Urinary system, female and male reproductive and endocrine system slides (description)
1/22
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
23 Terms
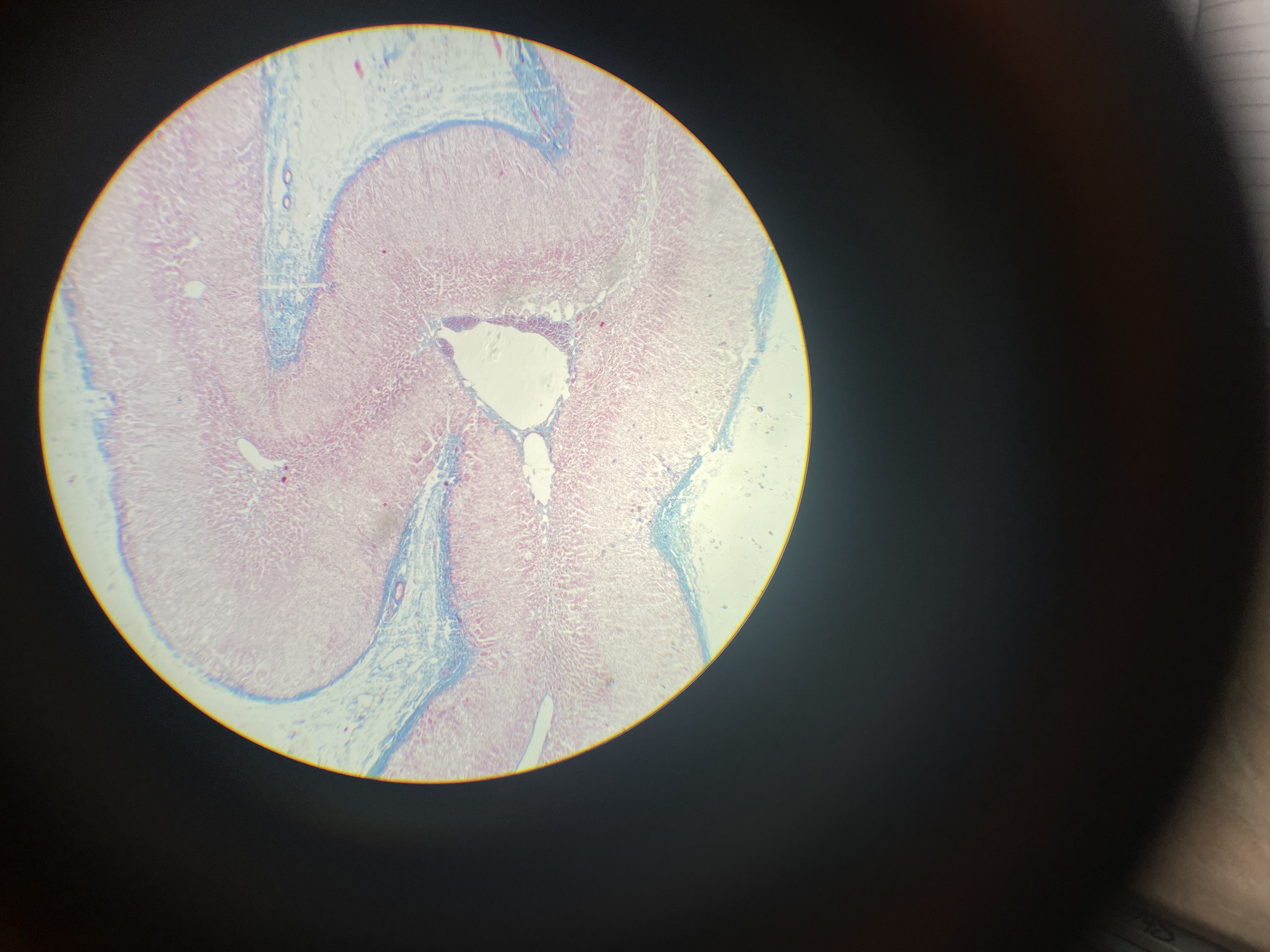
13a) glandula suprarenalis - azan
Outer Capsule - thin CT
Cortex (3 Zones):
Zona Glomerulosa (Outer):
closely packed columnar/pyramid cells (aldosterone and other mineralocorticoids).
Zona Fasciculata (Middle):
Large cells in columns/cords (cortisol and other glucocorticoids).
Zona Reticularis (Inner):
cells with acidophilic cytoplasm, in cords or clumps
secrete androgens
Medulla:
Chromaffin cells (secrete epinephrine/norepinephrine).
Large, pale-staining cells with granular cytoplasm.
supported by reticular fibres
medullary vessels (large veins drain organ)
Glomerulosa - SALT (androgens)
Fasciculata - SUGAR (cortisol)
Reticularis - SEX (androgens)

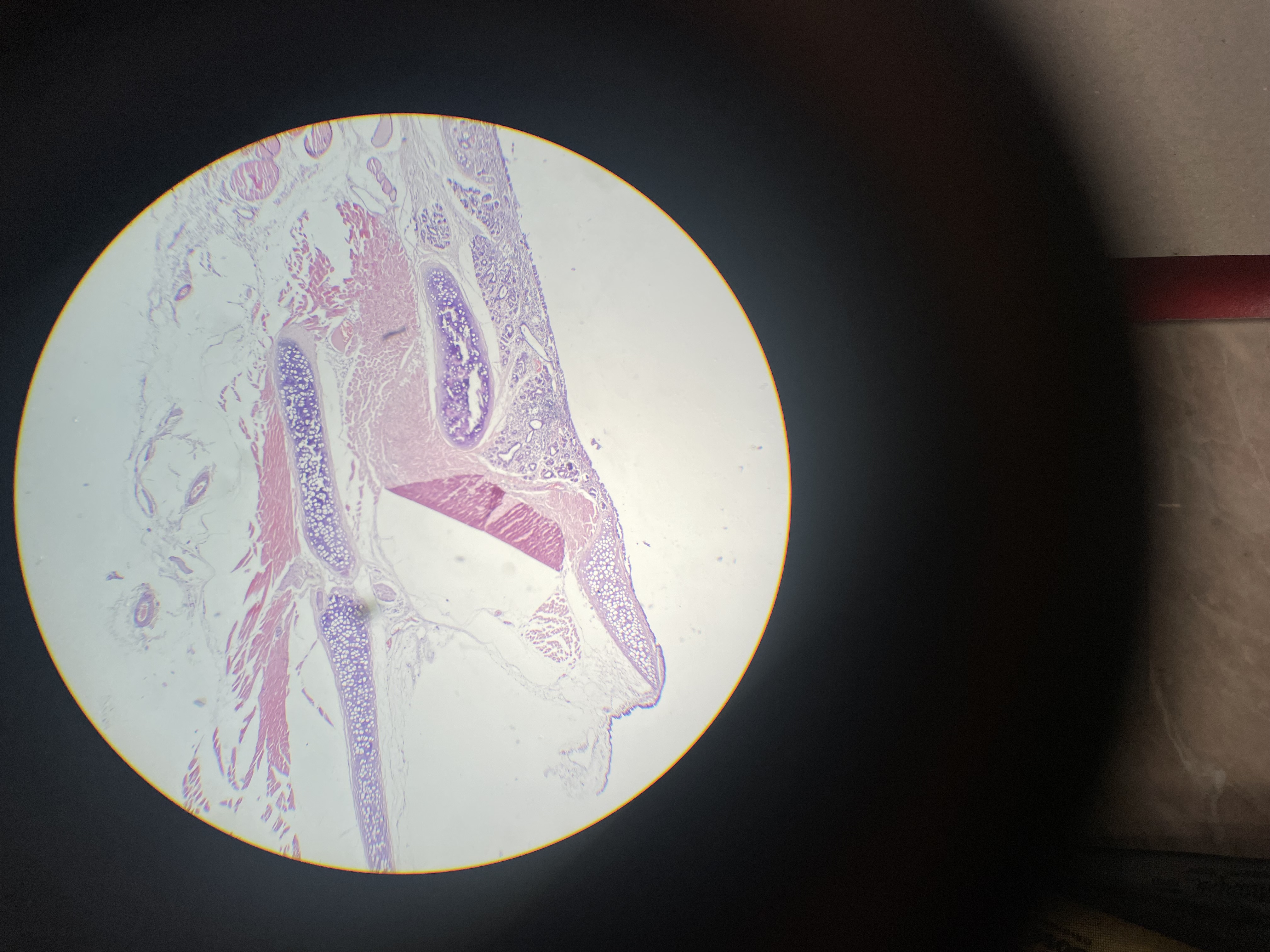
Thyroid gland - Azan
Made up of a stroma and a parenchyma. Stores its hormones.
Stroma- divided into lobes and lobules
Parenchyma - consists of:
follicular or principal
parafollicular or c cells
Stroma:
capsule - enclosed by a thin layer of CT (true and false)
trabeculae - CT extends inwards from the capsule to partially outline irregular lobes and lobules
Parenchyma:
Secretory follicles constitute the functional units of the gland
thyroid follicles - spherical follicles of varying size in which thyroid hormones are stored
thyrocytes (follicular cells) - follicles are lined by simple cuboidal to columnar epithelium, depending on function
thyrocytes secrete thyroid hormones when activated
parafollicular cells —> secrete calcitonin
colloid - the lumen of each follicle is filled with the gel-like mass called colloid
Capillaries surround each follicle
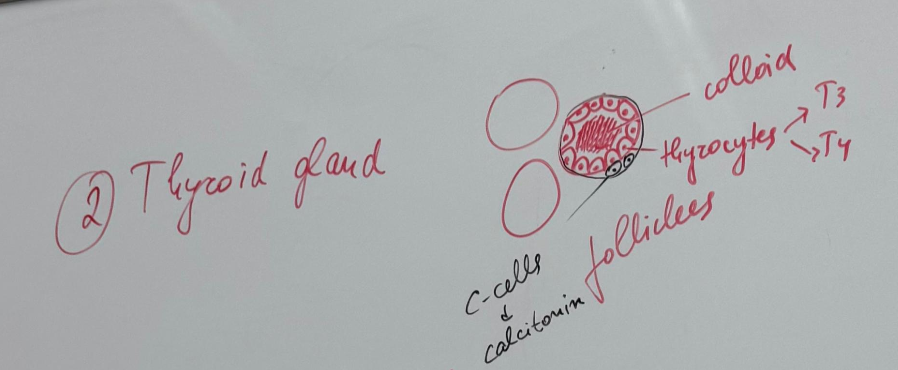
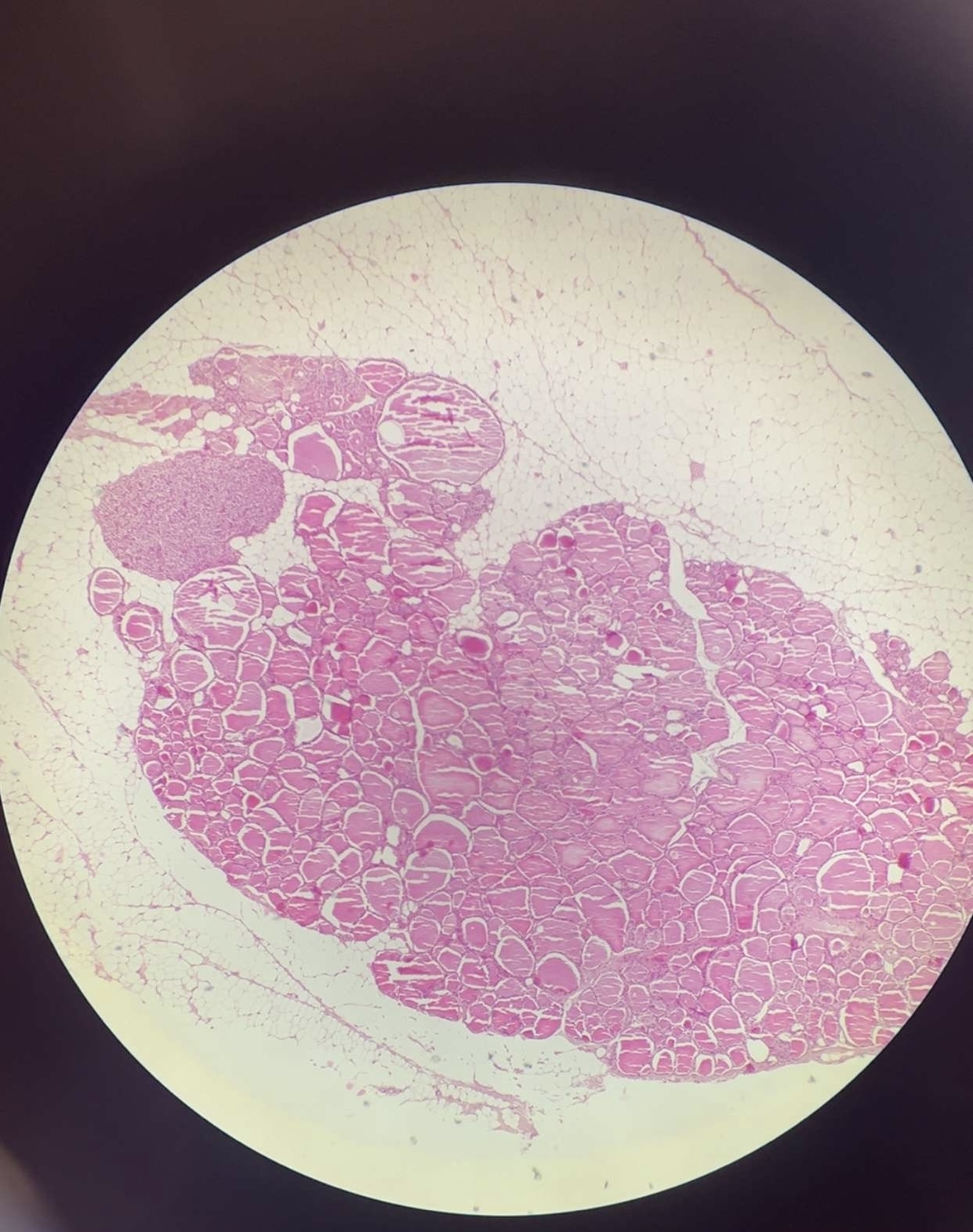
Thyroid gland - HE
Made up of a stroma and a parenchyma. Stores its hormones.
