general and oral pathology final exam
1/252
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
253 Terms
actinic keratosis overview
•Premalignant lesion caused by chronic UV exposure
•Represents early epithelial dysplasia of skin
•Strongly associated with sun-damaged skin
•Precursor to cutaneous squamous cell carcinoma
•Common in fair-skinned older adults
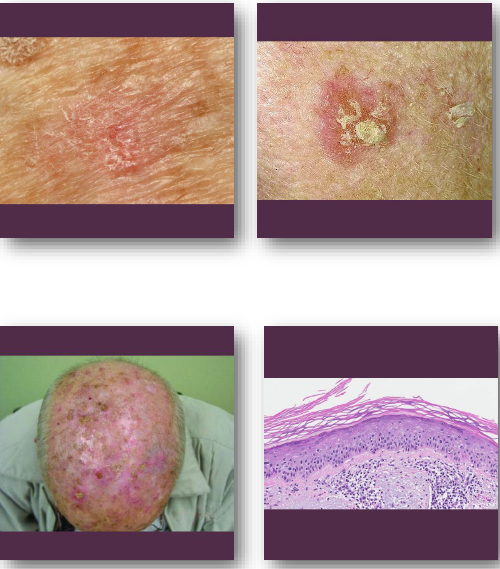
actinic keratosis clinical features
• Rough scaly patch on sun-exposed skin surfaces
• Color ranges from red to tan or brown
• Often easier to feel than to see
• Common on face, ears, and hands
• May be tender or completely asymptomatic
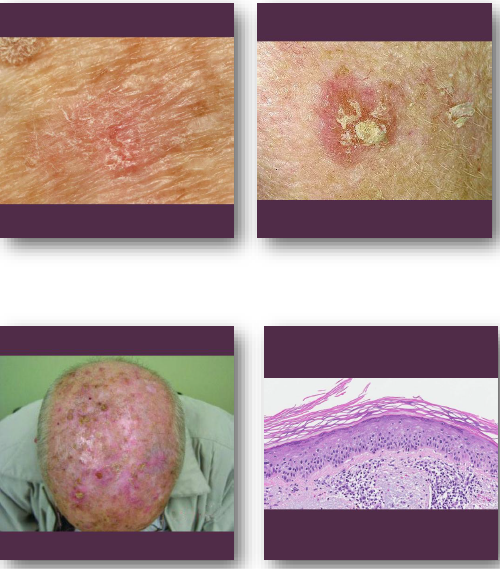
actinic keratosis management and prognosis
• Treated with cryotherapy or topical agents
• Sun protection prevents development of lesions
• Biopsy if lesion thickens or ulcerates
• May progress to squamous cell carcinoma
• Excellent prognosis with early treatment
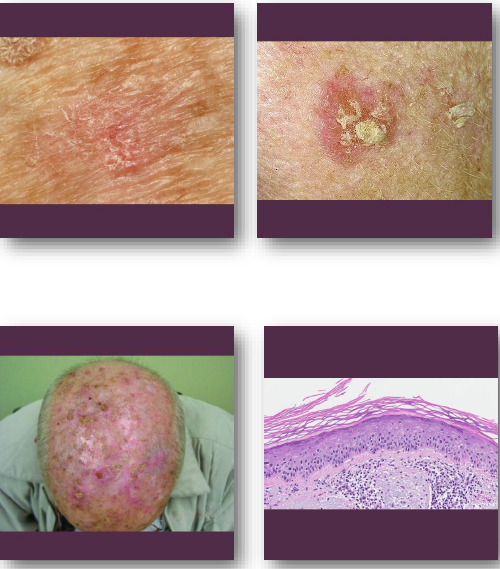
actinic cheilitis overview
•Premalignant lesion of lip from chronic UV exposure
• Represents epithelial dysplasia of vermilion border
•Strongly associated with fair skin and sun exposure
•Most commonly affects lower lip region
•Considered precursor to lip squamous cell carcinoma
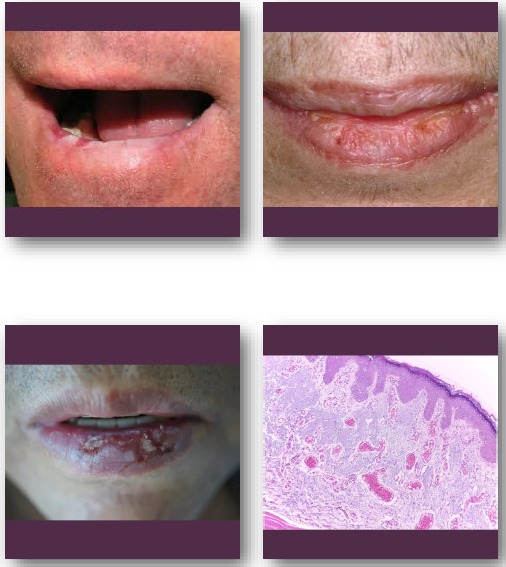
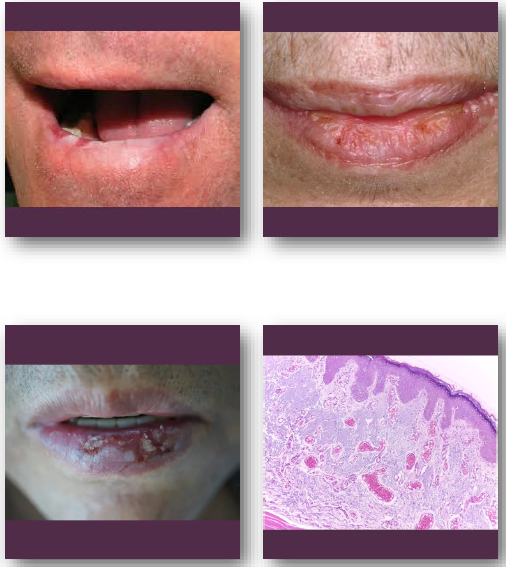
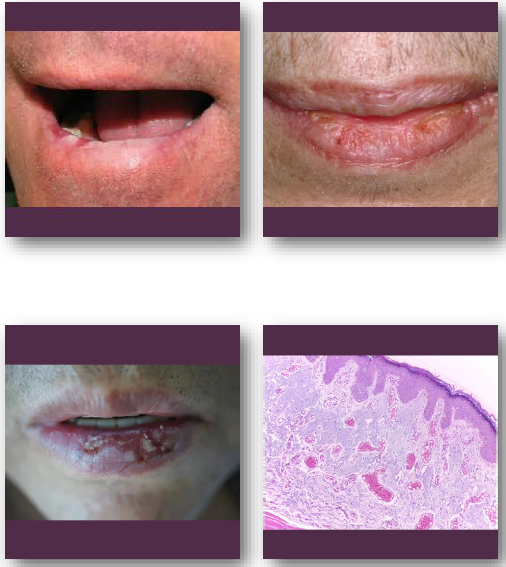
actinic cheilitis clinical feature
•Atrophic, dry, or scaly appearance of lower lip
•Blurring of vermilion border is common finding
•May show fissures, ulceration, or crusting
•Color ranges from pale to erythematous areas
•Usually chronic and slowly progressive
actinic cheilitis management and prognosis
•Biopsy recommended for suspicious or persistent areas
•Sun protection is essential preventive measure
•Topical therapy or surgical treatment may be used
•Regular follow-up required due to cancer risk
•Risk of progression to squamous cell carcinoma
basal cell carcinoma overview
• Most common malignant tumor of the skin
• Arises from basal layer of epithelium
• Strongly associated with UV exposure
• Locally invasive but rarely metastasizes
• Common in fair-skinned individuals
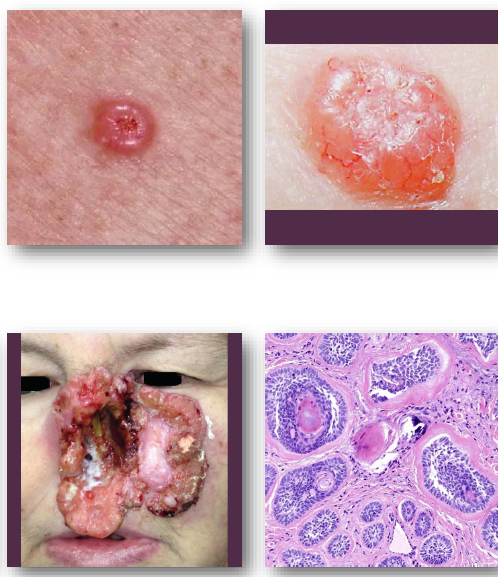
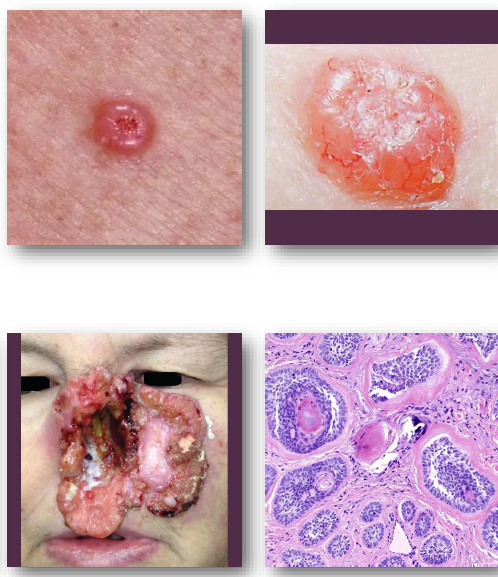
basal cell carcinoma clinical features
pearly papule with rolled and raised borders
central ulceration may be present
surface shows fine blood vessels
common on face and nose region
slow-growing but locally destructive
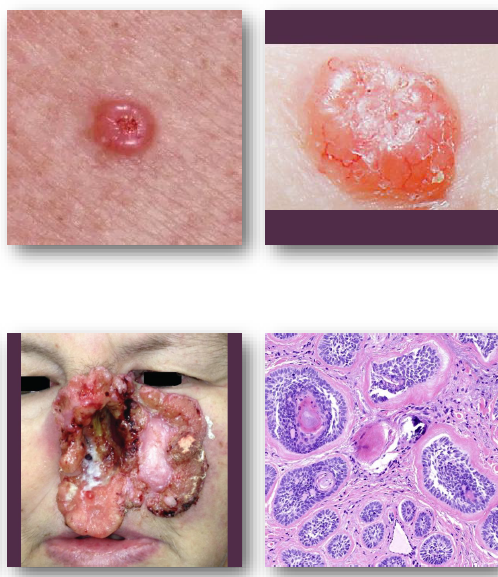
basal cell carcinoma management and prognosis
Surgical excision is treatment of choice
•Mohs surgery used for high-risk areas
•Excellent prognosis with early detection
•Recurrence possible if incompletely removed
•Rarely metastasizes to distant sites
cutaneous squamous cell carcinoma overview
•Malignant tumor of keratinizing epithelium
•Strongly linked to chronic UV exposure
•May arise from actinic keratosis lesions
•More aggressive than basal cell carcinoma
•Risk increased in immunocompromised patients
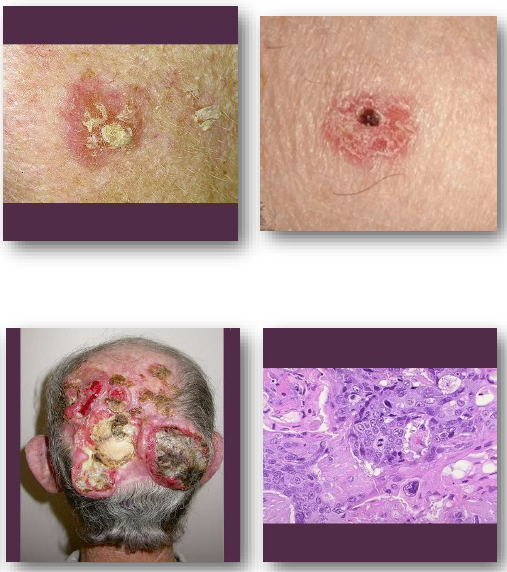
cutaneous squamous cell carcinoma clinical features
•Firm scaly or ulcerated skin lesion
•May present as non-healing ulcer
•Surface may crust or bleed easily
•Common on sun-exposed areas
•Often grows faster than basal cell carcinoma
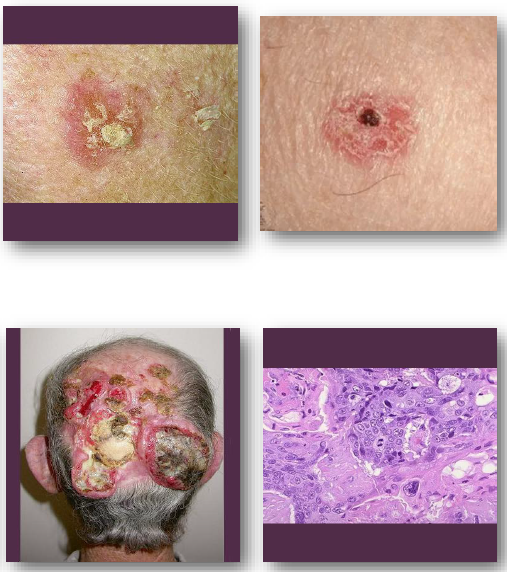
cutaneous squamous cell carcinoma management and prognosis
•Surgical excision with adequate margins required
•Radiation therapy used in selected cases
•Early detection improves clinical outcomes
•Greater risk of metastasis than BCC
•Requires close follow-up after treatment
