Lecture 22. GI Infections 3
1/37
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
38 Terms
Campylobacter jejuni etiology
1. Gram-negative, gull-wing or S-shaped rod
2. microaerophilic (5% O₂, 10% CO₂); grows at 42°C.
C. jejuni
what bacteria is indicated by this image and is associated with hemorrhagic enterocolitis
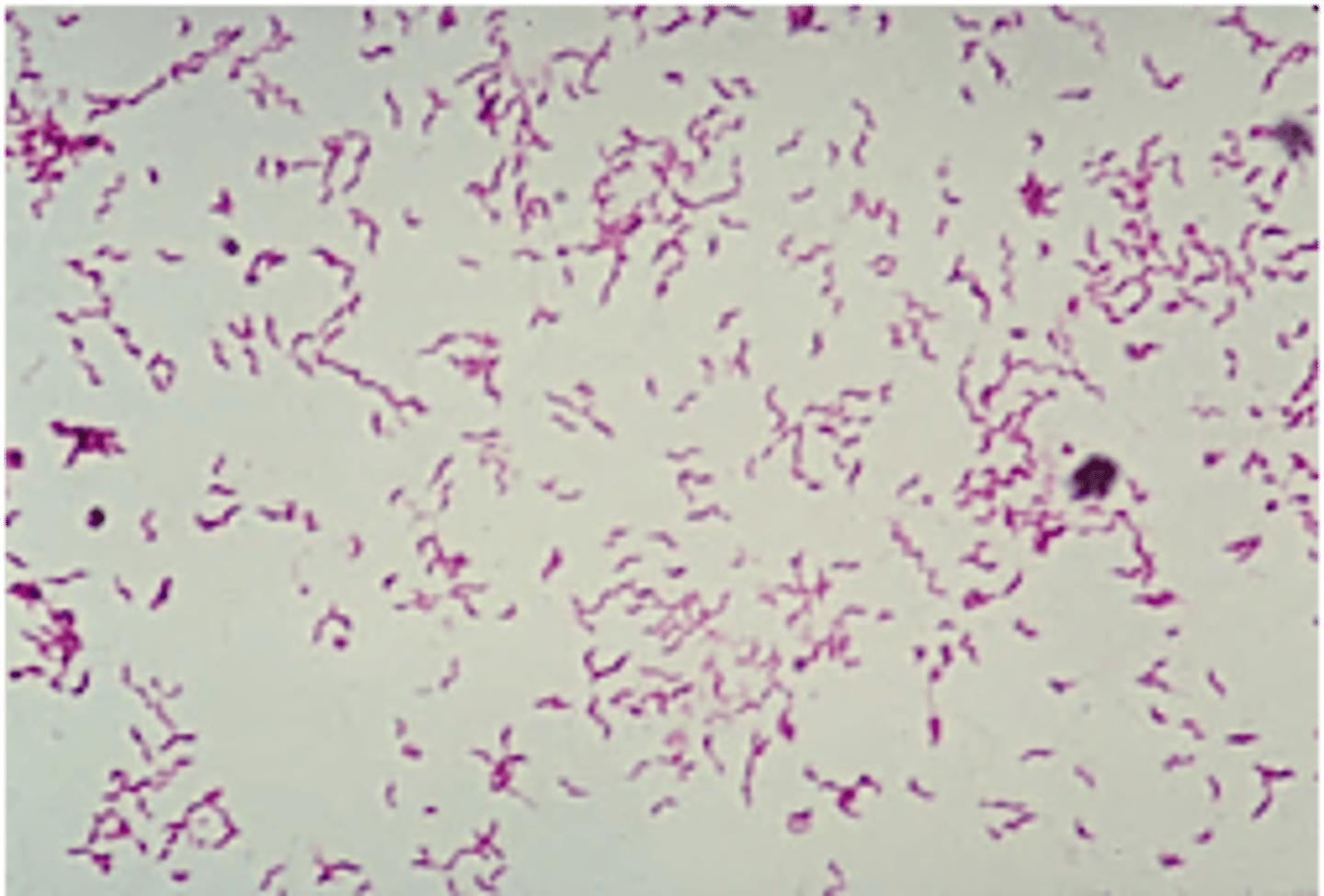
Transmission of Campylobacter jejuni
Fecal-oral route from inapparent carriers, milk, or frozen chicken.
