respiratory system
1/92
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
93 Terms
functions of the respiratory system
provides gas exchange, regulates blood pH, smell receptors, filters air, produces vocal sounds, excretes water and heat
pulmonary ventialtion
moving air into/out of the lungs
NO GAS EXCHANGE
external respiration
exchange of gases at the alveoli
internal respiration
exchange of gases between blood and tissues
structures of the respiratory system
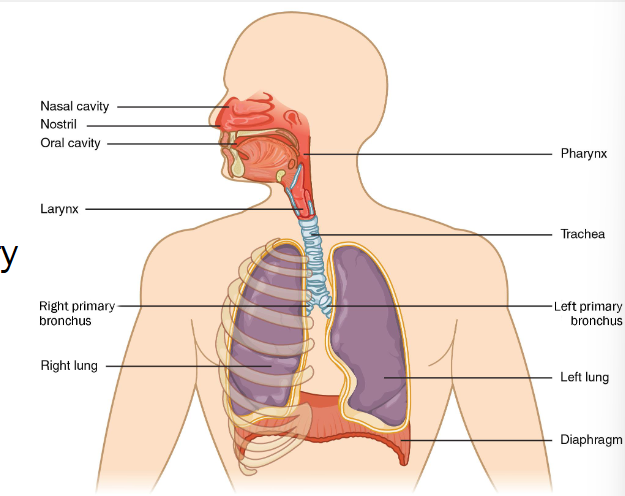
nose and nasal conchae
entry point, hyaline cartilage
conchae, lined with mucous, warms filters air via turbulence
sinuses
cavities within cranial bones
resonate sound
pharynxes
naso: respiratory only
oro and laryngo: respiratory and digestive
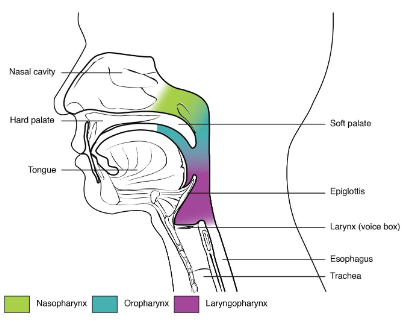
larynx
connect laryngopharynx to trachea
voice box
inferior to hypoid bone and epiglottis
trachea
wind pipe
c-shaped cartilage rings give support
anterior to esophagus
carina
internal ridge where trachea divides into primary bronchi
Bronchi
primary, secondary, tertiary, bronchioles, terminal bronchioles
label lungs
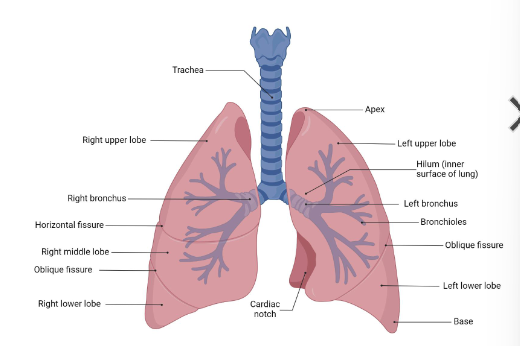
hilum
where bronchi, vessels, and nerves enter at here
pleura
visceral adheres to lung
parietal adheres to chest wall
space between is pleural cavity, filled with fluid
diaphragm
separates the thoracic and abdominal cavities
responsible for 75% of air that enters the lungs
internal intercostals helps with
exhalation
external intercostal help with
inhalation
innervation of the diaphragm
phrenic nerve
“C3, 4, 5 keep the diaphragm”
sympathetic nervous system
norepinephrine causes dilation of bronchial smooth muscle
pulmonary plexus
nerves form this in hilum of lung
parasympathetic nervous system
innervation via vagus nerve CN X
acetylcholine released
causes mucous secretion, constriction of bronchial smooth muscle
conduction zone
part of the respiratory system that bring air into or out of the lungs
nose, pharynx, larynx, trachea, bronchi, bronchioles, terminal bronchioles
respiratory zone
part of the system where gas exchange takes place
respiratory bronchioles, alveolar ducts, alveolar sacs, alveoli
upper respiratory tract
nasal cavity, oral cavity, pharynx
lower respiratory tract
trachea, bronchi, lungs, bronchioles, alveoli
larynx
bridge between upper and lower tracts
stratified squamous epithelium
part of larynx and pharynx
protection
respiratory epithelium
pseudostratified columnar or simple columnar
