The Skin's Response to Injury (Pt. 2 Skin & Immune System)
1/36
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
37 Terms
How does the epidermis respond to injury.
• Release of pro-inflammatory cytokines & growth factors by keratinocytes
• Altered proliferation & differentiation
• Hyperplasia, hyperkeratosis / parakeratosis
How does the dermis respond to injury?
• Stimulation of dermal inflammation
• Erythema (reddening), oedema, exudation
• Release of secondary cytokines / growth factors promotes further change
Reminder** What are key features of atopic dermatitis?
• Type 1 hypersensitivity (more later!)
• Multifactorial
Genetics + environment
• Type 1 hypersensitivity reaction to environmental allergens
Commonly house dust mites
Enhanced MC mediator release in these dogs
• Predisposition seems to be inherited
10% of dogs affected
Especially WHWTs, Cairns, Scotties, Boxers etc.
• Pruritic dermatitis, otitis and conjunctivitis
• Face, feet, ventrum
• Histology
Variable, often minimal
What is orthokeratotic hyperkeratosis?
Increase in thickness of anuclear stratum corneum
Grossly, animal would look flaky
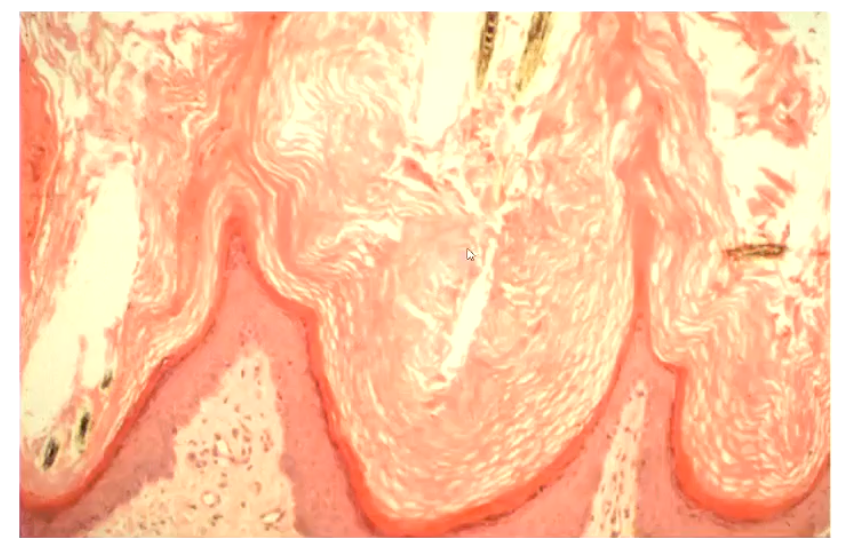
What is parakeratotic hyperkeratosis(perakeratosis)?
Thickened stratum corneum which has retained nuclei (Not normal)
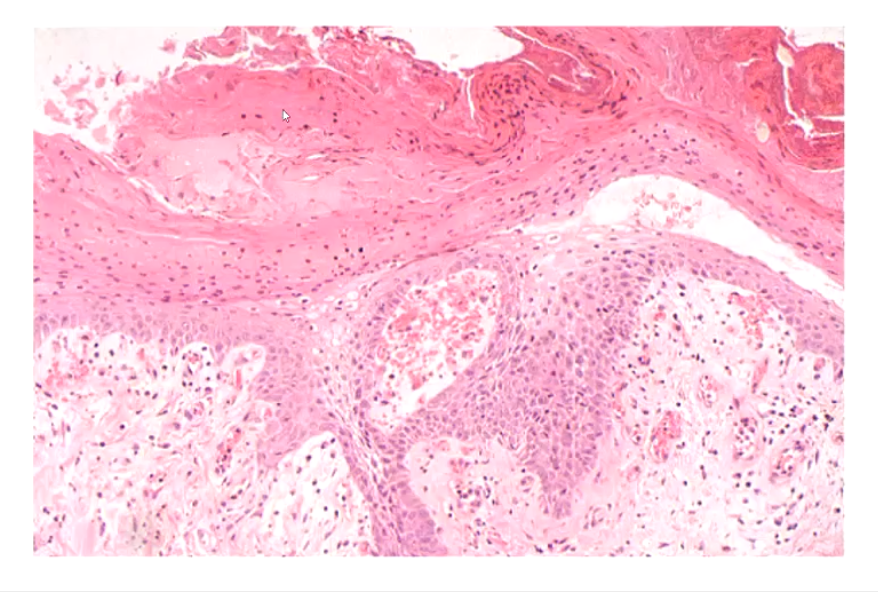
What is hypergranulosis?
