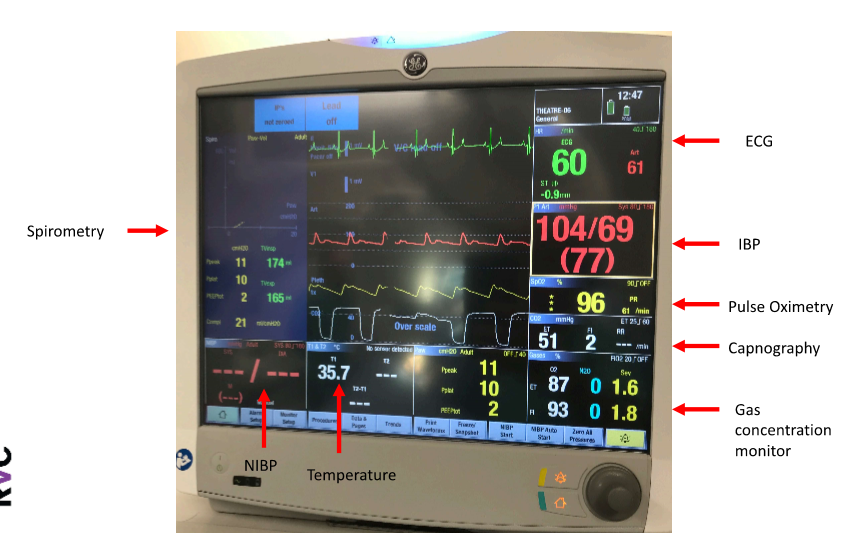
L29: Monitoring the anaesthetised patient
1/39
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
40 Terms
what should an anaesthetist be
Present at all times
Record keeping
Good understanding of
physiology
Pharmacology
Physics
Equipment
clinical information available
What is the anaesthetic record
Legal document of
Patients signalment
Drugs administered
Fluid therapy
Parameters every 5-10 minutes
important events
complications
Vital parameters of the animal in recovery
Why do we monitor patients
To maintain the body as close as possible to physiologically normality
To maintain adequate depth of anaesthesia
To promote patient and personnel safety
Legal requirement
What do you monitor when in anaesthesia
CNS
CVS
Respiratory system
Temperature
Neuromuscular function
renal function
Metabolic status
How do you monitor anaesthesia
Listen→ Ventilation sounds, alarms, gas leaks
Look → eye position, chest movements, mucous membrane colour
Feel → Pulse quality, rate rhythm, jaw tone, reflexes
Small → That volatile agent- is it a leak, a disconnection?
How do you monitor the CNS
Depth of anaesthesia → assessment of reflexes
Palpebral reflex
Corneal reflex
Gag reflex and jaw tone
Limb withdrawal reflexes
Perineal reflex (anal tone)
Righting reflex
Eye postioin
Movement of the globe
Lacrimation
Pupil size
ECG
BIS
what can alter cardiac output
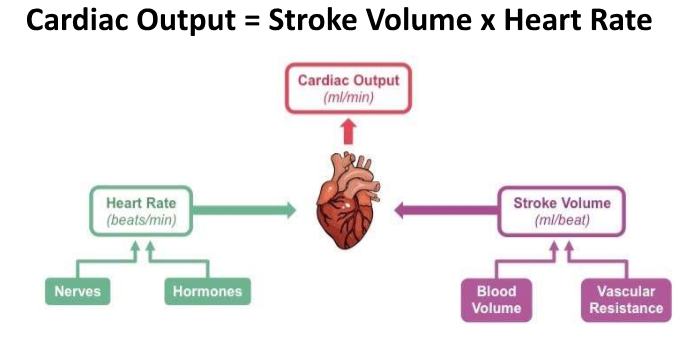
Why is it important to monitor the CVS
Factors determining tissue perfusion and oxygen delivery
How can blood pressure affect the CVS