Stroma- divided into lobes and lobules
Parenchyma - consists of:
follicular or principal
parafollicular or c cells
Stroma:
capsule - enclosed by a thin layer of CT (true and false)
trabeculae - CT extends inwards from the capsule to partially outline irregular lobes and lobules
Parenchyma:
Secretory follicles constitute the functional units of the gland
thyroid follicles - spherical follicles of varying size in which thyroid hormones are stored
thyrocytes (follicular cells) - follicles are lined by simple cuboidal to columnar epithelium, depending on function
thyrocytes secrete thyroid hormones when activated
parafollicular cells —> secrete calcitonin
colloid - the lumen of each follicle is filled with the gel-like mass called colloid
Capillaries surround each follicle
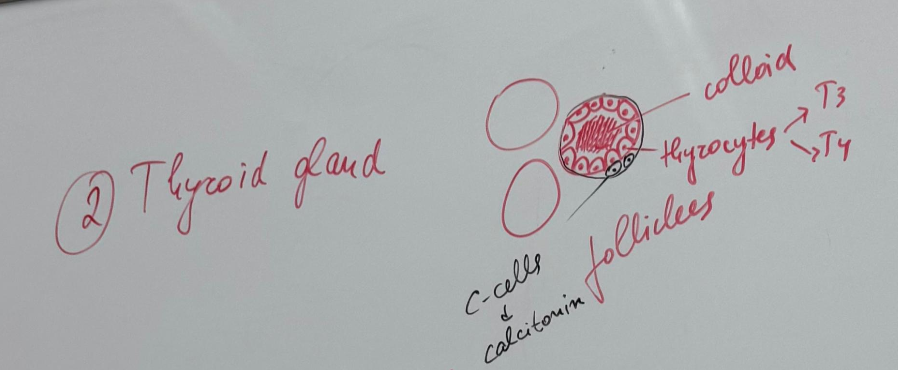
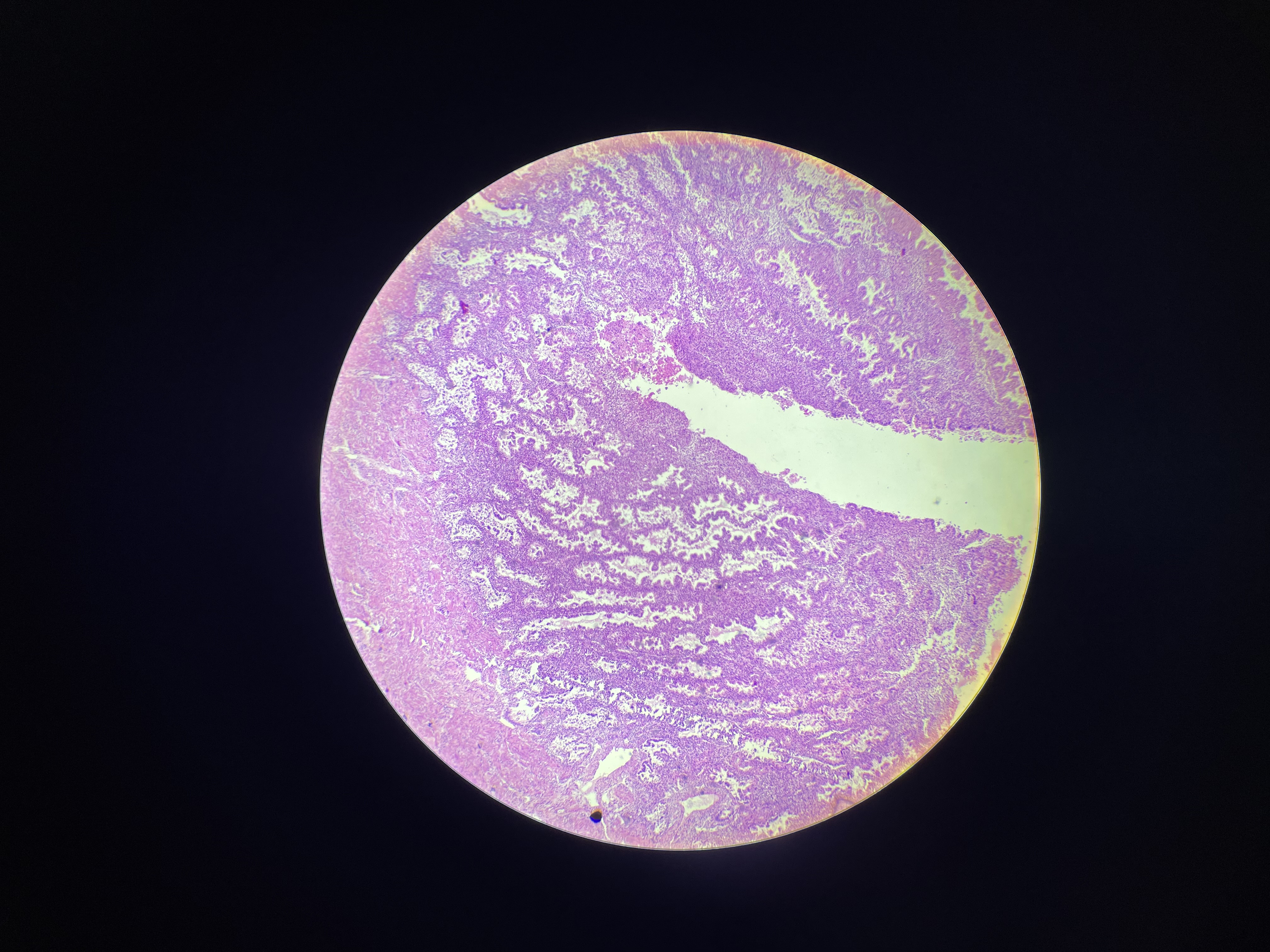
39) Uterus (secretory phase) - HE
Uterine wall is composed of 3 layers:
1) Endometrium: specialized mucosa that undergoes marked changes during menstrual cycle
functional layer: the upper 2/3 of the mucosa that develops
13) glandula suprarenalis - HE
Cortex (3 Zones):
Zona Glomerulosa (Outer):
Small, clustered cells (mineralocorticoids → aldosterone).
Zona Fasciculata (Middle):
Large, lipid-rich cells in columns (glucocorticoids → cortisol).
Zona Reticularis (Inner):
Dark, compact cells in nets (androgens).
Medulla:
Chromaffin cells (secrete epinephrine/norepinephrine).
Large, pale-staining cells with granular cytoplasm.
Central adrenomedullary vein (thin-walled, prominent).
• Medulla – Large blood vessels, Basophilic cells, well-developed granular endoplasmic reticulum, mth, vesicles - noradrenergic - dark, small, and adrenergic - large, light – produce adrenalin and noradrenaline

63) hypophysis/pituitary gland - HE
• The Adenohypophysis :
I. Chromophobic cells - grayish in
color - about 50% of all cells do not contain
granules, weakly stained, undifferentiated -
they are considered to be precursors of
chromophilic cells
II. Chromophilic cells
1. Acidophilic cells - red in color
a. Somatotropin-producing cells – produce
growth hormone
b. Lactotropic (mammotropic) cells -
produce prolactin
2. Basophilic cells - blue and red colored
a. Thyrotropic cells – release thyroid stimulating hormone - thyrotropin
b. Gonadotropic cells - produce luteinizing
hormone and follicle-stimulating hormone
c. Corticotropin cells - release corticotropic
hormone
I. Acidophilic cells - red in color
1. Somatotropin-producing cells – produce growth hormone, ovoid shape, centrally located nucleus, well-developed Golgi apparatus, large dense vesicles.
2. Lactotropic (mammotropic) cells – produce prolactin, multiple secretory granulosum of irregular shape.
II. Basophilic cells - large cells with pale blue colored basophilic granules.
1. Thyrotropic cells - release thyroidstimulating hormone - thyrotropin, relatively large cells, small, light, irregularly shaped granules, located peripherally.
2. Gonadotropic cells - produce luteinizing hormone and follicle-stimulating hormone, pleomorphic nuclei, well-developed Golgi apparatus, granular endoplasmic reticulum, secretory granules arranged like a rosary under the cell membrane, 200-400nm.
3. Corticotropic cells - release corticotropic hormone, polygonal shape, well-developed Golgi apparatus, granular endoplasmic reticulum, eccentric nucleus, large secretory granules, 400- 500 nm
Neurohypophysis:
• is built from nerve fibers and glial cells.
• They are separated in it the hormones of n. supraopticus et paraventriculris – the antidiuretic hormone and oxytocin

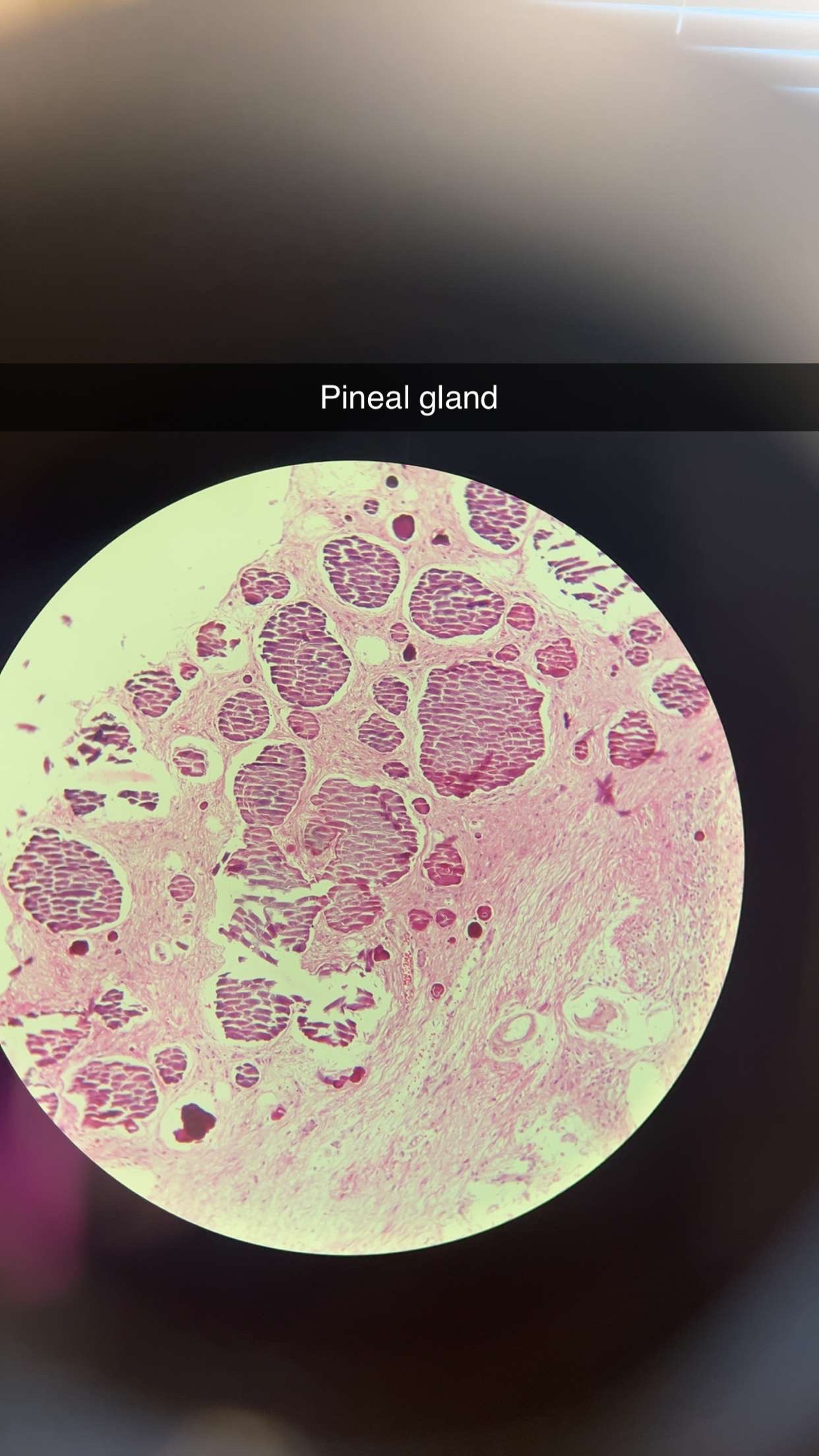
64) epiphysis/pineal gland - HE
Stroma - CT capsule gives septs, that divide the parenchyma
into lobes - lobuli
• Parenchyma - contains 2 main types of cells - pinealocytes and
astrocytes
• Pinealocytes have a cell body and 4-6 processions. There are
2 types of pinealocytes - type I and type II, and they are
classified according to different characteristics, including the
shape, presence or absence of folds of the nuclear membrane
and the structure of the cytoplasm.