Factors increasing spread of Campylobacter jejuni
Poor immune status and concurrent infections (e.g., parvo, salmonella, corona).
Main virulence factors of Campylobacter jejuni
1. Cytolethal distending toxin (CDT) - destroys villi and induces inflammation
2. adhesions- attach to mucosal epi cells
Clinical signs of Campylobacter jejuni
Hemorrhagic enterocolitis, bacteremia, fever, diarrhea;
what bacteria is associated with hemorrhagic enterocolitis
C. jejuni
who is primarily infected with C. jejuni
mainly affects animals <6 months old.
Diagnosis of Campylobacter jejuni
1. History, clinical signs
2. direct fecal exam
3. microaerophilic fecal culture.
what is revealed on dark field fecal exam that points to C. jejuni
darting motility
Primary treatment for Campylobacter jejuni infection
1. Fluid therapy
2. erythromycin (efficacy unknown).
Prevention of Campylobacter jejuni
Sanitation.
Clostridium perfringens morphology
Gram-positive, obligate anaerobic rod; forms spores and exotoxins.
C. perfringens
this bacteria is associated with hemorrhagic enterotoxemia
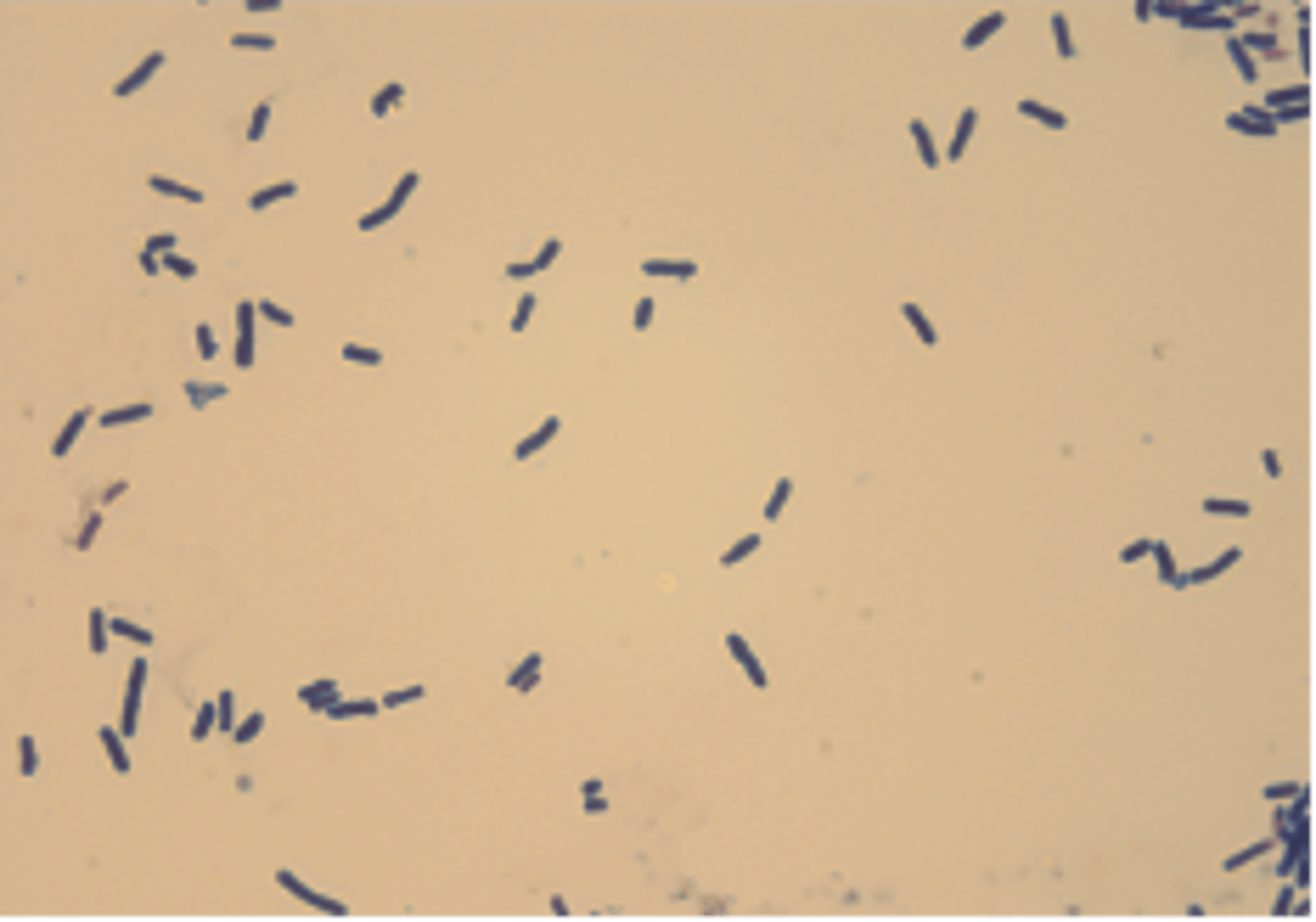
C. perfringens type associated with hemorrhagic enterotoxemia
Type C - produces alpha and beta toxins.
Predisposing factors for C. perfringens infection
1. High-energy diets
2. reduced peristalsis
3. antibiotic disruption of flora,
4. low trypsin in neonates.
transmission of C. perfringens
fecal-oral
what exotoxins are associated with type A clostridium
alpha
what exotoxins are associated with type B clostridium