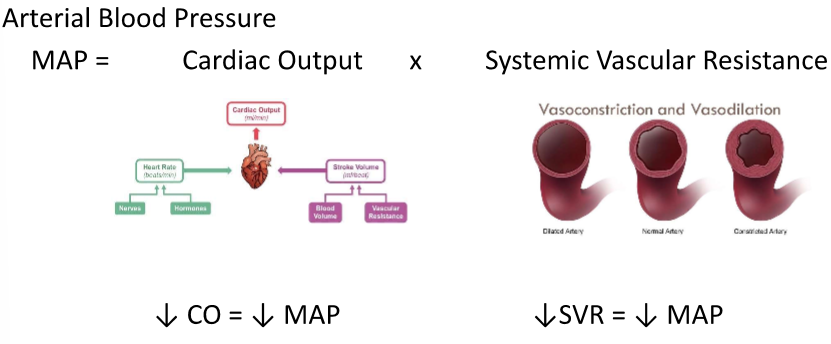
What are some normal blood pressures

How can you measure arterial blood pressure
non invasive monitoring (NIBP)
Oscillometry
Doppler
Invasive (IBP) monitoring
Direct arterial blood pressure
What is oscillometry
Accuracy depends on the cuff (40% circumference limb)
Cuff levelled with the heart
Gives SAP, MAP, DAP
MAP is the most accurate value
Tendency of under-estimation
What is a doppler and how does it work
Gives only one value → SAP
In cats value is between SAP and MAP
What is an IBP
Gold standard
Arterial catheter
Transducer at level of the heart
Heparinized saline to flush
What do you look at in IBP
Arterial blood gas
Acid base status
Efficiency of ventilation
pH
PaO2
PCO2
HCO3
Electrolytes
How do you troubleshoot low blood pressure
MAP= cardiac output x systemic vascular resistance
Assess depth of anaesthesia and reduce if possible
Intravenous fluid therapy (bolus 5-10 mL/kg)
Vasopressors
Positive inotropes (dobutamine)
Vasoconstrictors (ephedrine, phenylephrine, noradrenaline)
Avoid NSAIDS during hypotension
How do you monitor the cardiovascular system using electrocardiography
Heart rate
Heart rhythm
P waves
PR interval
QRS complex
ST segment
T waves
What types of stethoscopes are there
traditional stethoscope
Oesophageal stethoscope
Heart sounds
Heart rhythm
Lung sounds
What do you look for when monitoring the respiratory system by observing
Breathing rate (RR)
Breathing rhythm
Tidal volume (TV)/depth of each breath
Mucous membrane
Minute ventilation (MV)=TV x RR
What do different mucous membrane colours show
