(12.0) General Info
1/12
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
13 Terms
What are the physiological changes in older adults?
DECREASED MOBILITY
CHANGES IN SKIN AND HAIR
There’s more gray hair and it’s thinning
DECREASED SENSES
e.g, decrease vision and hearing
More at risk for chronic health issues
e.g, pneumonia, risk for falls, etc
Describe self-esteem and self-concept. What are some nursing considerations to promote better self-esteem?
Self-esteem is HOW A PERSON VIEWS THEMSELVES (either positive or negative)
Someone with positive self-esteem FEEL CAPABLE AND COMPETENT about the things they do
Nursing considerations:
PROMOTE VERBALIZING FEARS AND ANXIETIES
REINFORCE STRENGTHS/SUCCESSES
What is body image? What are some things that can negatively affect body image? What can nurses do to understand someone who is going through body changes?
Body image: How a person VIEWS THEIR OWN BODY—either positively or negatively
Things that can affect body image:
LOSS OF BODY PART
LOSS OF BODY FUNCTION (e.g, spinal cord injury, arthritis)
Social media
Cultural standards (e.g, in Korean beauty standards, you need to be pale and have large eyes and be skinny)
OTHER’S PERCEPTION of you
Nurses should ACKNOWLEDGE EMOTIONS (e.g, anger, depression, and denial) WHEN HELPING A PATIENT WITH SIGNIFICANT BODY CHANGES
What is the concept “sexuality” in general? What are some therapeutic communications nurses can use for the LGBTQ+ community? What are some rights LGBTQ+ have in equitable healthcare?
Sexuality: BROAD TERM TO DESCRIBE HOW INDIVIDUALS EXPERIENCE/EXPRESS THEMSELVES SEXUALLY
Therapeutic communication
“MIRROR LANGUAGE” — use the same phrases that someone would like to be called or another person wants to be called
e.g, if a female patient identifies as “he/him” instead of “she/her,” use the “he/him” and be respectful of that
Right for LGBTQ+
Advocate for the healthcare needs of all sexes/genders
Make sure that TREATMENT THEY RECEIVE IS RESPECTFUL AND RELEVANT
In terms of sexual activity for the elderly, what are the normal physical findings for older adults? What types of sexual dysfunction can happen? What can be some nursing educations for older adults and sexual activity?
Normal physical findings
REDUCE HORMONE LEVELS
Slow sex response
Increased lubrication or bodily changes
Sexual dysfunction that can happen
ERECTILE DYSFUNCTION + DECREASED VAGINAL LUBRICATION (this can be BECAUSE OF DIURETICS)
Diuretics can cause these dysfunctions since it REDUCES BLOOD VOLUME, decreasing blood flow to sex organs, altering hormone levels
REDUCE LIBIDO (antidepressants can cause this)
Nursing education for older adults
PROVIDE ALTERNATIVE MEANS OF EXPRESSIONS
e.g, promote hugging or cuddling as a way to express love instead of sucking their faces off
Explain the “BETTER” model
“BETTER” model helps guide nurses in ADDRESSING SEXUALITY
B = Bring up topic
E = EXPLAIN CONCERNS for everything in patient’s life
T = TELL patient that sexual dysfunction can happen
T = TIMING is important
E = EDUCATE on SIDE EFFECTS
R = RECORD ASSESSMENTS
What is GAS (General Adaptation Syndrome)? What are the stages of it?
GAS: Stages in HOW TO BODY RESPONDS AND COPES WITH STRESS
There “ARE” 3 stages
Alarm: Body TRIGGERS FIGHT OR FLIGHT RESPONSE
Hormones (epinephrine, norepinephrine, cortisone) are released, which cause elevated blood pressure and heart rate, heightened mental alertness
The body’s either going to tackle the stress head-on or try to avoid it
Resistance: The body TRIES TO GO BACK TO HOMEOSTASIS USING COPING MECHANISMS
The BODY FIGHTS THROUGH STRESS AND IS ABLE TO COPE because of the coping mechanisms
Exhaustion: When the BODY CANNOT FIGHT AGAINST THE STRESS, letting the stress consume the body
BODY CAN’T FIGHT ANYMORE, LEADING TO BURNOUT, WEAK IMMUNITY, AND HIGH RISK OF CHRONIC ILLNESS
How to prevent foodborne illness?
