Paediatric Skin
1/23
Earn XP
Description and Tags
SKIN
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
24 Terms
Develop an understanding of why rashes occur.
Differentiate between a blanching and non blanching rash and understand the underlying aetiology.
Awareness of Clinical Red flags and when to refer for immediate treatment.
Identify the most common causes of rashes in children
LOs : 4
Rash is due to inflammation or discolouration of the skin, which changes the skin’s normal appearance, colour and texture
Aetiology: allergies, infections, irritants, autoimmune conditions
Clinical presentation: itching, swelling, lumps, spots, or blisters
Dry scaly patches/lesions
What is a rash?
A rash that disappears or fades when you press on it, generally less serious
Cause: inflammation or vasodilatation of the blood vessels in the skin, usually due to viral infection, allergy, heat rash, and urticaria
Blanching rash definition and why it happens, what are the common causes
a rash that does not fade, or change in its colour when pressed
Why: erythrocyte extravasation ; blood that has leaked underneath the skin, it does not fade as not confined to blood vessels
common causes: meningococcal septicaemia, vasculitis, thrombocytopenia, trauma
LIKELY A RED FLAG ? Medical emergency
Non-Blanching rash definition and why it happens, what are the common causes
Non-blanching rash presence,
press the side of a glass firmly against a rash so you can see if it fades under pressure. If it doesn’t fade this will be classed as a non blanching rash
What is a glass test for?
Is this a non-blanching rash, do they appear systemically unwell
Any signs of anaphylaxis, ABCDE assessment
Abnormal physical obvs: NEWS OR POPS ( under 16s score)
Associated symptoms of fever, neck stiffness, photophobia, N&V
involvement of the mucus membranes, conjunctiva, oral cavity- think SJS (Stevens-Johnson Syndrome / Sepsis