Prominent granular layer associated with hyperkeratosis
Lots of granules in stratum granulosum → suggests inflammation
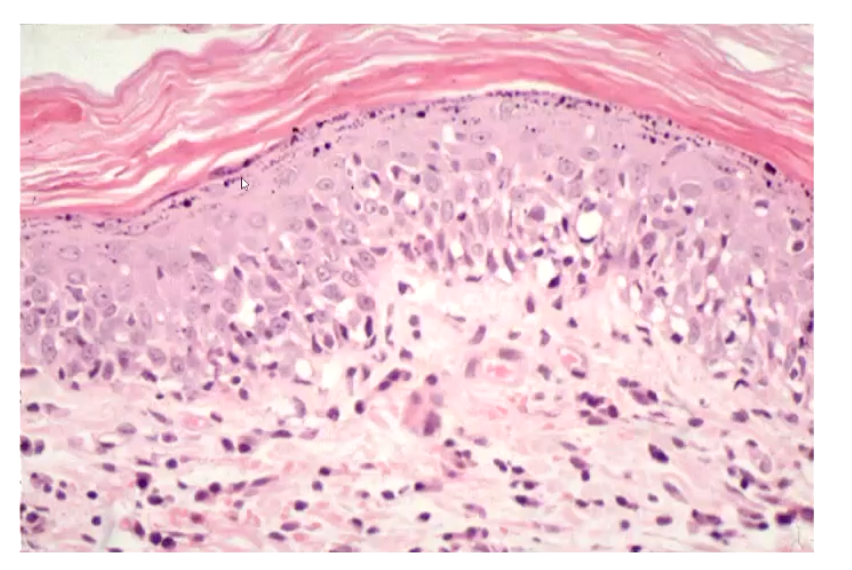
What is acanthosis?
Hyperplasia / hypertrophy of the spinous layer
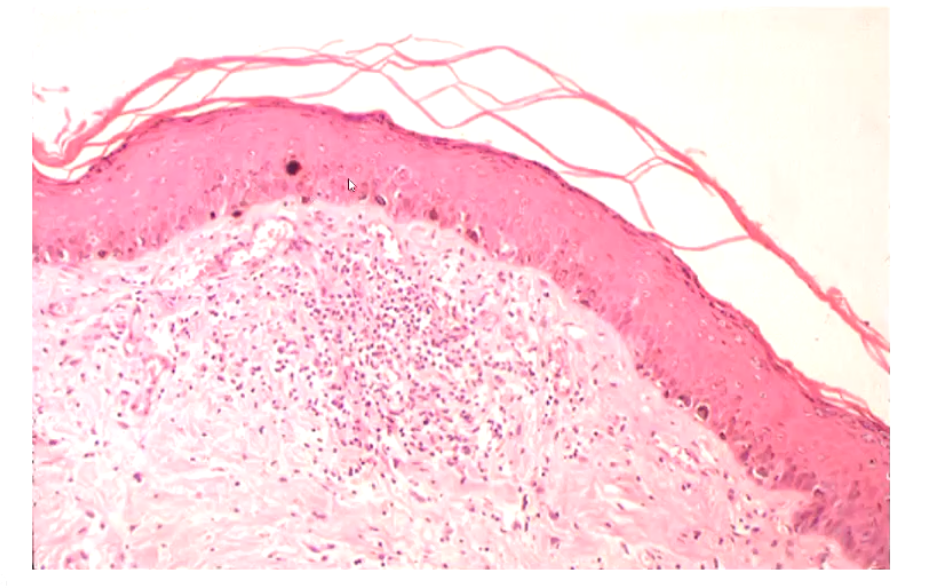
What is hyperplasia?
