MLS 334 Exam 4
1/168
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
169 Terms
Antibiotics
are medications used to treat bacterial infections by inhibiting the growth or destroying bacteria. They are ineffective against viral infections.
Bacteriostatic
drugs that stop bacterial reproduction
(ex: erythromycin)
Bactericidal
drugs that kill bacteria
(ex: penicillin)
Antimicrobial Agent
a chemical compound that kills or inhibits the growth of microorganisms
(ex: antibiotic, antifungal, etc.)
Antibiotic
-class of drugs that target bacterial infections
-can be natural, semisynthetic, or synthetic molecules that can treat or prevent disease
Intrinisic Resistance
natural-occurring resistance to antibiotics - found in chromosomes of bacteria
(ex: biofilms)
Acquired Resistance
Acquired from exogenous DNA (plasmid or through conjugation)
(ex: mutation)
enzymatic inactivation (b-lactamases)
Broad Spectrum Antibiotic
antibiotic that targets multiple types of bacteria
(ex: penicillin)
Narrow Spectrum Antibiotic
antibiotic that targets only a few bacteria
(ex: vancomyocin)
decrease likelihood of organism acquiring resistance
Targets of Antibiotics
cell wall
metabolic functions (basic metabolic functions - protein synthesis, nucleic acid synthesis, metabolism)
Which antibiotics target the cell wall?
b-lactams
penicillin
cephalosporins
vancomycin
Which antibiotics target the cell membrane?
Polymyxins
Whch antibiotics interfere with DNA synthesis?
nalidixic acid
fluroquinolones
Which antibiotics target protein synthesis through RNA polymerase?
rifampin
aminoglcosides
macrolides
B-Lactam Antibiotic - Target
cell-wall
bind penicillin binding proteins and inhibit synthesis of peptidoglycan layer in bacterial cell wall
B-Lactam Antibiotic - Mechanism
bind penicillin binding proteins and inhibit synthesis of peptidoglycan layer in bacterial cell wall
B-Lactam Antibiotic - Species Targeted
aerobic and anaerobic gram positive and gram negative organisms (broad)
Examples of B-lactam Antibiotics
Examples: "PCCM" Narrow to broad spectrum
Penicillin = The "OG" > used for Strep pyogenes and Syphilis
