PATH120
1/91
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
92 Terms
Perspectives of Path
Sharing circles
Storytelling to promote values and transmit teachings
Medicine wheel (holistic health)
What is Pathology?
The process of using tools to help identify an illness
Characterizing diseases which influence how they are treated
Molecular genetics
The Ideal Healthcare Journey
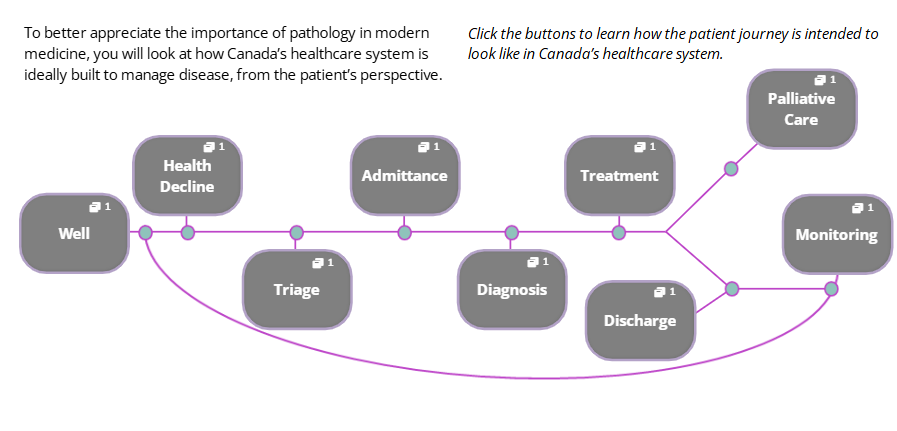
The Pathology Disease Paradigm
Cause (what caused this illness to occur)
Mechanism of action (how it develops)
Biochemical changes (how the cells and body alter in metabolism) - identified with testing
Morphological Changes (structural tissue change in appearance) - identified with testing
Functional Changes (symptoms associated with the disease) - identified with testing
Natural history (progression of the disease which determines prognosis)
Treatment (management or care of patient)
Complications (short and long term affect and factors that affect the patients)
Types of Learning
Learning by doing
Experimental learning
Storytelling
Knowledge keepers carry forward teachings and stories
Ceremonial speeches
Learning
Relationality, we are all related to one another, the natural environment, and the spiritual world
Concepts are organized into different worldviews and culture
Spiritual development and growth Is a big part of learning
7 grandfather teachings (humility, honesty, courage, love, wisdom, respect)
Holism and Health
Systems should be viewed as a whole
The medicine wheel and balance is different aspects of health
Cellular Biology (smallest to largest perspective)
The body is made up of cells which form tissues, organs and systems
Cells -> tissues -> organs -> systems -> human body

Plasma Membrane
outer skin of the cell made of phospholipids, require transporters to control movement in and out of the cell and receptors for communication with other cells
Nucleus Contents
Nucleus contains the genome which is stored in the form of DNA, where DNA is replicated and transcribed into RNA which after forms proteins.
Endoplasmic Reticulum
where protein is translated and processed, processing and packaging of proteins and other cargo into vesicles occurs
Lysosomes
digest waste in the cell and destroy viruses and bacteria
Endosomes
transport vesicles that sort, store, and organize contents of the cell
Peroxisomes
involves in the breakdown of hydrogen peroxide and reactive oxygen species and the molecules that produce them . this can cause a lot of damage if not neutralized by catalyze
Cytoplasm
the fluid that holds organelles within the plasma membrane
Cytoskeleton
acts as the skeleton and muscular system of the cell, holds the structure and generates force for cellular movement
Replication
occurs when the cell duplicates all of its genomic DNA in preparation for division so that each daughter cell receives a copy
Transcription
cells transcribe the sequences In DNA into RNA
Translation
mRNA is translated into amino acid sequences which fold to make protein
Mutation
Refers to changes in the DNA sequence of a cell. Some causes of mutations include DNA damage or errors in replication
There are cellular mechanisms capable of restoring a mutation back to its original sequence called DNA repair. In the case where safety features fail the new sequence may lead to change in amino acid sequence in the protein and altered function causing disease
G0 Phase
not a part of the cell cycle it is a phase that may enter when they are not actively dividing. Cell types found in this phase are most commonly nerve and muscle
G1 Phase
cells in this phase are active and growing but have not undergone division. The cells must pass through a checkpoint to star division. Majority of cell life is spent in this phase
S Phase
this is where cells replicate their entire genomes in preparation for division.
G2 Phase
phase: this is the last chance for cells to grow before division. In this phase DNA is checked and the size of organelles decrease
M Phase
cells are reorganized for cell division, protein synthesis is halted and the nucleus dissolves. The chromosomes move to opposite sides of the cells. The cell divides and the organelles return to their normal size
Stem Cells
Cell division can be asymmetric. Two daughter cells may be identical but their expression can be different
Stem cells are specialized cells that can divide to produce new stem cells, this is self renewal and can happen over several cell cycles.
Stem cells are found in the tissues of the body
Progenitor cells are stem cells that differ due to asymmetric division, these have the potential to divide into many other types of cells
Differentiation
Differentiation is when progenitor cells divide to replace specialized cells that were damaged or lost. When these cells divide they cannot change back or into any other type of cell
tissue renewal, certain tissues are continuously dividing to replace dead or missing cells in a process called tissue renewal
Necrosis
caused by a severe lack of resources necessary for life or due to trauma like freezing of physical injury. This results in the release of harmful chemicals which cause inflammation and damage to surrounding tissue.