mucous and cilia on the luminal surface
goblet cells
secrete mucus
mucociliary escalator
mucus + cilia
brings particles out of the lungs and into the pharynx to be swallowed
bronchi smooth muscle: sympathetic
dilate
bronchi smooth muscle: parasympathetic
constrict, increase secretions
label alveolus
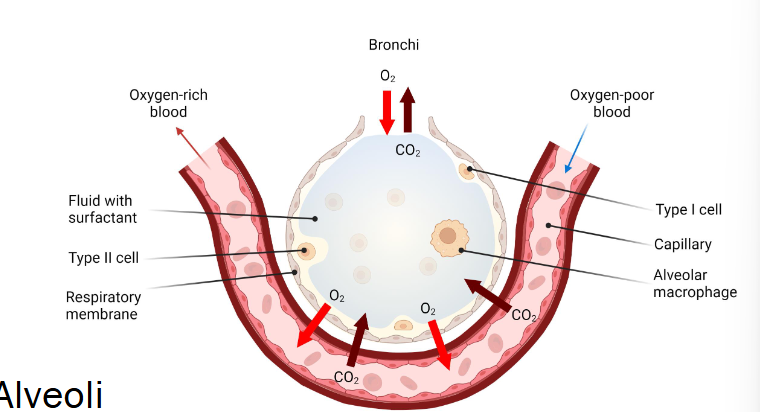
Type I cells
simple squamous, gas exchange
Type II
simple cuboidal, secrete surfactant
inspiration
inhalation
move air into the lungs
active process, requires muscle action
expiration
exhalation
move air out of the lungs
usually passive
pressure
collisions of molecules within the wall of the container
temperature
speed at which molecules move
Boyle’s law
pressure and volume are inversely related
if volume goes up
pressure goes down
if volume goes down
pressure goes up
“pump handle”
action of sternum
“bucket handle”
action of ribs
inhalation
diaphragm and external intercostal contract
increase volume, decrease pressure
exhalation
diaphragm relaxes, internal intercostal contract
decrease volume, pressure increase
tidal volume
volume of air inspired or expired during normal breathing
inspiratory reserve volume
all of the air that you can breathe in from the top of tidal volume (deep inhalation)
expiratory reserve volume
all of the air you can breathe out from the bottom of tidal volume during a forced exhalation
residual volume
air still present in lung after maximal exhalation
keeps lungs open
“dead space”
inspiratory capacity
tidal volume + inspiratory reserve volume
function residual capacity
residual volume + expiratory reserve volume
vital capacity
inspiratory reserve volume + tidal volume + expiratory reserve volume
total lung capacity
vital capacity + residual volume
Dalton’s law
sum of partial pressures
Henry’s law
the amount of gas dissolved in a liquid is proportional to the pressure of the gas above the liquid
external respiration
refers to the gas exchange that occurs between the alveolus and capillaries
oxygen moves from alveolus to the capillary
CO2 moves from capillary to the alveolus
gases move by diffusion
V with dot above
amount of air entering lungs per minute
Va
amount of air entering alveoli per minute
perfusion (Q with dot)
amount of blood that flows through the lung capillaries each minute
hypoxic conditions
pulmonary blood vessels constrict, forces blood to areas of higher oxygen
ventilation perfusion coupling
matching of pulmonary blood flow to oxygen
