Exam 4 Anatomy 403
1/100
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
101 Terms
digestive processes
break down food particles in chyme that the body can work with on a cellular level
-ingestion, secretion, mixing and propulsion, mechanial and chemical digestion, absorption, defacation
GI tract organs
(alimentary canal)
Mouth
Pharynx
Esophagus
Stomach
Small Intestine
Large Intestine
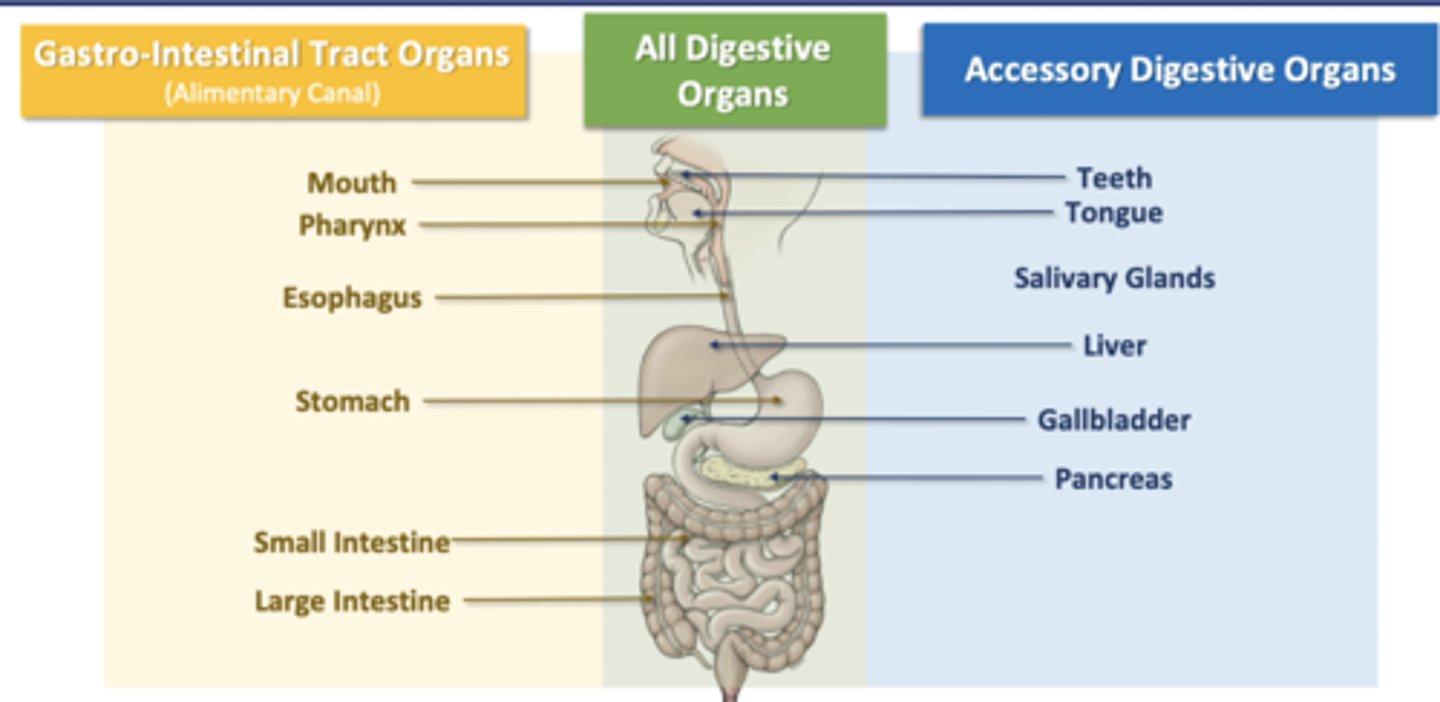
Accessory Digestive Organs
Teeth
Tongue
Salivary Glands
Liver
Gallbladder
Pancreas
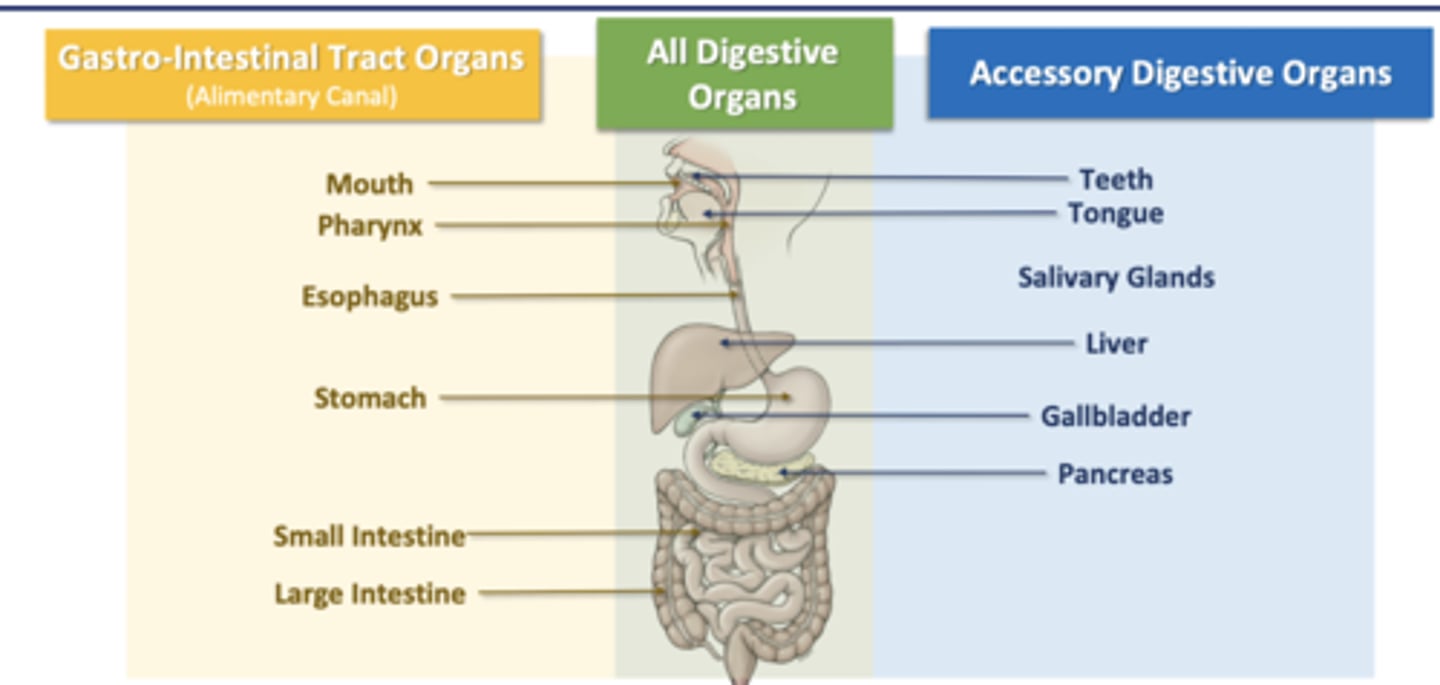
Develop and organization of gut
The gut starts out as a single embryological gut tube, rotates as it grows
-this gut persists into adulthood, organization of regions important
-regional and neurovascular supply relationships maintained in developed gut
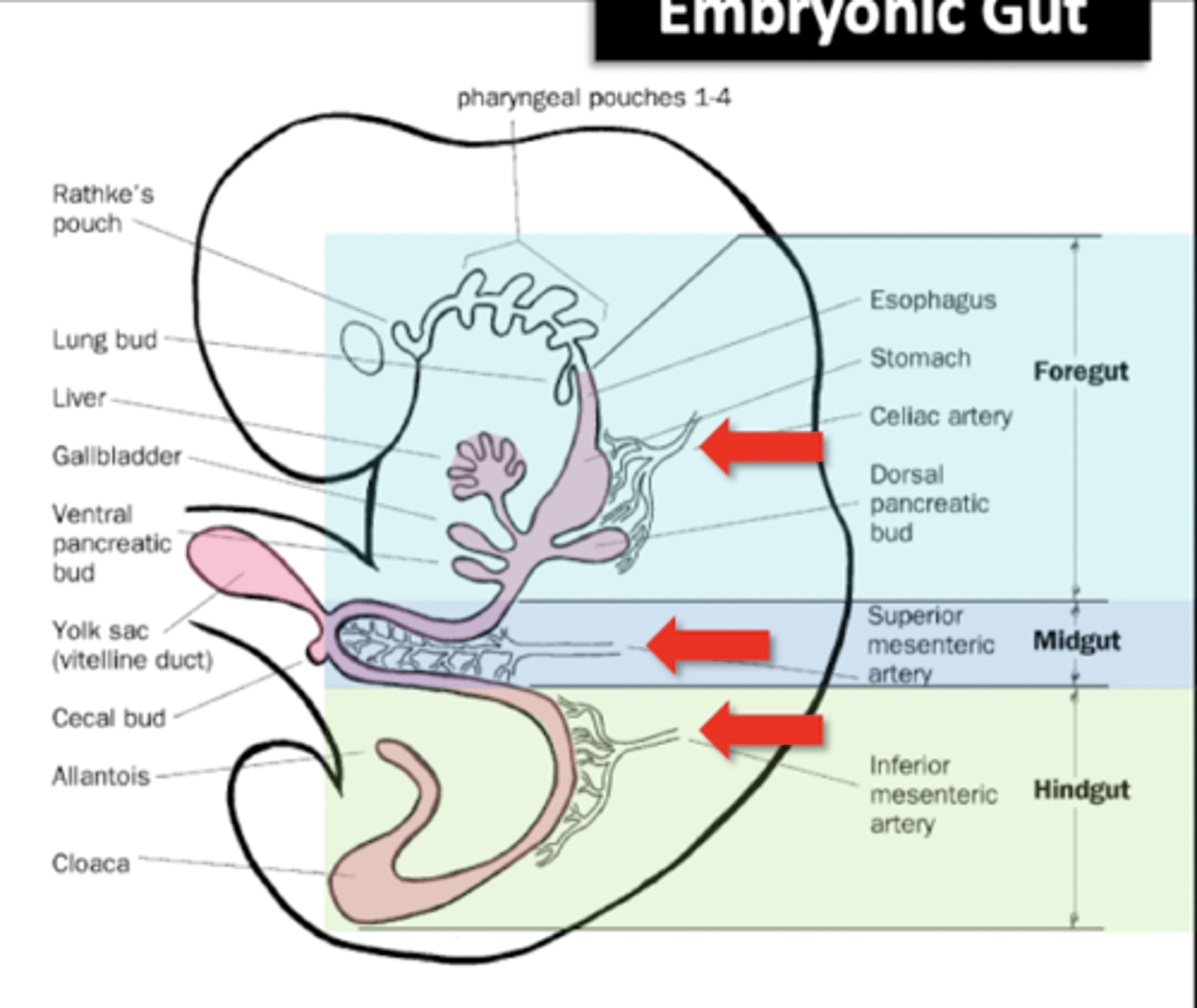
Regions of gut
Foregut (celiac trunk)
Midgut (SMA)
Hingut (IMA)
Organs in the Foregut
Esophagus (abdominal)
Stomach
Prox 2/3 Duodenum
Accessory Organs:
Liver and Gallbladder
Spleen
Pancreas
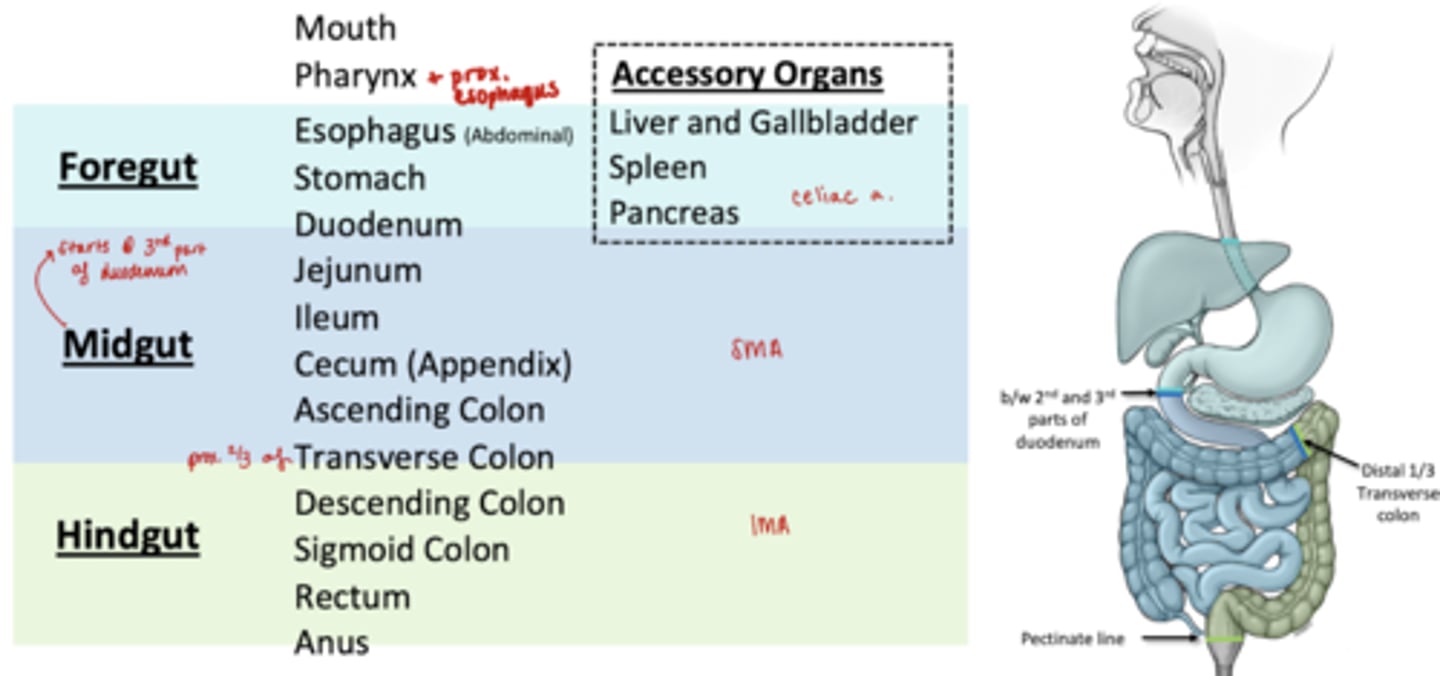
Organs in Midgut
Distal 1/3 of Duodenum
Jejunum
Ileum
Cecum (appendix)
Ascending Colon
prox 2/3 Transverse Colon
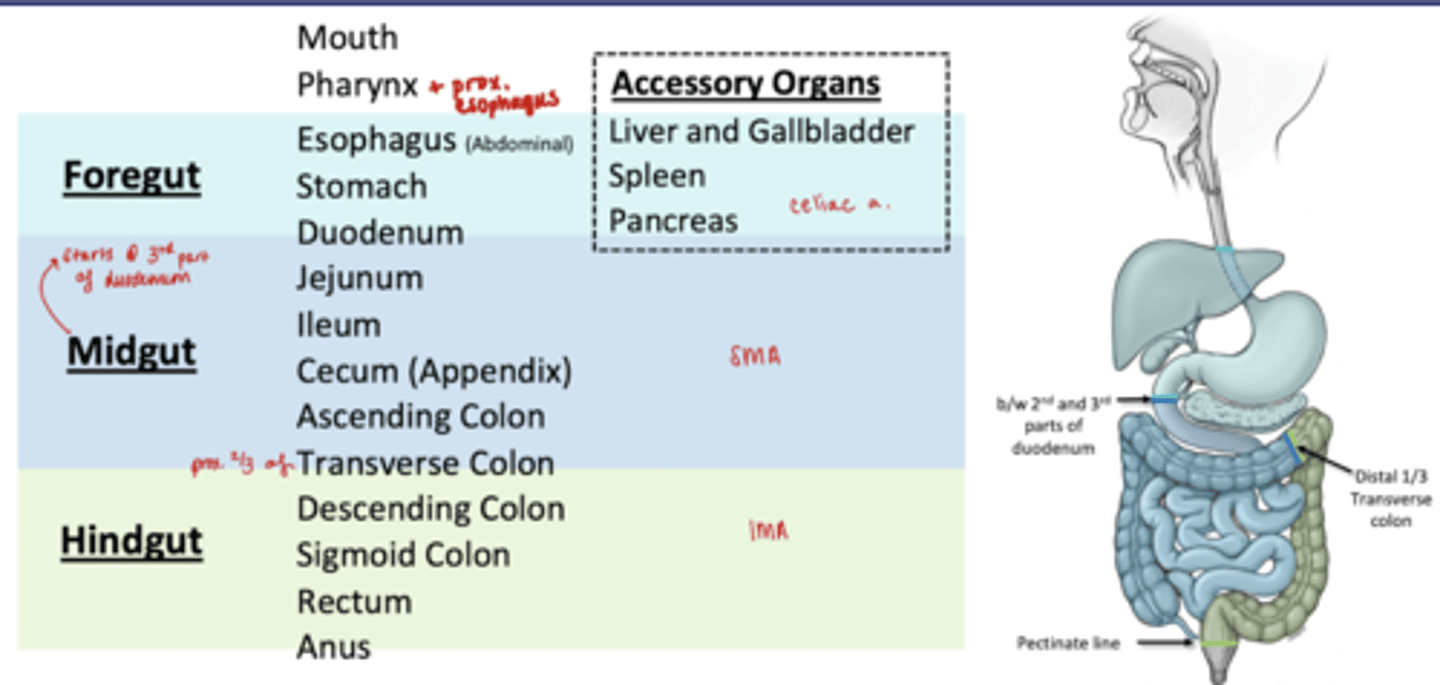
Organs in Hindgut
Distal 1/3 transverse colon
Descending Colon
Sigmoid Colon
Rectum
Anus
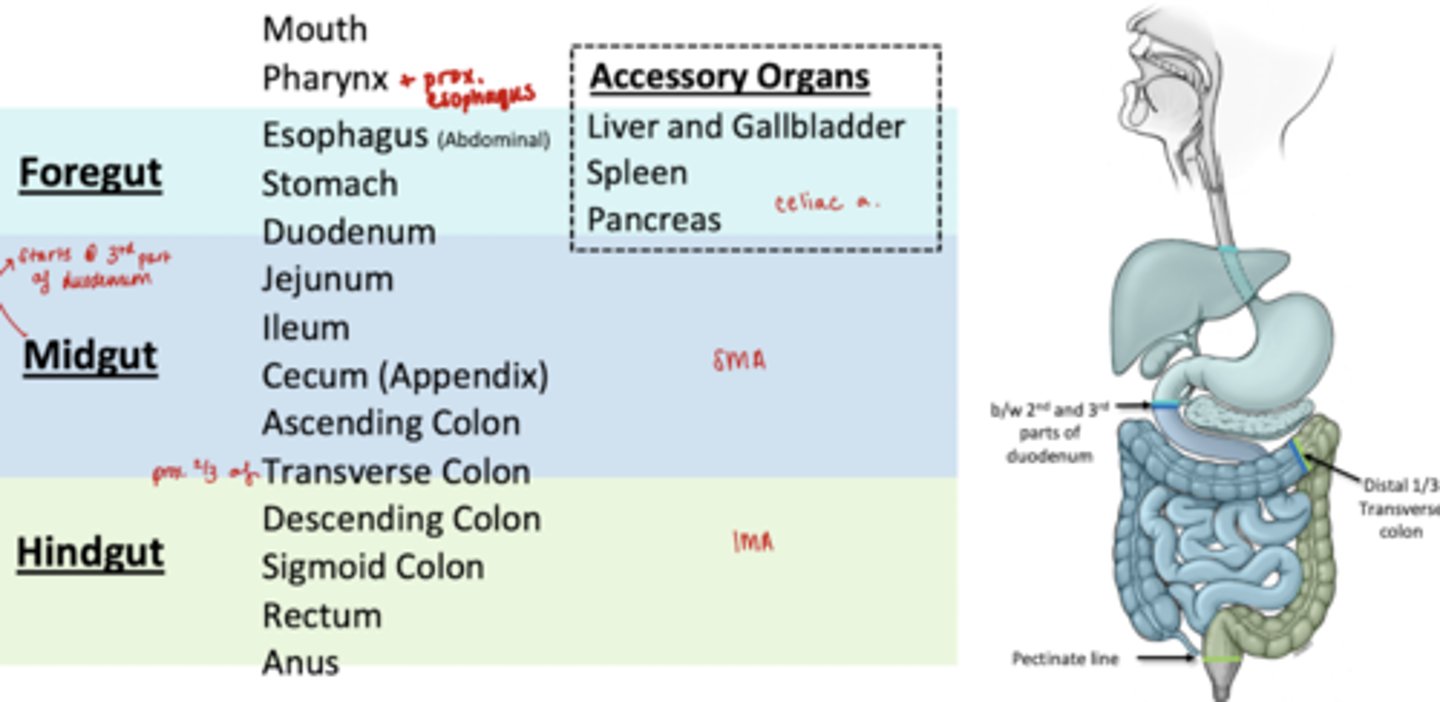
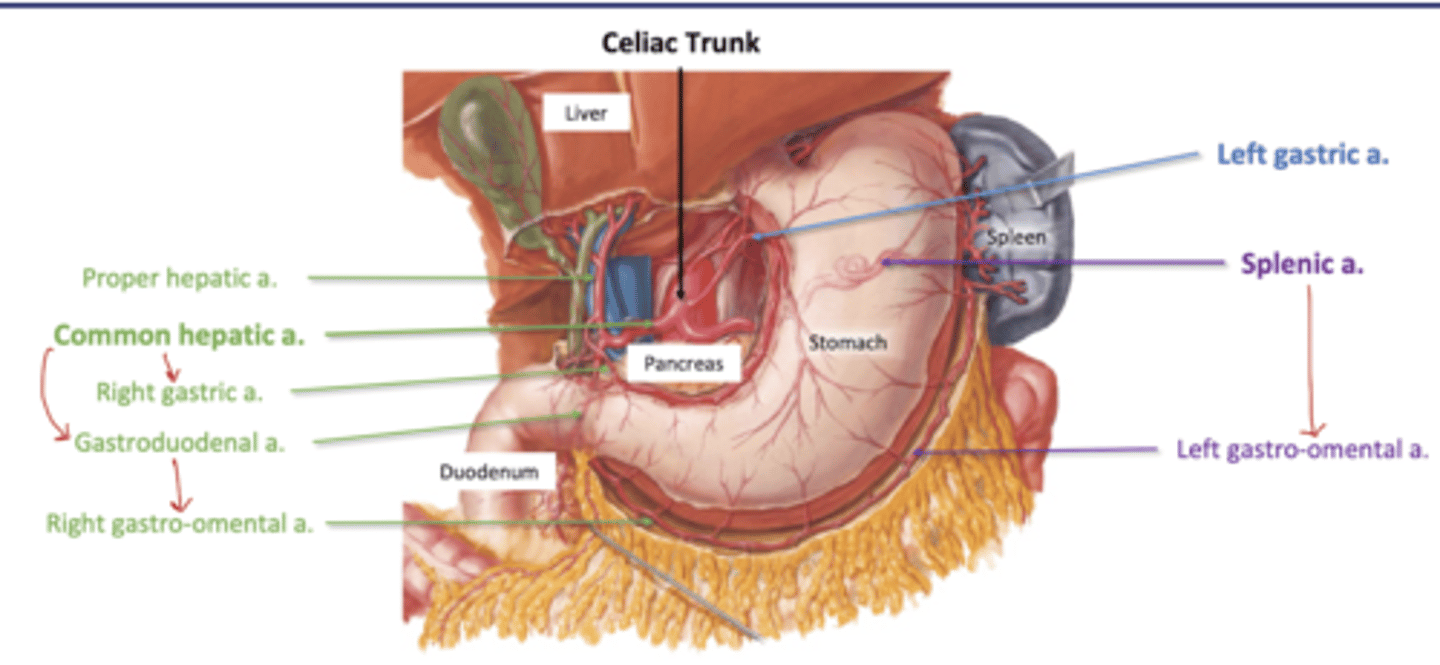
Celiac Trunk Branches
Common Hepatic
-R gastric (R lesser curvature)
-Gastroduodenal--> R gastro-omental (greater curvature)
-Proper Hepatic (liver)
L gastric a. (L lesser curvature)
Splenic--> Left Gastro-omental (greater curvature)
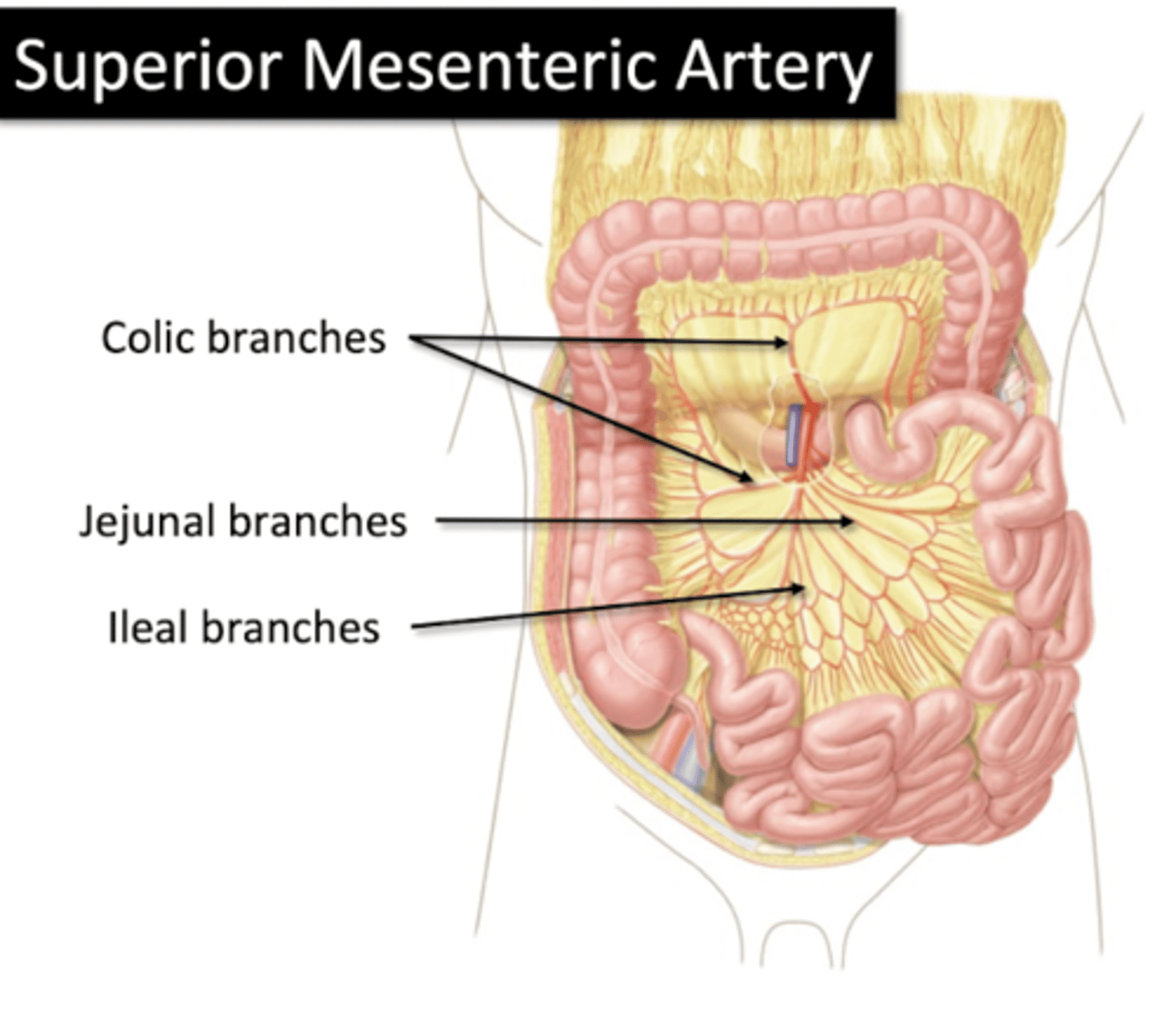
Super Mesenteric Artery
Arterial Supply of Gut
Colic Branches
Jejunal Branches
Ileal Branches
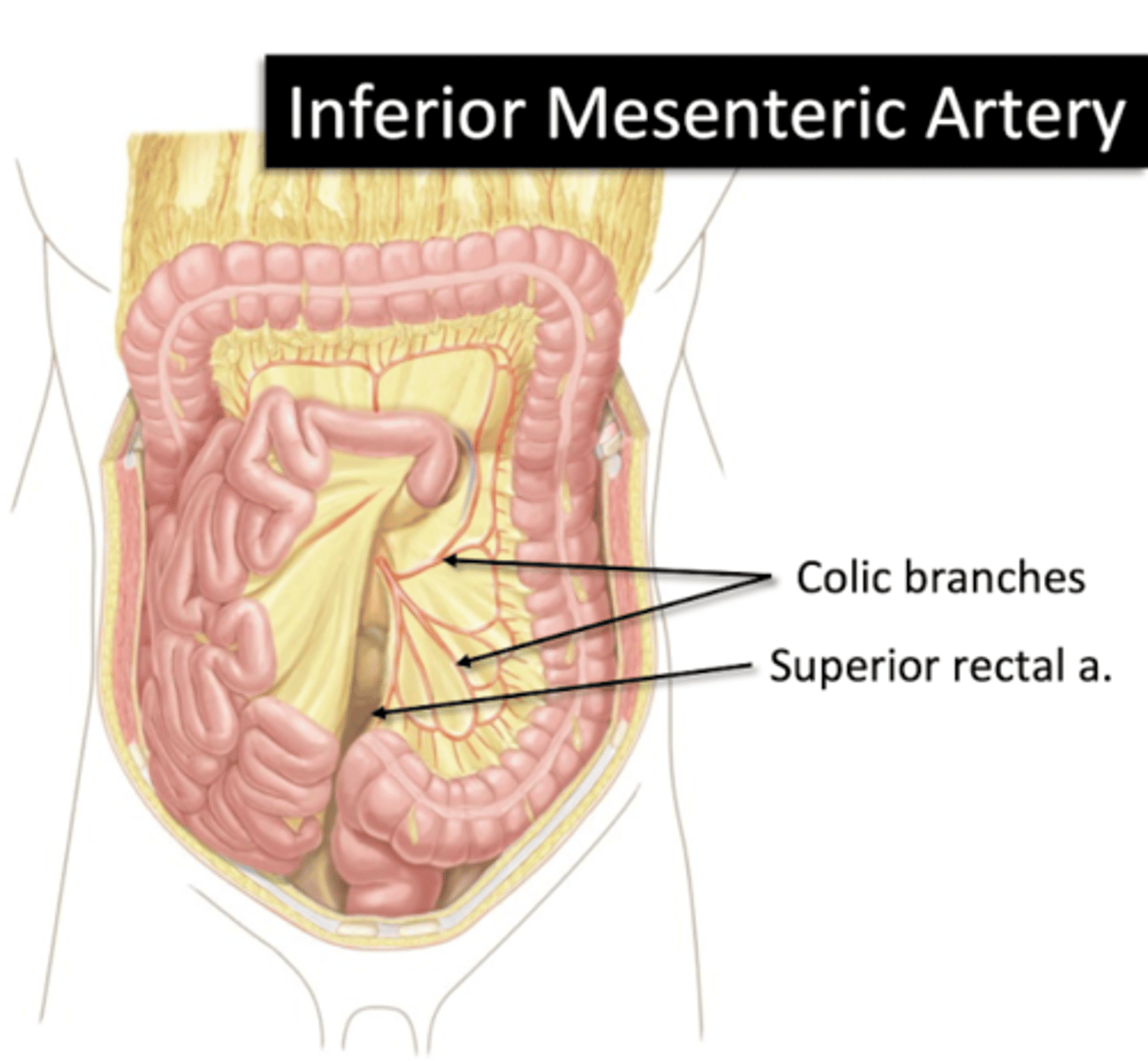
Inferior Mesenteric Artery
Arterial supply of Gut
Colic Branches
Superior Rectal a.
