Genetics and Reproduction
1/33
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
34 Terms
What are the basic features of the reproductive system
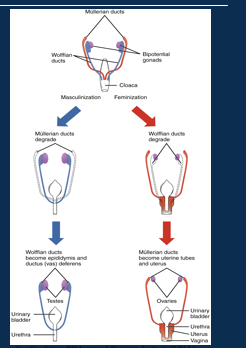
Male (XY) and female (XX) reproductive tracts develop from a common origin, which differentiate during foetal development.
Therefore, most structures are homologous and share the same basic features:
•Gonads – produce gametes (oocyte/ sperm), and hormones.
•Ducts – transport gametes and open to external environment.
•Accessory glands
•External genitalia.
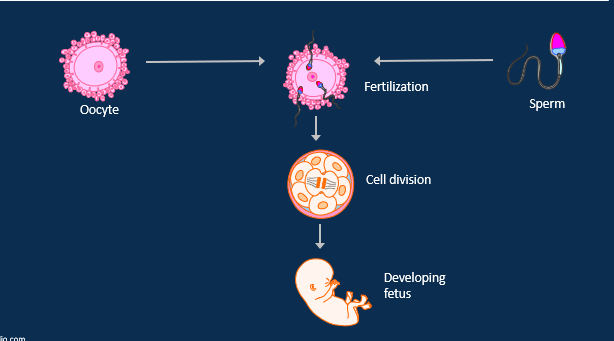
Describe reproductio
Label the female pelvic anatomy
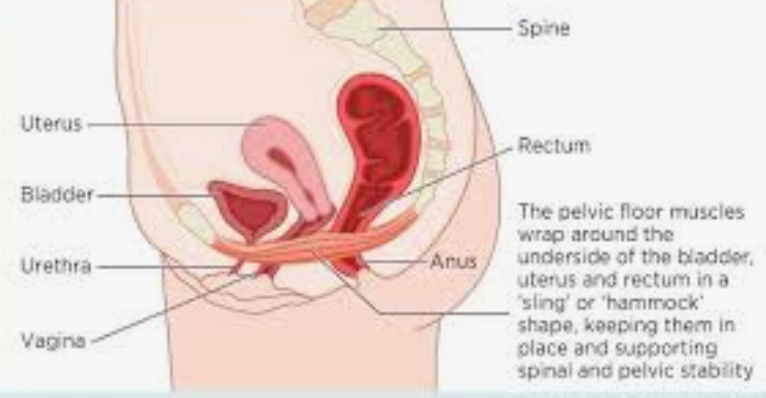
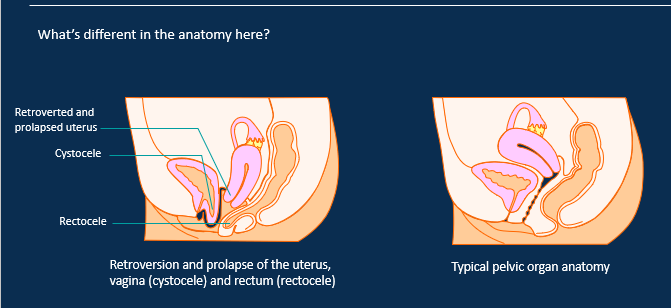
Label the female pelvic anatomy complications
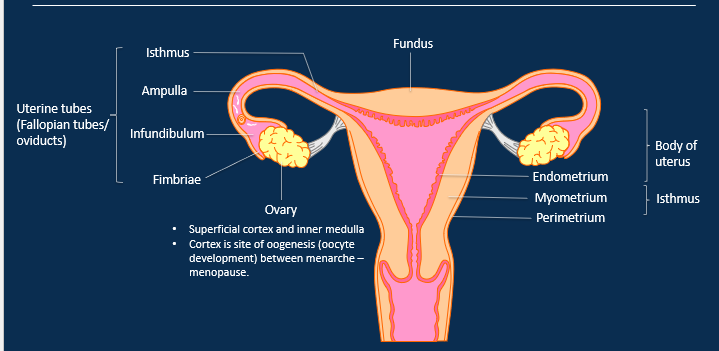
Label the ovaries and uterus
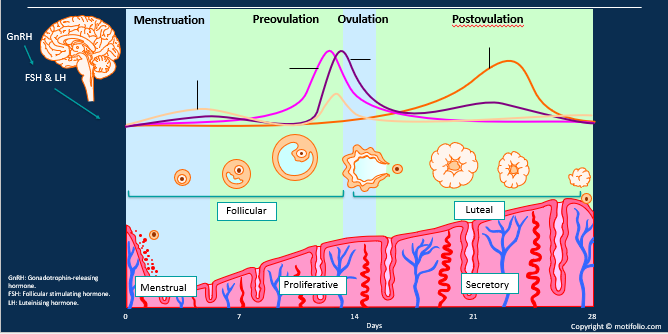
What are the phases of the menstrual cycle
Ovarian cycle/ oogenesis
Folllicular phase (1-14 days)
Luteal phase (15-28 days)
Uterine cycle
Menses (menstrual phase)
Proliferative phase
Secretory phase
Describe the follicular phase (1-14)

Describe the luteal phase

Describe the uterine cycle

Draw the diagram for the female reproductive cycle
Label the diagram of the uterus
How is cervical screening done
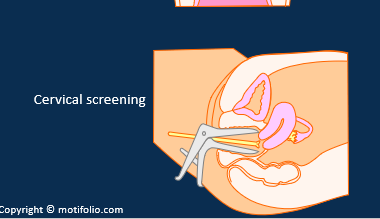
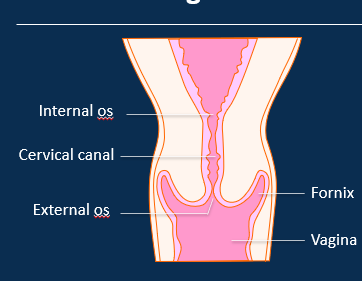
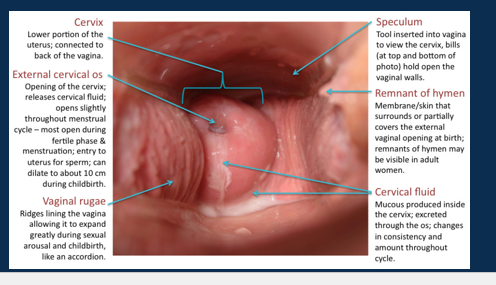
Label the cervix
Describe the different types of contraception that are in the femal tract
Combined oestrogen and progesterone
•Oestrogen lowers FSH = inhibits ovarian follicle development.
