GI Exam 2 Part 2: Pharmacology of peptic Acid Diseases
1/66
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
67 Terms
4 categories of action of drugs for peptic diseases
o Neutralizing gastric acid
o Reduce gastric acid secretion
o Enhance mucosal defenses/ "cytoprotectants"
o Antimicrobial activity
what are the 3 goals of treating peptic ulcer disease
-pain relief
-ulcer healing
-prevention of complications and ulcer recurrence
MOA of antacids
· Simply work by neutralizing hydrochloric acid
· They are weak bases that react with hydrochloric acid to form salts and water
· By increasing the pH of the stomach, antacids also inactivate pepsin (known to contribute to ulcer formation by digesting proteins in the stomach wall)
what pH level is pepsin activity significantly reduced?
pH>4
common antacid ingredients
o Aluminum hydroxide
o Magnesium hydroxide
o Calcium carbonate
o Sodium bicarbonate
3 parts of normal response to acid neutralization
o Increase gastrin release
o Increase acid output
o Increase volume of secretion
what is acid rebound
overproduction of HCl after stopping antacids
which ingredient in antacids are more likley to cause acid rebound
o Calcium carbonate is more likely to induce rebound vs Mg and Al-containing antacids
o Rapid vs slow acting antacids
what 2 factors determine the net buffering capacity of antacids
o Their ability to neutralize acid
o Time of residency in the stomach
aluminum hydroxide vs calcium carbonate antacids
aluminum hydroxide: act very gradually and their effects continue for several hours
calcium carbonate: act quickly and increase pH a lot so more likley to cause acid rebound
3 factors that affect how well a patient respond to antacids
o How much acid the patient secretes (hypersecretion)
o Rate at which antacids are emptied from the stomach
o Potency of the acid (ANC/ acid neutralizing capacity)
effect of aluminum-based antacids on GI motility
produce constipation
effect of Mg-containing antacids on GI motility
produce diarrhea
what is a possible consequence of absorption of un-neutralized sodium bicarbonate
can produce metabolic alkalosis
why should you be cautious with using antacids in patients with renal sufficiency
can cause some absorption of cations like Ca, Mg, Al, and Na
DDI of antacids
May chelate other drugs (avoid concomitant administration of other drugs such as tetracyclines, digoxin, propranolol)
what are the 3 histamine-2 receptor antagonists
famotidine, cimetidine, and nizatidine
MOA of histamine-2 receptor antagonists
· Are competitive inhibitors of H2 receptor in parietal cells
· H2 blockers also decrease (indirectly) gastrin and ACh-induced gastric acid secretion
3 effects of H2 antagonism
reduction in...
o Volume of gastric juices secreted
o Gastrin secretion
o H+ concentration
what are the 4 uses of histamine-2 receptor antagonists
o Duodenal ulcers, gastric ulcers, ZES, and GERD
adverse effects of H2RAs
usually well-tolerated
D, HA, muscle pain, constipation, fatigue
cimetidine DDI
inhibits CYP450-mediated drug metabolism
cimetidine effects other than on histamine
anti-androgenic effects by antagonizing the androgen receptor and increases estrogen levels by inhibiting its CYP-mediated metabolic inactivation
o gynecomastia in men
o galactorrhea in women
dicyclomine brand name
Bentyl
MOA of dicyclomine (lentil)
antagonizes the muscarinic ACh-R on parietal cells therby decreasing gastric acid secretion
why are anticholinergic agents rarely used?
because they're less effective and have less desirable side effects
ADEs of anticholinergic agents
o Dry mouth
o Blurred vision
o Cardiac arrythmias
o Urinary retention
what are PPIs
substituted benzimidazole prodrugs that block the activity of this transport protein for proton (H+) molecules
what cell type are proton pumps unique to?