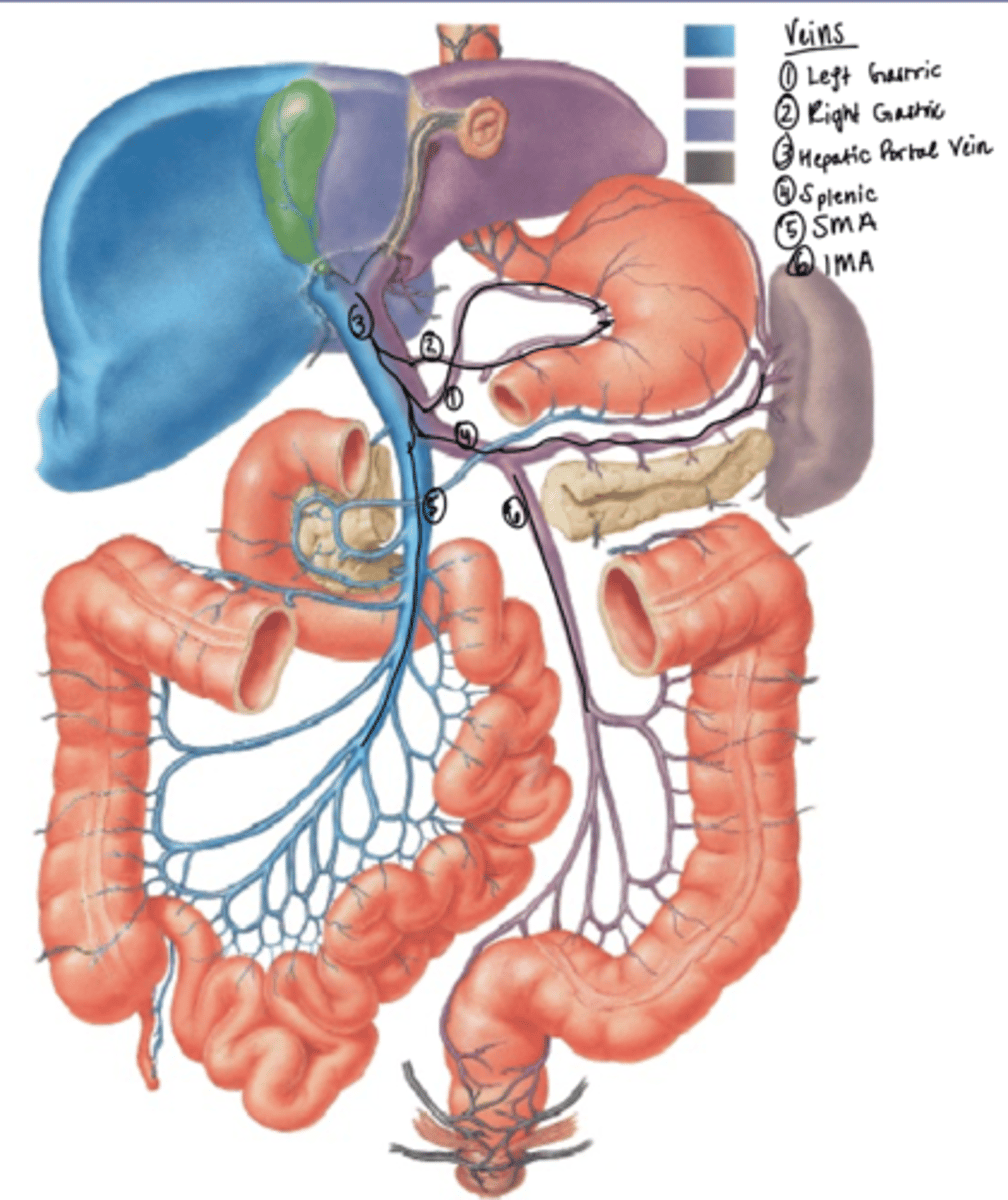
Hepatic Portal Vein
Drains to Liver- all venous blood from gut processes in liver before returning to systemic circulation
-SMV
-IMV
-Splenic vein
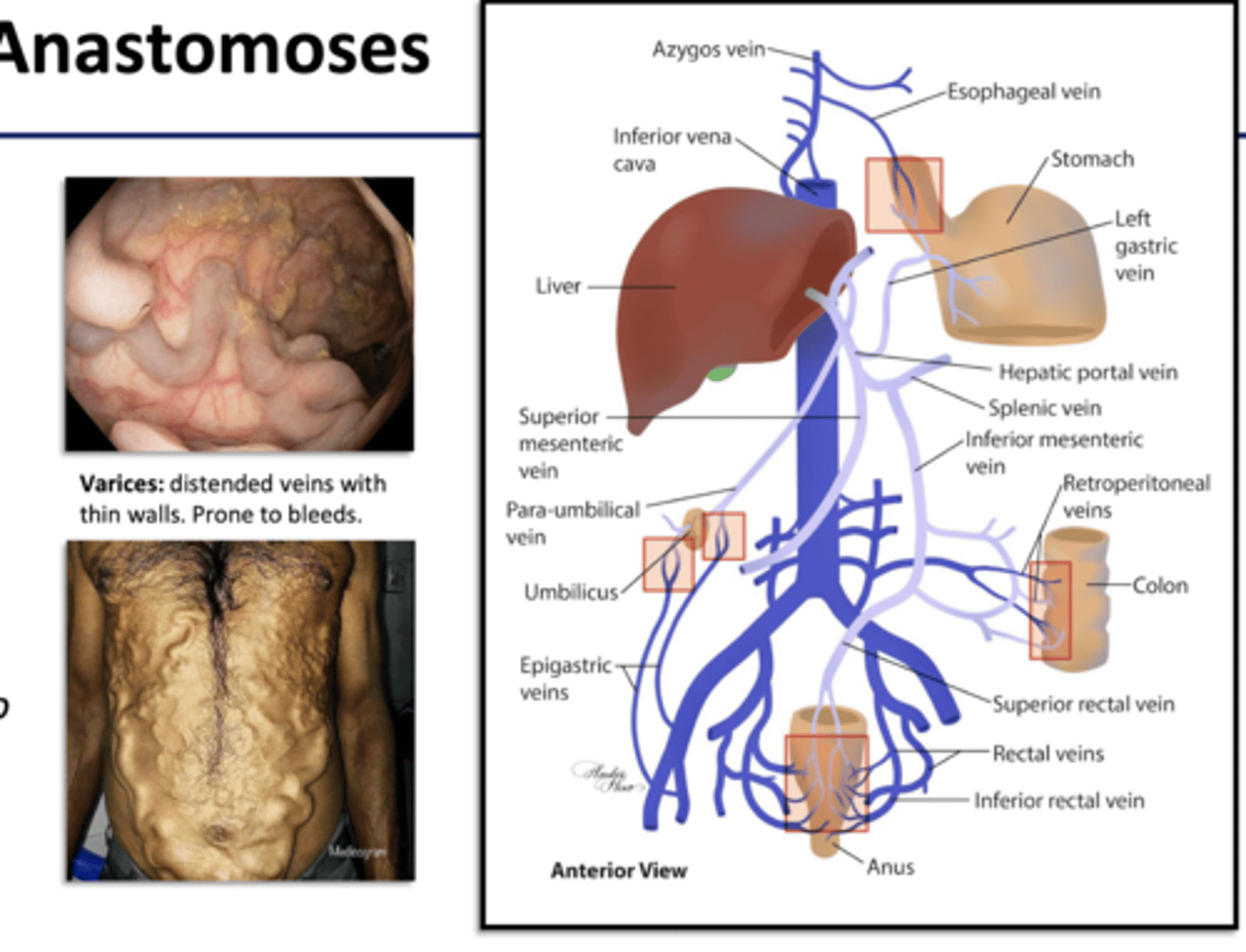
Portal Caval anastomoses
- small connections between portal v. tributaries of vena cava
- walls of organs
- body wall around umbilicus
- emergency route for blood if liver has blockages
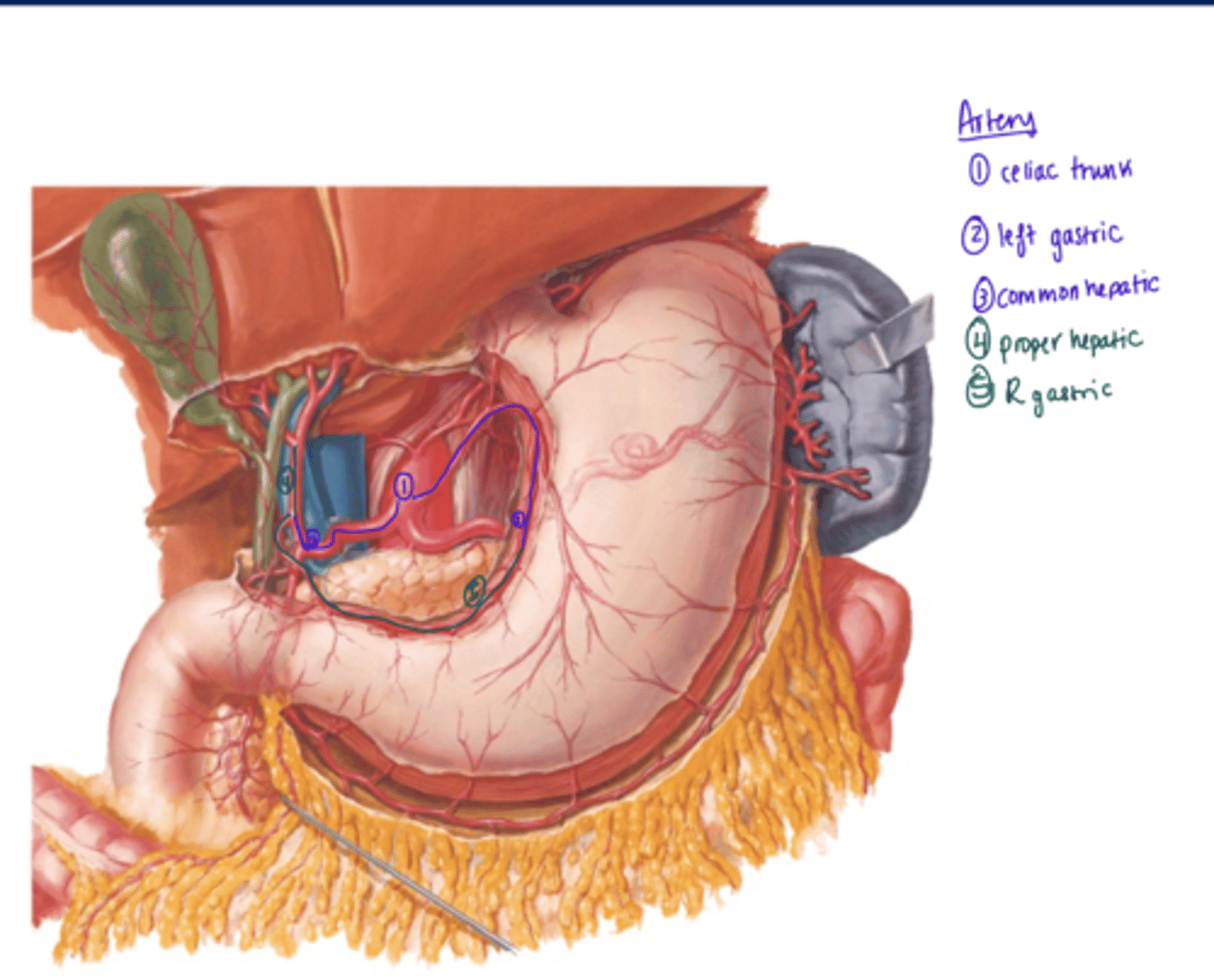
Flow of Blood in Gut (arteries)
1) Celiac Trunk
2) L Gastric
3) Common Hepatic
4) Proper Hepatic
5) R Gastric
Flow of Blood in Gut (veins)
1) L Gastric
2) R gastric
3) Hepatic Portal Vein
4) Splenic
5) SMV
6) IMV
all drain into IVC
Enteric Nervous System
-neurons located in gut
-innervate digestive organs
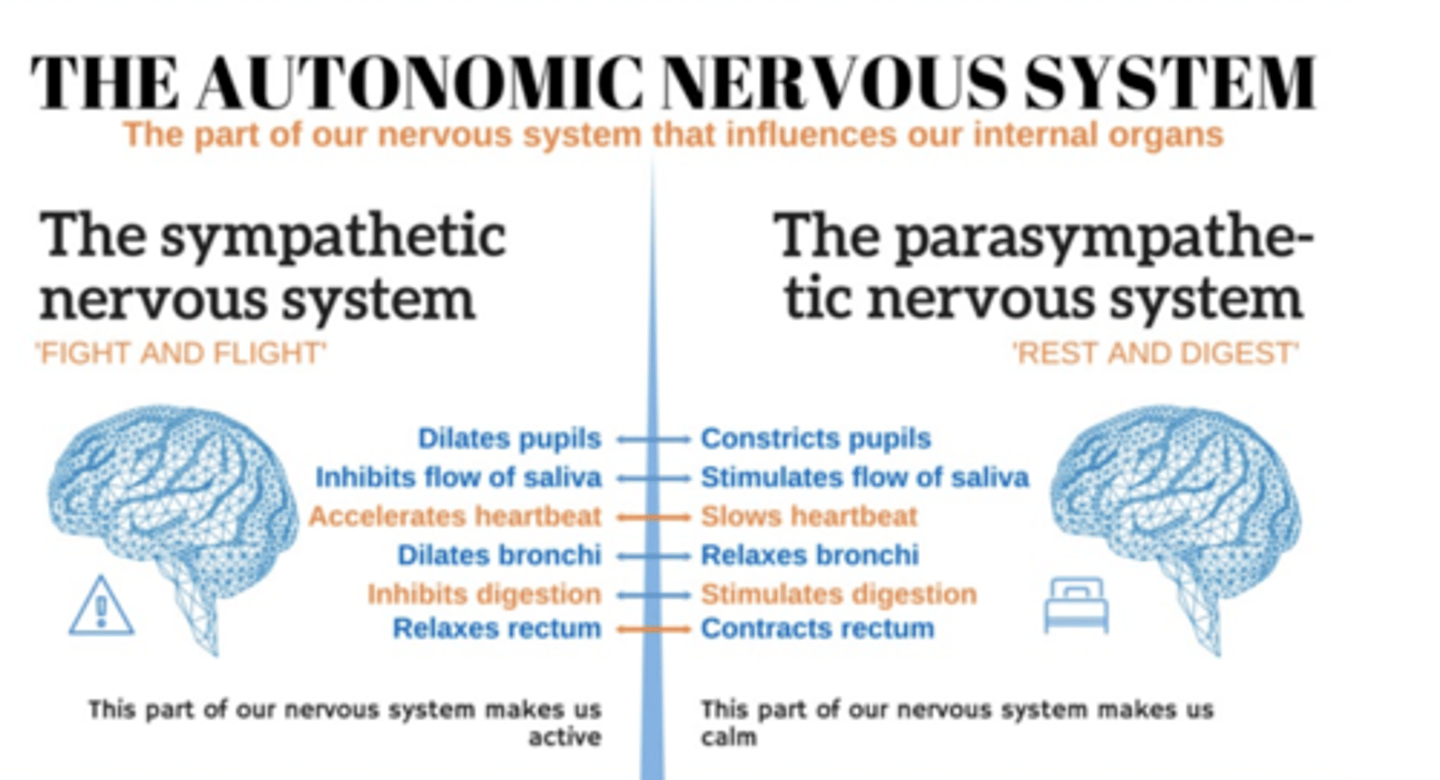
Autonomic Motor
-sympathetic and parasympathetic nervous system
Visceral Sensory
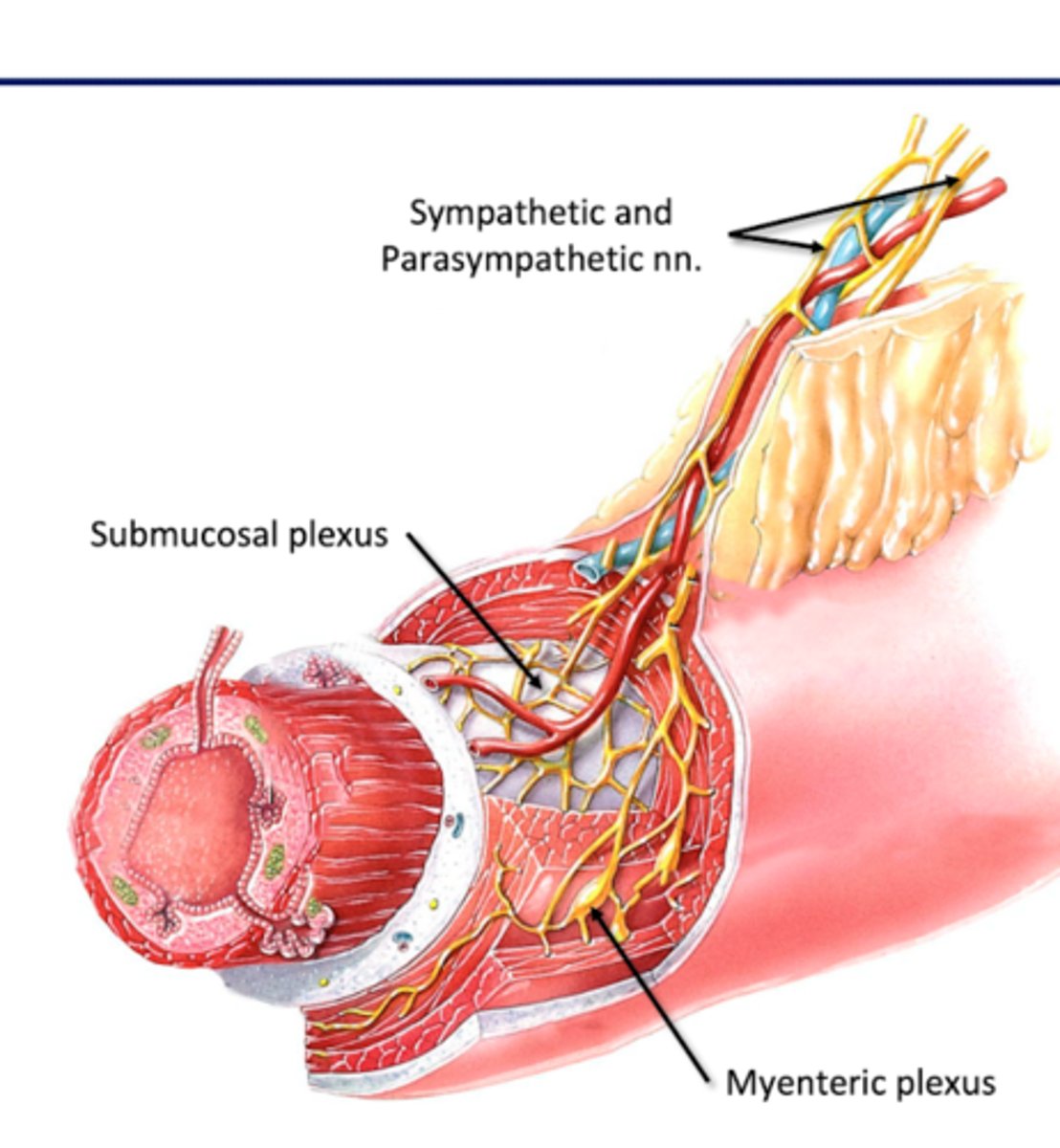
Submucosal (Meissner's) Plexus
Where: Submucosa (connective tissue layer deep to mucous membrane)
For: mucosal glands
--secrete mucosa and digestive chemicals in lumen of GI tract
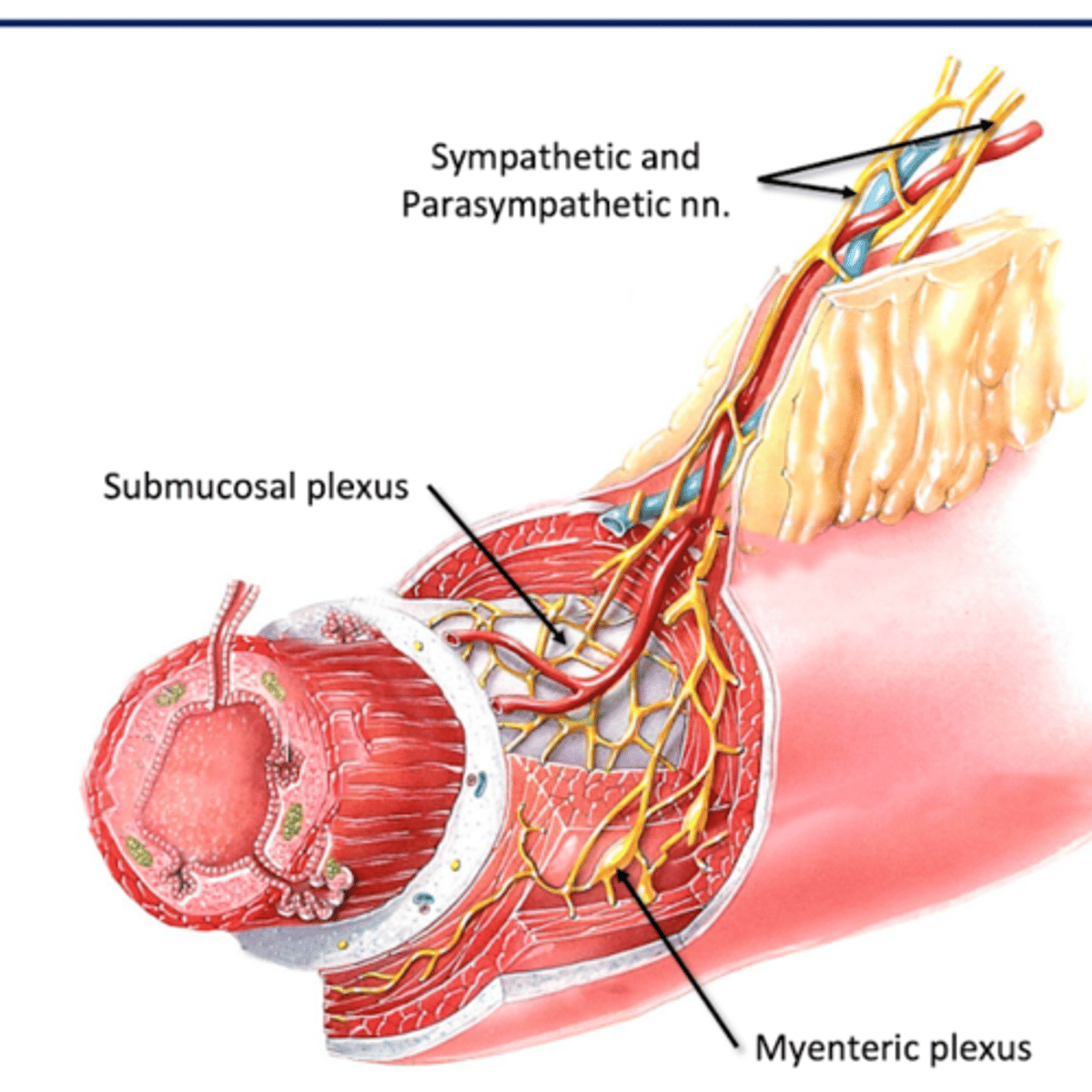
Myenteric (Auerbach's) Plexus
Where: Muscularis (muscular layer)
For: Gut Motility
-move contents through GI tract (peristalsis)
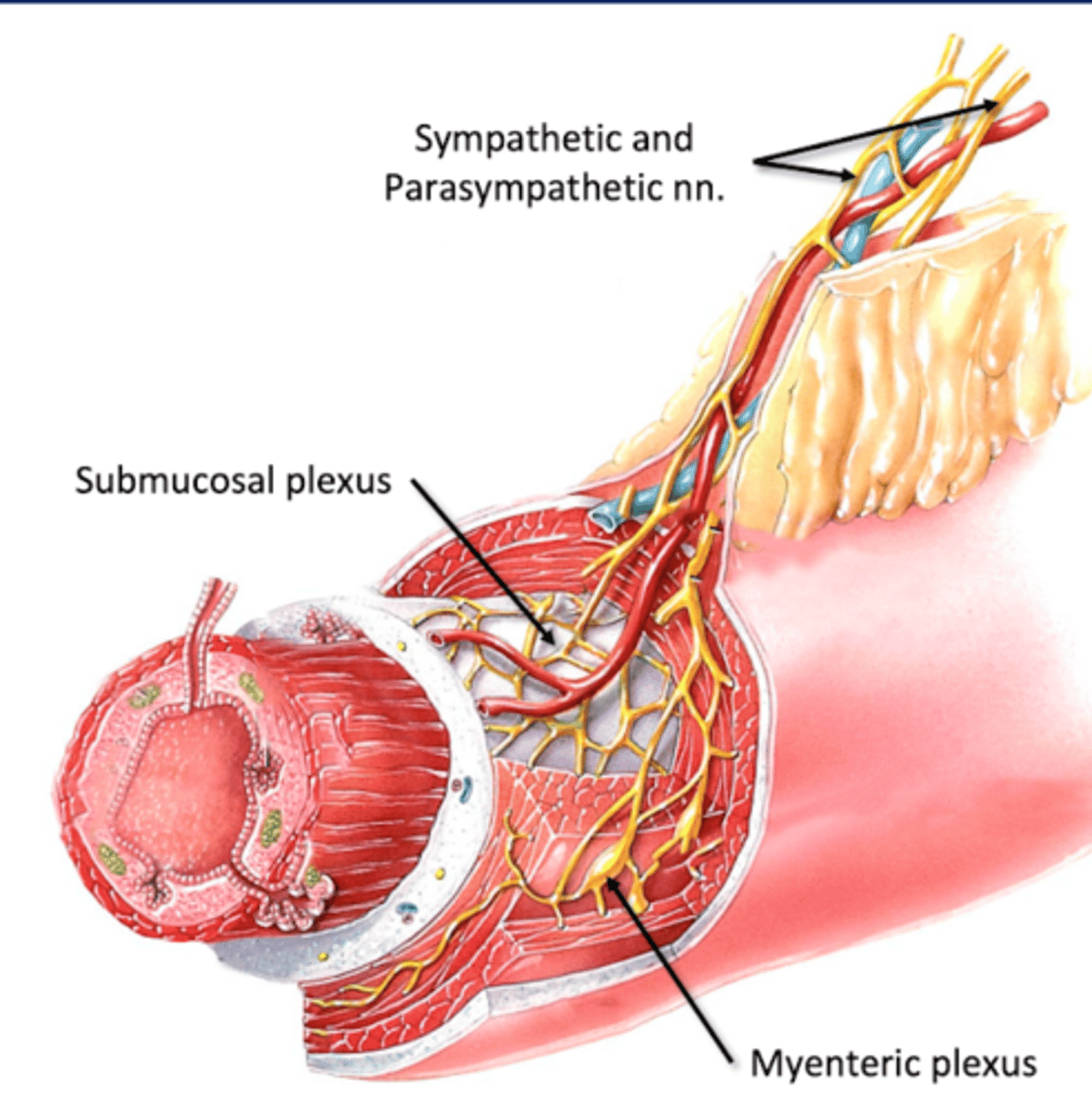
Sympathetic Supply of Gut
Thoracic Splanchnic nn. (greater and lesser)--> Synapse in prevertebral ganglia--> Foregut and Midgut Viscera
Lumbar Splanchnic nn--> synapse in prevertebral ganglis--> Hingut Viscera
-all symp innervation originates in spinal cord and travels to symp chain
-1st splanchic nn synapses at prevertebral ganglia
-2nd neuron follows blood vessels to target organ
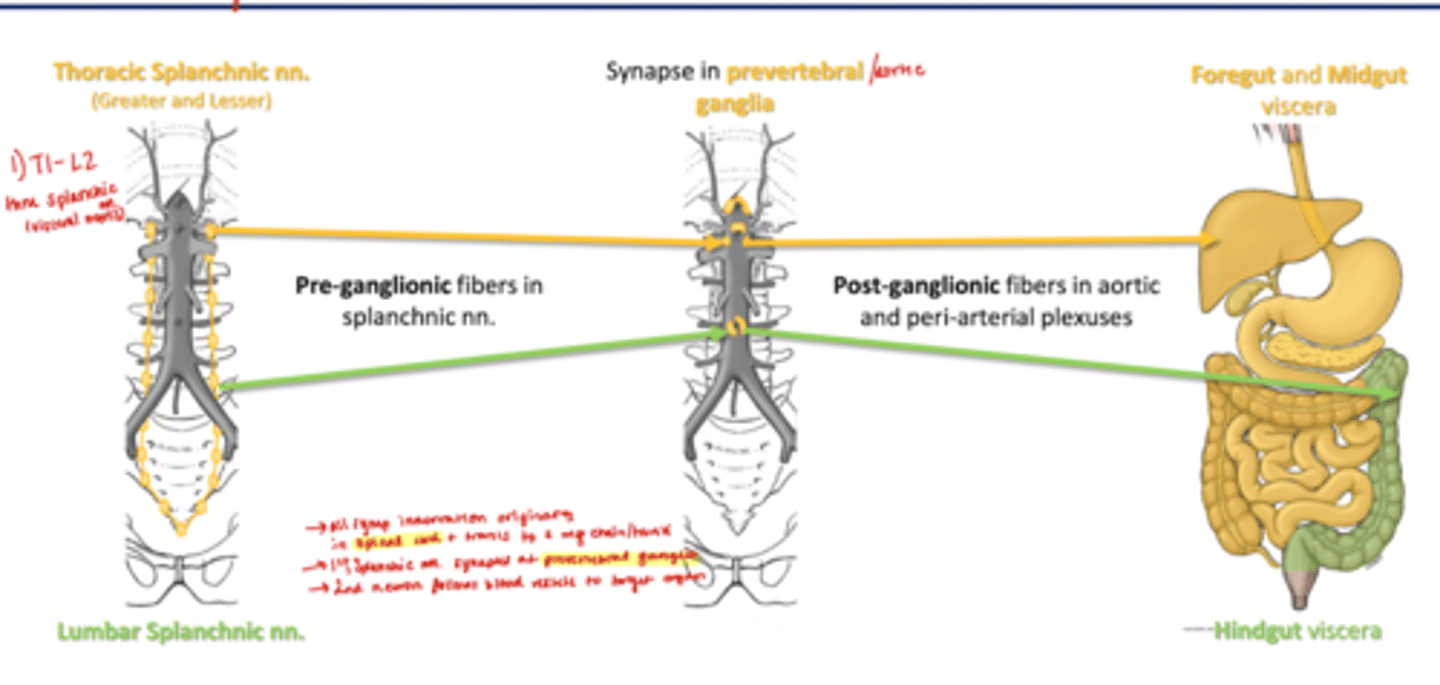
Sympathetic Innervation of Gut
*Inhibit Digestion by slow production of digestive juices*
Pre-ganglionic fibers in splanchnic nn
Post-ganglionic fibers in aortic and peri-arterial plexuses
Parasympathetic Supply of Gut
Posterior/Anterior Vagal Trunks (Vagus nerve)--> synapse in enteric ganglia--> foregut and midgut viscera
Pelvic Splanchnic nn (S2-4) --> synapse in enteric ganglia --> hingut viscera
-Vagus nerves carries preganglionic fibers for foregut/midgut; pelvic splanchnic for hindgut
-synapse at enteric ganglia within walls of small organ its innervating