Apoptosis
carefully regulated process where the cell breaks down in a controlled manner and the body is able to dispose of released cell components without inducing inflammation. This occurs frequently in the natural developmental process when a fetus loses webbing between its fingers inside the womb.
What is cancer?
Cancer is the name given to a collection of related diseases
In all types of cancer, some of the body's cells begin to divide without stopping and spread to surrounding tissues
Cancer is the uncontrolled growth of abnormal cells in the body
Cancer is defined as abnormal cell populations that 1. divide uncontrollably, 2. invaded and potentially spread to other tissues
Neoplasm
any abnormal tissue that forms when cells grow and divide more then they should, or do not die when they should
Tumour
a mass, any swelling or abnormal enlargement in or on the human body may be called a tumour, they can be benign or malignant
Benign
non cancerous
cannot invade or spread
attain sizes of 50kg or more without killing patient
have smooth and round contours similar to a sea sponge
Malignant
able to invade into other tissues (metastasis)
can start to spread or even kill before reaching 50g in weight
cancer is a malignant neoplasm
malignant tumours have a spikey contour reminiscent of a crab
Metastasis
troublesome characteristic of cancer that remains difficult to control. It is the major mechanism by which cancers kill
in most adult cancers invasion happens first, eventually the cancer attains the ability to spread through the bloodstream and colonize distant sites
carcinoma
Affects epithelial cells
Forms solid tumours
Ex: Prostate, breast, lung, and colorectal cancer
Sarcoma
Originates from tissues that support + connect body
Can develop in: Fat, muscles, nerves, tendons, joints, blood vessels, lymph vessels, cartilage, or bone
Lymphoma
begins in lymphocytes (infection fighting cells)
Glioma
Arises from CT of brain (cells that support neurons of the brain)
Leukemia
cancer of blood and bone marrow cells
Etiology of Cancer
Lifetime prevalence of cancer (Canada): 50%
Cancer is caused by genetic mutations
Impact of cancer on first nations peoples
Incidence: Higher incidence of cancer among First Nations (ex. Colorectal cancer)
Prevalence: Most prevalent cases are female breast and male prostate cancer.
Mortality: Mortality rate for most cancer types is significantly higher in First Nations peoples
Survival: 5-year survival rate across all cancers is generally lower compared to non-First Nations males and females
Proven Risk Factors of Cancer
Proven Carcinogens: Family history, tobacco use, age, HPV infection, and UV radiation
Misconceptions: WiFi, GMO’s, Deodorant, and Microwaves
How does tobacco cause cancer
inhaled tobacco contains toxic chemicals that damage epithelial lining of airway and lings. The epithelial tissue dies and specialized stem cells try to repair damage, traditionally after repair stem cells stop dividing and exit the stem cell cycle returning to resting rate, but sometimes persistent activation can occur making them vulnerable to oncogenic mutation leading to cancer
Silent Mutation
Change in DNA sequence that does not change/affect AA sequence or protein product
Oncogenic Mutation
Mutation that directly contributes to development of cancer
What mechanisms can potentially be prevented by mutation?
prevents cell from undergoing apoptosis
Increased ability to escape immune system
Capacity to enter and exit blood vessels (for metastasizing)
Challenges to treating cancer
Different tissue types respond differently to treatments
Continuous mutation occurs, leading to subclones that have varied responses to drugs (not all cells of tumour respond to drug)
diversity of tumours arise, making it complex to treat
Evolution/clonality of cancer
Transformation: normal cell undergoes mutation = tumour cell
Progression: Tumour cells divide = mutations in daughter cells = leads to tumour cell variants and clones
Proliferation: Rapid multiplication of cells = more mutations = growth advantages = subclones derived from same tumour
Tumour Heterogeneity: Many tumour cell variants and subclones arise (genetically different) and can have different physiological characteristics (ex. Metastatic, invasive, drug resistant, etc.)
