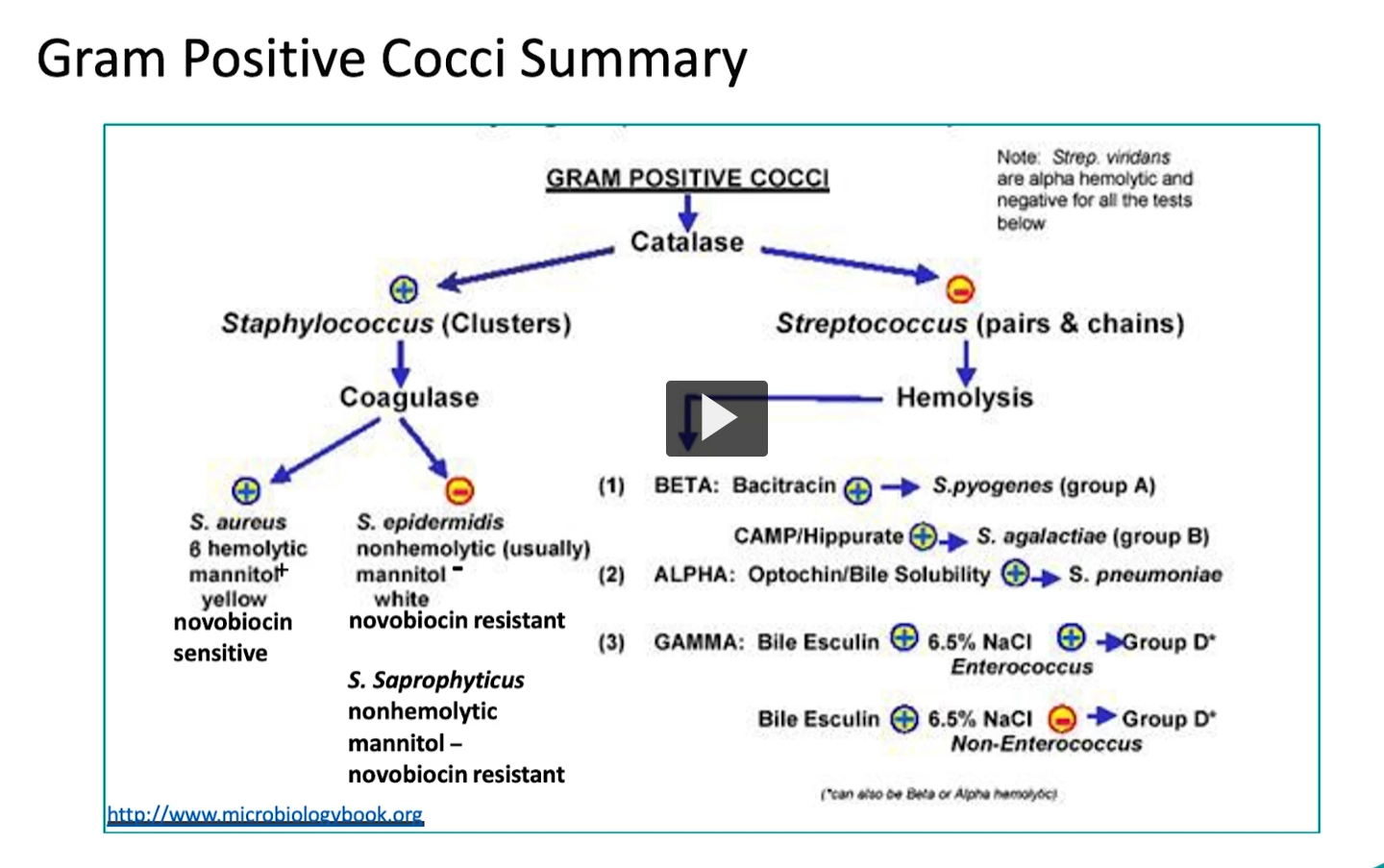
Gram Positive Cocci
1/24
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
25 Terms