Cephalosporins
Carbapenems = Broad champions but handle with care
Monobactams = One goal, gram negatives only
Glycopeptide Antibiotics - Target
cell-wall
bind to peptidoglycan precursor and inhibit peptidoglycan synthesis
Glycopeptide Antibiotics - Mechanism
bind to peptidoglycan precursor and inhibit peptidoglycan synthesis
Glycopeptide Antibiotics - Species Targeted
gram-positive organisms
Glycopeptide Antibiotics - Example
Vancomycin - Last line Drugs - Use Wisely
Polymyxin Antibiotics - Target
cell membrane
bind outer cell membrane and increase permeability = bacterial lysis (expand then explode)
Polymyxin Antibiotics - Mechanism
bind outer cell membrane and increase permeability = bacterial lysis (expand then explode)
Polymyxin Antibiotics - Species Targeted
gram-negative organisms
Polymyxin Antibiotics - Example
polymyxin B, polymyxin E
Aminoglycoside Antibiotics - Target
30S ribosomal subunit
inhibit intiation complex -> protein mistranslation = inhibiton of protein synthesis
Aminoglycoside Antiobiotics - Mechanism
inhibit intiation complex -> protein mistranslation = inhibiton of protein synthesis
Aminoglycoside Antiobiotics - Species Targeted
aerobic gram positive and negative organism AND M. tuberculosis
Aminoglycoside Antiobiotics - Example
G = Gentamicin- most common, effective against wide range of gram negatives
N = Neomycin- topically or orally for bowel prep and superficial skin infections
A = Amikacin- "armor plated" against resistance- resistant hospital pathogens
T = Tobramycin- Pseudomonas aeruginosa
S = Streptomycin- historical drug- used primarily for TB, plague and tularemia
Macrolide Antibiotics - Target
50S ribosomal subunit
Macrolide Antibiotics - Mechanism
Protein Synthesis Inhibitor - bind 23S rRNA and inhibit translocation and chain elongation = decreased protein synthesis
Macrolide Antibiotics -Species Targeted
aerobic and anaerobic gram negative and positive organisms
Macrolide Antibiotics - Example
Erythromycin
Azithromycin
Clarithromycin
Fluoroquinolone Antibiotics - Target
DNA gyrase
Inhibit DNA gyrase and topioisomerase IV = inhibition of DNA synthesis
