SSI: practice questions (week 12)
1/60
Earn XP
Description and Tags
focal + multifocal alopecia, pruritic diseases, erosions/ulcers/crusting diseases (feline dermatoses)
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
61 Terms
What anti-pruritic medication approved in cats has the fastest onset of action?
Prednisolone → a few hours
What is the primary pruritogenic cytokine that is a key target for some anti-pruritic medications?
IL-31
What anti-pruritic medication can be used in young dogs (<1 year of age) to provide relief of itch by reducing the amount of circulating IL-31?
Lokivetmab (Cytopoint) → monoclonal antibodies
Which antipruritic medications are contraindicated in dogs with neoplasia, demodicoses, or deep infection?
Prednisone (never in demodex) + JAK inhibitors (Apoquel/Oclacitinib)
Which antipruritic medication’s side effects can potentially be reduced by keeping the capsules in the freezer & administering the medication while frozen?
Cyclosporine
What are the two major classes of alopecia?
Which layers of the skin do surface pyodermas reach into?
Upper layers of epidermis
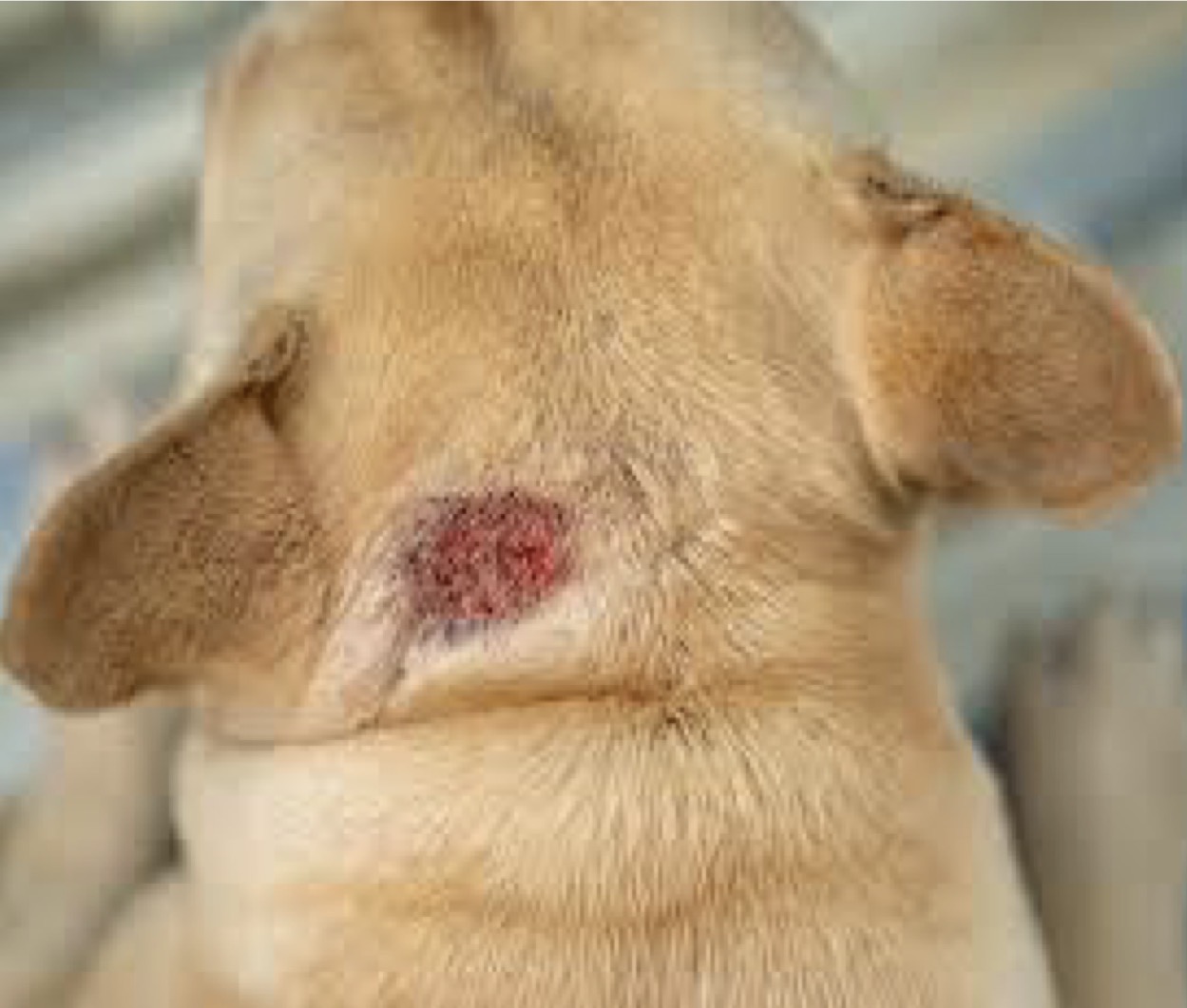
Which form of surface pyoderma presents rapidly as exudative, pruritic, erythematous, & painful spots on localized areas of the body (cheek, neck, thigh, rump), often from self-trauma due to underlying pruritus or pain?