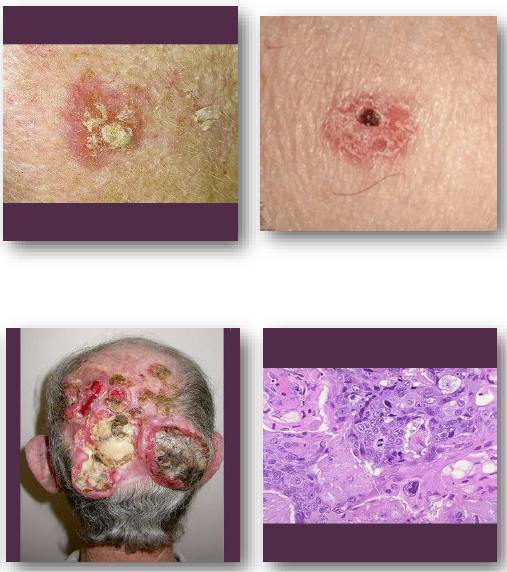
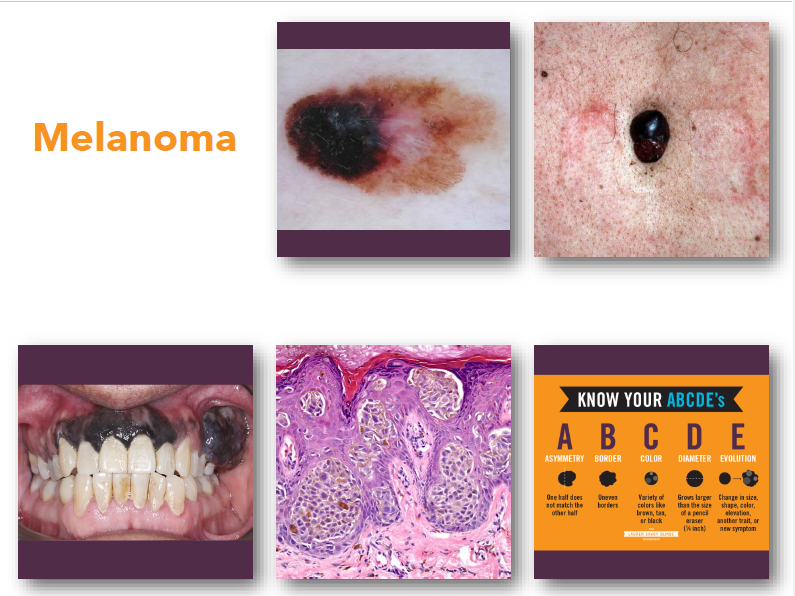
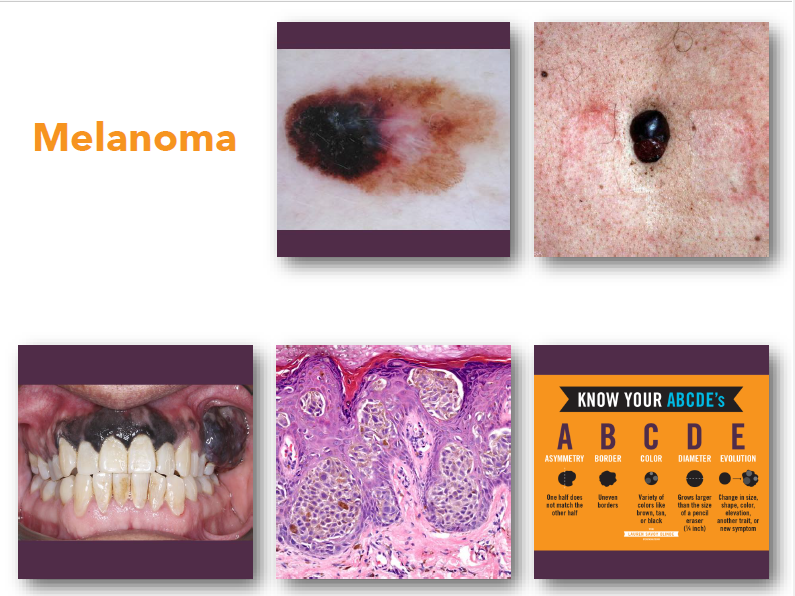
melanoma
•Malignant tumor arising from melanocytes
•Strongly associated with ultraviolet exposure
•Most dangerous form of skin cancer
•Early detection critical for survival
•May occur on skin or mucosal surfaces
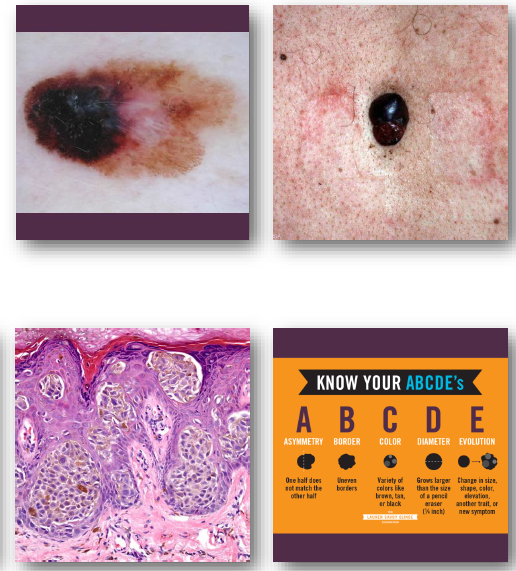
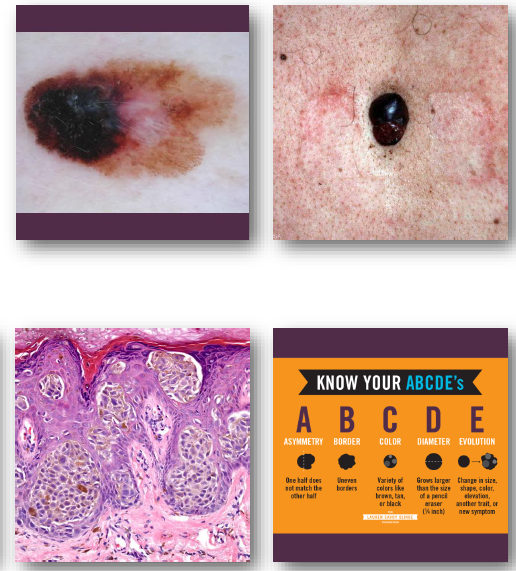
melanoma clinical features
•Irregular asymmetric pigmented lesion
•Varied colors including black and brown
•Borders often irregular or notched
•Diameter often greater than 6 millimeters
•Changes over time are critical warning sign
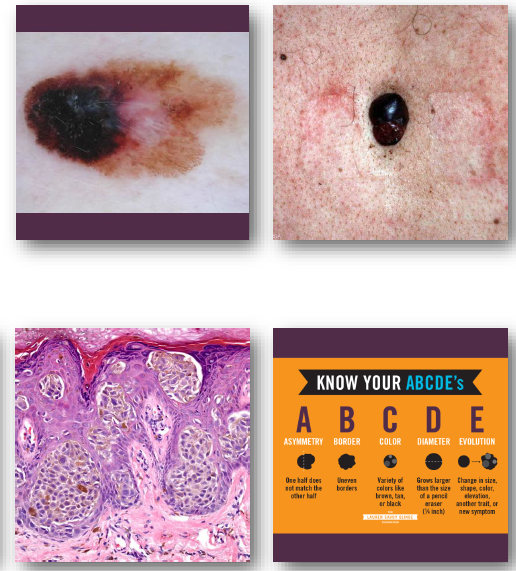
melanoma management and prognosis
•Early surgical excision is essential
•Prognosis depends on depth of invasion
•High risk of metastasis if advanced
•Requires urgent referral and treatment
•Survival improves with early detection
oral squamous cell carcinoma overview
•Most common Malignant tumor of oral stratified epithelium
•Strongly linked to tobacco and alcohol use
•HPV-related cases occur in oropharynx
•Often arises from premalignant lesions
•Includes several aggressive histologic variants
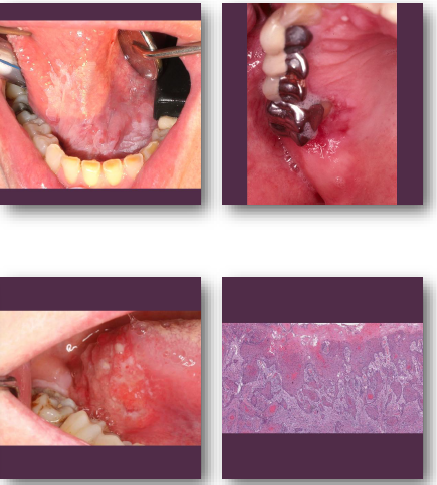
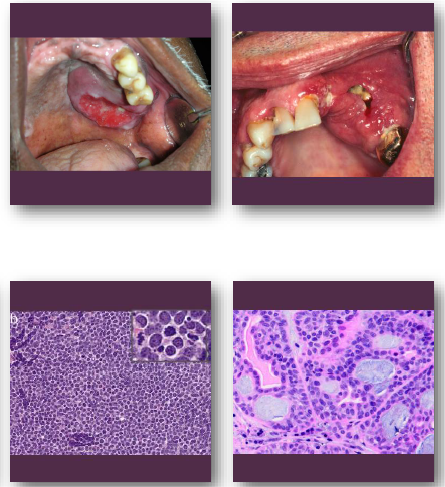
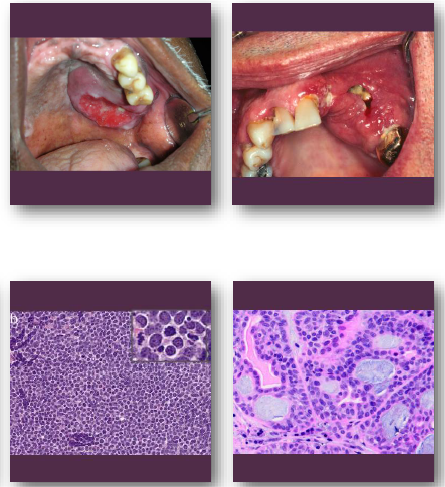
oral squamous cell carcinoma clinical features
•Non-healing ulcer or exophytic mass lesion
•Mixed red and white mucosal appearance
•Induration on palpation is key finding
•Common on tongue and floor of mouth
•May be painless early and painful later
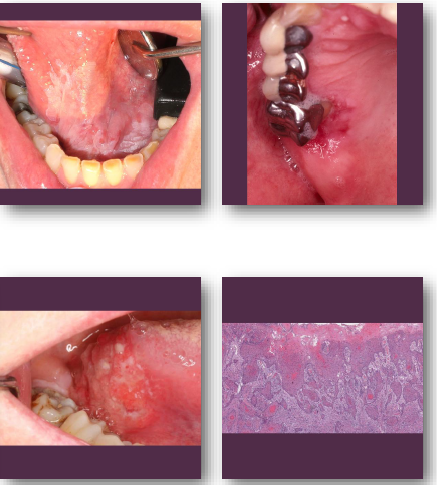
oral squamous cell carcinoma management and prognosis
•Requires biopsy for definitive diagnosis
•Treated with surgery, radiation, chemotherapy
•Prognosis depends on stage at diagnosis
•Variants may show more aggressive behavior
•Risk of recurrence and metastasis exists
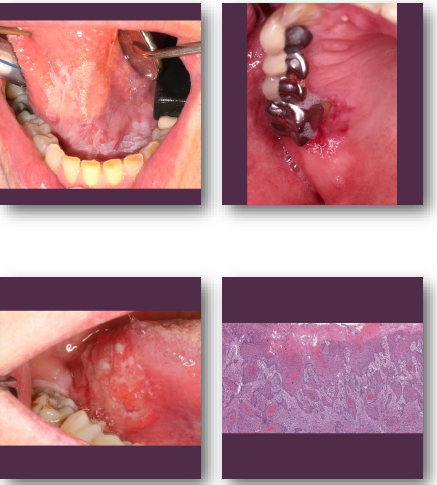
Verrucous carcinoma overview
•Low-grade variant of squamous cell carcinoma
•Strongly associated with tobacco use
•Slow-growing but locally invasive lesion
•Rarely metastasizes to distant sites
•Often arises from leukoplakic lesions
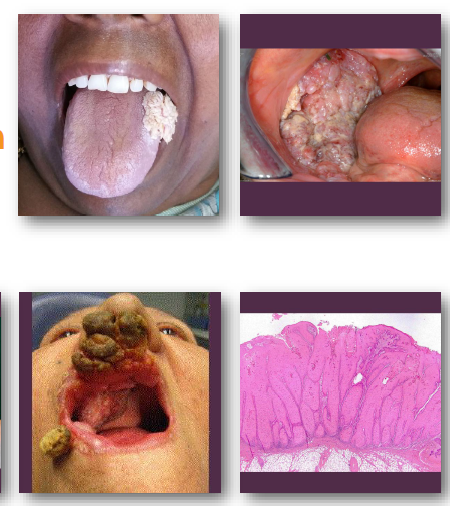
verrucous carcinoma clinical features
•Thick white verrucous or papillary mass lesion
•Broad-based lesion with slow enlargement
•Often involves buccal mucosa or gingiva
•Surface appears rough and warty (verrucous)
•Typically painless in early stages
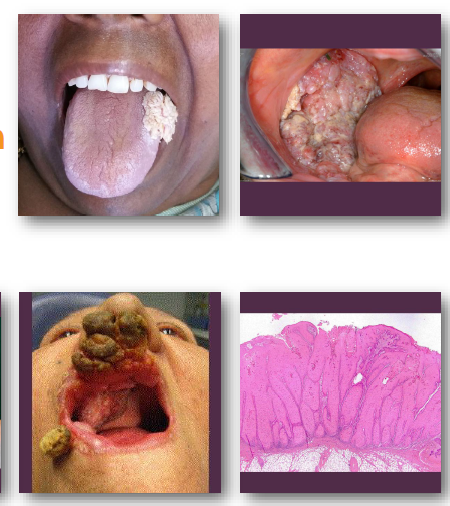
verrucous carcinoma management and prognosis
•Wide surgical excision is treatment of choice
•Radiation often avoided due to risk factors
•Recurrence possible if incompletely removed
•Excellent prognosis compared to SCC
•Very low metastatic potential
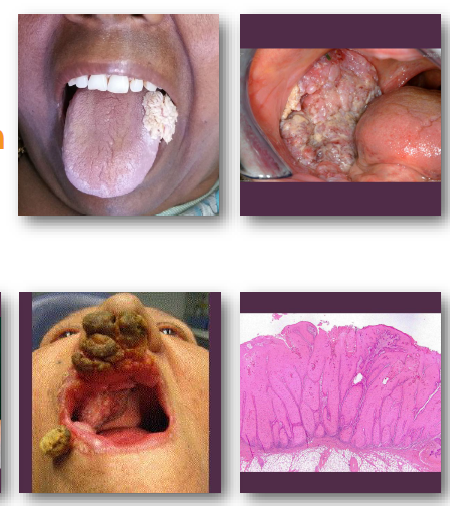
sinonasal papillomas overview
Benign epithelial tumors of sinonasal mucosa
•Includes inverted and exophytic variants
•Associated with HPV infection in some cases
•Locally aggressive with recurrence potential
•Small risk of malignant transformation exists
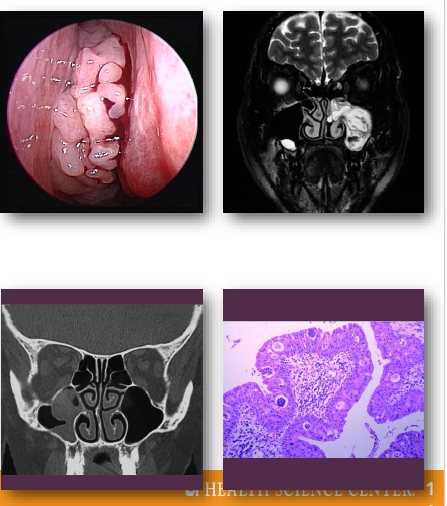
sinonasal papillomas clinical features
•Unilateral nasal obstruction or visible mass
•May present with epistaxis or discharge
•Often arises from lateral nasal wall
•May extend into adjacent sinus spaces
•Symptoms depend on size and location
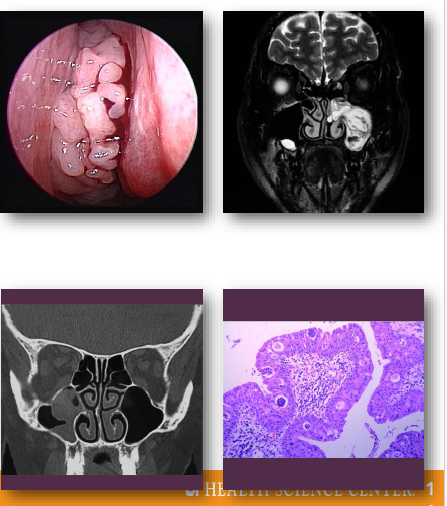
sinonasal papillomas management and prognosis
•Surgical excision required for treatment
Complete removal reduces recurrence risk
•Long-term follow-up recommended
•Recurrence relatively common
•Small risk of malignant transformation