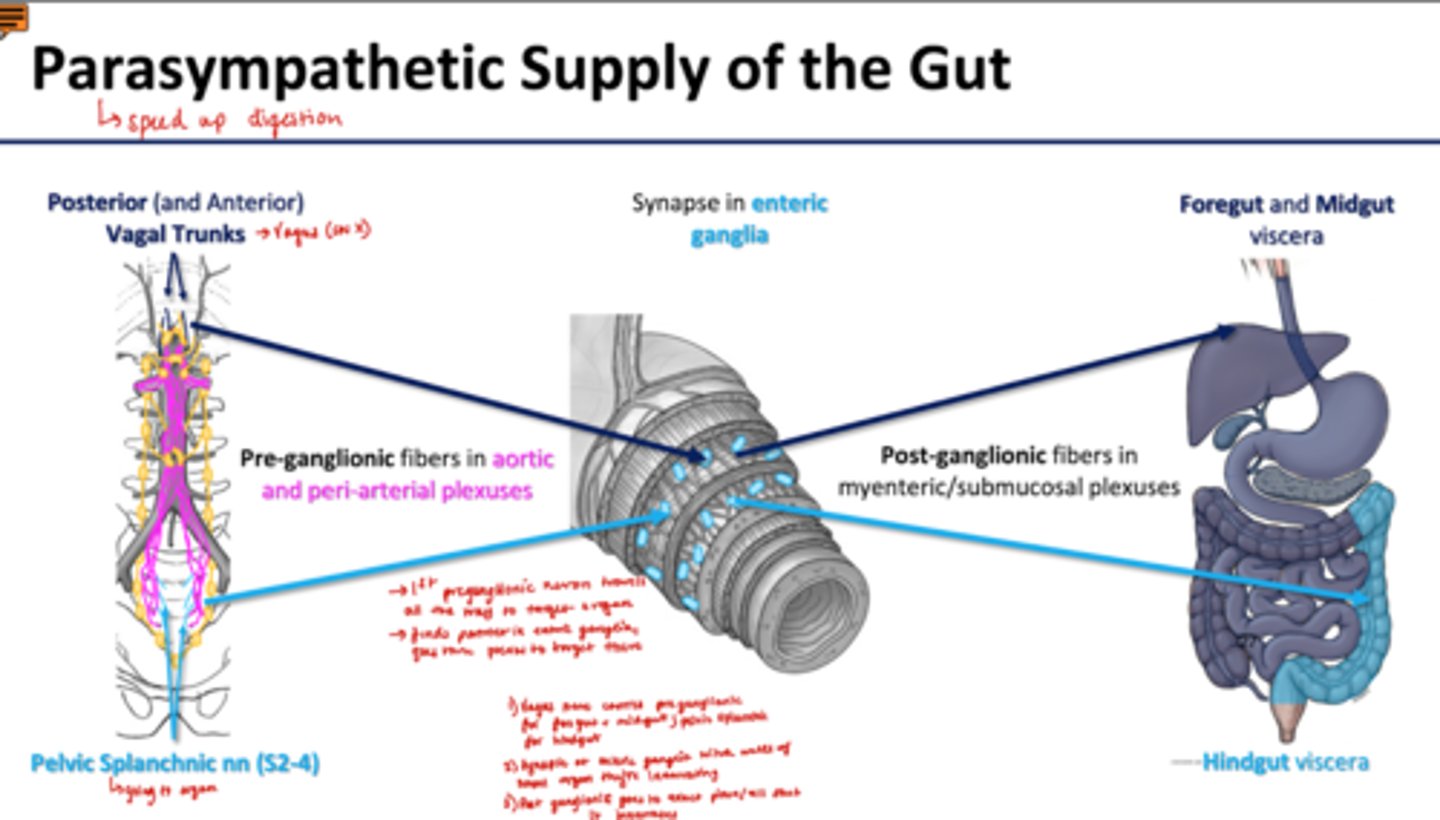
Parasympathetic Innervation of Gut
*speed up digestion, stimulates peristalsis*
Pre-ganglionic fibers in aortic and peri-arterial plexuses
Post-ganglionic fibers in myenteric/submucosal plexuses
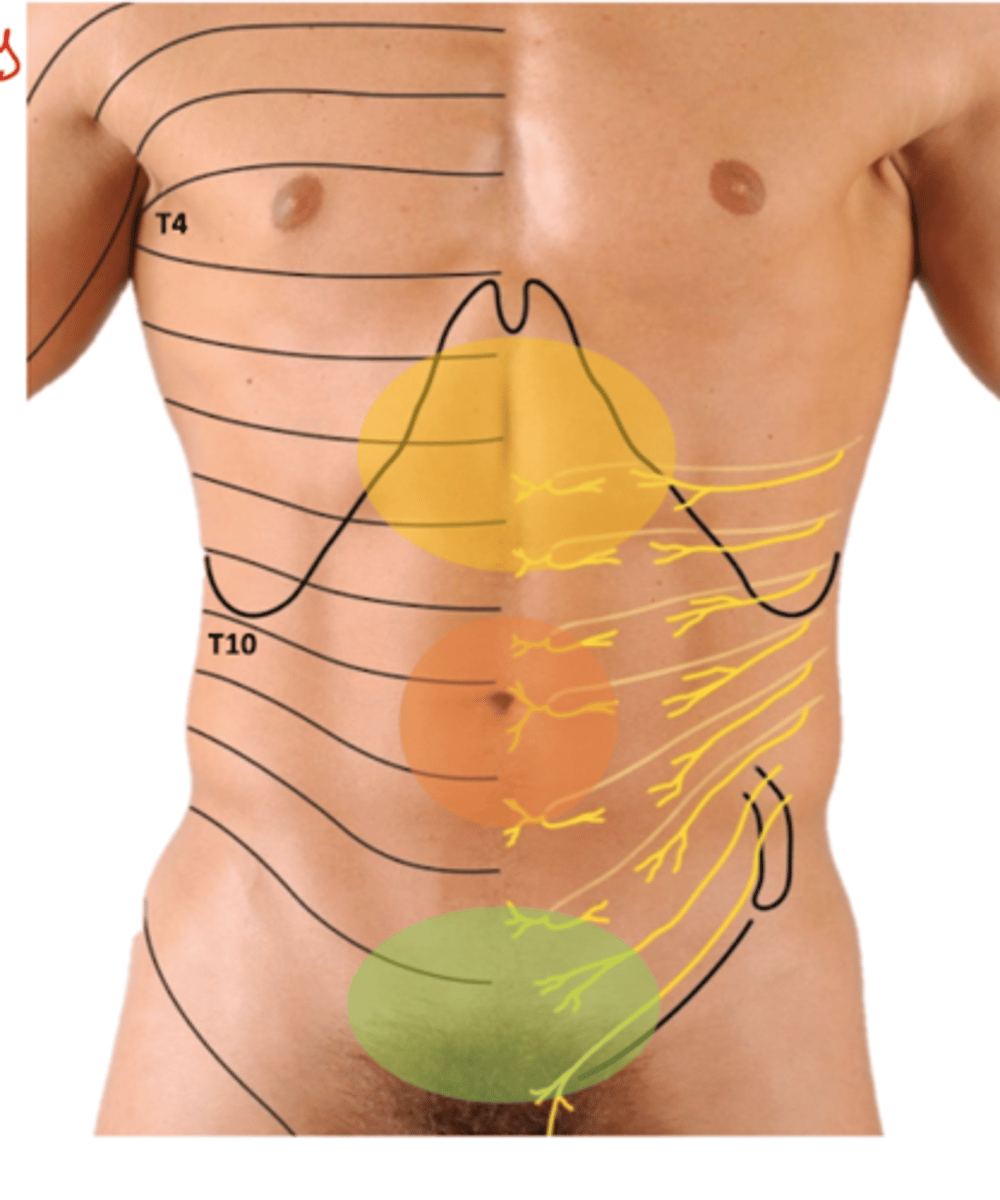
Sensory Innervation of Gut
-Enteric Reflex loops
-follow symp and parasymp pathways back to spinal cord
--synapse in same region as somatic sensory
Referred pain: visceral pain felt as somatic pain in body wall
-Foregut: epigastric
-Midgut: peri-umbilical
-Hingut: hypogastric
Layers of GI Tract
Superficial to Deep
1. Serosa/Adventitia
2. Muscularis
3. Submucosa
4. Mucosa
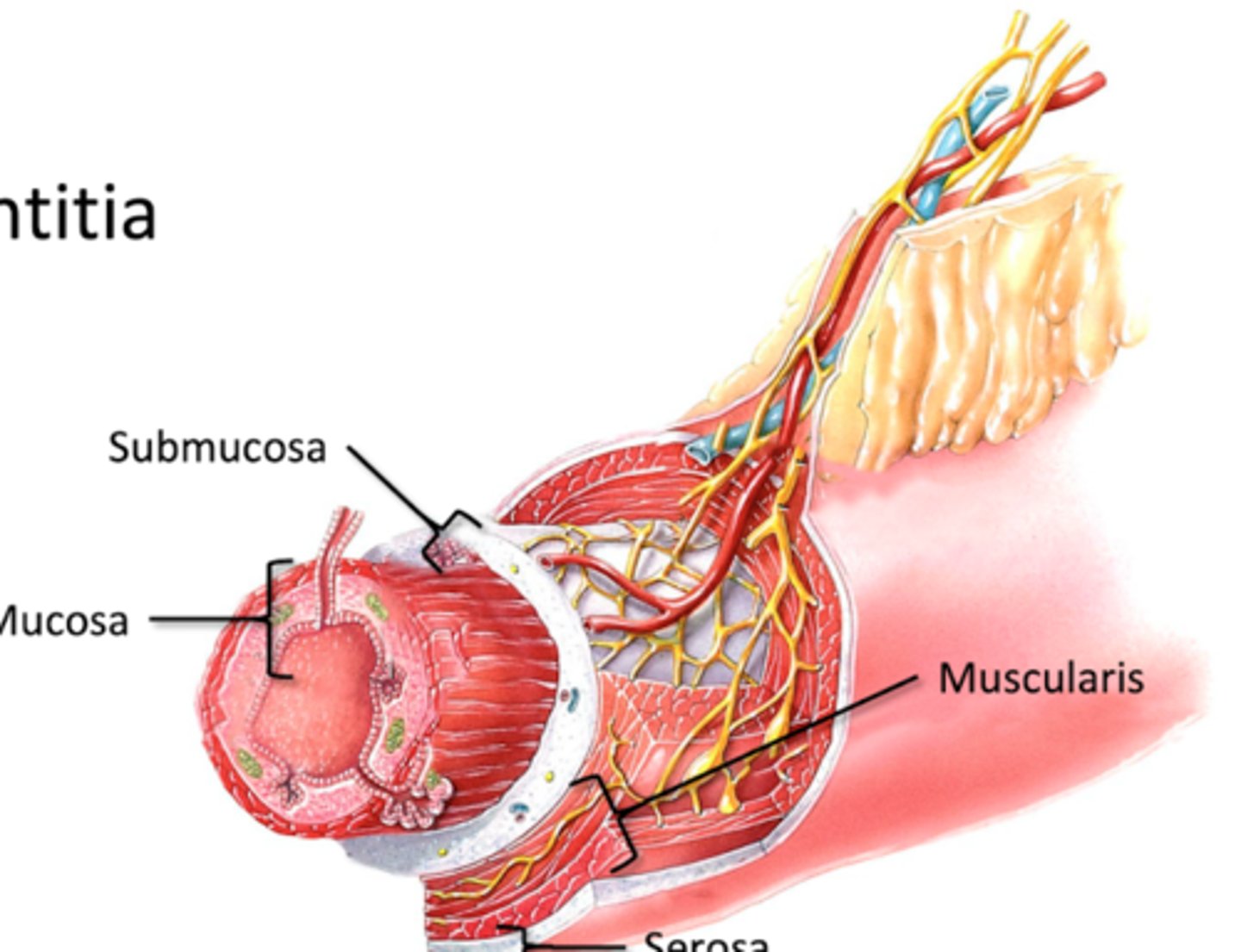
Mucosa
Deepest layer
-Epithelial Layer
-Areolar Connective Tissue
-Smooth muscle
Epithelial layer (mucosa)
Mouth/pharynx/esophagus: stratified squamous epithelium (protection)
Stomach/intestine: simple columnar epithelium (tight seal)
--replaced 5-7 days
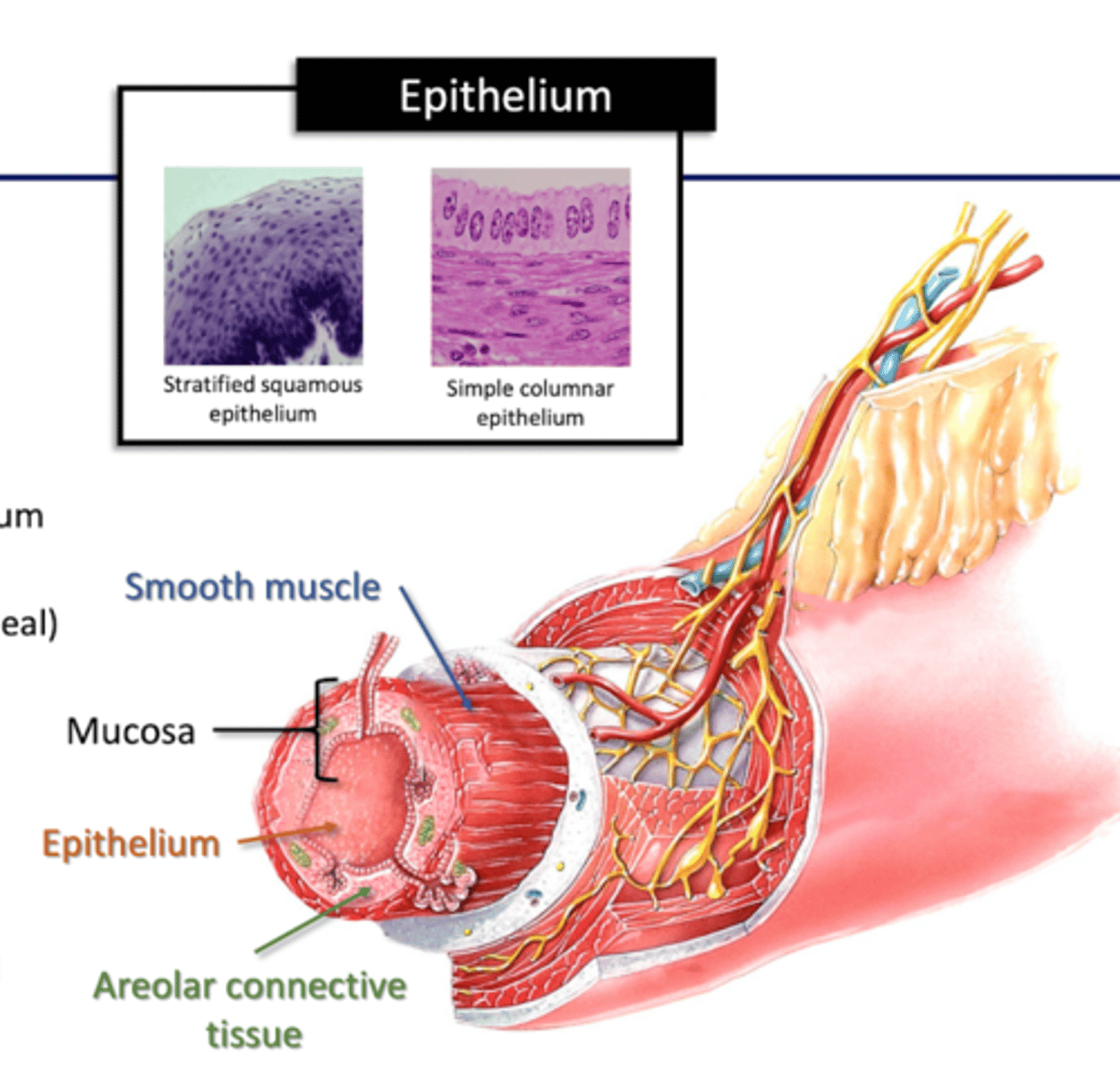
Areolar Connective Tissue and Smooth muscle (mucosa)
Areolar: blood and lymphatic vessels (MALT)
Muscle: -folds mucosa
-expose absorptive cells to GI contents
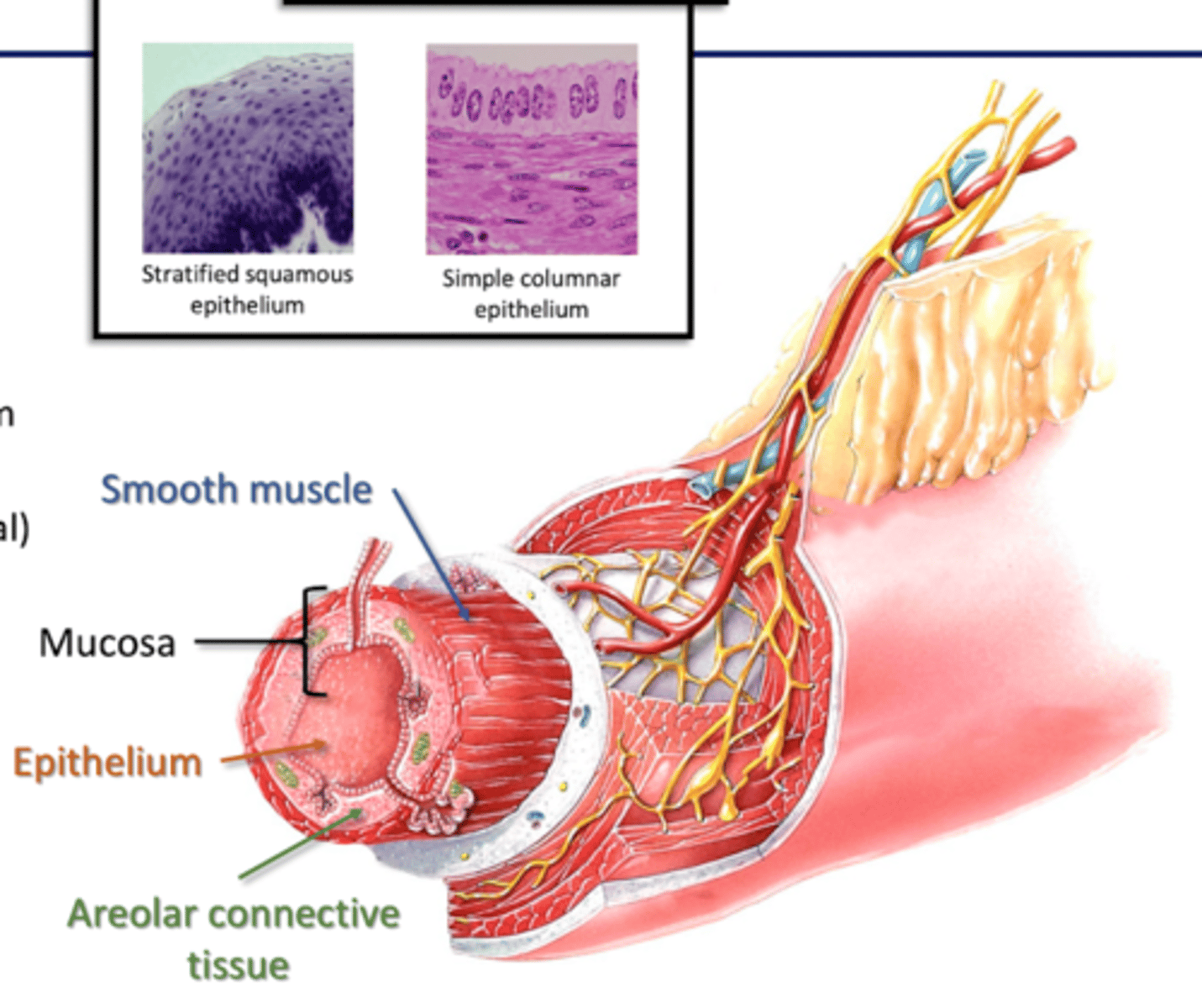
Submucosa
-Connective Tissue Layer (collagen, nerves, blood vessels)
-Submucosal Plexus
Submucosal Plexus (submucosa)
part of enteric nervous system
-Autonomic neurons
--Symp (splanchnic nn)
--Parasymp (Vagus)
-Enteric neurons
-regulates mucosal movement (smooth muscle), vasoconstriction, secretory glands of mucosa
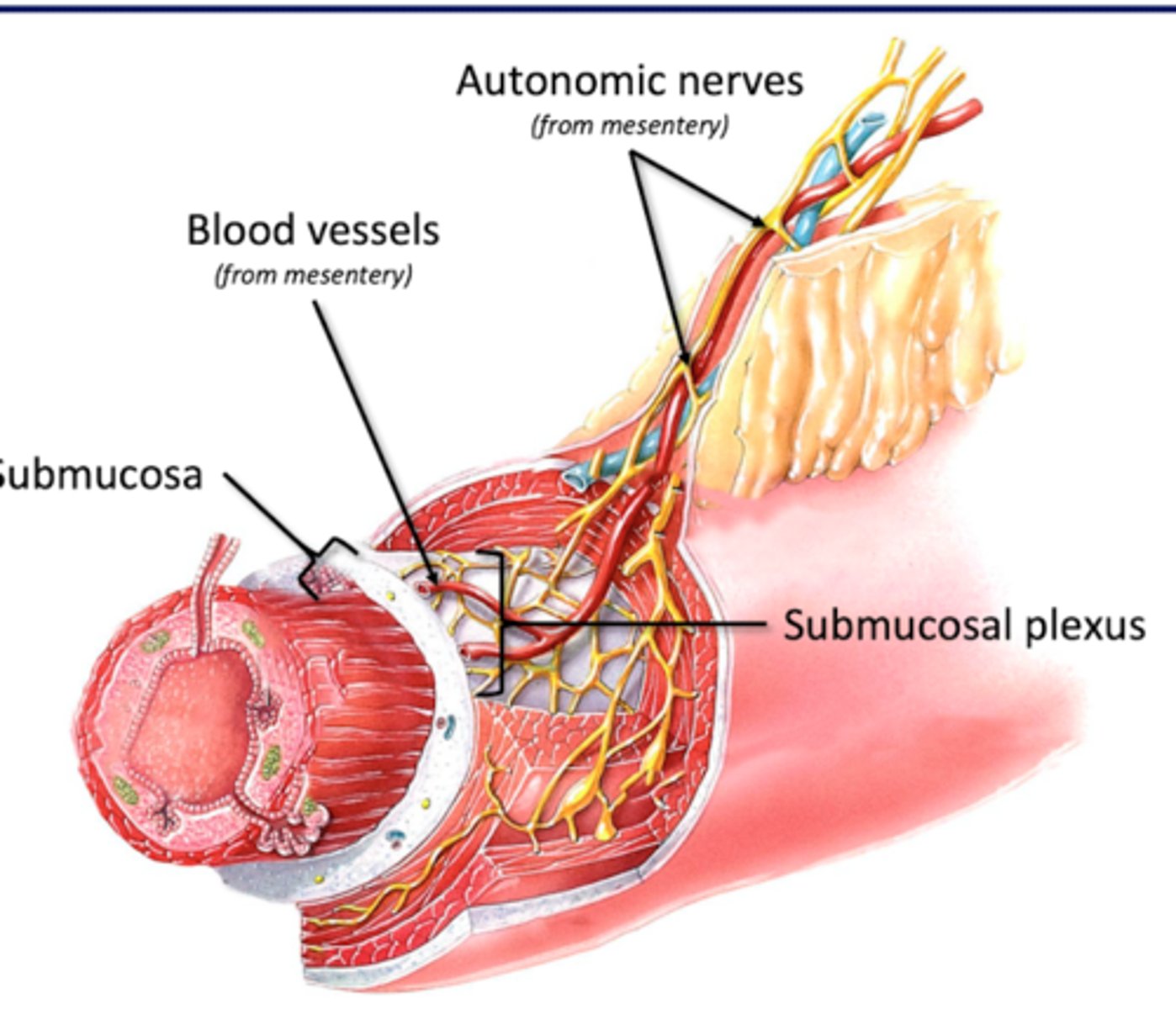
Muscularis
Upper GI tract: Mouth/pharynx/prox 2/3 esophagus
--skeletal muscle (swallowing)
Lower GI tract: Smooth muscle
-Longitudinal fibers (superficial): tube shorter to breakdown contents
-Circular Fibers (deep): narrow tube to propel contents
**does peristalsis**
Myenteric Plexus (muscularis)
Part of enteric nervous system
--autonomic (symp and para)
--enteric
-Control gut motility (smooth muscle)
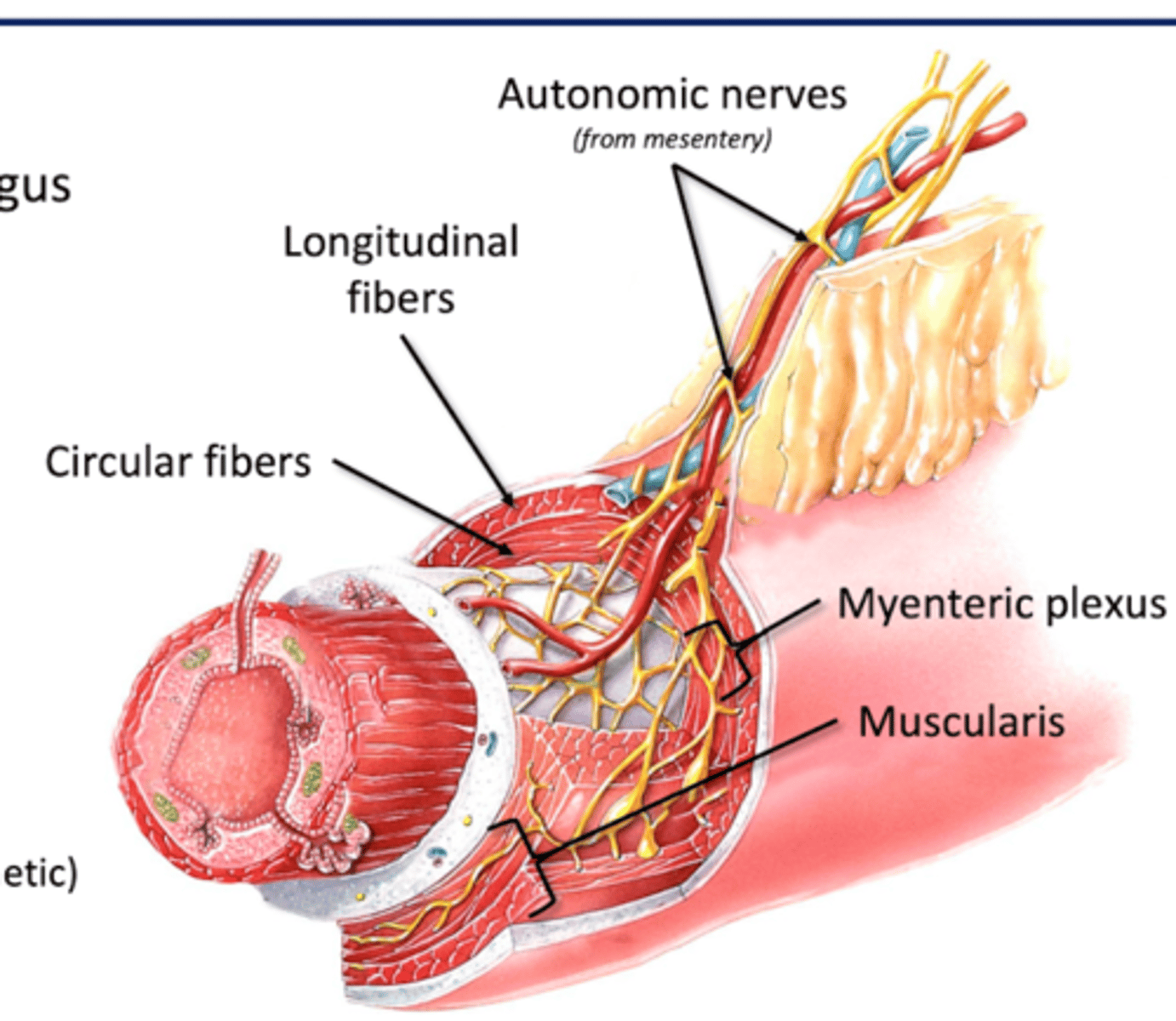
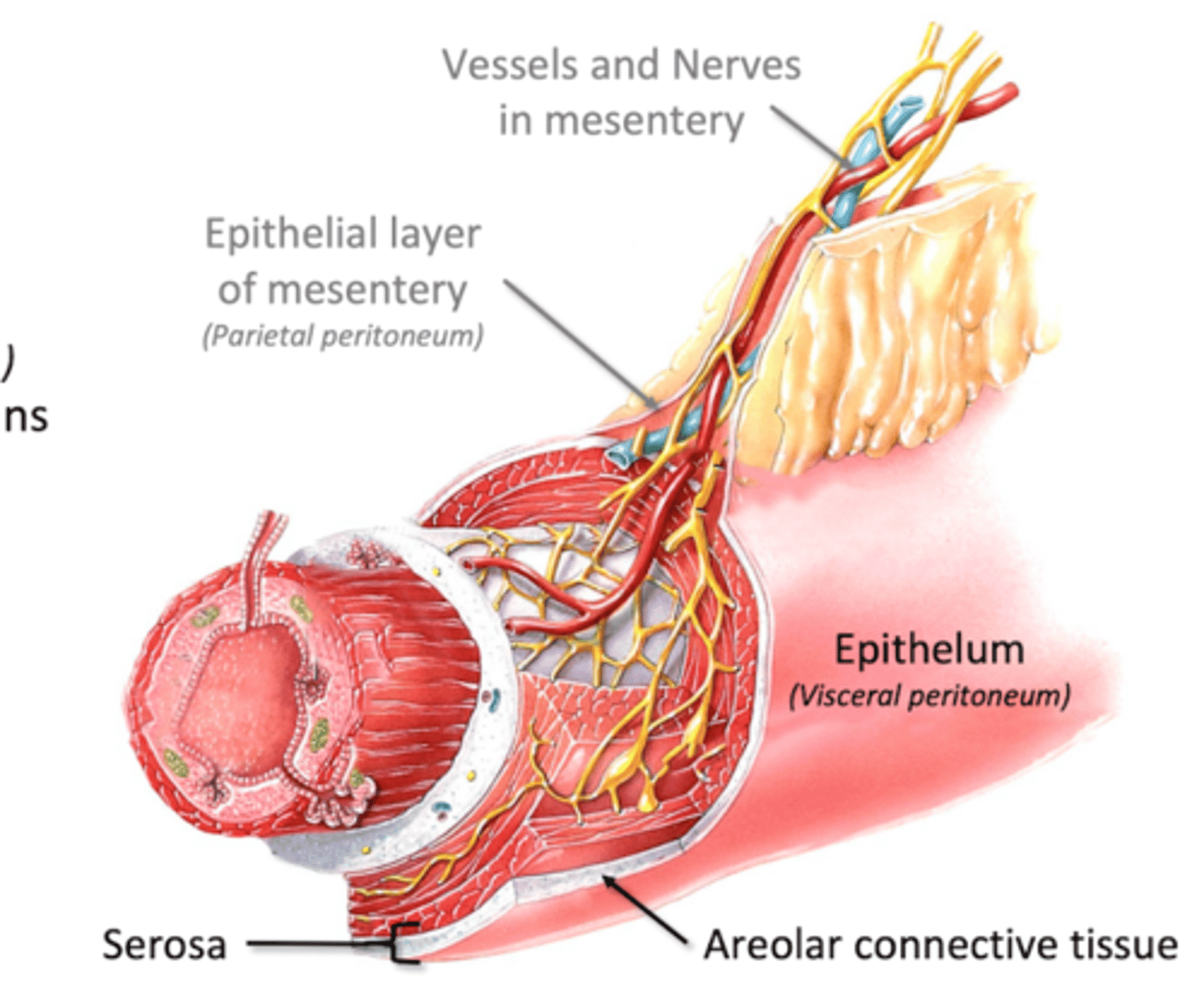
Serosa/Adventitia
Serosa: Serous membrane surrounding GI organs
-areolar connective tissue
-epithelium (visceral peritoneum): lubricates surfaces of GI organs
Adventitia: single layer of areolar connective tissue
-no epithelium
-found in esophagus and rectum
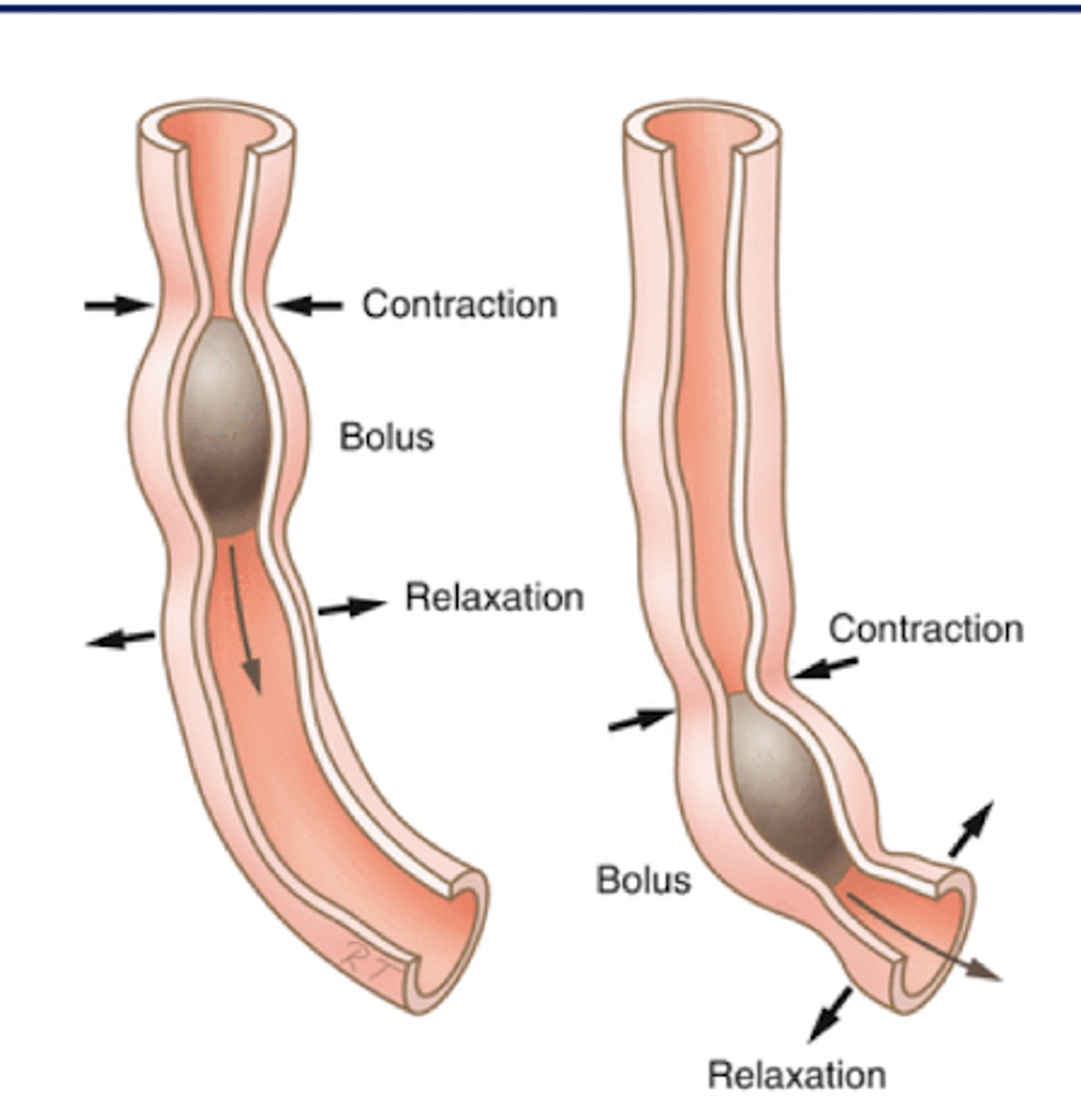
