BIOL 220 Soilborne Diseases
1/28
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
29 Terms
What is the mode of transmission and major portal of entry?
Mode of Transmission:
• Vehicle Transmission – Transmission by a contaminated inanimate or non-living reservoir/pathogen can multiply in (like Soilborne)
Major portal of entry:
• Broken skin (hypertonic environment, lysosomes, low pH)
• Inhalation of contaminated soil via respirator tract
• Ingestion of contaminated soil via GI tract (oral-fecal route)
What are some predisposing factors of the soilborne diseases?
Direct contact with soil
• Walking barefoot in contaminated areas + jobs that involve direct contact with soil
Open wounds or skin injuries
Poor Hygiene or sanitation
• Clean drinking water
• Inadequate sewage systems
Weak immune system
• Malnutrition
• HIV/AIDS
What are prevention methods for soilborne diseases?
• Education!
• Practice Good hand hygiene like before/after handling food and soil
• Wear PPE like mask for low air quality
• Avoid walking barefoot in soil
• Proper wound care – protect your wounds (if have open skin wounds = avoid contact with soil and water)
Tetanus: Causative Agent and Virulence Factor
Causative agent: Clostridium tetani
• Gram-positive bacteria, bacilli, obligate anaerobe (mostly found in the deep layers of soil)
• Can stay dormant for many years
Virulence factor:
• Endospore forming = allows for the survival of pathogen in harsh conditions
• Tetanospasmin (neurotoxin/exotoxin): disrupts/blocks neurotransmission → uncontrolled muscle contractions and spasms
Tetanus: S/Sx and Diagnosis
S/Sx:
• Toxemia (Toxins enter the blood stream)
• Spores enter through a skin break via fomite → enter anaerobic areas of the body (deep tissue) and germinate → produce potent neurotoxins → Target the Central nervous system
• Blocks relaxation pathway of the muscles = causes muscle spasms and contractions
• Head, neck and back muscle stiffness and spasms
• Respiratory muscle failure --> death
• severe hyperextension
Diagnosis: based on symptoms
Tetanus: Prevention, Treatment, and Predisposing factors
Predisposing factors
• Direct contact with fomites (contaminated non-living object that carries/spreads the pathogen) — EX: Rusty nails or sharp objects
Prevention: vaccines
• DTaP, TDaP & Td (Diphtheria, Tetanus & Pertussis)
Treatment:
• Antibiotics (Penicillin): attack pathogen
• Sedation drugs: help muscles relax
• Tetanus Immune Globulin (TIG) (artificial passive): attack toxins —- Medication that has antibodies against the tetanus toxin → Prevents tetanospasmin from from binding to nerve endings + muscle spasms and failure
• Opsonization, neutralization of toxins & agglutination
Gangrene Basics: Ischemia, Necrosis, Gangrene, and types of Gangrene
• Ischemia: blood vessel blockage = loss of blood supply to tissue (inadequate blood supply to an organ or
part of the body)
• Necrosis: death of tissue, irreversible process
• Gangrene: Tissue death (Necrosis) due to loss interrupted blood supply
• Several types of gangrene: Dry / Wet / Gas Gangrene
Dry Gangrene: type of gangrene, S/Sx, and Treatment
Type of gangrene: cut off blood supply to an area of tissue → Ischemia without infection
S/Sx:
• No Pus or bad odor
• Area becomes dry and shrunken
• Color: Brown, purple/blue or black
Treatment:
• Surgical removal of dead tissue
• Amputation in severe cases to prevent the spread of infection
Wet Gangrene: type of gangrene and S/Sx
• Bacterial infection of dead tissue
• S/Sx: Swelling, blistering and a wet appearance – Foul smelling
Gas Gangrene: Causative Agent and Virulence Factor
Alternative Name: Clostridial Myonecrosis
Causative Agent: Clostridium perfringens
• Gram positive bacteria, bacilli, endospore-forming, obligate anaerobe (grows in deep tissue wounds + necrotic tissue)