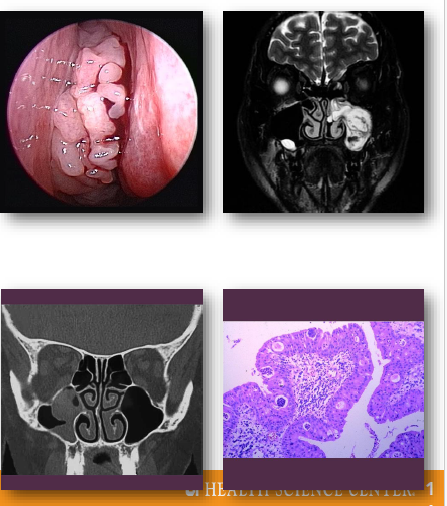
fungiform sinonasal papilloma
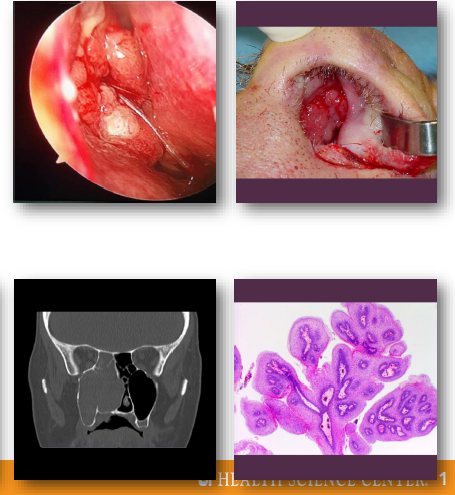
inverted sinonasal papilloma
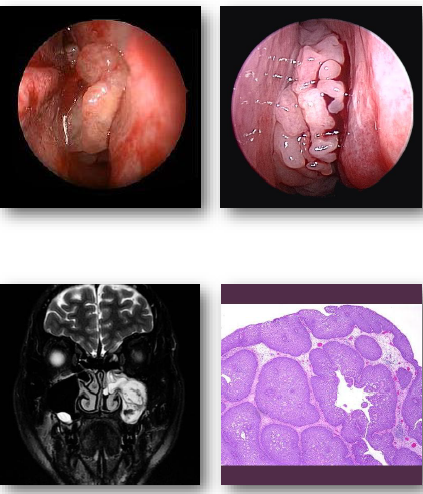
nasoparyngeal carcinoma overview
•Malignant epithelial tumor of nasopharynx
•Strongly associated with Epstein-Barr virus
•Higher incidence in specific populations
•Often presents late due to hidden location
•Early metastasis to regional lymph nodes
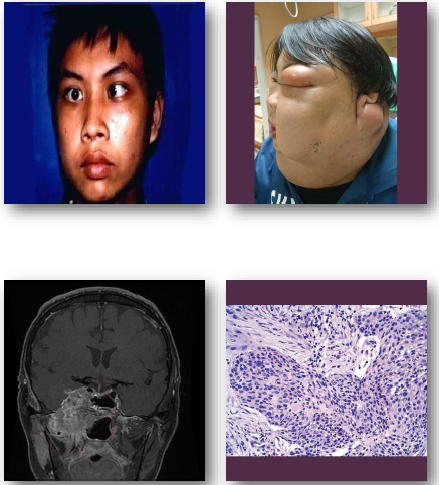
nasopharyngeal carcinoma clinical features
•Nasal obstruction or recurrent epistaxis
•Neck mass from lymph node involvement
•Hearing loss or ear fullness symptoms
•Headache or cranial nerve deficits
•Symptoms often subtle in early stages
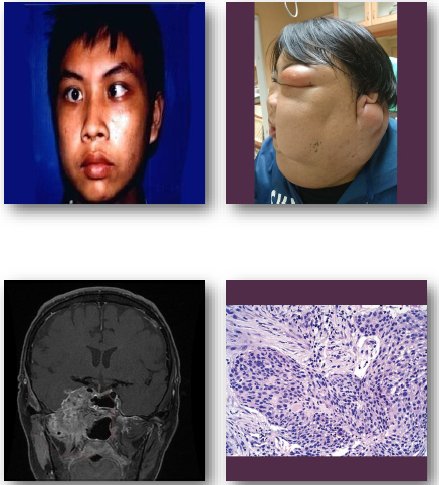
nasopharyngeal carcinoma management and prognosis
•Primarily treated with radiation therapy
•Chemotherapy used for advanced disease
•Prognosis depends on stage at diagnosis
•High risk of regional metastasis
•Early detection improves survival rates
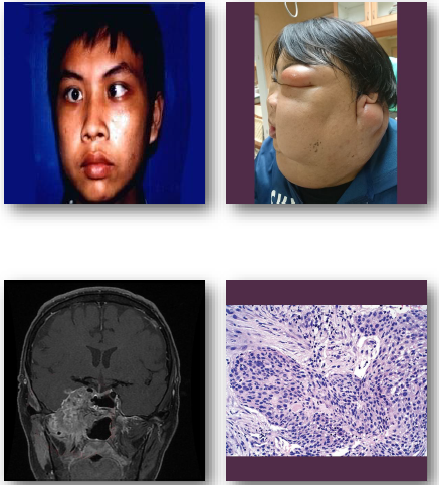
carcinoma of the maxillary sinus overview
•Malignant epithelial tumor of maxillary sinus
•Often squamous cell carcinoma histologically
•Associated with occupational and environmental exposures
•Frequently presents at advanced stage
•Close proximity to orbit and cranial structures
carcinoma of the maxillary sinus management and prognosis
• Requires combined surgical and oncologic therapy
• Radiation therapy commonly included in treatment
• Prognosis depends on stage at diagnosis
•Often poor due to delayed detection
Requires multidisciplinary management approach
oral manifestations of systemic disease
medical history includes a full review of systems
ROS surveys major body systems and functions
oral findings may signal undiagnosed disease or the first sign
some oral signs are specific, others non specific
recognition guides care and medical referral
endocrine system
glands secrete hormones into blood stream
hormones then regulate growth, metabolism, function
target organs respond via specific receptors
negative feedback controls hormone levels tightly
disorders reflect hypo- or hypertension states
pituitary gland overview
has anterior and posterior lobes
• Anterior lobe secretes multiple regulatory hormones
•Hormones include GH, ACTH, TSH, FSH, and LH
•Pituitary hormones regulate multiple target organs
•Not all disorders show oral findings clinically
pituitary hormones
regulate multiple target organs
GH, ACTH, TSH, FSH, and LH
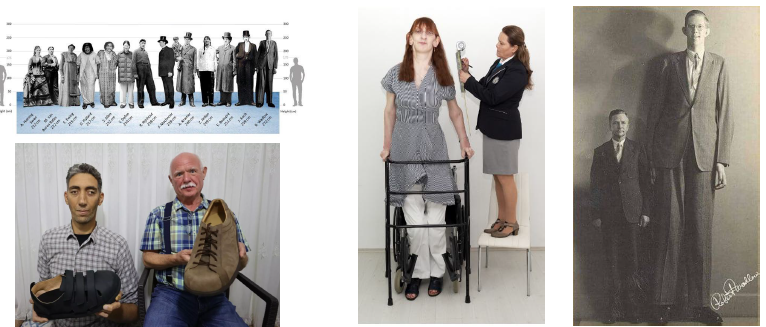
giantism clinical and radiographic features
GH excess in childhood before epiphyseal closure
marked with extreme height, long limbs, and large hands
disproportionate body growth and skeletal size
jaws enlarges with generalized macrodontia
oral structures with normal in form but enlarged
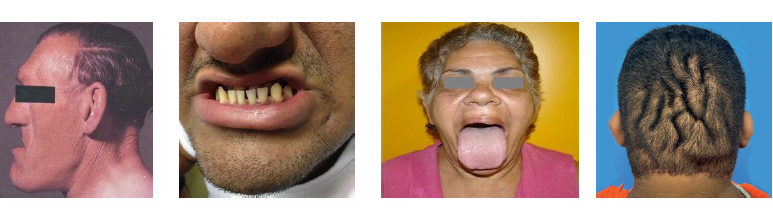
acromegaly clinical and radiographic features
GH excess after closure of epiphyseal plates
enlargement of hands, feet, and facial bones
mandibular prognathism with coarse features
macroglossia with spacing of normal teeth
associated systemic disease risk increased
hypopituitarism overview and etiology
reduced production of one or more pituitary hormones
often involves hypothalamus or anterior pituitary
GH deficiency leads to pituitary dwarfism state
may reflect hormone deficiency or tissue resistance
effects depend on specific hormone deficiency

hypopituitarism clinical and radiographic features
short stature with normal body proportions present
facial structures proportionate but small than normal
