biology biological diversity
1/423
Earn XP
Description and Tags
modules 4 and 6
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
424 Terms
plant passive defences physical
waxy cuticle, cellulose cell wall, stomata, bark, casparian strip
passive plant defences chemical
e.g catechol, bark resin, enzyme inhibitors like tannins, yeast on leaf surface
active plant defences
hypersensitivity- rapid death of tissue surrounding infection
reinforced cell walls (callose and lignin deposition)
plasmodesmata narrowing by callose
cytoplasm of nearby cells grows into xylem to make a callose wall
sieve pores of phloem blocked up by callose so sap can’t be transported
conservation agreements
CITES CBD CSS
what does CITES stand for
the convention on international trade in endangered species
what did CITES entail
-regulates trade in wild animal and plant species
-illegal to sell endangered species. limits trade made from endangered animals
-raise awareness
what does CBD stand for conservation agreement
the Rio convention on biological diversity
what did the Rio convention entail
-How to use resources sustainably
-how concerning biodiversity is a global responsibility
-government guidance
what does CSS stand for conservation
the countryside stewardship scheme
what does the countryside stewardship scheme do
-improve and extend wildlife habitats through management
- pay farmers to help regenerate hedgerows and wildflower borders, grassy strips
-use their flock to graze very fast growing species
in situ conservation
protecting species in their natural habitat for example marine conservation zones and wildlife reserves
ex situ conservation
protecting species outside of their natural habitat for example seed banks botanic gardens and zoos
signalling molecules in plant defence
phytoalexins, salicylic acid, ethylene, pheromones
what do phytoalexins do in plant signalling
disrupt pathogen metabolism, delay pathogen reproduction, disrupt bacterial cell surface membranes, stimulate the release of chitinase
role of salicylic acid in plant signalling
migrates through plant to unaffected areas and activates defence mechanisms that protect the plant against pathogens for a period. long-term protection called systemic acquired resistance
what does ethylene do in plant signalling
plants secrete it when pathogens are attacking. it vaporises and stimulates other leaves on the plant to react and other plants
primary non specific animal defences
skin/sebum, expulsive reflexes, mucous membranes, lysozymes, stomach acid
lysozymes role and where found
break down bacterial cell walls. found in blood, sweat, tears, breast milk
what is commensal bacteria and where is it found
non-pathogenic bacteria found in and on humans. E. coli and Candida albicans are common. found in skin, mouth, and intestines.
why is commensal bacteria good
compete with pathogenic microorganisms for nutrients and space and prevent them from invading host tissue
second line of defence molecules
phagocytes and antimicrobial proteins
second line of defence responses animal
blood clotting, inflammation, wound repair, phagocytosis
blood clotting cascade overview
platelets trigger a reaction cascade that results in the formation of fibrin which forms a scab
the inflammatory response charecteristics
redness, swelling, heat, pain, loss of function
what is inflammation
a local repsonse to infection and tissue damage
what happens in the inflammatory response
mast cells secrete the cell signalling molecule histamine, which causes vasodilation (increases blood flow through capilliaries) and fluid enters the tissues, creating swelling. some plasma leaves the blood and phagocytes, and cells release cytokines that trigger an immune response in the infected area
what are cytokines
cell signalling proteins that stimulate inflammation and an immune response
what are interleukins
a type of cytokine. IL-1 and IL-6 promote inflammation, IL-1 targetting the brain causing drowsiness and fever.
process of wound repair
scab is formed from blood clotting, stem cells divide by mitosis underneath. blood vessels form, collagen is produced, granulation tissue forms to fill the wound, stem cells move over the new tissue and produce epithelial cells, contractile cells cause wound contraction, unwanted cells die
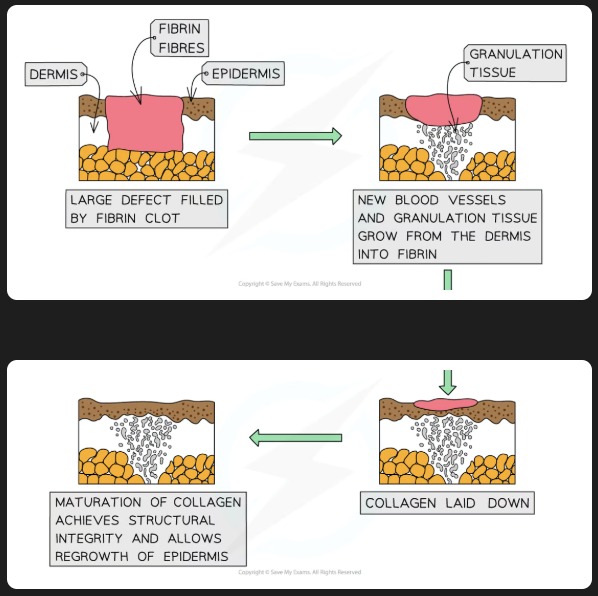
Blood clotting
-Collagen fibres are exposed
-platelets recognise and stick to them
-platelets release prothrombin activator
-prothrombin becomes thrombin
-thrombin cleaves fibrinogen into fibrin.