Thickened epithelium, forms pegs or projections of epidermis into the dermis
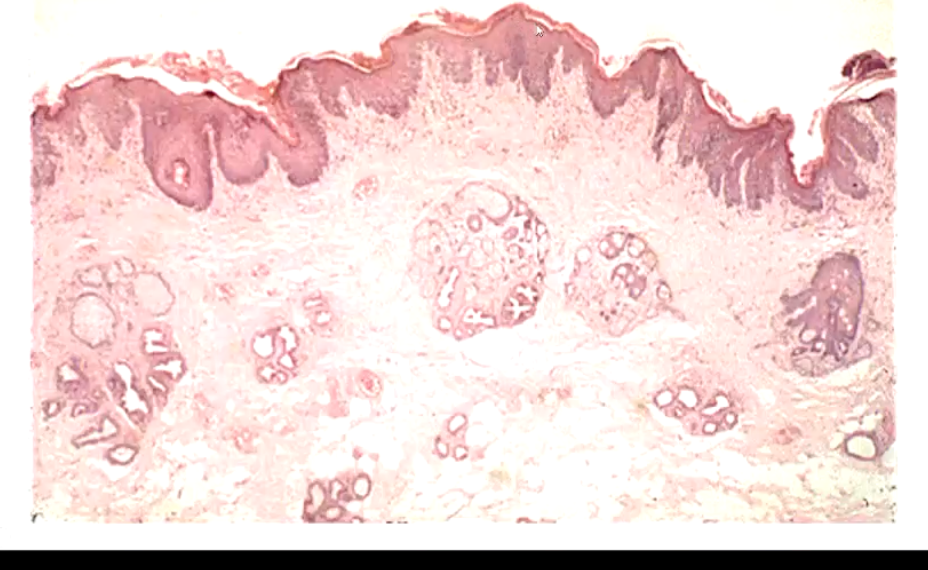
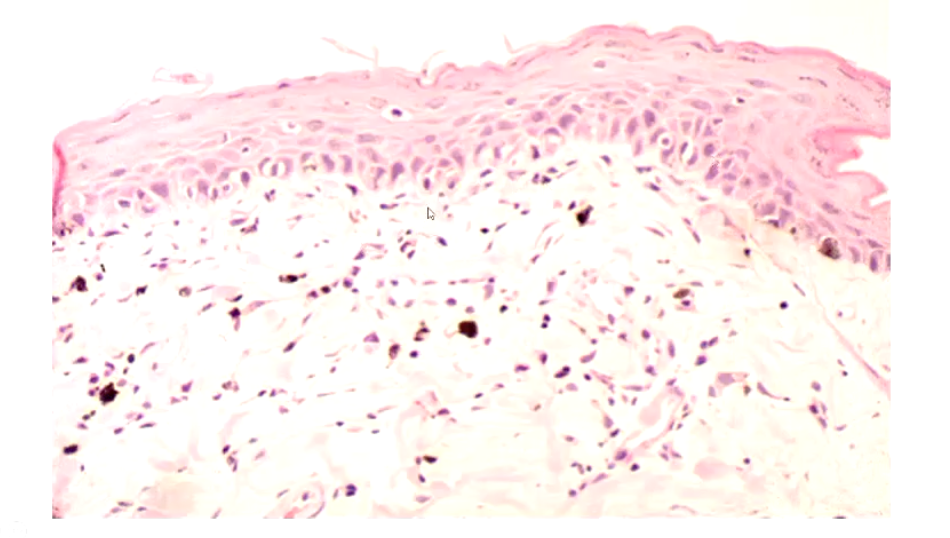
What is altered pigmentation associated with?