•Progesterone lowers LH = prevents ovulation, thickens cervical mucus, endometrial atrophy, decreases uterine tube motility.
•Pill, transdermal patch or vaginal ring.
Progesterone only
•Pill, implant, injection or intrauterine system (IUS).
Copper intrauterine device (IUD)
•Copper ions are spermicidal.

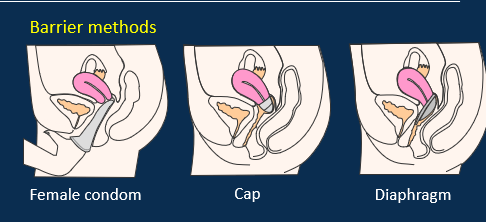
What are the barrier methods?
Female condom
Cap
Diaphragm
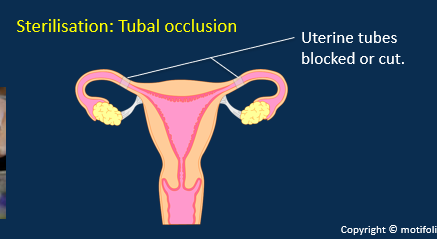
Describe sterilisation (tubal occlusion)
Describe the stages of menopause
Peri-menopause
Decrease in (ovarian) follicles, and fluctuations in oestrogen and progesterone= leading to irregular menstrual cycles. Usually begins late 40s and lasts 2-10 years
Menopause
Menstrual cycle ceases for 12 months resulting in infertility. Average age of 51.
Premature ovarian insufficiency (losing ovarian function before 40)
Post-menopause
12 months after last menses onwards.
Long-term systemic impacts.
What are the common symptoms of menopause
Vasomotor: hot flushes, night sweats, palpitations, headaches.
Psychological: low mood, irritability, difficulty concentrating, forgetfulness, loss of confidence.
Urogenital: vaginal atrophy, increased urinary frequency/ urgency/ dysuria and infection.
Connective tissue atrophy: reduced collagen synthesis results in dry and inelastic skin, hair and nails, muscle aches and bone/ joint pain.
Describe the aspects of menopause and how patient care can be improved with knowledge

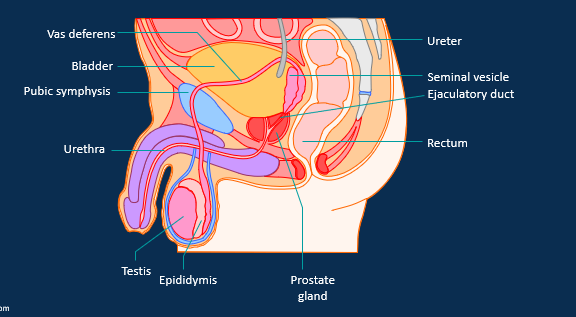
Describe male pelvic anatomy
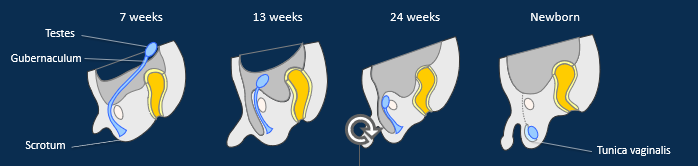
Describe the descent of the testes
•Testes develop in the abdominal cavity, fixed in position by a connective tissue cord - the gubernaculum.
