Phys Final Review
1/178
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
179 Terms
hypoventilation
right to left
cardiac output
hypoxemia: low arterial PO2 to tissues
→ _______
→ _______ shunt
→ low _______
→ anemia, carbon monoxide, cyanide
hypoxia
low tissue O2 delivery
hypoxemia
low blood O2
COPD
abnormal chronic inflammation causing structural airway & vascular changes
expiratory flow
Gas exchange
Hyperinflation
COPD
Decreased ________
Airway obstruction
______ abnormalities
_______ (can decrease inhalation volume)
productive
cyanosis
chronic bronchitis
______ cough >3 months
_____ (blue color)
Cor -pulmonae
peripheral edema
Wheezes
emphysema
enlargement of air spaces with loss of elasticity
elastic recoil
compliance
perfusion
emphysema
loss of _______ (difficulty exhaling)
________ increases due to hyperinflation
thin
mínimal Cough
pink puffer
_______ is NORMAL
pulmonary fibrosis
chronic epithelial damage to lung tissue → inflammation, fibroblast proliferation, & scarring
compliance
diffusion capacity
nonproductive
pulmonary fibrosis
decrease ______
decrease in ________
idiopathic
progressive dyspnea
_______ cough
fatigue
hypoxia
shrinking of lung lobes
honeycombing
tuberculosis
granulomas, necrosis, cavity formation
inhalation of droplets
middle/lower
upper
upper
Tuberculosis
caseous necrosis
transmitted by ________
primary TB: occurs in ______ lung
secondary TB: occurs in _____ lobes
HIV, >65, IV drug users, crowded settings
reactivation TB: _____ lobes common
low (<0.8)
normal OR increased
FEV1/FVC
obstructive disease: ____
restrictive disease: _____
increase (trapped air)
decreased (difficulty getting air in) and poor diffusion
lung volumes
obstructive disease: _____
restrictive disease: ______ and _______
acute bronchitis
short term respiratory inflammation lasting 2-5 weeks
virus
upper respiratory infection
dry; progressive
acute bronchitis
usually caused by ____
begins as ________
begin with ____ cough; then progresses to ______
asthma
inflammation and increased reactivity of airway smooth muscle causing bronchoconstriction and airflow resistance
beta-2; beta-2
non-productive
asthma
use _______ agonist to stimulate ______ receptors to bronchodilate
_________ cough
bronchiectasis
irreversible destruction and dilation of airways, specifically the bronchi and bronchioles
bilateral lower lung lobes
sputum
bronchiectasis
primarily impacts the __________ lobes
large amount of _____
finger clubbing
atelectasis
complete/partial collapse of normally expanded and aerated lung tissue at any structural level
intra-alveolar
ventilating; perfusion
gas exchange
atelectasis
loss of _______ pressure and surfactant
person isn’t _____ but _____ remains the same
decrease in ______ due to collapsed alveoli
common post-op complication
pneumonia
acute lung injury where inflammation from an organism affects lung parenchyma
pneumonia
alveoli fill with fluid and inflammatory cells... decrease in O2 diffusion
upper respiratory infection often precedes pneumonia
pleuritic chest pain
asymptomatic in elderly
aspiration pneumonia = R upper lung most affected
sarcoidosis
Non-caseating granulomas
Multi-organ disease
scaly/rashy appearance
Pneumoconiosis
Inhaled particles → fibrosis
Examples:
Silicosis
Asbestosis
pneumothorax
Air in pleural space → lung collapse
loss of negative pressure between layers
pleural effusion
Fluid in pleural space → compression of lung
Hypoventilation
V/Q mismatch
Right-to-left
Causes of Hypoxemia
High altitude
_______
Diffusion defect
______
______ shunt
Hypoxemia
cardiac output
Causes of Hypoxia
______
↓ ______
Anemia
perfusion; ventilaiton
O₂, CO₂
Shunt (Low V/Q)
_____ without _____
↓ ____ ↑ _____
Example: airway obstruction
ventilation; perfusion
Dead Space (High V/Q)
____ without ____
Example: pulmonary embolism
stretch, pH
CNS
smooth
secretion
Afferent/Efferent Control of Motility
Afferent (sensory):
Detect ____, ____
Send info to ____
Efferent (motor):
Control _____ muscle contraction
Control _____
CN IX & X
pharynx/esophagus
Key Reflex Example: Swallowing
Afferent: CN ___ & ___ → medulla
Efferent: medulla → _______
HCO3-
carbs
proteins
fats
Pancreatic Secretions
_______ → neutralizes acid
Enzymes:
Amylase → ___
Proteases → ___
Lipase → ___
nose
pharynx
larynx
Respiratory Tracts
Upper: what 3 parts?
