Burns
1/212
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
213 Terms
What are the 3 layers of the skin?
1. dermis
2. epidermis
3. subcutaneous
What are the functions of the skin? (there's a mnemonic)
- Sensation
- Heat regulation
- Absorption
- Protection
- Excretion
- Secretion
- vitamin D production
What temperature does cell damage occur in thermal burns?
>45°C (113°F)
What are the 3 zones of damage?
1. zone of coagulation
2. zone of stasis
3. zone of hyperemia
What is the zone of coagulation?
irreversible damage by thrombosis of blood vessels
What is the zone of stasis?
stagnation of microcirculation
What is the zone of hyperemia?
increase in circulation
How many patients per year seek treatment for burn injuries?
400,000
How many burn patients per year require specialized care?
40,000
How many burn-related deaths occur per year?
3,500
What % of fire-related deaths are due to inhalation injuries?
60-80%
What % of burns occur in the home?
70-75%
Who are at biggest risk for thermal burns?
extremes of ages (young children and older adults)
What part of the skin does 1st degree burn thermal involve?
epidermis only

What is the tissue appearance in a 1st degree thermal burn?
red, painful, tender "sunburn" appearance, without blisters

What is an example of a typical 1st degree thermal burn?
sunburn

What is the treatment for 1st degree thermal burns?
really nothing, heals within 7-14 days without scarring
What layers do superficial partial thickness 2nd degree thermal burns affect?
epidermis and into but not through dermis
What is the appearance of superficial partial thickness 2nd degree thermal burns?
blisters, exposed dermis is red/moist; very painful
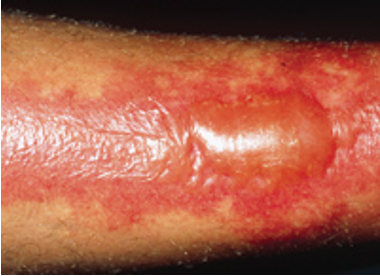
What is the treatment for superficial partial thickness 2nd degree thermal burns?
14-11 days to heal, with minimal scarring
What type of damage to 3rd degree thermal burns cause?
full thickness; damage to dermis and epidermis and adnexal structures
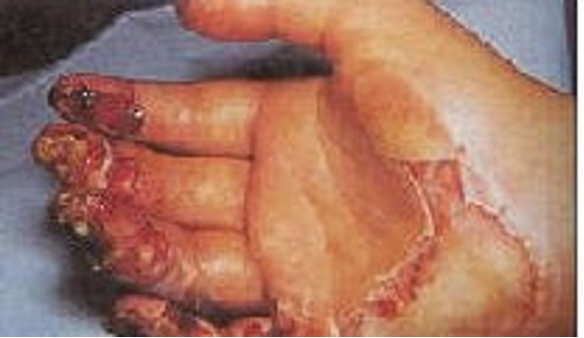
True or False: the more severe the thermal burn, the less pain?
true, starting around 3rd degree burns they may not think it's too serious because of lack of pain
true or false: you can only have one type of thermal burn?
false; you can have 3rd degree in one area (no pain), and 1st or 2nd in another (with pain)
How is a 3rd degree thermal burn described?
waxy white to charred black in appearance, again painless
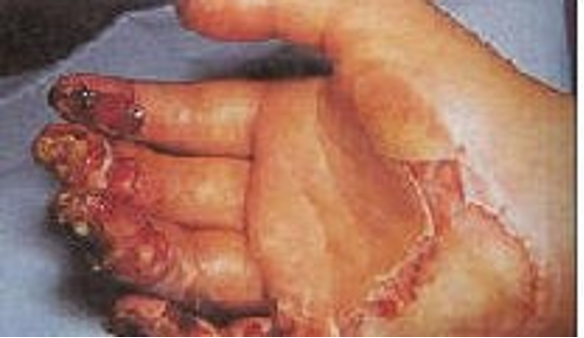
What is the treatment of a 3rd degree thermal burn?
surgical repair; skin grafitng
What must be done to calculate fluid replacement in thermal burns, when considering the extent?
determine total body surface area (TBSA)
What are the ways we can determine TBSA?
- palmar rule
- rule of nines
- lund and browder chart
What is the palmar rule?
patient's palm is 1% of body SA, so good for quick asessment of small body SA
What is the rule of nines?
also a quick assessment; division of body SA in multiples of 9, risk of overestimation though, which can lead to fluid overload (congestion problems, etc)
What is the Lund and Browder chart?
standardized age-based assessment, usually for patients who need long-term hospital care or burn center care
How does the rule of nines work in children?
over the age of 1, for each year above one, add 0.5% to each leg and subtract 1% for the head; this formula should be used until the adult rule of nine values are reached
What is the initial management of thermal burns?
- stop the burning process
- immediate life saving measures: ABCs
True or False: With really deep thermal burns, the burning can continue injuring tissue until treatment is started
true
What are we looking at for the history to help with initial thermal burn management?
mechanism of injury, PMHx, allergies, tetanus status, comorbidties
In initial thermal burn management, what are we looking for in the examination?
estimate the extent/depth of injury, assess for associated injuries
In intial thermal burn management what are the steps we're following in the ER?
