T cell Activation
1/9
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
10 Terms
Describe Naive T cell activation:
Location
What are Lymphnodes
List the locations of activation by type of infection
Naïve T cell activation
Location:
secondary lymphoid tissues;
APCs present Ag
Lymph nodes:
draining an infected or inflamed area is a depot of processed antigen on DCs and macrophages (MØ).
Types/Locations
blood infections:
activation occurs in spleen.
respiratory infections:
activation occurs in
adenoids,
tonsils,
other bronchial-associated lymphoid tissues.
GI infections:
Peyer’s patches,
other gut-associated lymphoid tissues.
Describe the mechanism for lymphocyte homing
Definition?
Mech
Lymphocyte Homing:
Definition:
movement of naïve T cells into secondary lymphoid tissues.
Mechanism:
Rolling:
weak interaction between naïve T cells and endothelial cells in lymph node HEV
L-selectin (T) - CD34 and GlyCAM-1 (HEV)
Slows down flow of circulating lymphocytes
LFA Activation:
CCL21 (HEV) - CCR7 (T)
Diepedesis
Activated LFA-1 binds ICAM1
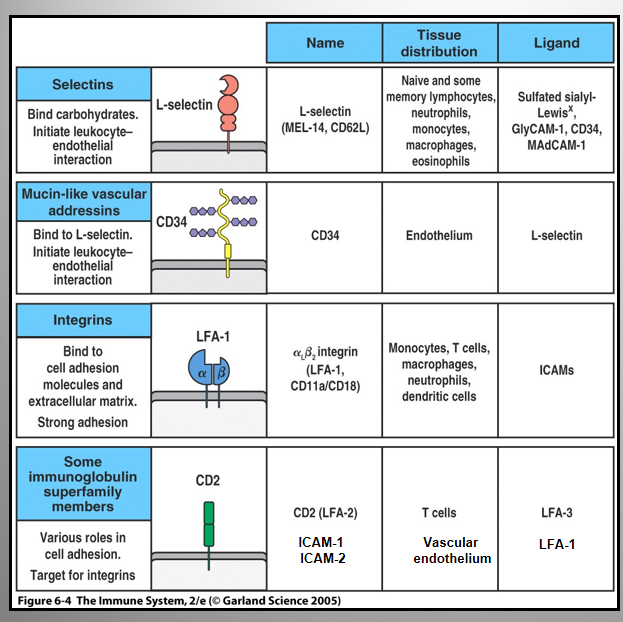
List the adhesion molecules involved in T cell-APC interactions
Initial Transient
Strong Adhesion
Describe the mechanism for LFA activation
Adhesion Molecules:
Initial Transient binding:
mediated by integrins and members of Ig superfamily.
LFA1 (T) - ICAM-1/2 (APC)
Strong Adhesion:
CD2 (T) - LFA-3 (APC)
ICAM-3 (T) - DC-SIGN (APCs)