• Type I - light pinealocytes - contain the neurotransmitter
serotonin, which is converted to melatonin, the main hormone
secreted by the pineal gland.
• Type II pinealocytes are known as dark pinealocytes because
they are more strongly stained and appear darker under a light microscope; contain melatonin in the dark
• In the interior of the lobes, corpora arenacea ("brain sand") -
calcium-containing formations - can be seen
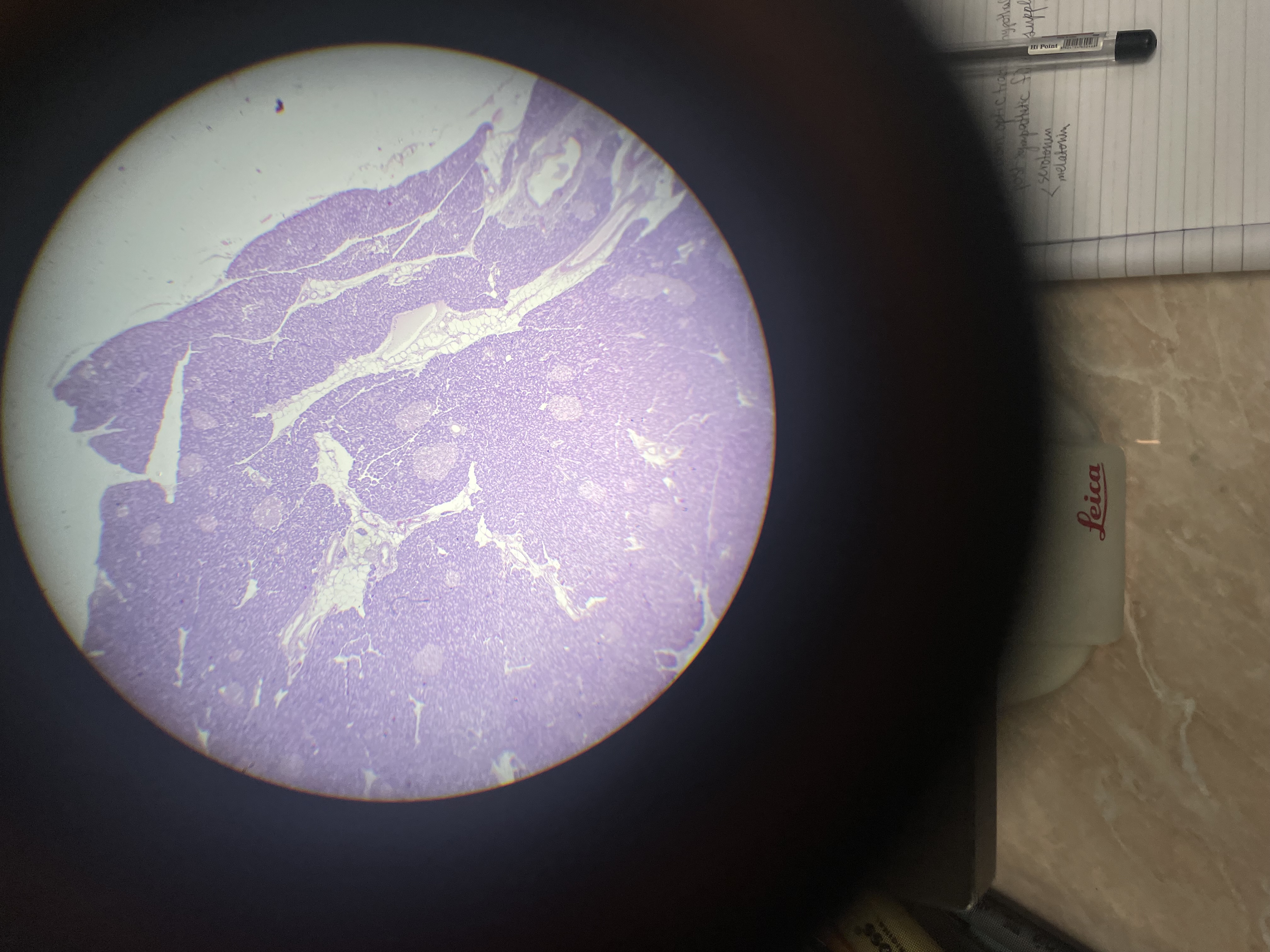
47a) pancreas - PAF
Exocrine Pancreas:
Serous Acini:
Pyramidal cells with basal nuclei and apical zymogen granules (digestive enzymes).
Centroacinar cells (pale-staining, part of intercalated ducts).
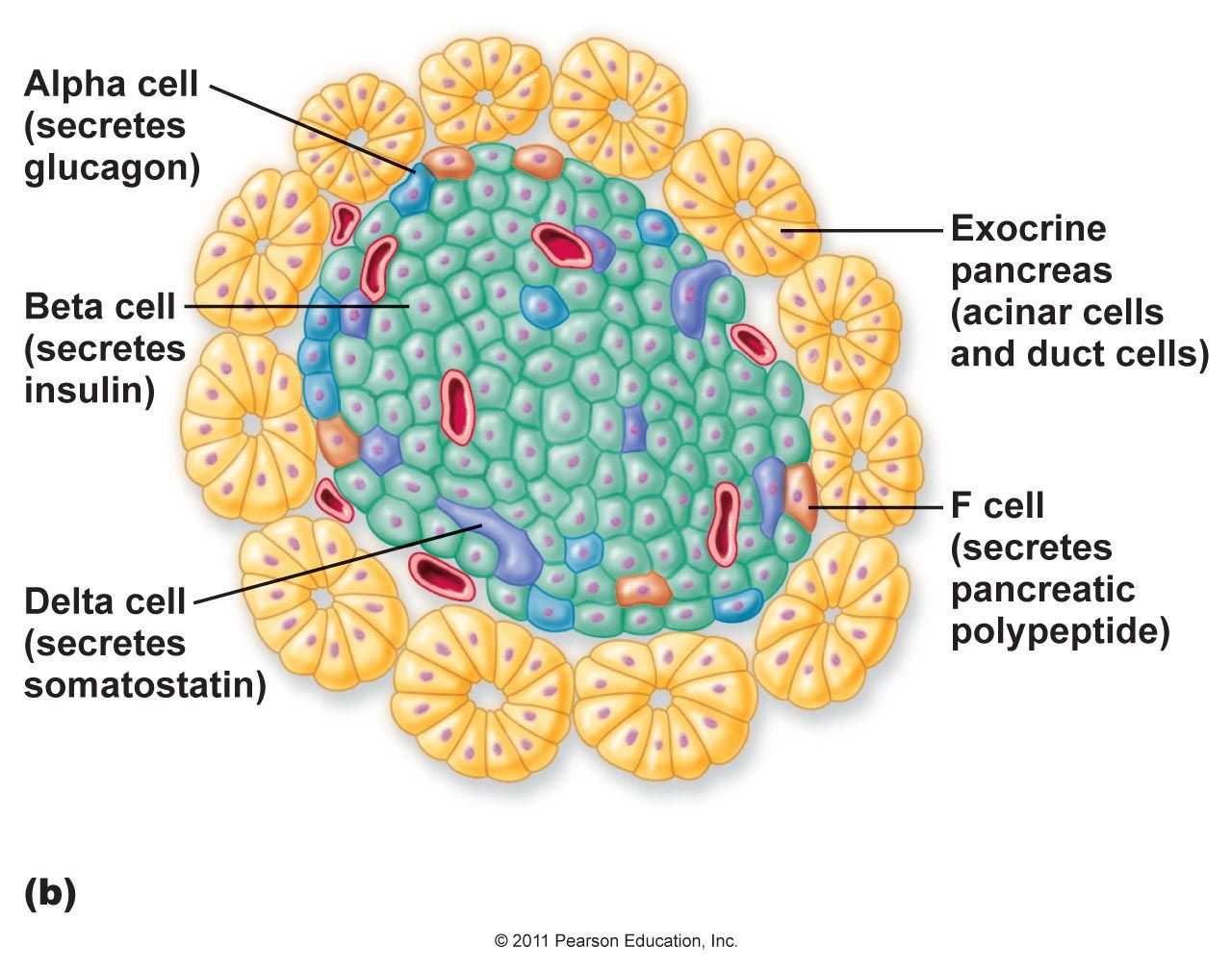
Endocrine Pancreas (Islets of Langerhans):
α (Alpha) Cells:
located peripherally, acidophilic granules with a mesh core and a narrow light halo peripherally (secrete glucagon → PAF: red/pink).
β (Beta) Cells:
basophilic granules with a dense core and a wide light halo peripherally, sometimes crystals with a rectangular shape (secrete insulin → PAF: blue/purple).