Pigmentary incontinence - the melanocytes are leaking melanin
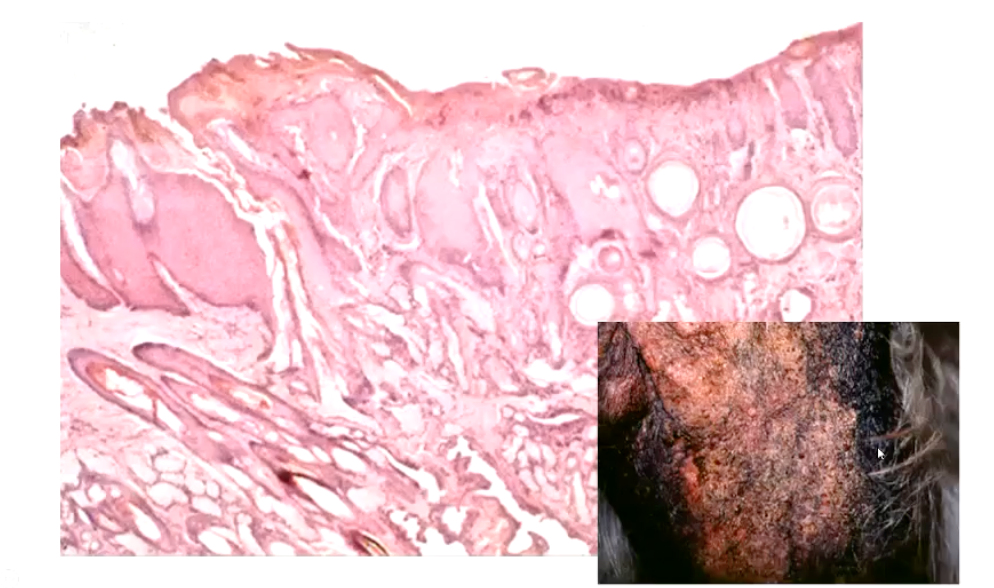
What is lichenification?
Hyperkeratosis, hyperplasia and dysplasia
Chronic inflammation, presence of cysts
Traumatic skin disease can be caused by what two main methods?
• Direct
Friction/pressure
Chemical (irritant contact dermatitis)
Heat (burns)
Light (phototoxicity)
• Indirect
Metabolic (photosensitivity)
How does self-trauma contribute to development of skin issues in animals?
• Major contributing factor in the development and progression of skin disease in animals
• Response to pruritus (or pain)
Action of various mediators
Epidermal & dermal sensory nerves
• Scratch reflex
Spinal reflex
Modulated by motor cortex neurones
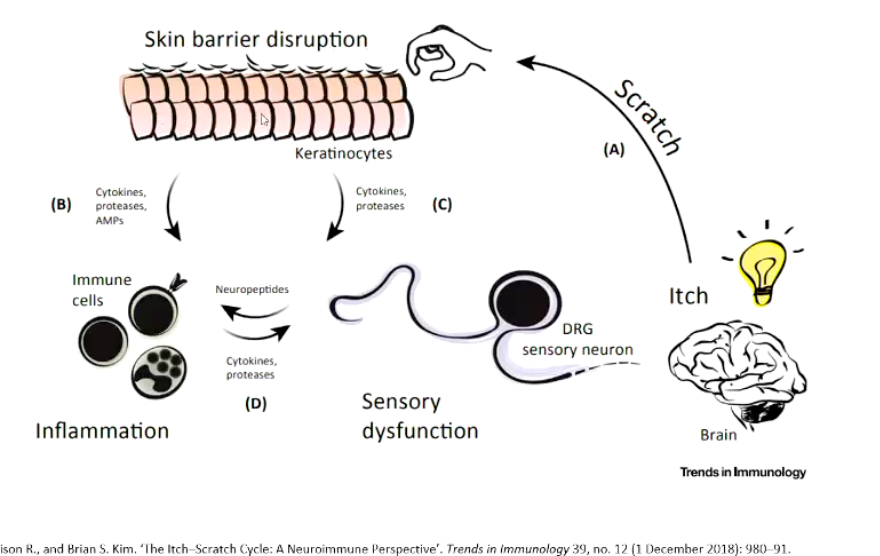
What is the itch-scratch cycle?