Etymology
“staphylo-” → from Greek staphylē = “bunch of grapes” 🍇
“-coccus” → from Greek kokkos = “berry” or “round grain”
👉 So literally:
“grape-like clusters of round bacteria”
Staphylococcus =
A genus of Gram-positive, spherical (cocci) bacteria that:
Appear in grape-like clusters under the microscope
Are commonly found on skin and mucous membranes
Are catalase-positive (helps distinguish from Streptococcus)
Can be aerobic or facultative anaerobes
Some species are normal flora, while others cause infections (e.g., skin infections, abscesses)
Key Species (with meaning)
Staphylococcus aureus
aureus = Latin “golden” → forms gold-colored colonies
Staphylococcus epidermidis
epidermidis = “of the skin” → normal skin flora
Staphylococcus saprophyticus
saprophyticus = “feeding on dead/organic matter
Clinical Features (from your slide, explained)
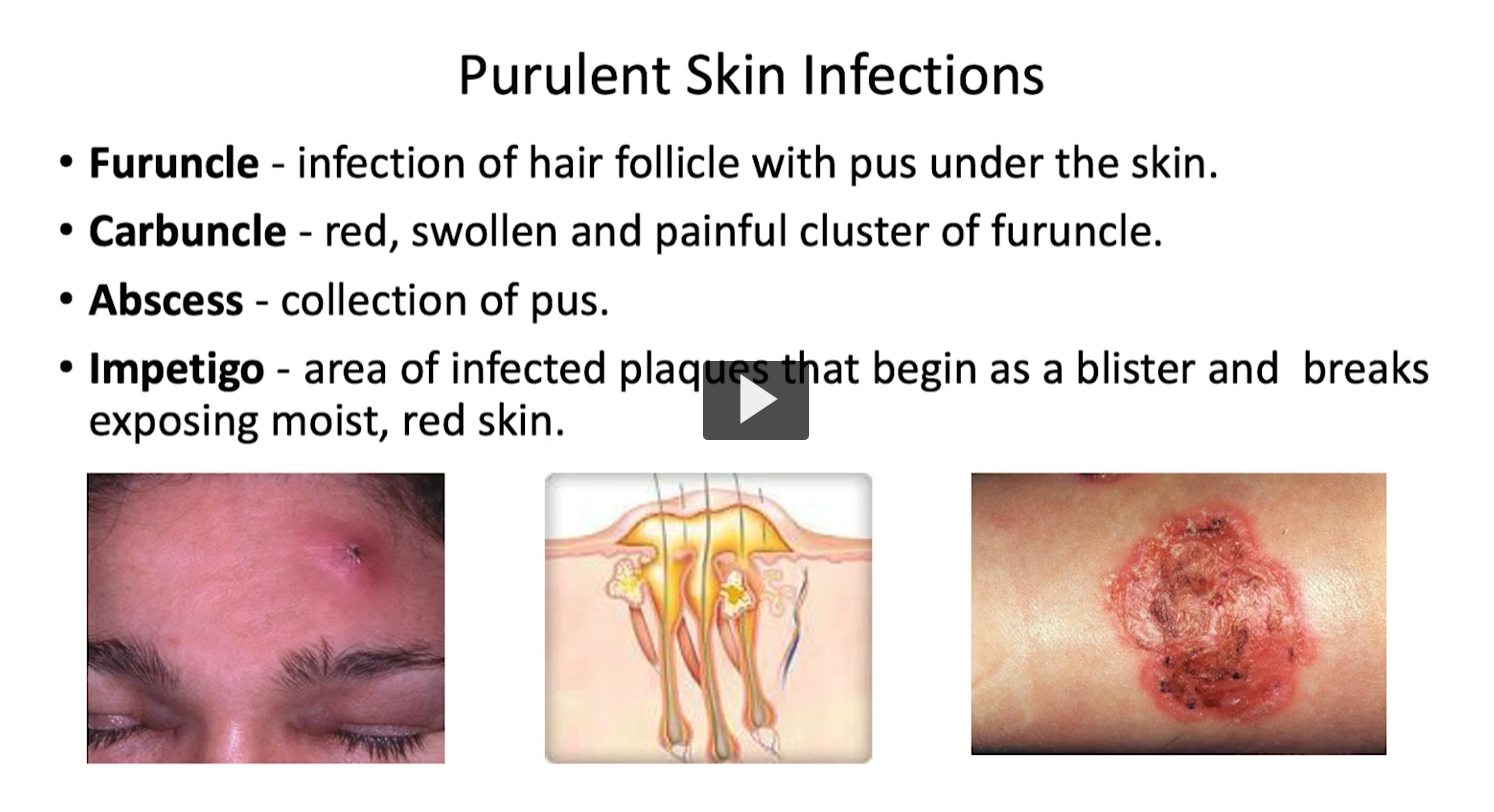
1. Purulent skin infections
Folliculitis → infection of hair follicles
Impetigo → superficial skin infection (often honey-colored crusts)
Carbuncles → deeper, connected abscesses
👉 Mostly caused by S. aureus
2. UTI
Commonly caused by S. saprophyticus
👉 Especially in young sexually active women
3. Opportunistic / Hospital-acquired infections
Seen in hospitalized or immunocompromised patients
👉 Often S. epidermidis (less virulent but opportunistic)
4. Systemic diseases
Pneumonia
Bacteremia (bacteria in blood)
Wound infections
👉 Mainly S. aureus → more aggressive