Cancer Associated Genes
Oncogenes: Mutated genes which produce proteins w/new or altered functions. Proto-oncogenes: Unmutated form of oncogenes (normal genes). Involved in growth factor receptor pathways (mediates homeostasis, injury repair, etc). Approx. 20 genes involved in this (proto-oncogenes) and have ability to become oncogenes via genetic mutations ● Mutation in only 1 allele = cancer. Associated with sporadic cancer (present in patients with no family history of cancer)
Tumour suppressor genes: Genes whose normal functions (ex. preventing cell growth and inducing cell death) are disabled by mutations. Act as cell cycle checkpoints and play role in controlled apoptosis. Both copies of tumour suppressor genes must be mutated = cancer. Common in familial cancers (patients with inherited component)
Tumour Suppressor Gene: TP53
Extensively studied and is usually mutated to some capacity in all cancers
➔ TP53 (found on chromosome 17) codes for the protein, p53, which regulates cell division
➔ Role of p53 protein (TLDR; ‘brakes’ on cells preventing quick cell division)
◆ Responds to genomic damage by activating repair and/or cell death programs
◆ This prevents the survival of cells with cancer-causing mutations
◆ p53 acts in G1 phase of cell cycle, prior to start of DNA replication
Mechanisms of p53
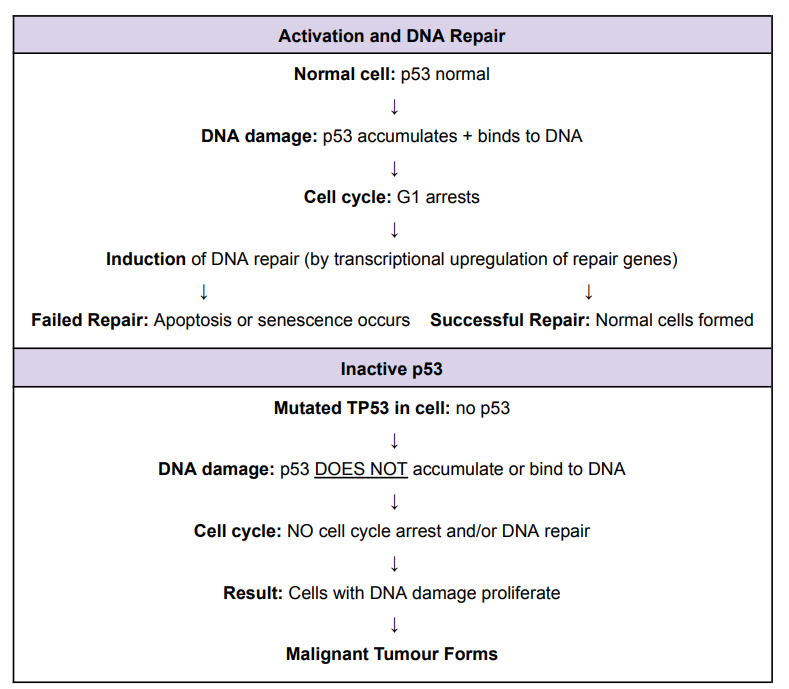
Oncogene: ERBB-1
➔ ERBB-1 gene (found on chromosome 7) codes for EGFR (Epidermal Growth Factor Receptor) protein
➔ In a 2020 Cancer Communications paper, EGFR abnormalities were assessed in 11,000 patients, and found that ERBB-1 gene was…
◆ Affected in over 25% of glioblastoma cases
◆ Affected in 15% of lung adenocarcinomas
➔ Role of EGFR
◆ Is a tyrosine kinase receptor that detects extracellular signals (ligands) and forms dimers which transmit a signal into the cell
● Induces gene expression!!
◆ Tightly regulated in normal cells to prevent unwanted proliferation
Gene Expression Through EGFR (It’s mechanism of action)
Ligand Binding: Components of EGFR undergo structural change = receptor activated
Phosphorylation: Phosphorylation of EGFR in cytoplasm = phosphorylation of secondary messengers = activated messengers transmit signal to nucleus
Gene Expression: Increased transcription of genes for cell proliferation and survival. ➔ Also drives mechanisms like cell migration across tissues and angiogenesis
Termination: To terminate signal, ligand is released or receptor is broken down (to avoid unwanted/excessive cell proliferation)
Oncogenic Activation of EGFR

EGFR as a Therapeutic Cancer Target