alpha, beta, epsilon
what exotoxins are associated with type C clostridium
alpha, beta
what exotoxins are associated with type D clostridium
alpha, epsilon
what exotoxins are associated with type E clostridium
alpha, lota
how does C. perfringens type C cause disease
damage intestinal microvilli and lead to damage of leukocytes, platelets, and RBCs
Common clinical signs of clostridial diarrhea
Sudden death, ADR, colic, abdominal pain, brown/bloody diarrhea, high mortality (50-100%).
Diagnosis of C. perfringens
1. History, clinical signs
2. necropsy (intestinal lesions)
3. anaerobic culture
4. toxin neutralization test.
what test is confirmatory for C. perfringens
toxin neutralization test (but not all produce toxins)
Treatment for C. perfringens infection
1. C-type antitoxin
2. antibiotics (metronidazole or penicillin)
3. supportive fluids and electrolytes.
Prevention of C. perfringens infection
Colostrum antibodies, vaccinating dams (multivalent vaccine), and sanitation.
Cause of CDAD (Clostridium Difficile Associated Diarrhea)
Clostridium difficile.
Major toxins produced by C. difficile
1. Toxin A (enterotoxin - fluid secretion)
2. Toxin B (cytotoxin - epithelial necrosis).
Pathogenesis of C. difficile
1. Causes pseudomembranous colitis in humans
2. acute necrotizing enterocolitis in animals.
Diagnosis of C. difficile
Detection of toxins in feces via cytotoxin test (toxin B), ELISA, or PCR (toxin genes)
Treatment for C. difficile infection
Tylosin, fluid therapy, sanitation.