LFA activation
Initial T-APC binding → T cell samples peptide: MHC complex (APCs) → induce conformational change on LFA-1 → stronger binding to ICAMs
more stabilized interaction that last several days
NOTE: LFA: Lymphocyte function-associated antigen, ICAM: Intercellular adhesion molecule
DC-SIGN: DC-specific ICAM-3 grabbing non integrin
Describe Initial T-Cell Activation
Describe the Binding/ Signaling pathway/ and effect of Signal 1 and 2
Describe the Binding and effects of Signal 3
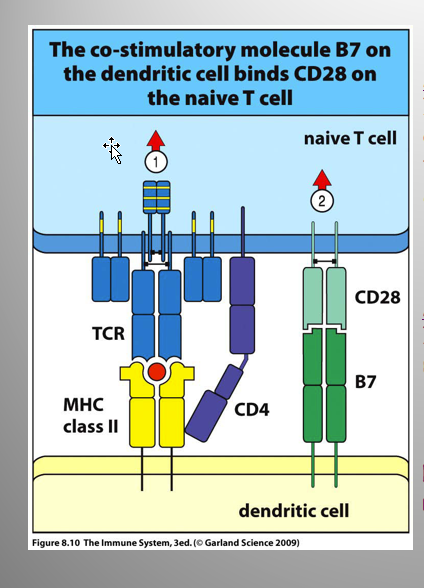
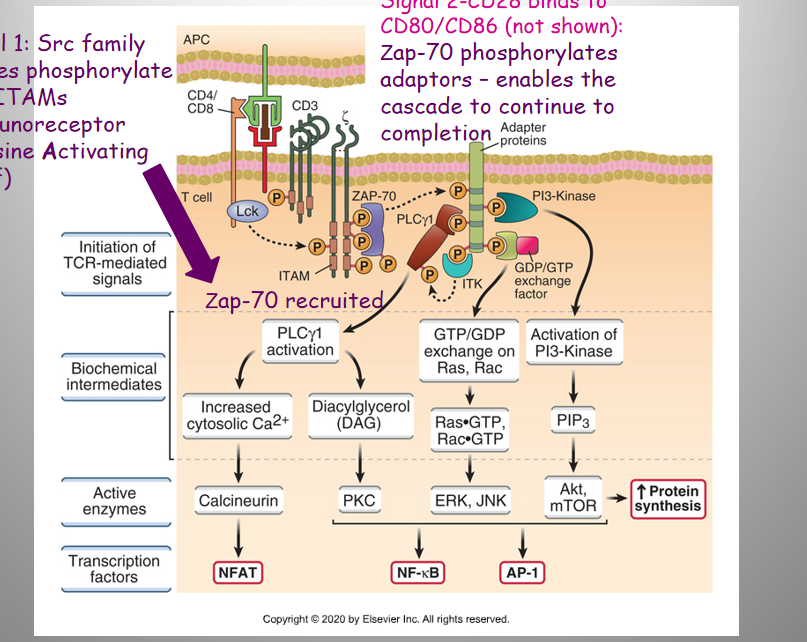
Activation Signals 1 and 2:
1:
Binding:
TCR complex + CD4/8 (T) - Peptide on MHC (APC)
Signaling Pathway:
Src family kinases → phosphorylate TCR ITAMs ((Immunoreceptor Tyrosine Activating Motif)) → downstream effects
2:
Binding:
Int. btw co-stimulatory molecules
CD28 (T) - B7.1 (CD80) or B7.2 (CD86) (APC)
Signaling Pathway:
Zap-70 → phosphorylates adaptors → continues cascade
Effect of 1 and 2:
activates NFAT, NK-kB, AP-1, Protein synthesis
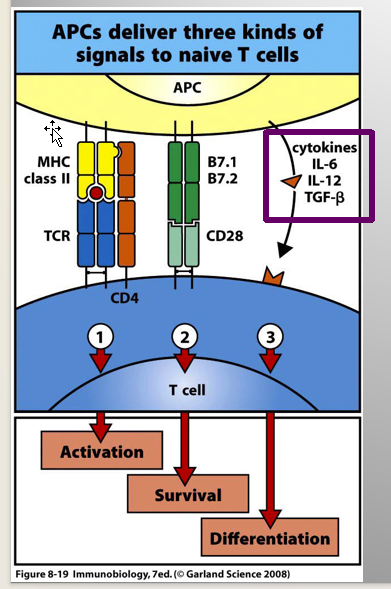
Activation Signals 3:
Binding:
Cytokines (APCs/other immunes cells) - T Cells
IL-6
IL-12
TGF-B
Effect:
influences subsequent effector function of CD4+
Cytokine Composition dependent
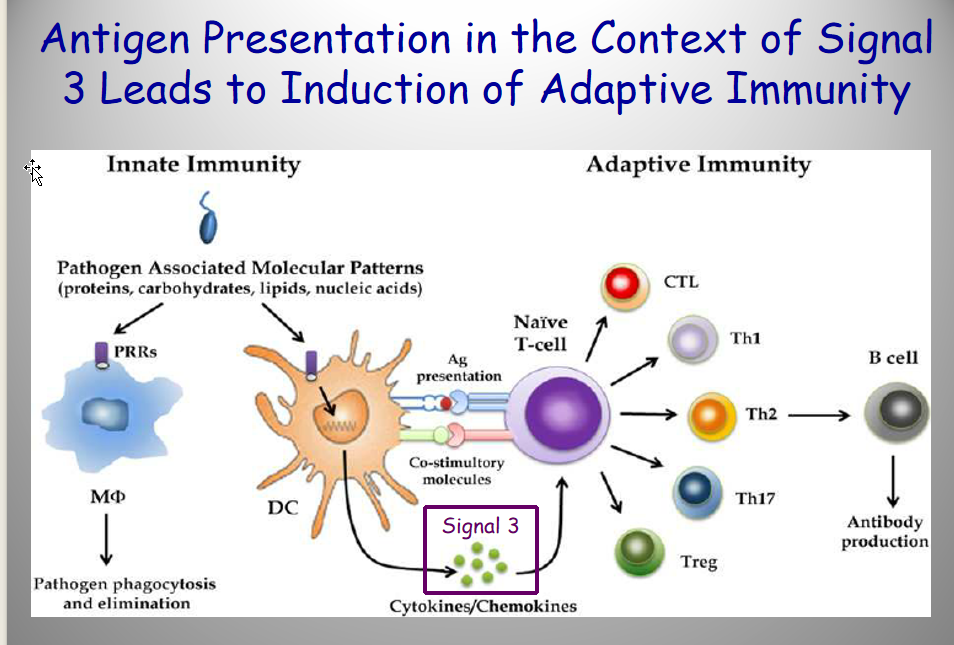
induce CD8+ T cell → CTLs (cytotoxic T lymphocytes)
Induction of Adaptive Immunity
What happens when Signals 1 or 2 are Missing?
