L17. Bone and Soft Tissue Pathology II
1/60
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
61 Terms
Paget's disease
Excessive bone resorption followed by abnormal bone formation
Paget's disease is also known as
osteitis deformans
True / False: Paget's disease has unknown etiology
true - genetics, virus, disease of osteoclasts
Paget's disease is --- or ---
mono or polyotic
majority are polystotic
What bone is commonly affected in Paget's disease?
Skull
Patient's with Paget's disease have a significantly higher risk of developing ----
osteosarcoma
In Paget's disease bone looks like af5 ---
jigsaw puzzle
Compound fracture
bone breaks through the skin
Comminuted bone fracture
bone fragments into many pieces
Greenstick fractures
usually seen in kids
bone breaks on one side and bends on the other
Displaced fracture
bone ends are out of normal alignment
Fracture Healing
Hematoma formation and inflammation = first week
Soft callus (2-3 weeks)
Hard callus (2-4 months)
Remodeling (several months to years)
Osteonecrosis presents as increased --- on radiographs
radio-opacity
What is the outcome of osteonecrosis?
removal of dead bone and formation of new bone
OR
bone collapse
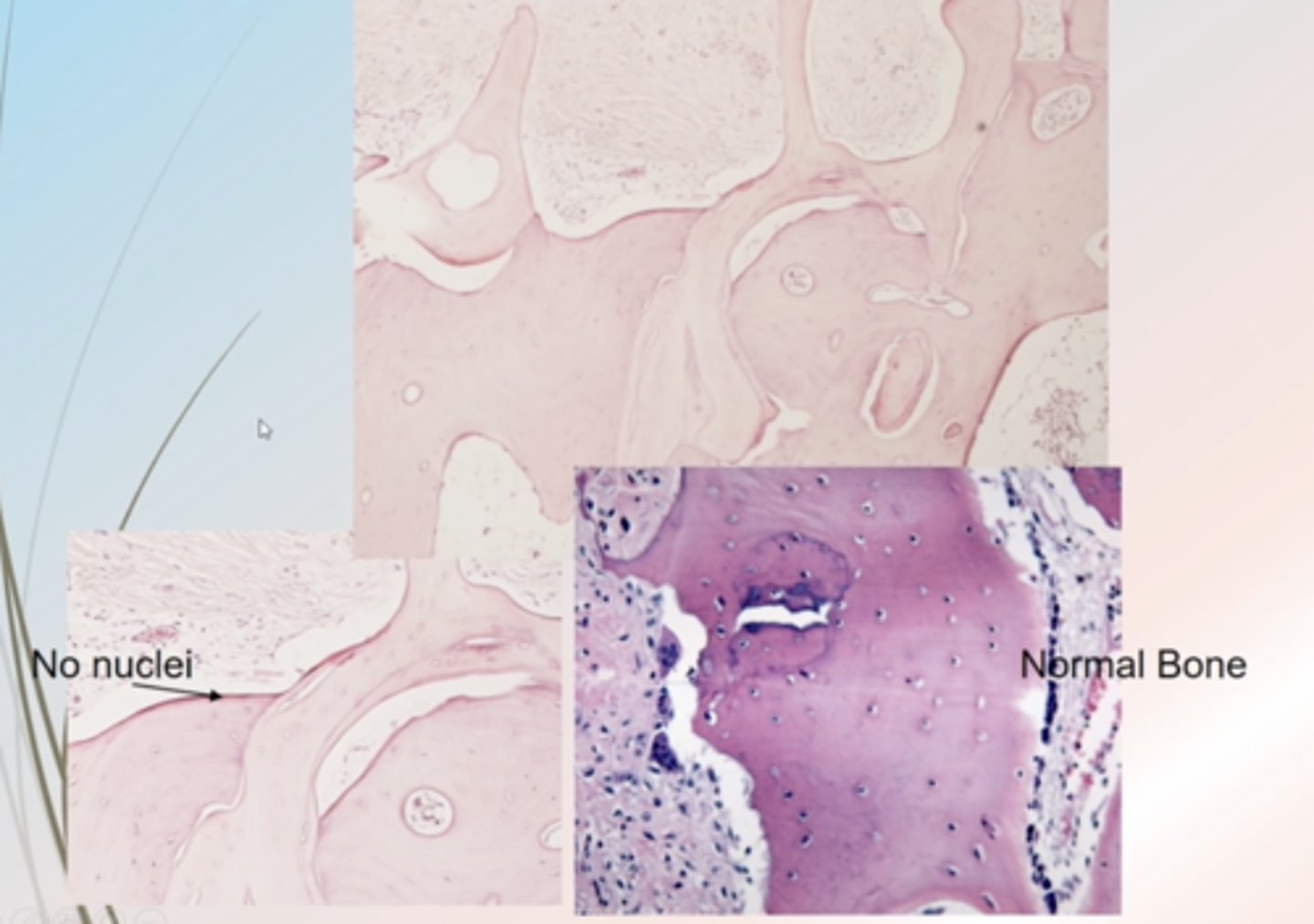
What is present on an H and E in osteonecrosis?