C. difficile
the disease state seen is this equine is associated w/ what pathogen
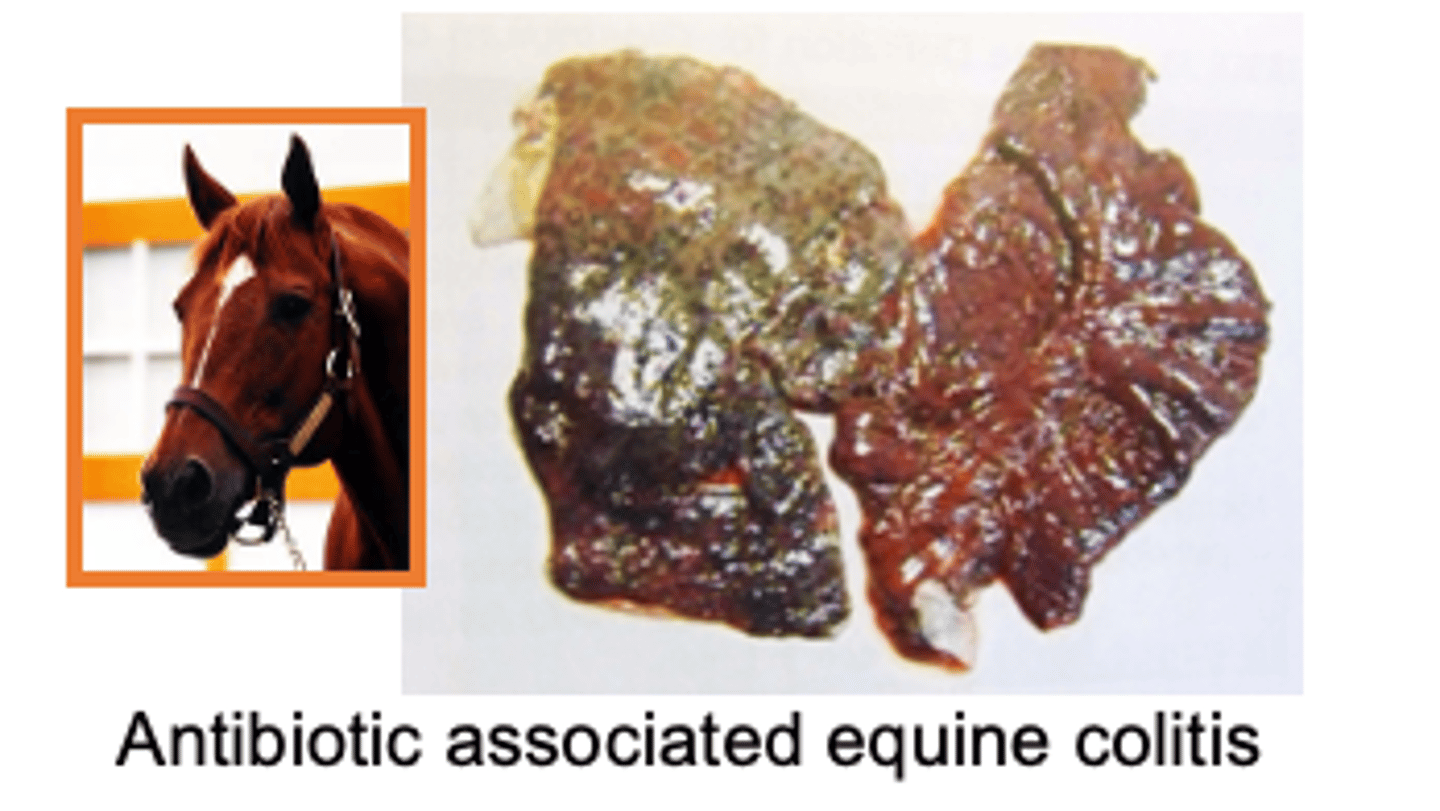
Clinical syndromes associated with C. perfringens type A
1. Necrotic enteritis in chickens, suckling pigs
2. yellow lamb disease
C. perfringens type A
the disease state in this pig is associated with what pathogen