W/O signal 1:
No effect on T cells
W/O signal 2:
T cell becomes anergic
What does TCR activation leads to?
Describe the main effect of immunosuppressive drugs; List them and their function
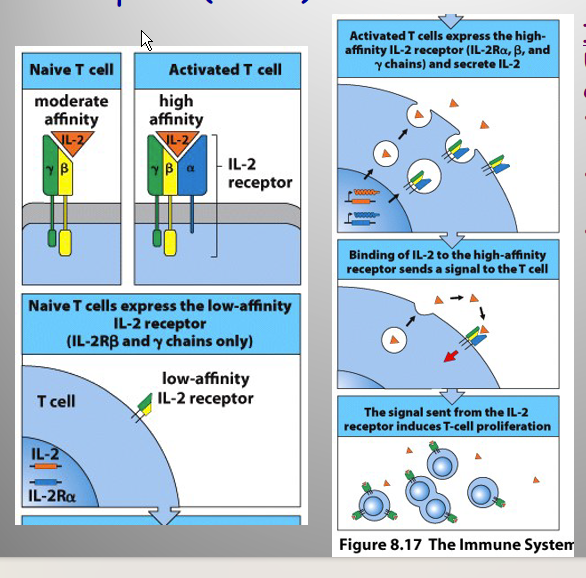
TCR Activation
→ IL-2 production + expression of High-Affinity IL2R (has alpha chain now) → T Cell Proliferation
Immunosuppressive Drugs:
Main Effect: block unwanted expansion of T cells:
List/Function:
Cyclosporin A + Tacrolimus (FK506)
disrupts TCR signaling.
Rapamycin
inhibits signaling downstream of the IL2R.
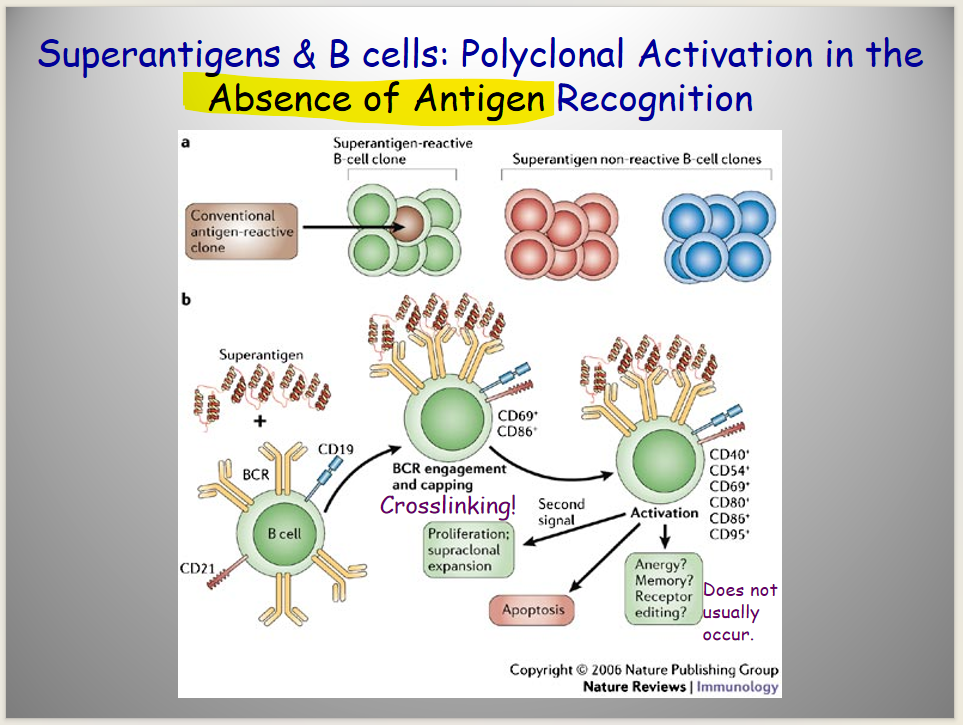
Describe superantigens:
Mech
Effect
superantigens
Mechanism:
binds both MHC protein + TCR together (@ positions outside the normal binding site (
Effect:
stimulates massive
T-cell activation,
cytokine release
systemic inflammation