Circular Fibers of GI tract
Propel bolus
-contract posterior
-relax anterior
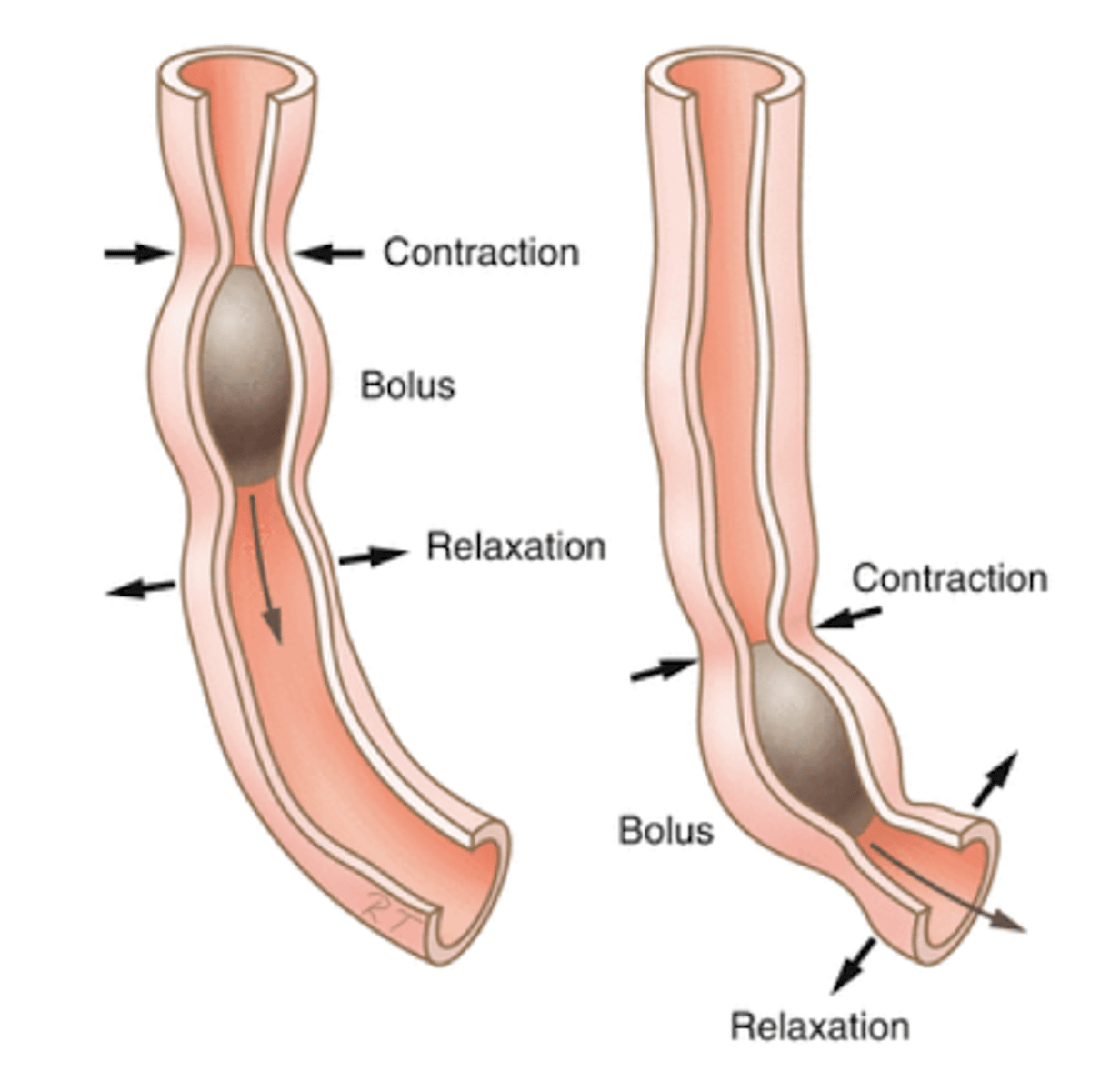
Longitudinal Fibers of GI Tract
Shorten Tract
-force more circular fibers into a smaller space
-reduces force individual circular fibers must produce
Peritoneal Sac
Larges serous membrane in body (makes serous fluid)
Lines:
-walls of abdominal cavity
-walls of abdominal organs
-blood vessels and nerves traveling between
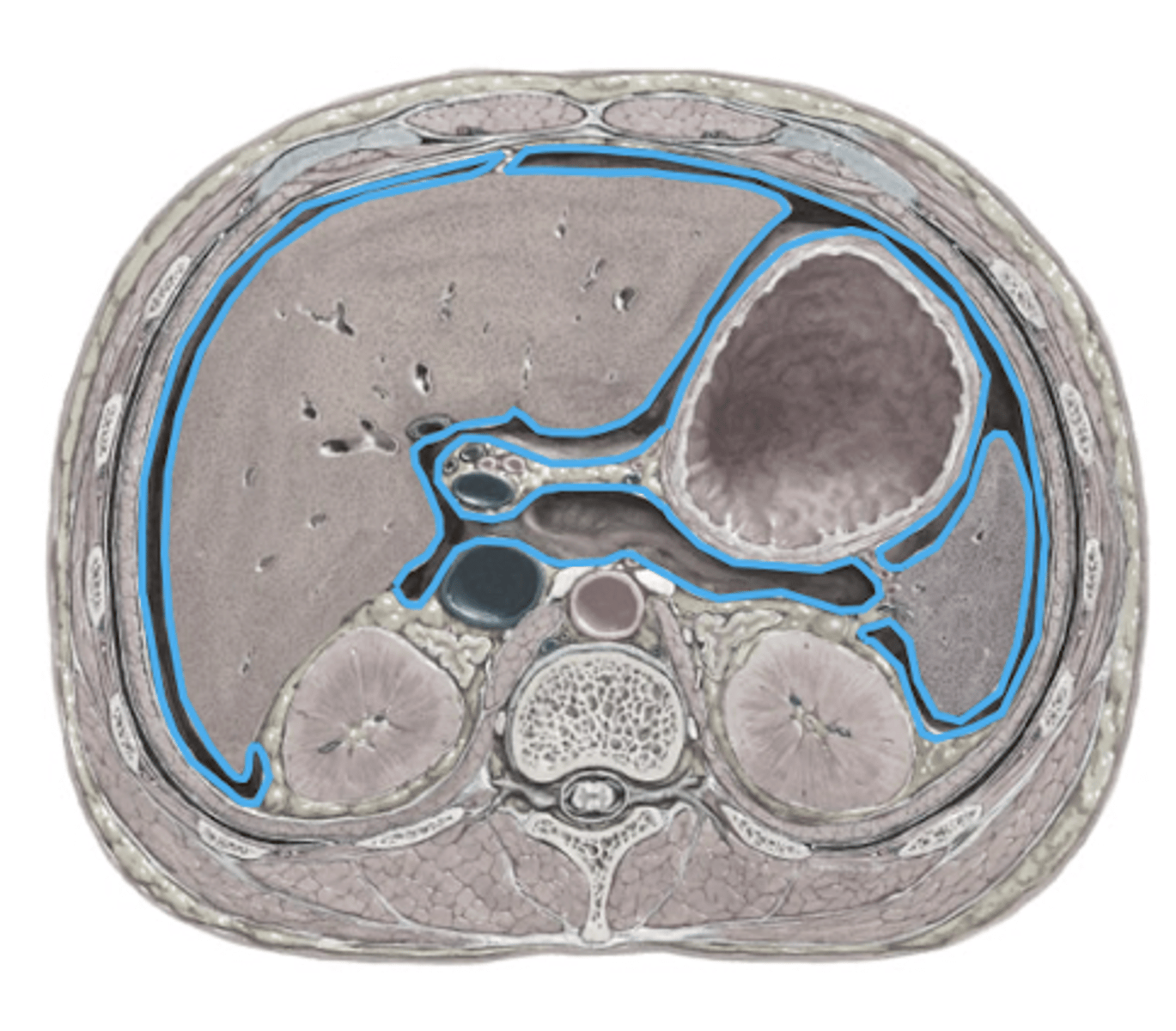
Peritoneal Sac Functions
Supports abdominal organs
-surrounds and adheres to surface
-tethers to posterior abdominal wall
Allows contraction of smooth muscle without gross movements
-prevents twisting and knots
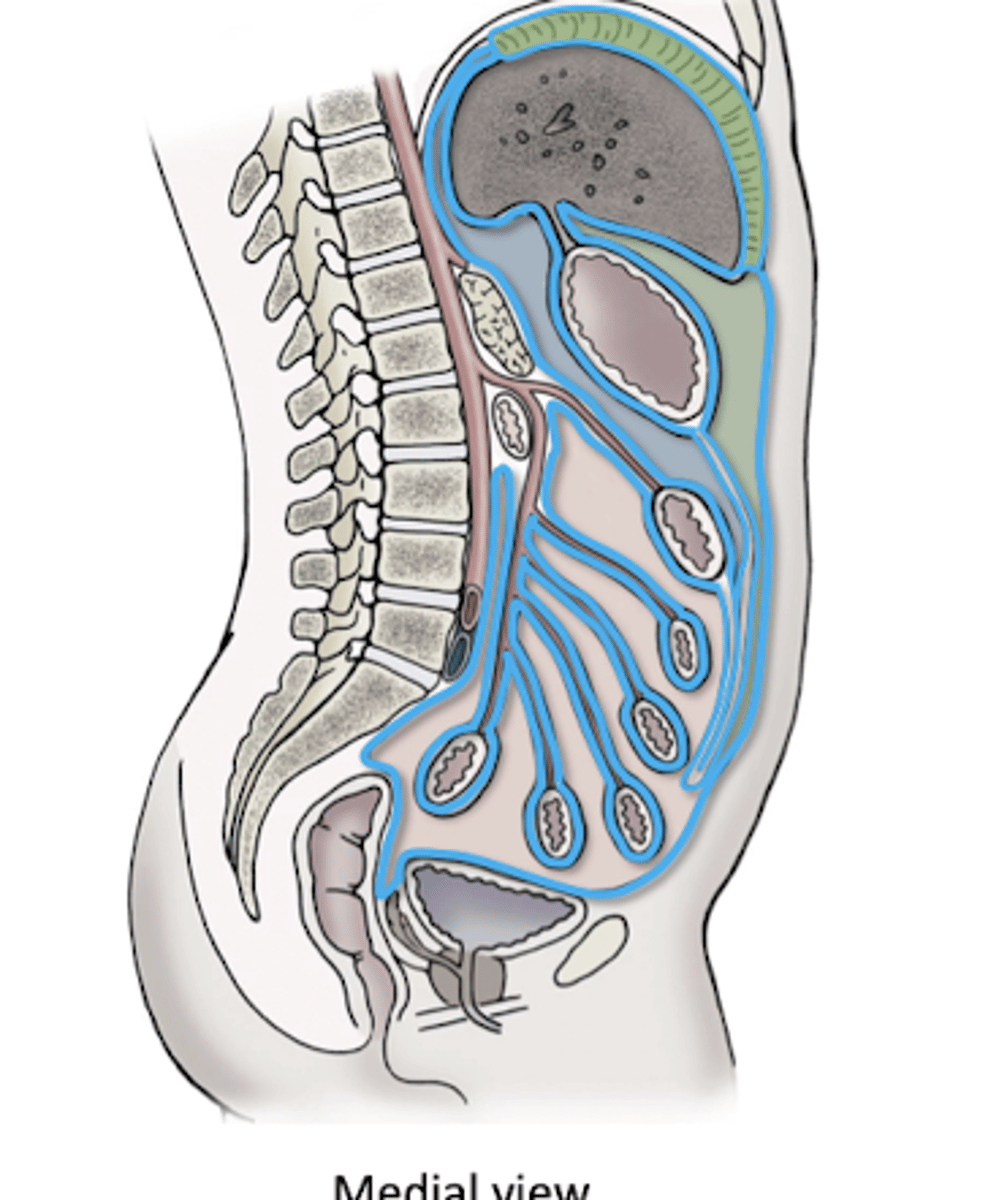
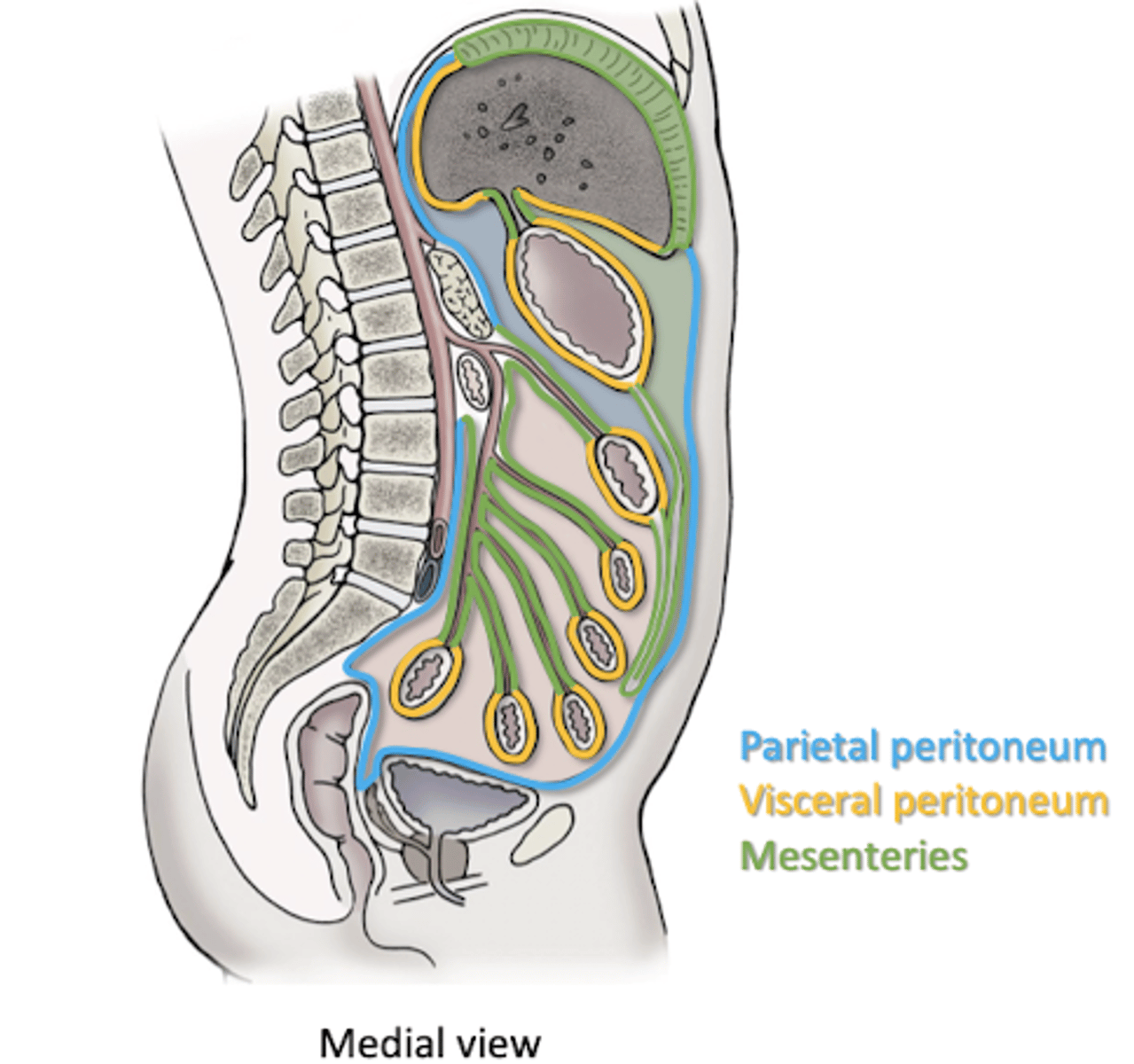
Division of Peritoneal Sac
Visceral Peritoneum
-wall of organs
Parietal Peritoneum
-abdominal wall
Mesentery/Ligament
-tethers wall to organ
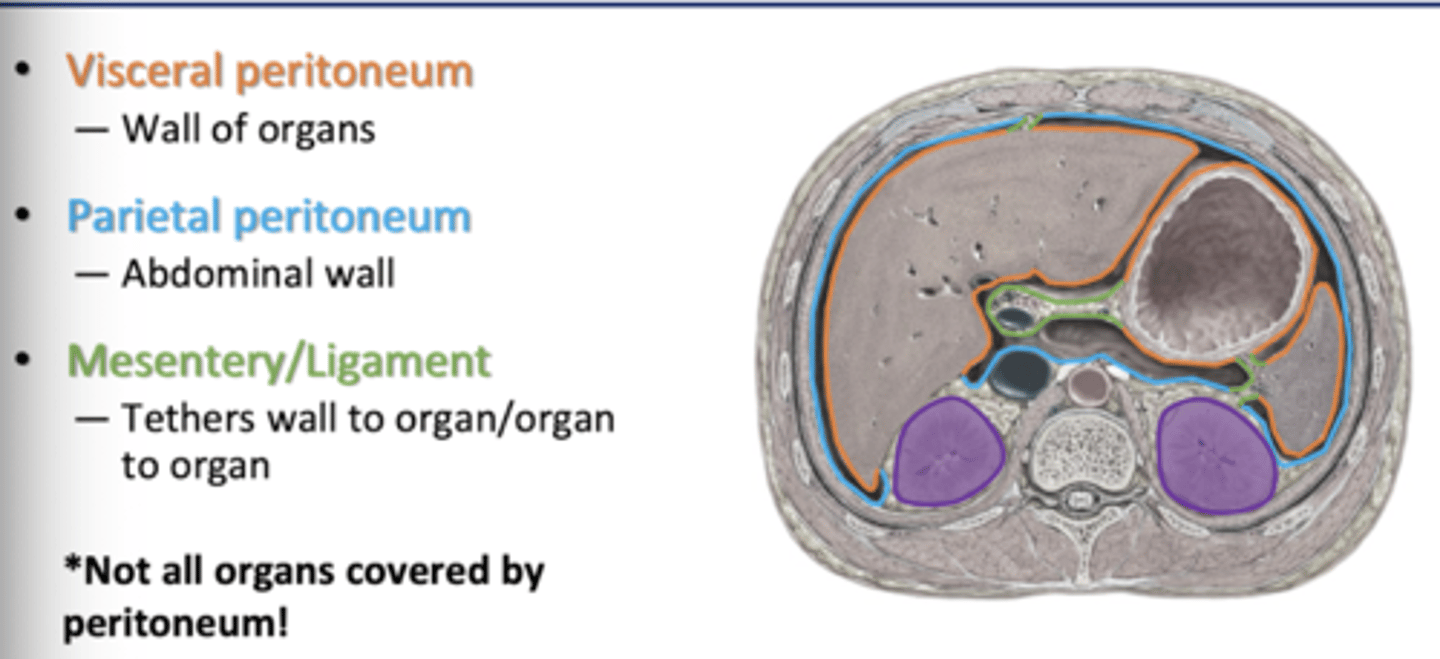
Retroperitoneal
posterior to peritoneal sac
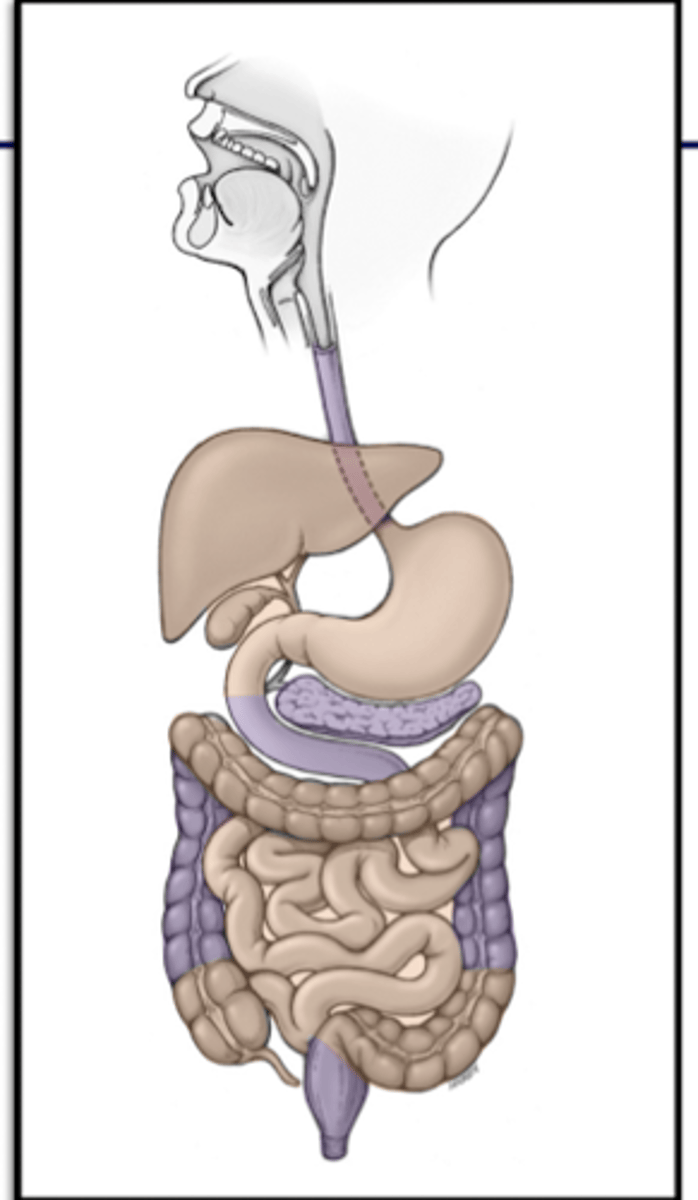
Intraperitoneal
-protrudes into peritoneal cavity
-walls covered by visceral peritoneum
-has a mesentery
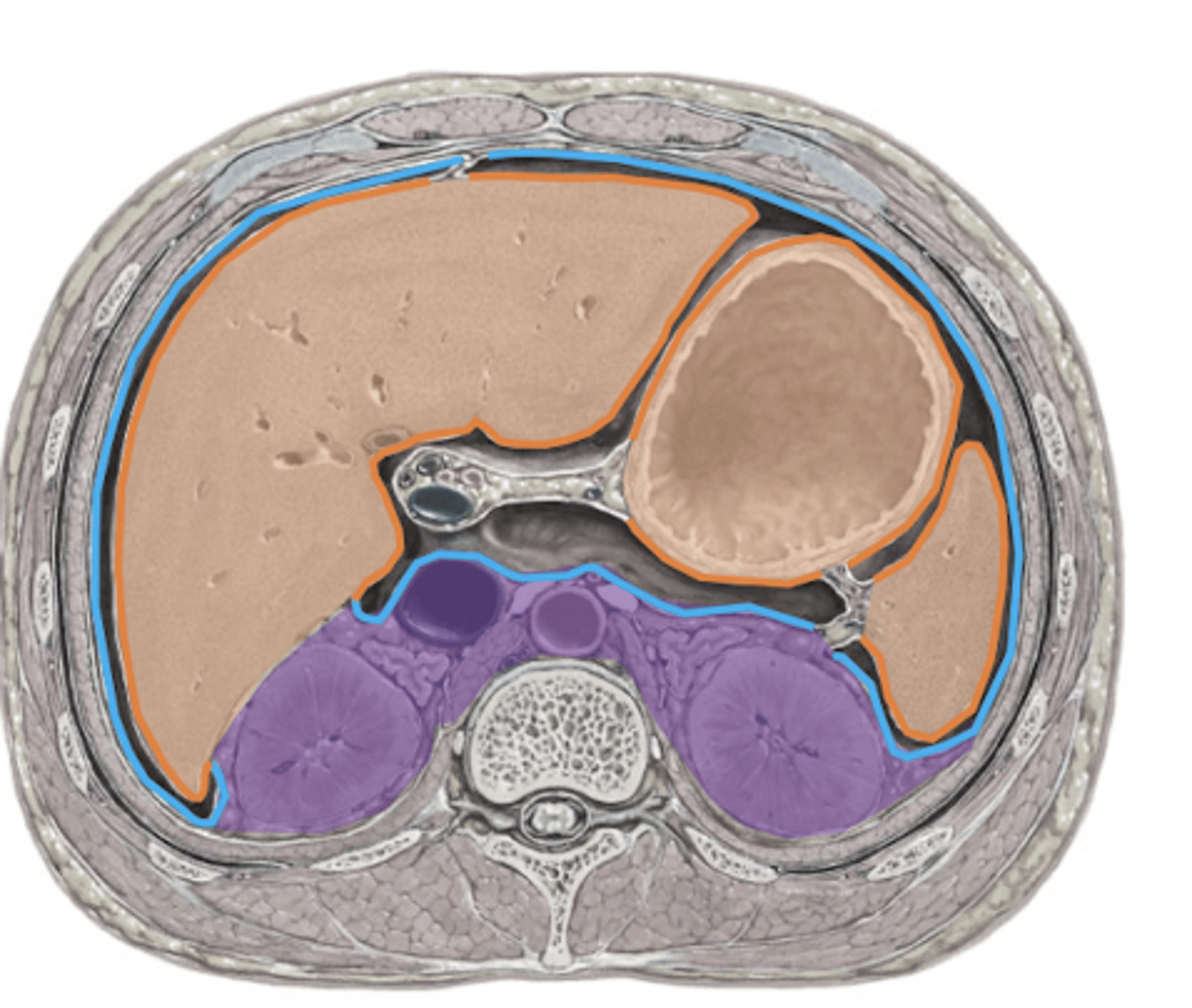
Organs that are Retroperitoneal
SADPUCKER
S-suprarenal organs (adrenals)
A- aorta and IV
D- duodenum (distal 3/4)
P-pancreas (head&body)
U-ureters and bladder
C-colon (ascending and descending)
K- kidneys
E-esophagus
R- rectum/anal canal (mid distal)
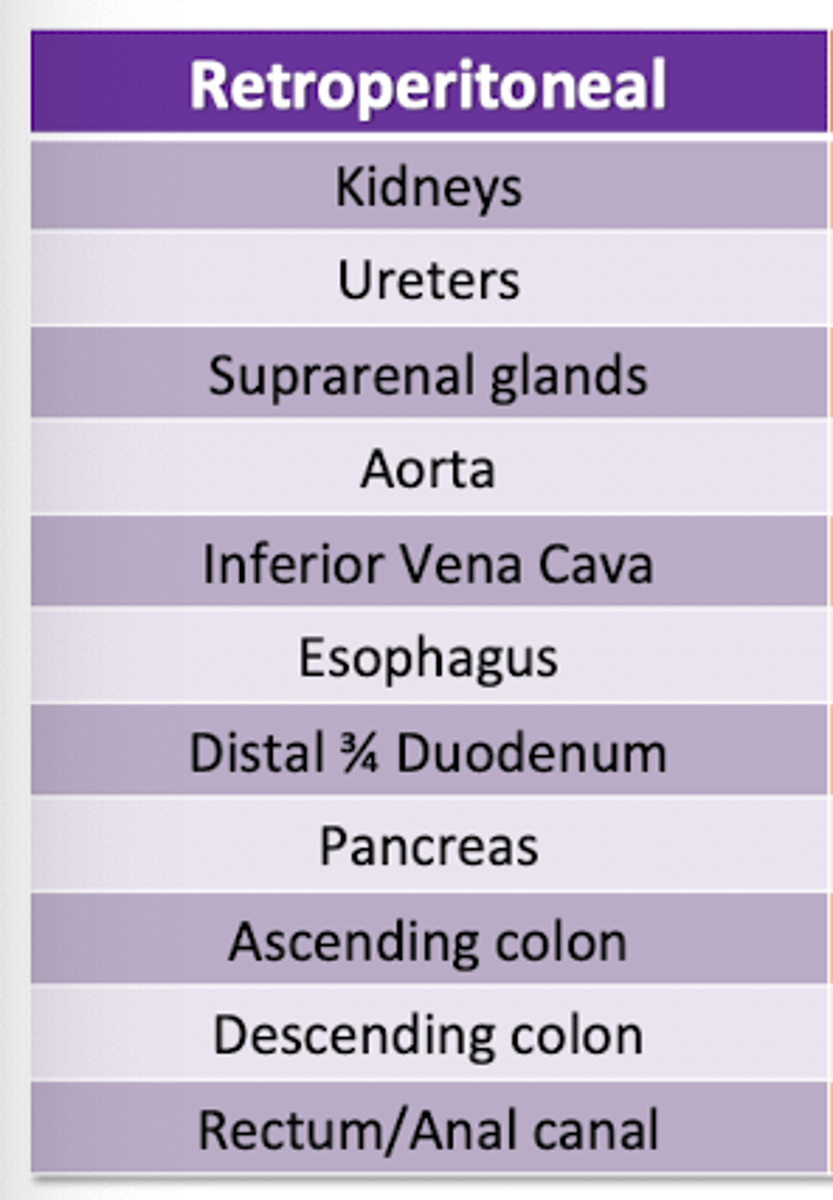

Organs that are Intraperitoneal
Stomach
Liver
Gallbladder
Spleen
Duodenum (prox 1/4)
Jejunum
Ileum
Cecum
Appendix
Transverse Colon
Sigmoid Colon
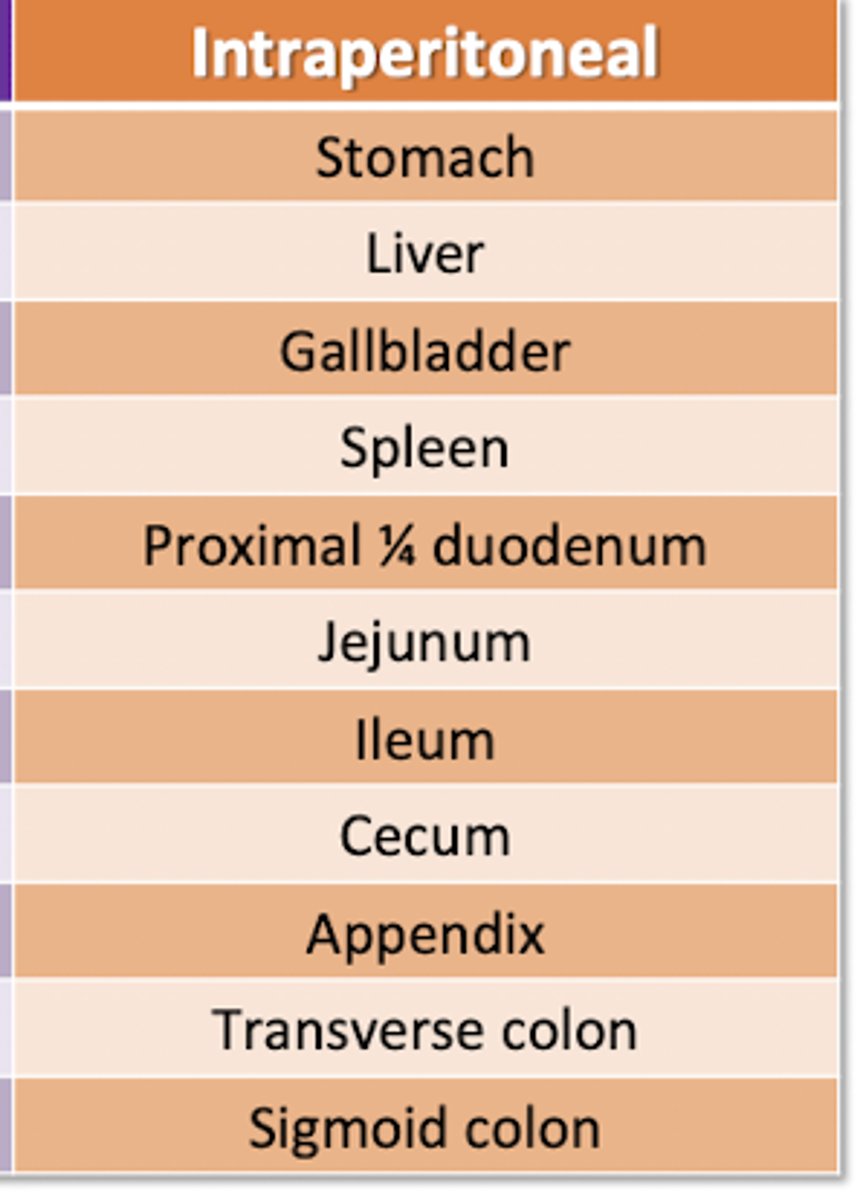

Mesenteries
2 layers of peritoneum
-tether abdominal organs to abdominal wall and each other
*passageway to organs for blood vessels, nerves, lymph vessels*
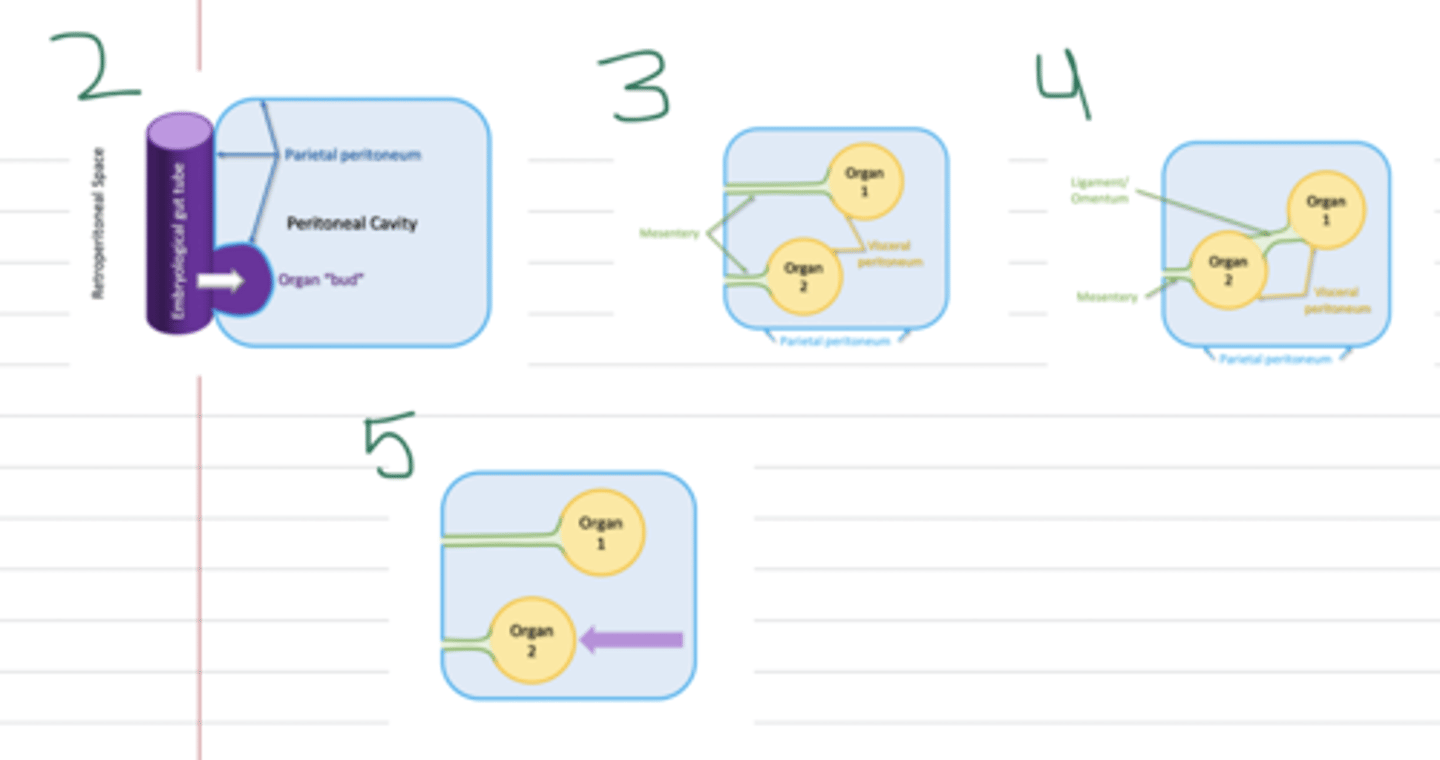
Formation of a Mesentery
1) All GI organs begin developing posterior to the peritoneal sac
2) Organs move anteriorly and press into the sac during development
3) Peritoneum pinches closed posterior to advancing organs
4) Organs rotate and mesenteries may fuse during development
5) Organs may move posteriorly after developing a mesentery
secondary retroperitoneal
organs that move posteriorly after developing a mesentery
-retain the same blood, lymph, and nerve supply as intraperitoneal