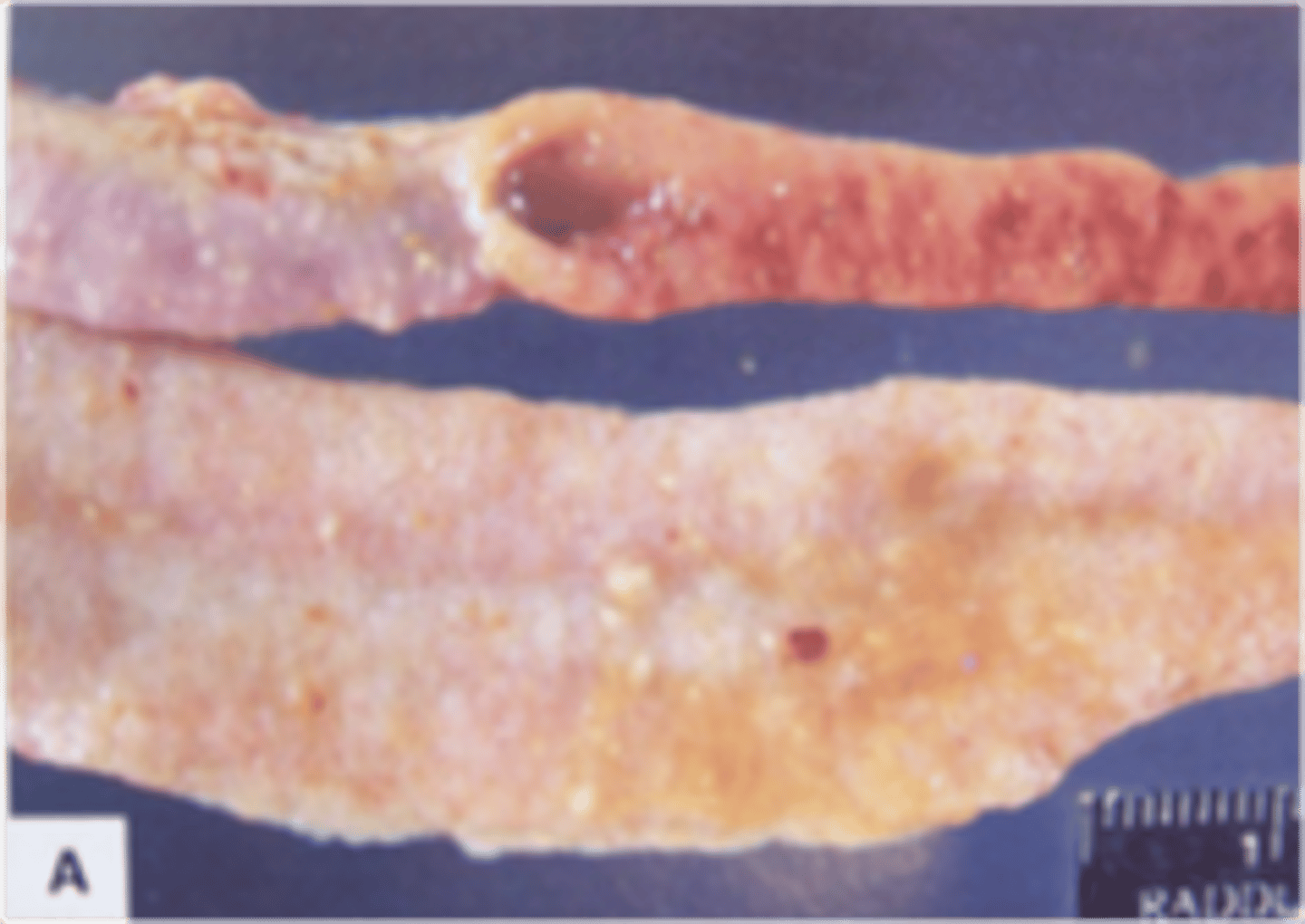
Clinical syndromes associated with C. perfringens type B
1. hemorrhagic enteritis
2. lamb dysentery (Europe, South Africa).
Condition caused by C. perfringens type D
"Overeating disease" and enterotoxemia in lambs - causes diarrhea and nervous signs.