-fibrin fibres reinforce clot
what is a phagocyte
white blood cells produced in bone marrow that perform phagocytosis
phagocyte function
remove dead cells and pathogens. non-specific immune response
types of phagocyte
neutrophil, macrophage, dendritic cells
what is phagocytosis
the process of recognising and engulfing cells or particles
neutrophil definition
short lived phagocytes that act in the body tissues. multilobed nucleus. released in large numbers during infection.
neutrophil mode of action
-attracted to pathogens or cells under attack by chemotaxis.
-recognise antibody molecules on pathogens and attaches to them.
-cell surface membrane extends out and around the pathogen, engulfing it and trapping the pathogen in a phagocytic vacuole.
-endocytosis. lysosome fuses to form phagolysosome, killing and digesting the pathogens, dying themselves.
what is a sign of dead neutrophils
pus
what is a macrophage
large long-lived phagocytes.
can become APCs
where are macrophages produced
bone marrow
where are neutrophils produced
bone marrow
what do macrophages mature from
monocytes, developing into macrophages when they leave the blood
where do macrophages reside
they reside in lungs, liver, spleen, kidney, lymph nodes
macrophages mode of action
initiate the specific immune response. don’t completely destroy pathogens, but take the antigens and become antigen presenting cells, whihc can be recognised by lymphocytes
what are dendritic cells
large phagocytic cells with lengthy extensions. large surface area.
where are dendritic cells found
throughout the body
what is the role of antigen presenting cells
t cell activation to provide a specific immune response
what can an antigen presenting cell present
the antigens from toxins, foreign cells and ingested pathogens
what are opsonins
chemicals that bind to and tag foreign cells, making them easily recognisable to phagocytes
what is a phagosome
a vesicle that forms within a phagocyte
what is a lysosome
vesicles that contain enzymes capable of breaking down biological polymers
what cells are involved in the cellular response
T cells (helper, killer/cytotoxic, regulatory, memory)
macrophage
where do t cell mature
the thymus gland
where to b cells mature
the bone marrow
where do t lymphocytes orginate from
they originate in the bone marrow
what happens when t cells mature
gain specific cell surface receptors called t cell receptors, which have a similar structure to antibodies
t cell role in immune response
-complementary t cells binds to antigen presenting cell, and divide by mitosis to produce clones
-differentiate into t helper and t killers
-clonal selection of b cells
-release interleukins that trigger phagocytosis and b cells
what is a t helper cell
a t cell that release interleukins that increase phagocyte activity and activate b cells
what is a t killer cell
search for antigen presenting cells and attatch to the antigens and secrete toxic substances to kill infected cells and the pathogen inside. secrete perforins
what is a perforin
a glycoprotein responsible for pore formation in cell membranes
what is a t memory cell
a t cell that remains in the blood after infection ready to be activated for clonal selection if there is reinfection
what is clonal selection
specific b or t lymphocytes containin receptors complementary to a particular antigen are selected and activated
what is clonal expansion
the process of rapid cell division resulting in the multiplication of genetically identical cell clones from a single parent cell
where are b lymphocytes found
the whole body, concentrated in the lymph nodes and spleen
what produces the humoral response
b lymphocytes
b cell activation