D- somatostatin:
irregular shape, larger less
dense granules without halo
PP-
pancreatic polyleptide, polygonal shape,
peripheral localization, small granules
D1-
vasoactive intestinal peptide
EC-
secretin, motilin, substance P
Type cells of GASTRO-ENTERO-PANCREATIC ENDOCRINE SYSTEM:
• G cells- gastrin, enkefalin; in duodenum and jejunum; stimulate secretion of pancreas, stomach and duodenum
• S cells –secretin; in duodenum jejunum; stimulate secretion of pepsinogen and bile
• I cells- cholecystokinin-pancreosymin; in duodenum and jejunum; stimulate secretion of bile, motility of bile bladder and concentration of enzymes from pancreas
• PP cells- pancreatic polypeptide; in duodenum and pancreas
• EC2 cells- motilitin and serotonin; in duodenum and jejunum • L cells- enteroglucagon; in small and large intestine
• D cells- somatostatin; in stomach, duodenum, jejunum, endocrine pancreas
• D1 cells- VIP, in all parts of gastrointestinal tract and endocrine pancreas
• K cells- stomach inhibitor peptide; in duodenum and jejunum
• M cells- neurotensin; in jejunum and ileum
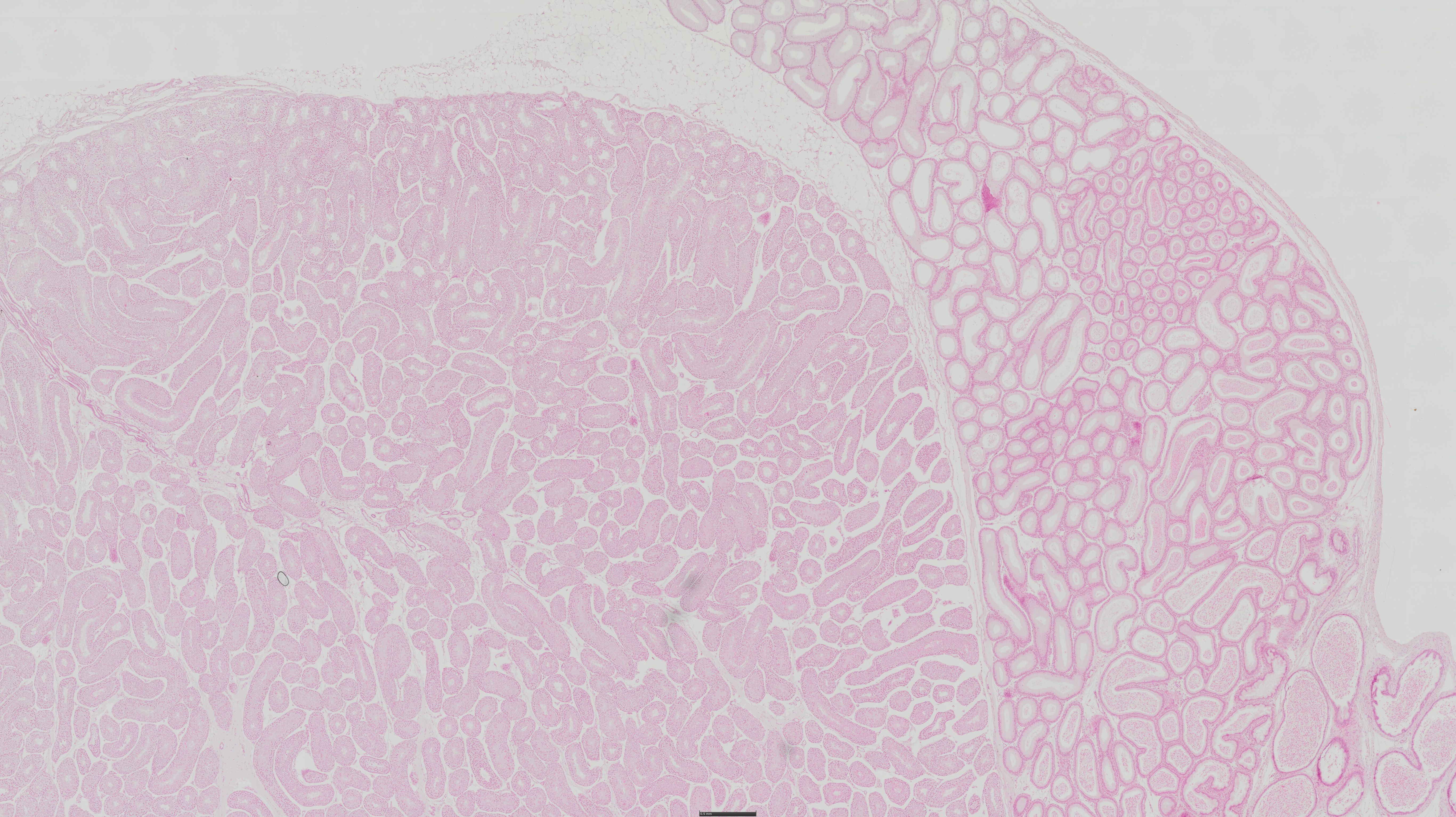
16) testis - HE
Covered from outside by CT capsule – tunica albuginea gives
septi, which divide the gland into lobules
Lobulus consists of:
1. tubuli seminiferi contorti – made up of multilayered
spermatogenic epithelium lying on the basement membrane,
consisting of 2 types of cells:
- Sertoli cells –, tall, columnar cell with euchromatic
ovoid or triangular nucleus, supporting cells, Sertoli –to- Sertoli junctions form the blood-testicular barrier
- spermatogenic cells– in different phases of
development – spermatogonia (type A dark and pale),
spermatogonia type B, spermatocytes (primary and
secondary) spermatids, spermatozoa
In the interstitium - between the convoluted tubules, there are
groups of endocrine cells - Leydig's cells- large, polygonal with eosinophilic nucleus, lipid droplets in cytoplasma
Tubuli recti – covered with a single-layer cubic epithelium,
builds rete testis
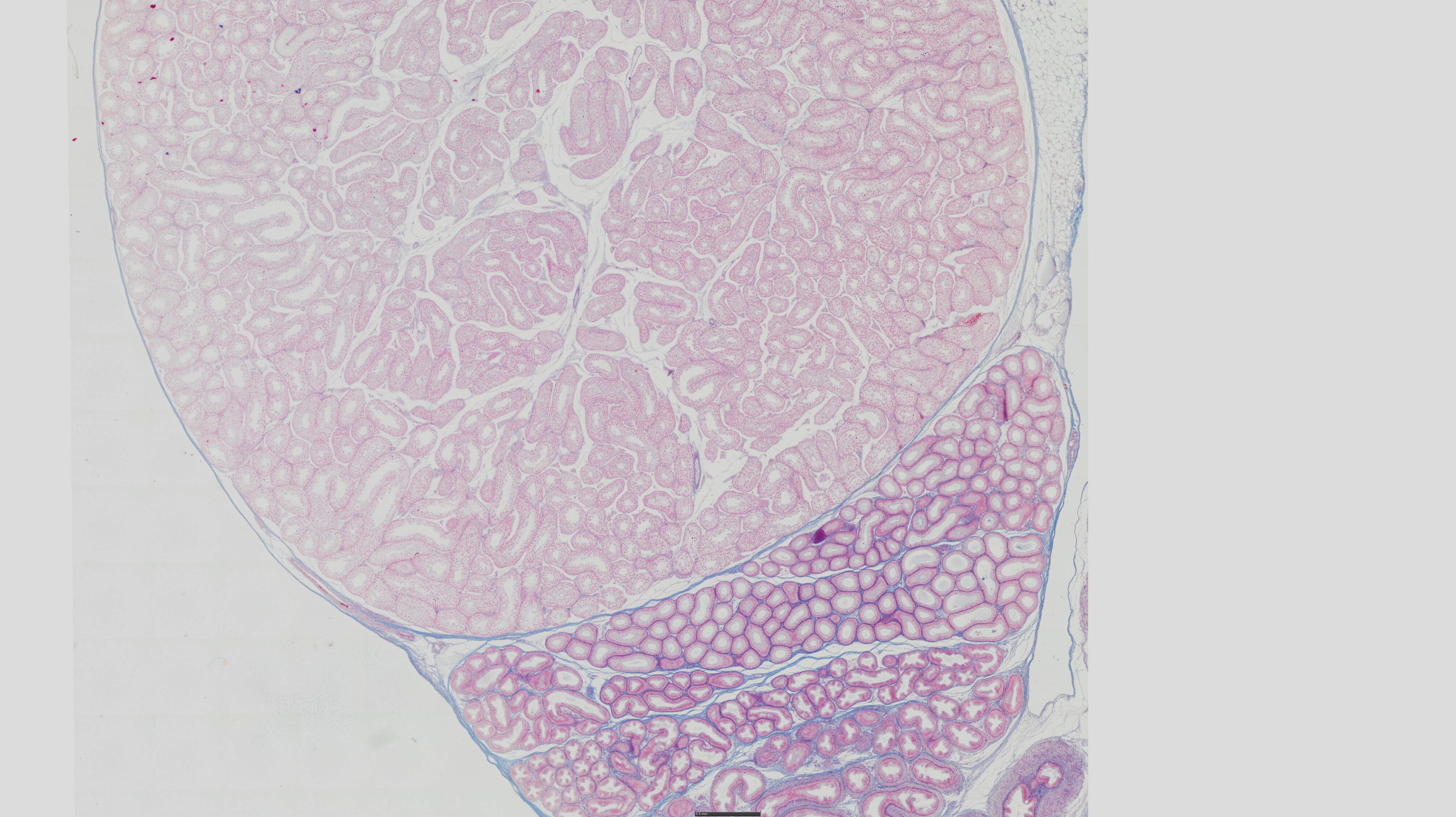
16) testis - azan
Covered from outside by CT capsule – tunica albuginea gives
septi, which divide the gland into lobules
Lobulus consists of:
1. tubuli seminiferi contorti – made up of multilayered
spermatogenic epithelium lying on the basement membrane,
consisting of 2 types of cells:
- Sertoli cells –, tall, columnar cell with euchromatic
ovoid or triangular nucleus, supporting cells, Sertoli –to- Sertoli junctions form the blood-testicular barrier
- spermatogenic cells– in different phases of
development – spermatogonia (type A dark and pale),