Chemotherapy ➔ Does not directly target EGFR ➔ Instead, kills rapidly-dividing cells in body
Antibody-based therapy ➔ Certain antibodies produced outside body are injected into patients ◆ Cause inactivation + destruction of target protein OR cell death via immune system activation ➔ EGFR ligand-binding domain is extracellular, making it susceptible to this kind of therapy
Kinase Inhibitors ➔ EGFR and secondary messengers have kinase activity ➔ SO, small molecule inhibitors can cross plasma membrane and disrupt signalling cascades
Colorectal Cancer
➔ Certain mutations in tumour suppressor genes are common in colorectal cancer
➔ These mutations can either be sporadic or familial
◆ Sporadic colorectal cancer: Mutation spontaneously occurs on both alleles of adenomatous polyposis coli (APS) gene.
◆ Familial colorectal cancer: An inherited mutation, most commonly occurs in mismatch repair genes (MSH2)
➔ The familial pathway can lead to Lynch Syndrome
◆ AKA Hereditary Nonpolyposis Colorectal Cancer (HNPCC) syndrome
◆ Most common hereditary colorectal cancer syndrome
◆ Caused by germline mutation (mutation in germ cell; egg or sperm, passed to offspring) in MSH2 gene
◆ Individual can be tested for this through genetic counselling + testing
Development of Colorectal Cancer
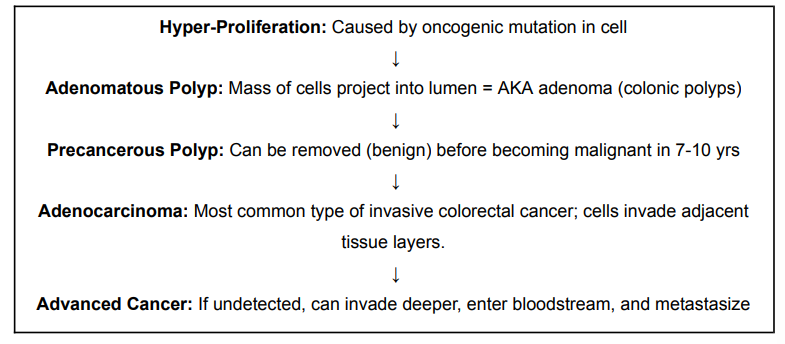
Characterizing Solid Tumours (By Stage and Grade)
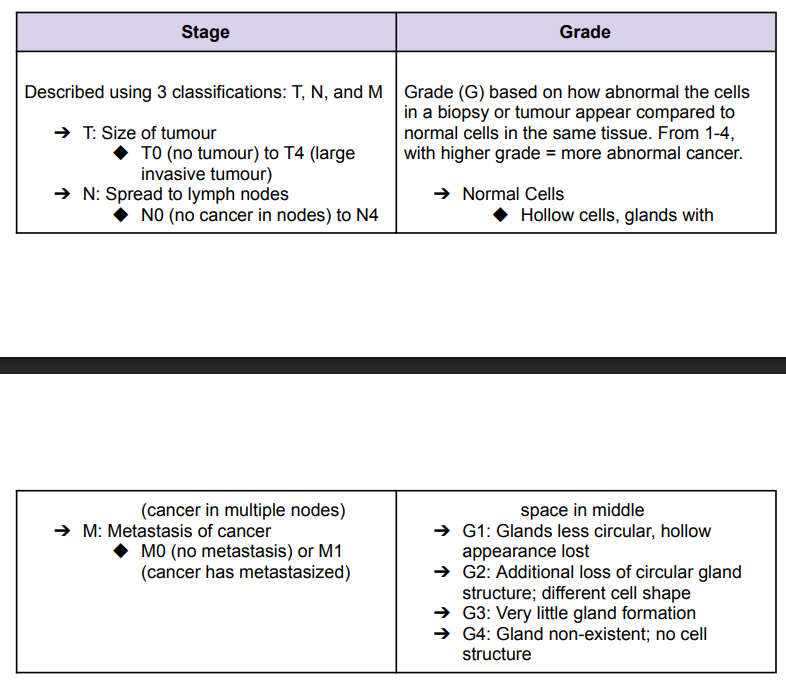
Prognostic Factors and Screeening for Colorectal Cancer
➔ Prognostic Factors for Colorectal Cancer
◆ Age + general health
◆ Response to treatment
]◆ Stage + grade
◆ Genetics
◆ Access and compliance
➔ Screening for colorectal cancer
◆ Regular screening (colonoscopies) is crucial for detecting precancerous polyps
◆ Done on patients with risk factors like family history or age
◆ Fecal Immunochemical Test (FIT) is an at-home screening tool
● Examines stool for small amounts of blood that could be caused by colorectal cancer
◆ Many people don’t get screened due to
● fear of screening tools
● no family history
● misconceptions with no symptoms ‘
● or concern over costs
Acute Myeloid Leukemia (AML)
➔ What are blood cancers?
◆ Begin in the bone marrow, where blood stem cells fail to mature into healthy blood cells
◆ These cells divide, producing cancer cells, and crowd out normal stem cells
◆ Decreased blood cells = fatigue, immune issues = lack of proper white blood cells, bleeding + clotting due to platelets
➔ Blood Cancer Stats in Canada
◆ Account for 10% of cancer diagnoses in Canada
◆ First nations have lower incidence of blood cancers compared to non-First Nations peoples, however, they have a lower survival rate for blood cancers