Begins with itch (sensed by brain)
Itched → disrupts skin barrier → keratinocytes can release proteases, cytokines and AMPs, these recruit immune cells
The immune cells release cytokines that make the sensory nerves more sensitive in response to inflammation
Brain is more likely to sense itch → increasing itching sensation
What is acral lick dermatitis?
Manifestation of skin disease in form of self trauma
• Common, multifactorial
May reflect underlying pyoderma
May be behavioral...
• Hairless plaques (red and often depressed), as the skin has become ulcerated from licking
• Aka 'lick granuloma' &
Misnomer - its not a granuloma...
Repetitive licking → chronic trauma → follicular damage and rupture → furunculosis
What is furunculosis?
Furunculosis in dogs is a deep skin infection and inflammation of the hair follicles, resulting in painful boils (furuncles) that can cause pimples, draining tracts, swelling, and ulceration.
What are hypersensitivity reactions?
• An exaggerated or inappropriate immune response to a mild pathogen or innocuous substance (allergen)
What is an autoimmune disease?
• A specific humoral or cell-mediated immune response against the body's own tissue components (auto-antigens)
When the body reacts to self
Reminder** What are the four types of hypersensitivity reactions?
• Type I - Anaphylactic, immediate
• Type II - Antibody-dependent, cytotoxic
• Type III - Immune complex mediated
• Type IV - Cell-mediated, delayed
Summarize the differences between the four types of immune reactions.
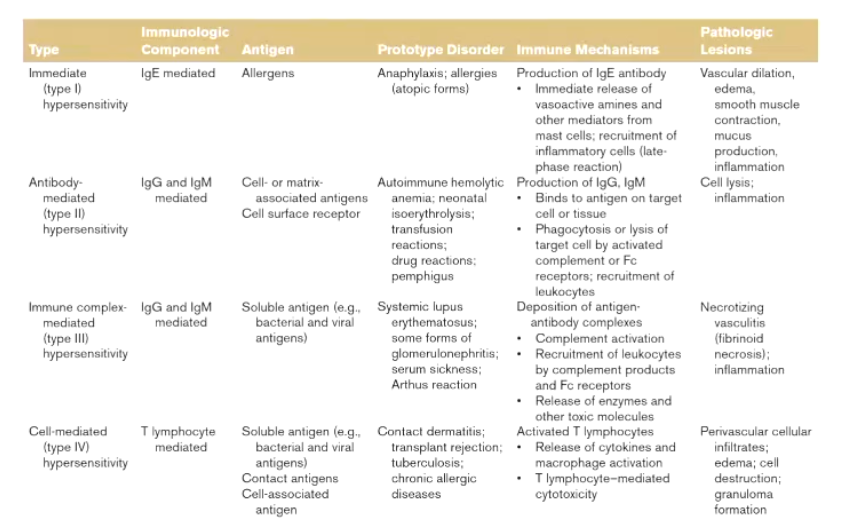
What are the main features of Type I Hypersensitivity?
• Production of antigen specific IgE
IgE is bound to mast cell membranes
Re-exposure to antigen
• Mast cell degranulation
Release of vasoactive mediators
Including histamine and prostaglandins
• Severe systemic reaction (anaphylaxis), or milder local reaction
Is type I hypersensitivty systemic or localized?