Extreme pain - possible causes, shingles is particularly painful, as a clinical marker
is the skin peeling blistering? SSS ( children)
Has the patient recently been commenced on any new medication ( possible ADR or allergic reaction)
Has the child been fully immunised ( e.g., the current meningitis vaccine is only children born after 2015, new schedules may be updates with more ages to be included)
What are the RED flags to rule out for skin rash? 9
Onset and duration: does the rash come and go
has the rash changed in appearance, is it spreading elsewhere
Where did it first appear
associated symptoms: recent illness, fever, pain, itch, oozing, bleeding and blistering
Exposures:, travel, medications, pets, bites or stings, recent sports ( golf) , new products/ lotions or potions, contact with others and outdoor exposures
Based on physical observation of the child, i.e. are they appearing full of energy, no systemic symptoms, have they recently been unwell: possibly a post-viral rash that appears after the child has fully recovered and rash appars post-immune response ( not a red flag), if they are still in diapers, more indication to check the less exposed areas, as rash could be hidden
Clinical assessment questions to assess the complication: 5
Notifiable disease report to UK Health Security Agency (UKHSA)
Highly contagious for those who haven’t been immunised
Symptoms include:
Coughin and sneezing
runny nose
fever
Red/sore eyes
Spots ( Koplik ) in mouth
Blanching rash which starts on the face and behind the ears
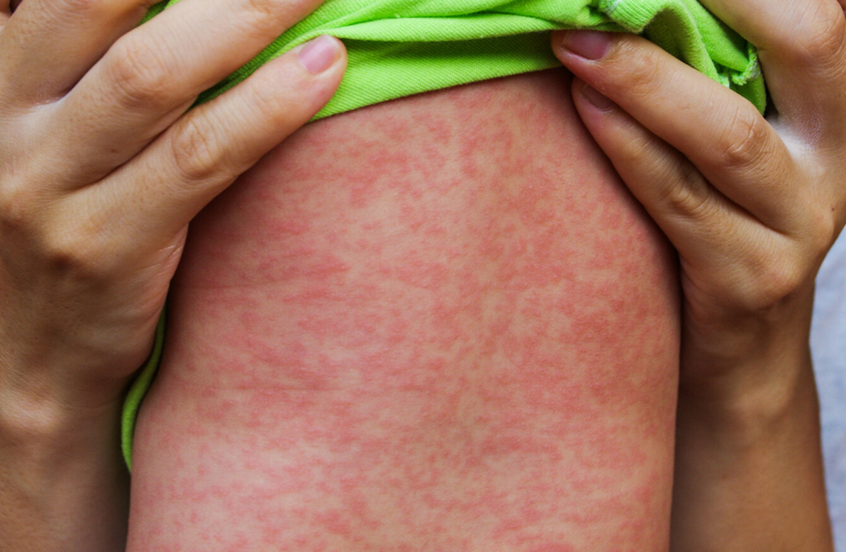
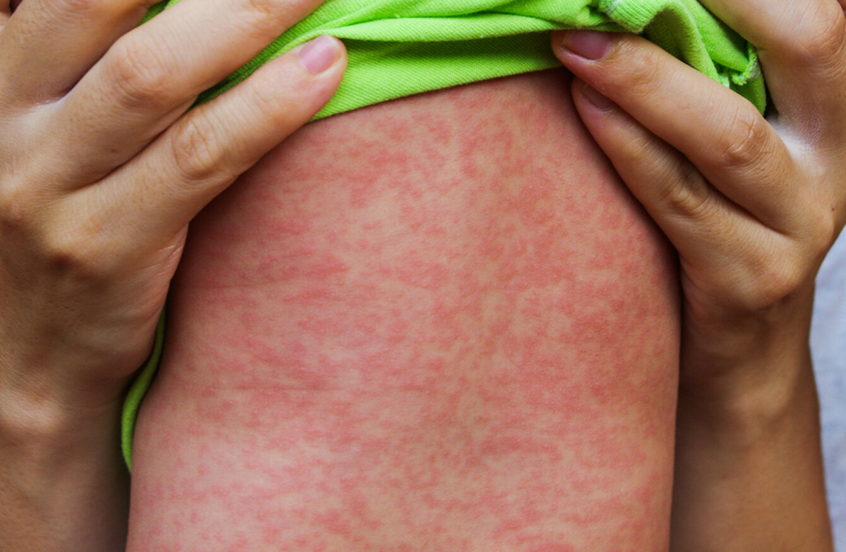
Measles: what does it look like, and clinical presentations: 6 points
Self-limiting illness normally improving after 1 week
Important to reduce cross-infection to others by self-isolating for 4 days after rash develops