• 20 – 25% mortality rate + Common cause of death during conflicts/war
Virulence Factors:
• Alpha toxin: excessive platelet aggregation → blocks blood vessels and deprive tissue/organs with oxygen supply; moves along the tissue and muscles
• Spores enter ischemic area of body/deep tissue wound → vegetative cells produce and release
alpha toxin → vascular and soft tissue damage
• Severe pain and swelling of an area: Pale → red → black/green-ish
• Prevents phagocyte function: creates an oxygen-deficient environment that helps pathogen grow
Gas Gangrene: S/Sx and Diagnosis
S/Sx:
• Tissue damage, severe pain and swelling
• Pale area → red and blackish green
• Gas filled Blisters from glucose fermentation: Bacteria feed on glucose in tissue to multiply → Pathogen ferment glucose to produce carbon dioxide and hydrogen gas
• Crepitus (cracking sound under skin due to gas bubble formation)
Diagnosis: S/Sx
Gas Gangrene: Treatment
Treatment:
• Immediate high doses of antibiotics (penicillin)
• Surgical removal of necrotic tissue, amputation
• Hyperbaric chamber: Increase the pressure experienced by the patient → help deliver oxygen to deprived areas
• Gas Gangrene should be treated as a medical emergency
What is Coccidioidomycosis & Histoplasmosis
both fungal diseases that affect the lower respiratory system (similar S/Sx)
Histoplasmosis: Causative Agent, Virulence Factor, Reservoirs, and Transmission
Causative agent: Histoplasma capsulatum (Dimorphic fungi: can exist in mold and yeast form)
Virulence Factor: Yeast form can multiply in phagocytes (similar to Mycobacterium tuberculosis); Not contagious
Reservoirs:
• Soil that is rich in bird or bat droppings
• Caves (spelunking), old buildings and chicken coops
Transmission: Via inhalation of microscopic fungal spores called conidia (AKA microconidia) located in contaminated soil when disturbed
Histoplasmosis: S/Sx
• Mostly asymptomatic (no S/Sx experienced by the patient)
• Acute histoplasmosis: Fever, cough, fatigue and chest pain
Chronic histoplasmosis:
• Flu like symptoms that resembles tuberculosis; typically found in people with preexisting lung conditions or weakened immune system
• Bloody cough, weight loss, night sweats, low grade fever,
• Lung lesions on chest X-Ray (white spots): Nodule/mass in the lung from an infection or autoimmune disease
Histoplasmosis: Diagnosis, Commonly Found, and Treatment
Diagnosis:
• Chest X-ray; lung lesions
• Serology: testing for antibody production against the fungi
• Biopsy: procedure where a small tissue sample is taken from the body for microscope exam → look for Yeast-forms in phagocytes
• Sputum sample
Commonly Found: in the Mississippi and Ohio River Valleys
Treatment:
• No Vaccine available
• Treatment with antifungals/antimycotics (Itraconazole; type of antifungal med)
Coccidioidomycosis: Alternative Name, Causative Agent, Mode of Transmission, and Virulence Factor
Alternative Name: Valley Fever or San Joaquin Fever
Causative Agent: Coccidioides Immitis
• Dimorphic fungus, produces fungal spores, can survive many temperatures
Mode of Transmission:
• Fungus pathogen grow in dirt/soil → fungus spores survive in air by the wind/digging → people/animals inhale from the air
Virulence Factor:
• Inhale fungal spores called arthroconidia: form spherules in tissue → release endospores
Coccidioidomycosis: S/Sx
• Mostly asymptomatic
Acute Coccidioidomycosis: Mild/few symptoms
• Like flu symptoms: Fever, cough, tiredness, red spotty rash
Chronic Coccidioidomycosis: common in people with a weakened immune system or preexisting respiratory conditions (Similar to Chronic TB)
• Low grade fever, bloody cough, weight loss, night sweats
Coccidioidomycosis: Commonly Found and Prevention
Commonly Found:
