Cardiovascular System (Heart Valves) Part 2
1/63
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
64 Terms
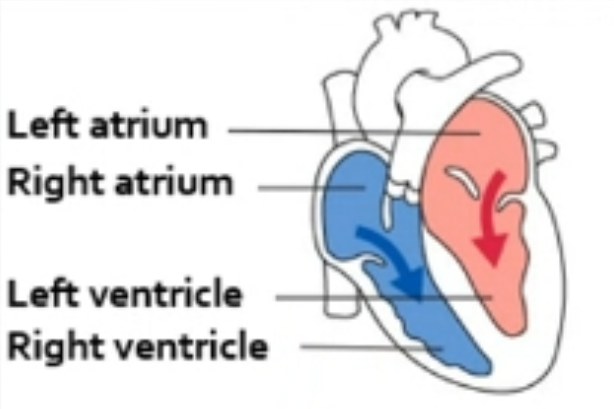
Atrioventricular (AV) Valves
To allow blood to flow in only one direction (from atria to ventricles) and prevent backflow.
Between the atria and ventricles
Where are the atrioventricular (AV) valves located?
Tricuspid valve
What is the other name for the RIGHT atrioventricular (AV) valve?
Bicuspid valve (Mitral valve)
What are the other names for the LEFT atrioventricular (AV) valve?
Phase 1: AV Valve Opening (Filling)
Operation of the AV Valves
Blood returns to atria, pressure forces AV valves open.
Phase 2: Ventricular Filling
Operation of the AV Valves
AV valve cusps hang limply into ventricles as they fill.
Phase 3: Atrial Contraction (Systole)
Operation of the AV Valves
Atria contract, pushing additional blood into ventricles. AV valves open (Atrial P > Ventricular P).
Phase 4: Ventricular Contraction (Systole)
Operation of the AV Valves
Ventricles contract, forcing blood against AV valve cusps. AV valves close.
Phase 5: AV Valve Closure Condition
Operation of the AV Valves
AV valves closed; Ventricular P > Atrial P.
Phase 6: Function of Chordae Tendineae
Operation of the AV Valves
Tighten during contraction to prevent valve cusps from everting (flipping backward) into atria.
No. The myocardium (heart muscle) has its own separate circulation system.
Does blood in the heart chambers nourish the myocardium?
Coronary arteries, Cardiac veins, Coronary sinus
What are the components of the heart’s independent nourishing circulatory system
Coronary arteries
Supply oxygenated blood to the heart muscle.
Cardiac veins
Drain deoxygenated blood from the myocardium.
Coronary sinus
Large vein that receives blood from cardiac veins
They branch directly from the aorta.
Where do coronary arteries originate?
Coronary arteries, Aorta
The _____ branch from the _____ to supply the heart muscle with oxygenated blood.
Right Atrium
The coronary sinus is a large vein on the posterior of the heart that receives blood from cardiac veins and empties into the?
Intrinsic conduction system (nodal system)
To generate and distribute electrical impulses that coordinate the contraction of the heart muscle.
Sets the rhythm of the heart and ensures depolarization in one direction only (atria to ventricles)
Spontaneously and independently of nerve impulses (automaticity)
How do cardiac muscles contract in relation to nerve impulses?
The Sinoatrial (SA) node
What is the name of the "pacemaker" of the heart?
This starts each heartbeat.
60–100 beats per minute
Atrial cells beat approximately ___ times per minute independently.
25–55 beats per minute (AV Node/Purkinje fiber rate)
Ventricular cells beat approximately ___ times per minute independently.
Autonomic nervous system (extrinsic) an dIntrinsic conduction system (nodal system)
What are the two main systems that regulate heart activity?
Special nervous tissue (specialized cardiac muscle cells)
The intrinsic conduction system is composed of what type of tissue?
75 beats per minute
What heart rate does the intrinsic conduction system enforce on its own?
Ensures depolarization proceeds in one direction only: Atria to Ventricles.
How does the intrinsic conduction system ensure heart muscle contraction is efficient?
The atria contract (Atrial systole)
What happens immediately after the impulse spreads from the SA node through the atria?
AV node
Where is the electrical impulse briefly delayed.
This delay allows the atria to finish contracting and empty blood into the ventricles before they squeeze.
AV bundle, Bundle branches, Purkinje fibers.
After the AV node delay, what is the path of the impulse to the ventricles?
Tachycardia
A resting heart rate exceeding 100 beats per minute.
Cardiac Cycle
One complete heartbeat, where both atria and ventricles contract (systole) and then relax (diastole).
Systole (Cardiac Cycle)
Contraction phase (heart muscle contracts to pump blood).
Diastole (Cardiac Cycle)
Relaxation phase (heart muscle relaxes to fill with blood).
75 beats per minute
What is the average adult resting heart rate?
