GPHC Exam - Preliminary Chapters
1/235
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
236 Terms
What is the main route of elimination of drugs by the body
Metabolism by the liver
At what stage does the liver need to be in for there to be a dose reduction
Severe liver impairment due to the liver reserve being large
In elderly patients what type of drug has reduced hepatic metabolism
Lipid soluble drugs due to the reduction in liver volume
Important for drugs with a narrow therapeutic window
What is one of the products the liver is responsible for synthesising
Blood proteins such as albumin (most abundant protein in blood)
Give examples of drugs which are highly protein bound
NSAIDs
Phenytoin
Warfarin
Prednisolone
Which types of drugs do not exert their therapeutic effect
drugs which are highly protein bound - as when they are bound to blood proteins they are not biologically active and do not exert therapeutic effect they are just carried along in the blood
When unbound they are free drugs which can act on target tissues to exert their therapeutic effect
How can liver impairment affect highly protein bound drugs
In severe liver impairment, low albumin levels is associated with reduced protein binding of drugs and therefore is a higher concentration of free drug in the blood causing toxicity in drugs which are highly protein bound
What is the liver responsible for synthesising in the blood
The liver is responsible for the synthesis of blood clotting factors
How does liver impairment affect the blood
In liver impairment there is a reduction in blood clotting factors resulting in blood taking a longer time to clot which increases the risk of bleeding - indicated by high INR and prolonged prothrombin time
Increases the sensitivity to oral anticoagulants e.g. warfarin or drugs that have a side effect of bleeding e.g. NSAIDs
Why is fat soluble vitamins affected by liver impairment
In liver impairment there is fat malabsorption (difficulting in digesting or absorbing). This includes malabsorption of fat soluble vitamins --> vitmain A, D, E and K
What is the name of the water soluble version on vitamin K and why may it be given
Menadiol - this can be given to prevent Vitamin K deficiency in malabsorption syndrome characterized by inability to absorb fatty substances
Why is Vitamin K so important and can happen if there is a deficiency
Vitamin K helps the blood to clot
deficiency is associated with an increased risk of bleeding
When can there be a reduction in bile excretion
In intra-hepatic or extra - hepatic obstructive jaundice.
What is obstructive jaundice
Where essential flow of the bile to the intestine is blocked
Which drugs are excreted in the bile
Fusidic acid and rifampicin - these can accumulate in liver impairment
How can severe liver disease cause hepatic encephalopathy
Certain drugs can further impair cerebral function and precipitate into a hepatic coma called hepatic encephalopathy
What type of drugs in severe liver impairment can cause hepatic encephalopathy
- Constipating drugs e.g. Opioids, TCAs
