Micro - Ch. 9
1/28
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
29 Terms
Define sterilization
Process that destroys or removes all viable microorganisms (including viruses and endospores)
Used for inanimate objects:
Surgical instruments, syringes, and commercially packaged food
Ex:
Heat (autoclave)
Sterilants (chemical agents capable of destroying endospores)
Define disinfection
Physical process or a chemical agent to destroy vegetative pathogens but not bacterial endospores
Removes harmful products of microorganisms (toxins) from material
Used on inanimate objects:
Boiling food utensils, 5% bleach solution on examining table, immersing thermometers in an iodine solution between uses
Ex:
Bleach
Iodine
Heat (boiling)
Define decontamination (sanitization)
Cleansing technique that mechanically removes microorganisms as well as other debris to reduce contamination to safe levels
Primarily used in food places such as restaurants that handle soiled utensils/containers:
Cooking utensils, dishes, bottles, cans
Ex:
Soaps
Detergents
Commercial dishwashers
Define antisepsis (degermation)
Reduces the number of microbes on the human skin
A form of decontamination but on living tissues
Involves scrubbing the skin (mechanical friction) or immersing it in chemicals (or both)
Ex:
Alcohol
Surgical hand scrubs
What are considered the most resistant microbial structures?
Endospores
The goal of sterilization is the destruction of bacterial endospores
If it kills endospores, it will kill all less resistant microbial forms
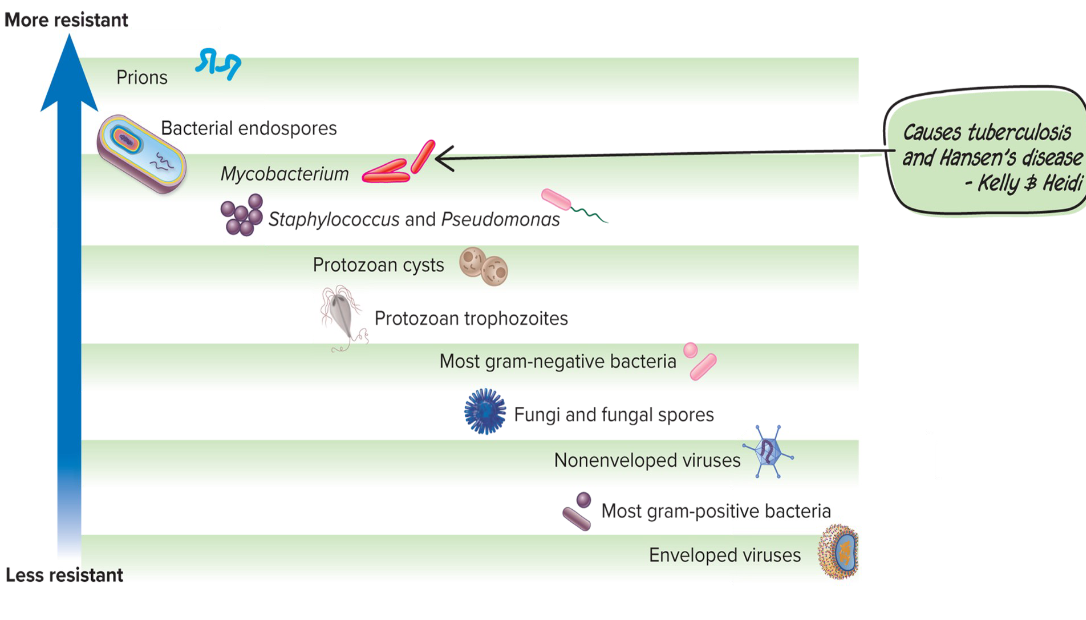
Rank the relative resistance of microbial forms from more resistant to less resistant
Prions
Bacterial endospores
Mycobacterium
Staphylococcus and Pseudomonas
Protozoan cysts
Protozoan trophozoites
Most gram-negative bacteria
Nonenveloped viruses
Most gram-positive bacteria
Enveloped viruses
Explain endospores
Function: resist heat, drying, freezing, radiation, and chemicals. Only formed under extremely stressful conditions in the cell
Vegetative cell: metabolically active cells
Endospores = metabolically inactive cell
What are critical medical devices?