Hematopoiesis
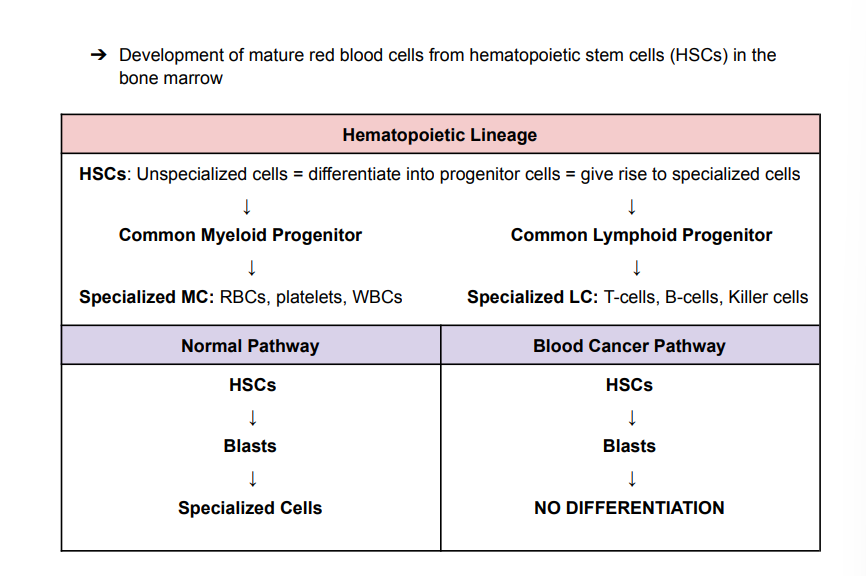
Classical blood cancer pathway:
Differentiation Block (DB) + Enhanced Proliferation (EP) = Blood cancer
◆ DB: Tumour suppressor gene involved in differentiation is lost in HSCs or common progenitors = accumulation of blasts (immature blood cells)
◆ EP: Then, another gene is mutated, and a proto-oncogene produces growth signals = leads to proliferation
Promyelocytes
Precursor to white blood cells and of myeloid lineage
Types of Leukemia
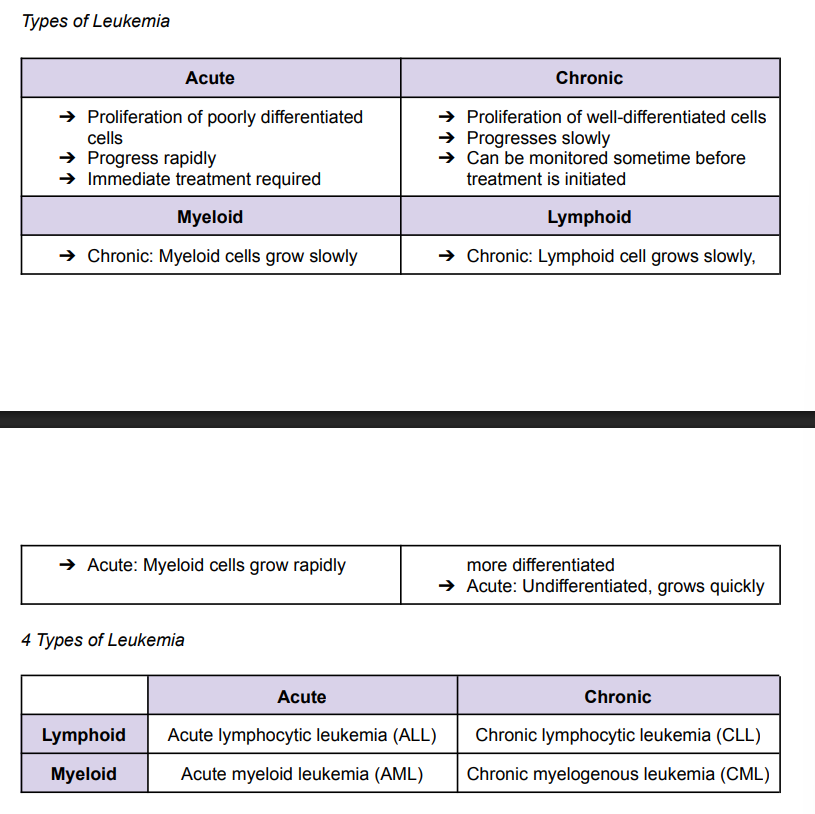
AML Chromosomal Translocations
Translocation: When chromosome breaks and is fused incorrectly
Break between two gene sequences, that fuse together and create a hybrid sequence
Codes for fusion protein
PML-RARα (hybrid sequence that codes for fusion protein!!)
A hybrid sequence that occurs during fusion of chromosome 16 and 17 of PML and RARA genes
Leads to leukemia
PML-RARα Oncogene and Leukemia Therapy (with ATRA)
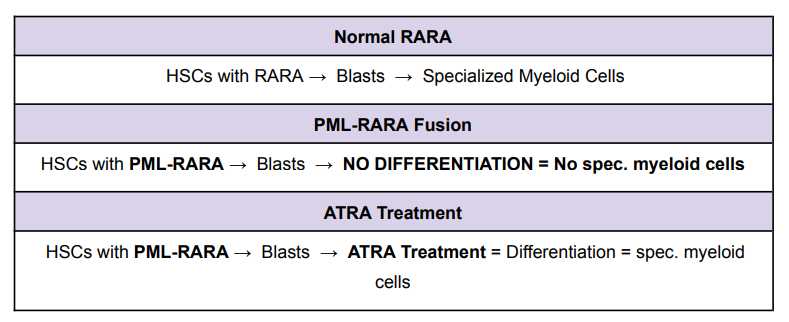
Prognostic Factors for Leukemia
◆ Age
◆ Weight
◆ Previous blood disorders
◆ Genetics
Immunotherapy
: A cancer treatment that utilizes the body’s immune system to fight cancer cells
◆ Benefits patients with high levels of immune checkpoint gene expression in cancer cells
Biomarkers
A measurable indicator of a state or condition in the body. Measured through blood, urine, and tissue samples.
◆ Biomarkers are important in screening (ex. Lynch Syndrome) and treatment options (ex. PML-RARA)
◆ Gene expression is a biomarker in cancer
◆ Other cancer biomarkers include: Small chemical products, enzymes, DNA, RNA, cancer cells, protein
3 Classifications of Biomarkers
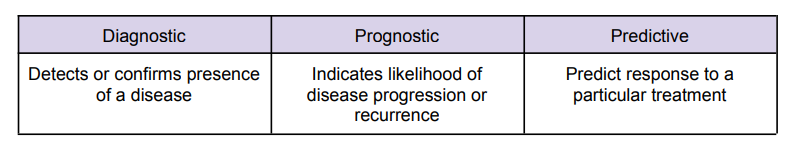
Genome Sequencing (Timeline)
◆ Human Genome Project: Took 13 years, completed in 2001, and cost over $1B
◆ Next-Gen Sequencing: Takes hours to complete, and costs less
◆ Tumor Sequencing: Databases of genomic tumour info helps to understand cancer pathways
◆ Data Analysis: Can be used to identify unknown biomarkers in certain cancers
◆ Application: Research helps to understand biological processes, identify new therapies, determine new diagnostic and prognostic factors, and improve patient outcomes
Intro to Infectious Disease and Population Health
➔ Infectious Agents: Organisms capable of producing infection or causing infectious disease
◆ Most common infectious agents are bacteria, viruses, fungi, and parasites
➔ Human Microbiome: Some collection of microbes that live symbiotically in and on humans. Found on skin and mucous membranes and crucial for human health.