Self-Care advice: constant hydration, eye warm water bathing, managing pyrexia
Advise patients of RED flags to observe for such as confusion, lethargy and signs of dehydration
High risk patients include, under 5s, pregnancy, immune suppresed
What is the treament of measles?
Highly contagious airborne virus, caused by the varicella zoster virus, commonly in younger children
can be difficult to diagnose initially, especially if the child is presenting with mild cold symptoms and only a few spots
Symptoms:
Extremely itchy rash
Fever
Abdominal pain
Swollen glands
Headache
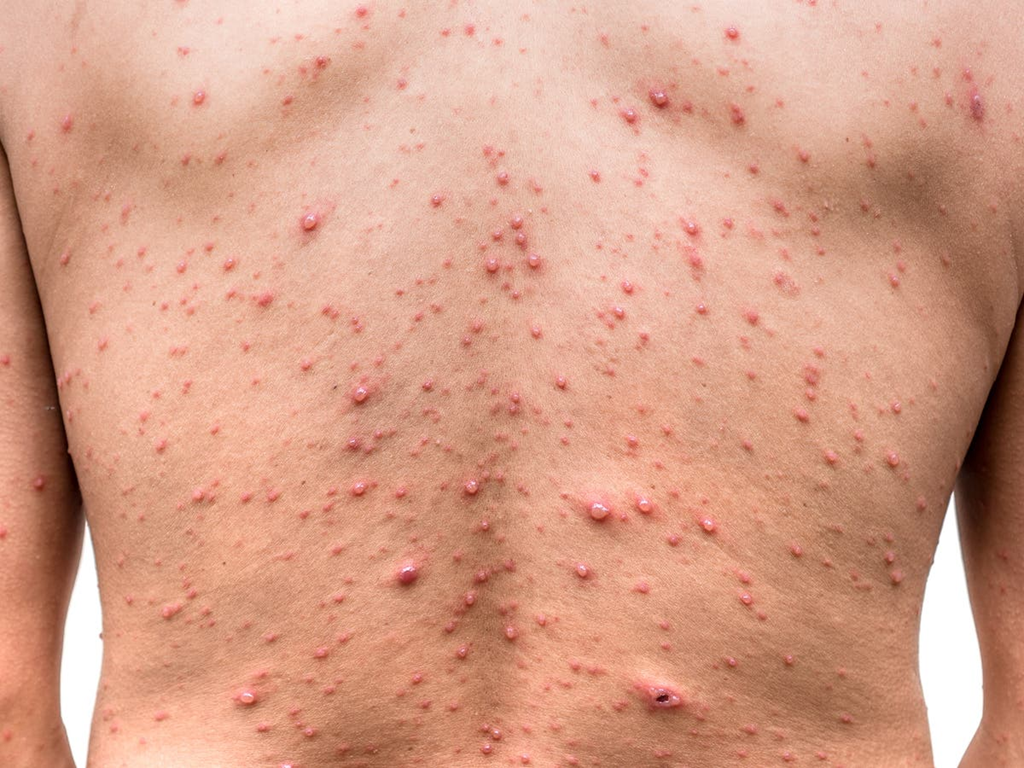
Chicken pox: what does it look like, and clinical presentations: 5 points
Aciclovir (POM) is only indicated for the seriously il patients, not usually indicated in normal presentation of unincomplicated chicken pox of healthy person
Manage symptoms: OTC, paracetamol, chlorphenamine, soothing creams; that prevent itching, scarring and 2ndary infection, Poxclin ( a relatively new foam formulation), and calamine and (aq) cream, in order to prevent itching as it’s vital to protect against scarring and 2ndary infection
Ibuprofen in contraindicated as it affects the immune response, and masks 2ndary infection, actual reason is still thereotical
Incubation period is 14-21 days, (long) before clinical symptoms appear
What is the treatment plan for chicken pox treatment? 4
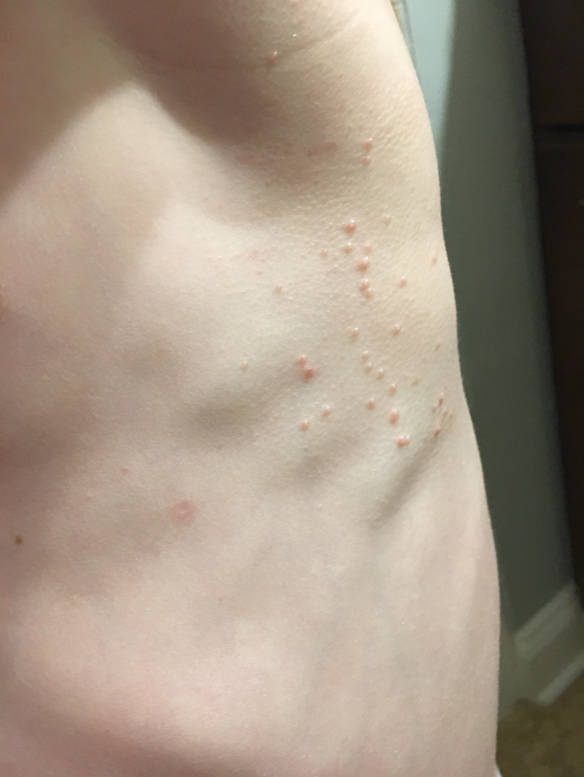
A common, benign, viral skin infection. causing small, firm, dome shaped pink or skin-colored bumps, usually with a central, shiny dimple. It’s contagious, via skin-to-skin contact or shared items, commonly in children, who are between 1-10 and is self-resolving, however can last from anywhere from, days to months and years
Molloscum contagiosum: what does it look like and how is it clinically presented?
