they will be captured by labeled antibody—forming a colored line on the strip
control line
test validation
test line
forms a colored line on the strip
lateral flow assay
allow for detection of viral antigens by their binding to labeled antibodies, then attached to a paper strip