Pyotraumatic dermatitis (“hot spot”)
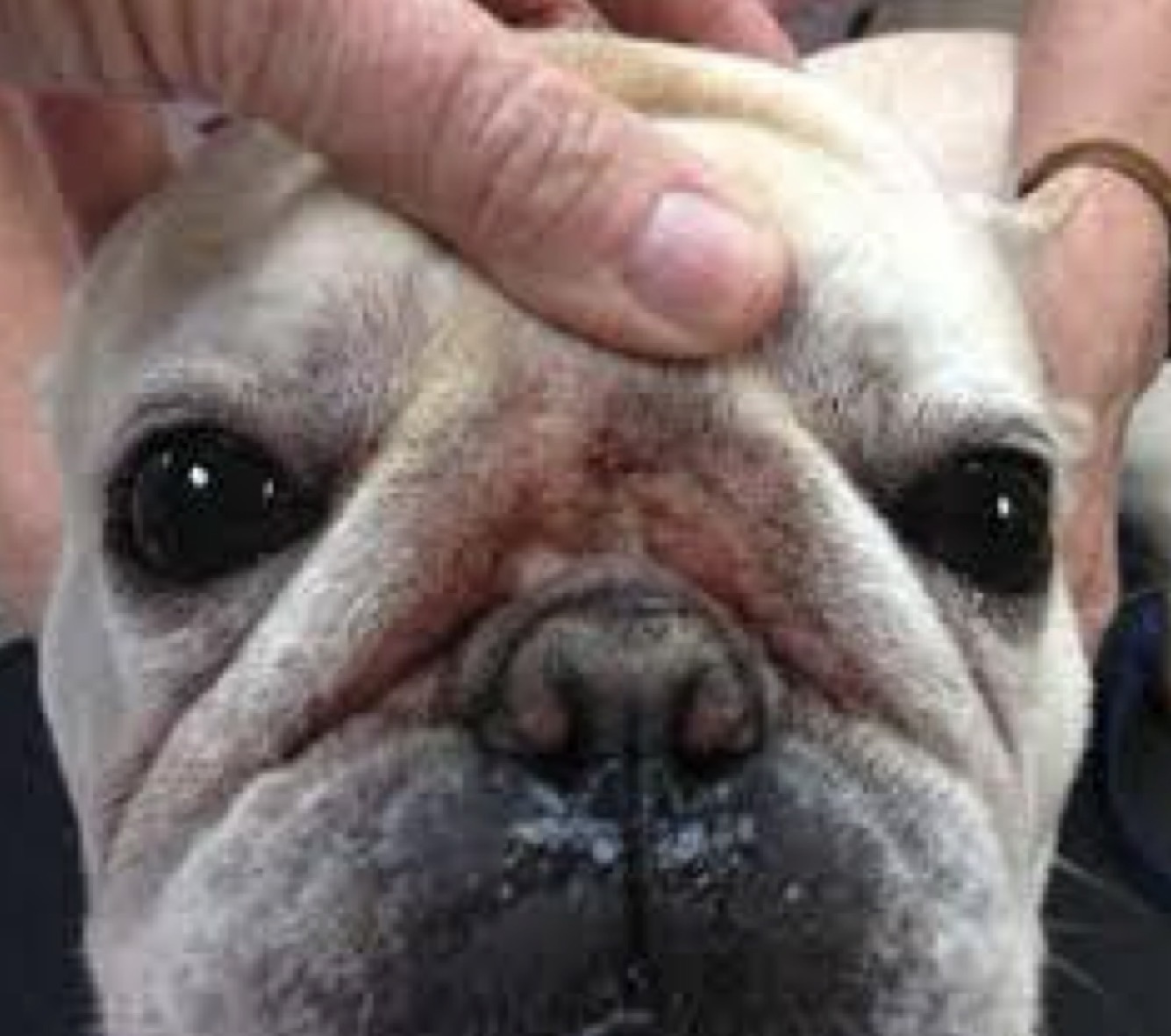
Which form of surface pyoderma presents in breeds such as Bulldogs, Boston terriers, Shar-Peis. Pugs, Mastiffs, etc., as erythematous, exudative, malodorous lesions in the facial, lip, vulvar, & tail folds?