Trachea → bronchi → bronchioles → alveoli
Respiratory Tracts
Lower: ____ → ____ → _____ → _____
conducting zone
lung zone
Air transport, warming, humidifying
Includes bronchi → terminal bronchioles
respiratory zone
lung zone
Gas exchange
Includes alveoli (Type I & II pneumocytes)
dead space
volume of the airways and lungs that doesn’t partake in gas exchange
physiologic dead space
total volume of lungs that doesn’t partake in gas exchange (anatomic and functional) and includes regions of the lungs that are ventilated but no gas exchange occurs (damaged)
Diaphragm
Thoracic
Pressure
Inspiration
_____ contracts
_____ volume ↑
_____ ↓ → air flows in
passive
Expiration
____ (elastic recoil)
Forced uses:
Abdominals
Internal intercostals
abdominal; ribs
volume
pressure
diaphragm (contracted)
_____ pushed down & ____ lift up when contracted
increase in intrathoracic ___
decrease in intrathoraric _____

inspiration
expiration
negative
alveoli
Alveolar pressure:
↓ during ___
↑ during ____
Intrapleural pressure:
Always ____
Transmural pressure:
Keeps ___ open
compliance
↑ compliance = easier expansion
Ease of lung expansion
affinity
unloading
CO₂
pH
temperature
Right shift (↓ _____, ↑ ____)
↑ ____
↓ ___ (Bohr effect)
↑ ______
affinity; unloading
metabolic activity
hypoventilation
lungs
tissues
Left shift (↑ ____, ↓ ____)
decrease in _____
increase in pH
______
____ = loading
____ = unloading
apex
base
Regional differences
____: high V/Q
____: low V/Q
bronchodilation
bronchoconstriction
Autonomic Nervous System &. Airway Resistance
sympathetic adrenergic (B2) = ______
parasympathetic cholinergic (M) = _______
intrapleural space
negative pressure of ________ generated by the opposing forces maintains the lungs open & chest wall from springing out

central chemoreceptors
Keep arterial CO2 in normal range
Respond directly to changes in ph & indirectly to changes in arterial PCO2
peripheral chemoreceptors
carotid & aortic bodies
respond to changes in PaO2, PaCO2, & arterial pH
causes increase in RR under...
→ PO2 below <60 mmlg
→ increase in arterial CO2 pH
→ decrease in arterial pH
innate
Immunity type
Present before exposure
Non-specific
Fast response
recognition
amplification
effector
termination
memory
phases of immune response in order
recognition
phases of immune response
innate/adaptive immunity
amplification
phases of immune response
proliferation
effector
phases of immune response
removal of antigens
termination
phases of immune response
dampening
memory
phases of immune response
long lived T & B lymphocytes
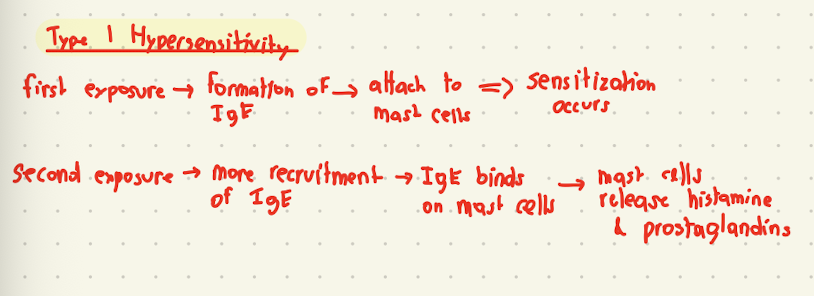
type IV
Hypersensitivity Type
cytotoxic T cells kill & destroy target cells
lymphokine cells activate macrophages which attached to target cells, release cytolytic enzymes = tissue destruction
hypothalamus
Releases releasing hormones (TRH, CRH, GHRH)
Controls pituitary
anterior pituitary
TSH → thyroid
ACTH → adrenal cortex
GH → growth
Prolactin → milk production
FSH/LH → reproduction
posterior pituitary