spermatogonia type B, spermatocytes (primary and
secondary) spermatids, spermatozoa
In the interstitium - between the convoluted tubules, there are
groups of endocrine cells - Leydig's cells- large, polygonal with eosinophilic nucleus, lipid droplets in cytoplasma
Tubuli recti – covered with a single-layer cubic epithelium,
builds rete testis
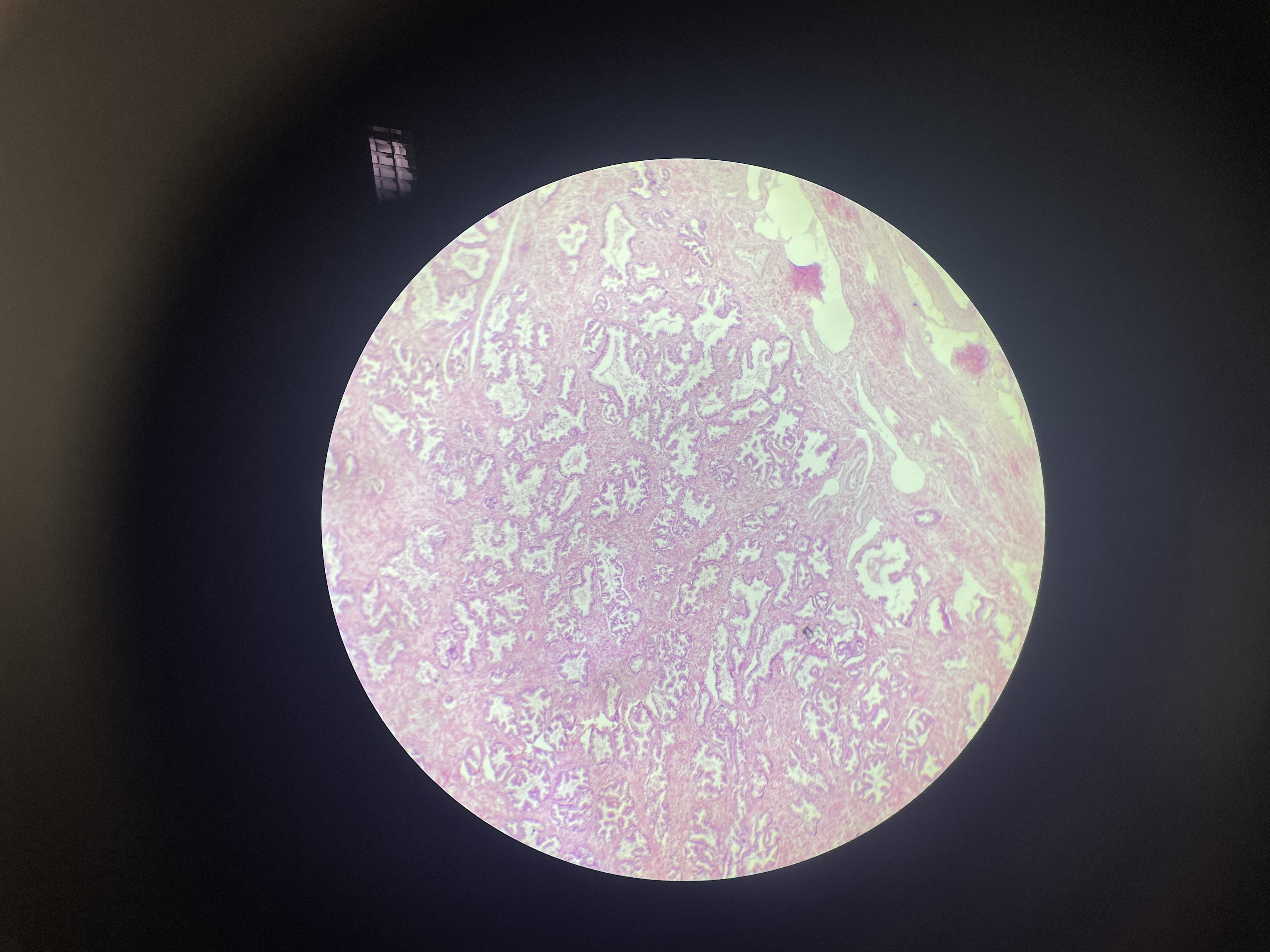
66) prostata - HE
Capsula prostatica
Stroma mylolastica (substantia muscularis) –connective tissue and smooth muscle cells
Parenchyma – smooth muscle cells and substantia glandularis – 3 layers glands:
periurethral (central )zone – gl. urethales
transitional zone- submucous glands
peripheral zone –gl. prostaticae- branched tubular glands, covered by simple columnar epithelium
In the glands, corpora amylacea (amyloid bodies) made of calcified glycoproteins, are observed
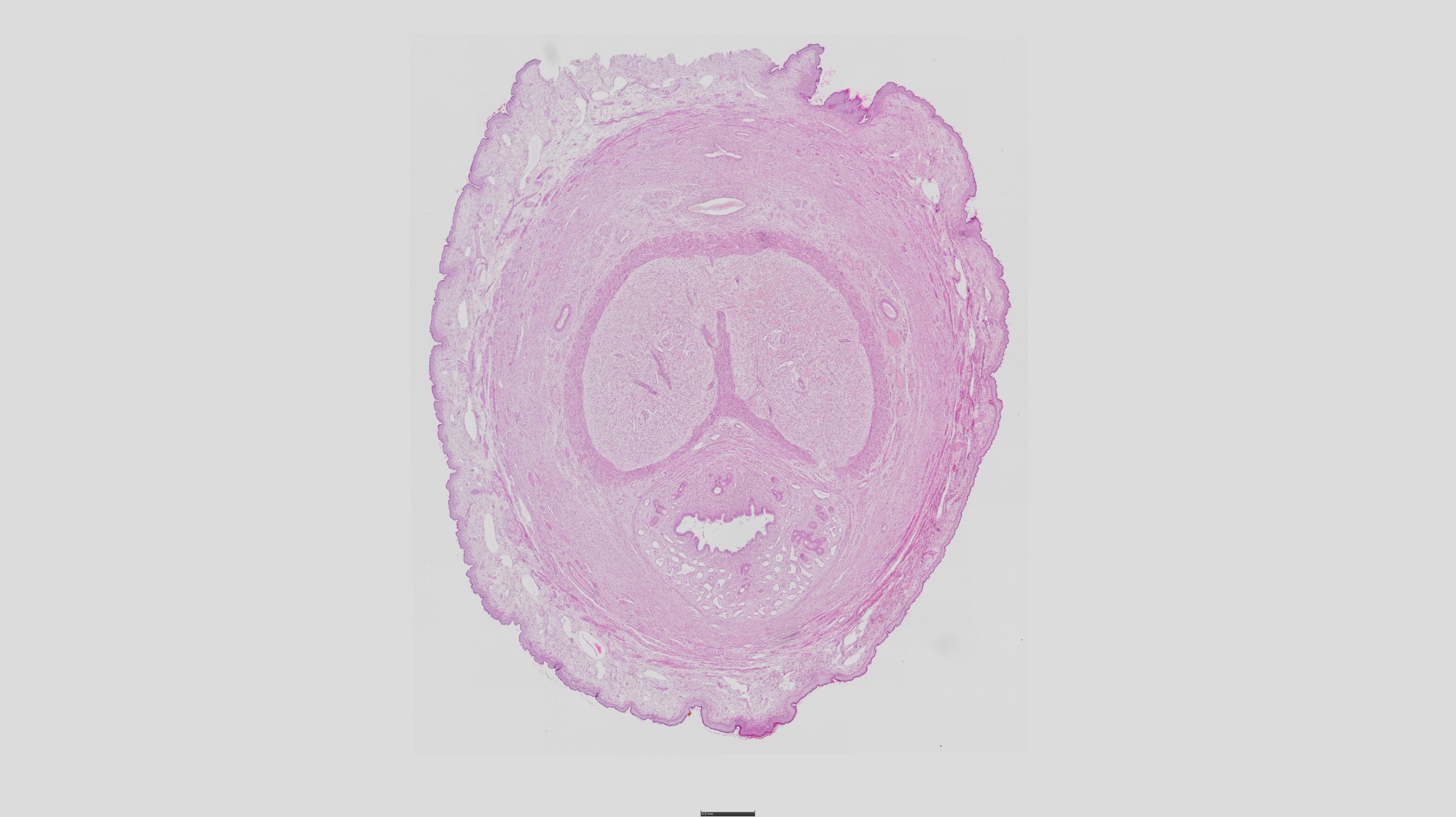
67) penis - HE
• Fascia penis – СТ trabeculae
• Corpora cavernosa –
• Tunica albuginea corporum cavernosum – elastic and collagen fibers
• Corpus cavernosi - made up of dense CTtrabeculae also containing muscle fibers, cavities lined from endothelium
• Corpus spongiosum –
• Tunica albuginea corpori spongiosi – elastic and collagen fibers; thinner than the white coat of corpus cavernosum, but with more elastic fibers
• Cavernae corpus spongiosi – cavities lined from endothelium, cavities surrounded by CTtrabeculae
• Urethra masculina – -The initial part (up to the colliculus urethralis) is covered by a transitional epithelium of Henle -Spongy part – covered by a single-layer cylindrical epithelium -End part (in fossa navicularis) –stratified squamous nonkeratinized epithelium
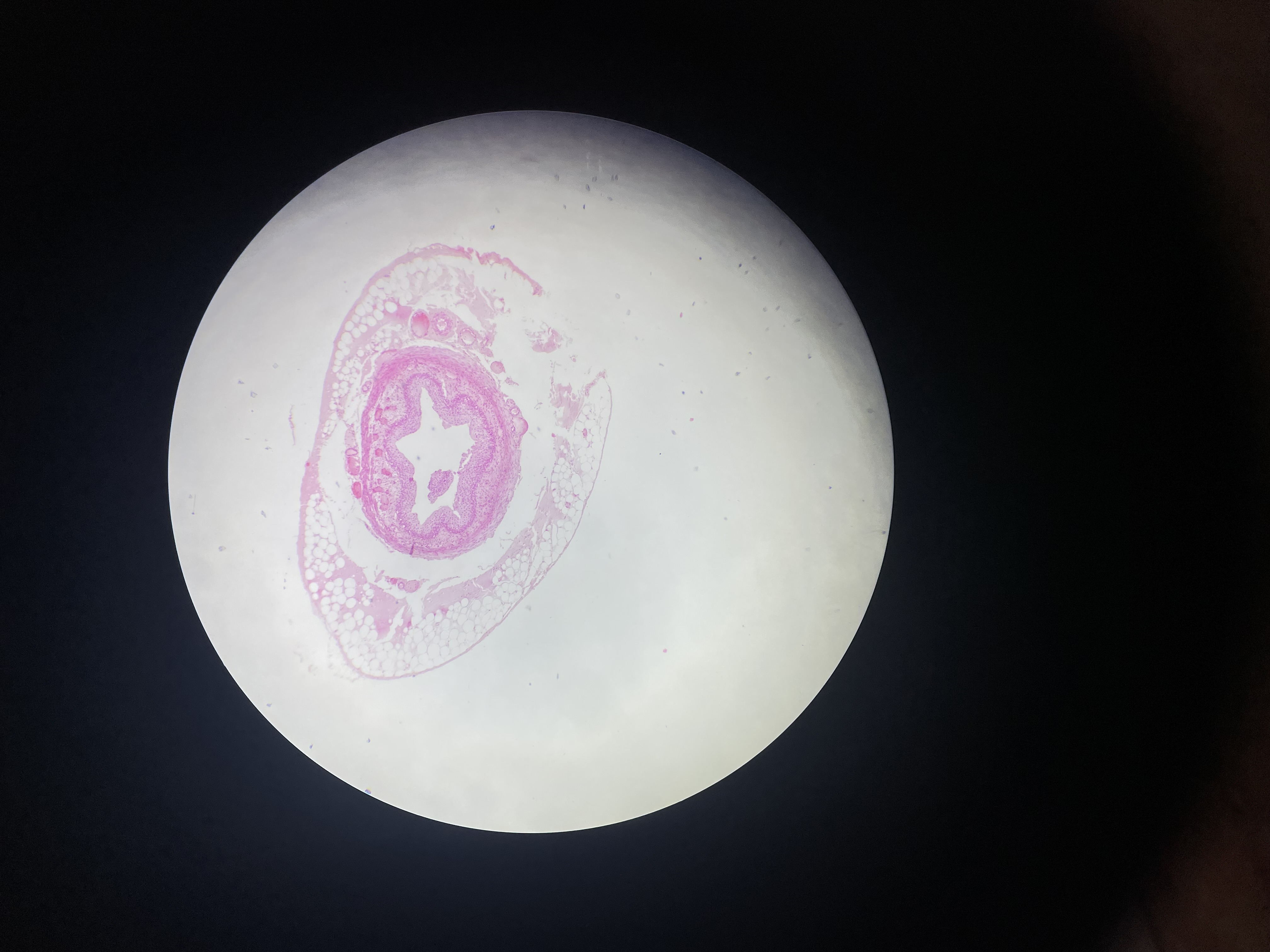
74) ductus deferens - HE
I. Tunica mucosa – plicae
1. L. epithelialis
pseudostratified columnar
epithelium: columnar cells
with stereocilia and basal cell
2. L. propria – loose connective
tissue – thin
I. Tunica muscularis
• Str. Longitudinale internum
• Str. circulare
• Str. longitudinale externum
• Tunica adventitia – loose
connective tissue
69) tuba uterina - HE
I. Tunica mucosa – plicae tubae uterinae
• L. epithelialis – single cylindrical ciliated
epithelium (cylindrical cells with cilia,
non ciliated cell= Peg cell and
undifferentiated cells)
• L. propria mucosae – CT
II. Tunica muscularis – smooth muscle tissue
• Str. circulare
• Str. longitudinale
Str. longitudinale internum – in the uterine
part of the tube
III. Tunica serosa –
• -tela subserosa -CT
• -mesothelium
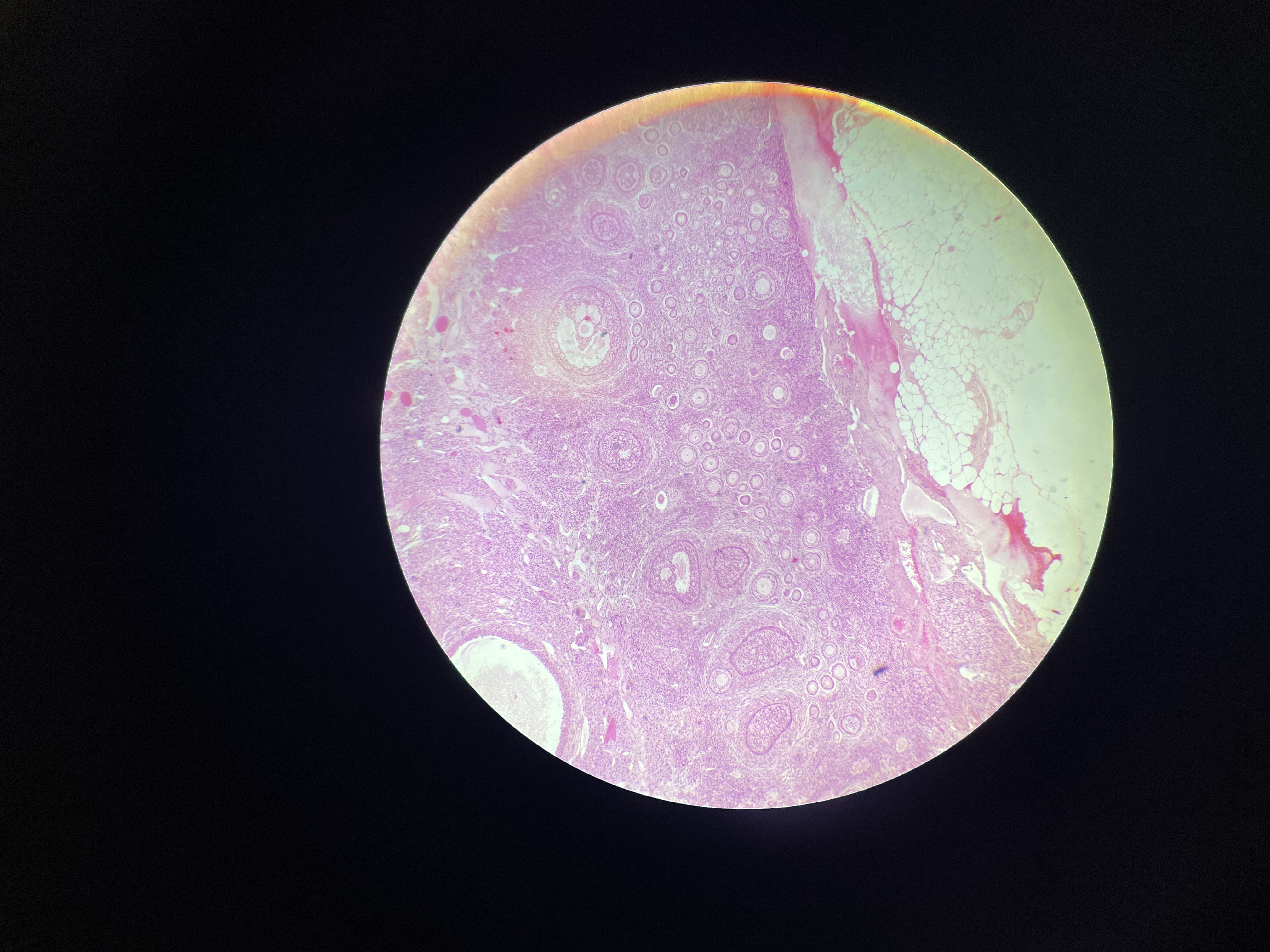
68) ovarium - HE