caused by Staph, A infection
Pustules & honey coloured crusty erosions
If left untreated, 2ndary infection, will occur and skin lesions will spread to other parts of the body
Strict infection prevention is required to prevent spread of infection to others
Topical treatment is 1st line
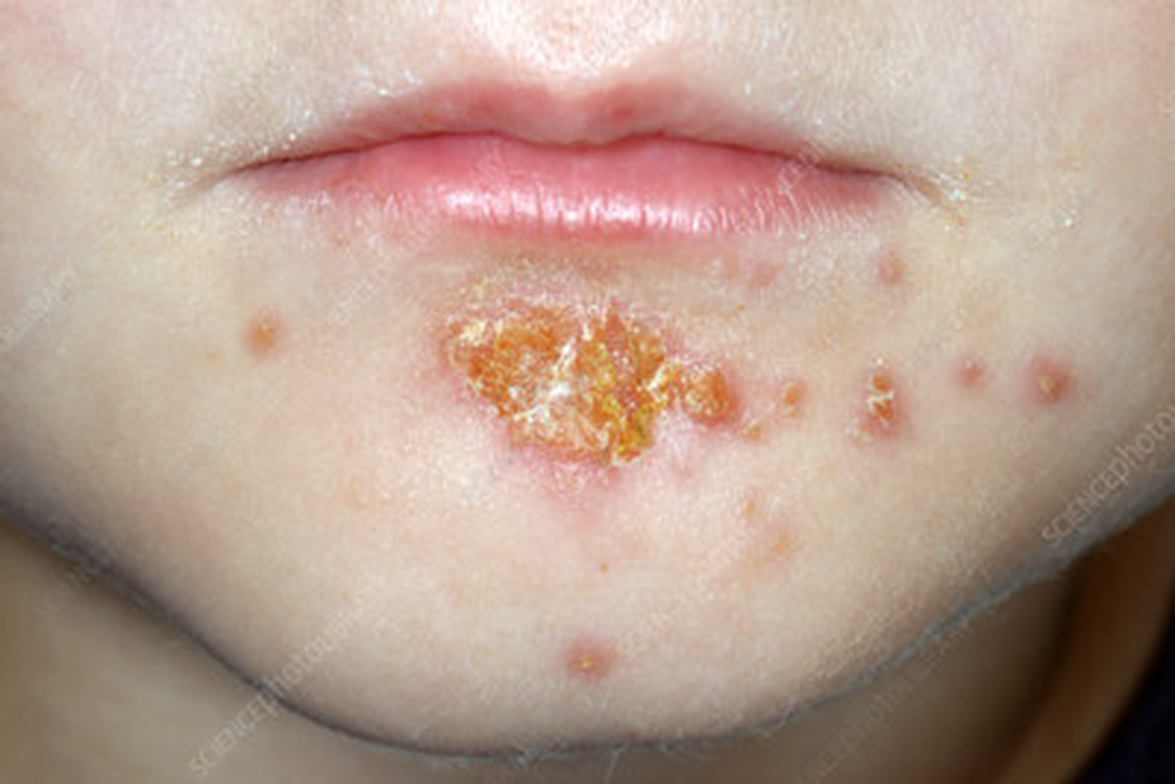
Impetigo: what does it look like, and clinical presentations: 5 points
If there’s less than 3 lesions/clusters and its not localised non bullous lesions
hydrogen peroxide 1% for 5 days
Fusidic acid 2% cream for 5 days
If there’s more than 4 lesions/clusters (widespread non-bullous lesions), give flucloxacillin for 5 days
What is the the treatment pathway for impetigo in pharmacy 1st?
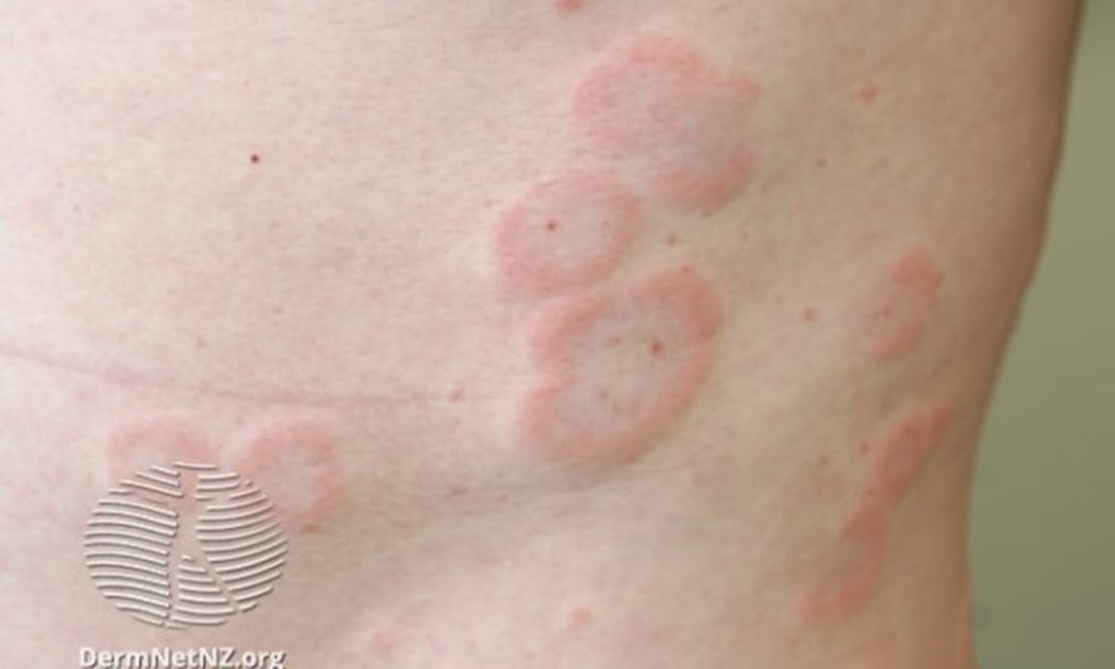
characterised as raised, itchy welts, on skins, with varying sizes
Triggers can be anything from allergies, emotions, illness, environmental, viral illness
Duration short or long depending on trigger
Caution: obsserve for signs of allergy, ABCDE assesssment
Though often only itchy, may also be burning or stinging sensation
Urticaria ( Hives): clinical presentation
Triggers and duration (5)
Acute Urticaria o
Non-sedating anti-histamine (Cetirizine, Loratadine, Fexofenadine) until GP review.