4 Classes of Microbes
Imbalance between ‘good’ and ‘harmful’ microbes can lead normal flora to become opportunistic and lead to potential pathogens
However, microbes that normally cause disease (always pathogenic) are called pathogens

Innate vs Adaptive Immune Responses
➔ The physical, chemical and cellular barriers in place to remove and prevent foreign pathogens from entering our bodies
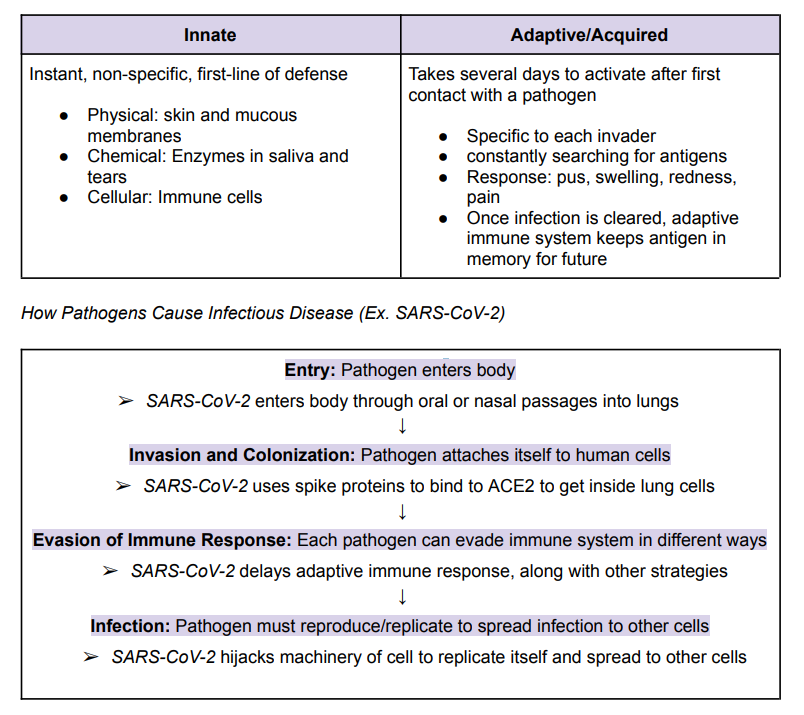
Three Conditions for an Infection to be Established in an Organism
Reservoir: Sites where pathogens can persist for long periods of time. Can be biological of environmental
Mode of Transmission: Transmitted through direct contact, droplets, vectors or vehicles. Some diseases are easier to transmit than others.
Opportunistic Conditions: Conditions like stress, surgery, or old age can encourage development of infectious disease.
Preventing transmission of infectious disease
◆ Eliminating reservoirs (Ex. eliminating mosquitos with malaria)
◆ Enhanced barriers (Ex. face masks, hand washing, social distancing)
◆ Vaccines
◆ Dev. of targeted medicines ➔ Chickenpox vaccine reduced prevale
➔ Chickenpox vaccine reduced prevalence of chickenpox dramatically (is now a routine immunization)
➔ Herd Immunity: When a significant proportion of the population is vaccinated and immune to disease, it indirectly can prevent those at high risk from contracting the disease.
◆ Some groups cannot receive vaccinations like infants, elderly, pregnant women, or the immunocompromised ➔ Infectious disease was used as a form of colonization (to control weakened populations)
◆ Smallpox used as biological warfare against indigenous peoples (blankets infected with smallpox given as a ‘gift’ to Indigenous peoples)
➔ First Nations Peoples experience infectious disease at higher rates than the general population (ex. Strep Throat and TB brought by European colonizers)
◆ Due to inadequate access to proper care facilities
Pathogenesis and Treatment of Bacterial Infections
➔ Bacteria can be classified based on structure of cell wall
◆ Gram positive: Thick peptidoglycan wall
◆ Gram negative: Thin peptidoglycan wall surrounded by an outer membrane
➔ Antibiotics: Medications used to stop growth of/kill microorganisms
◆ Bacteriostatic Drugs: Inhibit bacterial growth with help of host’s immune system (for non-life threatening situations)