Intertrigo (Skin Fold Dermatitis)
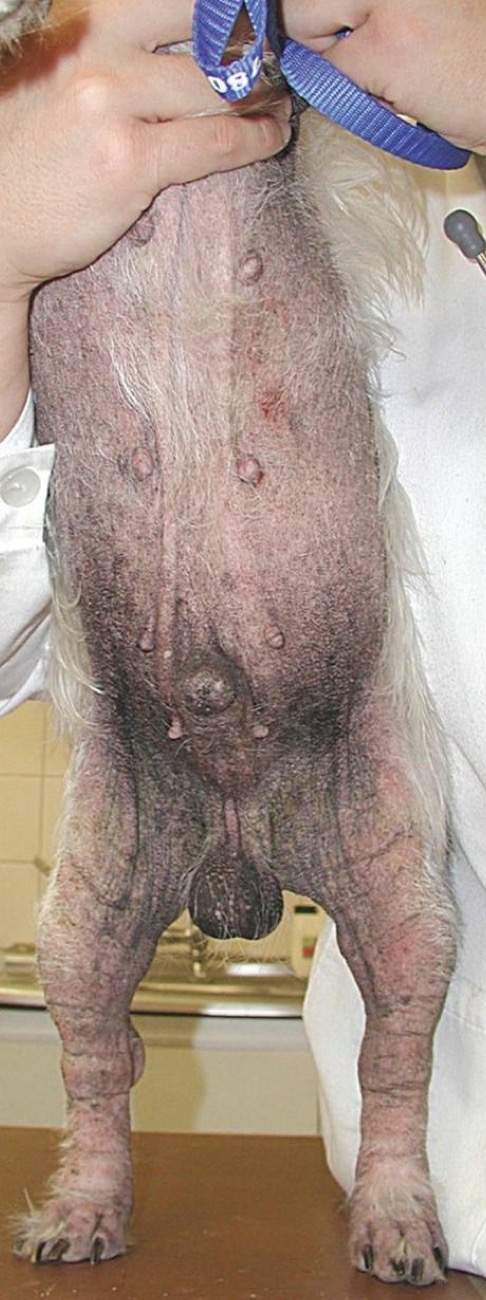
Which form of surface pyoderma presents as erythematous, exudative, lichenified, hyperpigmented areas on the ventral abdomen, interdigital spaces, & ear pinnae?
Bacterial Overgrowth Syndrome
What will you see on cytology in a patient with pyotraumatic dermatitis or intertrigo (surface pyodermas)?
Cocci ± neutrophils
What will you see on cytology in a patient with bacterial overgrowth syndrome?
Lots of bacteria without neutrophils (no inflammation present)
What is the recommended treatment for surface pyodermas in small animals?
-Topical antiseptics → chlorhex products, benzoyl peroxide, salicylic acid, sodium hypochlorite (dilute bleach), or bacitracin ointment for localized lesions
-Anti-inflammatory → topical glucocorticoids or short course of systemic glucocorticoids (5-7 days)
-address underlying cause
How does Photobiomodulation (PBM) work to decrease healing time in skin conditions?