maxilla and mandible reduced in overall size
teeth small with delayed eruption patterns
retention of primary teeth may be observed

hypopituitarism management and prognosis
diagnosis based on delayed growth and development
hormone testing confirms specific deficiencies
growth hormone therapy used before plate closure
early treatment improved growth and outcomes
systemic complications depend on underlying cause

non-achondroplastic short stature: overview
•Proportionate short stature due to endocrine causes
•GH deficiency leads to pituitary dwarfism state
•Hypothyroidism causes growth and development delay
•Genetic syndromes produce varied growth patterns
•Chronic disease may impair normal growth
thyroid gland
•Thyroid gland lies anterior to the larynx in neck
•Butterfly shape with two lobes and central isthmus
•Secretes T3 and T4 regulating metabolism rate
•Controlled by TSH from anterior pituitary gland
•Disorders reflect hypo-or hyperthyroid states
hyperthyroidism (graves disease) overview
•Excess T3 and T4 cause hypermetabolic state
•Often due to autoimmune Graves disease process
•Autoantibodies stimulate thyroid continuously
•Leads to thyrotoxicosis with systemic effects
•Most common in women age 20 to 40 years
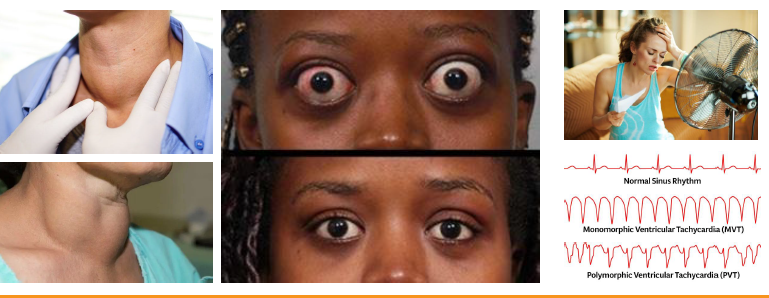
hyperthyroidism (graves disease) clinical features
•Heat intolerance, sweating, anxiety, tremor
•Weight loss despite increased appetite present
•Tachycardia, hypertension, cardiac strain risk
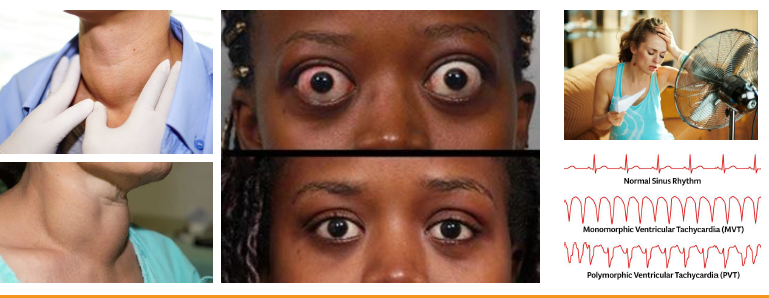
•Exophthalmos with protruding eyes characteristic
•Oral burning, caries, perio risk increased
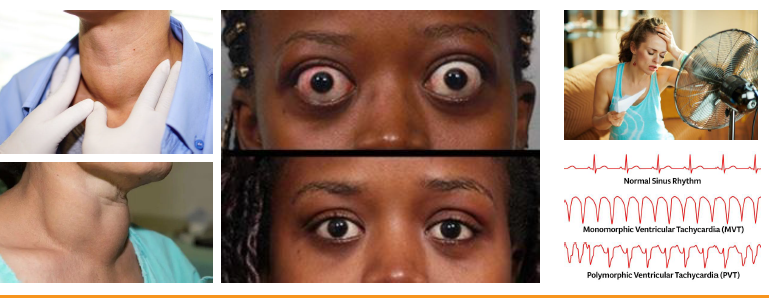
hyperthyroidism (graves) management and diagnosis
•Diagnosis confirmed with labs and iodine uptake
•Beta blockers used to control systemic symptoms
•Monitor for thyroid storm in untreated patients
•Short low stress appointments recommended
•Avoid epinephrine in uncontrolled cases
hypothyroidism overview and etiology
•Deficiency of thyroid hormones T3 and T4 present
•Most commonly due to Hashimoto thyroiditis
•Autoimmune destruction leads to gland failure
•More common in females age 45 to 65 years
•Associated with other autoimmune disorders
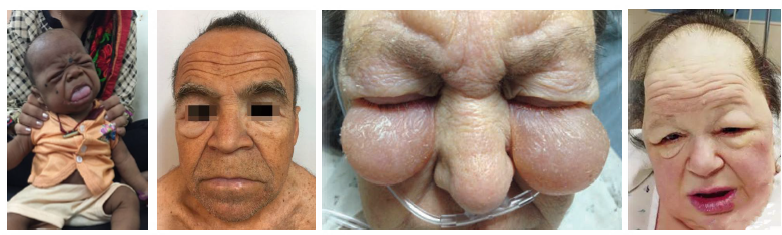
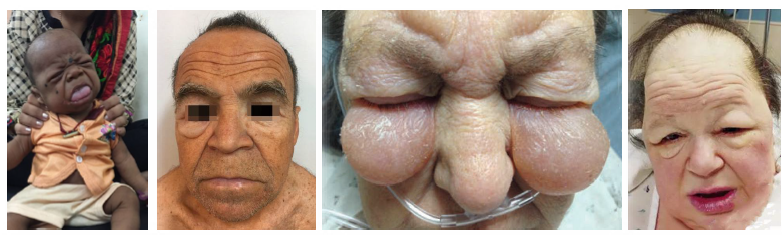
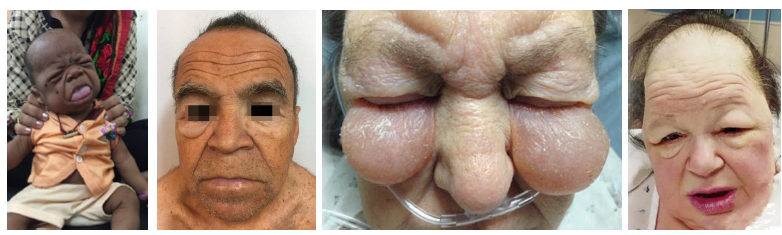
hypothyroidism clinical and radiographic features
Fatigue, weight gain, cold intolerance common
•Bradycardia, slowed metabolism, mental slowing (slow)
•Macroglossia with thick lips and facial features
•Delayed eruption and jaw osteoporosis noted
•Xerostomia and oral changes may be present
hypothyroidism management and prognosis
•Diagnosis confirmed by thyroid hormone levels
•Managed with synthetic thyroid hormone therapy
•Early treatment prevents severe complications
•Monitor for delayed healing and xerostomia
•Dental care modified based on disease control
parathyroid glands
• glands located adjacent to thyroid lobes
•Secrete PTH regulating serum calcium levels
•PTH mobilizes calcium from bone stores
•Increases intestinal absorption and renal retention
•Disorders reflect increased or decreased PTH levels
hyperparathyroidism overview
excess PTH increases serum calcium levels
primary due to tumor or gland hyperplasia
secondary due to chronic hypocalcemia states
renal failure common cause of secondary type
leads to bone resorption and systemic effects
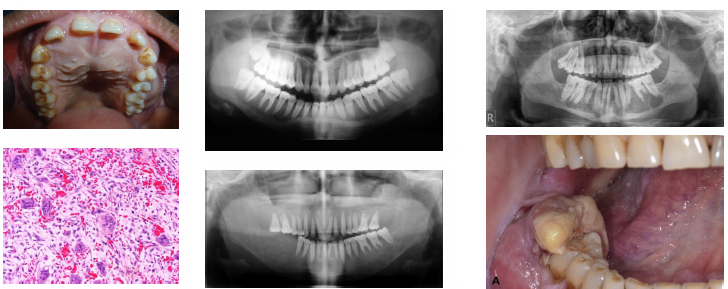
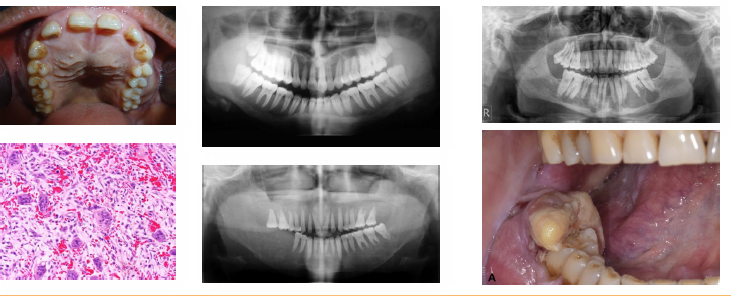
hyperparathyroidism clinical radiographic features
•"Stones bones groans" classic symptom pattern
•Renal stones due to hypercalcemia levels