Topical Anti-pruritic treatment- Calamine in aqueous cream or topical menthol 1% in aqueous cream)
Sedating anti-histamine- Chlorphenamine-nighttime itch
Prickly heat
Non-sedating anti-histamine (Cetirizine, Loratadine, Fexofenadine)
• Topical Anti-pruritic treatment- Calamine in aqueous cream or topical menthol 1% in aqueous cream)
Hydrocortisone cream- depending on age (OTC)
General advice- apply a cool damp towel for up to 20 minutes
What is the community pharmacy treatement/advice for acite urticaria ( hives or prickly heat)
Hair follicles that become trapped with sweat and lead to inflammation, i.e. could be observed in men’s beard, when shaving using blunt/unhygienic razors
usually, Hot tub, slip & slide, especially if not showering right after event, can lead to build-up of bacteria
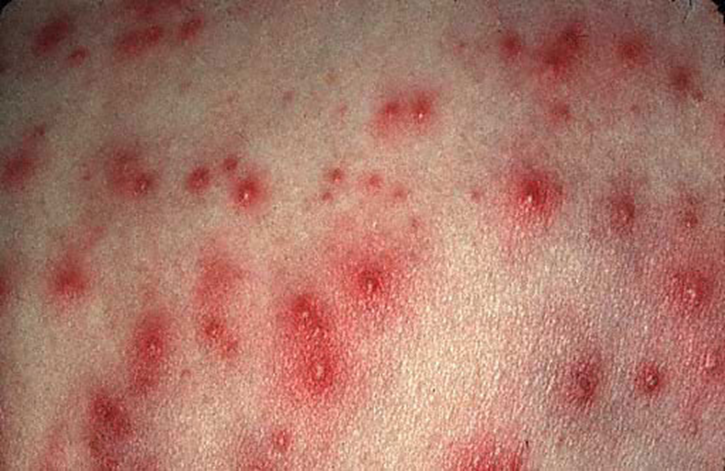
Aetiology and clinical representation of Hot Tub follicuulitis
Prevention (removing used swimwear, shower immediately after using, wash swimwear after use, regular cleaning, and maintenance of the hot tub.)
Topical antiseptics (to prevent infection) such as Dermol or Chlorhexidine
Mid topical steroids (to help reduce inflammation and itch)- Hydrocortisone OTC
Antibiotics
Treatment for Hot Tub Folliculitis: 4
Fluid-filled blisters on torso, between fingers, hands, and feet -viral, self-limiting
the actual virus stays in the childs’ faeces till 8 weeks, thus when changing nappies at home or nursery, important to let whoever changes their nappy to be aware, and caution with those pregnant
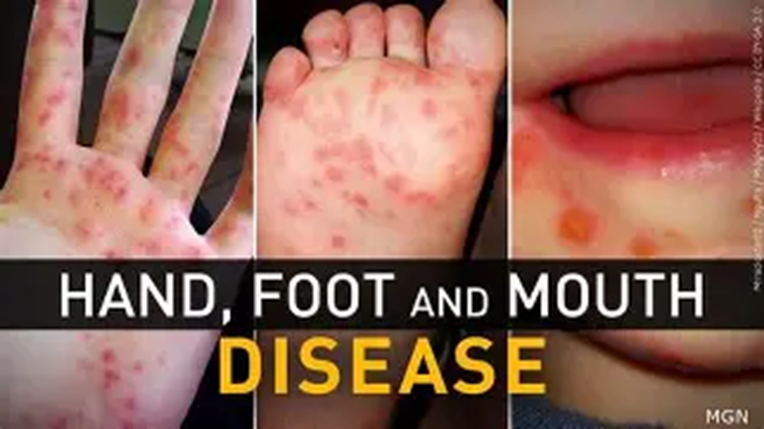
Hand, Foot and Mouth disease: Slapped Cheek syndrome, clinical presentation
Viral- Antibiotics unsuitable (unless secondary infection
Paracetamol/Ibuprofen to ease symptoms
Mouthwash (Chlorhexidine Digluconate, Hydrogen Peroxide 1.5%)
Ulcer treatment- e.g Anbesol/Bonjela oSore throat spray- (Benydamine 0.15% spray)
General advice- keep hydrated, soft foods, avoid spicy/salty foods.