- drugs that cause drowsiness or sedation as a side effect e.g. opioid analgesics sedating antihistamines, benzodaizepines, Z-drugs
Drugs that cause hypOKalaemia as a side effect e.g. loop and thiazide diuretics
How is hepatic encephalopathy treated
Osmotic laxative - lactulose
How is chronic liver disease categorised
By fluid overload - presents as oedema ( build up of fluid in the body causing affected tissue to become swollen) - oedema commonly occurs in the lower body in the ankles and lower legs
or as ascites ( build up of fluid in the lining of the abdomen known as the peritoneal cavity) - causes a swollen abdomen
What drugs can worsen oedema and ascites (fluid overload)
Drugs that have fluid retention as a side effect e.g. NSAIDs, Corticosteroids
What are the common signs and symptoms of hepatotoxicity
Jaundice (yellow skin and eyes)
Abdominal pain (upper right)
Nausea and vomiting
Malaise (feeling unwell)
Pruritus (Itching)
Dark Urine
Pale or clay - coloured stools
Drowsiness, confusion
Lab results with an increase in liver enzymes
What are the common hepatotoxic drugs
Alcohol
Amiodarone
carbamazepine
Co-amoxiclav
Fluconazole
flucloxacillin
Isoniazid
Itraconazole
Ketoconazole
Labetalol
Methotrexate
Paracetamol
Phenothiazines
pioglitazone
Rifampicin
Statins
Tolcapone
Tetracyclines
Valproate
Concurrent use of two or more of these drugs can increase the risk of hepatotoxicity
What drugs are enzymes inhibitors
SICK FACES COM
Sodium valproate
Isoniazid
Cimetidine
Ketconazole
Fluconazole
Alcohol (binge)
Chloramphenicol
Erthromycin
Sulphonamide
Ciprofloxacin
Omeprazole
Metronidazole
What drugs are enzymes Inducers
SCRAP GPS
Smoking
Carbamazepine
Rifampicin
Alcohol (chronic)
Phenytoin
St John's wort
Griseofulvin
Phenobarbital
Sulfonylurea
What effect does liver enzymes inhibitors have on metabolism
Drugs that are liver enzyme inhibitors decrease metabolism of other drugs which can increase plasma concentration of that drug leading to toxicity
What effect does liver enzymes inducers have on metabolism
Drugs that are liver enzymes inducers increase the metabolism of other drugs which can decrease the plasma concentration leading to sub-therapeutic effect
Why does grapefruit juice interact with drugs
Grapefruit juice contains CYP3A4 inhibitors which can increase the plasma concentration of drugs and cause possible toxicity
What are the common drugs that interact with grapefruit juice
CVS drugs - Amiodarone, dihydropyridine CCB, Statins, Verapamil, Dronedarone, Ranolazine
CNS drugs - Sertraline, Quetiapine
Immunosuppressants - Tacrolimus, Ciclosporin
Other drugs - Phosphodiesterase - type 5 inhibitors, Colchicine
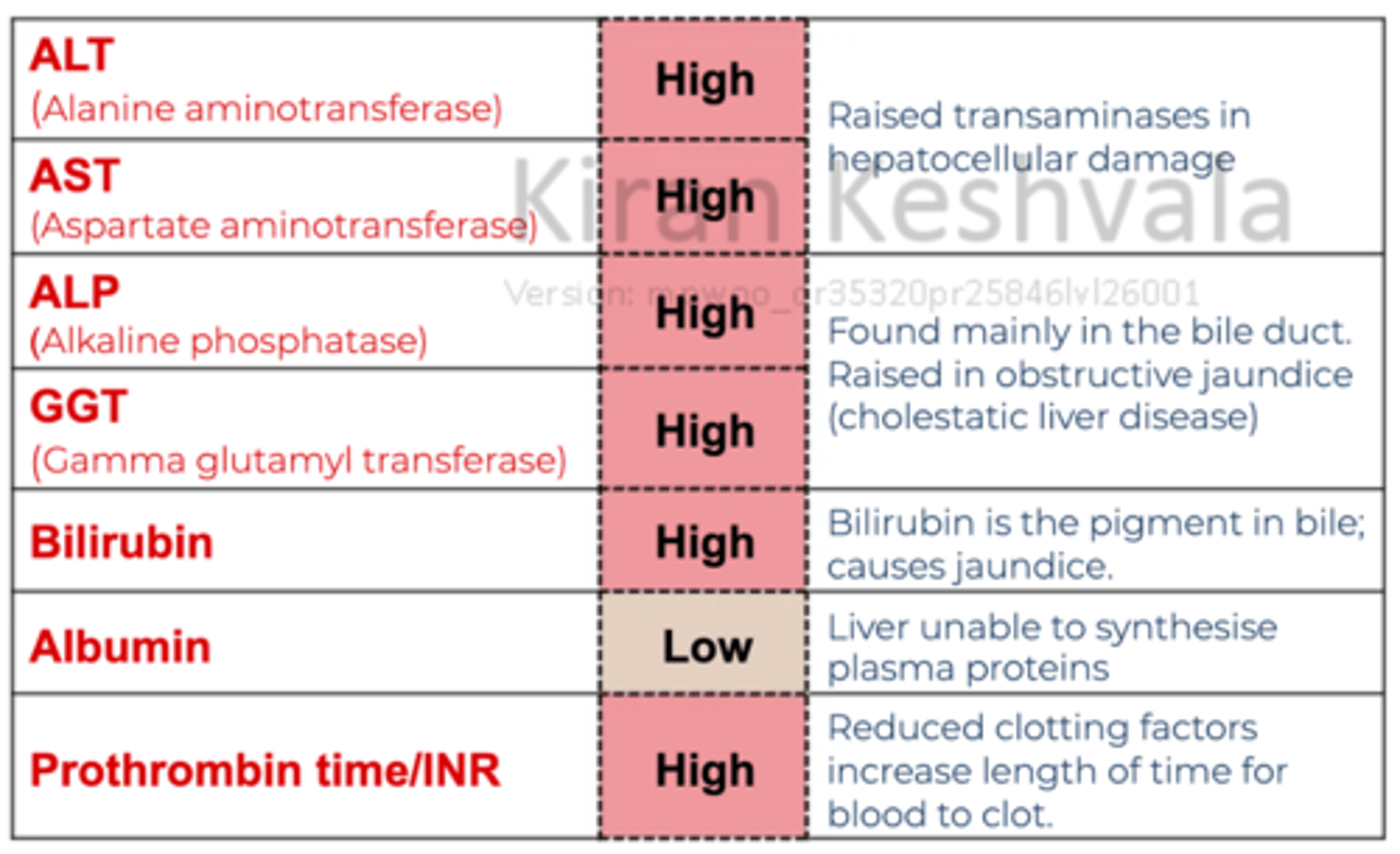
What are the lab test results in liver impairment
ALT - High
AST - High
ALP - High
GGT - High
Bilirubin - High
Albumin - Low
Prothrombin time/INR - High
How are drugs excreted from the body
By the kidneys, via urine
For this to happen effectively, the kidneys needs efficient glomelur filtration
What is glomelur filtration