KEEP FOOD HOT AFTER COOKING
DON’T WASH ANYTHING CHICKEN RELATED to prevent spread of microbes in the sink or other kitchen places
WASH HANDS
Give only PASTEURIZED FRUIT JUICES TO CHILDREN
Pasteurized fruit juices are good for children because the heat kills harmful bacterias that are in the juice
⭐ What is constipation? What causes it? How can it be managed? What is the difference between constipation and diarrhea?
Constipation: When it’s hard to poop (and it’s INFREQUENT and you have to really push it out) because it’s HARD AND DRY
It’s happens when WASTE MOVING TOO SLOWLY THROUGH THE COLON, ALLOWING IT TO ABSORB TOO MUCH WATER
Some causes: AGE, INADEQUATE FLUID/FIBER INTAKE, USE OF LAXATIVES, DECREASED MOVEMENT (immobile OR sedentary lifestyle)
It’s REALLY IMPORTANT TO EAT FIBER WHEN YOU’RE CONSTIPATED since it SOFTEN’S THE STOOL, allowing easier bowel movement
It’s managed by INCREASING FIBER AND WATER CONSUMPTION
Even though the cause of constipation is too much water absorption because it moves through the colon slowly, you WANT TO DRINK MORE WATER so that the STOOL IS ALREADY WELL HYDRATED and DOESN’T NEED TO ABSORB MORE WATER
When you eat a lot of fiber for constipation, it's important that you also increase your water intake because the fiber needs a lot of fluids to work properly for it to moisten the stool
If you eat a lot of fiber but don't drink enough water, it can worsen the condition of Constipation
Diarrhea: WATERY STOOL (opposite of constipation)
DECREASE FIBER INTAKE (since fiber makes poop even softer), but EAT MORE BANANAS, RICE, APPLESAUCE, OR POTATOES
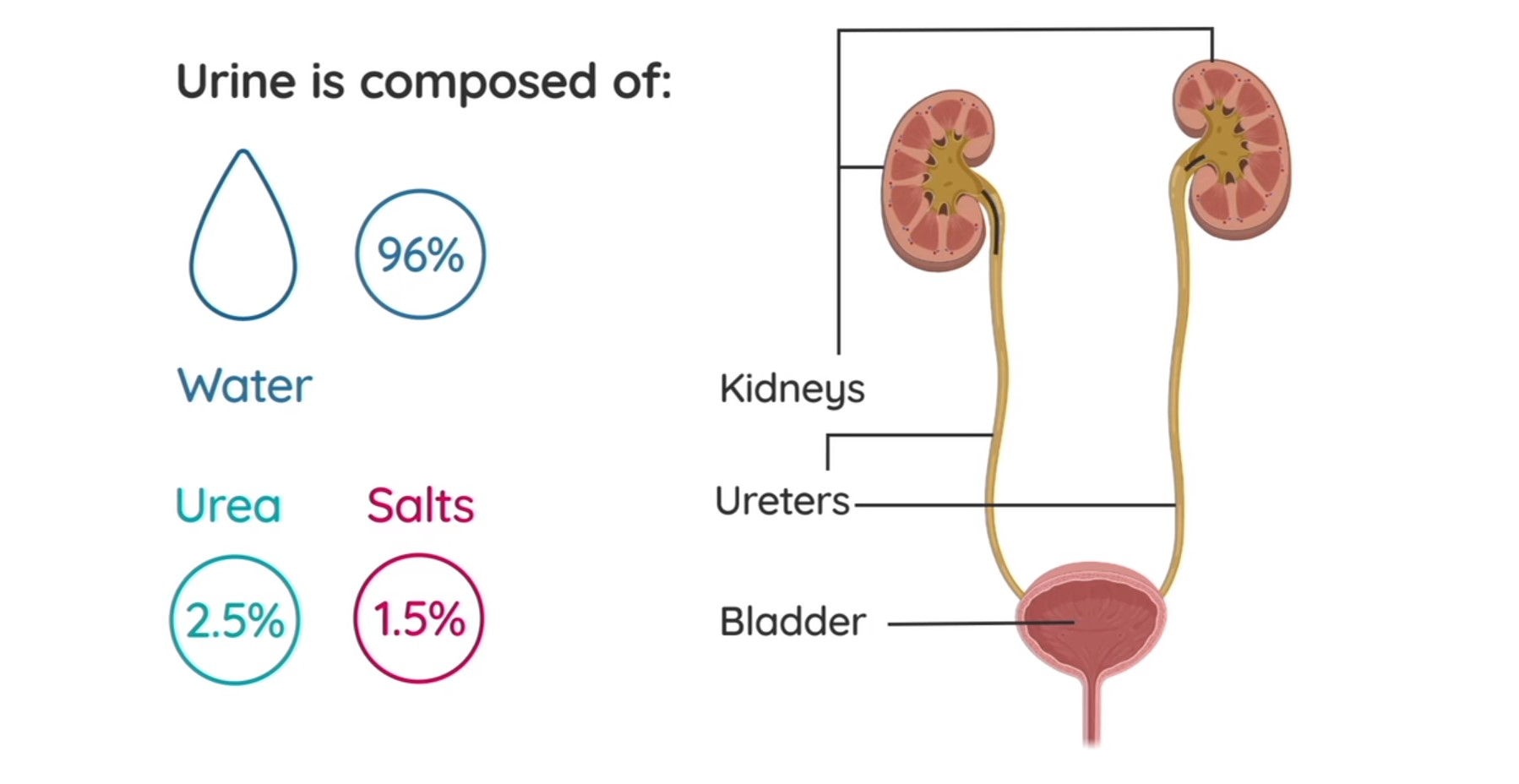
What is the path urine takes?
Kidney
Ureters (these are the little prongs sticking out of the kidneys)
Bladder
Urethra
Explain the different types of incontinence: Stress, Urge, Overflow, Reflex, Functional, Transcient
Stress incontinence: end up peeing a little because of PHYSICAL PRESSURE (stress) ON THE BLADDER