• Germinative epithelium – simple
cuboidal epithelium
• Tunica albuginea – dense
connective tissue,
• Stroma ovarii (interstitium ovarii)
– CT; contain endocrine cells
• Medulla – loose connective
tissue, large contorted blood vessels,
lymphatic vessels, nerves
• Cortex
• Follicles :
• folliculi primordiales –made up
of a first-order oocyte surrounded by a
layer of simple satellite (follicular) cells
• folliculi primarii- oocyte in
diplotene of first meiotic division
surrounded by 1 or several rows of cubic
follicle cells
• folliculus secundarius – oocyte
with pronounced zona pellucida; cavities
filled with follicular fluid appear between
the follicular cells; externally, the follicle
is surrounded by:
-Theca interna – thecal cells – produces
estrogens under the stimulation of FSH
and progesterone shortly before
ovulation
-Theca externa – loose connective tissue
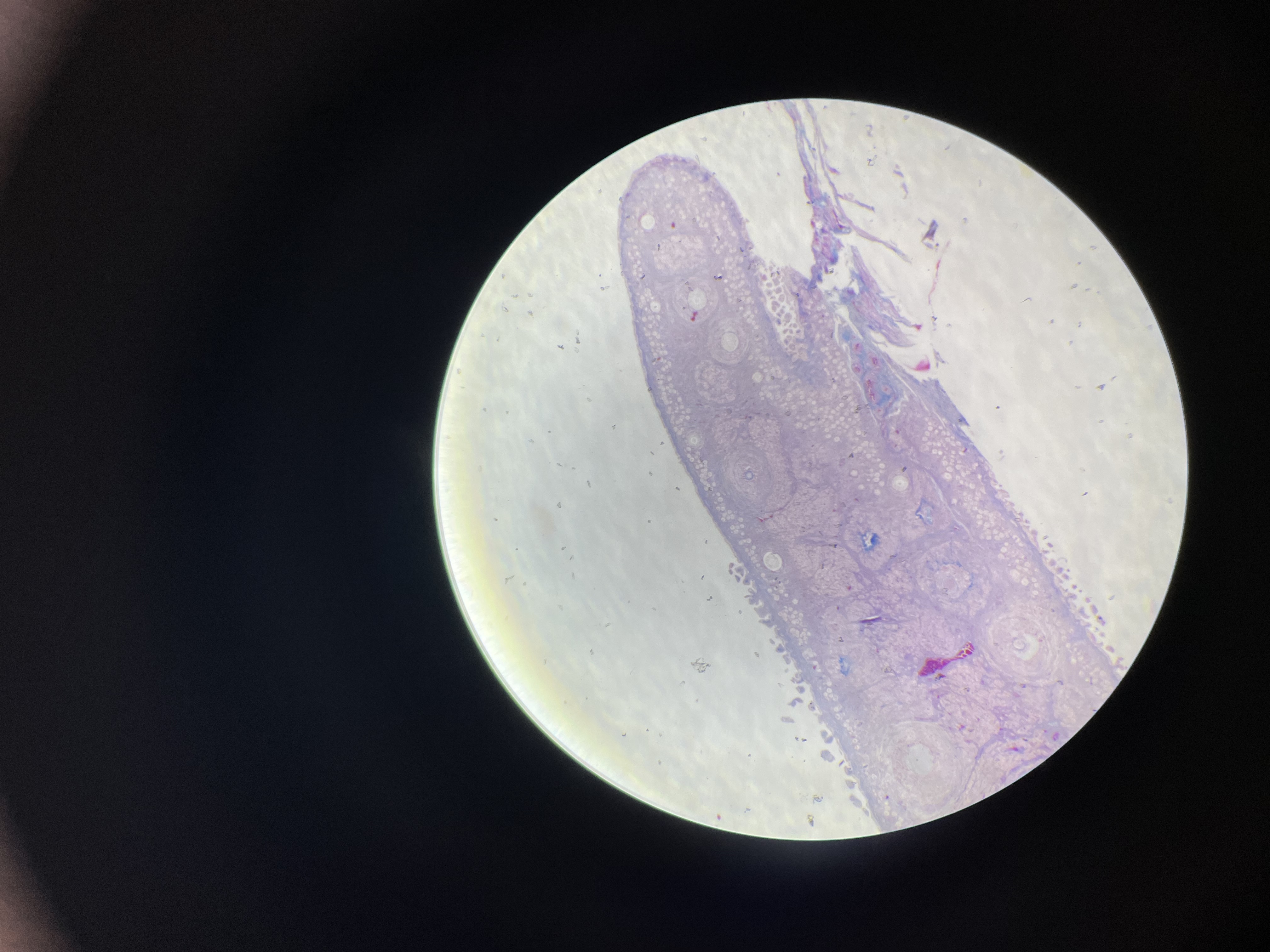
68a) ovarium - azan
Highlights connective tissue (blue):
• Germinative epithelium – simple
cuboidal epithelium
• Tunica albuginea – dense
connective tissue,
• Stroma ovarii (interstitium ovarii)
– CT; contain endocrine cells
• Medulla – loose connective
tissue, large contorted blood vessels,
lymphatic vessels, nerves
• Cortex
• Follicles :
• folliculi primordiales –made up
of a first-order oocyte surrounded by a
layer of simple satellite (follicular) cells
• folliculi primarii- oocyte in
diplotene of first meiotic division
surrounded by 1 or several rows of cubic
follicle cells
• folliculus secundarius – oocyte
with pronounced zona pellucida; cavities
filled with follicular fluid appear between
the follicular cells; externally, the follicle
is surrounded by:
-Theca interna – thecal cells – produces
estrogens under the stimulation of FSH
and progesterone shortly before
ovulation
-Theca externa – loose connective tissue
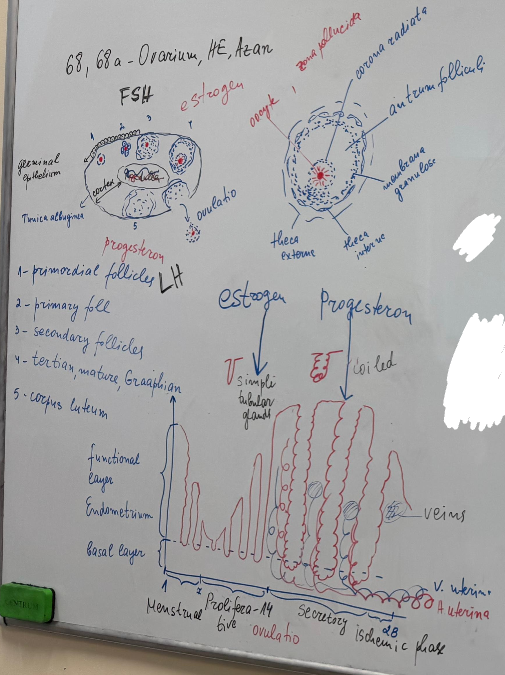
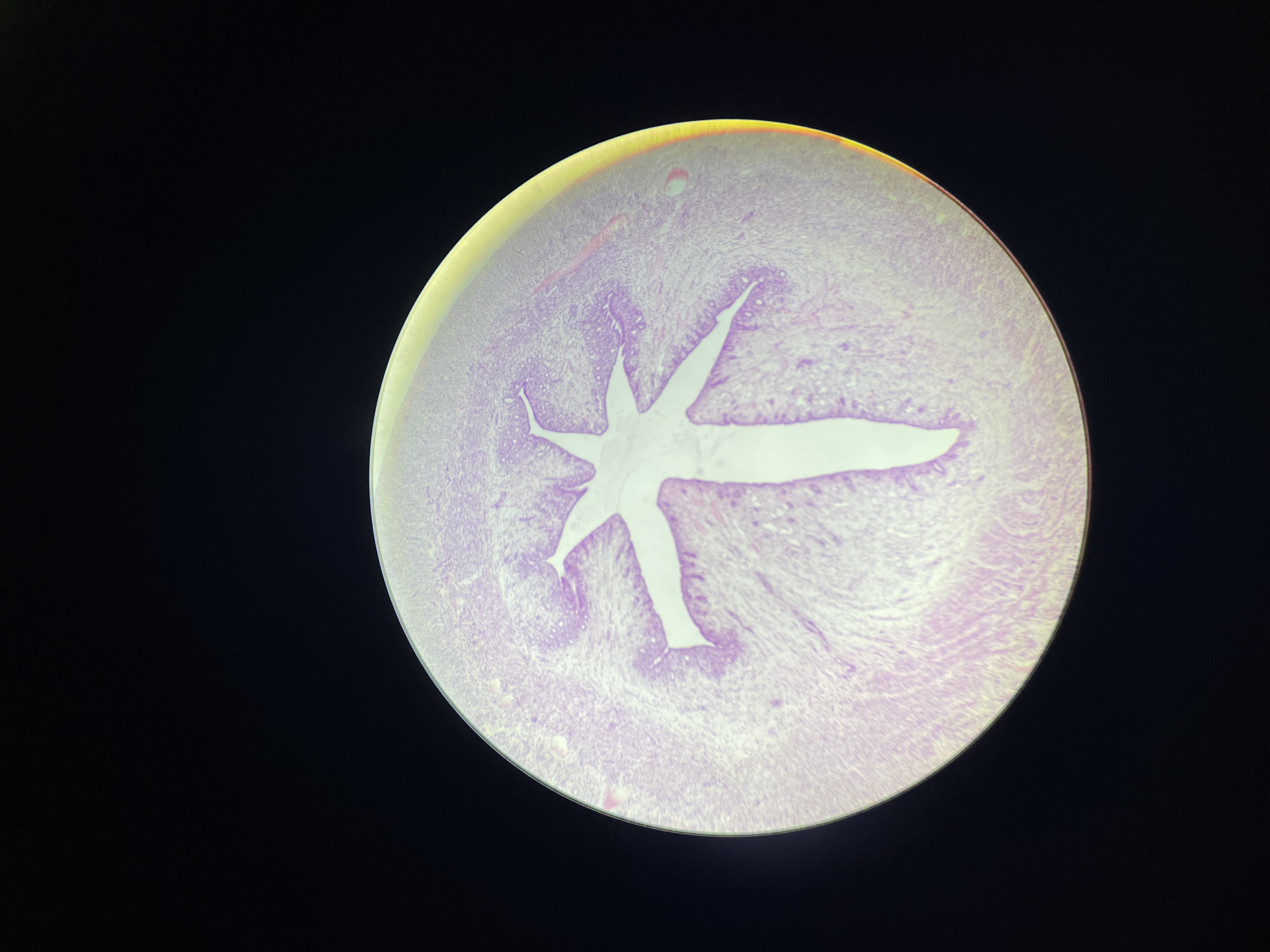
39) uterus (proliferative phase) - HE
I. Tunica mucosa = endometrium: pars basalis and pars
functionalis
• L. epithelialis – simple columnar epithelium
• L. propria – CT, (gll. uterinae)
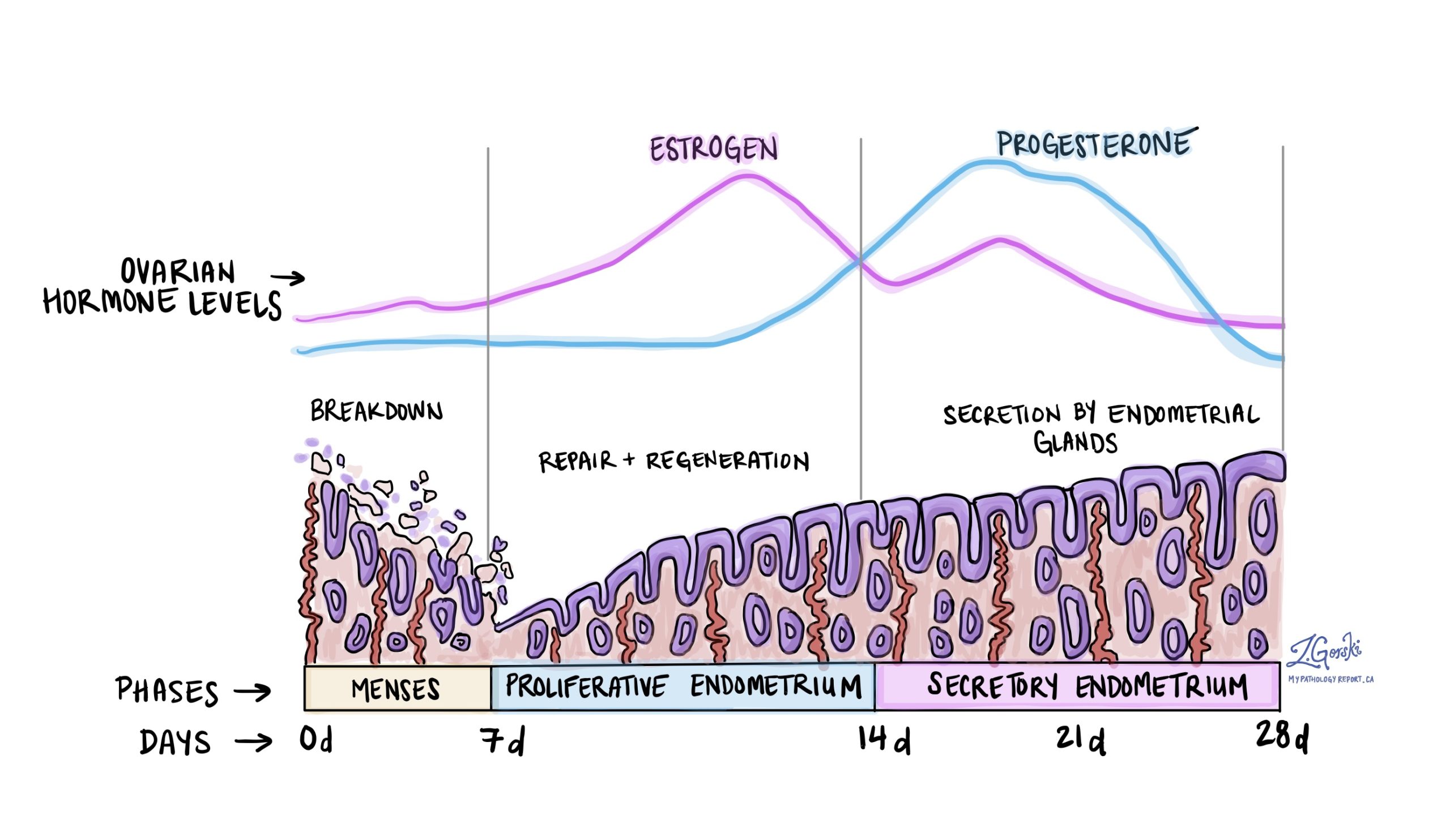
• menstrual cycle (28 days)
Proliferative phase - 6th to 14th day - regulated by ovarian
estrogens - regeneration of the mucous membrane from the
glands in the basal layer, formation of simple tubular glands
II. Tunica muscularis = myometrium
The myometrium is the middle (thickest) layer of the uterine
wall. It consists of tightly packed smooth muscle cells (uterine
myocytes), as well as stroma, blood and lymphatic vessels,
nerves.