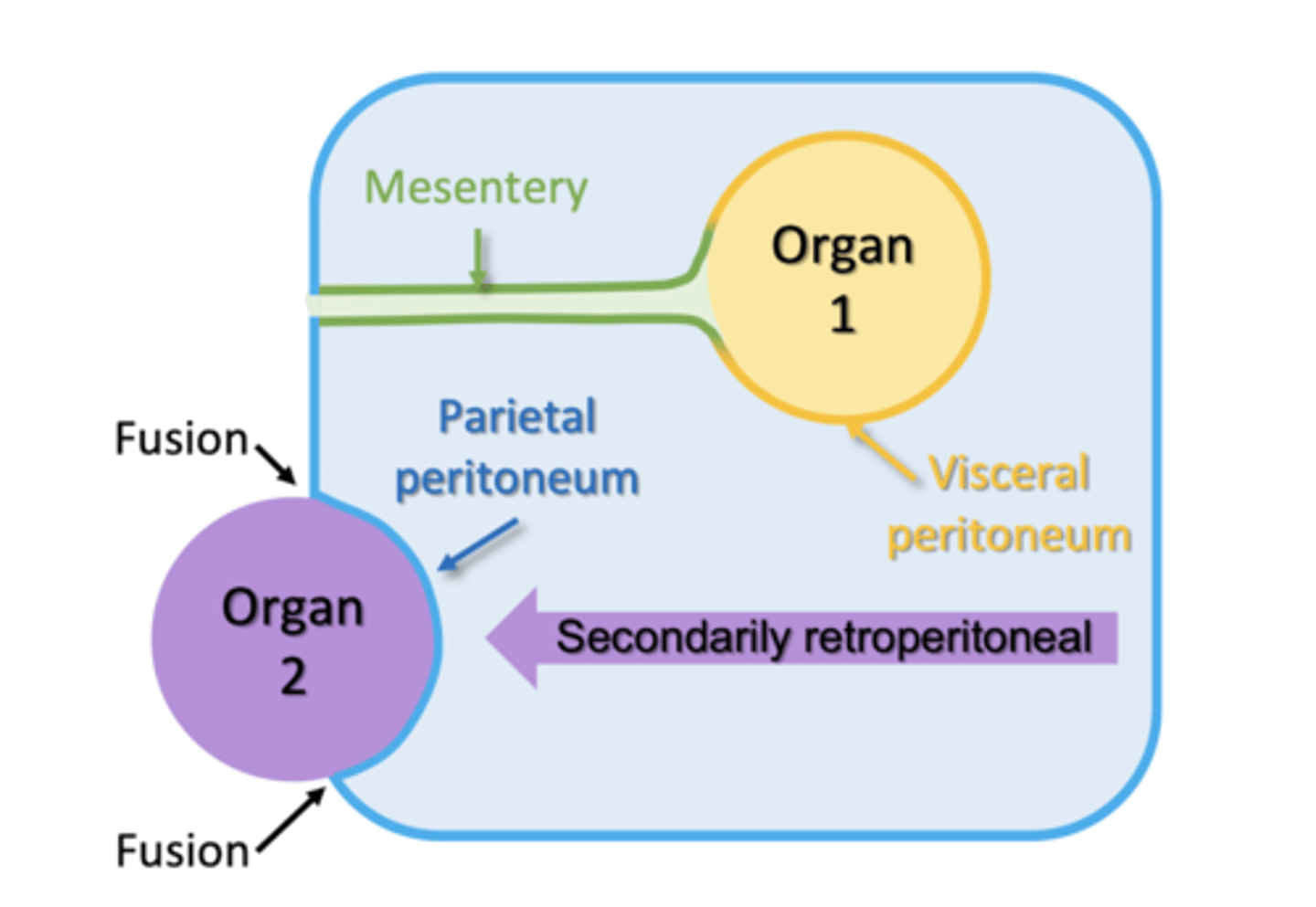
Organs that are secondary retroperitoneal
Distal 3/4 duodenum
Pancreas
Ascending Colon
Descending Colon
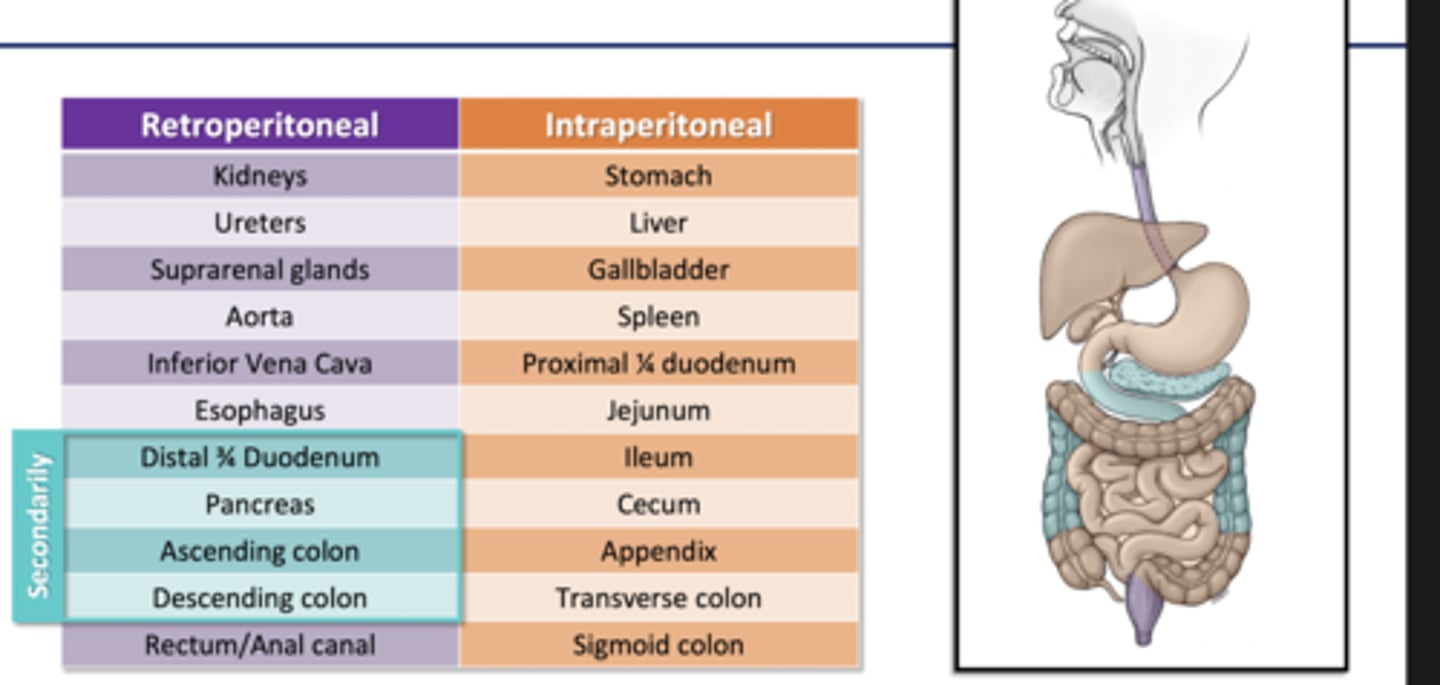
major peritoneal folds
1) the mesentery
2) mesocolons (transverse and sigmoid)
3) greater omentum
4) lesser omentum
5) falciform ligament
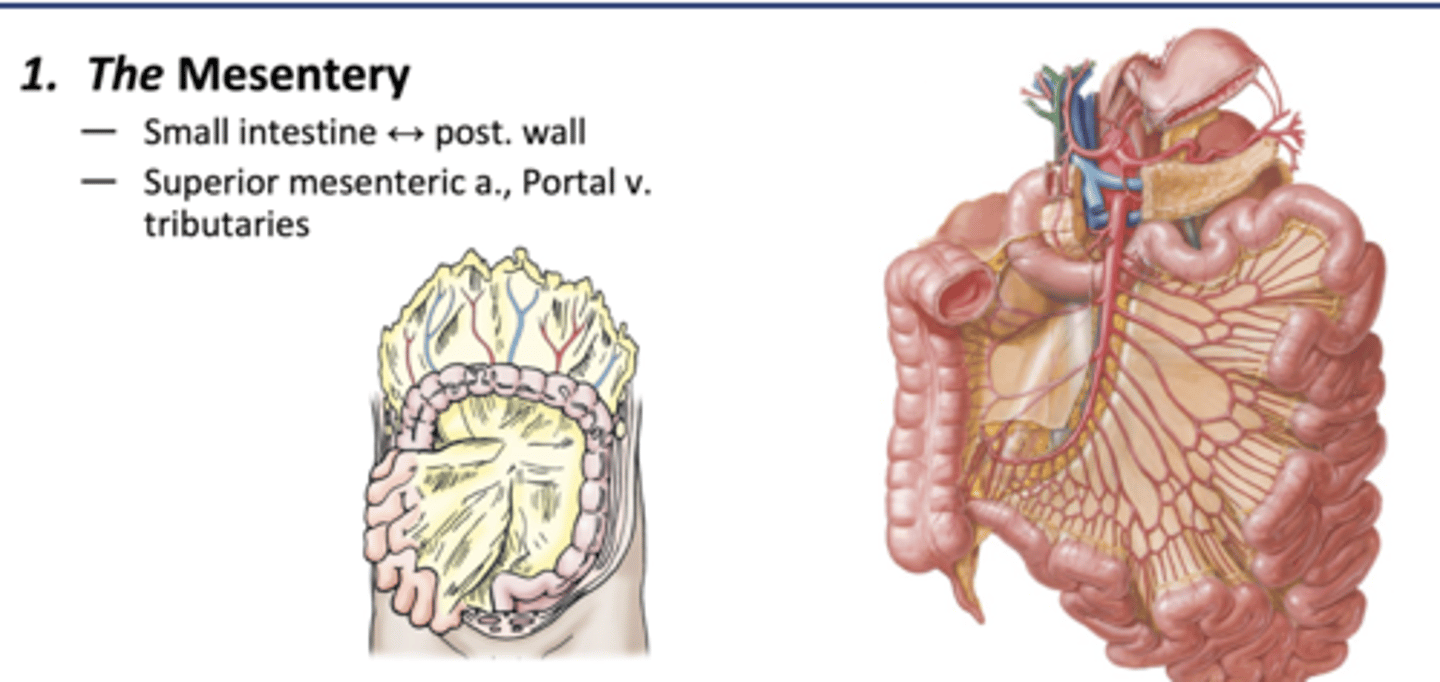
The Mesentery
-Peritoneal fold that attaches the small intestine to the posterior wall
-Superior mesenteric a, portal vein tributaries
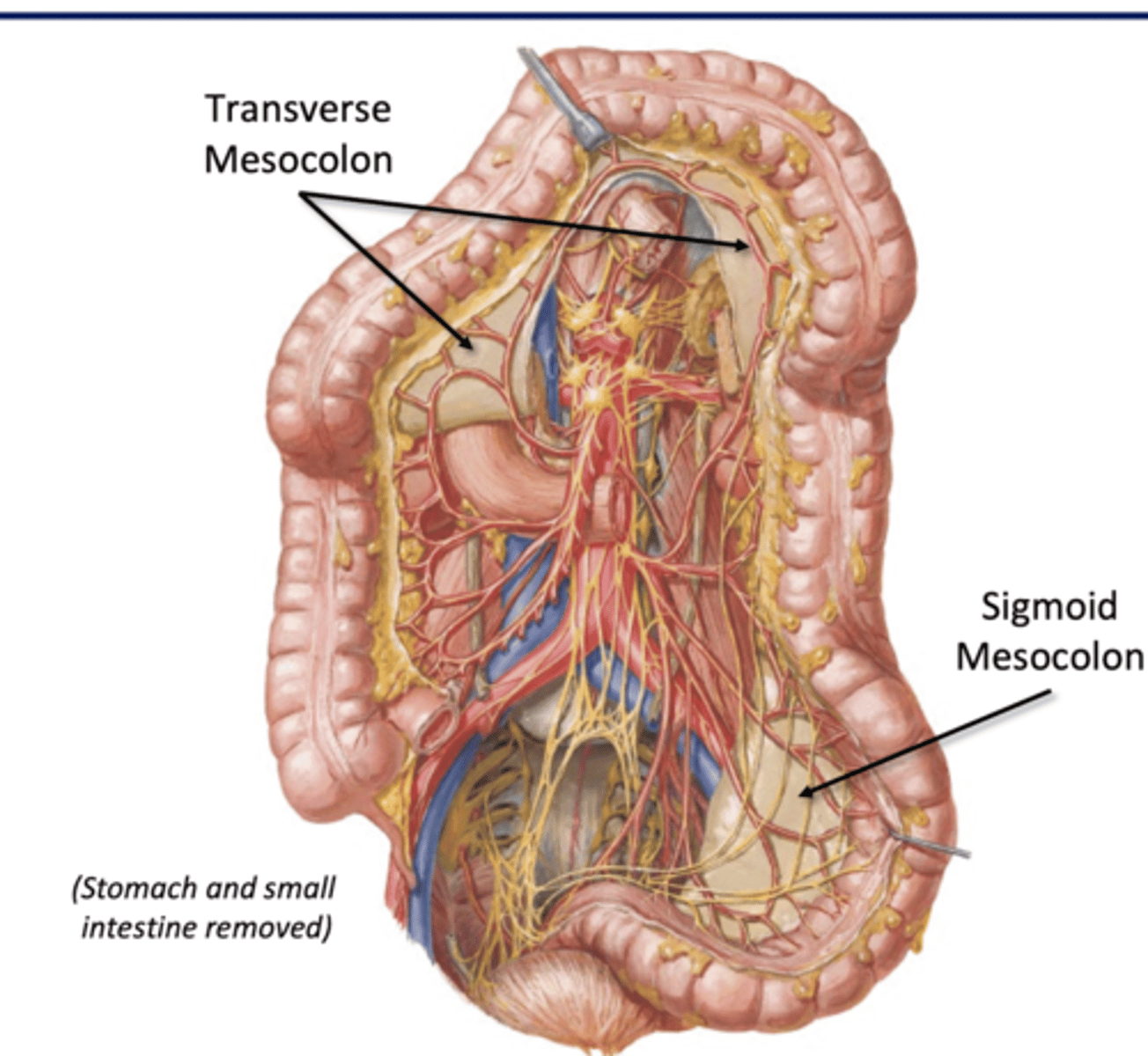
Mesocolons
Transverse
-transverse colon to post wall
-superior mesenteric a, portal vein tributaries
Sigmoid
-sigmoid colon to post wall
-inferior mesenteric a, portval vein tributaries
**no mesentery for ascending/descending colon bc they secondarily retroperitoneal**
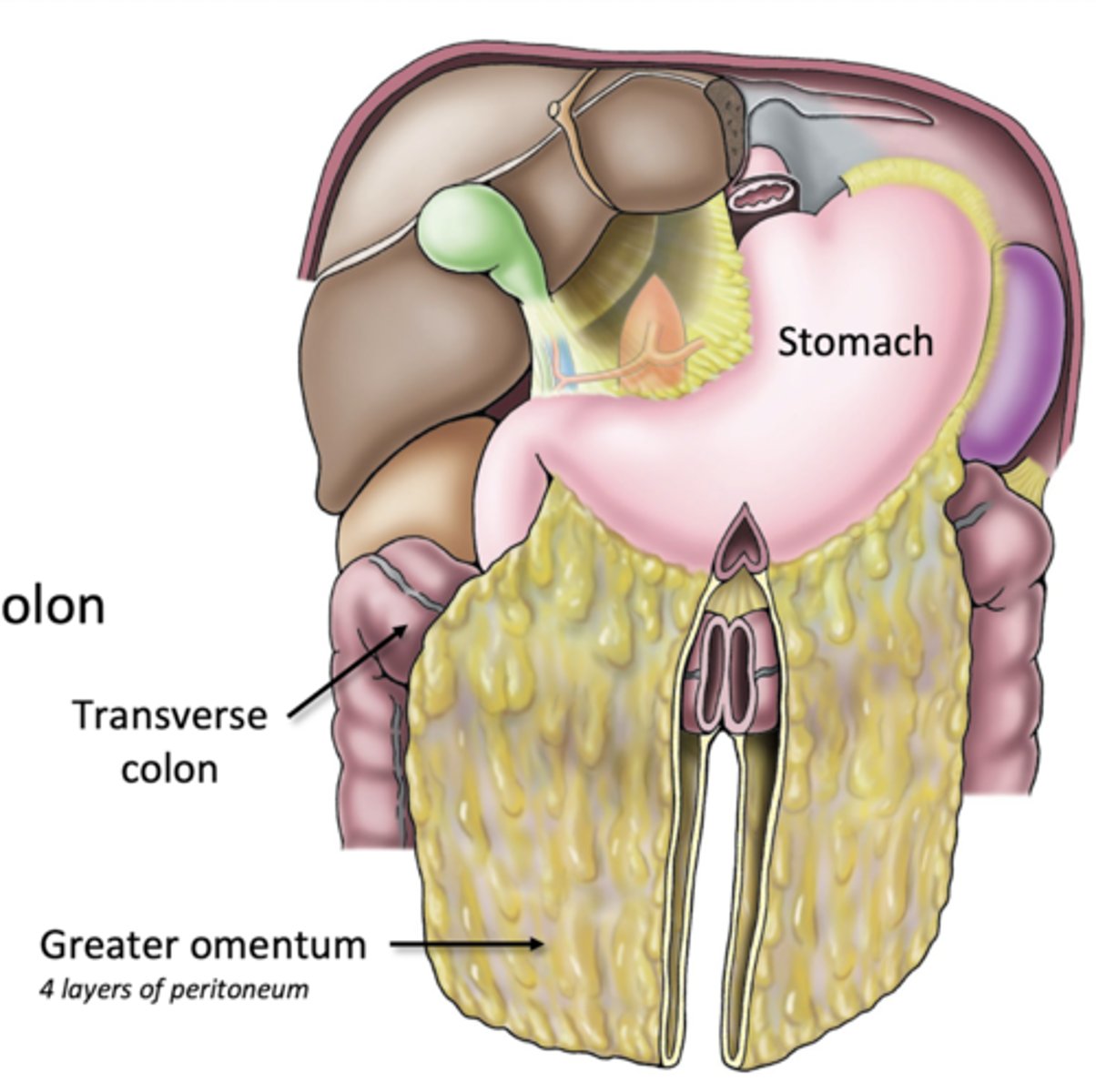
Greater Omentum
greater curvature of stomach to transverse colon
-many lymph nodes to combat GI infections
Lesser Omentum
-lesser curvature of stomach to liver
--by hepatogastric ligament
-Duodenum to liver
--by hepatoduodenal ligament
-Celiac trunk branches, portal v tributes
-bile duct
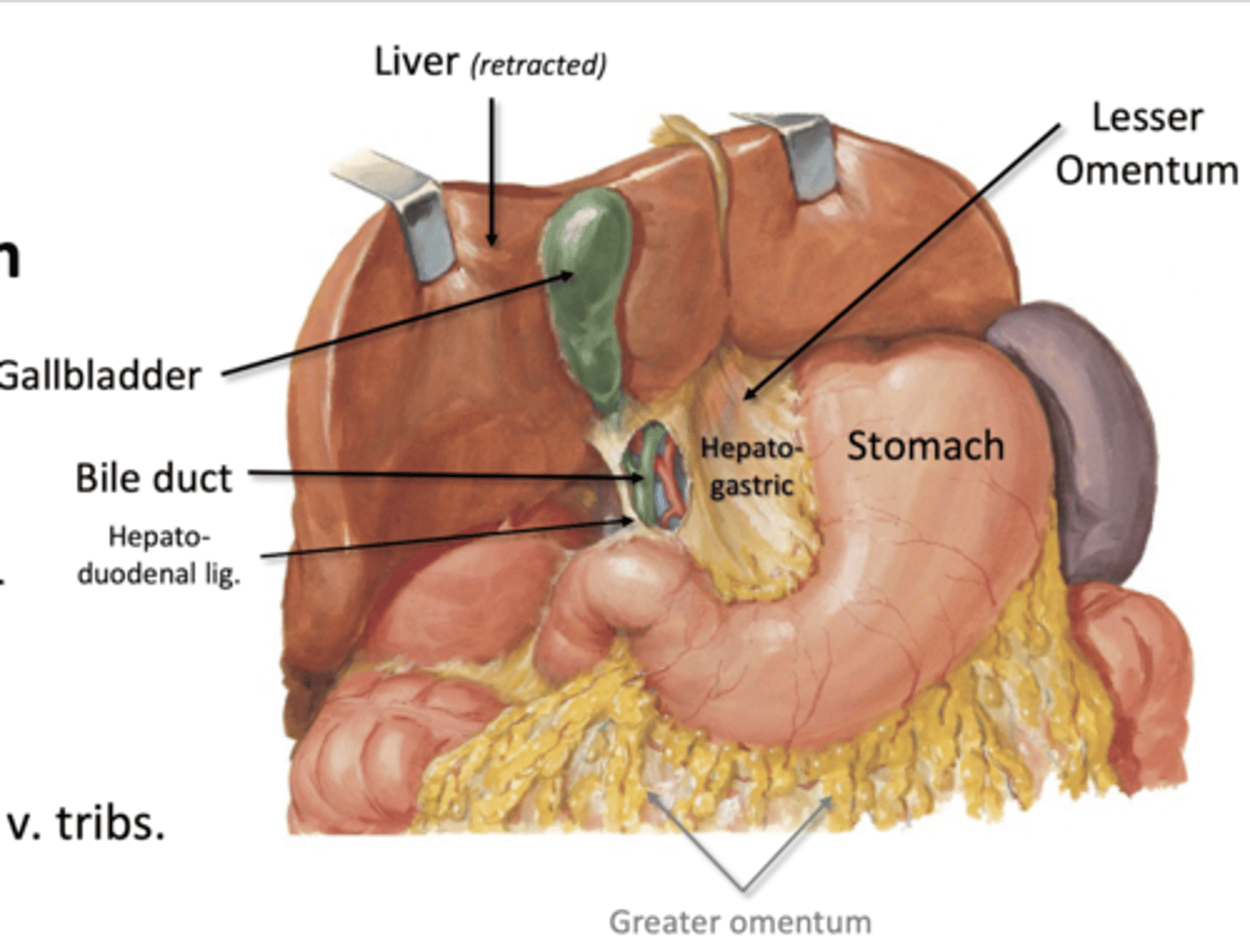
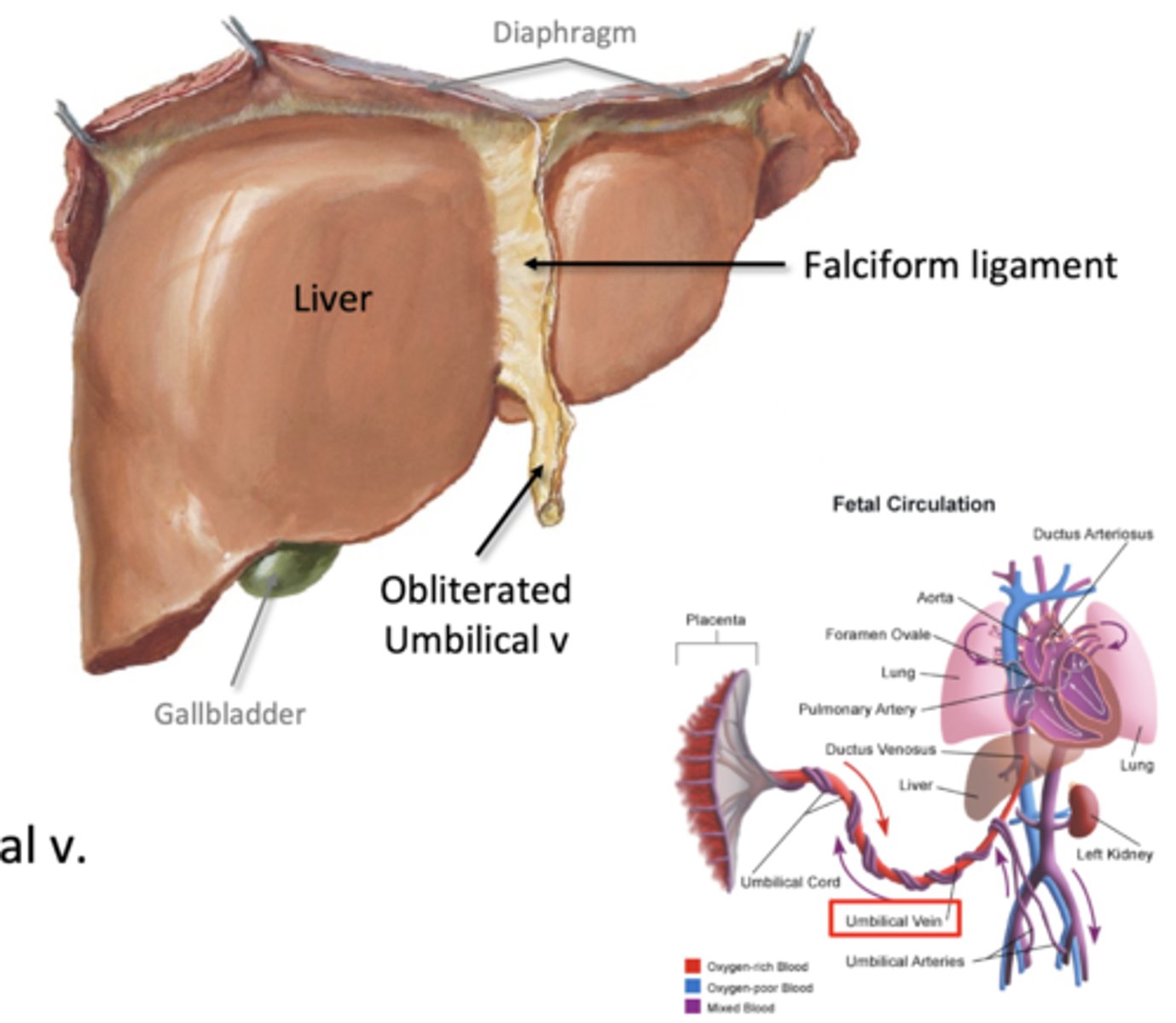
falciform ligament
liver to anterior wall
-pathway of obliterated umbilical vein (round ligament)
-extends to the umbilicus (belly buttone)
oral cavity boundaries
Anterior: lips (labia)
Lateral: cheeks
Superior: hard and soft palate
Inferior: mylohyoid muscle
Posterior: fauces
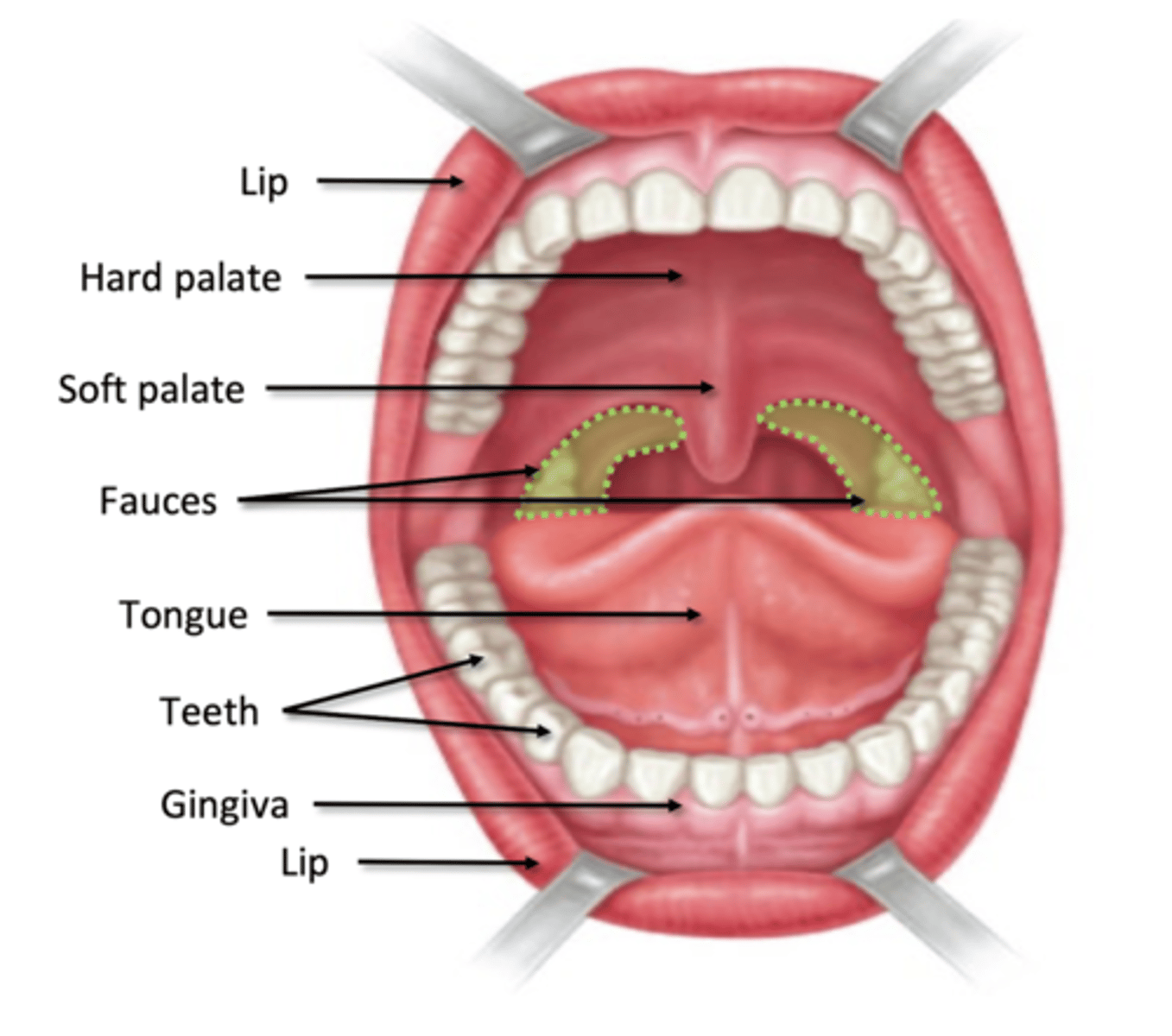
oral vestibule
space between cheeks/lips and gingivae
mucosa (oral cavity)
lines palate, interior cheeks and lips, gingivae, tongue
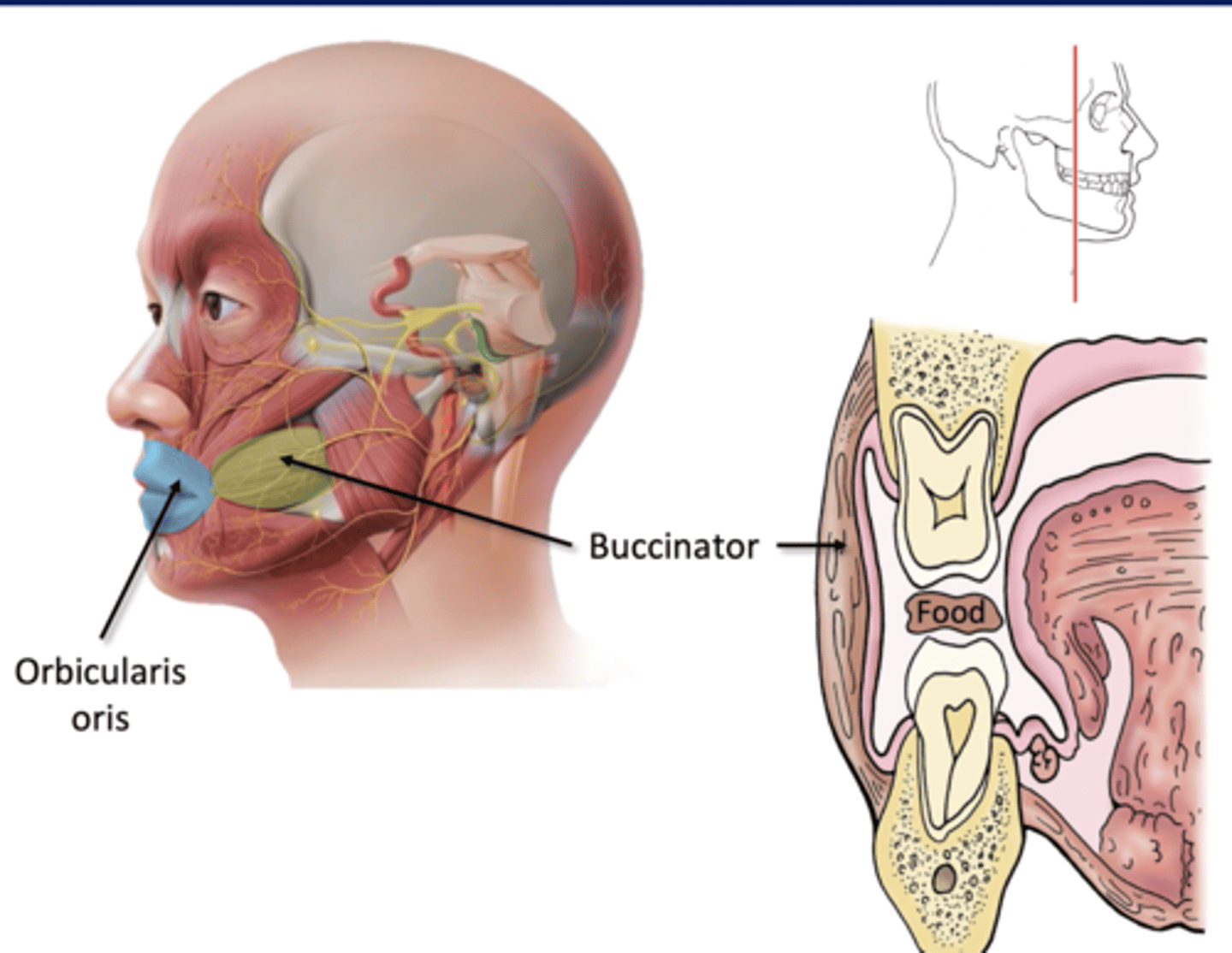
Structures of Ingestion
Lips: open to receive food, close to maintian
-orbicularis oris m
Cheeks: hold food between teeth
-buccinator m
*Facial Nerve (CN VII)*
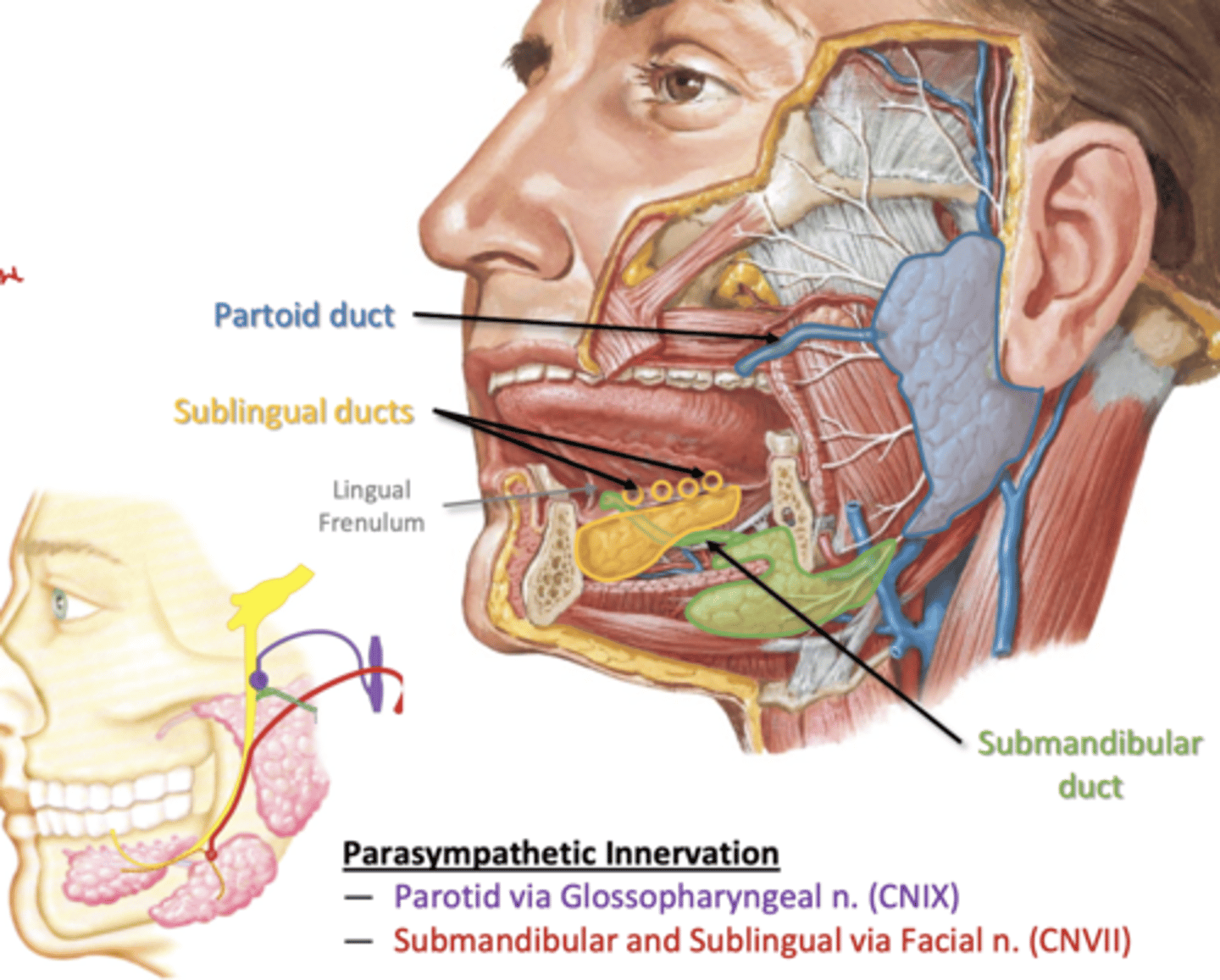
Salivary glands
-many small glands in mucosa
3 major bilateral glands:
--Parotid- outside cavity
--Submandibular- outside cavity
--Sublingual- inside cavity
-parasymp stimulation/ symp suppression
Saliva
99.5% water
-Digestive enzymes:
--amylase: starch
--lingual lipase: triglycerides
Innervation of salivary glands
Parotid- Glossopharyngeal nerve (CN IX)
Submandibular and Sublingual- Facial Nerve (CN VII)