Fluoroquinolone Antibiotics - Mechanism
inhibit DNA gyrase and topioisomerase IV = inhibition of DNA synthesis
Fluoroquinolone Antibiotics - Species Targeted
aerobic gram positve and negative organisms (some anaerobic gram negative)
Fluoroquinolone Antibiotics - Example
Examples: Ciprofloxacin (workhorse for gram negatives), Levofloxacin
F = Fluoroquinolone family-"all roads end with - floxacin"
L = Locks DNA gyrase > prevents unwinding of bacterial DNA
O = Only aerobes (primarily)
X = Crosses tissue walls > Achieves high levels in lungs, urine, bone and prostate
Sulfonamide Antiobiotics - Target
folic acid synthesis
Sulfonamide Antiobiotics - Mechanism
prevent bacterial THF (active form of folic acid) = decreased DNA methylation
Sulfonamide Antiobiotics - Species Targeted
aerobic gram positive and negative organisms
Sulfonamide Antiobiotics - Bacteriocidal or Bacteriostatic
both bactericidal AND bacteriostatic
Sulfonamide Antiobiotics - Example
Examples: Trimethoprim-sulfamethoxazole (Bactrim)
Sulfa starts it- Tri ends it
Used in uncomplicated UTI when local resistance is low (UTI-> Bactrim for 3)
The minimal inhibitory concentration (MIC) is the ______ antibiotic concentration needed to _____ the growth of an organism.
lowest; inhibit
When does antimicrobial suscpetibility testing need to be performed?
Susceptibility Testing
- culture results in isolation of bacteria that is involved in patient infection
-isolate is involved in pt infection and suscpetibility against particular antibiotics is unknown or uncertain
What agency is responsible for providing guidance for AST reporting?
Clinical and Laboratory Standards Insititute (CLSI)
Why should AST not be performed on organisms that are considered normal flora or considered contaminants?
does not provide useful information and may promote unnecessary antibiotic usage
Streptococcus pyogenes is universally susceptible to what antibiotic?
peniciliin
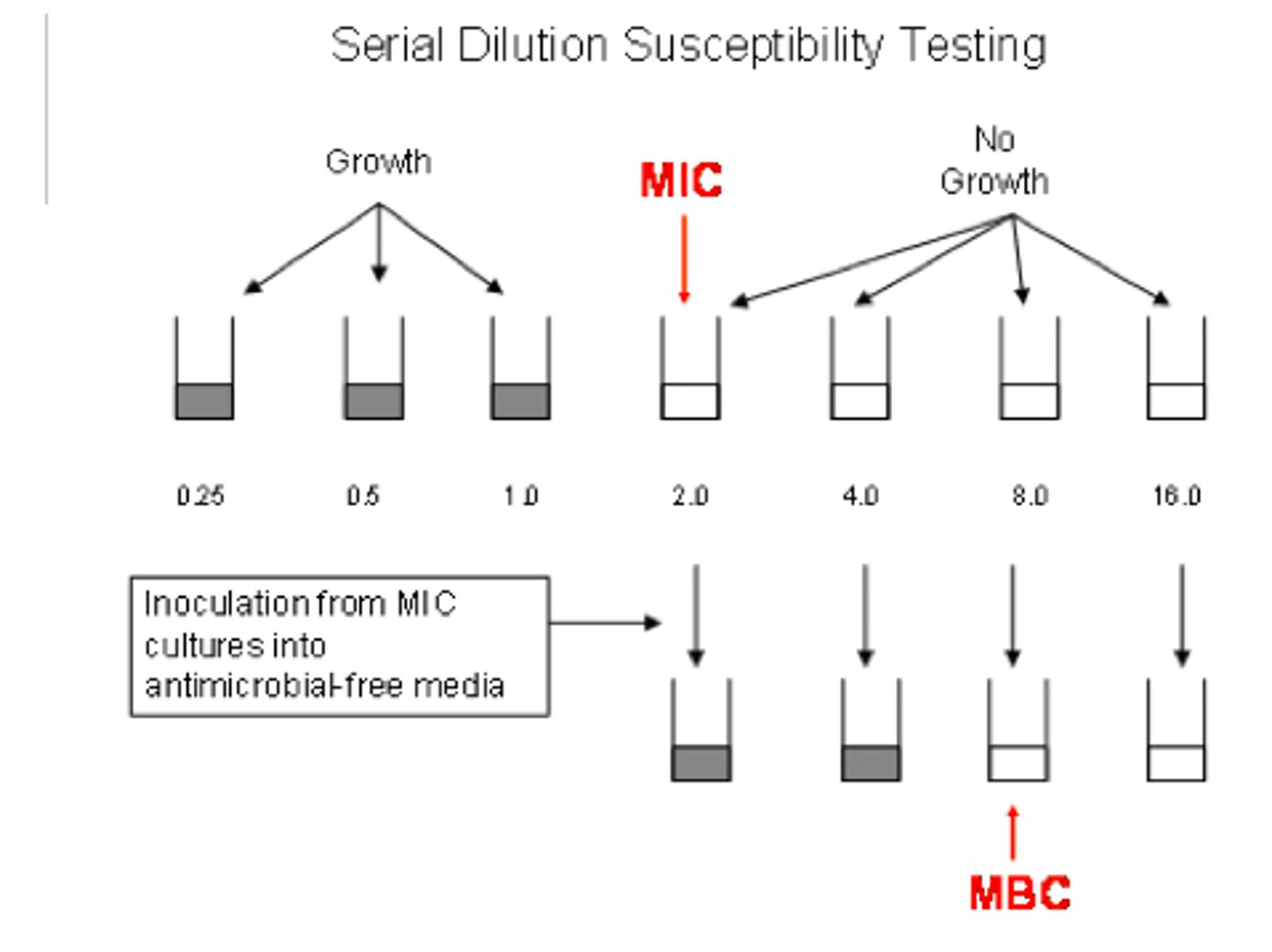
Dilution Susceptibility Testing
-Serially dilute the antibiotic in broth or agar, add a fixed inoculum of bacteria to each concentration