•As fetus grows, the testes become more anterior/ inferiorly positioned relative to the body.
•From fetal month 7, rapid growth and hormones stimulate the gubernaculum to contract, and testes are pulled into the scrotum through the anterior abdominal wall, creating the inguinal canal.
•Testes take blood/ lymph vessels and nerves with them, forming the spermatic cord.
•Portion of peritoneum separates to form serous membrane around testes, called the tunica vaginalis. Abdominal skeletal muscle forms a layer of cremaster muscle around the testes (cremaster reflex).
•Cryptorchidism (undescended testes) occurs in 1:25 full term births (higher rates in premature births).
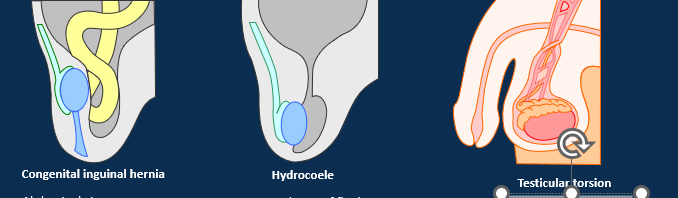
What are some testes complications
Congenital inguinal hernia
Abdominal viscera can protrude into persistent inguinal canal.
Can occur in adulthood due to weakness in abdominal wall.
Hydrocoele
Accumulation of fluid in tunica vaginalis (peritoneal fluid or produced as the result of inflammation)
Testicular torsion
Blood supply occluded by twisting of the spermatic cord.
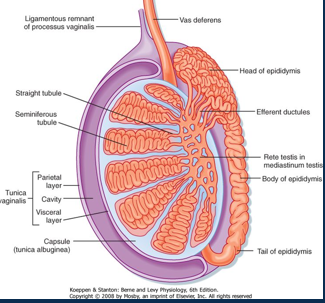
Describe the testes
•Testes sit in their own scrotal cavity
•To regulate temperature, scrotum has:
- Dartos (smooth) muscle in dermis
- Cremaster (skeletal) muscle lining.
Cremaster reflex tests L1-2 spinal nerves.
•Surrounded by double serous membrane of tunica vaginalis.
•Tunica albuginea separates testes into lobules.
•Lobules are packed with seminiferous tubules – the site of sperm production.
•Physically developed but functionally immature sperm are passed to the rete testes and then epididymis for storage.
Describe spermatogenesis
•Spermatogonia are stems cells found at the periphery of seminiferous tubules.
•Interstitial cells (cells of Leydig) produce testosterone.
•Sustentacular (Sertoli) cells support and nourish developing sperm
•Divide by mitosis to produce two daughter cells
•One daughter cell differentiates into primary spermatocyte. Undergoes meiosis I to crossover maternal and paternal genetic material and meiosis II to produce four haploid spermatids (23 chromosomes in total).
