16 - Female reproduction
1/17
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
18 Terms
Ovaries
female gonad. Production of gametes. Covered in simple cuboidal germinal ET.
Tunica albuginea: thin Dense irregular CT deep to germinal ET.
Ovum development and release 1
FSH makes primary oocytes enlarge. The follicle cells become stratified Cuboidal granulosa cells around oocyte. This is the multilaminar primary follicle. Zona pelicuda forms between PO and granulosa cells Theca interna is a vascular cell layer of stroma external to basal lamina. Theca externa: fibrous outer layer of stroma, smooth muscle cells that contract during ovulation
Ovum development and release 2
Secondary follicle formation. Granulosa cells continue to proliferate in inner layer. Antrum forms intercellular space fills with follicular fluid. Cumulus oophorus forms, mound of multiplied granulosa cells Layers of cells left surrounding oocyte is corona radiata.
Ovum development and release 3
only one develops into mature Graafian follicle Primary oocyte detaches and floats in follicular fluid. Continued meiosis forms secondary oocyte and 1st polar body. Follicle ruptures and releases ovum into infundibulum of uterine tube.
Events after ovum release
Corpus hemorrhagicum: follicle cells fold in under influence of LH, antrum fills with blood
Corpus luteum
Granulosa lutein cells: large, pale-staining; derived from granulosa cells; secrete progesterone, estrogens, and inhibin.
Theca lutein cells: smaller, fewer in number, darker-staining than granulosa lutein cells; derived from theca interna cells; produce progesterone and estrogen precursor
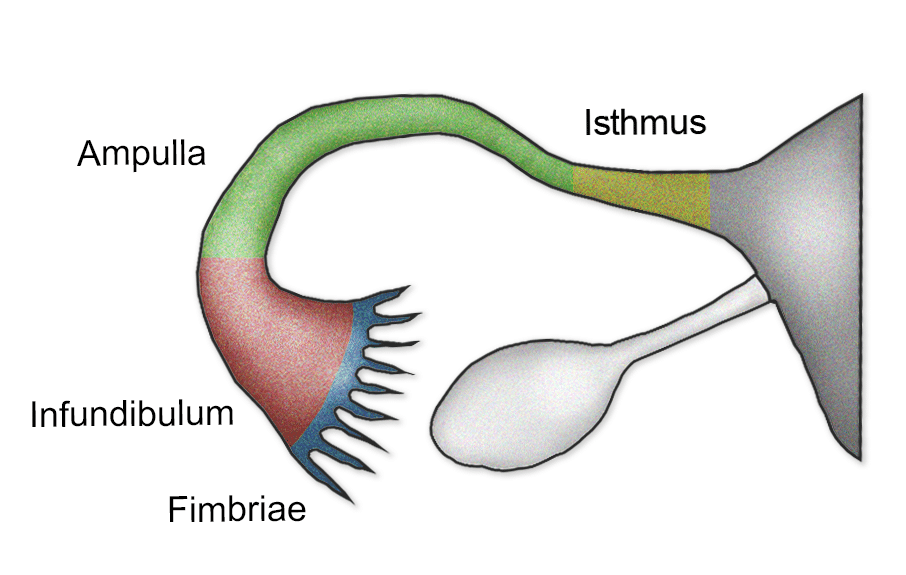
Uterine/Fallopian tube
4 segments. Infundibulum
ampulla(site of fertilization)
isthmus, intramural region
Mucosa: ciliated cells and Peg cells(nonciliated secretory)
Uterus
3 layers superficial to deep: Perimetrium, Myometrium, Endometrium
Body: major portion
Fundus: Superior to entry of uterine tubes
Cervix: Cylindrical portion that projects into vagina.
Endometrium
site of blastocyst implantation during pregnancy.
Endometrium: Proliferative/Follicular phase
glands respond to estrogen, elongating and coiling
Endometrium: Secretory/Luteal phase
Begins after ovulation, thickens endometrium to prepare for possible pregnancy
Endometrium: Menstruation
resets the system if not pregnancy occurs.
Uterus: Cervix
Endocervical canal lind by simple columnar ET. Ectocervix lined with Strat.SET. Myometrium replaced with elastic CT.
Vagina
Mucosa Lined with nkStSET. Muscularis composed of inner circular layers and outer longitudinal smooth muscle layers. Adventitia/Serosa is dense fibrous CT. No glands, lubrication comes from lamina propria and cervical glands. The squamous ET is glycogenated which makes them more spherical than other SqET. This is a distinct feather of vaginal SqET.
Labia majora
Resembles typical skin, adipose, hair follicles, apocrine glands, sebaceous glands.
Labia minora
no hair follicles, no adipose tissue, some sweat/sebaceous glands, but no apocrine. Many nerve fibers.
Clitoris
erectile tissue, nerve endings.
Mammary glands
Glands are compound tubuloaveolar glands. 15-20 lobules radiate out from the nipple. Lobes are drained by their own lactiferous duct. Each duct is dilated to form a lactiferous sinus for milk storage.
Colostrum
initial secretion from mammary glands before milk. Stimulates the GI tract. Concentrated and low fat in humans. After a couple days, prolactin is secreted which has higher fat content