parietal cells
what facilitates the MOA of PPIs
the pH of the stomach
PPI MOA
Irreversibly inhibit the H+/K+-ATPase in gastric parietal cells
o Produces dose-dependent inhibition of gastric acid secretion that persists even after the drug disappears from the plasma
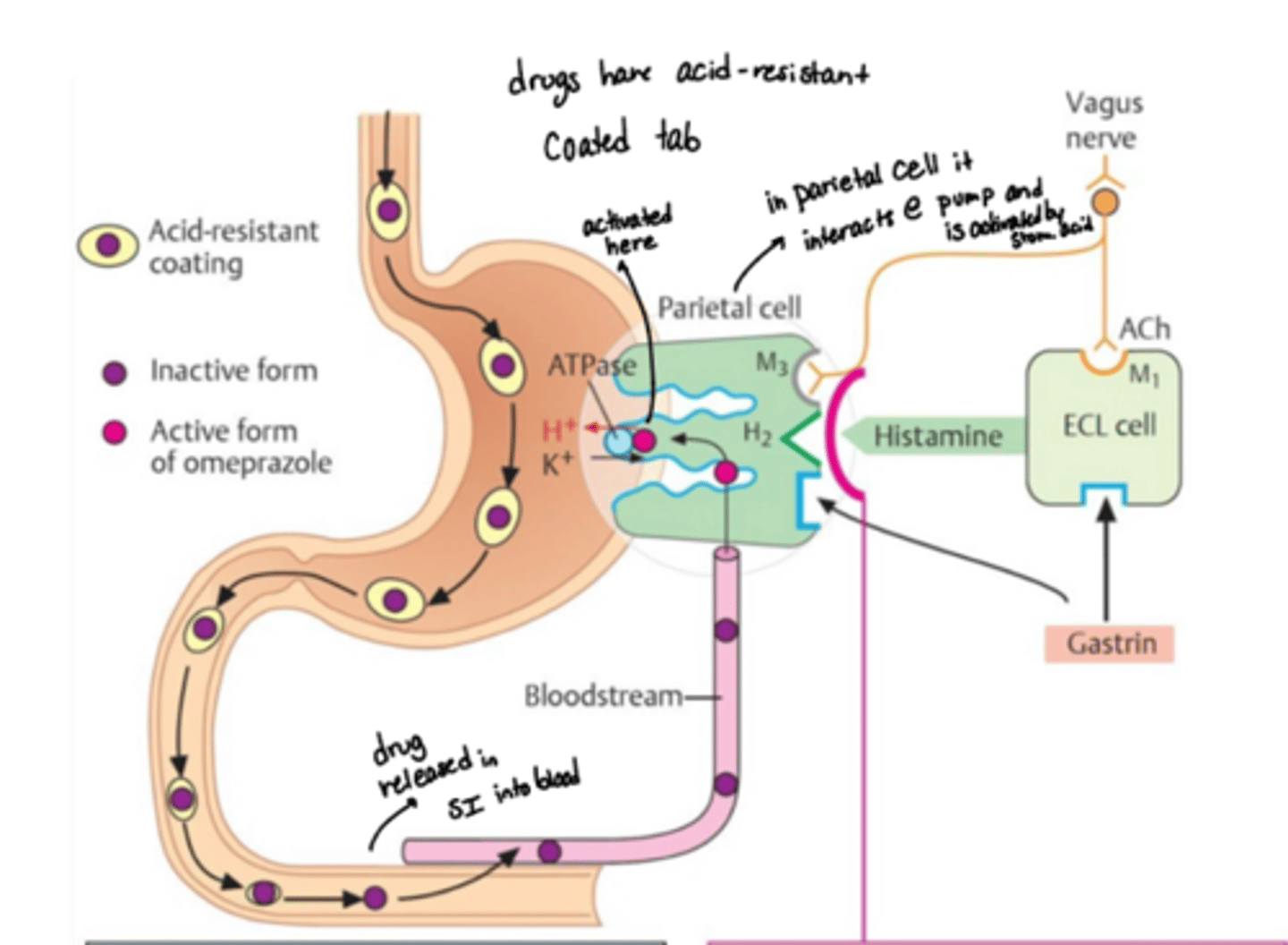
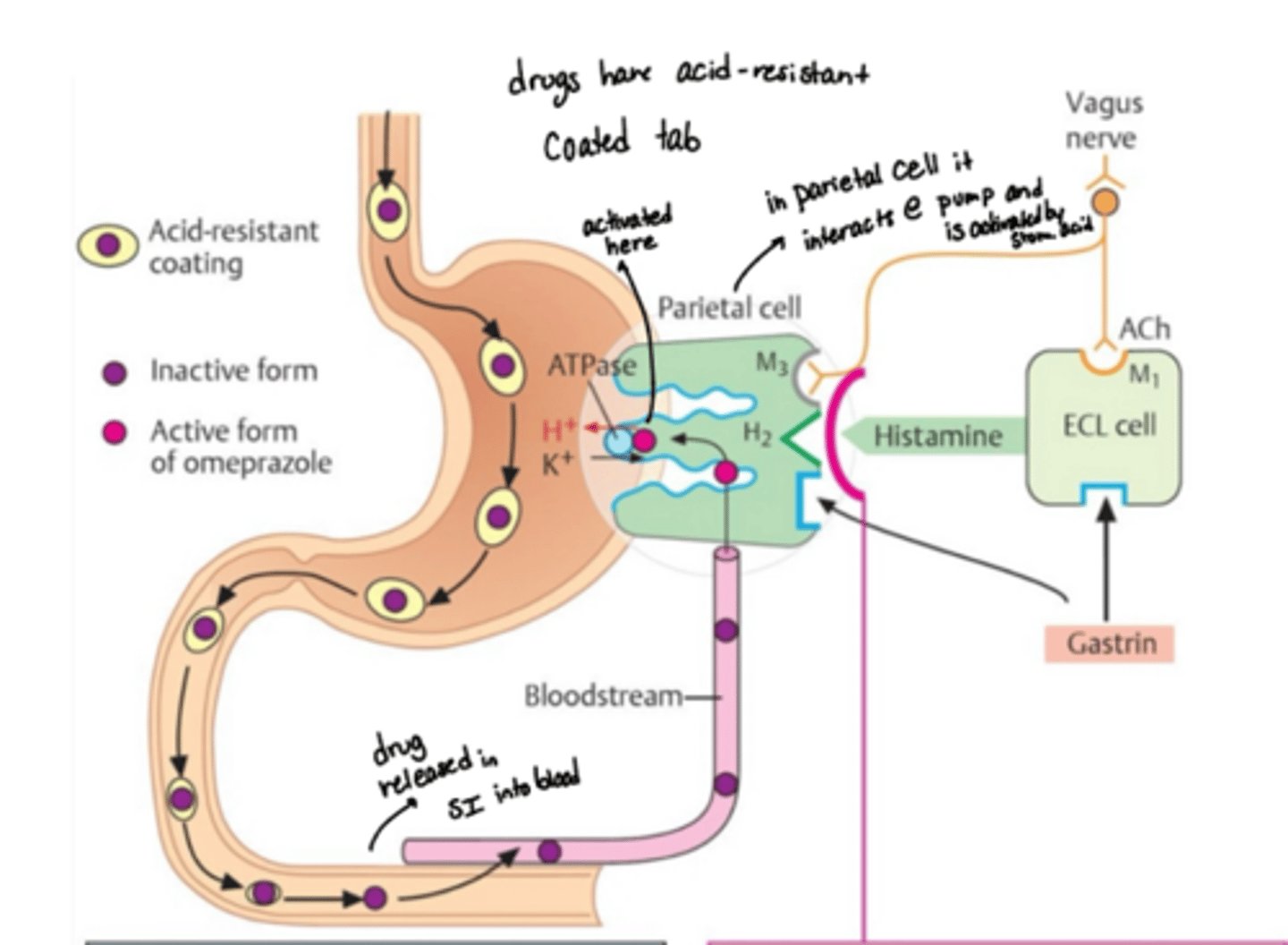
what environemnt are PPIs active vs inactive
PPIs are inactive at neutral pH, but they are weak bases so in acidic stomach they’re activated
how are PPIs activated from their prodrug form?
require activation from the parietal cell canaliculus (side of cell that faces the acidic lumen of the stomach)
o PPIs are activated only when bound to the proton pump and exposed to the acid of the stomach
describe the release path of PPIs
· PPIs need to pass intact through the stomach into the intestines where the drug is released from its enteric coating formulation for absorption into the blood
· The pro-drug reaches the parietal cells via blood
· The pro-drug then diffuses into the canaliculi of parietal cels facing the lumen where the acidic environment converts the pro-drug into a sulfonamide reactive intermediate
· The active drug then binds to sulfhydryl groups of cysteine residues in the pump, leading to irreversible activation
PPI and infections
increase in pH may mean other bacteria may be able to tolerate the environment (C. diff, salmonella, E. coli)
DDI of PPIs
competition with clopidogrel for CYP2C19
both these drugs need to be activated by this enzyme
PPI possible side effects?