III. Tunica serosa = perimetrium
• Tela subserosa
• Mesothelium
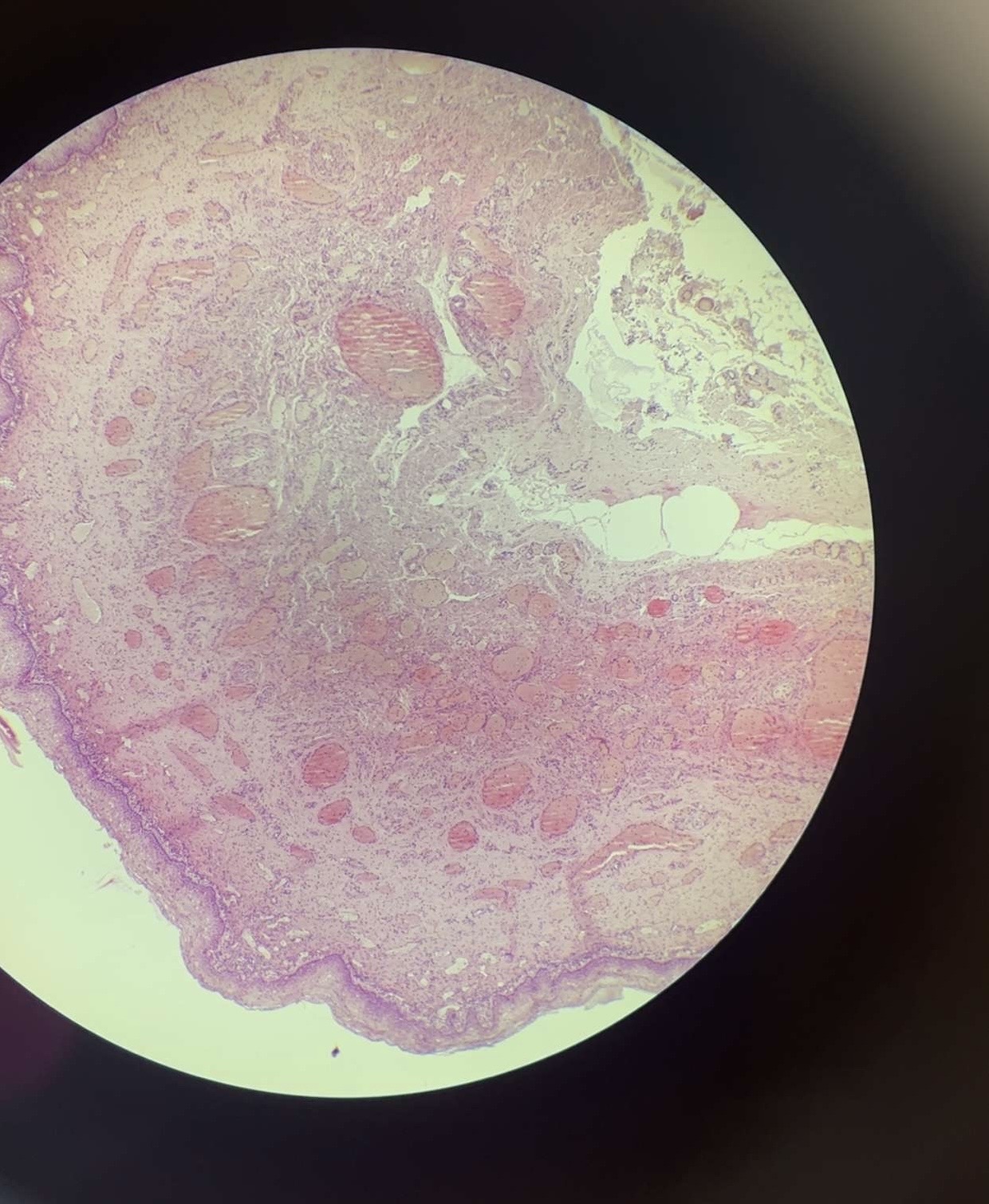
70) vagina - HE
I.Tunica mucosa
• L. epithelialis – stratified
squamous nonkeratinized
• L. propria – thick CT layer
containing blood vessels,
lymph follicles - no glands
II. Tunica muscularis – smooth
muscle tissue
• Str. circulare
• Str. longitudinale
• Tunica adventitia – CT
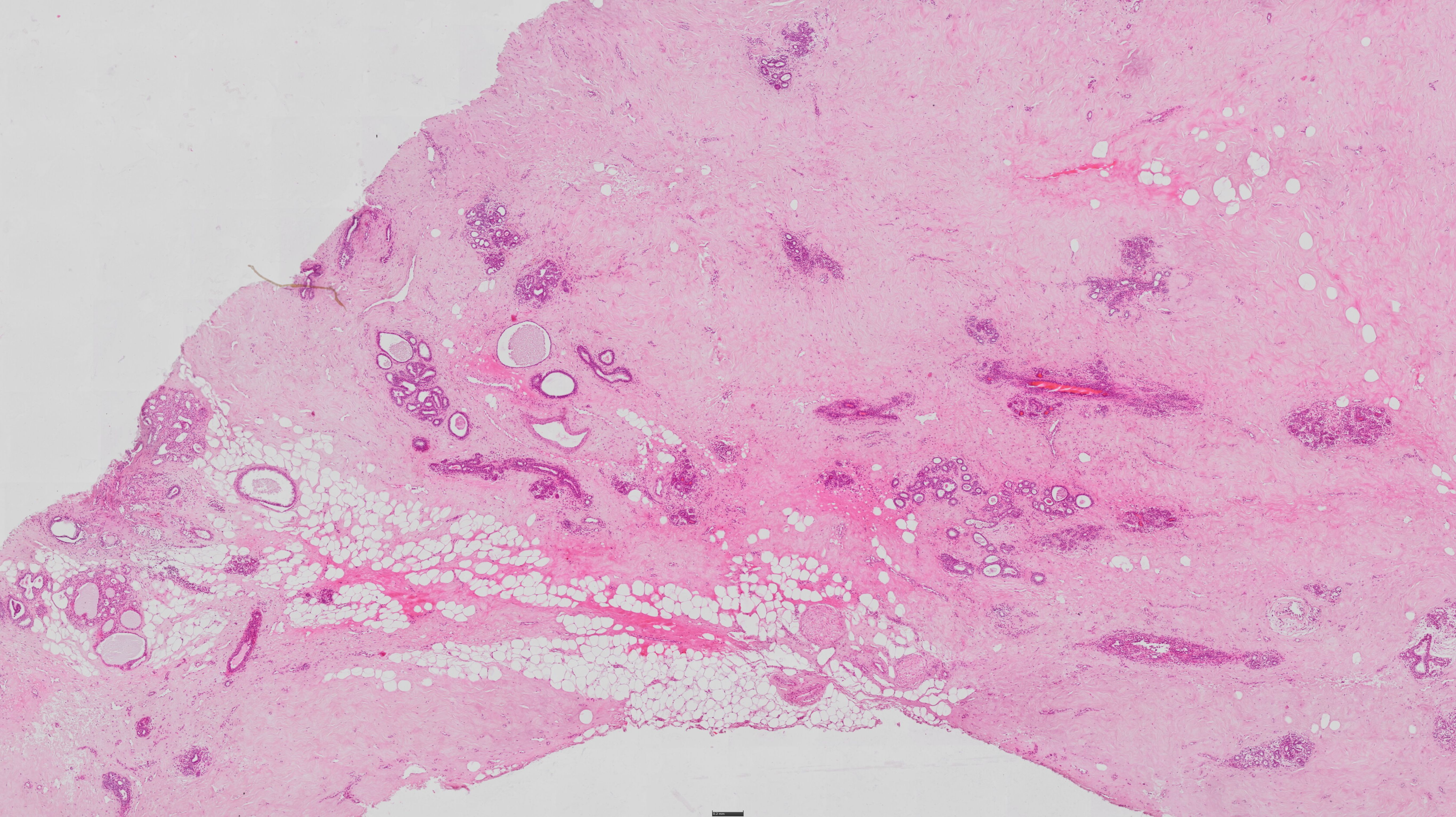
62) glandula mammaria - HE
• The non-lactating
mammary gland is made up
of 2 main components:
• Stroma - CT rich in fat cells
located around a loose
network of dense CT -
Cooper's ligaments.
• The parenchyma is
represented by groups of
milk ducts (ductuli lactiferi).
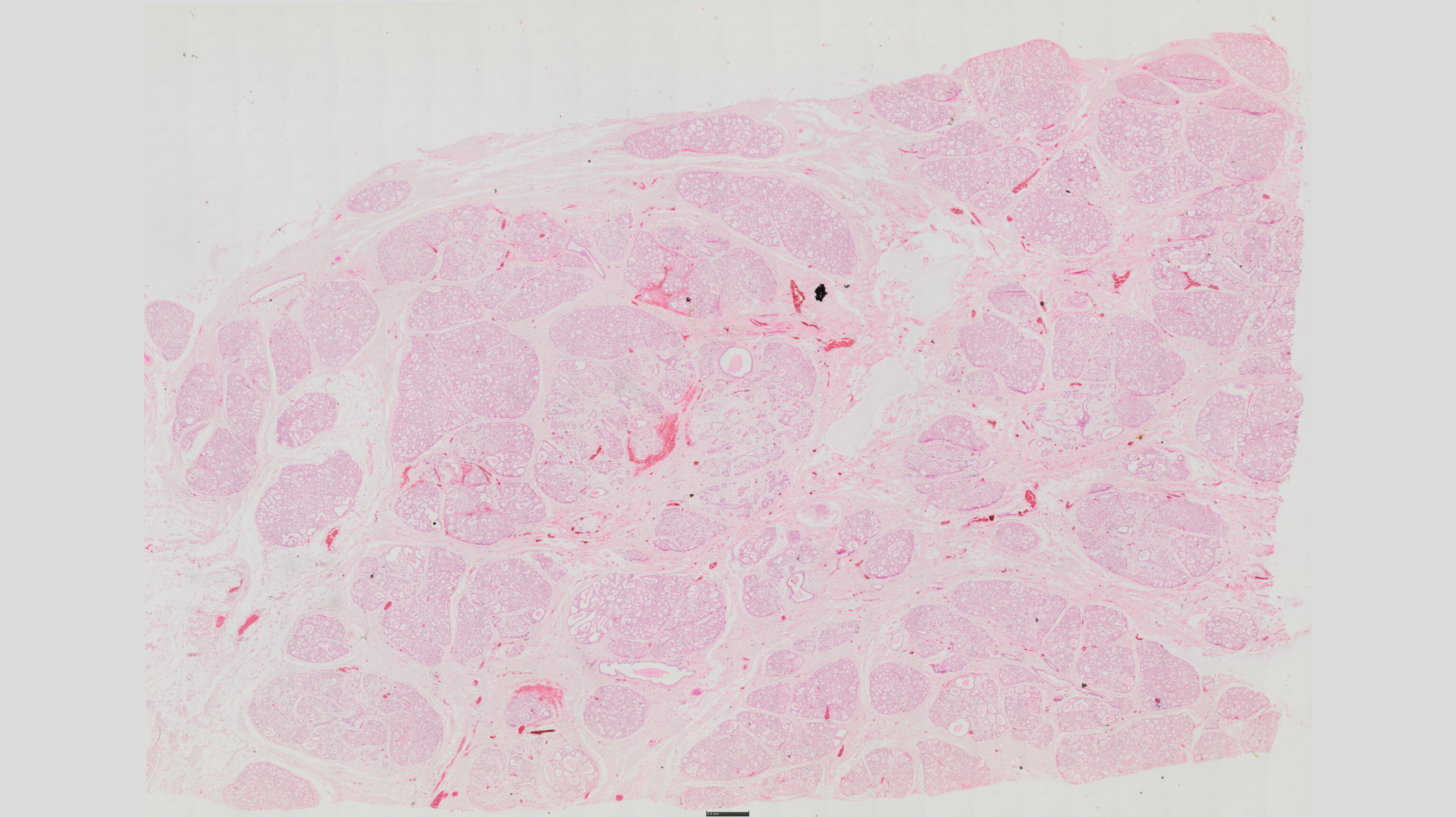
62) glandula mammaria (lac) - HE
• The mammary gland is composed of 15-25
secretory lobules surrounded by fatty tissue
The lobules are made up of tubuloacinous
glands. The stroma is made up of lipocytes
surrounded by a loose network of dense CT
(Cooper's junctions)
• The parenchyma is represented by acini
grouped in lobules. These are small pear-shaped glands known as terminal ductal
lobular units (TDLUs), in which milk is
secreted under the influence of prolactin.