Folliticulis: S. aureus
Etymology
“follicul-” → from Latin folliculus = “small bag” or “sac” (hair follicle)
“-itis” → Greek = “inflammation”
Folliculitis = inflammation of a hair follicle
Common Causes
Most common: Staphylococcus aureus
why?
Step-by-Step Mechanism 1. Normal colonizer of skin
S. aureus commonly lives on:
Skin
Nose (nares)
👉 So it’s already in the right place
2. Entry into hair follicle
Hair follicles are natural openings in the skin
Entry is easier when:
Shaving (micro-cuts)
Friction (tight clothes)
Sweat/occlusion
👉 Bacteria get trapped inside the follicle
3. Adhesion + colonization
S. aureus has adhesins (surface proteins) that stick to:
Keratin
Extracellular matrix
👉 Helps it anchor inside the follicle
4. Virulence factors → tissue damage
S. aureus produces:
Coagulase → forms fibrin “shield” (hides from immune system)
Cytotoxins (e.g., leukocidins) → kill immune cells
Enzymes → break down tissue
👉 This allows local invasion and survival
5. Strong neutrophil response → PUS
Immune system sends neutrophils
Bacteria + dead neutrophils + debris = pus
👉 That’s why folliculitis looks like:
Small pustules centered on hair
Opportunistic / Hospital-acquired infections
Seen in hospitalized or immunocompromised patients
👉 Often S. epidermidis (less virulent but opportunistic)
2. UTI
Commonly caused by S. saprophyticus
👉 Especially in young sexually active women
Because S. saprophyticus colonizes the genital/perineal area, adheres strongly to the urinary tract, and is mechanically introduced into the bladder during sexual activity.
Step-by-step explanation 1. Normal colonization near the urethra
S. saprophyticus lives in:
Perineum (skin around genitals)
Vaginal flora
👉 So it’s already right next to the urethral opening
2. Female anatomy = short urethra
Female urethra is:
Short (~4 cm)
Close to vagina + anus
👉 Bacteria have a very short distance to reach the bladder
3. Sexual activity = mechanical transfer
During intercourse:
Bacteria are pushed into the urethra
👉 This is why UTIs are sometimes called:
“Honeymoon cystitis”






α-toxin (most high-yield)
a-toxin (alpha-toxin) is named for being the first of several hemolysins identified from Staphylococcus aureus.
Mechanism: Forms pores in cell membranes
Effects:
Damages:
RBCs
WBCs
Platelets
Disrupts smooth muscle in blood vessels
Causes:
Tissue necrosis
Severe local damage
👉 Think: “punches holes in cells → everything leaks out → cell dies”
⚠ β-toxin
Works with α-toxin
Enhances tissue destruction
β-toxin = “the second classified toxin” produced by the bacterium
The Greek letters (α, β, γ, δ) are just a naming system, not describing structure directly
So β-toxin literally means: “the second toxin (poison) identified in this group
Why this matters clinically
These toxins explain why S. aureus causes:
Pus (kills neutrophils)
Abscesses (localized destruction)
Necrotic skin infections