ADH → ↑ water reabsorption
Oxytocin → uterine contraction & milk ejection
thyroid
T3/T4 → ↑ metabolism
Calcitonin → ↓ Ca²⁺ (minor role)
Parathyroid
PTH → ↑ Ca²⁺
Bone resorption
Kidney reabsorption
GI absorption (via vitamin D)
adrenal cortex
Cortisol → stress, ↑ glucose
Aldosterone → ↑ Na⁺, ↓ K⁺
Androgens → sex characteristics
adrenal medulla
Epinephrine/Norepinephrine
Fight-or-flight response
pancreas
Insulin → ↓ blood glucose
Glucagon → ↑ blood glucose
Somatostatin → inhibits both
kidney
Erythropoietin (RBC production)
Renin (BP regulation)
insulin (fed state)
↓ blood glucose
↑ storage (glycogen, fat, protein)
glucagon (fasting state)
↑ blood glucose
↑ glycogenolysis & gluconeogenesis
↑ lipolysis
somatostatin
“Brake system”
↓ insulin & glucagon
GH
GH
Pituitary Disorders
Hyperpituitarism
____ excess → gigantism (kids), acromegaly (adults)
Hypopituitarism
____ deficiency → dwarfism
SIADH
Too much ADH
Water retention → hyponatremia
Diabetes Insipidus
Too little ADH
Excess urination + dehydration
hyperthyroidism
↑ metabolism
Weight loss, heat intolerance, tachycardia
Graves disease = most common
hypothyroidism
↓ metabolism
Weight gain, cold intolerance, fatigue
Myxedema (severe form)
Hyperparathyroidism
endocrine pathology
↑ Ca²⁺ → bone breakdown
Kidney stones
Fractures
Hypoparathyroidism
↓ Ca²⁺ → tetany
Muscle spasms
addison’s disease
Adrenal disorder
LOW cortisol
Hypotension
Weight loss
Hyperkalemia
cushing’s disease
Adrenal disorder
Moon face, buffalo hump
Hyperglycemia
Muscle wasting
high cortisol
sertoli
leydig
Gonadal Sex
Male (Testes)
_____ cells → antimüllerian hormone
_____ cells → testosterone
theca
granulosa
Gonadal Sex
Female (Ovaries)
_____ cells → progesterone + androstenedione
_____ cells → estradiol
sertoli cells
Spermatogenesis is supported by ______ cells
pregnancy
implantation
uterine
Progesterone
Maintains ______
Prepares uterus for _______
Decreases _____ contractions
Thickens cervical mucus
estrogen
FSH
FSH/LH
Follicular Phase (Day 0–14)
Dominant hormone: ______
Events:
Follicle development (____ hormone)
Endometrial growth
Negative feedback → ↓ ___/___
LH
estrogen
Ovulation (Day 14)
Trigger: ___ surge
Caused by:
High ______ → positive feedback
progesterone
Progesterone + estrogen
Luteal Phase (Day 14–28)
Dominant hormone: _______
Corpus luteum produces:
______ and _______
Prepares uterus for implantation
progesterone + estrogen
Menses
↓ ______ and ______
Shedding of endometrium
FSH/LH
testes
Fetal Development
GnRH → _____/____ begin early
SRY → _____ develop first
FSH & LH
Puberty
Pulsatile GnRH → ↑ ____ and _____
Leads to:
Testosterone (male)
Estrogen (female)
Secondary sex characteristics develop
estrogen
FSH & LH
Aging (Menopause)
↓ ____
↑ ____ and ____ (loss of feedback)
type 1
hypersensitivity type
Fast (minutes)
Mast cell degranulation → histamine
type II
hypersensitivity type
Antibodies attack cells directly
Myasthenia gravis
Graves disease
Hemolytic anemia
type III
hypersensitivity type
Antigen + antibody complexes deposit in tissues
lupus