It is the first step in making urine - process used by the kidneys to filter excess fluids and waste products out of the blood and into the urine collecting tubules to allow for elimination from the body
Why does renal impairment increase the risk of drug toxicity
In renal impairment there is reduced renal excretion of a drug or its metabolites which can give rise to toxicity
What precautions should be taken when prescribing medications to patients with renal impairment
Depending on the severity of renal impairment, dose reductions may be required
Renal function test should be done before prescribing any drug that requires a dose reduction or modification in renal impairment if even mild renal impairment is suspected
How can the total maintenance doses be reduced in renal impairment
Maintenance doses can be reduced by either reducing the size of the individual dose OR by increasing the intervals between the doses
How should dosing in renal impairment be managed for narrow therapeutic index drugs
Recommended regimens should be regarded only as a guide to initial treatment, subsequent doses should be adjusted according to the clinical response and the monitoring of plasma drug concentration
List other problems that occur in renal impairment
Increased sensitivity to some drugs - even if elimination is not impaired
Many side effects are poorly tolerated
Some drugs are not effective when renal function is reduced e.g. thiazides - as they rely on efficient glomerular filtration
How can these problems that occur in renal impairment be solved
By either dose reductions
By using an alternative drug
Why might a loading dose be necessary for some drugs in patients with renal impairment, even if the maintenance dose is reduced
In some drugs, although the maintenance dose will be reduced it is important to give a loading dose if an immediate effect is required. This is because the plasma half life of drugs excreted by the kidneys is prolonged in renal impairment and take about FIVE times the normal half life of the normal drug to reach steady state plasma concentrations
What is a loading dose
Initial higher dose of a long acting drug which is given at the beginning of a course of treatment in order to quickly achieve therapeutic plasma concentration
How does renal function change with age?
Renal function declines with age.
What should be assumed when prescribing for the elderly?
At least some degree of mild renal impairment should be assumed.
The elderly excrete drugs slowly and are highly susceptible to nephrotoxic drugs
What is a significant risk factor for Acute Kidney Injury (AKI)
Dehydration
During intercurrent illness, what is there an increased risk of
During intercurrent illness there is an increased risk of AKI particularly in patient with an eGFR < 60ml/min
What should be considered for potentially nephrotoxic or renally excreted drugs in patients with renal impairment
Potentially nephrotoxic or renally excreted drugs may require a dose reduction or temporary discontinuation
What are the sick day rules in terms of drugs
They are a list of drugs that should be temporarily stopped during ANY illness that can result in dehydrations.