if no air enters the lungs, Va/Q zero
blood flows, no gas exchange occurs
air enters lungs, blood does not flow
Va/Q = infinity
pulmonary embolism
internal respiration is a
process that occurs between capillaries and tissues
O2 delivered to tissues
CO2 picked up and carried to lungs for excretion
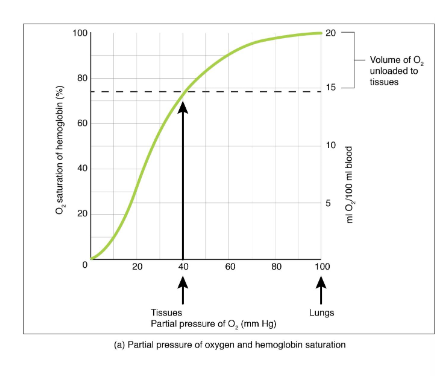
hemoglobin
picks up oxygen where partial pressure is highest
releases oxygen where partial pressure is lowest
Alveolar highest, tissue lowest
carbon dioxide carried as
bicarbonate ions
tissue has highest
alveolar has lowest
O2- hemoglobin saturation curve “O2 stat”
saturation curve: effect of pH
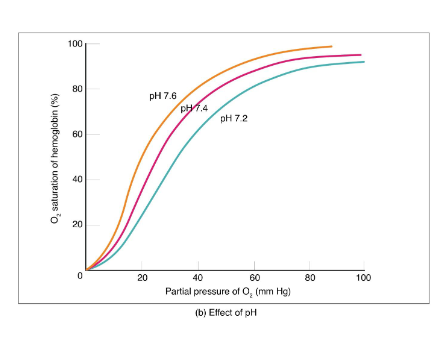
hemoglobin affinity/stickiness of O2 shifts to right
less oxygen bound at lung
more oxygen delivered at tissue
pH lower
P co2 higher
higher temperature
hemoglobin affinity curve shift to left
more O2 bound at lung
less O2 delivered at tissues
pH higher
P co2 lower
lower temperature
effect of pregnancy
fetal hemoglobin has a higher affinity for oxygen than maternal hemoglobin
carbon dioxide transport
70% carried as bicarbonate ion
23% carried in hemoglobin
7% dissolved in plasma
buffer
acts as a H+ and/or OH– “sponge” so that pH is kept relatively constant
carbonic acid - bicarbonate buffer system
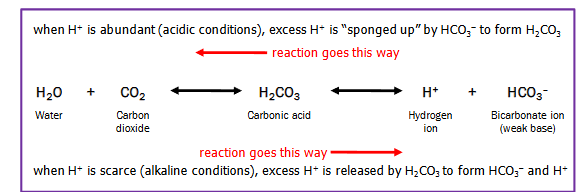
too acidic?
pushes reaction left
more CO2 is made
too alkaline?
pushes reaction to the right
more H+ and HCO3- are produced
inspiratory center/dorsal respiratory group
active in tidal breathing
stimulates phrenic and intercostal nerves
expiratory center/ventral respiratory group
only activated consciously or with exercise
abdominal muscle contract
forced exhalation
pneumotaxic center
part of pons
limits duration of inspiration, prevents lungs from getting too full
apneustic center
part of pons
coordinates transition from inhale to exhale
tachypnea
rapid breathing
hyperventilation
excessive ventilation
low blood CO2, high blood pH, alkalosis
apnea
temporary halt in ventillation
hypoventilation
decreased ventilation, high blood CO2, low blood pH, acidosis
acidosis increases
respiratory rate, “blowing off” CO2
alkalosis decreases
respiratory rate, retain CO2, increase H+
earliest viable premature babies are
about 23 weeks gestation
surfactants
reduce surface tension in water and break hydrogen bonds
secreted by type II alveolar cells
surfactant production appears at about
20 weeks gestation
lungs begin to develop at
fourth week of pregnancy