“leuko-” → from Greek leukos = “white”
“-cidin” → from Latin caedere = “to kill”
👉 Leukocidin = “white cell killer”
Definition
Leukocidins are exotoxins produced by Staphylococcus aureus that:
Kill white blood cells (especially neutrophils and macrophages)
Work by:
Forming pores in cell membranes
Increasing permeability → cells swell and burst
1. Pyrogenic
“pyro-” → Greek pyr = fire 🔥
“-genic” → “producing”
👉 Pyrogenic = “fever-producing”
2. Toxin
From Greek toxikon = poison (originally arrow poison)
👉 Toxin = a poisonous substance produced by organisms
3. Superantigen
“super-” = excessive / above normal
“antigen” = substance that stimulates immune response
👉 Superantigen = an antigen that overstimulates the immune system
Definition
Pyrogenic toxin superantigens (PTSAgs) are exotoxins produced by Staphylococcus aureus that:
👉 Massively activate the immune system in a non-specific way, causing:
Widespread T-cell activation
Huge cytokine release (cytokine storm)
Fever and systemic inflammation


Exfoliative
“ex-” = out / away
“folium” (Latin) = leaf
👉 Exfoliate = “to peel off like leaves”
2. Toxin
From Greek toxikon = poison
3. Exfoliatin / Epidermolytic
“epidermo-” = epidermis (outer skin layer)
“-lytic” = breaking
👉 Epidermolytic toxin = “breaks the outer skin layer”
Definition
Exfoliative toxin (A & B) is an exotoxin produced by Staphylococcus aureus that:
👉 Acts as a protease to:
Break down proteins that hold skin cells together
🔬 Mechanism (HIGH-YIELD)
Targets desmoglein-1 (cell adhesion protein in epidermis)
Causes:
Separation of epidermal layers
Skin cells lose attachment → peeling
👉 Think:
“cuts the glue between skin cells”
⚠ Types (from your slide)
ET-A
Heat (thermo) stable
Chromosome-encoded
ET-B
Heat labile
Plasmid-encoded
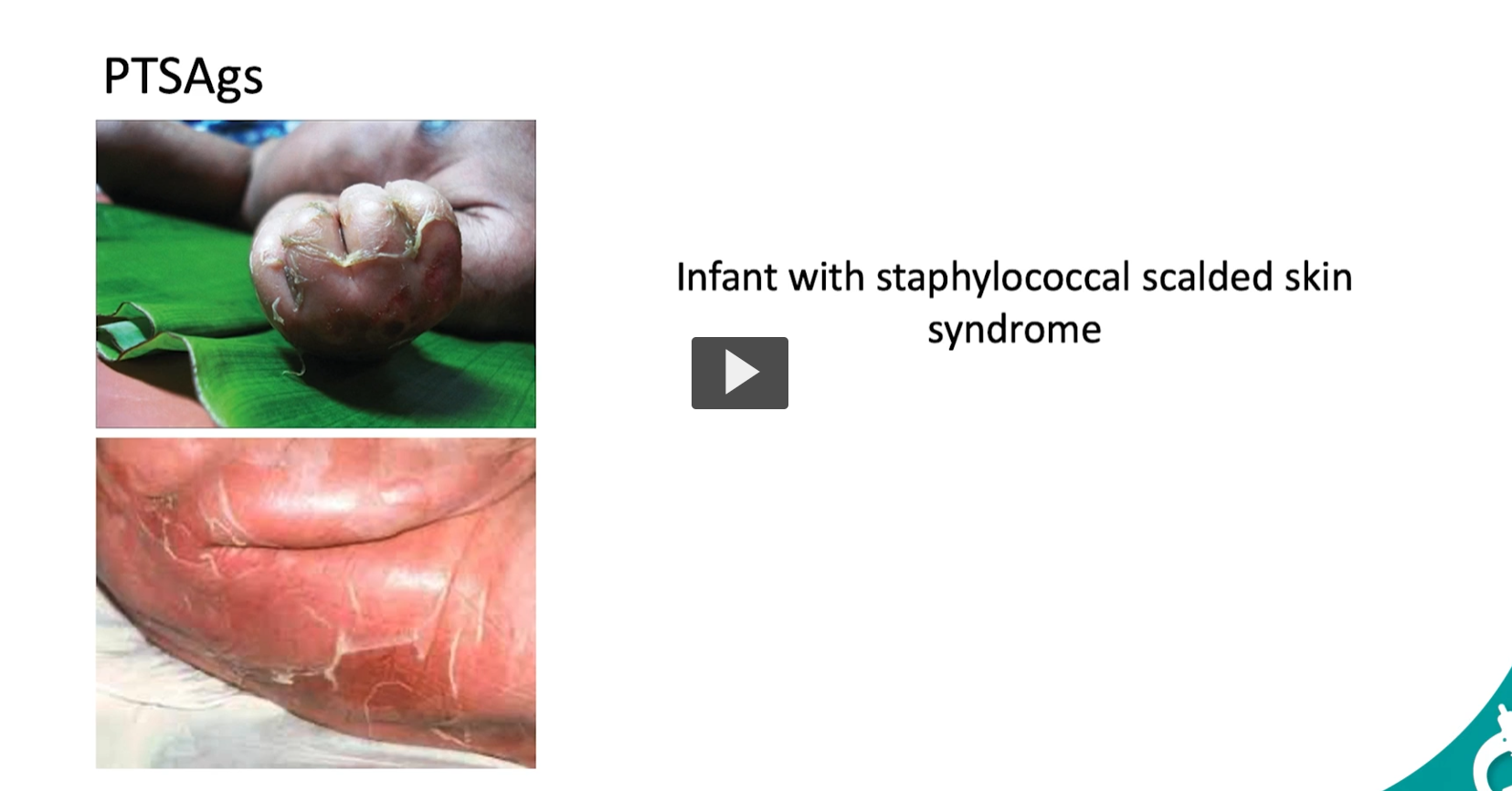
🩺 Clinical Effect Staphylococcal Scalded Skin Syndrome (SSSS)
Skin looks like it’s been burned/scalded
Features:
Blistering
Peeling (exfoliation)
Positive Nikolsky sign (skin slips off easily)
Most common in:
Infants