◆ Bactericidal Drugs: kills susceptible bacteria without help from host's immune system
◆ Broad-spectrum: Kills wide range of bacteria
◆ Narrow-spectrum: Only active against small group of organisms
➔ Antimicrobials: Any agent, natural or synthetic, that stops growth/kills microorganisms (usually antibiotics, but can also be bleach, etc)
Antibiotic Target
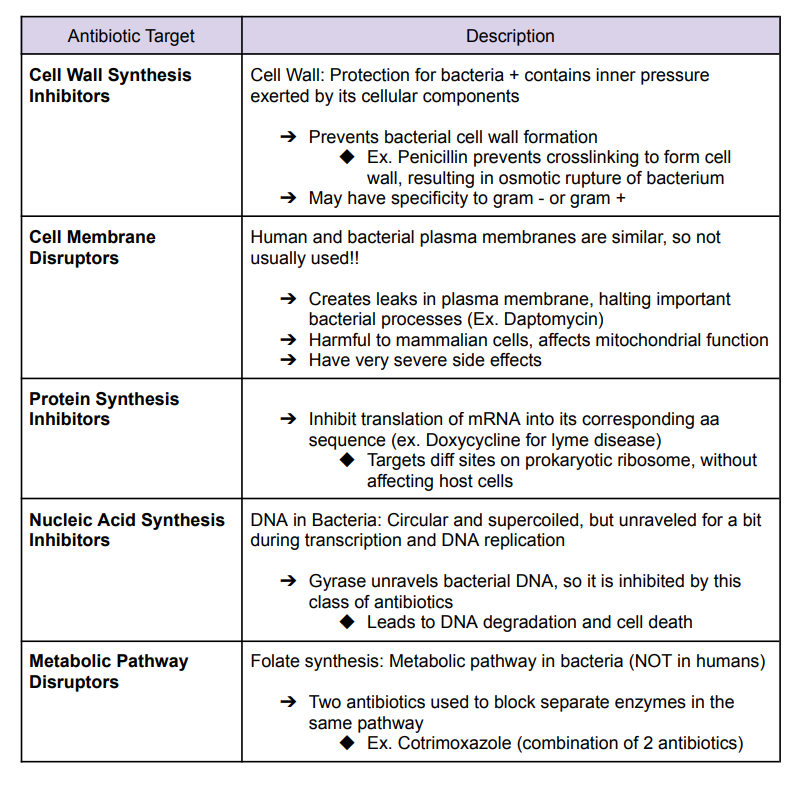
Evolution of Antibiotic Resistance
➔ Bacteria have developed mechanisms to resist effects of antibiotics
◆ Alters Targets: Mutation or enzyme modifies structure of target drug, so it becomes ineffective
◆ Restrict Target Access: Unable to enter cell, or pumped out immediately upon entering
◆ Develops Drug Specific Enzyme: Bacteria develops enzymes to destroy or modify antibiotic so it won’t work
Development of Antibiotic Resistance
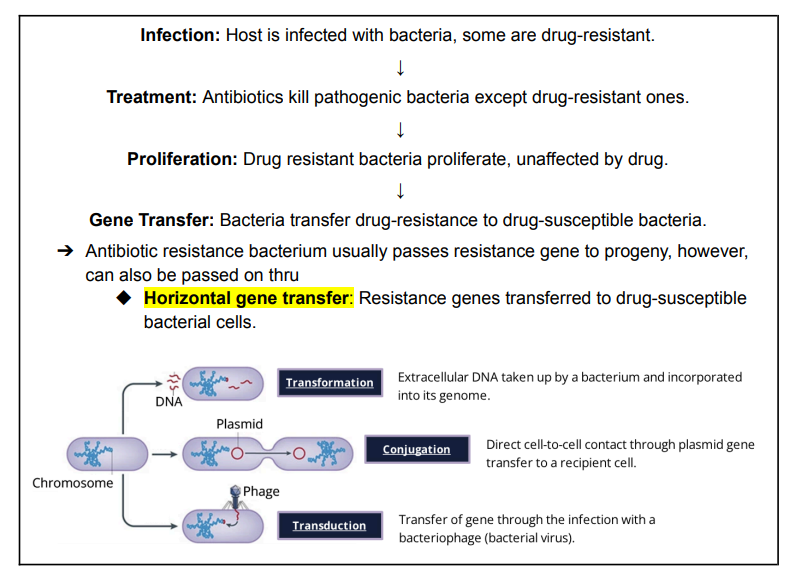
Selective Pressure
Antibiotic-resistant strain will only be maintained if antibiotic stimulus is present. If not, the antibiotic-resistant strain will die off.
MRSA and CPO
Two antibiotic resistant bacteria that are present in hospital acquired infections; patients who acquire them are put on… ◆ Contact precautions: Infection prevention + control interventions intended to prevent transmission of infectious agents
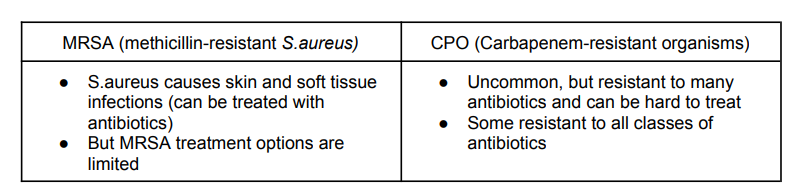
Evolution of S.aureus to MRSA
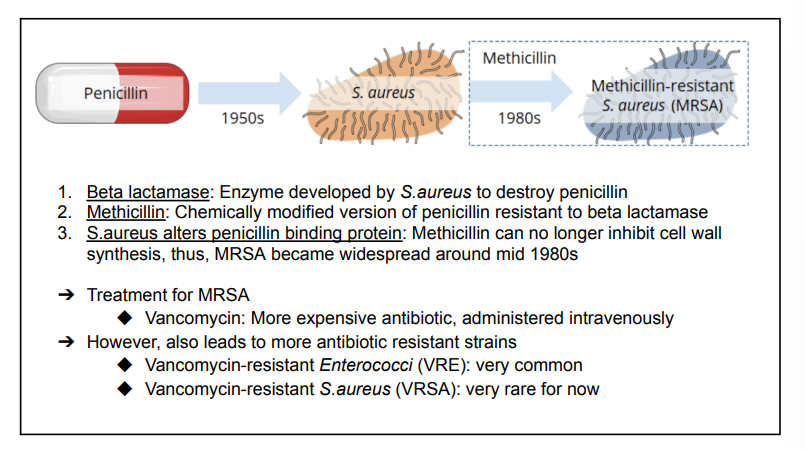
Multi-drug Resistance
Species of bacteria that have acquired mechanisms of resistance to multiple antibiotic classes
Global Antibiotic Resistance
➔ Evidence for worldwide antibiotic resistance
◆ Emergence of beta lactamases and carbapenem resistance
➔ Overuse of antibiotics create ideal environment for bacteria to develop resistance
◆ Hospitals: Non-prescription antibiotics use is unregulated
◆ Agriculture and aquaculture: animals treated with antibiotics frequently
➔ Burden of antibiotic resistance is very high
➔ Regulation of antibiotic use in high-income countries is crucial
➔ Antibiotics are sold without prescriptions and not well regulated in low- and middle-income countries
◆ Due to lack of testing and funding, and political and healthcare sector leadership
◆ Antibiotics may be lower quality, allows for more resistance
➔ Antibiotic drug discovery is decreasing today!