They are covered with a single-cylindrical
epithelium lying on a basement membrane,
under which stellate-shaped myoepithelial
cells are located.
• Intralobular ducts, interlobular ducts, sinus
lactiferus, ductus lactiferus. The epithelium
of the ducts, except for the ductus
lactiferus, is a single cuboidal or low cylindrical epithelium and surrounded by
myoepithelial cells. Ductuli lactiferi –
stratified squamous nonkeratinized
epithelium.
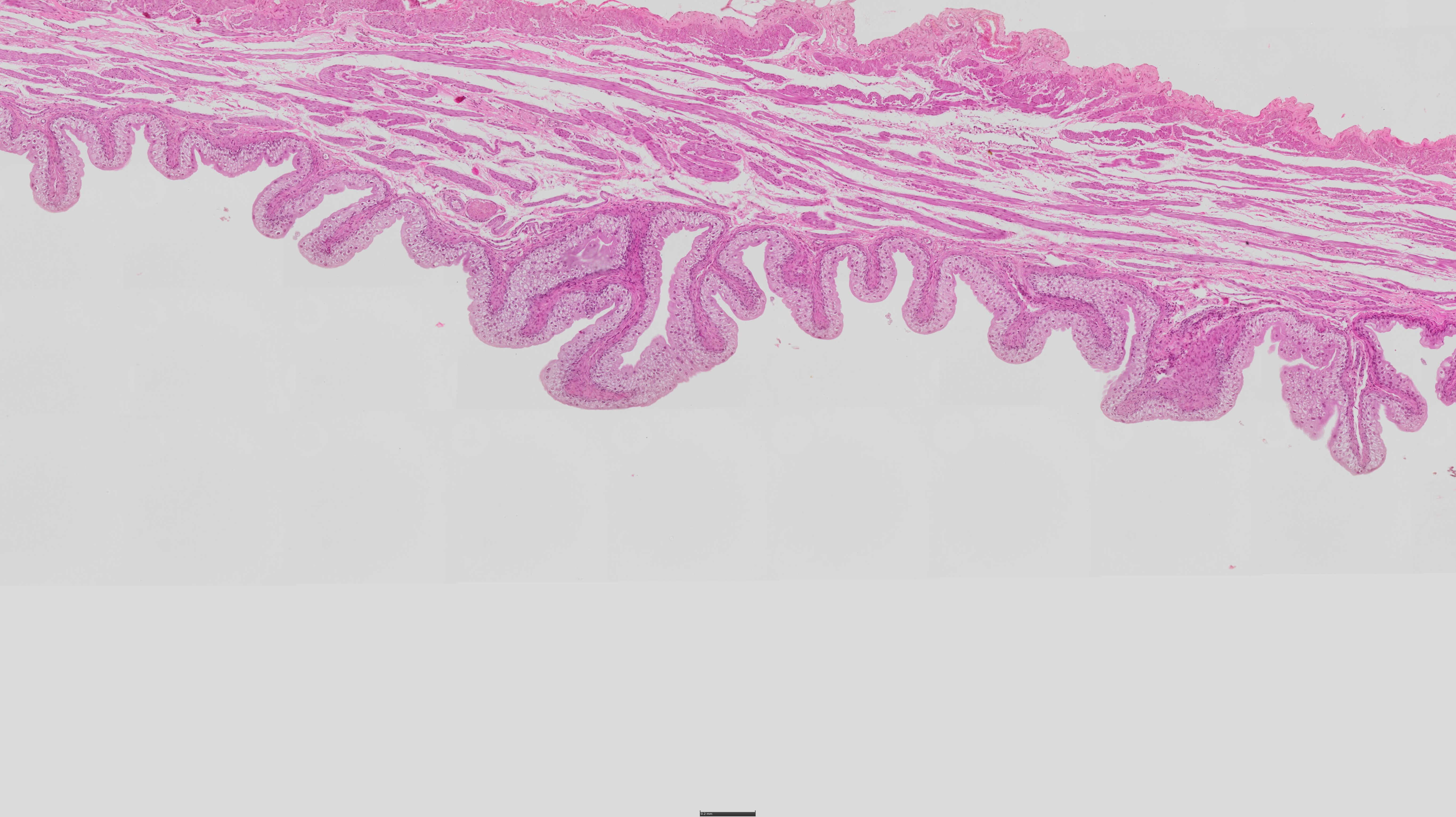
20) vesica urinaria (urinary bladder) - HE
Mucosa:
Transitional Epithelium (Urothelium):
Dome-shaped superficial cells (umbrella cells) – stretchable.
Stratified layers: Basal (cuboidal), intermediate (polygonal), superficial (large, rounded).
Lamina Propria: Loose connective tissue (no glands).
Muscularis (Detrusor Muscle):
Three indistinct smooth muscle layers:
Inner longitudinal, middle circular, outer longitudinal.
Thick, interwoven bundles (allows expansion).
Adventitia/Serosa:
Adventitia: Fibrous CT (posterior/inferior surfaces).
Serosa: Mesothelium-covered CT (superior surfaces).
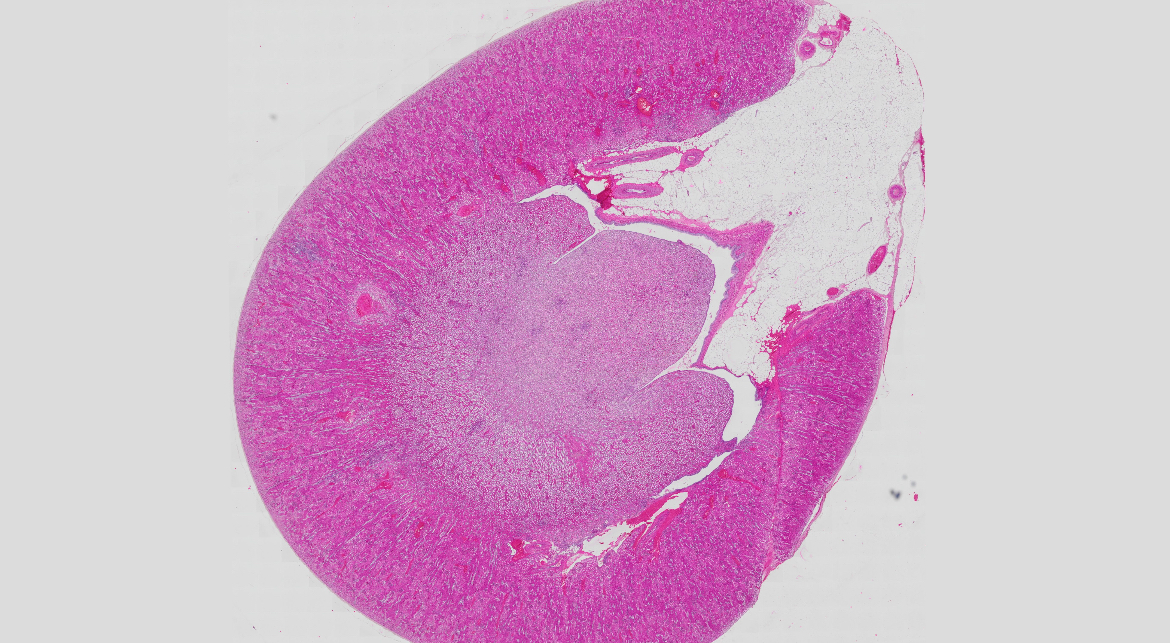
11) Ren - HE
Fascia renalis
Capsula adiposa
1.Capsula fibrosa – connective tissue
2. Cortex:
• Malpighian corpuscles (corpusculum renale):
• glomeruli – capillary loops
• capsula glomeruli – 2 layers:
- lamina visceralis – podocytes
- lamina parietalis – simple squamous epithelium
• tubulus contortus proximale (proximal
convoluted tubules)– narrow lumen; covered
with conical cells with microvilli on the apical surface and basal
invaginations on the basal surface
• tubulus rectus proximale
• tubulus contortus distale (distal convoluted
tubules )– wide lumen, made up of cubic cells with significantly
less folds
• tubulus rectus distale
• tubulus renalis arcuatus (convoluted collecting duct)
3. Medulla:
• ansa Henle
-pars decdendens (thin part) – single low-cubic epithelium
- pars ascendens (thick part) – single cubic epithelium
• tubuli colligens recti– single columnar epithelium
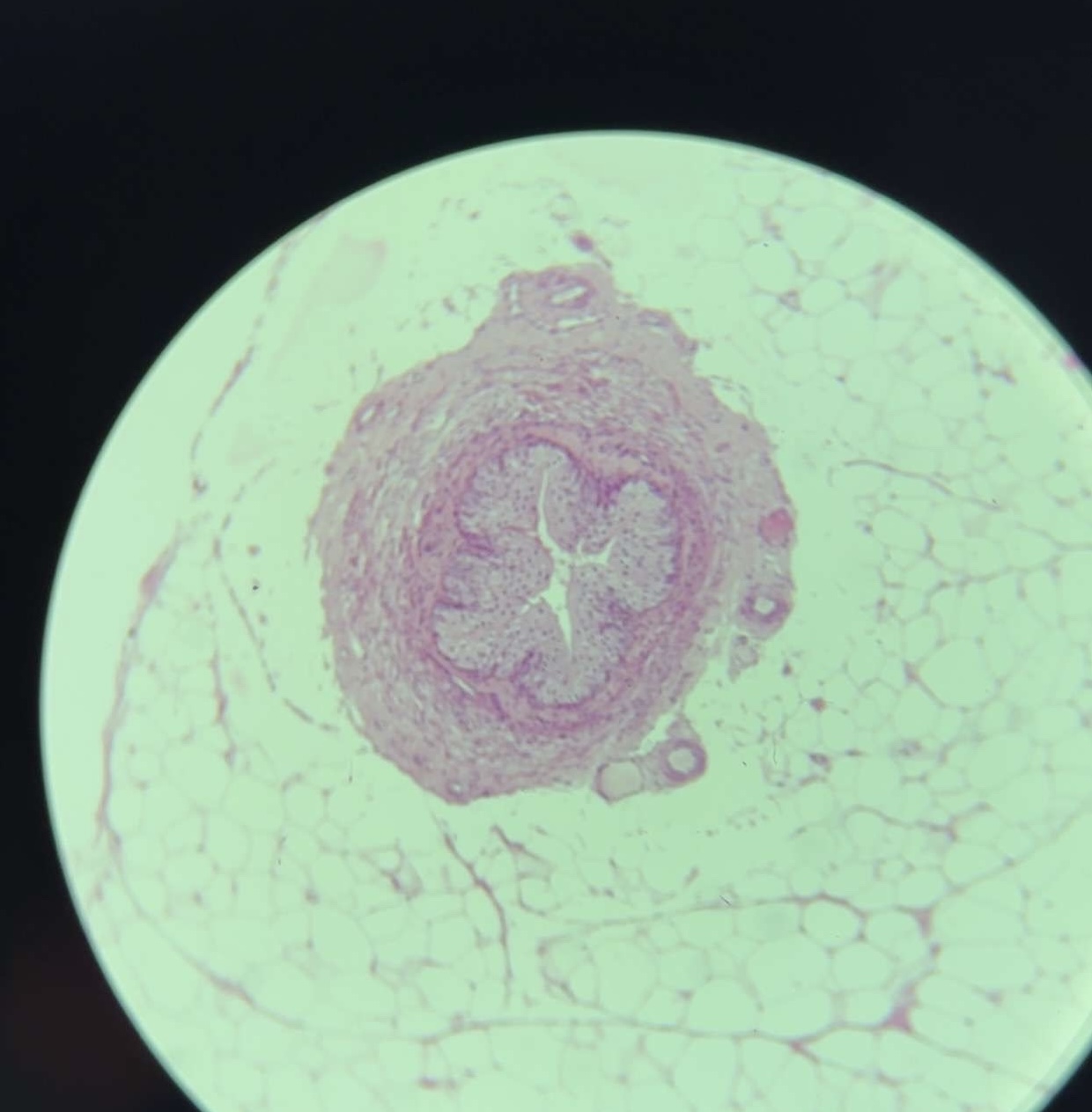
Ureter - HE
1. Layers & Key Features:
Mucosa:
Transitional epithelium (urothelium) – Dome-shaped cells with surface umbrella cells.
Lamina propria – Loose connective tissue (pale pink).
Muscularis:
Inner longitudinal + outer circular smooth muscle (bright pink).
Lower ureter adds a third outer longitudinal layer.
Adventitia:
Dense irregular connective tissue with vessels/nerves.