List the drugs that should be stopped due to sick day rules
DAMN
DIURETICS (exacerbates dehydration; electrolyte imbalance)
ACE INHIBITORs/ARBs (nephrotoxic and reduces eGFR)
METFORMIN (increased risk of lactic acidosis in RI)
NSAIDs (nephrotoxic and reduces eGFR)
When should DAMN drugs usually be restarted
Restarted 24-48 hours after normal eating and drinking
According to NHS scotland cards, when do sick day rules apply
When you are unwell with any of the following:
- Vomiting or diarrhoea (unless only minor)
-Fevers, sweats and shaking
What are the signs and symptoms of AKI
Reduced Urine output
Nausea and vomiting
Confusion and drowsiness
Abdominal pain
Fatigue
Lab results: Reduced eGFR and CrCl
Increase in serum creatinine
List the Common Nephrotoxic drugs
ACEi/ARBs
Aciclovir
Aminoglycosides
Aminosalicylates
Amphotericin
Ciclosporin
Cyclophosphamide
Glycopeptides
Lithium
Methotrexate
NSAIDs
Tacrolimus
Trimethoprim
Why should nephrotoxic drugs be avoided in patients with renal disease
Nephrotoxic drugs should be, if possible, avoided in patients with renal disease as the consequences of nephrotoxicity are likely to be more serious when renal reserve is already reduced
What is the MHRA/CHM advice given in 2019 for renal function test
Use the appropriate estimate of renal function to avoid the risk of adverse drug reactions
What is the prefered formular for renal function test
COCKCROFT-GAULT FORMULA
((140-age) x constant x weight)/serum creatine
constant: Male 1.23 female 1.04
When should the ideal body weight be used to calculate the creatinine clearance
where fat is likely to be the major contributor to body mass
BMI >40
Why is creatinine used to estimate renal function
Creatinine is a substance used by the body at a fairly constant rate.
It is excreted unchanged by the kidneys via glomerular filtration
How does serum creatinine indicates renal function
If filtration in the kidney is deficient, serum creatinine rises
Higher the serum creatinine is the greater the degree of renal impairment
The greater the volume of creatinine cleared per minute the better kidney function
How is Chronic kidney disease categorised
Using a combination of GFR and albumin:creatinine ratio (ACR)
What is the significance of decreased GFR and increased ACR in assessing kidney function.
Decreased GFR and an Increased ACR is associated with an increased risk of adverse outcomes.
E.g. if a patient has an eGFR of 14 ml/min and an ACR of 15 mg/mol the patient has a CKD classification of G4 A2 which is severe renal impairment
What is the cautionary and advisory label for drugs that colour Urine
'This medicine may colour your urine. This is harmless
What drugs colour your urine RED
Dantron e.g. Co-danthrusate
Doxorubicin
Levodopa (dark - red bodily secretions)
What drugs colour your urine YELLOW - BROWN
Nitrofurantoin
Senna
What drugs colour your urine PINK/ORANGE
Phenindione
What drugs colour your urine BLUE
Triamterene
What drugs colour your urine ORANGE
Rifampicin (also colour bodily secretion such as tears which can stain contact lenses)
Sulfasalazine (bodily secretion - same as above)
What can prostaglandin analogues cause
Irreversible brown pigmentation of the iris
What can happen to stool when taking Iron
Colour the stools a tarry colour
What is the pain management oral drug of choice
Morphine (CD 2)
(Morphine with an oral strength below 13mg/5ml is a CD 5)
Alternative choice: Oxycodone
What is the typical dose of oral morphine in pain management
Immediate - release: 30mg 4 hourly
Modified release: 100mg 12 hourly, 24 hourly
(when pain is stable: switch from immediate - release <4 hours of last dose)
What is the max dose increments of morphine
1/3 or 1/2 of total daily dose every 24 hours
When is parenteral opioids given
When the patient is unable to take opioids by mouth
e.g. Difficulty swallowing, Severely weak, experience severe N&V or in a coma
What is the parental dose of morphine
Morphine (IV, IM, SC) - 1/2 oral dose
Diamorphine (IV, IM, SC) = 1/3 oral dose - more soluble so larger dose given in smaller volume - this avoids fluid overloading the patient - preferred way
What is the recommended concentration for SC Diamorphine, and why should saline be used instead of water for injection above 40mg/ml?