No nuclei
No osteoblasts or osteoclasts
Why is cartilage difficult to heal?
It is avascular so difficult to regenerate
Osteomyelitis
infection of the bone and bone marrow
What is the most common cause of osteomyelitis?
staph aureus
Children can be diagnosed with osteomyelitis secondary to ---
hematogenous spread (spread though blood)
Adults can be diagnosed with osteomyelitis secondary to ---
open bone fracture
What is the most common cause of osteomyelitis in patients with sickle cell anemia?
salmonella
What is needed for diagnosis of osteomyelitis?
bone biopsy / culture and blood culture
True / False: patients with osteomyelitis are typically extremely sick (fever, malaise, elevated ESR)
true
True / False: in reference to osteomyelitis, radiographic changes can be minimal or radiolucency with rim of sceloris
true
Chronic osteomyelitis symptoms include low grade fevers, inflammation persists for months to years with presence of --- and ---
necrotic bone and fistulous tract
What are the most common causes of chronic osteomyelitis?
Diabetes
Peripheral vascular disease
Types of joints
synovial
non-synovial
Non-synovial joints
Fibrous
- tooth socket = gomphosis
Cartilaginous
- intervertebral discs and pubic symphysis
What is the function of synovial fluid?
allows articulating surfaces of bones to glide upon each other
Articular cartilage is a specific type of --- that covers the ends of bones in joints and provides a smooth surface for movement
hyaline cartilage
Synovial lining is filled with --- (phagocytes) and --- (fibroblasts)
synoviocytes A = phagocytes
synoviocytes B = fibroblasts
Synoviocytes secrete ---
hyaluronic acid
Synovial membrane is surrounded by a ---
fibrous capsule
True / False: hyaline cartilage is vascularized
false = avascular
True / False: hyaline cartilage lacks blood vessels, lymphatics, and nerves. It is made of water, hyaluronic acid, proteoglycans, and collagen type II
true
Degenerative joint disease is also referred to as ---
osteoarthritis
Osteoarthritis
inflammation and and degeneration of joints
results in overuse and wear of the bones
Osteoarthritis is an --- disease
over-use
inflation and degeneration of joints resulting in the interaction of articulating surfaces with one another
Rheumatoid arthritis
systemic auto-immune disorder
inflammation of synovial joints
Who is more prone to rheumatoid arthritis?
Females > males
30 - 50 years old
Rheumatoid arthritis has ---- meaning it effects blood vessels, lungs, heart, and skin
extra-articular effects
What is the genetic factor increase for rheumatoid arthritis?
HLA II + environment
Inflammatory cytokines
IL-1, IL-6, TNF-alpha
What is the term for inflammatory cells in rheumatoid arthritis?
pannus
What is the difference in systems affected in osteoarthritis versus rheumatoid arthritis?
OA: affects weight bearing joints
RA: affects small joints
Rheumatoid arthritis is a --- arthritis affecting small joints of the hands and feet = metacarpal phalanges (MCP) and proximal inter carpal phalanges (PIP)
symmetric
What is the key feature of rheumatoid arthritis progression?
Pannus = thickened abnormal soft tissue mass in joint space
- inflammatory cells, lymphocytes, plasma cells, macrophages, dendritic cells
True / False: angiogenesis contributes to all bone diseases
true
What is the end result of rheumatoid arthritis?
fibrous and bony ankylosis
What is the clinical course of rheumatoid arthritis?
chronic with acute exacerbations
Treatment for rheumatoid arthritis?
NSAIDS
COX-2 inhibitors
TNF antagonists
methotrexate
Lesion created by rheumatoid arthritis
rheumatic nodulus
Septic arthritis
hematogenous spread of infection to synovial joints
Gout
uric acid crystal deposition in joints and soft tissues
type of arthritis
Pseudogout
calcium pyrophosphate crystal deposition in joints and soft tissues
Main lesions created by gout
tophus at tendons and ligaments
Gout have --- shaped crystals that are --- for birefringence
needle shaped crystals
negative for birefringence
Pseudogout have --- shaped crystals that are --- for birefringence
rhomboid shaped crystals
postive for birefrigence
Which has chalky deposits: gout or pseudo gout
pseudogout
TRue / False: pseudo gout may be confused with differential diagnoses of osteoarthritis, gout, and mycobacterial infections due to granulomatous histological presentation
true