Stimulates mitochondria + increases growth factors (EGF, VEGF, FGF) needed for healing → decreases inflammation in epidermis + dermis, promotes angiogenesis, increases collagen production
-do NOT use in neoplasia
Which layers of the skin do superficial pyodermas reach into?
Epidermis + hair follicles
What is the most common form of superficial pyoderma, leading to follicular papules, pustules, epidermal collarettes, & a “moth-eaten” focal alopecia appearance on the ventral abdomen or medial thighs?
Superficial Bacterial Folliculitis (SBF)
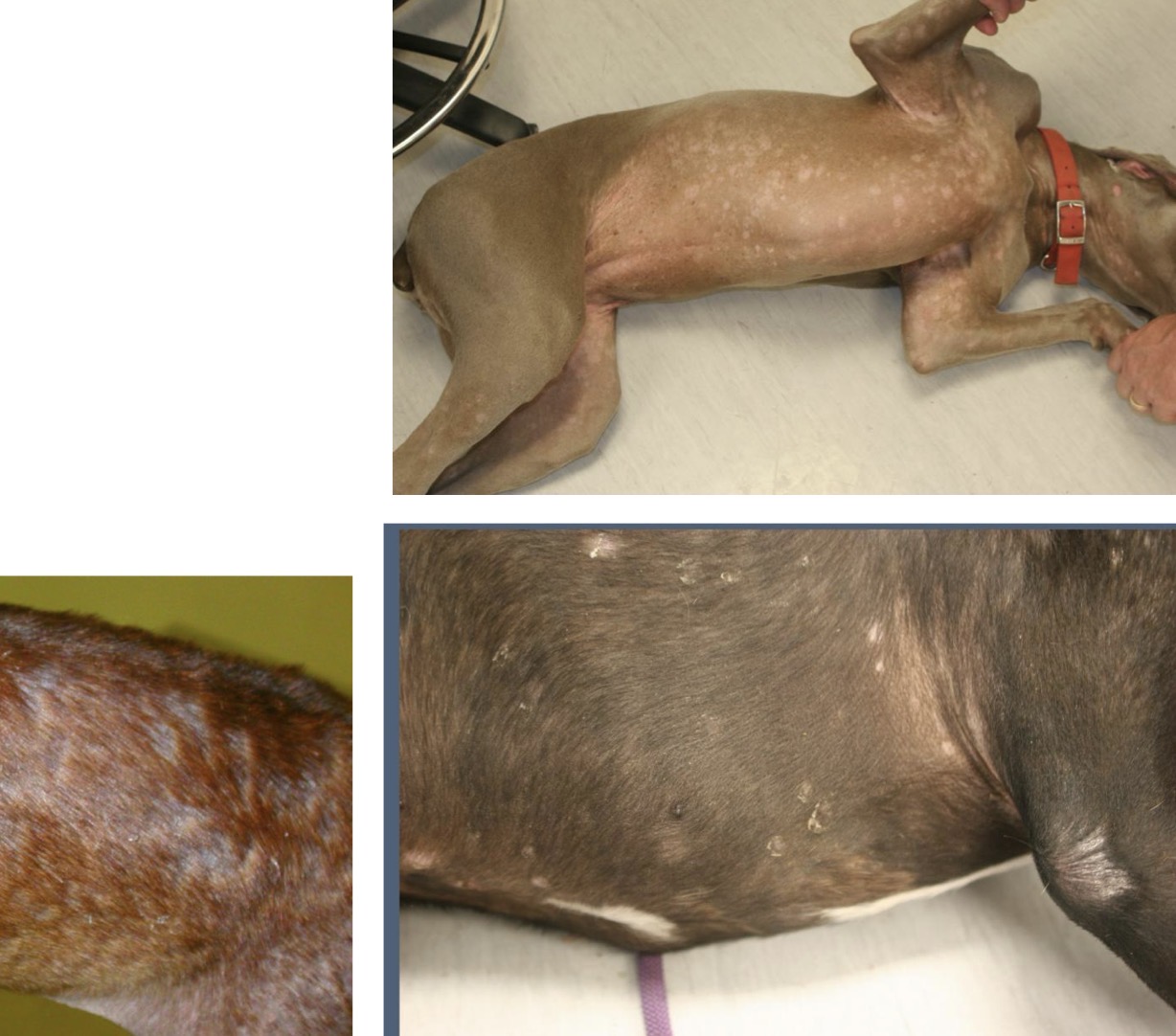
Which form of superficial pyoderma appears as large, expansile epidermal collarettes with an erythematous rim (target lesion appearance)?
Exfoliative Superficial Pyoderma
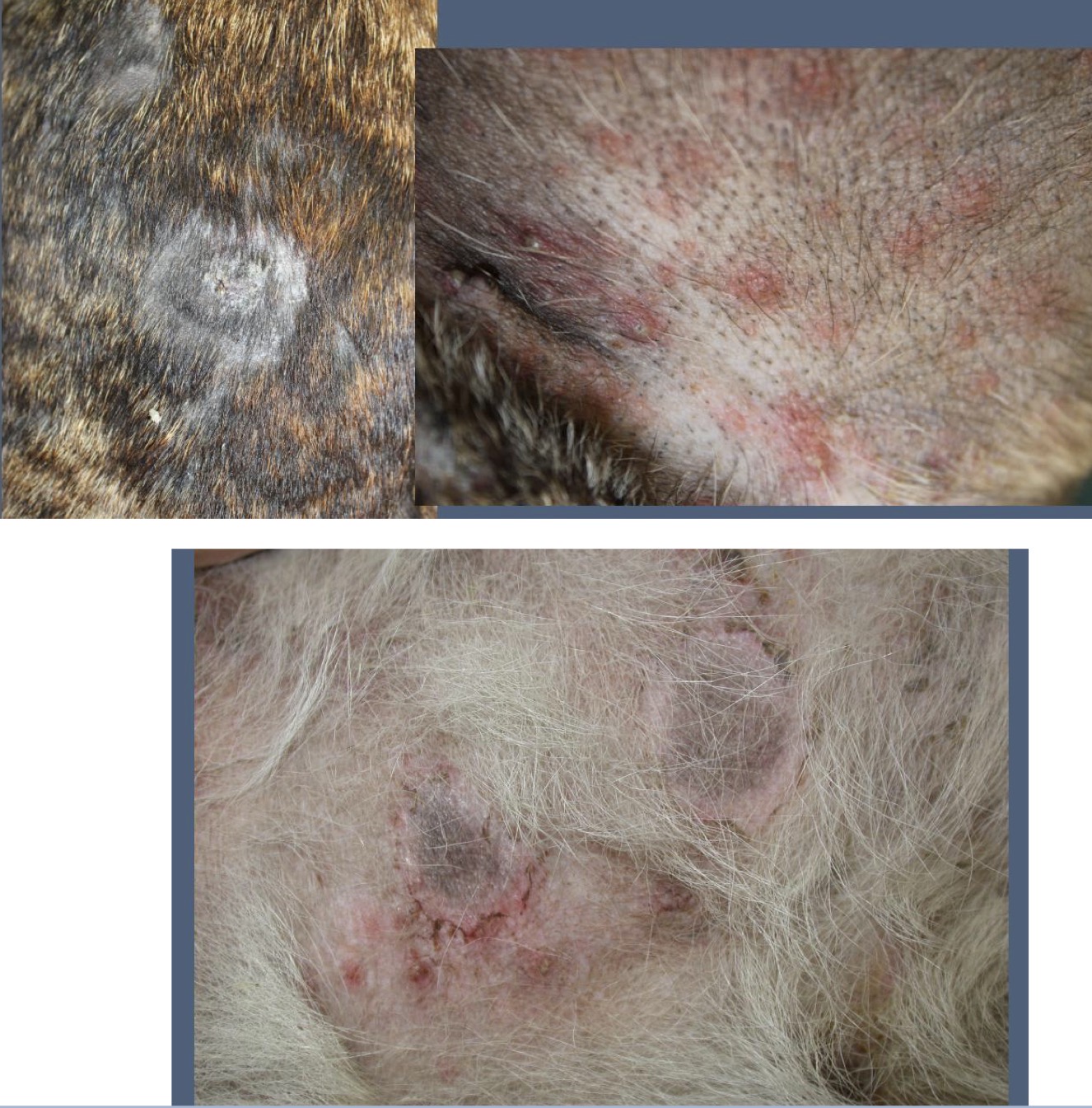
Which form of superficial pyoderma appears as non-follicular pustules in young dogs (puppy pyoderma) around the inguinal + axillary regions or as larger lesions in immunocompromised adults?