Can be systemic (anaphylaxis) OR localized to skin OR systemic with skin involvement
What occurs when the IgE’s are crosslinked?
This is the sign for the mast cell to degranulate
What are the immediate response and late phase reactions occuring after mast cell degeneration?
Immediate Response
Vasodilation
Vascular Leakage
Smooth Muscle Spasm
Late-Phase Reaction
Leukocyte infiltration
Epithelial Damage
Bronchospasm
What is anaphylaxis?
• Immediate systemic reaction caused by rapid, IgE-mediated, immune release of potent mediators from tissue mast cells and peripheral basophils
Rapid onset, may cause death
• Involves skin +/- mucosal tissue; respiratory system; gastrointestinal system and cardiovascular system
• Release of vasoactive mediators > systemic vasodilation & increased vascular permeability > hypotension & tissue hypoperfusion
What can trigger anaphylaxis?
Food
Medications
Venoms
Unidentified
<30% of cases in humans
**Note: not all reactions involve IgE, some triggers directly stimulate mast cells
What are some examples of Type I hypersensitivity reactions?
• Atopic dermatitis
Damage to skin → allows antigen in → inflammation is caused by IgE and mast cells
• Insect bite hypersensitivity
• Flea bite hypersensitivity
• Culicoides spp. hypersensitivity ('sweet itch')
• Drug eruptions, food allergy etc..
Atopic dermatitis and flea bite hypersensitivity account for most cases of skin disease in dogs and cats
In what animals is insect bite hypersensitivity most common in? What are common triggers?
• Allergic dermatitis
Acute or more often chronic
• Common
Horses, dogs, cats, humans
Equine Leucocyte Antigen (MHCII) risk factors recognised in horses
• Triggers include:
Fleas (e.g. Ctenocephalides spp.)
Biting midges (e.g. Culicoides spp.)
Black flies (Similium spp.)
Mosquitoes (Culicidae family)
Type I Hypersensitivity
:. classed as an atopic disorder in human & equine medicine
What are the key features of flea bite hypersensitivity? (flea allergy dermatitis)
• Type 1 hypersensitivity (and/or Type IV)
• Common - no breed predilection
• May be seasonal - summer & autumn
• Pruritic, papular dermatitis
e.g. miliary eczema
• Dorsal lumbosacral area, neck, inner thighs, abdomen
• Histology: May include eosinophils in dermal infiltrate and/or intraepidermal eosinophilic abscesses
What is miliary dermititis?
Miliary dermatitis in animals, primarily cats, is a skin reaction pattern characterized by small, crusty bumps that resemble millet seeds, often caused by allergies to fleas, food, or other environmental factors
What are the key features of Type II Hypersensitivity?
• Direct damage mediated by antibodies to exposed cell surface antigens
Antigen usually endogenous, something normal to the dog
• Binding of antibody (IgG or IgM) +/- complement to self-antigen
Normal cell is phagocytized or complement is activated, leading to inflammation and tissue injury
• Underlies various autoimmune disorders affecting various tissues
Pemphigus, pemphigoid (epidermal cells)
Haemolytic anemia (red blood cells)
Which is why with blood transfusions → you must be very cautious on the second transfusion
What are the key features of pemphigus?
Type II Hypersensitivity Reaction
Antibodies produced target proteins in intercellular junctions of epidermal cells (self-cells)
Antibody-mediated activation of proteases
Disruption of intercellular adhesions
• Vesiculobullous lesions
The deeper the layer of the skin which is targeted produces a more severe condition, as opposed to a more superficial target
What is Type III hypersensitivity?
Also known as immune-complex hypersensitivity
Occurs in three phases
Phase I – Immune Complex Formation
Antigens and antibodies bind in circulation to form soluble immune complexes.
Usually happens when there is persistent antigen exposure (e.g. infection, autoimmune antigen). (More antibody than antigen, producing large complexes)
Phase II – Immune Complex Deposition
These immune complexes deposit in tissues such as blood vessel walls, kidneys, joints, or lungs.