•Ground glass bone with lamina dura loss
•Brown tumors cause jaw radiolucencies
•Bone and root resorption may be evident
hyperparathyroidism management
•Diagnosis shows elevated PTH and calcium levels
•Primary treated with surgical gland removal
•Secondary managed by correcting hypocalcemia
•Vitamin D and diet used in renal patients
•Dental findings may prompt initial diagnosis
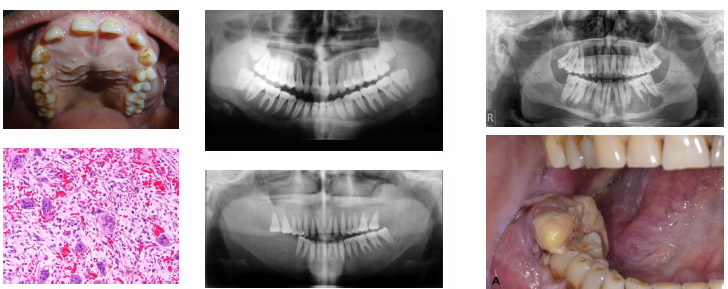
stones, bones, groans,
hyperparathyroid issues
kidney stones, lesions pulled out of bone, groans of pain due to whole process
adrenal glands
sit atop kidneys bilaterally
cortex produces steroid hormones in three zones
aldosterone regulates blood pressure and balance
cortisol controls metabolism and stress response
medulla secrete epinephrine for fight response
cushing syndrome overview and etiology
•Excess cortisol causes hypercortisolism state
•Often due to long term corticosteroid therapy
•Pituitary ACTH tumors may increase cortisol
•Leads to metabolic and systemic disturbances
•Associated with immune suppression effects
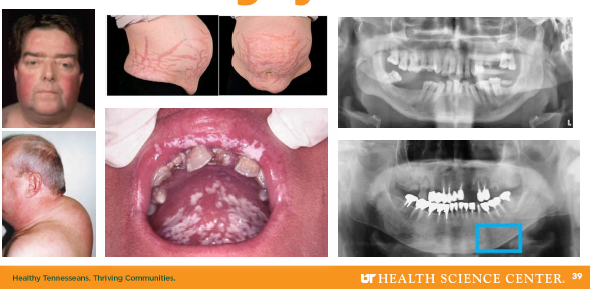
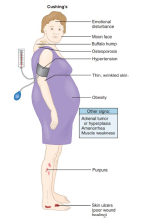
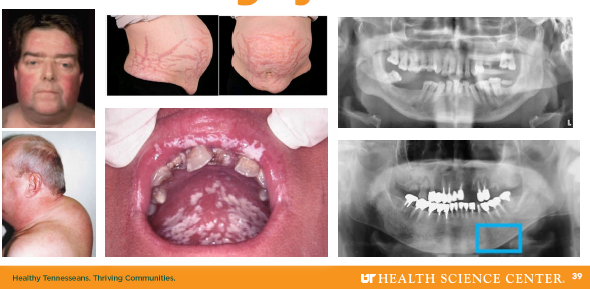
cushing syndrome clinical features
Moon facies and buffalo hump fat deposits
•Truncal obesity with limb muscle wasting (skinny limbs)
•Skin fragility with bruising and striae
•Hyperglycemia and mood disturbances common
•Oral infections and periodontal risk increased
(extra cushion)
cushing syndrome management
Diagnosis via cortisol testing and exam
•Surgical removal for endogenous causes
•Medication cases require careful adjustment
•Monitor infection risk and healing capacity
•Stress dose steroids may be required
addison disease overview and etiology
• Adrenal insufficiency with decreased cortisol levels
•Often due to autoimmune or gland destruction
•May result from infection tumor or hemorrhage
•Leads to metabolic and endocrine dysfunction
•Risk of adrenal crisis during physiologic stress
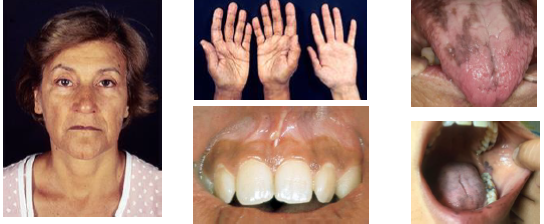
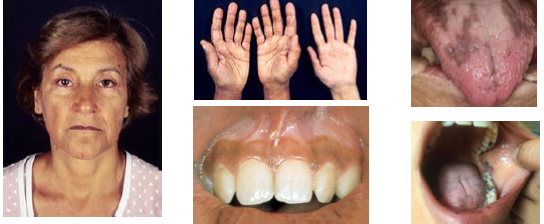
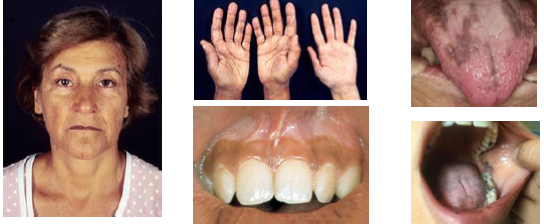
addison’s disease clinical features
• Fatigue weakness weight loss and nausea present
•Hypoglycemia due to cortisol deficiency state
•Diffuse skin hyperpigmentation bronze appearance
•Oral mucosa shows brown macules or patches
•Pigmentation may increase over time gradually
addisons disease management
•Diagnosis confirmed with ACTH stimulation test
•Managed with lifelong corticosteroid replacement
•Monitor for signs of adrenal crisis risk
•Stress reduction critical during dental care
•Early detection improves outcomes significantly
pancreas
•functions as endocrine and exocrine organ
•Beta cells produce insulin in islets of Langerhans
•Insulin released in response to elevated glucose
•Regulates carbohydrate and fat metabolism
•Exocrine pancreas produces digestive enzymes
diabetes mellitus overview and etiology
•Chronic hyperglycemia due to insulin dysfunction
•Type 1 due to autoimmune beta cell destruction
•Type 2 involves insulin resistance and deficiency
•Leads to impaired glucose use and fat metabolism
•Ketoacidosis occurs in uncontrolled cases
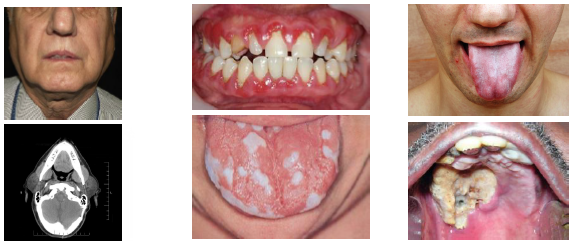
diabetes mellitus clinical features
•Polyuria (frequent urination), polydipsia (frequent drinking), polyphagia (frequent eating) classic triad
•Fatigue weight loss and vision changes present
•Xerostomia and burning mouth symptoms common
•Increased risk of candidiasis and infections
•Periodontal disease risk significantly elevated
diabetes mellitus management
•Control blood glucose with diet and exercise