White→ anaemia, intense vasoconstriction
Yellow → Jaundice, carotens
Grey/purple/cyanotic → Poor tissue oxygen delivery (not observed at least 5 g/dL of deoxyhaemoglobin
Navy blue→ Excess of nitrous oxide (severe cyanosis)
Cherry red → Carbon monoxide poisoning
Muddy brown → metaHb (nitrate, paracetamol poisoning)
Brick red/brown → Systemic inflammatory response, sepsis
How do you assess ventilation with capnography
CO2 in respiratory gases
End-tidal (ET) and inspiratory (Fi) CO2
Continuous
Non-invasive
Et-CO2 tension reflects the systemic arterial CO2 tension
EtCO2 = PACO2 = PaCO2
What is capnography
Measures how well the animal is ventilating
Normal range 35-45 mmHg (4.5-6 kPa)
Values > 60 mmHg (>8kPa) may require mechanical ventilation
What are types of capnography
sidestream technology
Mainstream technology
what are the phases of capnography

What do different capnograms look like
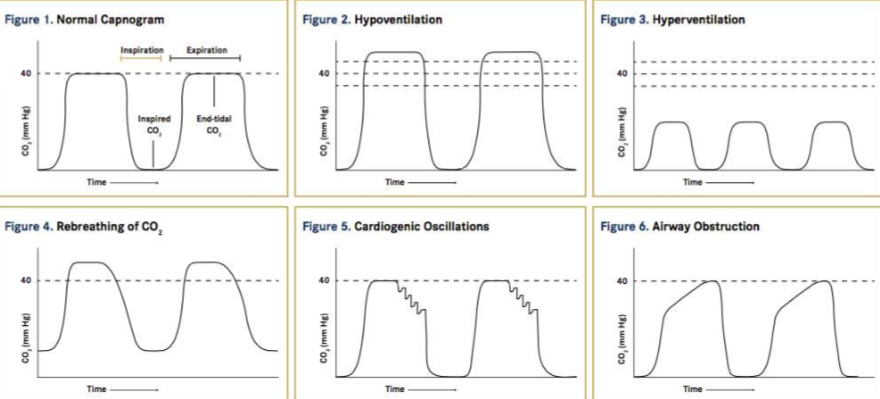
What does an increase in CO2 show
increase CO2 = hypercapina
alveolar hypoventilation
increased cardiac output
Hyperthermia
Bicarbonate administration
What does a decrease in CO2 show
Decrease in CO2=hypocapnia
Decreased cardiac output (shock, cardiac arrest)
Hypothermia
Hyperventilation/panting
Pulmonary thromboembolism
How do you assess ventilation with spirometry
Connected to the ET tube
Continuous
Non-invasive
Tidal volume
Airway pressures
Compliance
How do you monitor anaesthetic gas concentration
Continuous
Non invasive
Measures Et and FI concentration of gases
Helps in assessing depth of anaesthesia
Need to know the MAC of the agent in a certain species