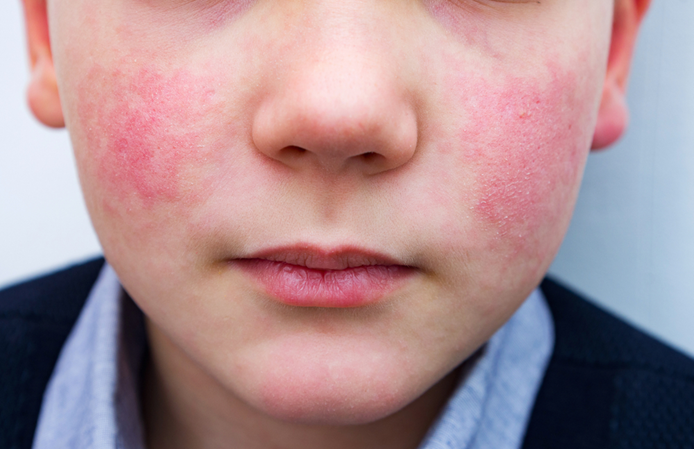
Slapped cheek syndrome
Viral- Antibiotics unsuitable (unless secondary infection)
Paracetamol/Ibuprofen to ease symptoms
Rest and fluids to prevent dehydration
Community Pharmacy treatment for HFM disease: ( very similar to measles) 5
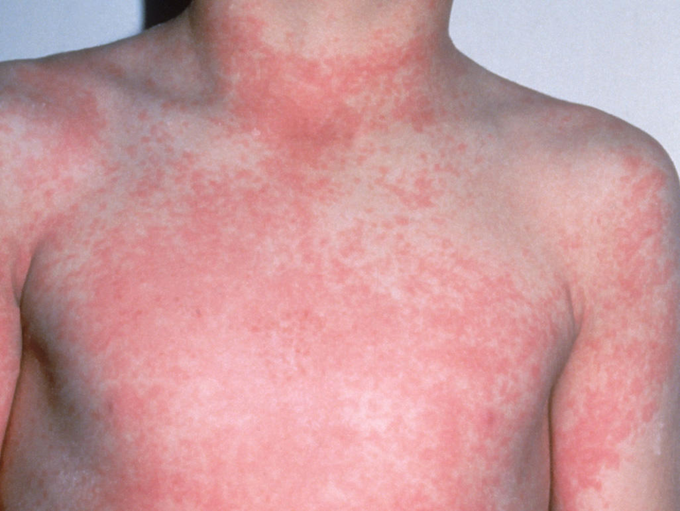
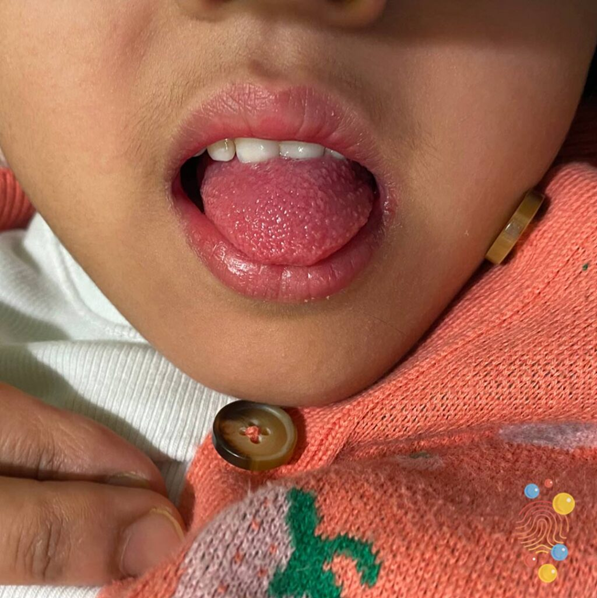
Scarlett Fever Rash : very similar to other rashes, i.e measles, urticaria, how the actual rash presents clinically is somewhat different; strawberry tongue, fever and sandpaper fee
Clincal presentation of this rash
Clinical Pathway Pharmacy first for Sore Throat
important to differentiate between Scarlet Fever and Acute Bacterial Sore throat.