•Insulin required in type 1 patients
•Type 2 managed with meds and lifestyle changes
•Monitor healing infection and periodontal status
•Screen burning mouth for undiagnosed diabetes
diabetes mellitus clinical implications
•Schedule appointments after meals to reduce risk
•Prevent hypoglycemia during dental procedures
•Glucometer useful for monitoring glucose levels
•Check glucose if patient shows symptoms
•Keep glucose source available for emergencies
acanthosis nigricans overview
•Cutaneous disorder linked to endocrine dysfunction
•Most commonly associated with insulin resistance
•Strongly linked to type 2 diabetes mellitus
•May be drug induced or related to malignancy
•Can signal undiagnosed systemic disease
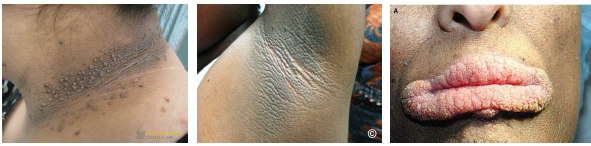
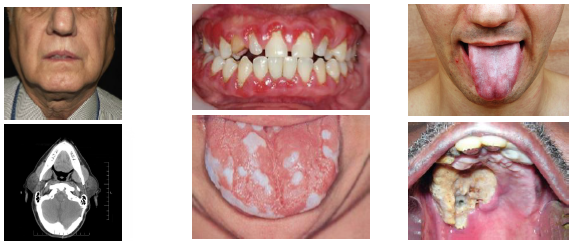
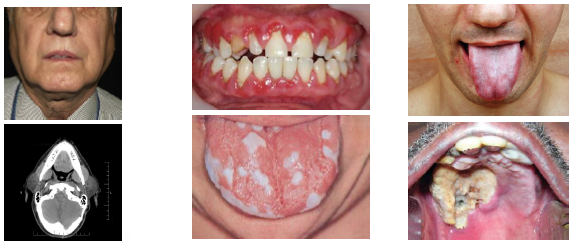
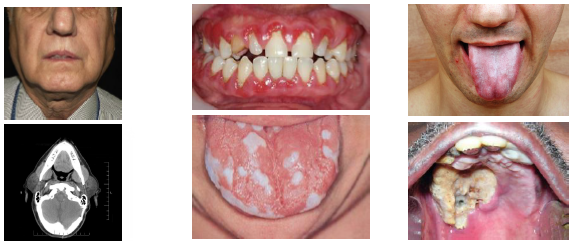
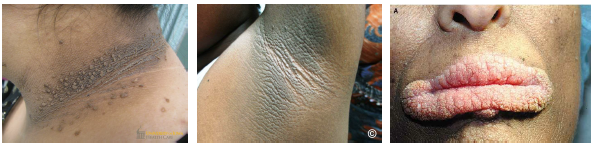
acanthosis nigricans clinical features
•Dark thick velvety skin in flexural areas
•Common in neck axilla groin and skin folds
•May involve lips palate or oral mucosa rarely
•Papillomatosis may appear on lips or palate
•Lesions typically asymptomatic in presentation
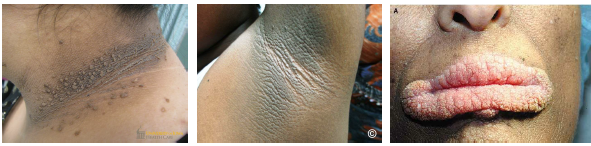
acanthosis nigricans management
•Screen patients for diabetes and insulin resistance
•Evaluate for possible underlying malignancy
•Review medications contributing to condition
•Treat underlying cause to reduce lesions
•Lesions may resolve with systemic control
anemia overview and etiology
•Reduction in RBCs or hemoglobin levels present
•Leads to decreased oxygen carrying capacity
•May result from loss destruction or deficiency
•Causes include iron folate or B12 deficiency
•Associated with chronic disease or malignancy
anemia clinical and radiographic features
•Fatigue weakness dizziness and headaches common
•Pallor of skin and oral mucosa often observed
•Dyspnea and tachycardia in severe cases
•Reduced oxygen leads to systemic symptoms
•Oral mucosa may appear pale clinically
anemia management and prognosis
•Diagnosis based on RBC indices and hematocrit
•Hemoglobin levels assess oxygen carrying status
•Identify and treat underlying cause of anemia
•Postpone elective care if symptoms severe
•Monitor for fatigue dyspnea and weakness
hemoglobinopathies overview and etiology
•Disorders affecting hemoglobin structure or function
•Hemoglobin composed of heme and globin chains
•Globin contains alpha and beta polypeptide chains
•RBC biconcave shape aids gas exchange function
•May be inherited or acquired abnormalities
hemoglobinopathies clinical features and lab findings
•Impaired oxygen transport leads to anemia
•Symptoms include fatigue weakness and pallor
•RBC shape and function may be altered
•Lab findings show abnormal hemoglobin levels
•Severity varies by specific disorder type
hemoglobinopathies managment
•Diagnosis based on hemoglobin analysis tests
•Management depends on specific disorder type
•May require transfusions or supportive care
•Monitor for complications and systemic effects
•Dental care adapted to disease severity
thalassemia overview and etiology
•Inherited disorder with defective hemoglobin production
•Beta thalassemia involves reduced beta chain synthesis
•Minor form has mild anemia and normal iron levels
•Major form lacks normal beta globin production
•Severe anemia develops after birth over time
thalassemia management and prognosis
•Diagnosis based on hemoglobin and genetic testing
•Major form requires regular blood transfusions
•Iron overload may complicate long term care