Mastication
crushing or grinding of food between the teeth produced by movements of jaw
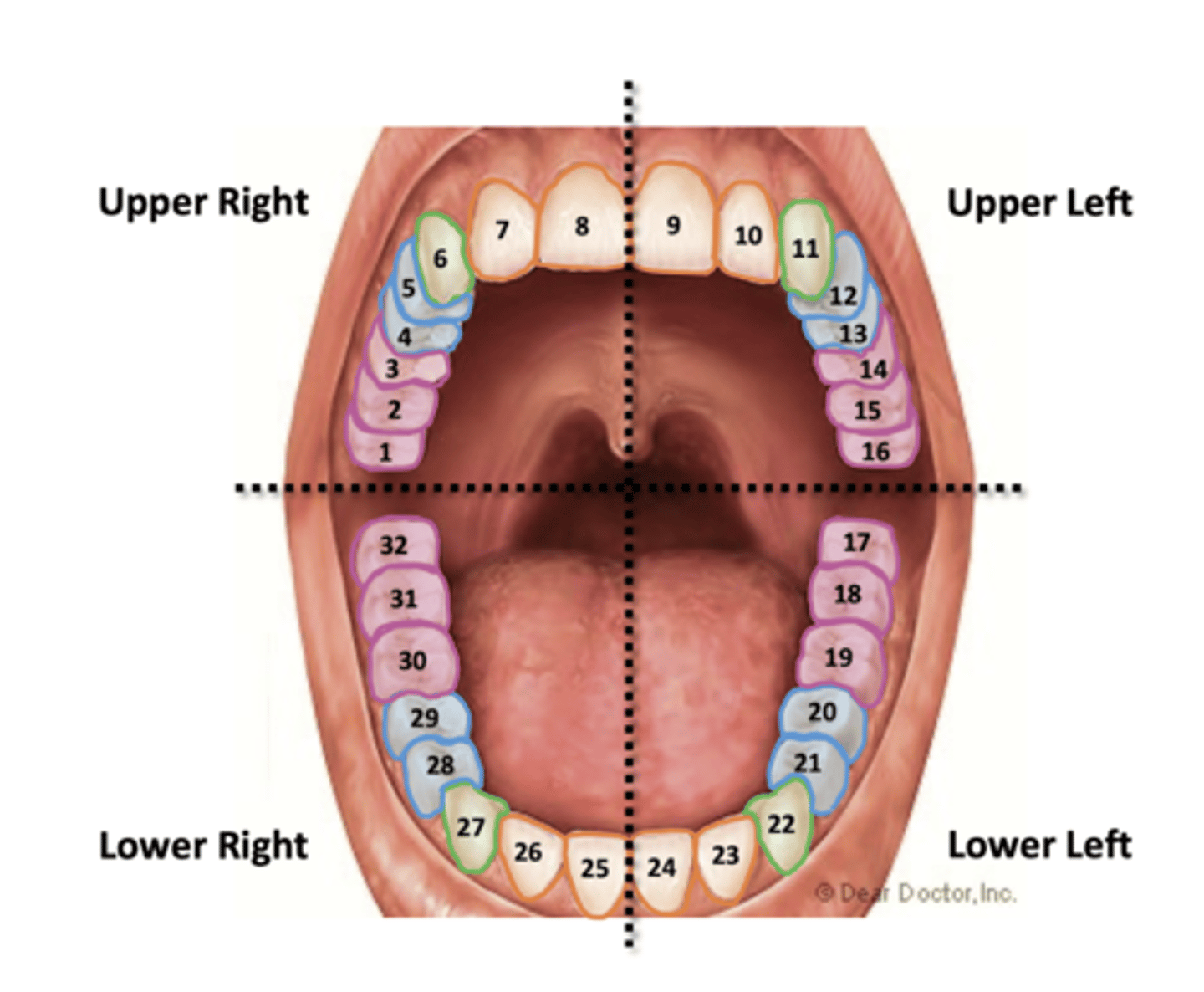
Teeth
per quadrant:
2 insicors
1 canine
2 premolars
3 molars
naming starts from upper right
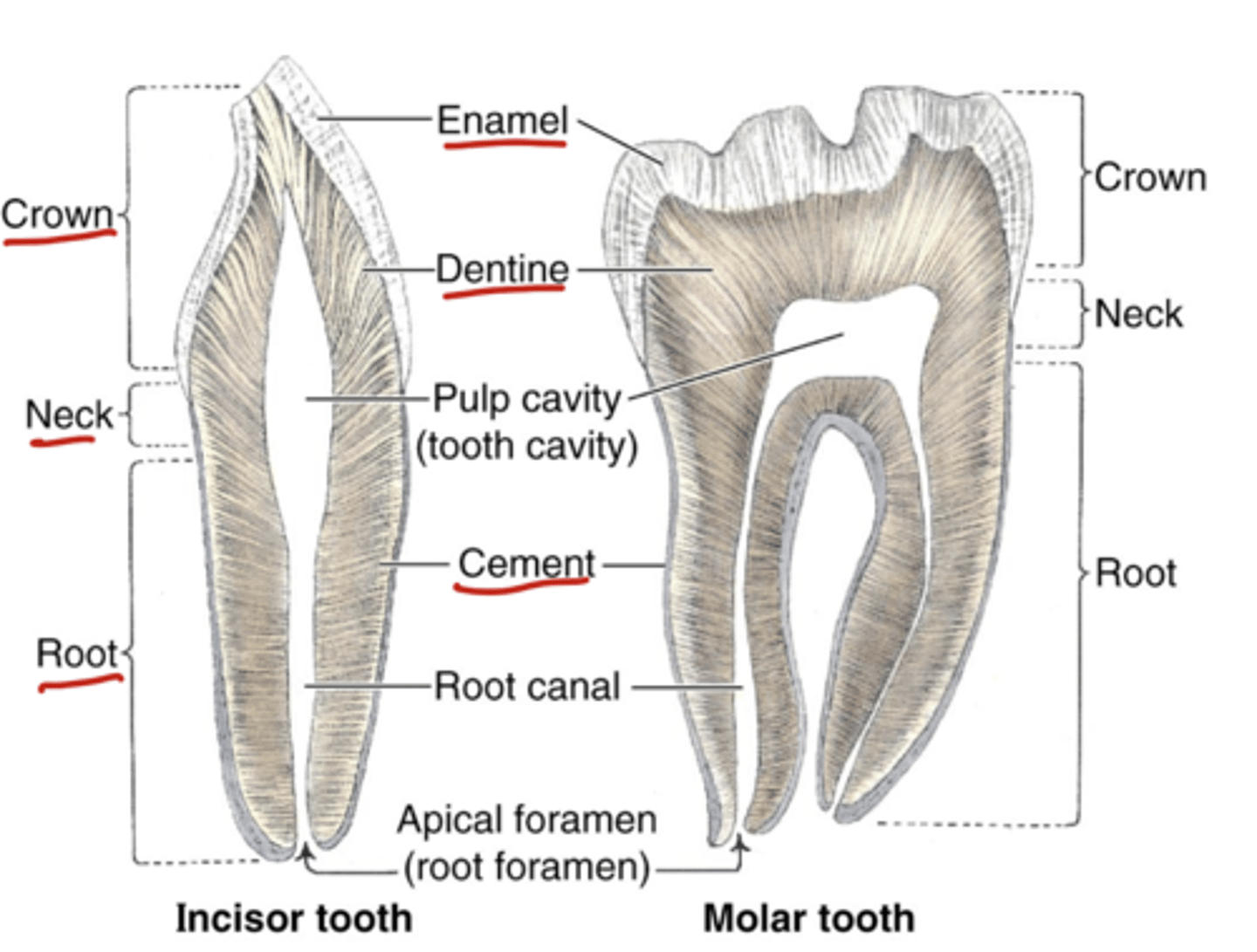
Structures of Teeth
Crown (visible portion), neck, root, enamel, dentine, cement, pulp cavity (neurovasculature)
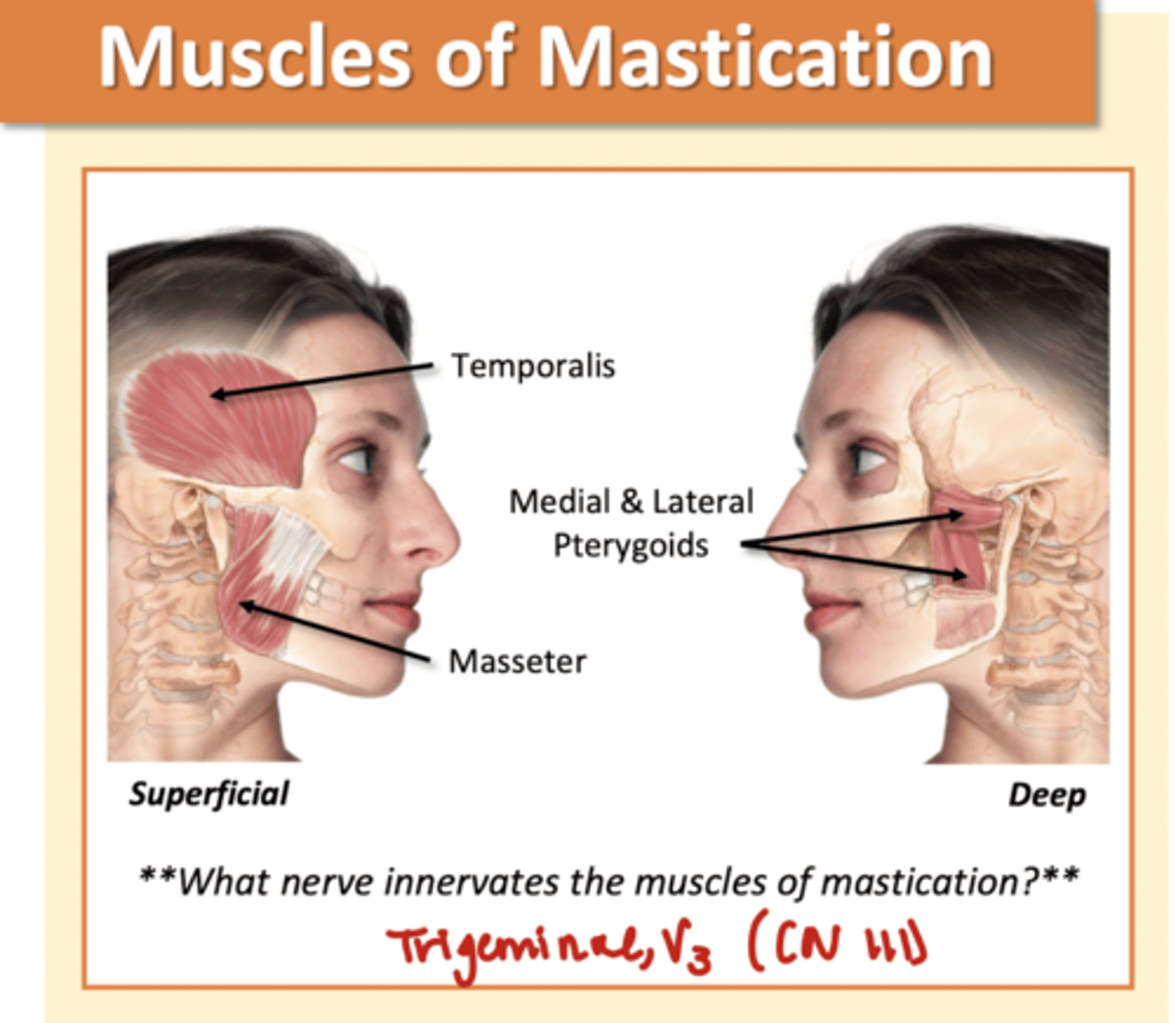
Muscles of Mastication
Temporalis
Medial/Lateral Pterygoids
Masseter
*Trigeminal, V3 (CN III)*
-involved in mechanical digestion
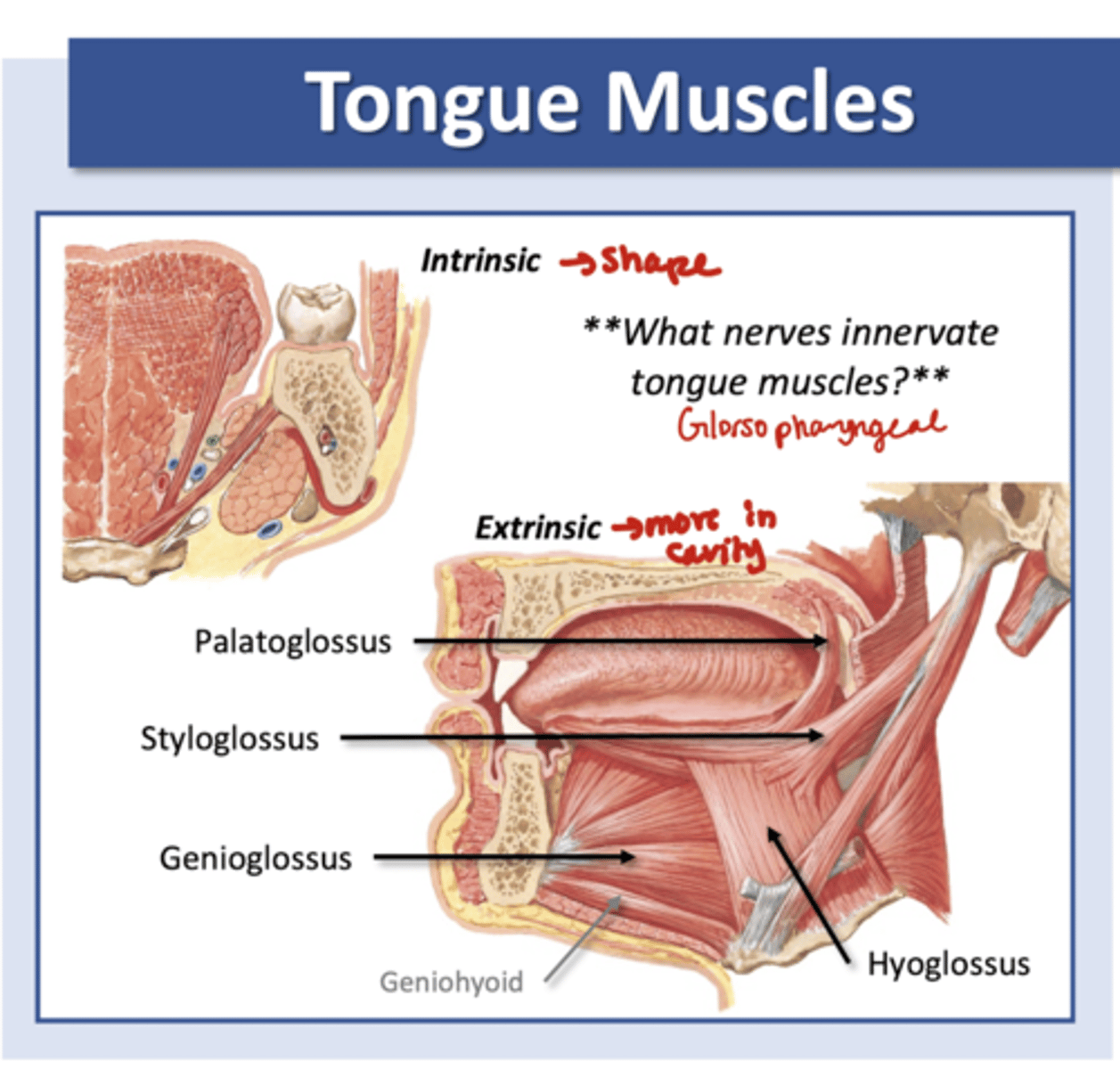
Tongue Muscles
Intrinsic--> shape
Extrinsic--> move in cavity
Palatoglossus, Styloglossus, Genioglossus, Hyoglossus
*Glossopharyngeal (CN IX)*
-involved in mechanical digestion and mixing and propulsion
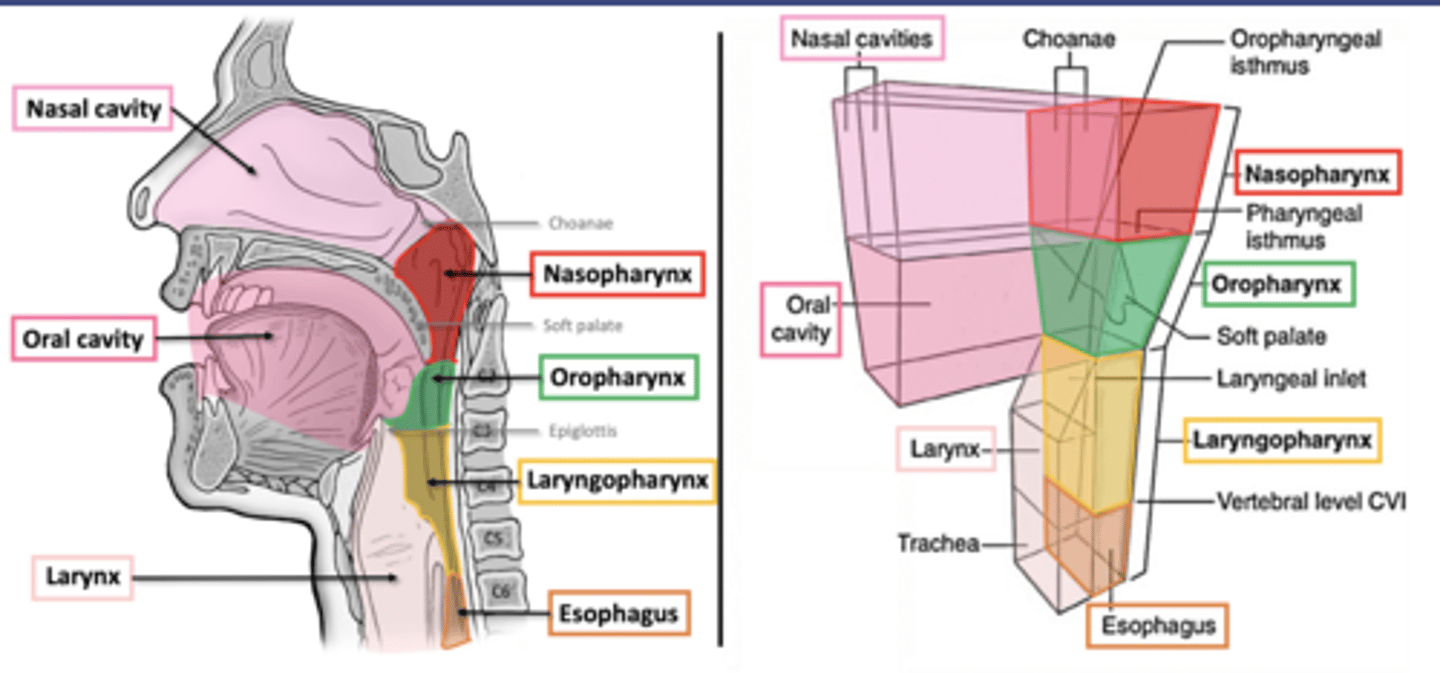
The pharynx
beginning of respiratory pathway
-mixing and propulsion
-naso, oro, and laryngopharynx
Voluntary Phase of Swallowing
extrinsic muscles of tongue push bolus into oropharynx
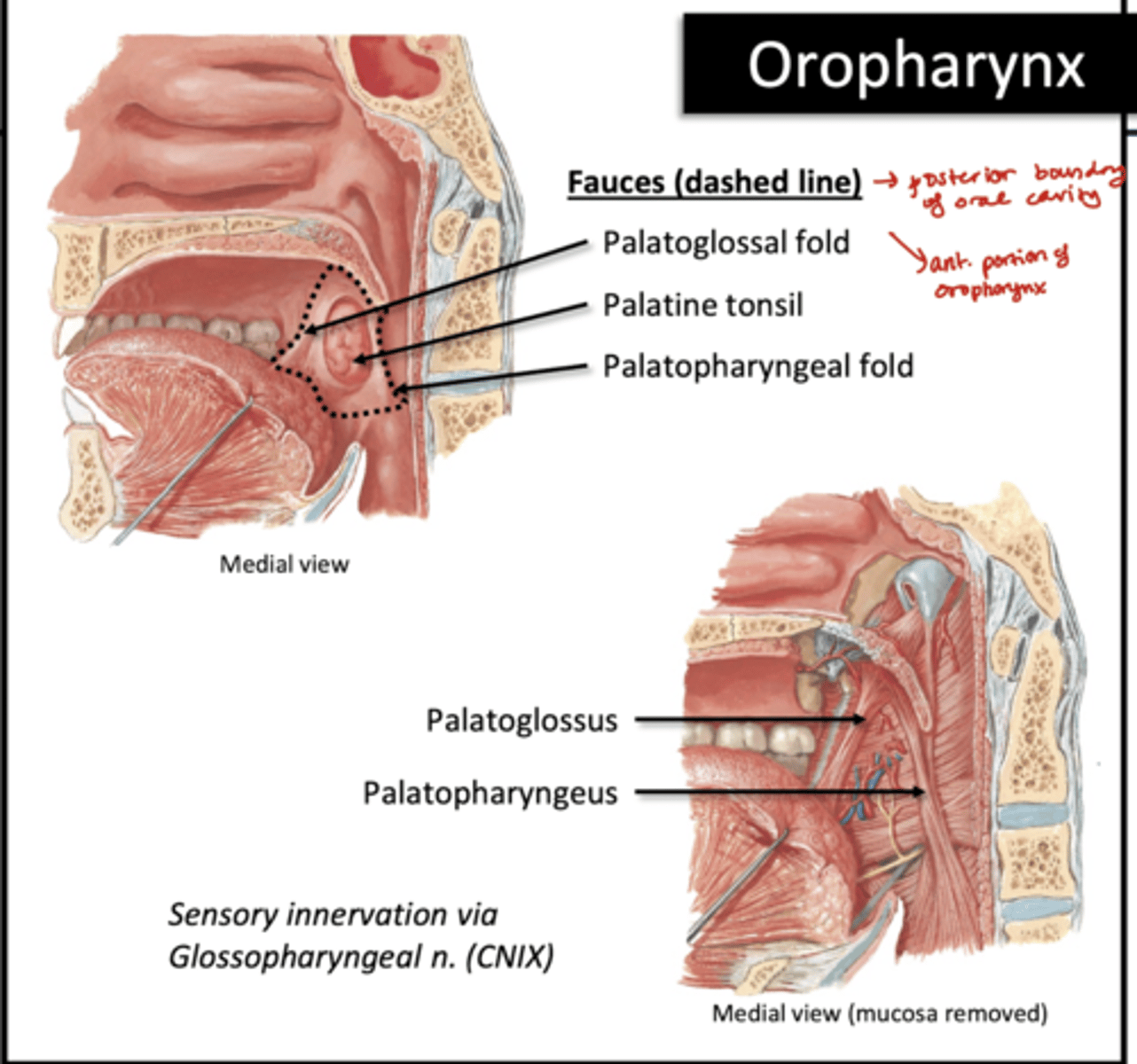
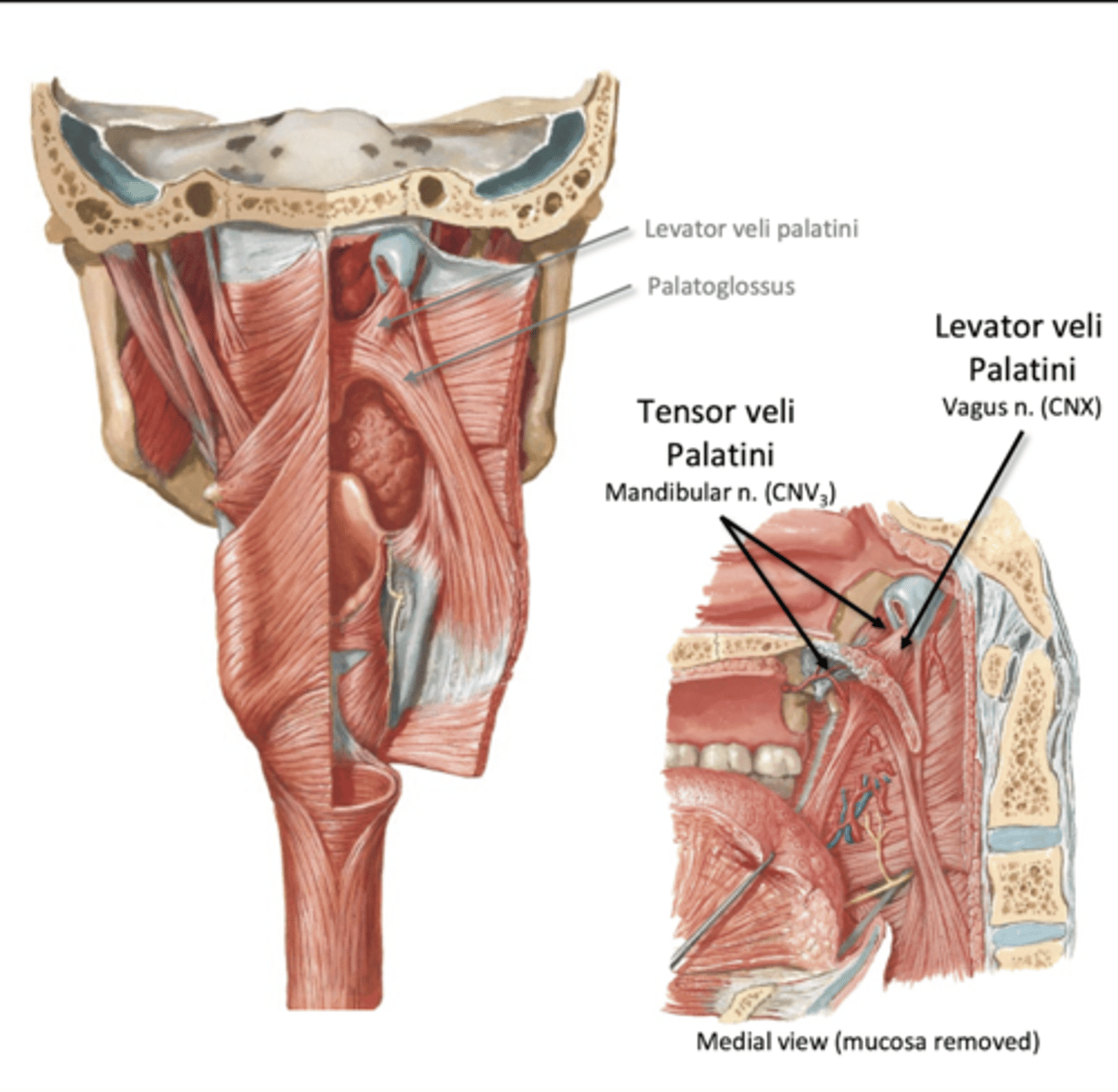
Involuntary phase of swallowing
"pharyngeal phase"
-breathing pauses
-soft palate activates
--Lifts (levator veli palatini)
--Tenses (tensor veli palatini)
--closes passage between oro and naso pharynxes
Involuntary phase continued
-vocal cords close
-epiglottis bends over larynx
-pharyngeal constrictors fire
Sup, Middle, Inf pharyngeal constrictor muscles (Vagus CN X)
-help propel bolus down
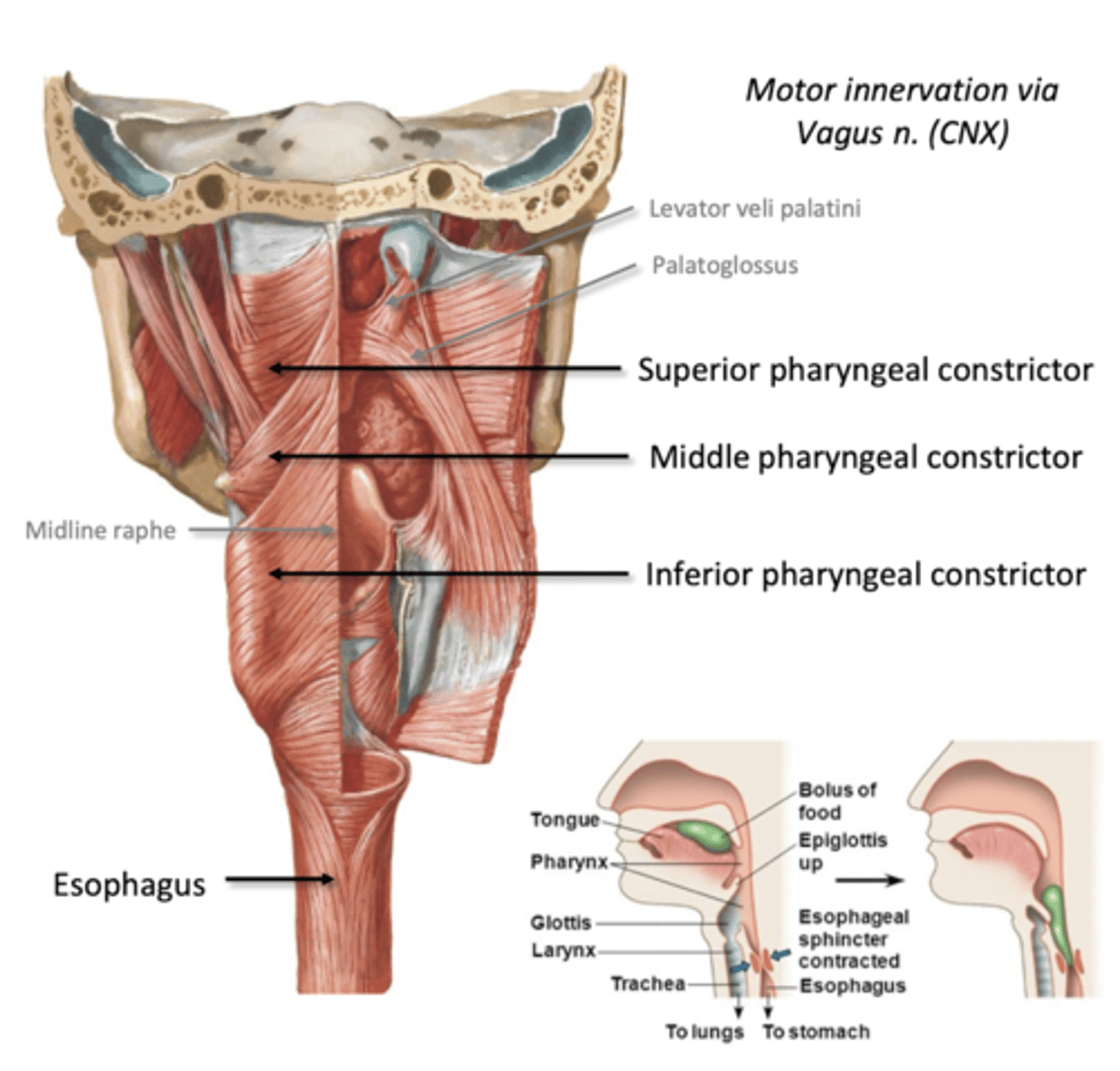
Esophagus
Connects pharynx to stomach
-mixing and propulsion
propulsion in esophagus (passive)
passive transport: mucosa
-lubricated: mucous
-Sturdy: nonkeratinized stratified squamous epithelium
--overlapping cells resilient to wear and tear from boluses moving through
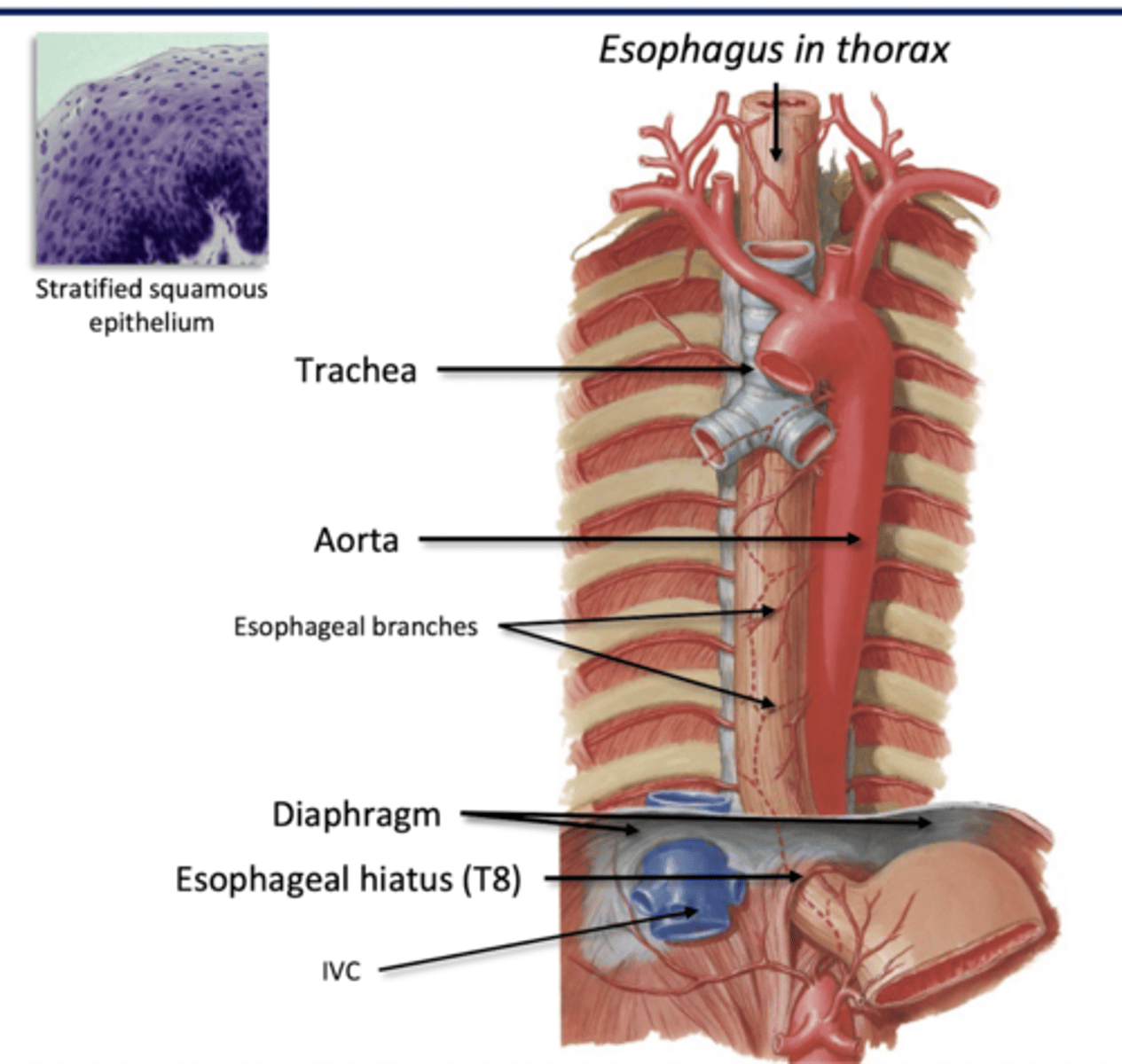
propulsion in esophagus (active)
Active Transport: Muscularis
Longitudinal and Circular fibers
-proximal 1/3 skeletal muscle
-middle 1/3 mixed
-distal 1/3 smooth muscle
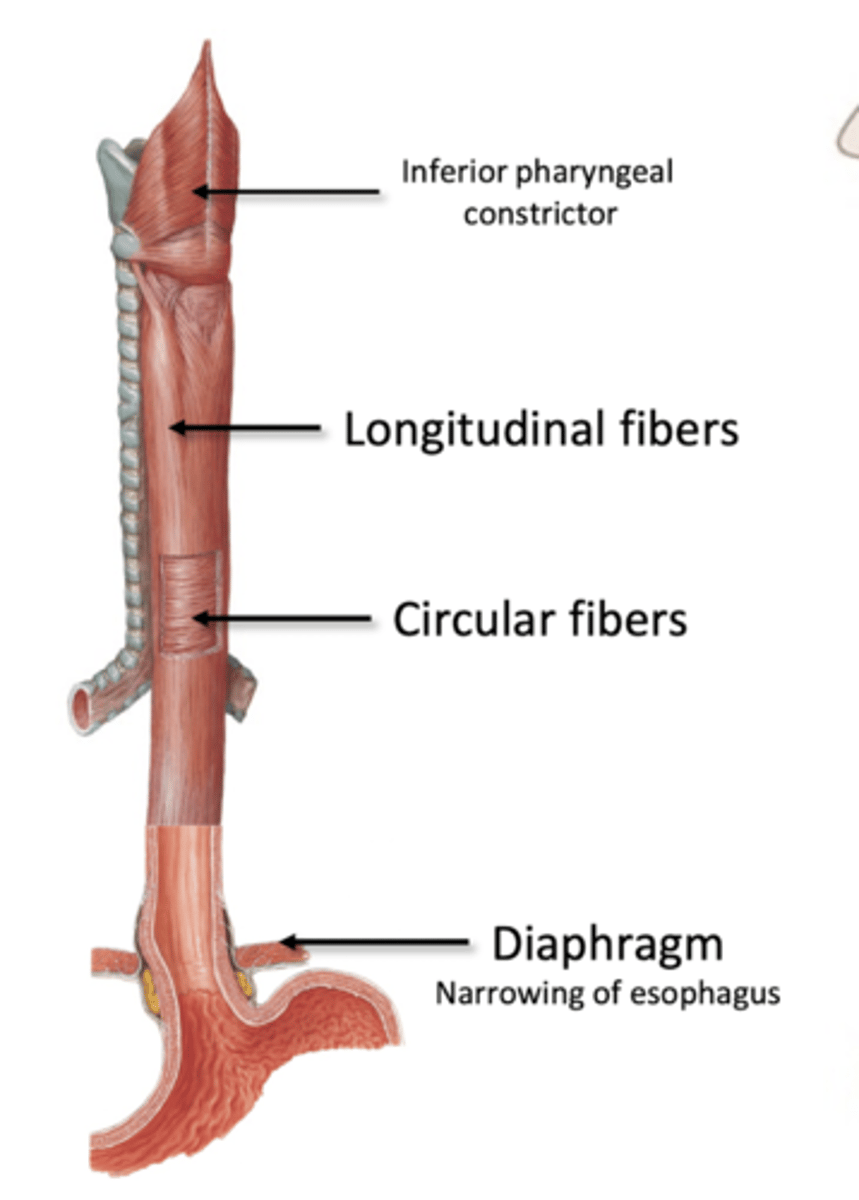
Peristalsis (esophagus)
1. Circular muscle fibers above bolus contract (push to stomach)
2. Longitudinal muscle fibers below bolus contract (to shorten and widen tube)
3. Repeat cycle, and lower esophageal sphincter relaxes to pass into stomach