Scarlet fever- sand paper rash on torso, strawberry tongue, fever, sore throat.
Acute Bacterial sore throat- Pus/inflamed tonsils, sudden onset, no cough, fever.
Trearment:
Scarlet Fever:
Antibiotic – Phenoxymethylpenicillin first line (or Clarithromycin if pen v allergic) for 10 days
(Consider Pill school counselling for patients- Tablets better adherence as medicine very bitter.
Acute Sore throat- Treatment, Antibiotic – Phenoxymethylpenicillin first line (or Clarithromycin if pen v allergic) for 5 days (Pharmacy First)
How to differentiate Scarlet fever from other ailments and treatment pathway
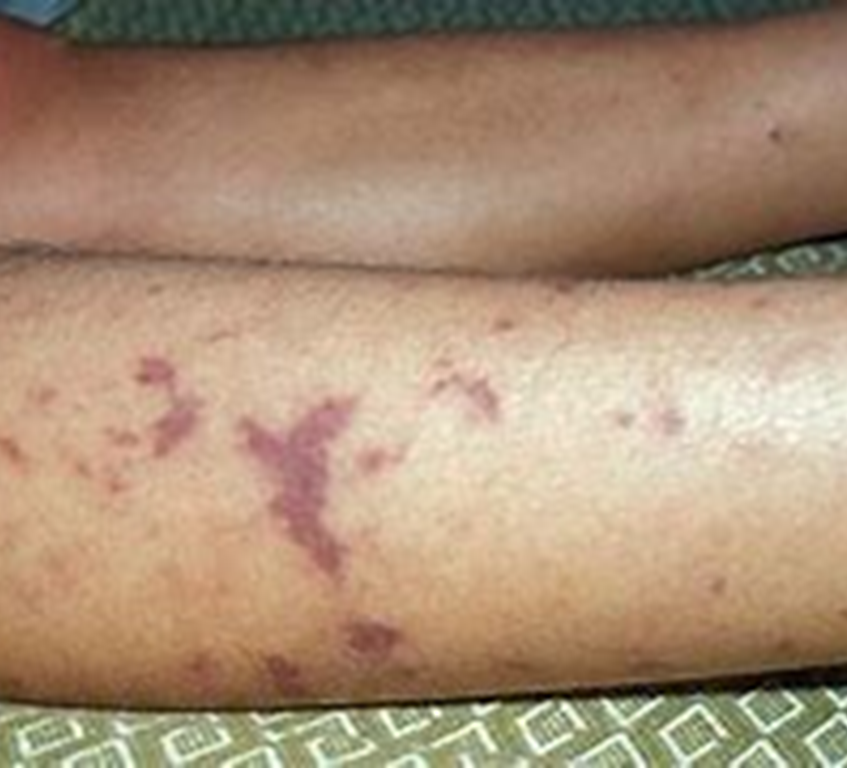
Meningitis:non blanching purpuric type rash, bruising beneath the skin. Likely due to meningitis- importance here is to identify that the rash is non blanching and where to safely sign post to- likely AED for immediate assessment and treatment
•Differentials- HSP/ ITP/ Kawasaki syndrome.