Toxic-Shock-Syndrome Toxin-1
Etymology 1. Toxic
Greek toxikon = poison
2. Shock
From French choc = sudden impact/collapse
👉 In medicine: circulatory collapse (low blood pressure)
3. Syndrome
Greek:
“syn-” = together
“dromos” = running/course
👉 Syndrome = a group of symptoms occurring together
4. Toxin (TSST-1)
TSST-1 = Toxic Shock Syndrome Toxin-1
👉 The first identified toxin causing this syndrome
Definition
TSST-1 is a superantigen exotoxin produced by Staphylococcus aureus that:
👉 Triggers massive, non-specific activation of T-cells
→ leads to a cytokine storm

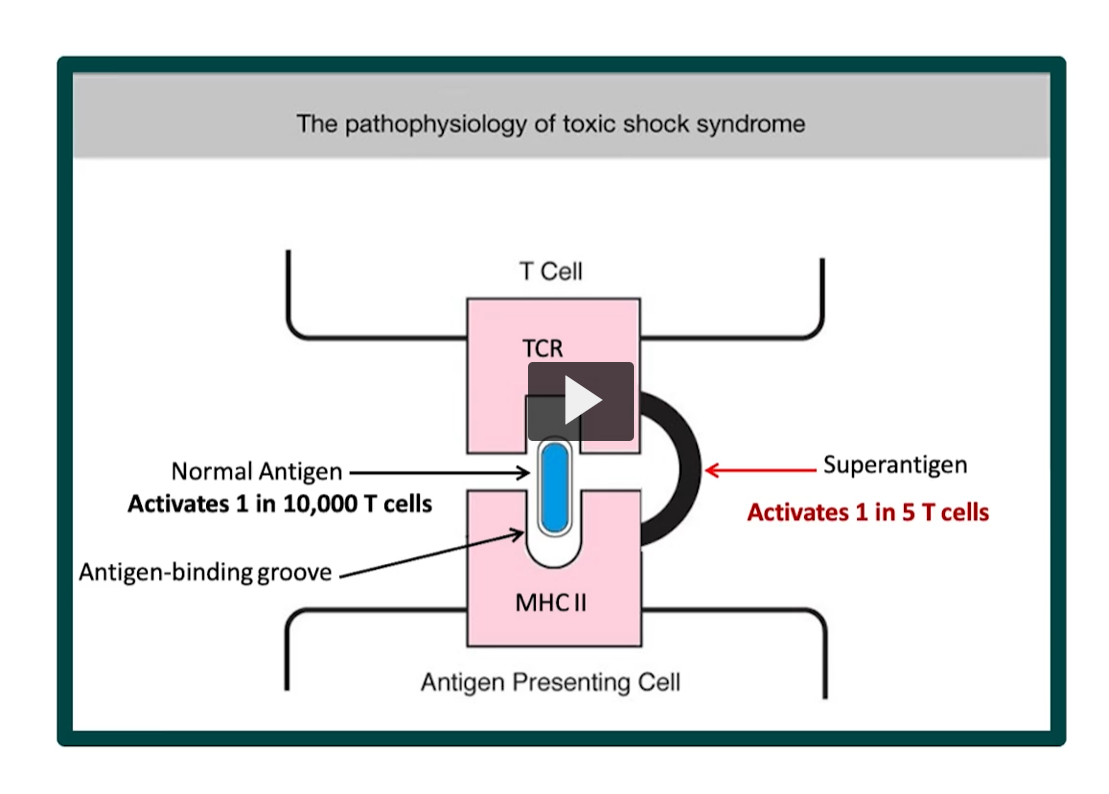
Normal Antigen Presentation
Antigen sits in MHC II groove
TCR recognizes specific antigen
👉 Activates:
~1 in 10,000 T cells (very controlled)
🔴 Superantigen Mechanism (TSST-1)
Produced by Staphylococcus aureus
👉 Instead of normal binding:
Superantigen links MHC II directly to TCR
Bypasses the antigen-binding groove
👉 Result:
Activates:
1 in 5 T cells (~20%)
⚡ What happens next?
Massive activation → cytokine storm
Releases:
IL-1 → fever
TNF-α → hypotension (shock)
IL-2 → T-cell proliferation





“strepto-” → from Greek streptos = “twisted” or “chain-like”
“-coccus” → from Greek kokkos = “berry” or “round”
👉 Streptococcus = “chains of round (spherical) bacteria”
Definition
Streptococcus is a genus of Gram-positive, spherical (cocci) bacteria that:
Grow in chains or pairs (diplococci)
Are catalase-negative (key distinction from Staphylococcus)
Are non-motile and non–spore forming
Often live in the:
Respiratory tract
Gastrointestinal tract
🔬 Key Characteristics (from your slide, explained)🟣 Gram-positive cocci
Thick peptidoglycan → stain purple

Important Exception
Streptococcus pneumoniae
Viridans streptococci
👉 DO NOT have Lancefield antigens
→ Cannot be classified this way


S. pyogenes produces hemolysins = toxins that destroy red blood cells (RBCs) → causes β-hemolysis (clear zone on blood agar)
👉 Two main ones:
Streptolysin O
Streptolysin S
🔴 1. Streptolysin O (SLO) 📖 Key Features
O = Oxygen-labile (inactivated by oxygen ❌)
Works only in anaerobic (low O₂) conditions
👉 That’s why:
Hemolysis is better seen below the agar surface
💥 What it does
Forms pores in cell membranes
Kills:
RBCs
WBCs
Platelets
🧪 Clinical importance
Highly antigenic → body makes antibodies
These are measured as:
ASO (Anti-Streptolysin O) titer
👉 Used to diagnose:
Rheumatic fever
Post-strep infections
🟡 2. Streptolysin S (SLS) 📖 Key Features
S = Stable in oxygen ✅
Works on surface of agar
👉 Responsible for:
The visible β-hemolysis (clear zone) you see in lab
💥 What it does
Also destroys RBCs → contributes to hemolysis
❗ Key difference
NOT antigenic
👉 No antibody formation → no diagnostic test