osteoporosis and bone fractures from decreased absorption of Ca in higher pH
kidney disease and dementia associations
how does mucosal erosion and ulceration occur in peptic acid diseases
pepsin-mediated hydrolysis of mucosal proteins
MOA of mucosal protective agents
create a barier in stomach and intestinal mucosa that prevents damaging effects of HCl and pepsin
they also bind pepsin and bile salts
misoprostol brand name
cytotec
what is mistoprostol and when is it used
o Prostaglandin E1 analog (PG stimulate mucus and bicarbonate production)
o Used when treatment with NSAIDs inhibits endogenous PG synthesis
when should mistoprostol not be used
in women of child-bearing potential
sulcralfate brand name
carafate
what is sucralfate made of
Complex of aluminum hydroxide and sulfated sucrose
MOA of sucralfate
o Undergoes polymerization and cross linking at low pH of stomach
o Binds tightly to the necrotic/ulcerated tissue
o Forms complex gel with mucus; mucus stabilized; diffusion of HCL and pepsin to mucosa is impaired
why does sucralfate have little side effects
not absorbed into the blood
duodenum and sucralfate
Although the pH of duodenum is >4, sucralfate retains its viscosity and binds tightly to the ulcerated intestine as well
colloidal bismuth compounds MOA
o Second coating agent (not mucus-like)
o Bismuth salts combine with mucus glycoproteins to form a barrier that protects the ulcer from further damage by acid and pepsin
o Bismuth is also known to stimulate secretion of bicarbonate, PG, and mucus
colloidal bismuth effect on H. pylori
o Colloidal bismuth has been shown to impede the growth of H. pylori
§ used in combination with antimicrobial agents and PPIs in patients that are H. pylori positive
what is H. pylori
gram-negative, spiral shaped bacterium that is flagellated
what is the most common cause of non-NSAID associated peptic ulcer disease?
H. pylori
where can H. pylori be found
found in the antrum of the stomach in a significant number of patients with duodenal and gastric ulcers
how does H. pylori survive in the acidic conditions of the stomach and thrive
because it produces ammonia from urea by urease enzymes
the ammonia neutralizes the gastric acid and allows the bacteria to escape digestion
it can then proliferate, migrate, and form infection
destroys mucosa and causes immune-mediated inflammation and mucosal cell death
what does H. pylori prevalence correlate with
socio-economic status and older age
what are the 5 types of treatmets for H. pylori?
· antibiotics
· antisecretory agents
· mucosal protectants
· antisecretory agents that enhance mucosal defenses
· antacids
antibiotic ulcer therapy
A. Combinations must be used:
Bismuth:- disrupts cell wall of H. pylori
Clarithromycin- inhibits protein synthesis
Amoxicillin- disrupts cell wall
Tetracyclin- inhibits protein synthesis
Metronidazole
- used for bacterial resistance
clarithromycin function in combination antibiotic ulcer therapy
inhibits protein synthesis
amoxicillin function in combination antibiotic ulcer therapy
disrupts bacteria cell wall
tetracycline function in combination antibiotic ulcer therapy
inhibits protein synthesis
metronidazole function in combination antibiotic ulcer therapy
bacterial resistance
bismuth (pepto bismol) function in combination antibiotic ulcer therapy
disrupts cell wall of H. pyrlori; coating agent
what do PCABs (potassium competitive acid blockers) target?
target the proton pump in gastric parietal cells (the cells responsible for secreting peptic acid into the stomach
what is an example of a PCAB
vonoprazan
what does PCAB stand for?
potassium competitive acid blockers
MOA of PCABs
bind to proton pumps like PPIs but non-covalently (reversible)
potassium-dependent
benefit of PCABs
they don't irreversibly bind so they can be controlled by the timing of the dosing strategy
PPIs depend on the half-life of the proton pumps
vonoprazan brand name
Voquesna