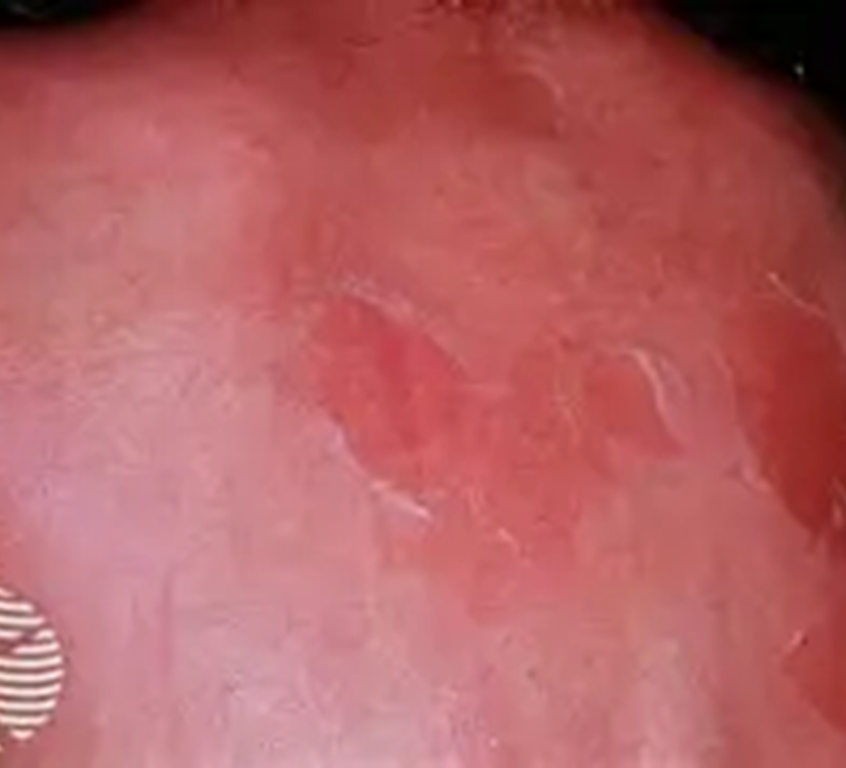
SSS: scalded skin syndrome, caused by Staph A. bacteria. Superficial blistering and peeling of the skin resembles scald injury but no history of burns.
•Child is normally pyrexic with general lethargy.
•Painful blistering rash appears 24-48 after initial symptoms start.
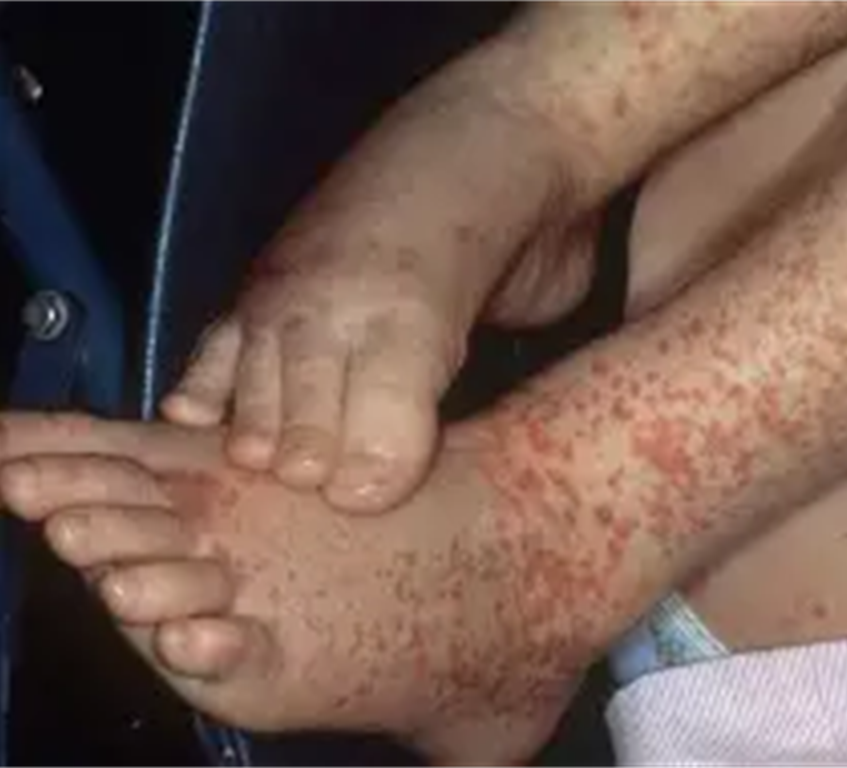
3.•HSP- Henoch- Schoenlein Purpura- non blanching rash normally forms in lower limbs and lower part of torso.
•Auto immune condition- multiple triggers-form of vasculitis. Affects the blood vessels, causing them to rupture beneath the skin.
Child will experience abdo pain and general myalgia ( joint pain
What are the 3 red flag rashes, and their clinical presentations
UKHSA ( UK Health Security Agency)
Condition to be aware of in Community Practice
Scarlet Fever- Routine notice ( within 3 days)
Chickenpox- Routine notice
Measles- Urgent notice ( 24 hours )
Meningitis- Urgent notice
What are the notifiable diseases 5 and what organisational body is that?