-Bacteria will grow in the tubes up to the drug concentration at which they are inhibited
-interpret as suscpetible, intermediate, or resistant
Dilution Susceptibility Testing - Priniciple
determine the lowest concentraion of antimicrobial required to inhibit growth of bacterial isolate (MIC value)
Antibacterial Resistance
Intrinsic resistance- innate characteristic of organism
Acquired resistance- changes in usual genetic makeup leading to altered cellular
physiology
Mechanisms of resistance
" Lack of affinity of the drug for bacterial target
. Prevent access of drug to relevant site of action
. Biofilms
. Efflux
· Enzymatic inactivation
. Example: B- laotamases
McFarland Standard
A standardized reference solution used to estimate the concentration of bacteria in a culture, allowing for consistent comparisons in antimicrobial susceptibility testing. It typically contains a specific concentration of suspended bacteria, equivalent to a certain optical density.

Disk Diffusion Testing
-disks impregnated with specific drugs are placed on agar plates inoculated with test microbe in 0.5 McFargland Standard
-drug diffuses from disk into agar, establishing concentration gradient
-observe clear zones (no growth = zone of inhibition) around disks and compare to standard table
-reported as susceptible, intermediate, or resistant
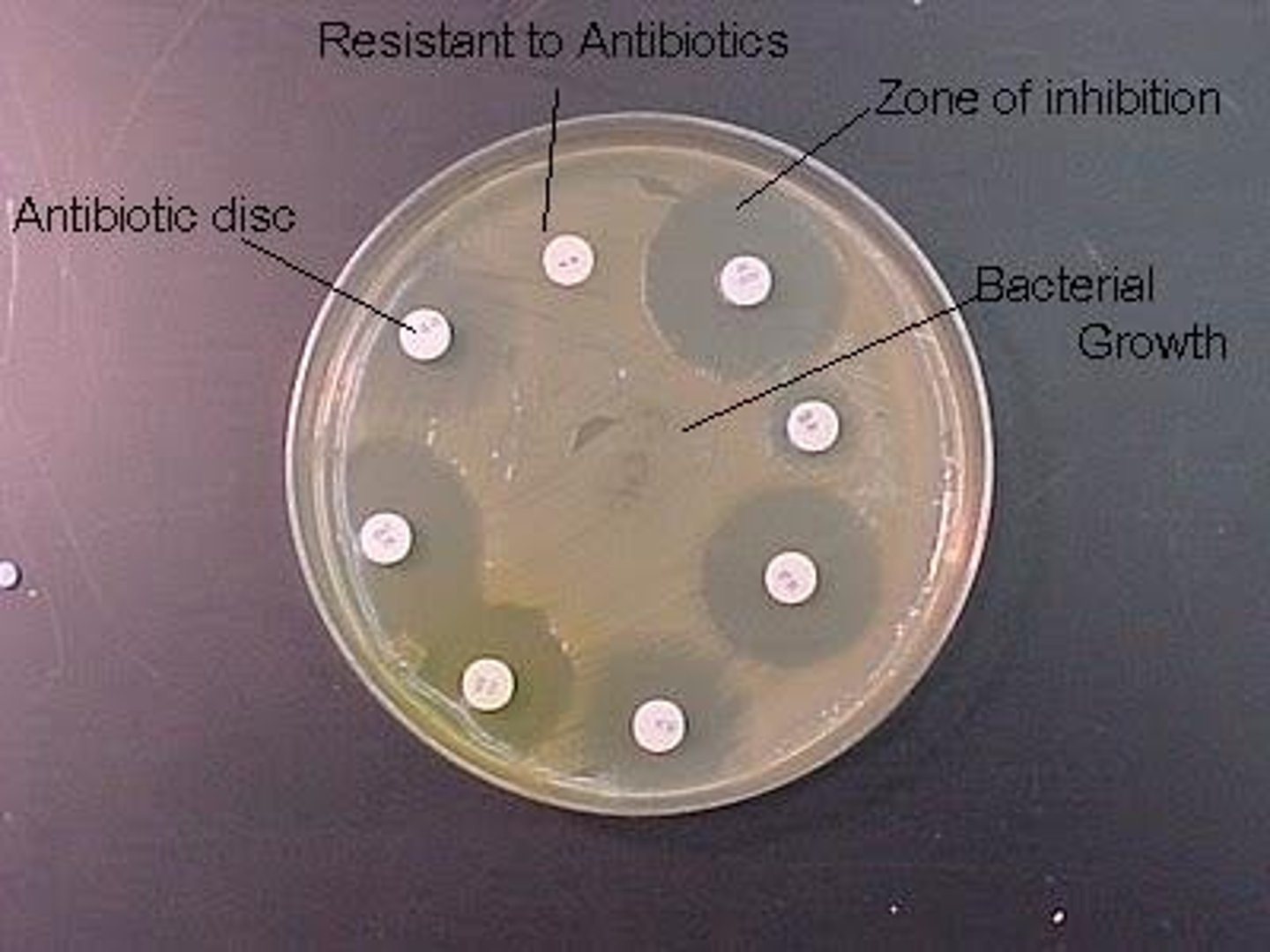
Kirby Bauer Principle
Priniciple of Disk Diffusion Testing
bacteria are placed on a MacFardland plate of solid growth medium and antibiotic disks are added to the plate.
allow the bacteria to grow overnight
areas of clear media surrounding the disks indicate that the antibiotic inhibits bacterial growth
Report result as Resistant (R), Intermediate (I) or Susceptible (S).

Broth-Microdilution Tests
.Good for an occasional antibiotic, not an entire panel
Good for fastidious organisms with high growth requirements
.Use less media and antibiotics
Breakpoint (cutoff)
. Point where effective tissue concentration can be achieved for bacterial inhibition
.Results based on two wells
What is a zone of inhibition?