Impetigo
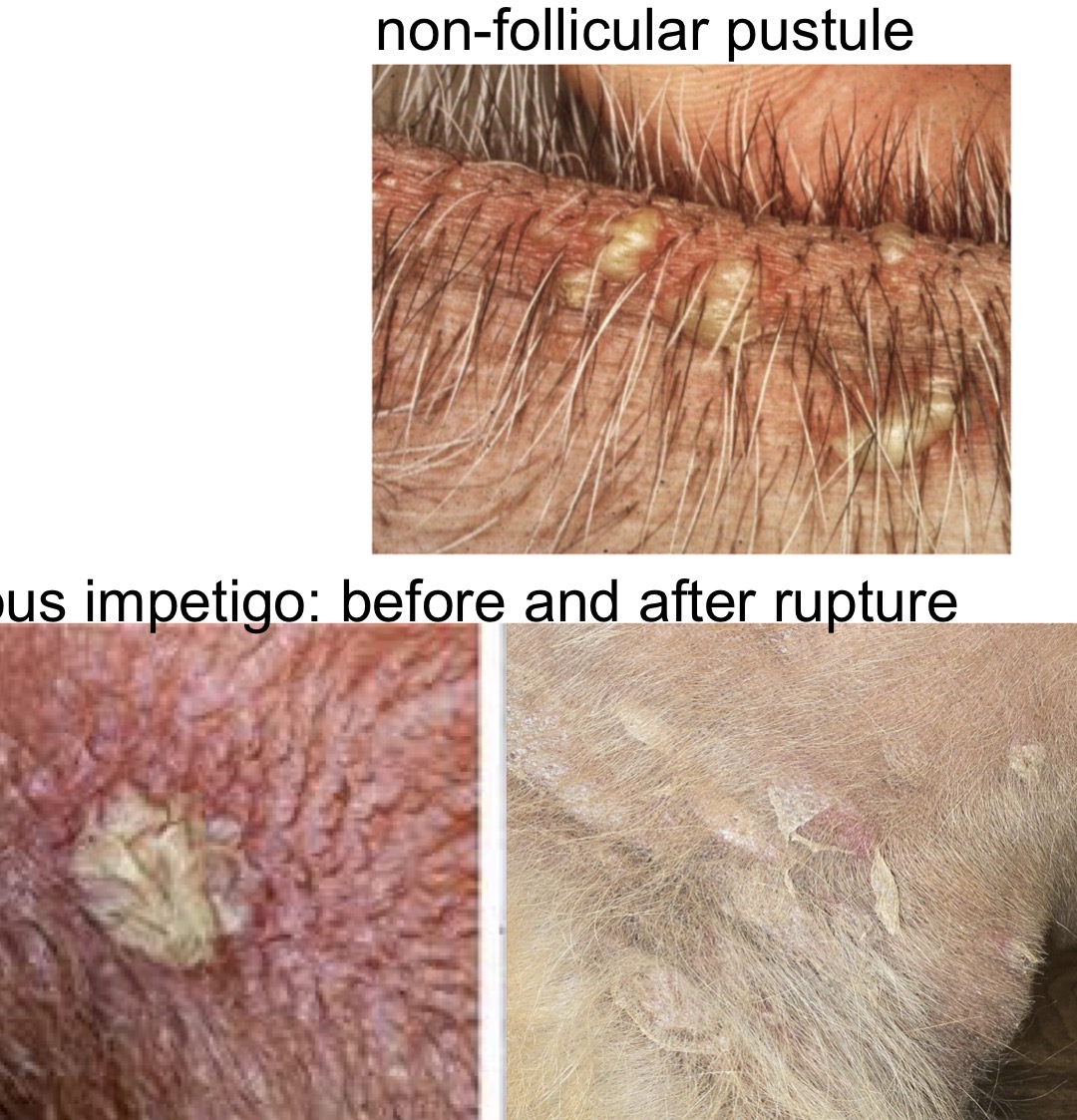
Which form of superficial pyoderma appears as erythematous, erosive crusts at mucocutaneous junctions (oral, nasal, ocular, or private regions)?