Deposition occurs especially where filtration or high pressure favors trapping (e.g. glomeruli, synovium).
Phase III – Immune Complex–Mediated Inflammation
The deposited complexes activate complement and attract neutrophils and macrophages.
These cells release enzymes and reactive molecules that cause inflammation and tissue injury.
When they bind to antibody and degranulate they cause by stander damage to the vessel causing the hallmark lesion → Vasculitis
What is Type IV Hypersensitivity?
• Same processes as cell-mediated immunity to microbial infection
NOT dependent on antibody
• Balance swings from protection to tissue damage
Especially if the stimulus is great or unusually persistent
• Sensitised T-cell population develops after initial contact with antigen via APCs
Re-exposure → lymphocyte activation - cytokine release → macrophage infiltration
• Tissue damage is due to activated macrophages and cytotoxic T-cells
Causes inflammation + accumulation of cells which can form granulomas
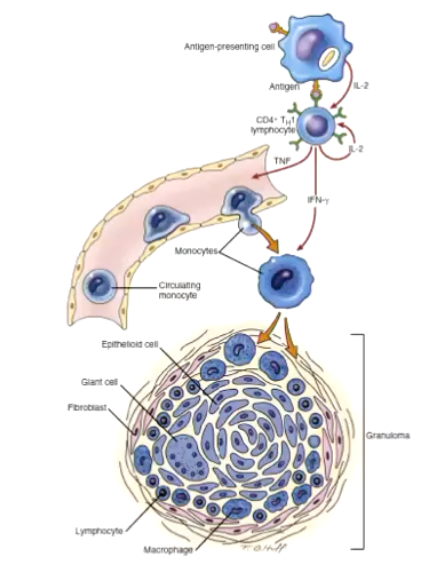
How do granulomas form?
Granuloma Formation
Granulomas form when the immune system tries to wall off substances it cannot eliminate, such as persistent microbes, foreign material, or self-antigens.
Persistent stimulus:
A pathogen (like Mycobacterium), foreign body, or resistant antigen remains in tissue and can’t be cleared by macrophages.Chronic macrophage activation:
Continuous immune signaling (especially IFN-γ from T helper 1 cells) activates macrophages, which enlarge and transform into epithelioid cells (specialized macrophages with secretory function).Cell aggregation:
Epithelioid cells cluster together, often fusing to form multinucleated giant cells.T-cell involvement:
Lymphocytes (mainly CD4⁺ T cells) surround the macrophage core, maintaining activation through cytokine release.Fibrosis (optional):
Over time, fibroblasts lay down collagen around the lesion, forming a fibrous capsule to isolate the persistent irritant.
Why is the tuberculin test an example of delayed hypersensitivity?
Inject cow with two proteins - Purified Protein Derivative: Mycobacterium avium and M. bovis injected
Day 4 both sites checked:
M. bovis vs M. avium
1-4 mm inconclusive
>4 mm reactorW
Why is the formation of a granuloma in cattle tested for TB indicative of a positive result?
In sensitized animals, memory Th1 cells recognize the antigen and release cytokines (especially IFN-γ).
Reaction (the “delayed” part):
Over 24–72 hours, cytokines recruit macrophages and lymphocytes to the site, causing localized swelling and induration.
This visible thickening of the skin indicates a positive DTH response and suggests prior exposure or infection.
What is allergic contact dermatitis?
Another type of Type IV hypersensitivity
• Chemical (hapten) binds to epidermal proteins to form allergen, thus provoking the immune response
• Not commonly diagnosed in animals
... and difficult to distinguish from irritant contact
• Variably pruritic maculopapular dermatitis
Sparsely haired regions affected especially ventrum
Also feet, legs, perineum, scrotum, chin and pinnae
• Histology
Non-diagnostic dermatitis, often chronic