• dry desert soils of American southwest
• Arizona, Central California, Texas, Northern Mexico, New Mexico
• Climate change → increasingly dry areas → increase in people affected
Prevention:
• Avoiding dry areas where dust gets kicked up into the air
• Wearing a mask/covering + Air filters
Coccidioidomycosis: Diagnosis and Treatment
Diagnosis:
• Culture lung tissue or sputum sample
• Chest X-ray: Presence of lung lesions
• Patient Location within the last month
Treatment:
• Antifungals/antimycotic medication (Itraconazole)
• No Vaccine available
Hookworm infection: Causative Agent and Virulence Factor
Causative Agent: parasitic helminths (treat both types as one on exam)
1. Necator americanus (New world hookworm) from Americas
2. Anycyclostoma duodenale (Old world hookworm) from Middle East
• Kingdom Animalia, Phylum Nematoda (Roundworms)
• Hooked shaped body, separate sexes and contain specialized mouth parts
Virulence factor:
• Complex life cycle with multiple stages and hosts
Hookworm: Transmission and Reservoirs/Hosts
Transmission:
• Hookworm Larvae in contaminated soil will penetrate bare skin – usually through the feet
Reservoirs / hosts:
• Dogs, cats, Farm animals (pigs, goats and sheep), wild carnivores
What is the Life cycle of hookworm
• Adult hookworms mature in the small intestine of the human host (worms feed on blood and tissue)
• Eggs are secreted with feces → release into the environment → develop into filariform larvae (infective stage)
• Larvae penetrate skin → attach to the intestinal wall and produces eggs
• Can be passed through the oral-fecal route via the consumption of eggs
Hookworm: S/Sx
Initial S/Sx: Itchy rash at the hookworm site of entry “ground itch”
S/Sx of large number of worms:
• Anemia, fatigue, weakness, abdominal pain and diarrhea
• Lack of healthy Erythrocytes (Red blood cells) due
to hookworms feeding on blood and other tissues
Hookworm: Prevention, Diagnosis, and Treatment
Prevention:
• Avoid direct contact with contaminated soil
Diagnosis:
• Microscope: Stool examination to detect hookworm eggs
• Serology: Complete Blood Count (CBC) to count RBCs and hemoglobin and iron levels
Treatment:
• Antiparasitic/Anthelmintic drugs (Mebendazole)
Ascariasis: Causative Agent, Virulence Factor, and Mode of Transmission
Causative Agent: Ascaris lumbricoides (parasitic helminth)
• Kingdom Animalia, Phylum Nematoda
• Largest parasitic round worm: Separate sexes + special mouth parts
Virulence Factor:
• Complex life cycle with multiple stages and hosts (can infect swine/pigs)
• Structure is the infective stage: Ascaris lumbricoides eggs
Mode of Transmission: Oral-Fecal route
• Eggs are shed in the feces → Contaminated food, water or SOIL → ingested by another person
• Ascariasis eggs can survive for several months
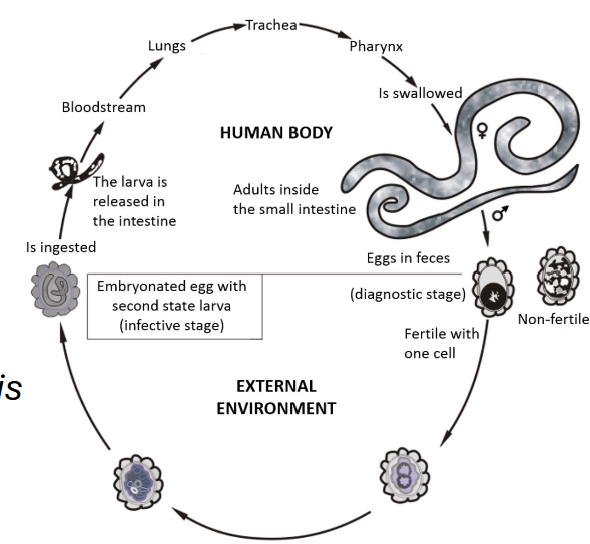
What is the lifecycle stages of Ascariasis
• Ingest infective eggs from contaminated soil.
• Larvae hatch in the intestine → migrate to the lungs → ascend the throat to be swallowed again
• Once back in the small intestine, they mature into adult worms → reproduce and pass new eggs
in the feces, starting the cycle again.
• The entire process from ingestion to the shedding of new eggs takes two to three months
Ascariasis: S/Sx and Predisposing factors
S/Sx:
• Often asymptomatic in light infections
• Heavy infections: Passage of food, fluid or gas through the intestines is blocked → cause intestinal blockage, malnutrition and impaired growth (and development) in young children
Predisposing factors:
• Ingesting contaminated feces via food or water via Inadequate Sanitation, poor hand hygiene
Ascariasis: Diagnosis and Treatment
Diagnosis: Microscopically examine stool for eggs; based off S/Sx
Treatment: antiparasitic/antihelminth drugs (Mebendazole)