Mucocutaneous Pyoderma
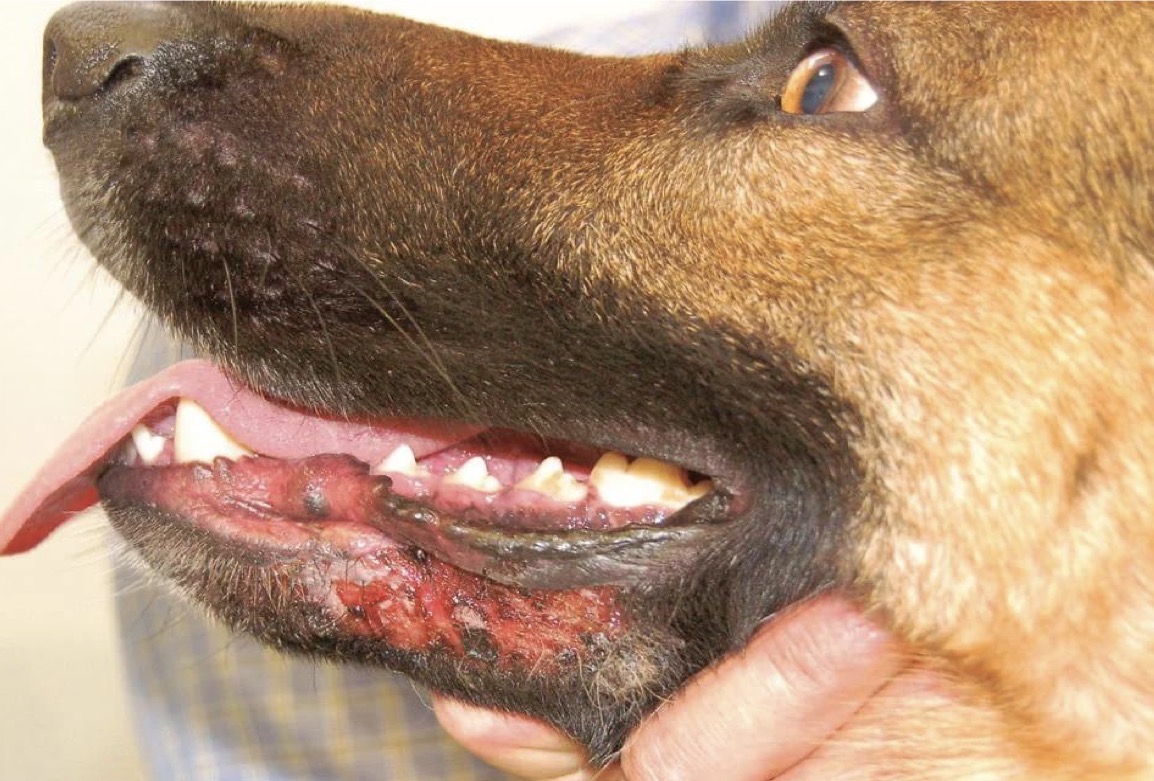
What will you see on cytology in a small animal with a superficial pyoderma?
Intracellular + extracellular cocci with neutrophils
What other follicular diseases should you rule out before ruling in superficial pyoderma in a small animal patient?
Demodex, Dermatophytosis, Pemphigus foliaceus
What is the recommended treatment plan for a small animal patient with a superficial pyoderma?
-Topical antiseptics → chlorhex products, benzoyl peroxide, salicylic acid, sodium hypochlorite (dilute bleach), or bacitracin ointment for localized lesions
-Anti-inflammatory → topical glucocorticoids or short course of systemic glucocorticoids (5-7 days)
-Systemic antimicrobials (if topicals fail) → should base off culture, but go for three C’s (Cephalexin, Clindamycin, Amoxi-Clavulanate) for 2 weeks
What are the typical three C’s for antimicrobial treatment of dermatological infections in small animals?
Cephalexin, Clindamycin, Amoxicillin-Clavulanate
Which layers of the skin do deep pyodermas reach into?
Dermis ± SQ tissue
Which form of deep bacterial pyoderma presents commonly in GSDs as painful hemorrhagic bullae, thick crusts, draining tracts, nodules, ulcers, or scarring in areas of high friction with associated fever, lethargy, & lymphadenopathy?