•Testes produce specialised sperm with head/ acrosome, neck, and tail, but requires further maturation by rest of reproductive tract to become functional – process called capacitance.
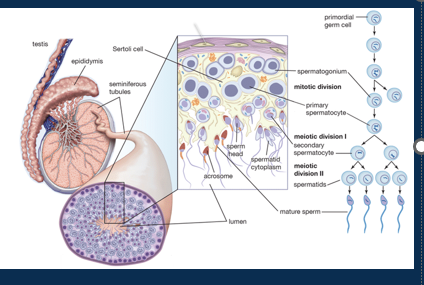
Label the male reproductive tract
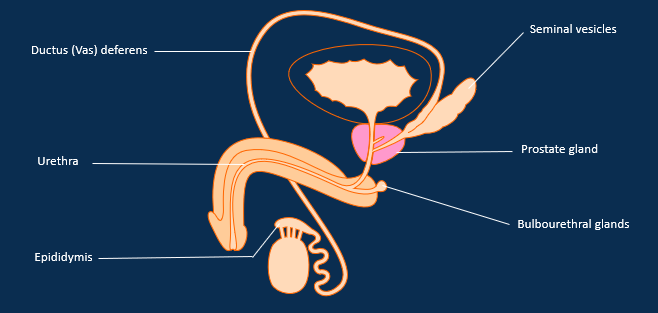
Male reproductive tract
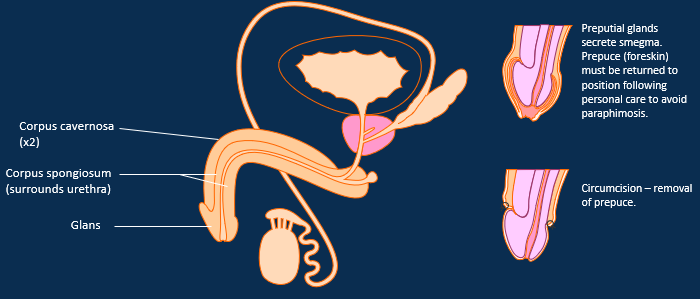
More detal about the male reproductive tract
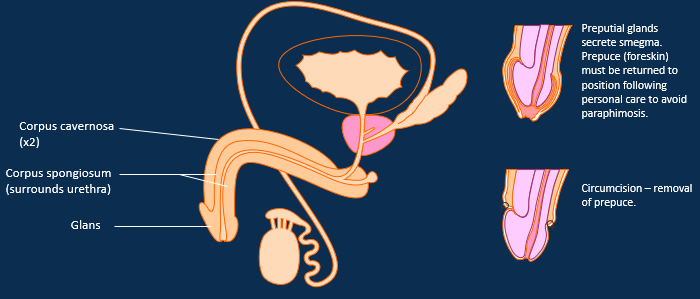
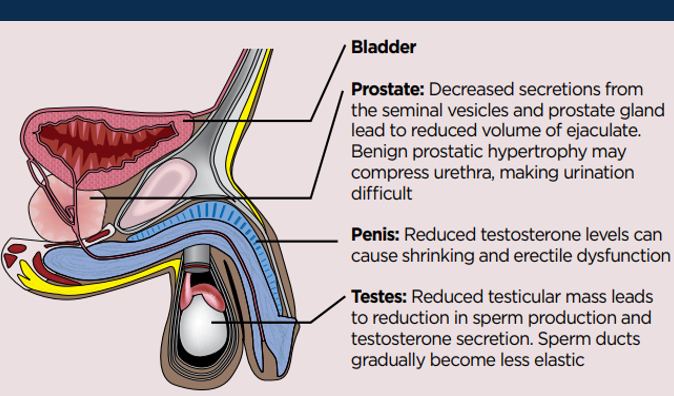
What are the changes in testes later on in life
• Testosterone levels decrease by approx. 1% per year in males from the age of 30
• Very gradual testosterone decline is associated with:
-atrophy of external genitalia
-decrease in sperm production – maintain fertility
-decreased seminal prostatic secretions
-benign prostatic hyperplasia - risk of UTI
What is late-onset hypogonadism
•10 - 20% of males develop testosterone levels below normal range, called late-onset hypogonadism. Can be asymptomatic or associated with symptoms of:
- Erectile dysfunction - Reduced muscle and bone mass - Low mood
- Loss of libido - Anaemia
What is andropause
•Some people experience difficult physical and psychological in mid-life – dubbed ‘andropause’. However, often multifactorial underlying causes related to life stressors and co-morbidities, rather than hormone deficiency.
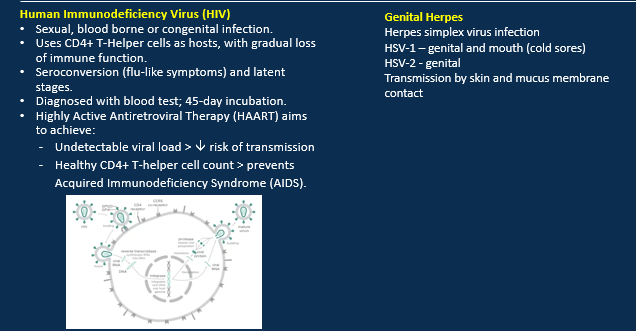
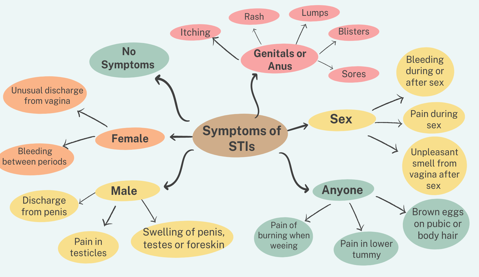
Symptoms of sexually transmitted infections (STIs)
Sexual health testing
•Home STI self-sampling kits available for routine and asymptomatic testing: blood, urine and swabs.
•If symptomatic or known exposure to an STI, sexual health or genitourinary medicine (GUM) clinics provide assessment and treatment.
•STI tests may not detect infection during the early incubation period.
•National Chlamydia Screening Programme – sexually active women and people with a womb or ovaries aged <25, annually or at change of partner.
•Human Papilloma Virus (HPV) surveillance during cervical screening for people with a cervix between 25-64 years old.
• Antenatal screening for Syphilis, HIV and Hepatitis B.
What are the different bacterial STIs

What are the viral STIs