the area around the antibiotic disk in which bacteria cannot grow (area of no growth)
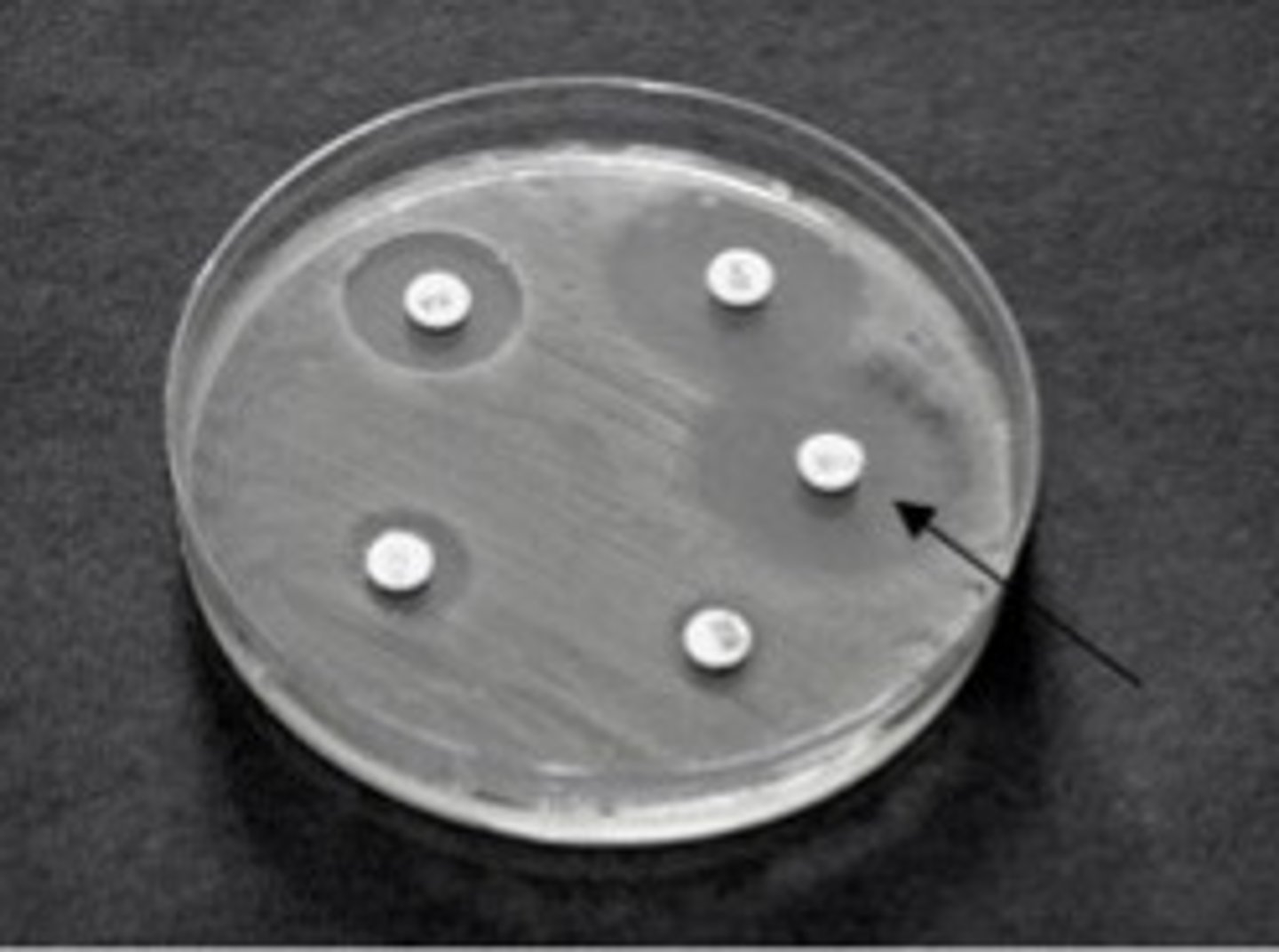
E-test
-Uses strips instead of disks
-strips contain varying concentrations of antibiotic
-Intersection of elliptical zone of inhibition with strip indicates MIC

What is the purpose of infection prevention and control?