- airway
- check ABG
- check carboxyhemoglobin level
- chest radiograph
- establish IV access
- watch UO
- NG tube
- moist saline dressing
- IV narctocis
- admit or transfer to brun unit as indicated
When should we be cautious using narcotics?
head injury or hypoxia
What labs/imaging are we running during inital thermal burn management?
CBC, CMP, T&C, UA, and ECG
What do we do for wound management in thermal burns?
- analgesics
- clean burn with mild soap and water (pretty much most painful part)
- Debride wound as needed
- chemoprophylaxis (usually antibiotic)
- sterile dressing with daily dressing changes (usually needed in everything after 2nd degree superficial)
What chemoprophylaxis can be used in 1st degree thermal burns?
possible bacitracin cream
What chemoprophylaxis can be used in 2nd degree superficial thermal burns?
bacitracin cream
What chemoprophylaxis can be used in 2nd degree deep thermal burns?
- silver sulfadiazine cream
- mafenide acetate cream
- bacitracin cream
What chemoprophylaxis can be used in 3rd degree thermal burns?
- silver sulfadiazine cream
- mafenide acetate cream
- bacitracin cream
What chemoprophylaxis can be used in 4th degree thermal burns?
- silver sulfadiazine cream
- mafenide acetate cream
- bacitracin cream
- possible voriconazole cream
- possible systemic antibiotics
What is secondary management for thermal burns?
- infection prevention
- pain management
- wound healing
- metabolic support
- psychologic support
- manage complications
What do we do if a thermal burn patient starts to exhibit rapid metabolism or tachycardia
manage with propranolol
What is the clincal presentation of inhalaltion burns?
- hx of exposure to a fire in an enclosed space
- facial burns
- singed nasal hair
- soot in mouth/nose
- carbonaceous sputum
- hoarseness
- dyspnea
- expiratory wheezing
- stridor
How many products are capable of causing a chemical burn?
25,000 products
What body sites are most frequnetly affected by chemical burns?
face, eyes, extremities
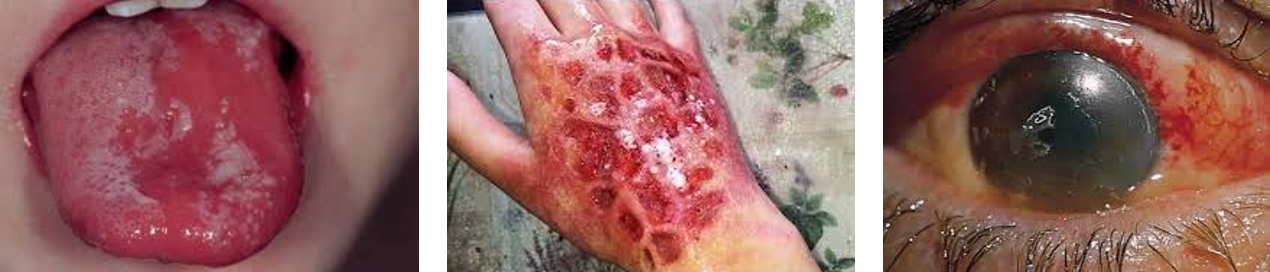
What the 2 classifications of chemical burns?
separated by chemical activity
acid: pH <2.0
base: pH >12.0
What can acid-related chemical burns cause?
coagulation necrosis, superficial tissue burns
What can base-related chemical burns cause?
liquefaction necrosis; deeper, more extensive tissue damage
Why can base-related chemical burns cause more damage?
the base will degrade fats, lipids, and proteins
How do we classify chemical burns?
- chemical activity (pH)
- strength of agent
- concentration (like %?)
- duration (how long on skin?)
- quantity (amount?)
How are ocular chemical burns managed?
- irrigate
- remove contacts
- check pH, continue to irrigate until normal pH is restored
- check acuity
- consult opthalmology
For ocular injuries from chemical burns, what is the irrigation process?
minimum of IL NS for a minimum of 20-30 minutes continous irrigation
What are the two things that can cause electrical burns?
1. alternating current (AC)
2. direct current (AC)
Where is alternating current found?
household electricity
Where is direct current found?
industrial injuries, batteries, lightning
How are the entrance and exit wounds in AC electrical burns?
entrance wounds and exit wounds around the same size because of the alternating
How are the entrance and exit wounds in DC electrical burns?
small entrance wound, large exit wound because the energy builds before leaving, causing more damage
What is the management for electrical burns?
- ABCs (assume spinal injury)
- trauma protocol
- fluid resuscitation
- EKG and cardiac monitoring for 24 hrs
- thorough examination
- asses for posterior shoulder dislocation and other associated injuries
- consider referal to burn center
What labs should be done in cases of electrical burns?
CBC, BMP, UA, urine myoglobin, CK, cardiac enzymes
What are other considerations for electrical burn management?