Measures in Place to Prevent Antibiotic Resistance
1. Surveillance: Monitoring antibiotic use + resistance.
2. Stewardship: Appropriate + careful use of antibiotics across industries and sectors
3. Research and Innovation: Continuous research in antibiotic discovery
4. Infection Prevention + Control: Strict adherence to proper prevention practices.
Viral Infections and 1918 Pandemic
➔ 1918 Influenza Pandemic (caused by influenza virus)
◆ Virus spread in 3 waves, today is the seasonal flu
◆ No quarantine measures in place for travel within country ◆ Measures put in place were unsuccessful
◆ Department of Health founded in 1919 as a result
➔ The 1918 pandemic had severe impact on communities
◆ Ex. Indigenous patients or minorities were segregated and given inadequate care
◆ Some remote communities protected themselves by preventing anyone from entering or exiting the village, protecting themselves and other communities
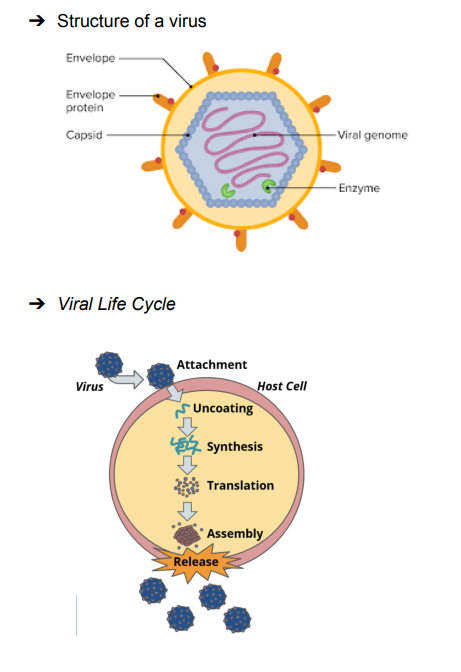
Pandemic and Vaccination
➔ COVID-19 Pandemic (Caused by SARS-CoV-2)
◆ Respiratory disease characterized by fever, cough, and fatigue
◆ Part of coronavirus family (spherical, enveloped, with single-stranded RNA)
◆ Contains spike proteins
➔ COVID-19 Infection control measures
◆ Distancing, closures, masking, washing, staying at home, quarantining, tracing
SARS-CoV-2 Mechanism of Infection

COVID-19 Vaccines
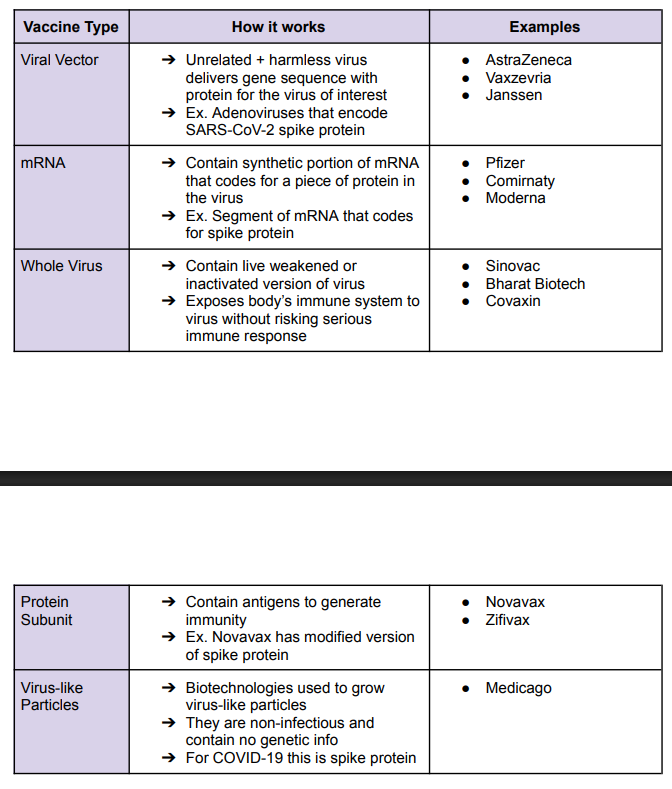
Future of Understanding and Managing Disease in 21st Century
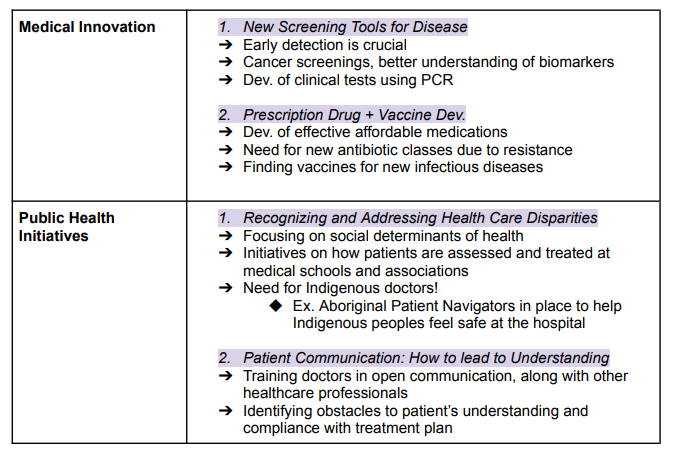
Amplifying Indigenous Voices
◆ Protective Factors: Self-government, land control, control over cultural activities
◆ Prevention: Community-based approaches, gatekeeper training, peer-support groups
◆ Spirituality: Using Indigenous concepts of well-being + spiritual practices (ex. Pow-wows, sweetgrass ceremonies, and sweat lodges)