Useful during “low flow anaesthesia “
How do you want to monitor the respiratory system with oxygenation
Observe- mucous membranes
Pulse oximetry
Non-invasive, continuous, measured at the level of arterioles
Arterial blood gas analysis
Invasive, Intermittent results, possible complications
What is pulse oximetry
Measures oxyhaemoglobin (HbO) as a % of the total haemoglobin in the arterial blood
SpO2%
Pulse rate
Adequacy of tissue perfusion
How does pulse oximetry work
Majority of oxygen in the blood is carried by Hb
SpO2 %
Measurement of saturation enables estimation of oxygen content and oxygen delivery to tissues
what is the equation for rate of oxygen delivery (ml per minute)

What is normal pulse oximetry
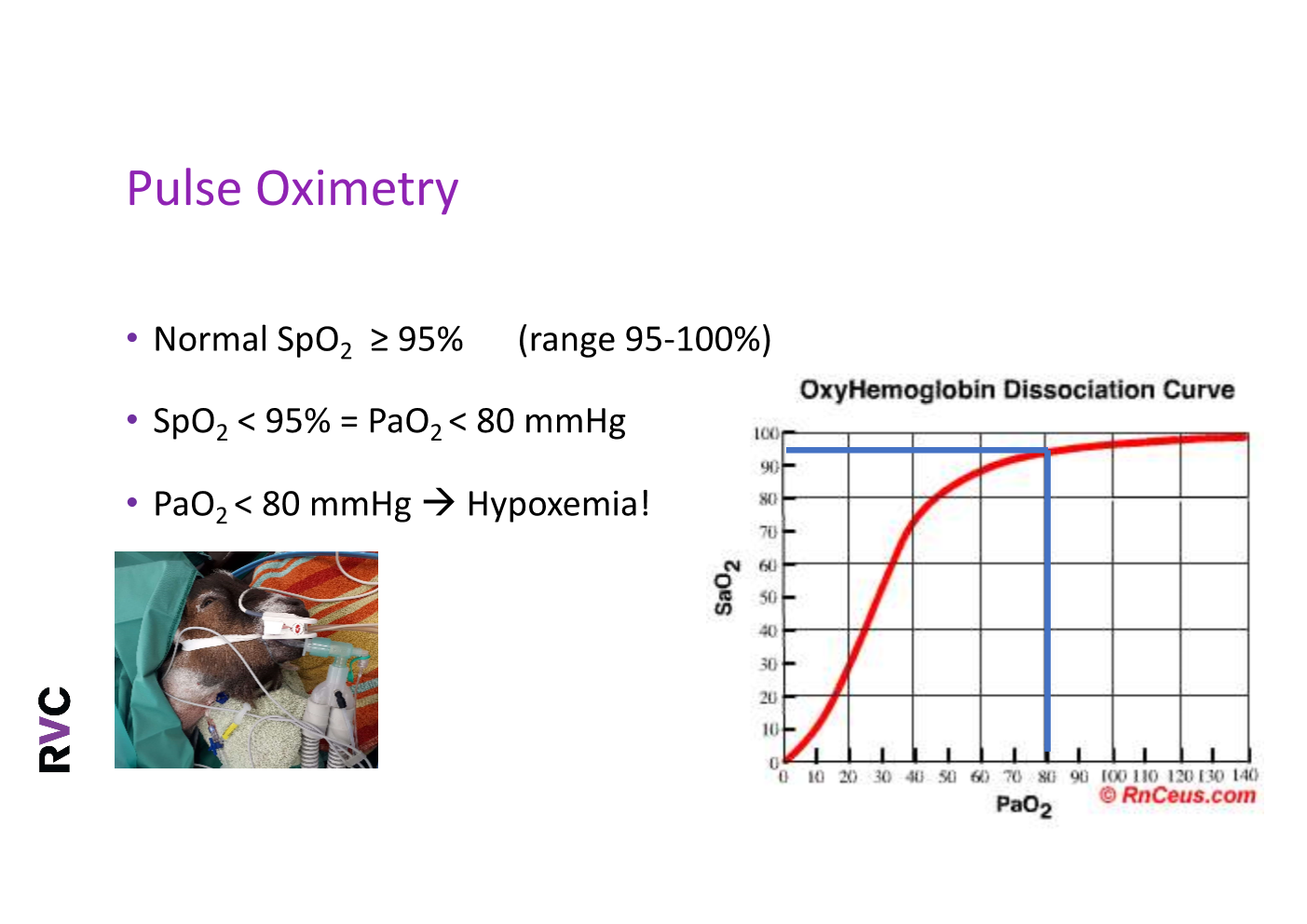
when is pulse oximetry not a good measurement
animals under anaesthesia breathing 100% O2
Room air has only 21% O2
Good to check in recovery when animal is back on breathing room air
What do you do if SpO2 is less than 95%
Check probe position
Check oxygen supply and FiO2
check perfusion
BP
Use of alpha2-agonist
Hypoxaemia
right to left shunting
anatomical: tetralogy of fallot
Intrapulmonary: Perfusion of unventilated alveoli
Ventilation/perfusion mismatch
impaired diffusion
hypoventilation
How do you use a thermistor
Probe placed in oesophagus or rectum
Non invasive
continuous
Are larger or smaller animals more at risk of hypothermia
smaller due to increased surface area to body mass ratio
what are the stages of hypothermia

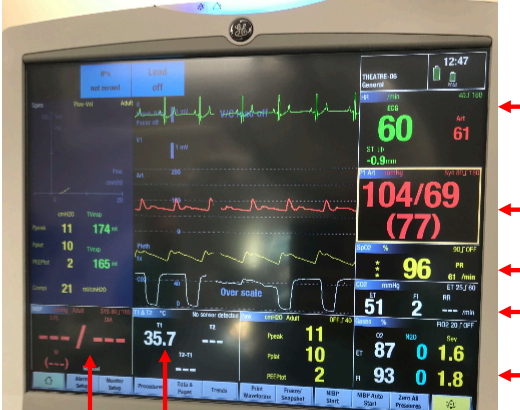
Label this machine