•Supportive care improves survival outcomes
•Gene therapy shows future treatment potential
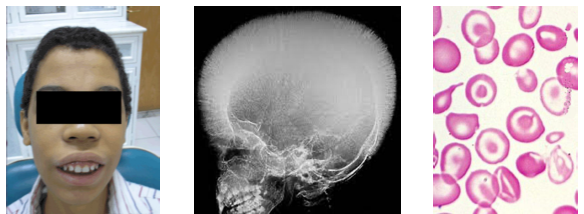
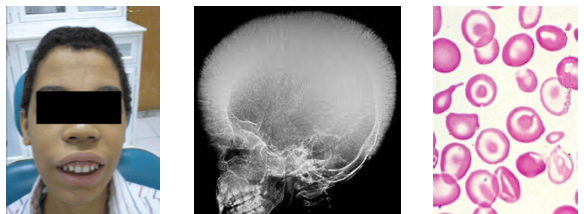
thalassemia clinical and radiographic features
•Growth retardation and hepatosplenomegaly present
•Bone marrow expansion alters facial structure
•Chipmunk facies with maxillary enlargement
•Hair on end skull radiographic appearance
•Delayed eruption and abnormal tooth morphology
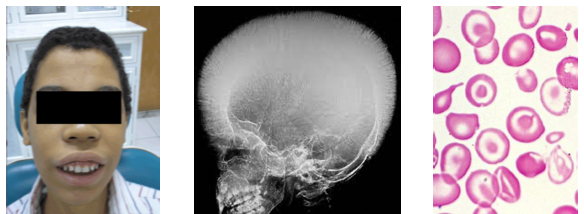
sickle cell disorder overview and etiology
•Inherited mutation in beta globin chain of hemoglobin
•Two genes cause disease one gene causes trait (recessive)
•RBCs become sickle shaped under low oxygen
•Sickling triggered by stress infection dehydration
•Leads to vessel obstruction and tissue ischemia
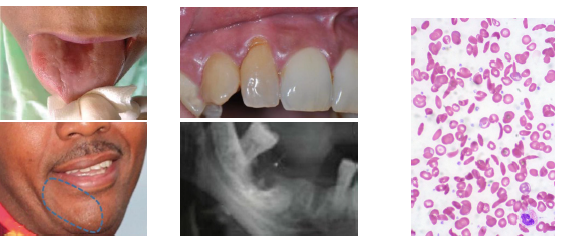
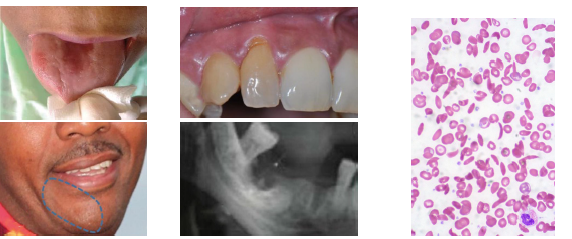
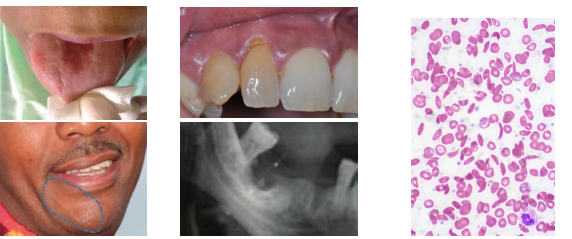
sickle cell disorder clinical features
•Painful sickle cell crises from tissue ischemia
•Delayed growth and tooth eruption in children
•Pale mucosa and loss of tongue papillae
•Oral ulcers and angular cheilitis may occur
•Radiographs show hair on end bone pattern
sickle cell disorder management
•Prevent crisis by reducing stress and infection
•Antibiotic prophylaxis often recommended
•Short appointments reduce physiologic stress
•Avoid hypoxia during dental procedures
•Epinephrine use may be limited cautiously
iron deficiency anemia overview
•Most common anemia worldwide affecting populations
•Caused by reduced iron availability or absorption
•Seen in children women and elderly patients
•May result from diet demand or blood loss
•GI disease may impair iron absorption significantly
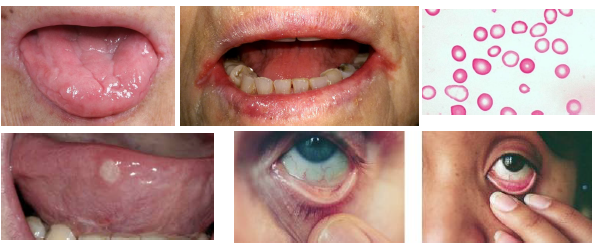
iron deficiency anemia clinical features
•Atrophic glossitis with smooth glossy tongue
•Angular cheilitis at commissures common finding
•Burning tongue symptoms may be reported
•Oral mucosa appears pale on examination
•Increased risk of candidiasis infections
generally not good if male presents, could indicate more serious implications such as a GI bleed
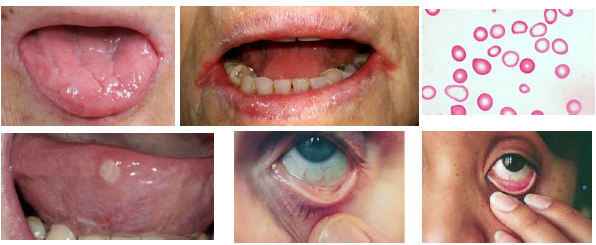
iron deficiency anemia management
•Diagnosis based on iron studies and RBC indices
•Management includes dietary iron supplementation
•Treat underlying cause of deficiency present
•Severe cases may require parenteral iron therapy
•Symptoms improve with correction of deficiency
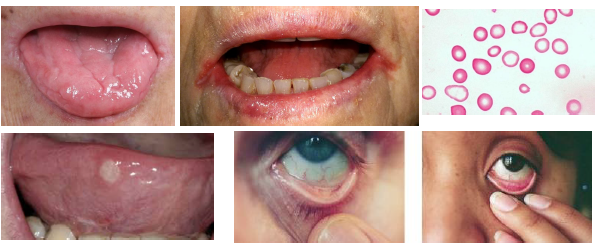
plummer-vinison syndrome overview
•Syndrome seen most often in postmenopausal women
•Triad includes glossitis dysphagia and anemia
•Caused by chronic iron deficiency anemia
•Esophageal webbing leads to swallowing difficulty
•Considered premalignant condition with cancer risk
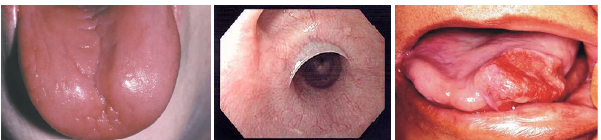
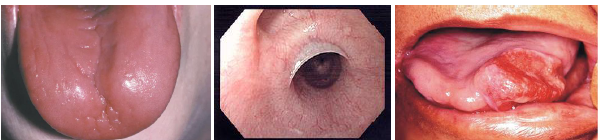
plummer vinison syndrome clinical features
•Tongue smooth shiny and erythematous surface
•Burning sensation of tongue commonly reported
•Dysphagia due to esophageal web formation
•Oral mucosa may appear pale clinically
•Increased cancer risk in oral tissues present
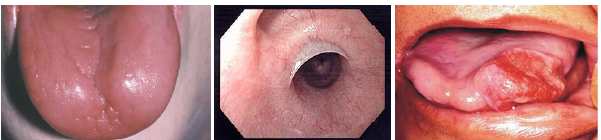
plummer-vinison syndrome management
•Treat with iron supplementation to correct anemia
•Monitor for oral and esophageal malignancy
•Refer for evaluation of swallowing difficulty
•Delay elective care if severe anemia present
•Regular follow up important for early detection
pernicious anemia overview and etiology
•Autoimmune destruction of gastric parietal cells
•Loss of intrinsic factor impairs B12 absorption
•Leads to defective red blood cell production