b cells with complementary antibody receptors bind to antigen presenting cells. clonal selection. also binds with interleukins and t helper cells
clonal expansion in b cells
activated b cells divide by mitosis to produce clones. some differentiate to plasma cells and some memory cells
plasma cell
a type of b cell that mass produces antibodies. short lived
primary immune response
response to a newly encountered antigen. time delay, weaker, and more short lived
secondary immune response
response to a previously encountered antigen. stronger more long lasting
what happens in the primary immune response
clonal selection and expansion of specific t and b cells, synthesis of antibodies
how long does the primary immmune response take to produce antibodies
10-17 days
why is the secondary immune response quicker
more memory cells present to be selected than the original clone than before so more antibodies can be quickly produced
what do b memory cells divide into
plasma cells and more memory cells
types of t memory cells
memory helper t cells, memory killer t cells
what are antibodies
globular glycoproproteins called immunoglobulins
what structure do antibodies have
quaternary. y shape. two heavy polypeptide chains disulfide bonded to two light polypeptide chains. constant and variable region
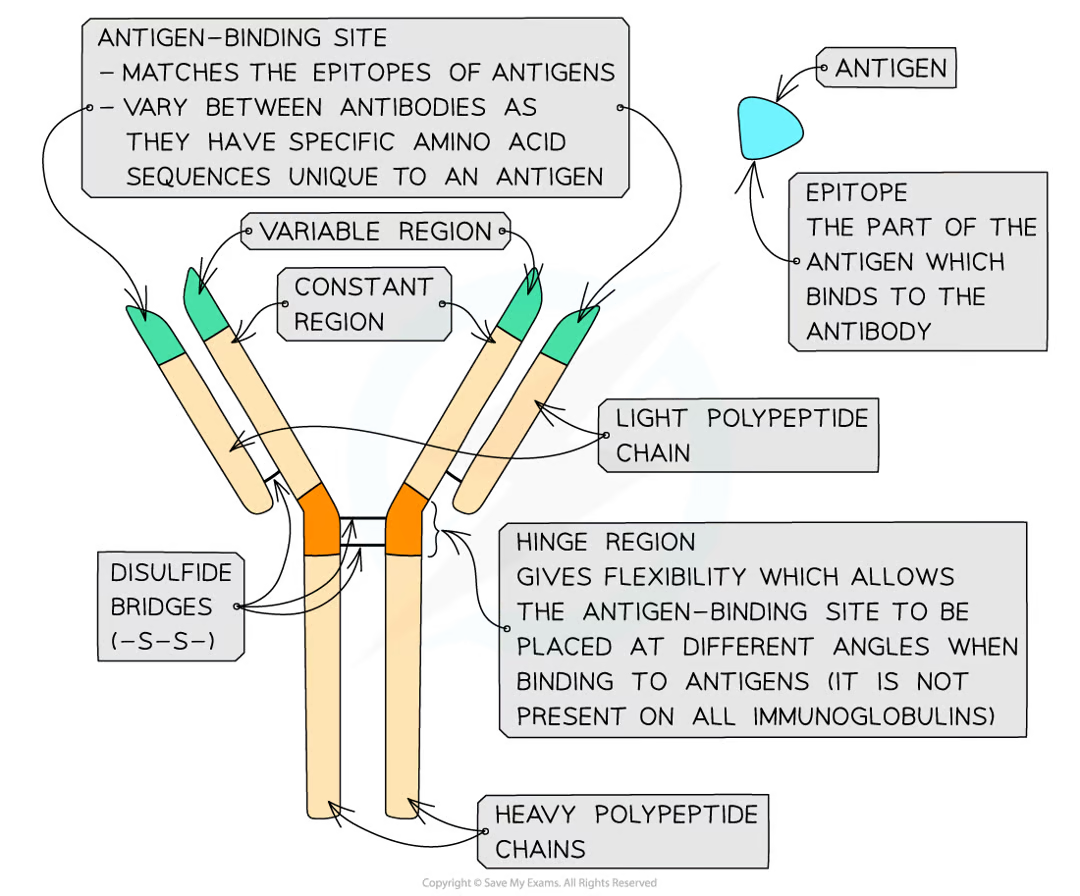
how many types of mammalian antibody are there
there are 5 types
what is the constant region of an antibody for
binding to b cells
what is the variable region of an antibody for
binding to specific antigens to form antigen-antibody complex
what is the hinge region of an antibody
gives flexibility to the antibody and allows antigen binding sites at different angles
antibodies function
destroy pathogens directly or by activating other immune cells. anti-toxins, opsonins, agglutinins
antibodies as antitoxins
binding to toxins produced by pathogens neutralising them
antibodies as opsonins
attatch to pathogens, making them easily identifiable to phagocytes. called opsonisation
antibodies as agglutinins
cause pathogens with antigen antibody complexes to clump together. called agglutination. makes phagocytosis easier
antibodies deactivating pathogens
attatch to bacteria flagella making them less active. phagocytosis easier
antibodies stimulating cell lysis
work with complement protein to cause holes in cell wall and lysis
active natural immunity and example
immune system naturally exposed to pathogen and produces antibodies against it. eg catching a cold
active artificial immunity example
vaccination is an example
active immunity
antigen enters the body triggering a specific immune response
passive immunity
antibodies not produced by infected person
passive natural immmunity example
antibodies passed from mother to child through breastmilk
passive artificial immunity example
injection of antibodies or tetanus antitoxin
what is an autoimmune disease
the immune system attacks one or more self-antigens. targeted towards a single organ or the entire body
rheumatoid arthritis
autoimmune disease that solely affects the joints. begins in the fingers and hands, spreading to shoulders and elsewhere.
rheumatoid arthritis symptoms
muscle spasms, inflamed tendons, lethargy, constant joint pain
causes of autoimmune disease
not fully understood. inheritable
herd immunity
indirect protection from an infectious disease when a population is immune through vaccination or previous infection
ring vaccination
when a person gets an infection, those in close contact are vaccinated against it
what could a vaccine contain
dead or inactivated pathogens, attenuated pathogen strains, harmless version of toxin, isolated antigens, genetically engineered antigens
what is an attenuated pathogen
a weakened version