Deep Bacterial Folliculitis/Furunculosis (DBFF)
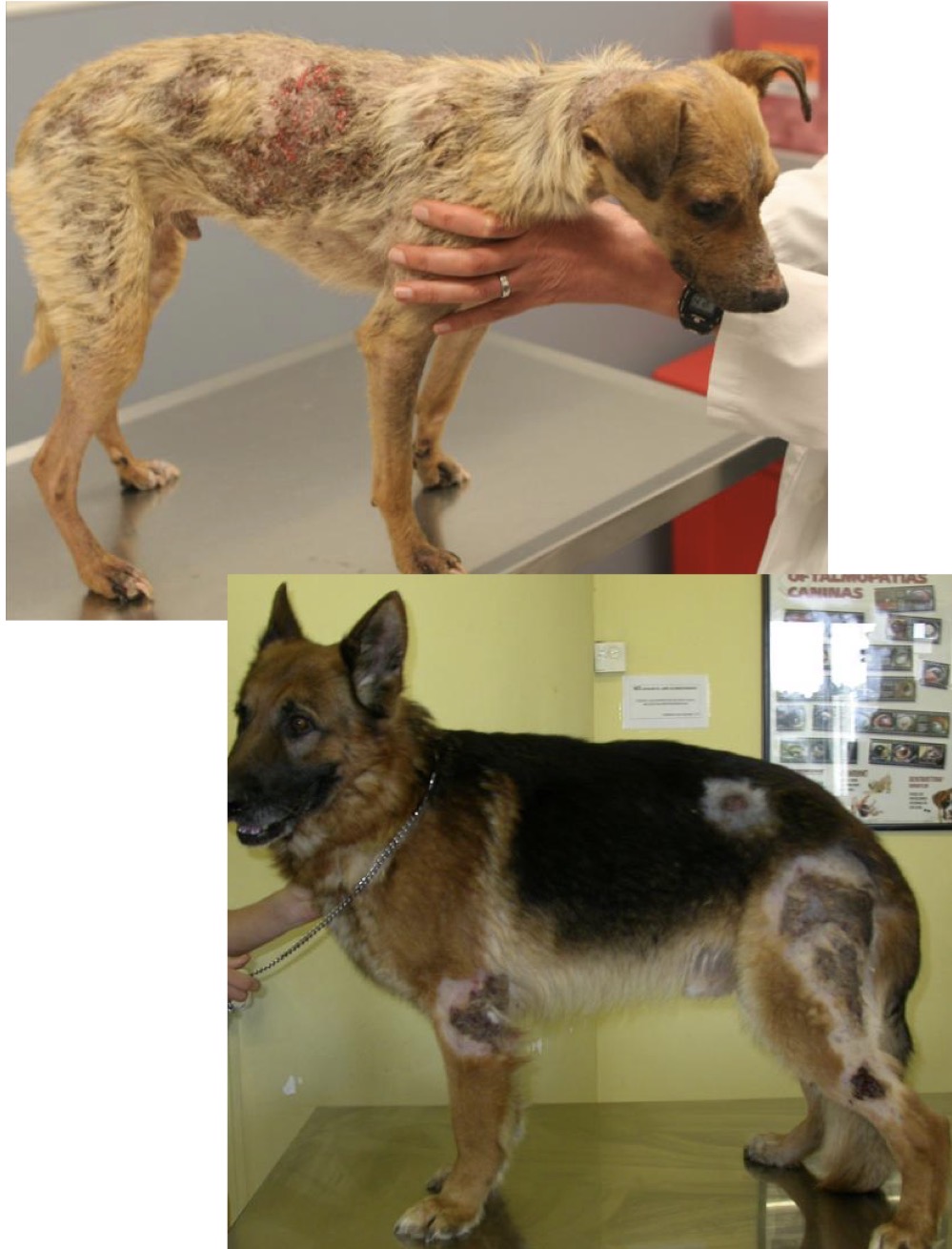
Which bacterial pathogen is the most common etiologic agent involved in Deep Bacterial Folliculitis/Furunculosis (DBFF)?
Staphylococcus spp.
-second is Pseudomonas spp.
Which form of deep pyoderma is associated with “lick granulomas”?
Acral Lick Dermatitis/Furunculosis
What will you see on cytology in a small animal with a deep pyoderma?
Low numbers of bacteria, lots of neutrophils, macrophages → pyogranulomatous inflammation
What will you see on a cytology in a case of pemphigus foliaceus?
Acantholytic keratinocytes
What is the recommended treatment plan for a small animal patient with a deep pyoderma?
-Systemic antimicrobials after C/S → 3 week course or until infection resolves
-Adjunctive topical + anti-inflammatory therapy → antiseptics + PBM + glucocorticoids
-Pain management → Gabapentin + topical anesthetics (lidocaine or pramoxine sprays, EMLA cream)
For which types of pyoderma should we only use topical antimicrobials to treat?
Surface + Superficial
-if topicals not working for superficial, you can try systemic approach
Which antibiotics do Methicillin-Resistant Staphylococcus Pseudintermedius (MRSP) organisms show resistance to due to the mecA gene that produces PBP2a (penicillin-binding protein)?