reduce dissemination (spread) of infections
Healthcare-associated infection (HAI)
an infection the patient acquires while recieving treatment for medical/surgical issues
>48 hrs after med tx
<30 days surgery
Examples of HAIs
-catheter associated urinary tract infection (CAUTI)
-central line associated bloodstream infection (CLABI)
-ventilator associated pneumonia (VAP)
-surgical site infection (SSI)
- clostridium difficle (C. diff) common in patients with multiple Abx
Surveillance
ongoing, systematic collection, analysis, interpretation and dissemination of data regarding a health-related event for use in public health action to reduce morbidity and mortality and to improve health (CDC)
Causes of HAIs
-instrumentation
-increased use of antimicrobial agents
-lack/failure of aspetic technique
-healthcare not just in hospitals (changing landscape)
Total Surveillance
All infections recorded, analyzed and assessed
Infection Rate
Analysis of the speed of spread or frequency of an infectious disease within a population
(can compare to other facilities)
Targeted Surveillance
focus on specific, high-risk, high-volume procedures
Baseline Data
Historical occurrence of infections over time
Outbreak
Upward trend of infections above baseline data
Index Case
first case in an outbreak
Incidence
# new HAIs during month / # patient days durng month
Prevalence
# of active HAIs / # of pts in hospital
Standardized Infection Ratio (SIR)
actual # infection / predicted # infections
Charecteristics of a Virus
Obligate intracellular parasites
microscopic "parasites" that lack the ability to live and reproduce outside a host
much smaller than bacteria
known for widespread diseases and outbreaks
Steps of an Outbreak Investigation
1. Verify the diagnosis and confirm the outbreak
(establish definition)
2. Confirm that an outbreak exists
(cases meet definiton)
3. Find additional cases
4. Charecterize cases
(collect demo info about cases)
5. Form a hypothesis
6. Test the hypothesis
(control groups and data collected)
7. Insititute control measures
8. Evaluate effectiveness of control measures
9. Communicate the findings
Viral Structure
-made of genetic material, a protein coat, and an envelope containing lipids
-capsid --> protein coat
-envelope (if present) surrounds capsid
Viral Genome
genetic material of a virus (double or single stranded DNA or RNA)
Viral Capsid
protein coat that surrounds the genetic material of the virus
Viral Nucleocapsid
genome + capsid
Virus Envelope
-surrounds the capsid of some viruses
-helps the virus to enter the cell
-makes it more susceptible to enviornmental changes (pH, temp, chemicals)
Virion
complete virus particle
Viral Classification
-Type of nucleic acid (DNA or RNA)
-Number of strands to the nucleic acid (Single stranded or double stranded)
-morphology
-Presence or absence of viral envelope
Viral Replication Steps
1. Absorption or Attachment
2. Penetration
3. Uncoating
4. Replication and Translation
5. Assembly or Maturation
6. Release or Egress
Nonenvoloped ssDNA Viruses
parvovirdiae
Nonenveloped dsDNA virues
adenovidiae
papillomaviridae
Enveloped dsDNA viruses
herpesviridae
hepadnaviridae
poxviridae
Nonenveloped ssRNA virus
picornaviridae
calcividae
hepeviridae
enveloped ssRNA viruses
Flaviviridae
Togaviridae
Retroviridae
Orthomyxoviridae
Paramyxoviridae
Rhabdoviridae
Coronaviridae
Arenaviridae
Bunyaviridae
Deltavirus
Filoviridae
and MANY MORE
nonenveloped dsDNA viruses
reoviridae
Viral Replication - Absorption
step 1
virus attaches to specific cell-receptors (glycoproteins) through adhesion molecules
Viral Replication - Penetration
step 2
naked virons = directly into cell membrane
enveloped virons = membrane fusion into cell
endocytosis = enter in cytoplasmic vacuole
Viral Replication - Uncoating
step 3
genome release from capsid
DNA -> nucleus
RNA -> cytoplasm
Viral Replication - Replication and Translation
step 4
viral genomes tells host to make more viral proteins and replicate viral genome
Viral Replication - Assembly or Maturation
step 5
building blocks:
capsid protein subunits -> capsomers -> combine form capsid -> capsid and genome form nucleocapsid -> form genomes
Viral Replication - Release or Egress
step 6
naked virus = lysis
enveloped = budding
What type of virus structure makes it more susceptible to environmental changes?
envelope
What type of specimens are preferred for viral specimen collection?
aspirated secretions
What type of swab may be used for viral specimen collection?
dacron or rayon
(NOT calcium alginate)
What is the preferred transport time for viral specimen collection?
immediatetly
<2 hours
within 4 days?
Advantages of Serological Assays
detect nonculturable viruses (hepatitis)
Help determine immune status (MMR, VZV, HAV, HBV)
Help monitor immunosuppressed or transplant patients
Good for epidemiology and prevalence
Disadvantages of Serological Assays
Not good for severe immunosuppression
Reactivating viruses always have antibodies
Infants with maternal antibodies
Rarely have paired sera samples
Cross-reactivity of viruses
What is the principle of serologic assays?
detect viral antibodies to measure host response using paired sera samples (2 sampels 7-10 days apart = acuate and convalescent stages)