S. pyogenes produces exotoxins that:
👉 Spread beyond the throat/skin
👉 Cause systemic disease (rash, shock, tissue destruction)
🔴 1. Erythrogenic toxin (Pyrogenic exotoxin) 📖 What it does
Causes the rash of scarlet fever
🧠 Mechanism
Acts as a superantigen → massive cytokine release
Leads to:
Fever
Red “sandpaper” rash
Strawberry tongue
⚠ Key idea
Bacteria stay in the pharynx
But toxin spreads through bloodstream
👉 Disease = toxin-mediated, not direct invasion
⚡ 2. Pyrogenic Exotoxin A (SpeA) 📖 What it does
Causes Strep toxic shock–like syndrome
🧠 Mechanism
Superantigen
Activates huge numbers of T-cells → cytokine storm
💥 Results
High fever
Hypotension
Multi-organ failure
👉 Very similar to S. aureus TSST-1
💀 3. Exotoxin B (SpeB) 📖 What it is
A protease enzyme
🧠 What it does
Breaks down proteins in tissue
Rapidly destroys:
Fascia
Muscle
⚠ Clinical effect
👉 Necrotizing fasciitis (“flesh-eating disease”)
Extremely fast spreading
Severe pain
Tissue death (necrosis)
These are physical components on the bacteria (not toxins) that help it:
👉 Stick to cells
👉 Avoid the immune system
👉 Survive and spread
🔴 1. M Protein (MOST IMPORTANT) 📌 What it does 🧲 Adherence
Helps bacteria attach to throat (pharyngeal) epithelial cells
👉 First step in infection
🛡 Blocks opsonization
Prevents complement (C3b) from coating the bacteria
👉 Without opsonization:
Immune cells can’t recognize it easily
🚫 Antiphagocytic
Stops neutrophils/macrophages from engulfing (phagocytosis)


Big Picture
These enzymes are called “spreading factors” because they help bacteria:
👉 Break through tissue barriers
👉 Escape immune traps
👉 Spread rapidly through the body
🧪 1. DNases (Deoxyribonucleases) 📌 What they do
Break down DNA
🧠 Why that matters
Infection sites contain lots of dead cells + neutrophils
These release DNA → thick pus
👉 DNase:
Liquefies pus
Helps bacteria move through infected tissue
🧪 Clinical clue
Body makes anti-DNase antibodies
👉 Used to detect recent strep infection (like ASO)
🧬 2. Hyaluronidase 📌 What it does
Breaks down hyaluronic acid
🧠 Why that matters
Hyaluronic acid = “glue” of connective tissue
👉 When broken:
Tissue becomes loose
Bacteria can spread between cells
💡 Nickname
👉 “Spreading factor” (classic exam term)
🩸 3. Streptokinase 📌 What it does
Breaks down fibrin clots
🧠 Why that matters
Body tries to trap bacteria in clots
👉 Streptokinase:
Dissolves the clot
Frees bacteria → spreads infection
Group A Strep causes 2 categories of disease:
🔥 1. Suppurative (pus-forming, ACTIVE infection)
👉 Bacteria are present and invading tissue
⚠ 2. Non-suppurative (post-infectious, IMMUNE-mediated)
👉 Bacteria are gone, but immune system causes damage


Streptococcus agalactiae etymology combines Greek and Latin roots meaning "chain-forming berry without milk." It derives from streptos (twisted/chain), kokkos (berry/sphere), and agalactiae (no milk), referencing its chain-like structure under a microscope and its historical identification as a cause of bovine mastitis that stops milk production
Big Picture
Group B Strep is:
👉 Normal flora in women
👉 But becomes dangerous when transmitted to newborns
🌍 1. Normal Flora
Found in vagina (5–35% of women)
👉 Usually harmless in adults
🔬 2. Hemolysis
β-hemolytic (like Group A)
But:
Less clear hemolysis
👉 Lab clue: weaker clearing on blood agar
. MOST IMPORTANT CLINICAL POINT
👉 Most common cause of:
Neonatal sepsis
Neonatal meningitis