Expected to come into contact with sterile tissues
Must be sterilized before use
What are semicritical devices?
Come into contact with mucosal membranes
Must receive high-level disinfection, preferably sterilized
What are noncritical devices?
Do not touch the patient or only touch intact skin
Require only low-level disinfection unless they become contaminated with blood or body fluids
What is the difference between microbicidal agents and microbistatic agents?
Microbicidal: Agents that kill the microbe
Microbistatic: Agents that only inhibit growth (removal = growth again)
Explain agents vs. processes
Sterilization and disinfection are processes
Agents used in the processes:
Bactericide
Fungicide
Virucide
Sporicide
Germicide/microbicide
Define bactericide
Chemical that destroys bacteria except for those in the endospore stage. Irreversible
Ex:
Alcohols
Phenolics
Quaternary Ammonium Compounds (Quats)
Define fungicide
Chemical that can kill fungal spores, hyphae, yeasts
Ex:
Chlorine compounds
Copper compounds
Hydrogen peroxide
Define virucide
Chemical known to inactivate viruses, especially on living tissue
Ex:
Halogens
Aldehydes
Sodium Hypochlorite
Define sporicide
An agent capable of destroying bacterial endospores
Ex:
Ethylene Oxide (EtO)
Peracetic Acid
Glutaraldehyde
Define germicide/microbicide
Chemical agents that kill microorganisms
Ex:
Formaldehyde
Chlorine dioxide
Define bacteristatic
Chemical agents that prevent the growth of bacteria on tissues or on objects in the environment. Reversible
What are the dry heat methods?
Incineration - sterilization
Dry oven - sterilization
Describe the incineration/dry oven method
A flame is the most rigorous of all heat treatments
The flame of a Bunsen burner reaches 1,870°C at its hottest point
Reduces microbes and other substances to ashes and gas
Sterilization
What is dry heat?
Dehydrates the cell
Denatures proteins (dry and moist heat)
At very high temperatures, oxidizes cells, burning them to ashes
What are moist heat methods?
Steam under pressure/autoclaving - sterilization
Boiling water, hot water, pasteurization - disinfection
Describe the autoclave method
Can be used for:
Glassware
Cloth (surgical dressings)
Metallic instruments
Liquids
Some media
Cannot be used for:
Substances that repel moisture (oils, waxes)
Substances that are harmed by it (powders)
Heat-sensitive items (plastic Petri dishes)
Sterilization
Describe the boiling water: disinfection method
Boiling water bath can decontaminate items in the clinic and home
100°C will not kill all resistant cells - good for disinfection and not for sterilization
Boiling water for 30 minutes will kill most non-endospore-forming pathogens
Disadvantage: items can be easily recontaminated when removed from the water
Disinfection
Describe the pasteurization: disinfection of beverage method
Fresh beverages such as milk, fruit juices, beer, and wine are easily contaminated during collection and processing
Because microbes have the potential for spoiling these foods or causing illness, heat is frequently used to reduce the microbial load
Pasteurization is a technique in which heat is applied to liquids to kill potential agents of infection and spoilage, while at the same time retaining the liquid’s flavor and nutritional value
Disinfection
Describe the effects of cold
Principal benefit of cold treatment is to slow growth of cultures and microbes in food during processing and storage:
Cold merely retards the activities of most microbes
Most microbes are not adversely affected by gradual cooling, long-term refrigeration, or deep-freezing
Temperatures from -70°C to -135°C can preserve cultures of bacteria, viruses, and fungi for long periods
Describe the radiation method
Radiation emitted from atomic activities and dispersed at high velocity through matter or space:
Gamma rays
X rays
Ultraviolet radiation
What are radiation methods?
Ionizing: X ray, cathode, gamma - sterilization
Nonionizing: UV - disinfection
Describe the filtration method
Effective method to remove microbes from air and liquids
Fluid is strained through a filter with openings large enough for the fluid to pass, but too small for microbes
Used to prepare liquids that cannot withstand heat such as serum, vaccines, drugs, IV fluids, enzymes, and media
Alternative method for decontaminating water, milk, and beer without altering their flavor
High-efficiency particulate air (HEPA) filters are used in hospital rooms and sterile rooms