Oxacillin + All B-lactams (penicillins, cephalosporins, carbapenems)
What antibiotics are reserved for the treatment of MRSP?
Rifampin, Chloramphenicol, Amikacin, Gentamicin
-high risk side effects with these, so must monitor labs
Which dermatophytosis occurs as a superficial fungal infection of keratinized structures (hair shafts + stratum corneum), using proteolytic/keratolytic enzymes to break down keratin to be used as nutrition?
Ringworm
Which dog breeds are predisposed to ringworm?
Yorkshire terriers <1yr old
-also hunting or other working dogs
Which cats can be asymptomatic carriers of ringworm?
Long-haired/Persian cats
How long after exposure to ringworm do animals typically show infection clinically?
1-3 weeks post-exposure
Besides circular alopecia, erythema, scales, & crusts, what other unique clinical signs can dogs or cats show in a ringworm/dermatophytosis infection?
Dogs: kerions (deep)
Cats: pseduomycetoma (deep)
-also nail changes (onychomycosis)
What are some of the diagnostic tests that we can perform to diagnose ringworm/dermatophytosis in small animals?
-Wood’s lamp → only M. canis will fluoresce
-Trichogram evaluation → mineral oil mount
-Fungal PCR → cannot distinguish active infection from fomite carriage
-Fungal culture → Mackenzie Toothbrush technique
-Biopsy → nodular lesions with special stains (PAS, GMS)
What are the recommended topical treatments for small animal patients with ringworm (dermatophytosis)?
-Miconazole + chlorhexidine shampoo twice weekly
-Lime sulfur dip 2-4% (calcium polysulfide) twice weekly
-Enilconazole 0.2% solution twice weekly
-Terbinafine 1% OR Miconazole 1-2% lotion daily
What are the recommended systemic treatments for small animal patients with ringworm (dermatophytosis)?
First-Line:
-Itraconazole 5mg/kg daily or pulse protocol (week on/week off)
-Terbinafine 30-40mg/kg daily
Second-Line:
-Griseofulvin 50mg/kg daily (contraindicated in pregnant animals + FIV+ cats)
-Fluconazole/Ketoconazole 5-10mg/kg daily
How long should you continue treatment for ringworm (dermatophytosis)?
Until 2 consecutive negative follow-up fungal cultures are performed 2-4 weeks apart + a negative PCR
OR
1 negative fungal culture + a negative Wood’s lamp exam + resolution of lesions
How does Demodex canis initially present in canine patients?
Hypotrichosis/alopecia, mild erythema, comedone formation, scaling
What are the predilection sites for demodex canis?
Face, periocular areas, feet
Who is more likely to show localized demodicosis on the face/head or front limbs & how is it treated?
Juveniles → resolves spontaneously without treatment
What is the treatment for generalized demodicosis in dogs of any age?
Miticidal ± Antimicrobials
What is the commensal Demodex spp. infection that is primarily seen in terrier breeds, causing a greasy hair coat on the dorsal trunk & is only pruritic if a secondary infection (like Malassezia) is present?
Demodex injai
What is the recommended treatment for generalized canine demodicosis?
Isoxazolines (topical or PO)
-others: Amitraz rinses or macrocyclic lactones
Which feline demodicosis presents with pruritus as a primary clinical sign?
Demodex gatoi
What is the recommended treatment for feline demodicosis?
Isoxazolines (topical or PO) → Bravecto, Credelio, Revolution Plus
-others: Lime sulfur 2% dips, Amitraz baths, Moxidectin/imidacloprid spot-on (Advantage Multi), or Ivermectin
Which diagnostic cytology approach should be used for moist or exudative skin lesions?
Impression smear → look for undisturbed pustules/crusts
Which diagnostic cytology approach should be used for dry, greasy, or interdigital skin lesions?
Tape prep
Which diagnostic cytology approach should be used for claw fold skin lesions?
Toothpick
Which diagnostic cytology approach should be used for finding parasites or deep fungal organisms?
Skin scraping
Which diagnostic cytology approach should be used for ears, interdigital, mucosa, or skin fold lesions?
Swab cytology
Which diagnostic cytology approach should be used for looking at hair cycle stage, pigment, fungal elements, or follicular mites?
Hair plucks (trichogram)
Which stain does not need to be used for evaluating tape cytology?
Methanol-blue → chemical fixative (already in tape)
What kind of samples do not need to be heat fixed so we do not damage the sample?
FNA samples
What is Phovia Fluorescent Light Therapy’s mode of action?
It uses polychromatic light energy to target multiple layers of skin
Which layer of the skin provides the primary barrier that helps prevent allergens from entering a dog’s body?
Stratum corneum
What are the 3 types of lesions associated with eosinophilic granuloma complex in cats?
Eosinophilic plaque, eosinophilic granuloma, indolent ulcer