SC Diamorphine can be given up to a strength of 250mg/ml with physiological saline or water for injection
Above 40mg/ml water for injection should only be used as saline can cause precipitation
Which opioids can be given rectally
Morphine
Oxycodone
Why are transdermal opioids given
Chronic Pain stabilised on an immediate release opioid dose
What are the two transdermal preparation of opioids
Fentanyl Patches (72 - hourly)
Buprenorphine patch (72 hourly, 4 - day/7 day)
Not suitable for people in acute pain or rapid changing pain levels
When aren't transdermal patches suitable
Transdermal patches are slow release preparations which take a long time to reach steady state plasma level. This means they do not provide fast pain relief and doses CAN NOT be rapidly titrated to match rapidly changing pain levels
When can immediate release morphine be given with transdermal patches
As breakthrough pain
When switching a patient to opioid patches due to possible opioid-induced hyperalgesia, how should the equivalent dose of the new opioid be adjusted
The equivalent dose of the new opioid is reduced by 1/4 to 1/2.
What is opioid induced hyperalgesia
Condition where long term opioid use can cause the patient to become more sensitive to pain
What is breakthrough pain
Pain that occurs between regular doses of a strong opioid such as morphine is known as breakthrough pain
What are rescue doses
When breakthrough pain occurs, additional doses known as 'rescue doses' of IMMEDIATE RELEASE preparation is given
What are the common opioids used for breakthrough pain and why
Oral morphine solution or oxycodone oral solution is given as they are more flexible in providing various fractions of doses as opposed to a fixed dose tablet or capsule
What medication is unlicensed to use for breakthrough pain
Fentanyl - Buccal, sublingual or nasal preparations can be given as unlicensed rescue doses for breakthrough pain
How long before a painful activity should rescue doses be given and give an example of such activity
30 MINUTES before e.g wound dressing
What is the standard dose for breakthrough pain
1/10th - 1/6th of the total daily dose every 2 - 4 hours as required
Can be up to hourly if pain is severe or in the last days of life
When does pain management need to be reviewed
If a patient is taking breakthrough doses frequently - twice daily or more - their pain management needs to be reviewed
What is a one of the most common side effect of opioids
Opioid - induced Constipation
What is the treatment for opioid induced constipation
Treated with a fecal soften laxative and a peristaltic stimulant laxative
Lactulose + senna
Give another example of a laxative that can be used in opioid induced constipation and explain why it is used only in terminally ill patients
Co-danthramer OR Co-danthrusate - contain a combination of a fecal soften and a stimulant laxative dantrone
dantrone is carcinogenic so reserved only to be used in terminal ill patients
What is Methylnaltrexone used for in the context of opioid-induced constipation
Methylnaltrexone is an opioid receptor antagonist which is licensed to be used in opioid induced constipation if other laxatives are inadequate
When does the opioid induced side effect nausea and vomiting occur
Usually at the start of therapy of strong opioids however most patients build a tolerance to it
What drug treatment can be given for opioid induced N&V side effect and for how long
Prokinetic anti-emetic can be co-prescribed for initial opioid induced N&V treatment for 4-5 days. e.g. metoclopramide
Alternatively the antipsychotics Haloperidol can be given
What is another common side effect of opioids
Dry Mouth
How can you counsel a patient who is experiencing dry mouth due to opioids
Maintain good oral hygiene
Can suck on ice cubes or pineapple chunks, chew sugar free gum can help moisten the mouth or use artificial saliva
What can dry mouth be associated with
Oral candidiasis
This can be treated with Antifungal treatment - nystatin, miconazole, fluconazole
According to the WHO analgesic ladder, what can be used for pain due to bone metastases
radiotherapy, bisphosphonates and strontium
What drug treatment can be given to patients with Neuropathic pain
A trial of tricyclic antidepressant such as amitriptyline.
Anti-epileptics can be added or substituted if pain persists - gabapentin and pregabalin are licensed for neuropathic pain
Ketamine can be used under specialist supervision if poor response to opioids
What drug treatment can be given to pain due to nerve compression e.g. by a tumour pressing on a nerve
Treated by a corticosteroid e.g. Dexamethasone which via its anti inflammatory action reduces the oedema around the tumour thus reducing compression
At age are patients considered to be elderly
Aged 65 and over
When prescribing in the elderly what should be considered
Dosage should be substantially lower compared to younger patient
Common to start with about 50% of the adult dose
Some drugs should be avoided all together - long acting sulfonylurea and benzodiazepines