0.8 seconds
What is the normal length of one cardiac cycle (at a heart rate of 75 bpm)?
Atrial diastole (ventricular filling)
Heart is relaxed
Pressure in heart is low
Atrioventricular valves are open
Blood flows passively into the atria and into ventricles
Semilunar valves are closed
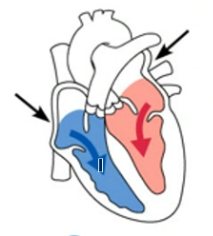
Atrial systole
Ventricles remain in diastole
Atria contract
Blood is forced into the ventricles to complete ventricular filling
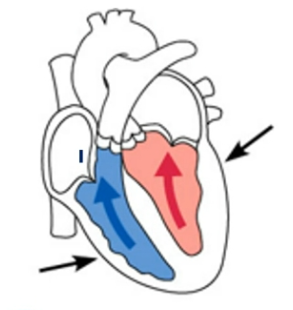
Isolovumetric Contraction
Atrial systole ends; ventricular systole begins
Intraventricular pressure rises
AV valves close
For a moment, the ventricles are completely closed chambers
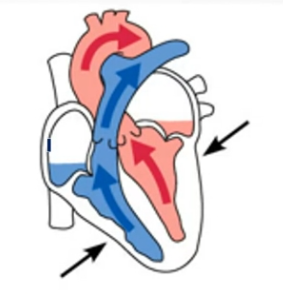
Ventricular Systole (Ejection Phase)
Ventricles continue to contract
Intraventricular pressure now surpasses the pressure in the major arteries leaving the heart
Semilunar valves open
Blood is ejected from the ventricles
Atria are relaxed and filling with blood
Isovolometric Contraction
Ventricular diastole begins
Pressure falls below that in the major arteries
Semilunar valves close
For another moment, the ventricles are completely closed chambers
When atrial pressure increases above intraventricular pressure, the AV valves open
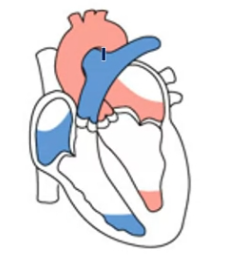
Heart Sound: "Lub" (S1)
Longer, louder heart sound.
Caused by closing of the AV (Atrioventricular) valves.
Timing: Start of ventricular systole.
Heart Sound: "Dup" (S2)
Short, sharp heart sound.
Caused by closing of the semilunar valves.
Timing: End of ventricular systole / Beginning of diastole.
Cardiac Output (CO)
The volume of blood pumped by each ventricle (side) of the heart in 1 minute.
Total blood pumped in 1 minute.
Stroke Volume (SV)
The volume of blood pumped by each ventricle in one contraction (per heartbeat).
Blood pumped in 1 heartbeat.
70 ml
What is the average Stroke Volume (SV) per heartbeat in the left ventricle?
Heart Rate (HR) x Stroke Volume (SV)
Formula for Cardiac Output (CO)?
Starling’s Law of the Heart
The law stating that the heart's stroke volume increases in response to an increase in the volume of blood filling the ventricles (preload).
Stretch of the Cardiac Muscle
What is the critical factor controlling Stroke Volume?
Venous return
What is the primary factor influencing the stretch of heart muscle?
Neural (ANS) Controls, Hormones and Ions
What are the two main types of factors that modify the basic heart rate?
Speeds up heart rate
How does the Sympathetic Nervous System affect heart rate?
Slows and steadies heart rate
How does the Parasympathetic Nervous System (specifically the vagus nerve) affect heart rate?
Epinephrine and thyroxine
Which hormones speed up heart rate?
Calcium (Ca2+), Sodium (Na+), and Potassium (K+)
Which ions modify heart activity?
Tunica intima (Inner), Tunica media (Middle), Tunica externa/adventitia (Outer)
What are the three layers (tunics) of blood vessels (excluding capillaries), from inside to outside?
Tunica Intima
It forms a friction-reducing lining (endothelium) for blood flow.
Tunica Media
Structure: Smooth muscle and elastic tissue.
Control: Controlled by the sympathetic nervous system (for vasoconstriction/dilation).
Tunica Externa (or Adventitia)
Function: Forms the protective outermost covering, supporting and anchoring the vessel.
Composition: Mostly fibrous connective tissue.
Capillaries
Which type of blood vessel consists only of a single tunica intima layer?
Arteries
Have a heavier/stronger tunica media than veins.
Heavier, stronger, stretchier tunica media; high pressure.
Smaller Lumen
Veins
Thinner tunica media; low pressure; possess valves to prevent backflow.
Larger Lumen
Valves
Structural feature of veins that prevents backflow of blood.
Skeletal muscle "milking" (contraction)
What mechanism helps move blood through veins back toward the heart?