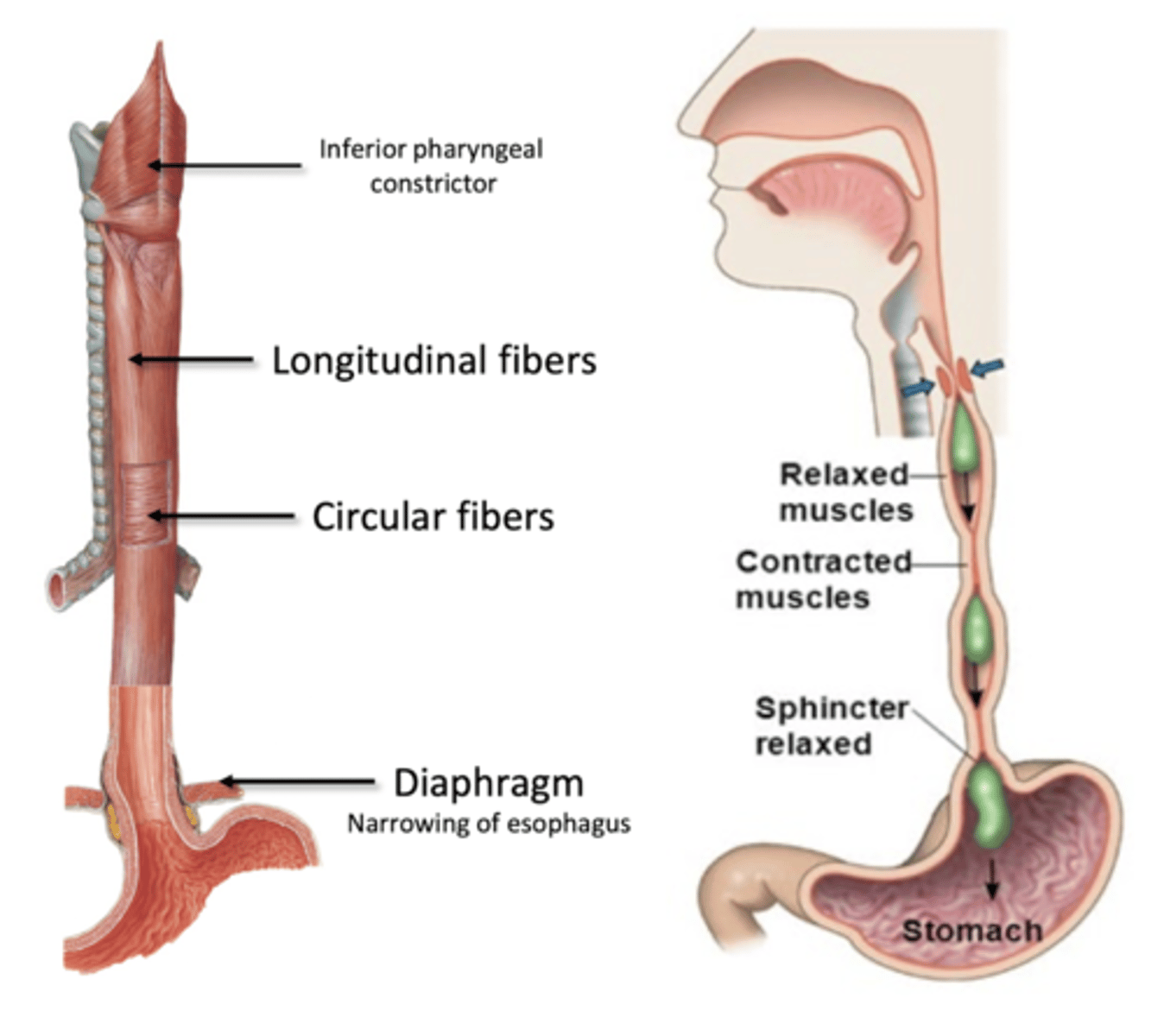
Stomach
involved in secretion ,mixing and propulsion, mechanical/chemical digestion
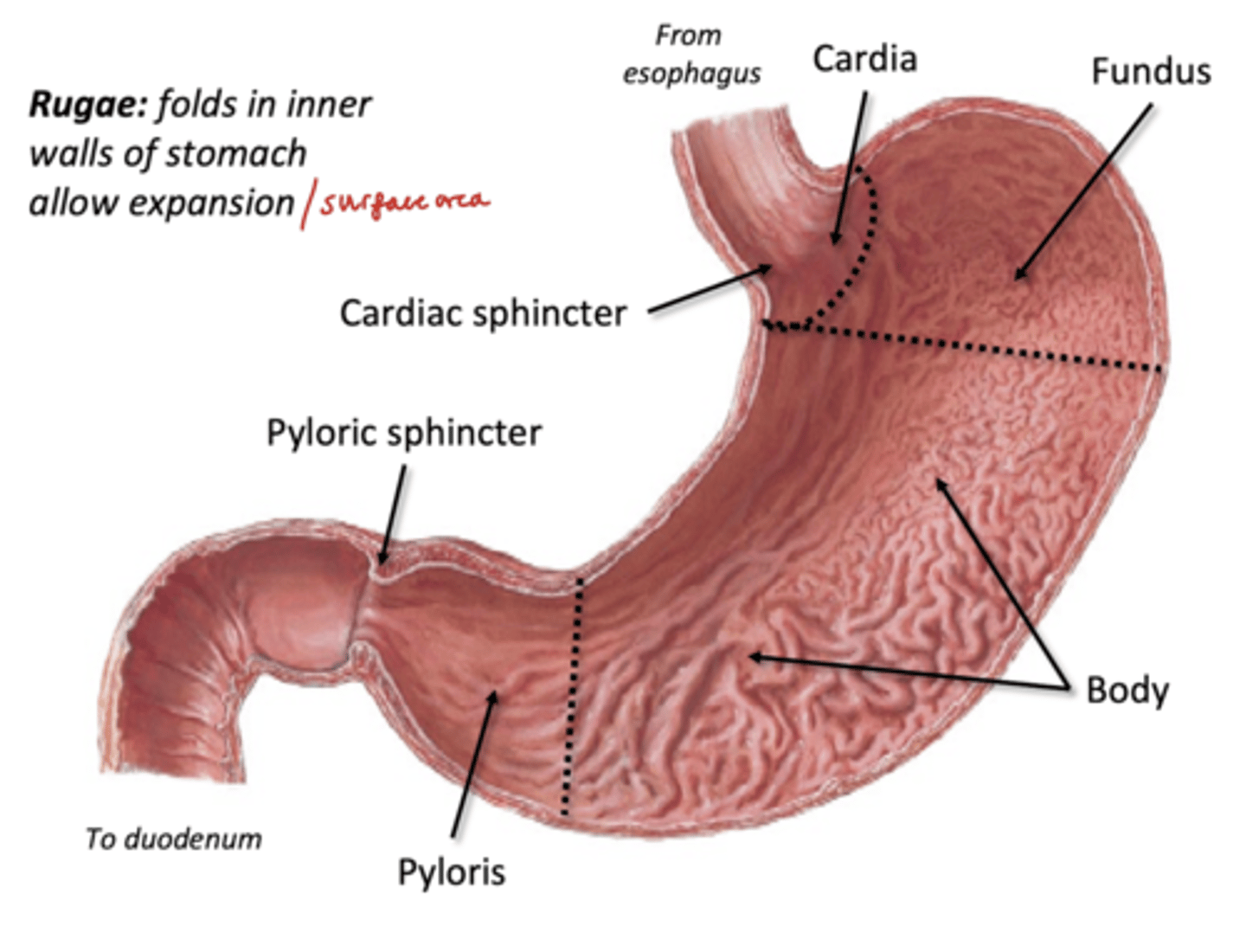
Feautures of the stomach
4 Regions: Cardia, Fundus, Body, Plyoris
-lesser and greater curvature
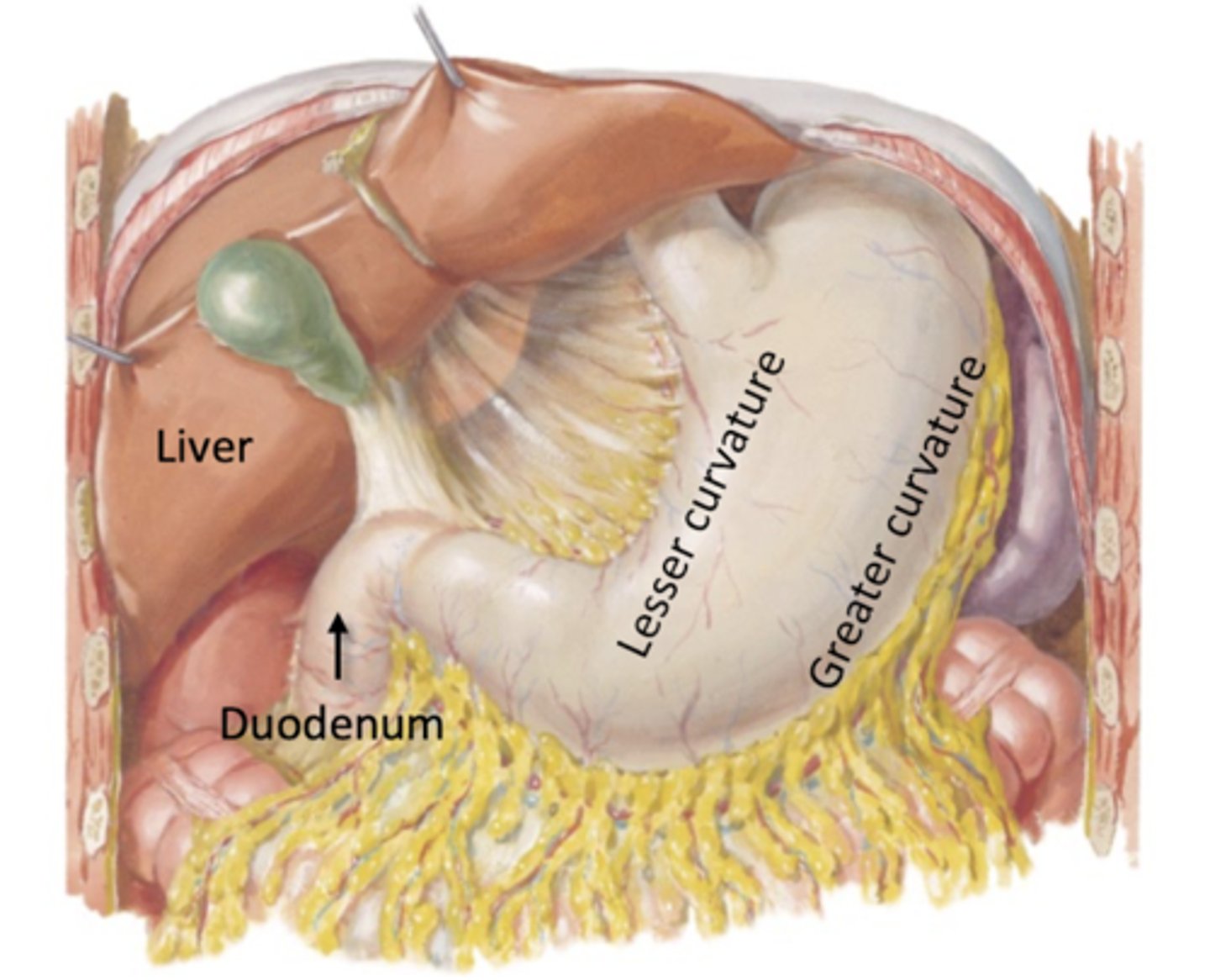
Stomach Innervation/Vasculature
Parasympathetic: Vagus
Symp: thoracic splanchnics, synapse at celiac ganglion
Artery: Celiac trunk bb
Vein: portal vein tributaries
Cardia (region of stomach)
-surrounding meeting of esophagus
-home to cardiac sphincter: physiological sphincter (not a true ring)
--can cause acid reflux
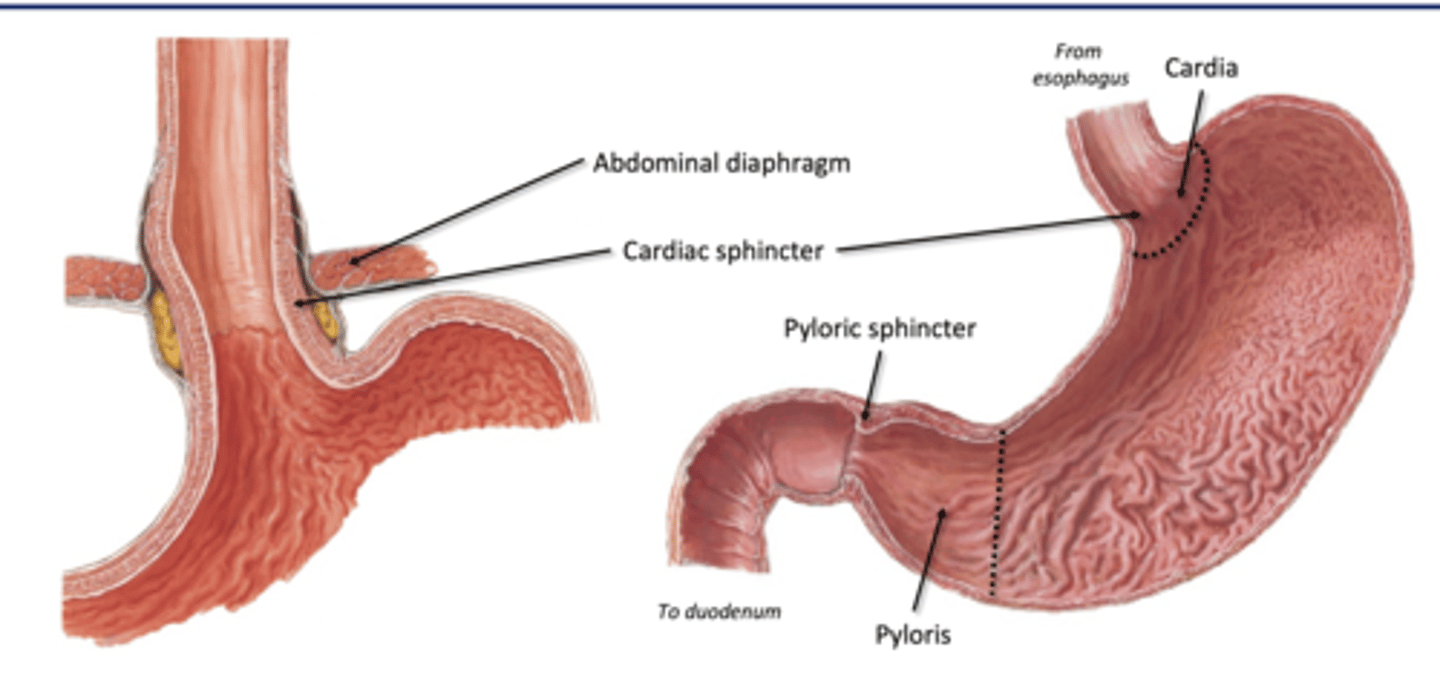
Fundus (stomach region)
rounded upper portion of the stomach, usually houses lots of gases
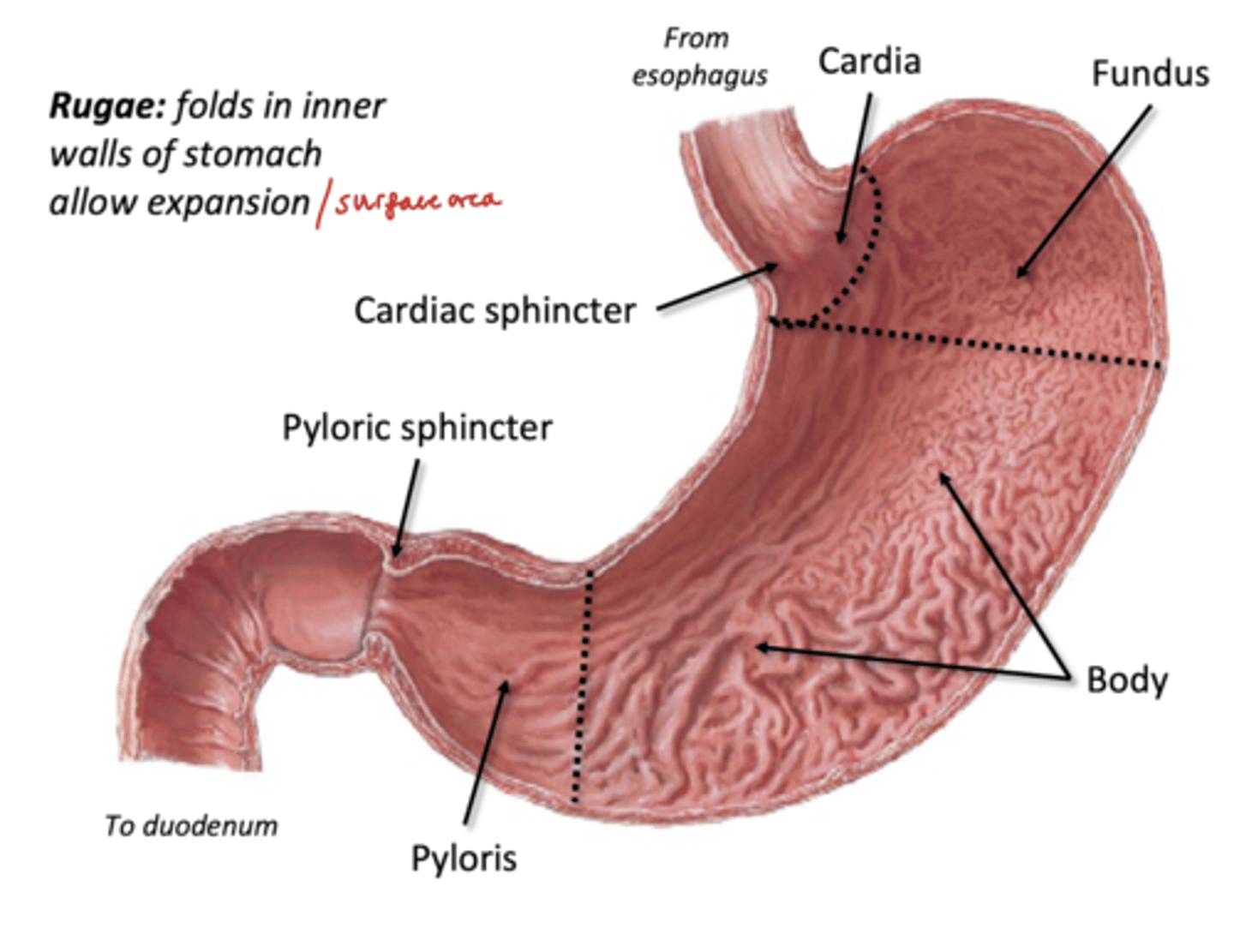
Body (stomach region)
-has Rugae: folds in inner walls of stomach to allow expansion/surface area for digestive glands
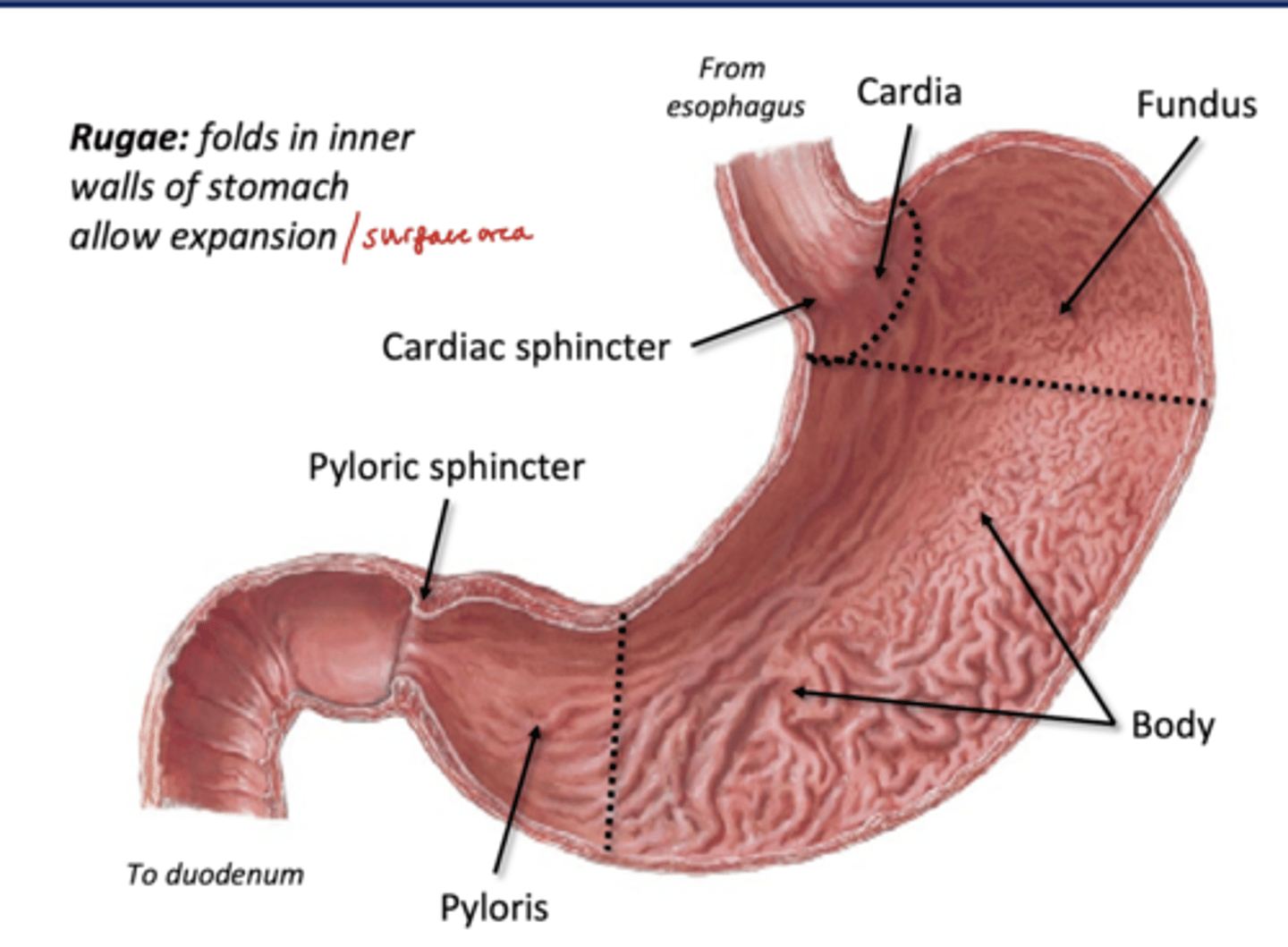
Pyloris (stomach region)
Distal most portion of stomach
-narrows to meet duodenum, guided by pyloric sphincter (true ring of muscle)
--open small amount to regulate rate the stomach empties
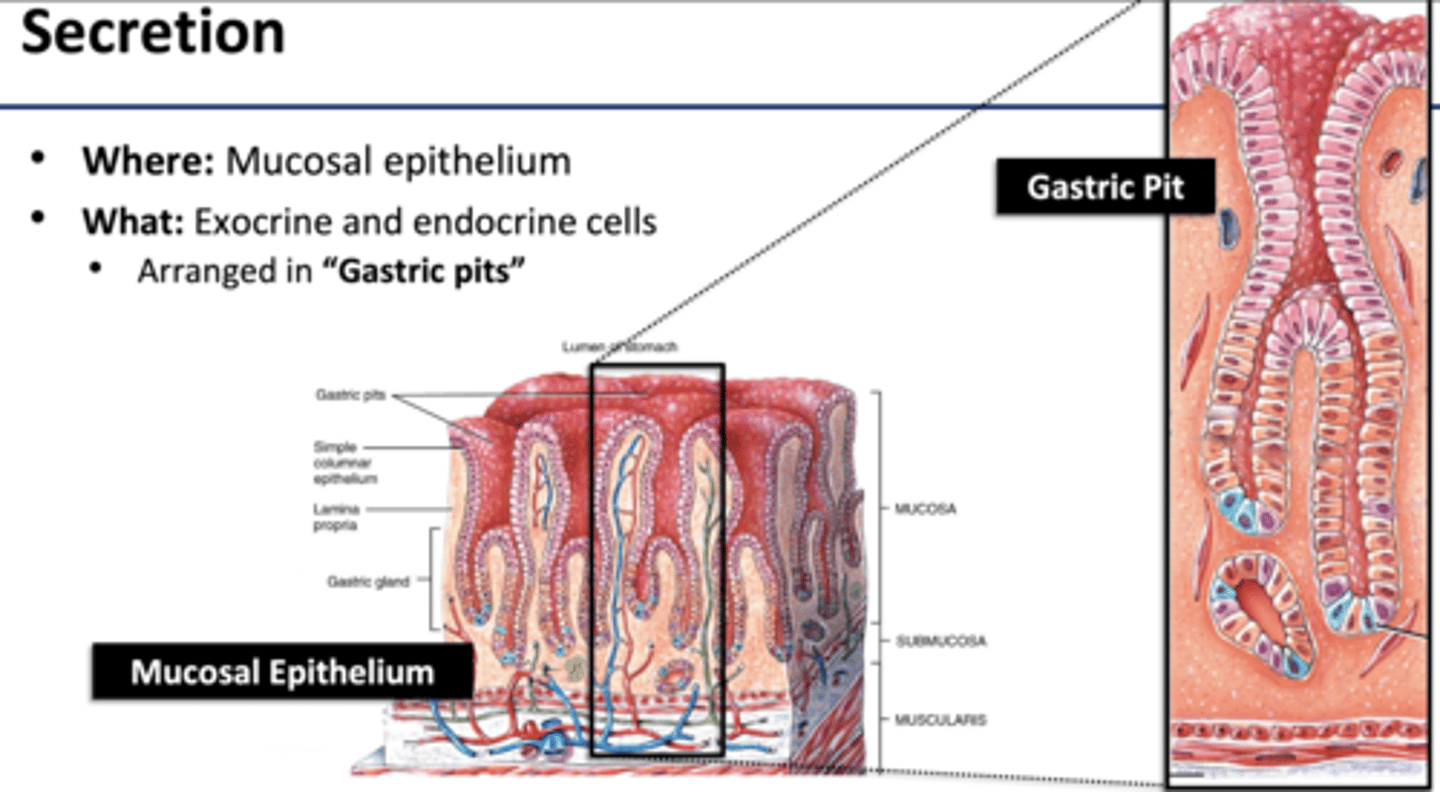
Secretion in Stomach
Muscosal Epithelium cells: produces acid
Exocrine and endocrine cells arranged in Gastric Pits
--pits made by connective tissue lamina propia
Exocrine Cells (stomach)
-responsible for chemical digestion
Mucous Cells
Chief cells: pepsinogen, gastric lipase
Parietal Cells: Hydrochloric acid
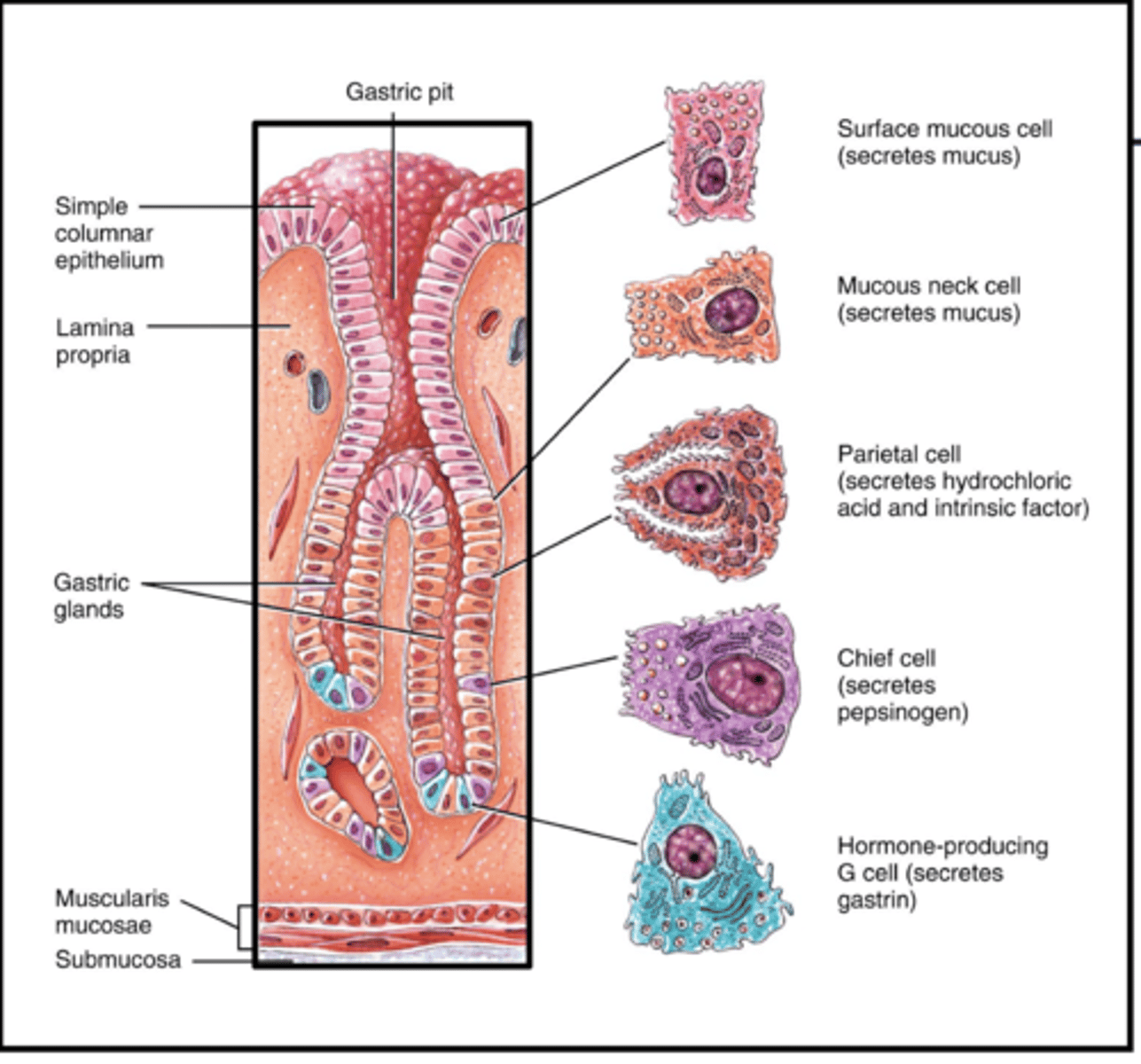
Endocrine Cells (stomach)
G cells
-gastrin: stimulates gastric juice + increases gut motility
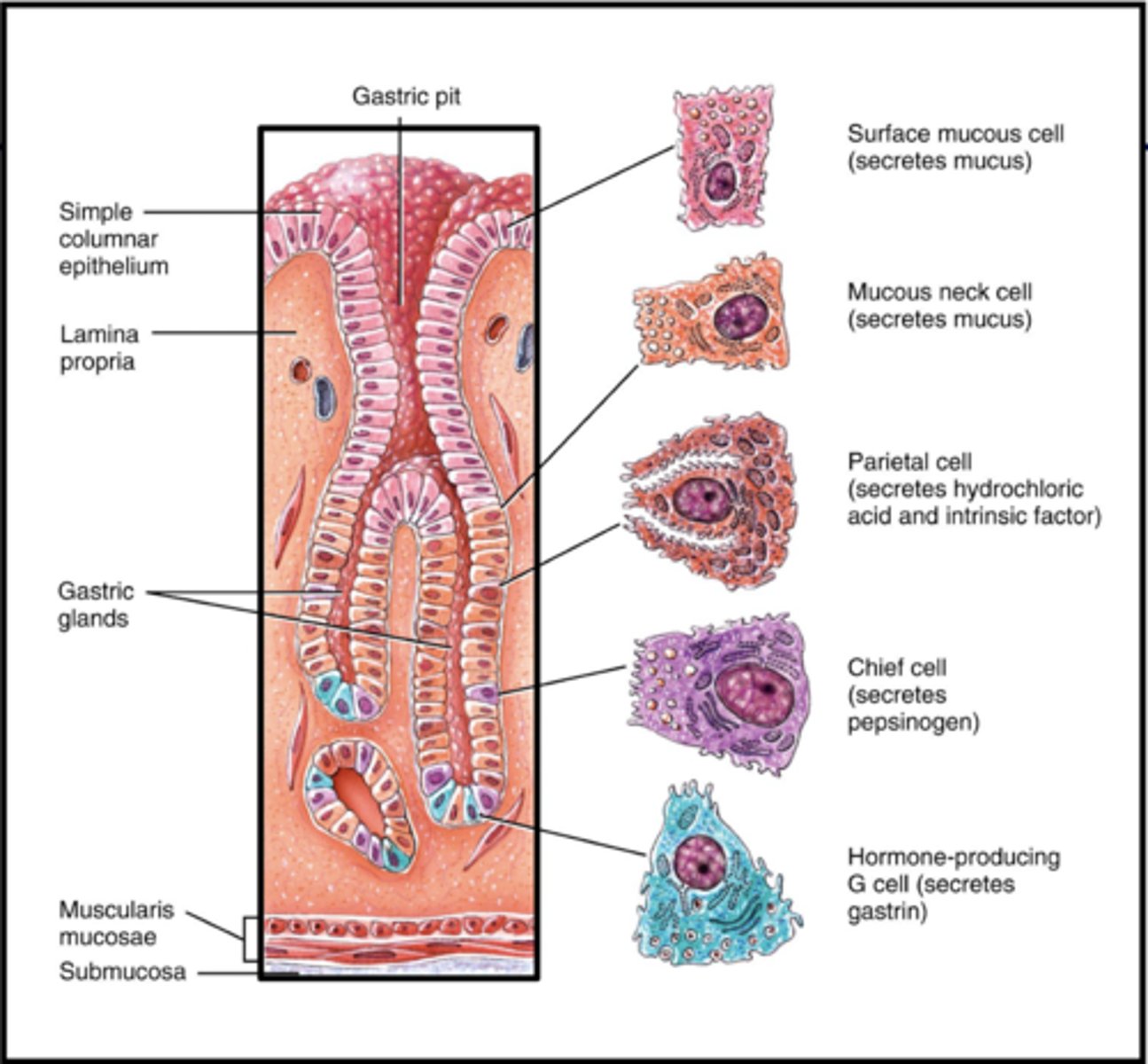
Mucous cells
-Secrete mucous
-absorb water, ions, come drugs (aspirin), alcohol
Chief cells
Pepsinogen (pepsin with HCL)
-breaks aa peptide bonds
-clump and digest milk proteins
Gastric Lipase
-triglycerides --> fatty acids and monoglycerides
Parietal Cells
Intrinsic Factor: absorb vitamin B
-Hydrochloric acid
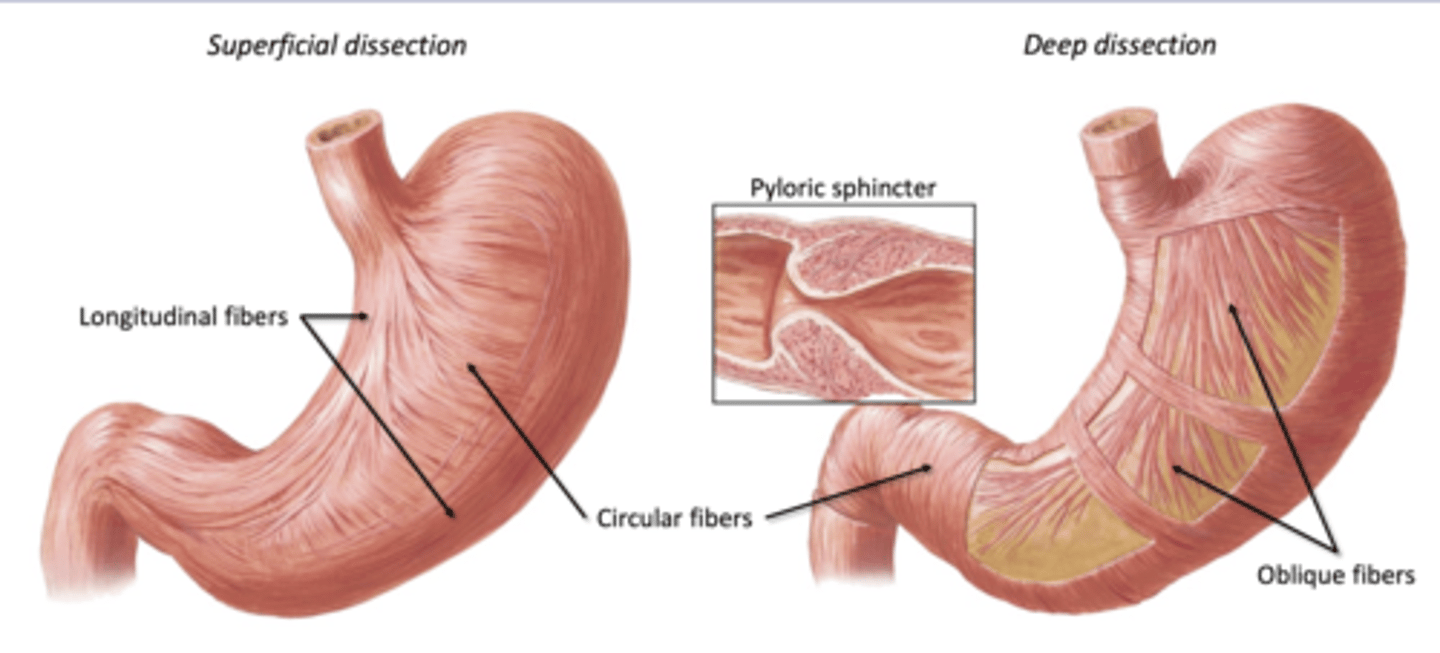
Mixing and Propulsion in Stomach
Muscularis:
-3 layers of muscles
--longitudinal and circular and oblique
Churning: mix with acid and gastric juices
Peristalsis: move toward duodenum
Pancreas
Involved in Secretion and Chemical Digestion
-Secondary Retroperitoneal
-posterior abdominal wall behind stomach