e.g, when you laugh too much and you end up peeing a little
Urge incontinence: has the sudden, intense, and uncontrollable need to urinate that results in the involuntary loss of urine
Overflow incontinence: CONSTANT DRIBBLING OR LEAKAGE BECAUSE THE BLADDER IS TOO FULL and can’t empty normally
Reflex incontinence: Involuntarily LOSE A MODERATE AMOUNT OF URINE WITHOUT WARNING
Functional incontinence: USED TO URINATE PROPERLY, but LOST ABILITY because of FACTORS THAT INTERFERE WITH ABILITY
e.g, someone immobile can’t pee when they want to, so they lose the ability to pee properly and just go
The person's bladder is still working fine, but because of physical or mental illness, it prevents them from going to the bathroom on time, leading to incontinence
Transient incontinence: TEMPORARY LOSS OF BLADDER CONTROL because of infection/irritation, temporary impairment, diseases, or medications
T for TEMPORARY loss of bladder control
What are diuretics? What do we use them for? What labs should we monitor? What are some nursing interventions if labs were out of range?
Diuretic: a “WATER PILL” that PROMOTES ELIMINATION OF WATER IN THE BODY
Opposite of antidiuretics, which INCREASE water absorption, INCREASING blood pressure
These HELP REMOVE EXCESS SODIUM IN BODY
Use diuretics to DECREASE BP and REDUCE FLUID BUILDUP by PROMOTING URINE ELIMINATION
Labs to monitor: POTASSIUM, BUN, and CREATININE
Nursing interventions for abnormal lab values:
If hypokalemic: PUT ON POTASSIUM DIET (e.g, banana, potatoes, etc) and NOTIFY THE PROVIDER
If hyperkalemic: HOLD OFF ON MEDS
If hyponatremic/dehydrated: MONITOR FOR THIRST
In general, MONITOR THE BLOOD PRESSURE AND I/O
What is UTI? What should nurses educate the clients on?
UTI (urinary tract infection): This is an INFECTION IN THE URINARY TRACT because it BACTERIA (E coli) MULTIPLES WITHIN THE URINARY SYSTEM
Client education
DRINK 2000-3000 mL of FLUIDS (water)
Doing this HELPS FLUSH OUT BACTERIA via urine
WIPE FROM FRONT TO BACK
Avoid bubble baths