Td status, antibiotics, and wound management (case by case) if large, open wound, seizure prevention
What is a "flashover"?
high-voltage electric short circuit made through the air between exposed conductors
How can heat loss occur?
- conduction
- convection
- radiation
- evaporation
What is conduction?
heat is directly transmitted when there's a change of temperature (ex. going from inside warmth to outside cold)
What is convection?
movement of particles causing heat particles to rise and be released into the environment (ex. boiling water)
What is radiation?
admission of heat through electromagnetic waves
What is evaporation?
heat loss from the conversion of water to gas
How can heat be gained or conserved?
- shivering
- thyroid mediated increase in metabolic rates
- peripheral vasoconstriction
- behavioral response
What controls heat gain/conservation?
controlled by the hypothalamus
What are the causes of hypothermia?
expsoure to cold or impaired heat production or both
What are the specific reasons for hypothermia?
- accidental environmental exposure
- metabolic disorders
- hypothalamic/CNS dysfunction
- drugs
- sepsis (body can't maintain heat)
- dermal disease
- acute incapacitating illness
- massive fluid/blood resuscitation (fluid is colder than body temp)
What is the clinical presentation of mild hypothermia?
- tachycardia/tachypnea
- HTN
- shivering
- impaired coordination
- poor judgement
- apathy
- pale, cold, numb skin
- dysarthria
What is the clinical presentation of moderate hypothermia?
- shivering stops
- bradycardia
- dilated pupils
- slow/absent DTR
- cold diuresis
- loss of volunatry muscle control
- confusion
- lethargy
- LOC
True or False: we have to get the patient to a core body temp, before declaring them deceased?
true
What is the clinical presentation of severe hypothermia?
- complete cessation of shivering
- rigid muscles
- severe hypotension or undetectable BP
- fixed/dilated pupils
- absent pulses and respirations
- coma
What cardiac dysfunction can hypothermia cause?
- sinus bradycardia to slow A.fib (not typical presentation) to V. fib to asystole
- increased cardiac muscle irritability
What ECG changes occur in hypothermia?
- prolonged p wave, QRS duration
- T wave inversion
- muscle tremor inversion
- osborne (j wave)
What is an Osborne (j wave)?
delayed ventricular depolarization and early depolarization
True or False: if we're seeing bunny ears, that's always a LBBB
false; if the patient has hypothermia and is shivering like crazy, more likely an osborne (j wave)
What is the evaluation and management of hypothermia?
- history
- PE
- labs: BMP, ABG, ECG
- ABC
- IV access and volume resuscitation
- rewarm
What are the methods of rewarming for mild hypothermia?
passive or active external warming
What are the passive rewarming methods for mild hypothermia?
- transport from cold
- adequate shelter/heat
- remove wet garments
- layer clothes/blankets
- warm, sweet beverage
What are the active external rewarming methods for mild hypothermia?
- heated blankets
- warm bedding/blankets
- warm packs to trunk
- immersion into a 40°C bath
What temperatures does frostbite occur?
-20°C (-4°F), with wind increasing risk
Who are the high-risk groups of frostbite?
- military
- outdoor workers
- elderly
- homeless
- drug/ETOH
- psych
What are the symptoms of 1st degree frostbite?
numbness, erythema, welling, dysesthesia, white plaques, no loss of tissue
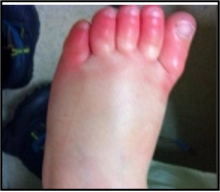
What are the symptoms of 2nd degree frostbite?
edema, erythema, blister formation within 6-12 hours
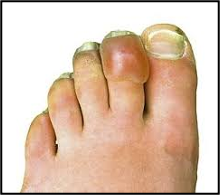
What is there a risk of anytime there's blisters?
secondary infection
What are the symptoms of 3rd degree frostbite?
tissue loss involving the entire thickness of skin, hemorrhagic blisters, blue-gray discoloration, "block of wood" then burning throbbing pain
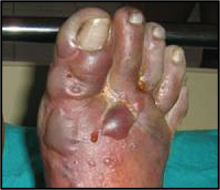
What are the symptoms of 4th degree frostbite?
freezing of subcutaneous tissue, muscle, bone, tendon, little edema, skin is mottled with non-blanching cyanosis forming deep, dry black mumified eschar
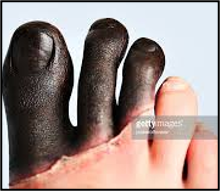
True or false: putting on two layers of socks and shoving them inside boots helps avoid frostbite?
false; because of the vasoconstricitve effect it actually cause increased risk
What is the prognosis of 1st degree frostbite?
excellent
What is the prognosis of 2nd degree frostbite?
good
What is the prognosis of 3rd degree frostbite?
poor
What is the prognosis of 4th degree frostbite?
poor
What is hyperthermia?
elevation of core body temperature above the normal diurnal range of 36 to 37.5°C due to failure of thermoregulation
What is the main cause of hyperthermia?
imbalance between metabolic heat production/environmental heat load and normal heat capacity/loss heating