Features of the Pancreas
Head (resting on duodenum), Neck (close to pylorus), Body, Tail (touching spleen
Pancreas Innervation/ Vasculature
-Parasympathetic: Vagus
-Sympathetic: thoracic splanchnics, synapse at celiac ganglion
-Artery: Celiac trunk bb, Super Mesenteric bb
-Vein: Portal vein tributaries
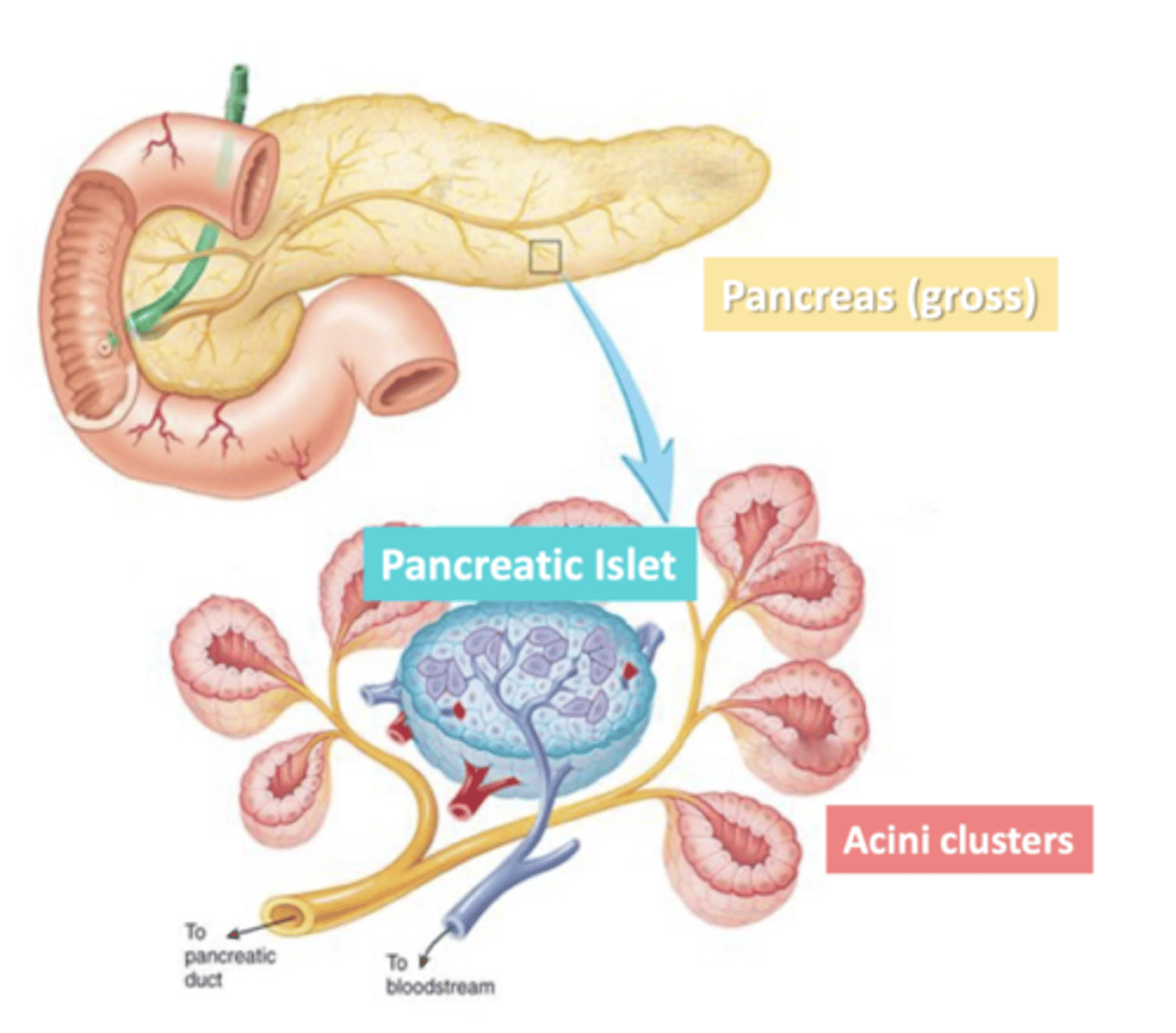
Acini
clusters of exocrine cells
-secrete digestive (pancreatic) juice through pancreatic duct
-surrounded a duct they secrete into
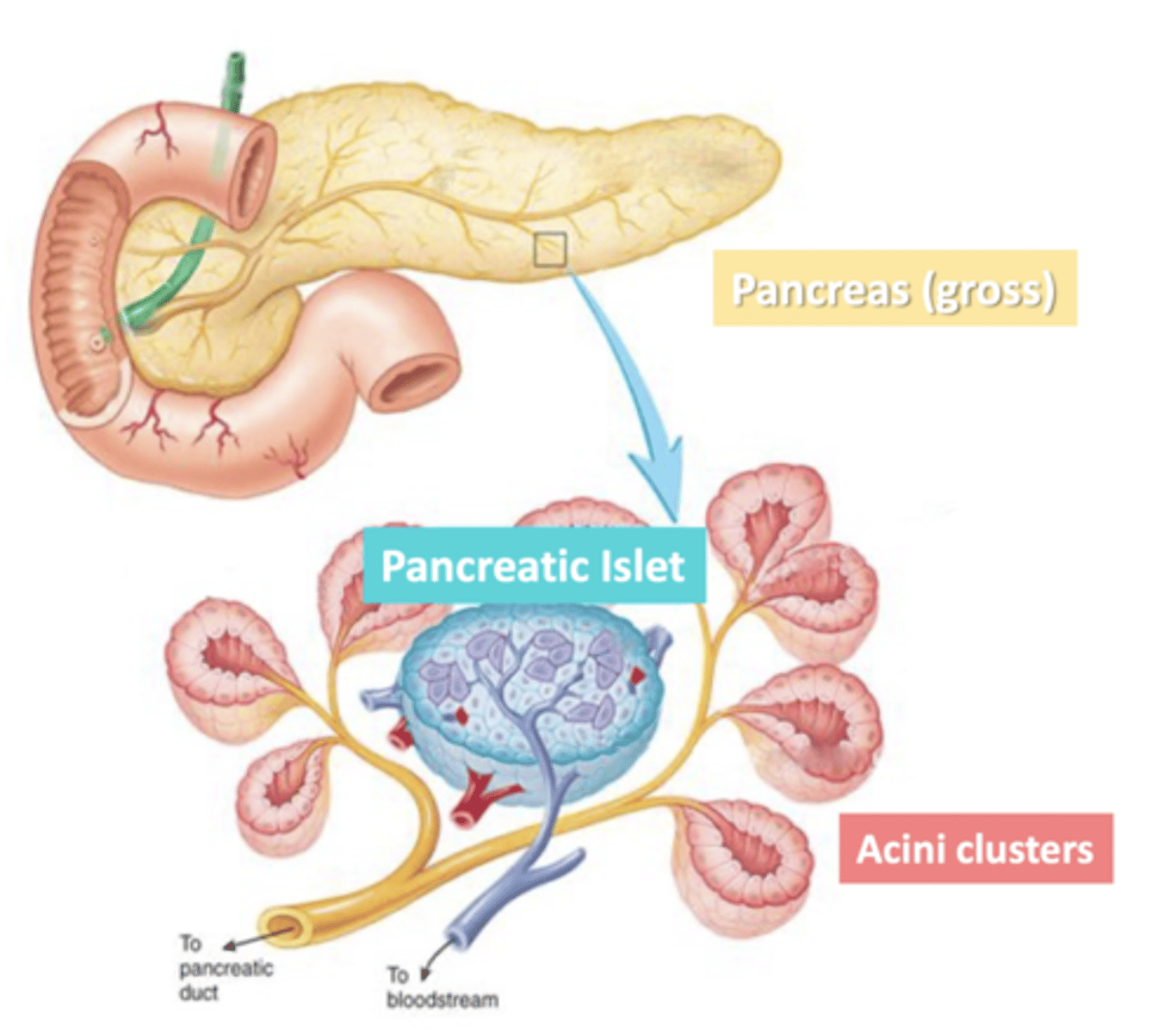
Pancreatic Islets
clusters of endocrine cells
-secrete hormones to regulate blood sugar
Pancreatic Juice
-Water
-Salts
-Sodium Bicarbonate
-Digestive enzymes to break down:
--starch, proteins, triglycerides, DNA/RNA
what is the function of sodium bicarbonate produced by pancrease
to neutralize acid, duodenal contents come straight from stomach and are highly acidic.
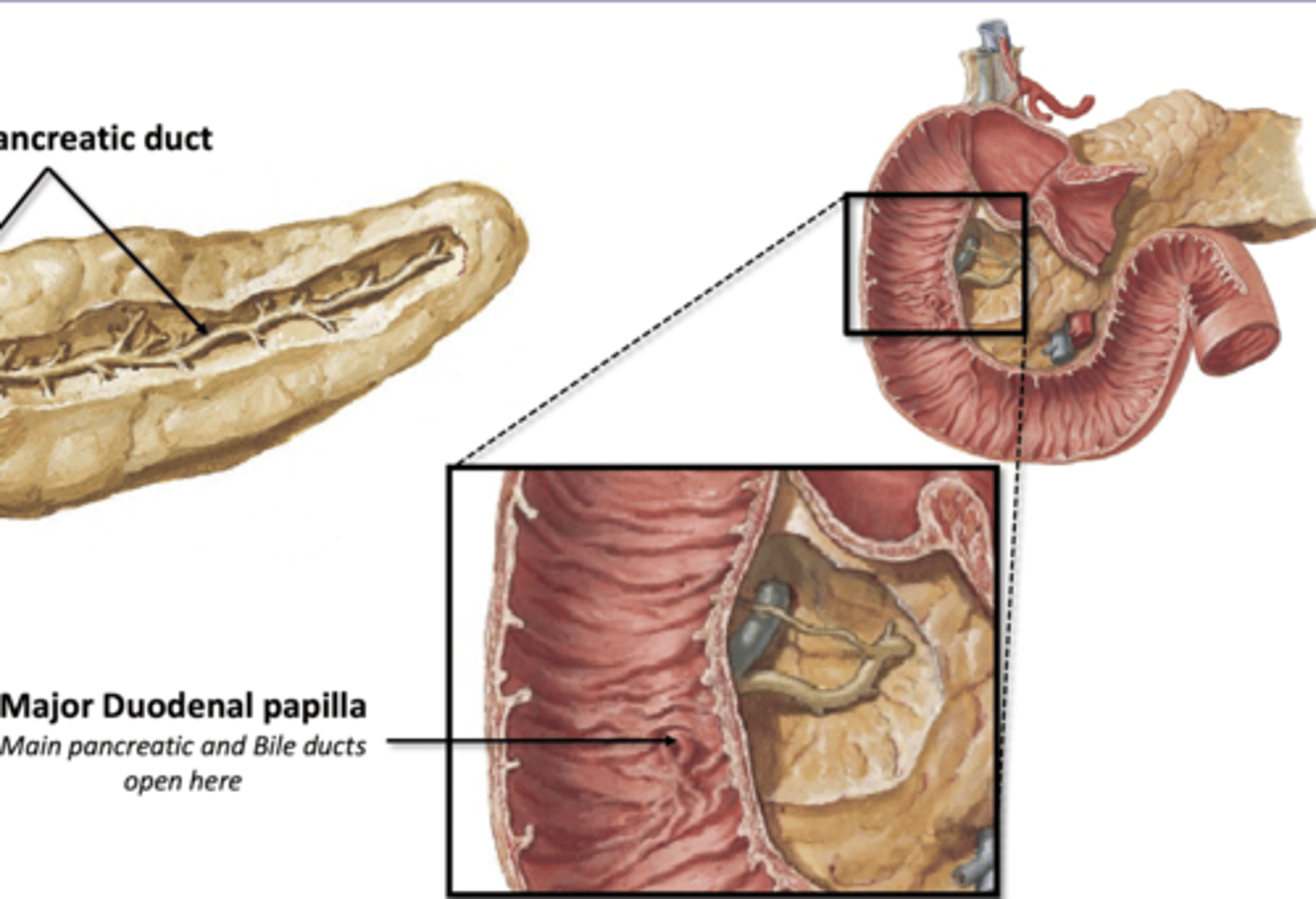
Pancreatic Ducts
Main pancreatic duct- joins with bile duct from liver to enter duodenum together
Accessory Pancreatic Duct
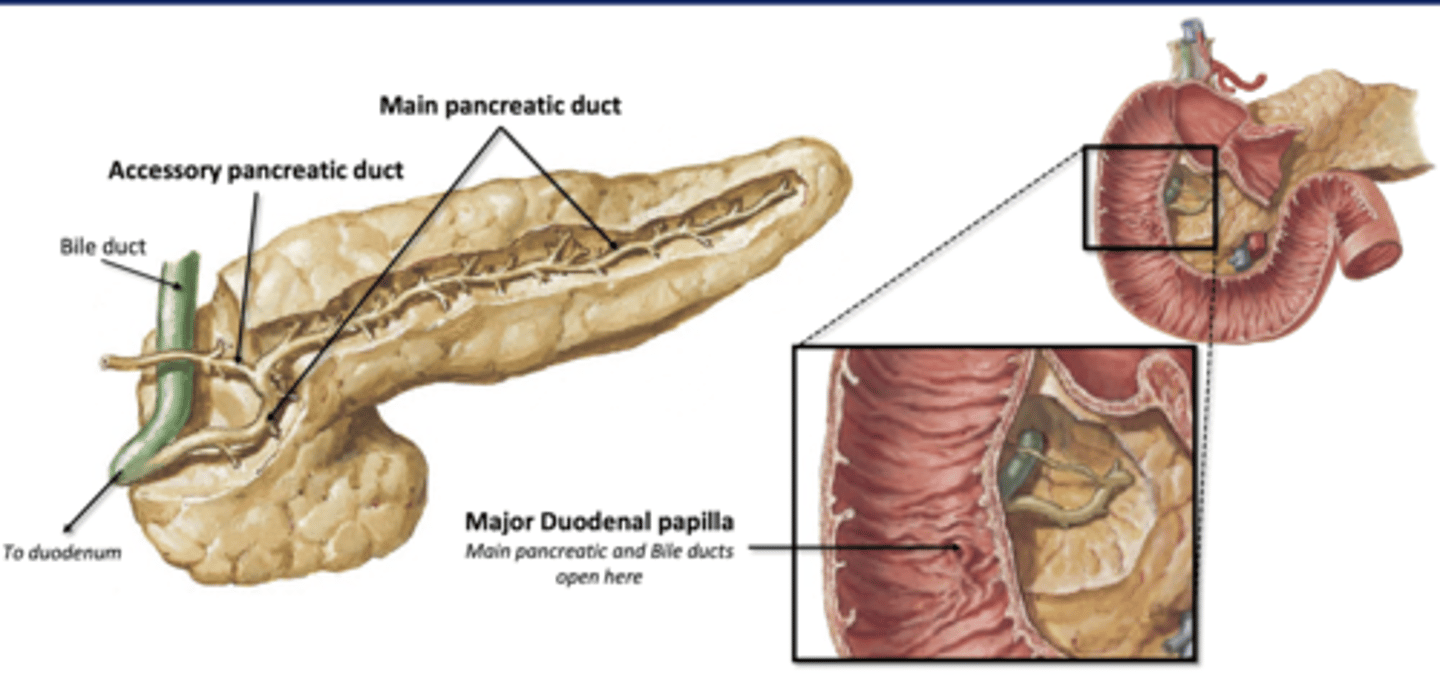
Major Duodenal Papilla
Where main pancreatic and bile ducts enter the duodenum
-guarded by sphincter muscle
-only opens after a meal
Liver Functions
Blood filtration, excretion, metabolism, storage, secretes bile
-secretion and chemical digestion
Liver Innervations/Vasculature
Parasymp: Vagus
Symp: thoracic splanchnics, synapse at celiac ganglion
Artery: celiac trunk bb
Vein: portal vein
Features of Liver
-gallbladder sits on inferior surface (bile storage)
Right and Left lobe, separated by falciform ligament
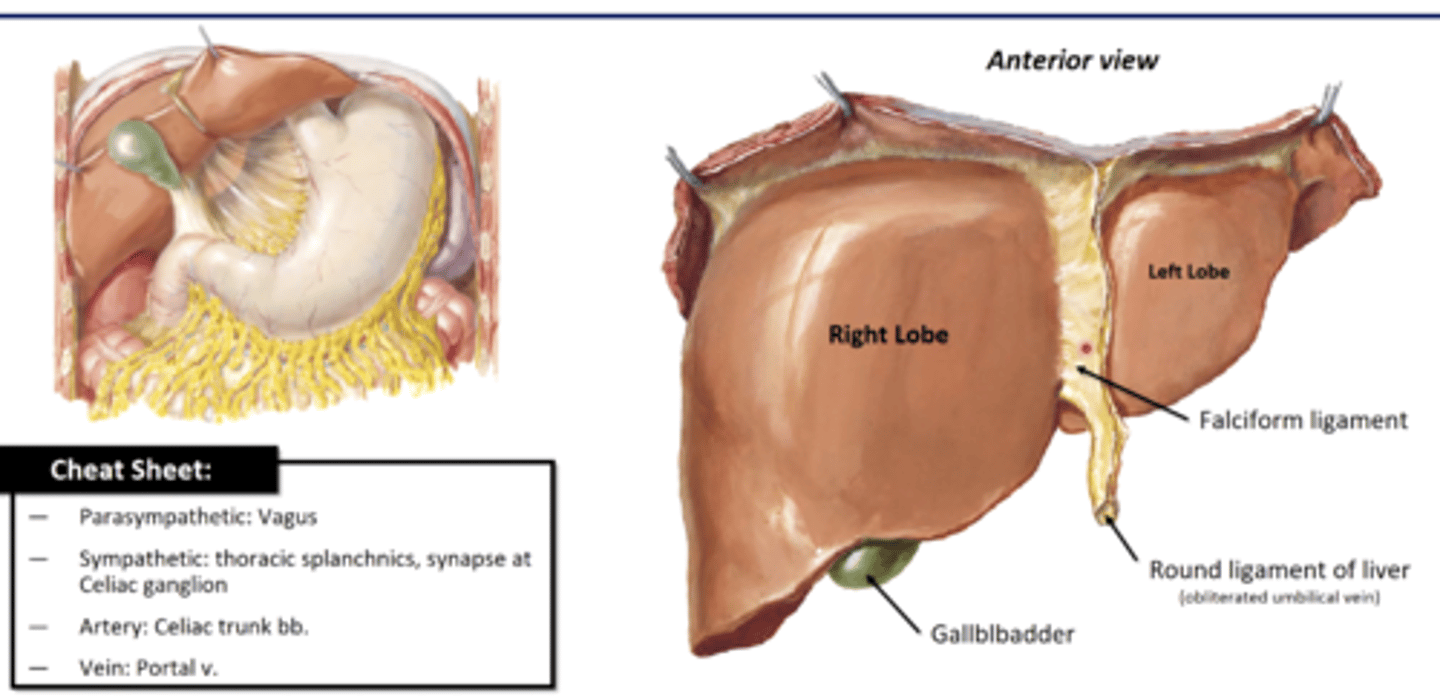
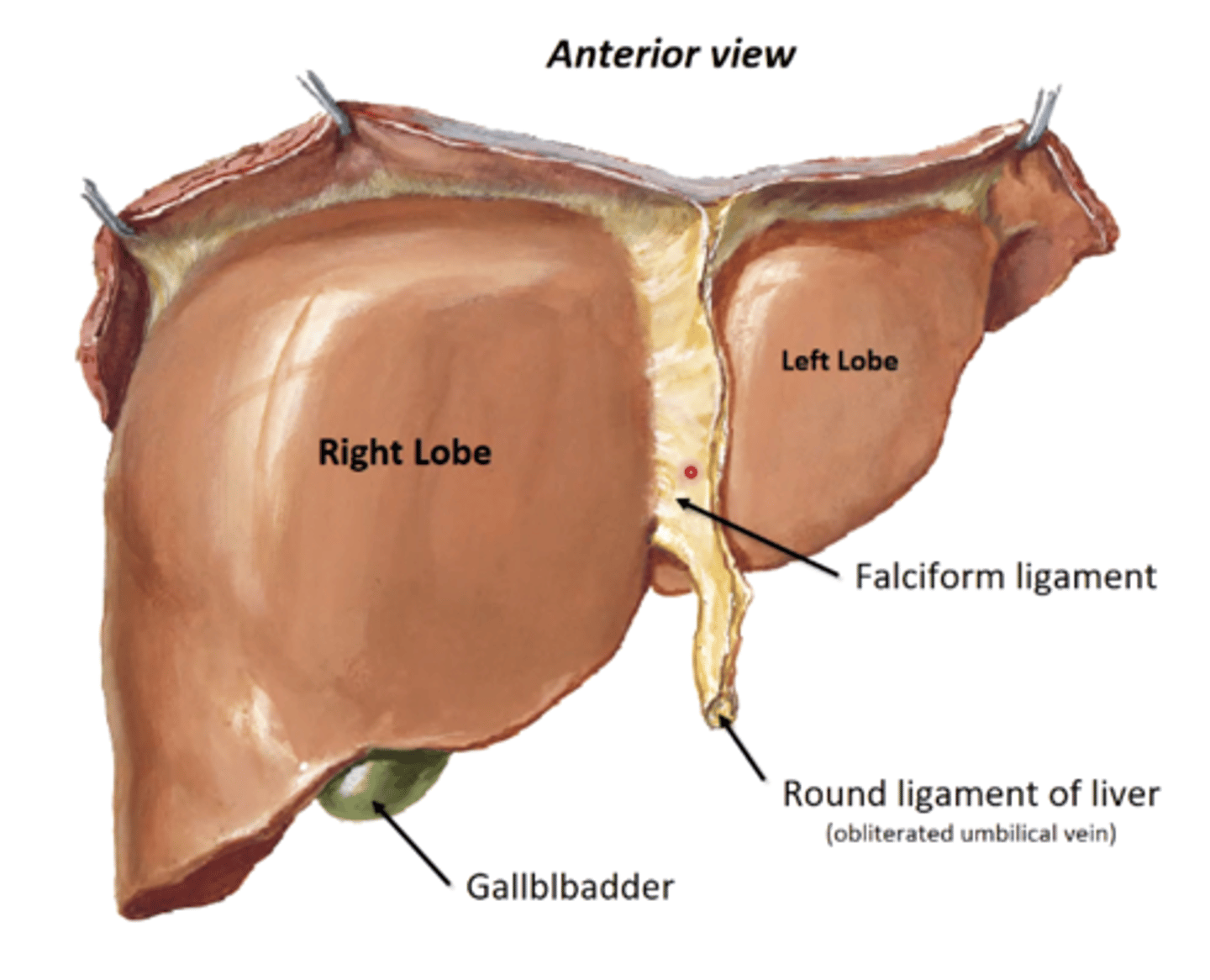
Falciform ligament
-separates R and L lobes of liver
-double fold of peritoneum that attaches liver to ant. abdominal wall
-has Round ligament of liver (obliterated umbilical vein) running in lower margin
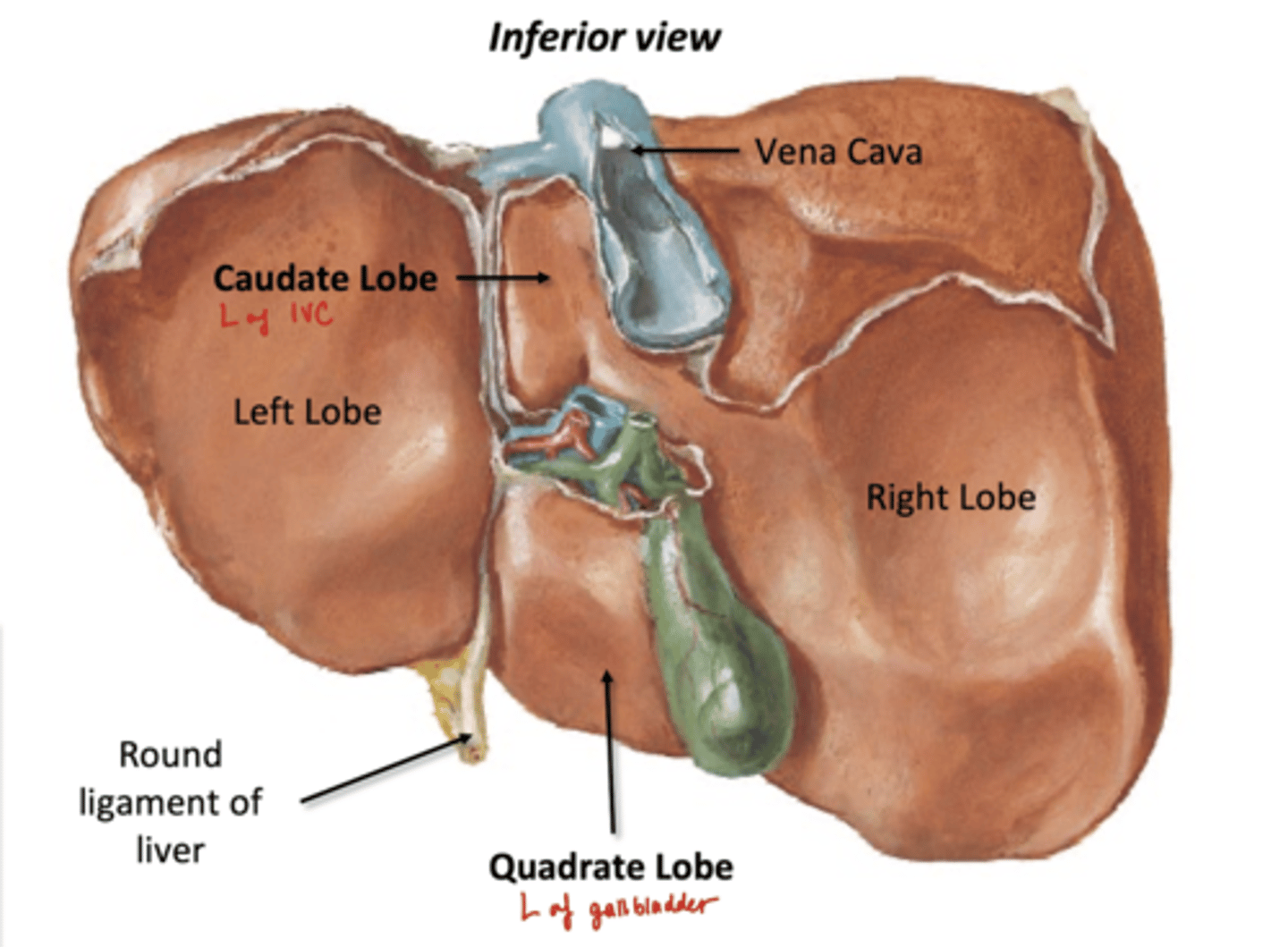
Inferior Surface of Liver
Individual lobes, but part of Left lobe
-Caudate Lobe- left of IVC
-Quadrate Lobe- left of gallbladder
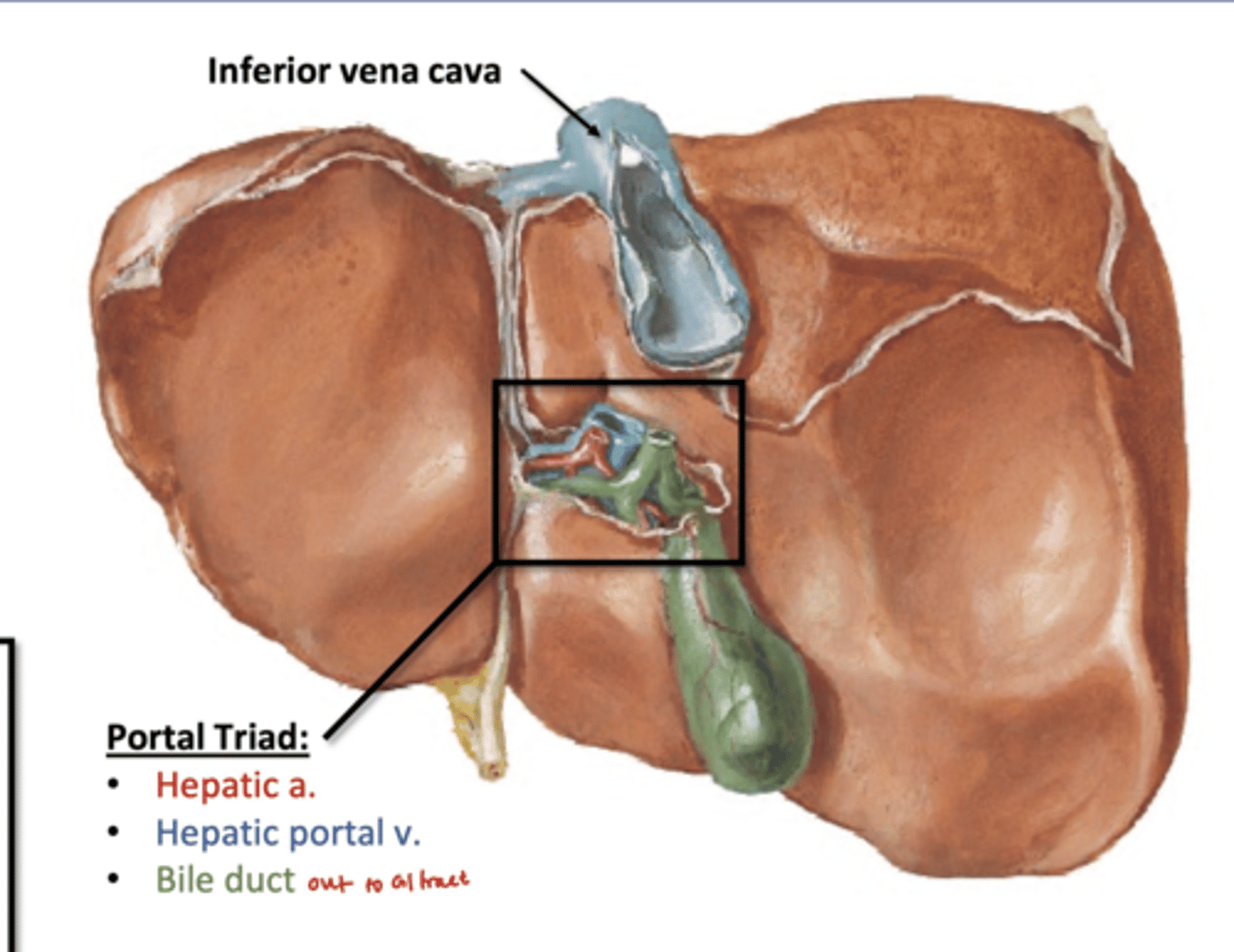
Porta Hepatitis: hilum of liver
Portal Triad
Through Porta Hepatitis:
portal vein, hepatic artery, bile duct
-bile duct carry bile out to GI tract
-hepatic a supplies arterial blood to liver
-portal vein drains all of digestive organs