•Associated with atrophic gastritis and cancer risk
•Seen in gastric surgery or strict vegetarian diets
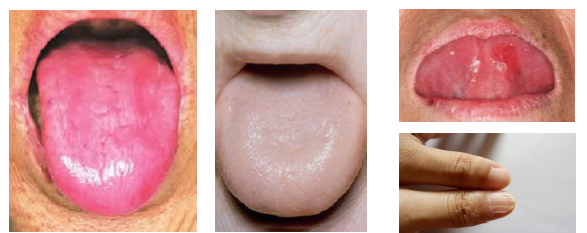
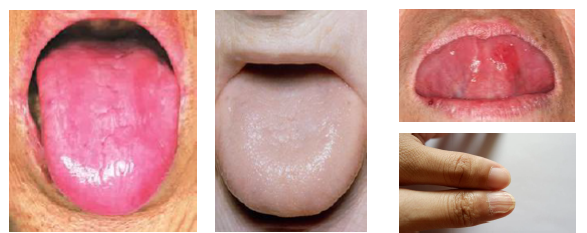
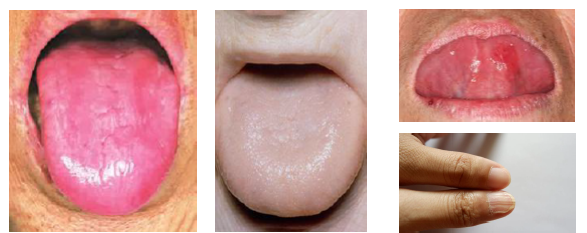
pernicious anemia clinical features
•Fatigue weakness dizziness and dyspnea common
•Neurologic symptoms include numbness tingling
•Burning tongue and oral discomfort present
•Patchy erythema and mucosal atrophy noted
•Glossitis with smooth depapillated tongue
pernicious anemia management
•Diagnose with vitamin B12 level testing
•Manage with B12 injections or nasal therapy
•Oral lesions improve with treatment correction
•Refer patients with burning tongue symptoms
•Monitor for gastric cancer risk long term
bleeding disorders overview / etiology
•Disorders impair normal blood clotting process
•Caused by platelet or clotting factor defects
•May result from disease or medication effects
•Liver produces most clotting factors in blood
•Deficiency leads to prolonged bleeding risk
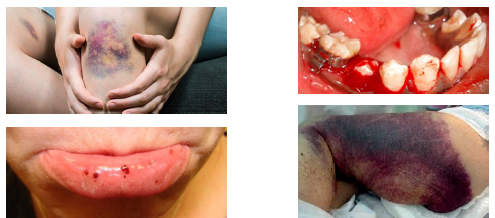
bleeding disorders clinical features
•Easy bruising and mucosal bleeding common
•Petechiae small pinpoint hemorrhages present
•Purpura larger red purple mucosal lesions
•Ecchymosis large bruise like discolorations
•Lesion color changes as blood breakdown occurs
bleeding disorders management
Evaluate history of bleeding and medications
•Lab tests assess clotting factors and platelets
•Modify treatment to reduce bleeding risk
•Avoid trauma during dental procedures
•Coordinate care with physician when needed
polycythemia vera overview and etiology
•Overproduction of red blood cells increases viscosity
•May also increase white cells and platelets
•More common in elderly males population
•Thickened blood slows circulation significantly
•Increased risk of thrombosis and vascular events
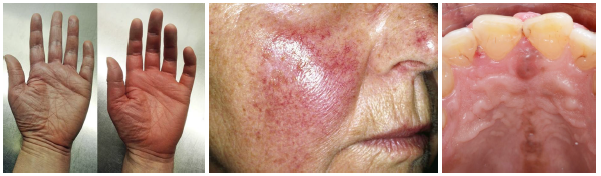
polycythemia vera clinical features
•Fatigue dizziness headaches and dyspnea common
•Cyanosis due to reduced oxygen delivery present
•Hypertension frequently observed clinically
•Gingival bleeding may occur spontaneously
•Thrombosis and hemorrhage may alternate
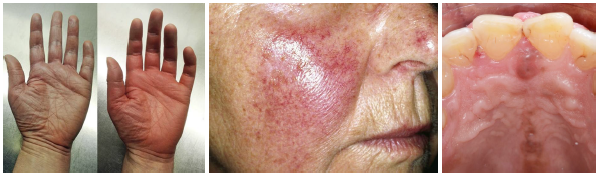
polycythemia vera management
•Managed with phlebotomy to reduce RBC volume
•Anticoagulants used to prevent thrombosis
•Assess bleeding risk before dental treatment
•Monitor for clotting and hemorrhage episodes
•Coordinate care with physician prior to care
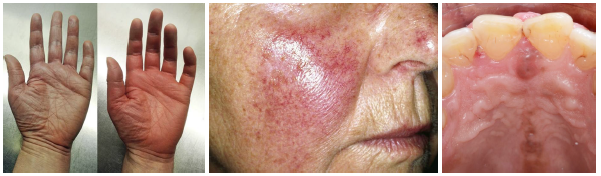
hemophilia / von Willebrand disease overview and etiology
•Bleeding disorders due to clotting factor deficiency
• Includes hemophilia A B and von Willebrand disease
• vWD due to defective platelet adhesion protein
•Hemophilia involves missing clotting factors VIII IX
•Inherited or acquired disorders affect hemostasis
hemophilia / von Willebrand clinical features
easy bruising and prolonged bleeding common
Nosebleeds and gingival bleeding often present
•Bleeding after dental procedures prolonged
•Severity varies from mild to life threatening
•May remain undiagnosed until trauma occurs
hemophilia / von Willebrand management
•Diagnose with clotting factor and platelet testing
•Avoid aspirin and NSAIDs due to bleeding risk
•Factor replacement therapy may be required
•Plan procedures to minimize bleeding trauma
•Coordinate care with physician before treatment
hemophilia A overview / etiology
•Inherited deficiency of clotting factor VIII
•Most common form of hemophilia disorder
•X linked recessive trait affects mostly males
•Carrier mothers pass gene to affected sons
•Severity depends on factor VIII levels present
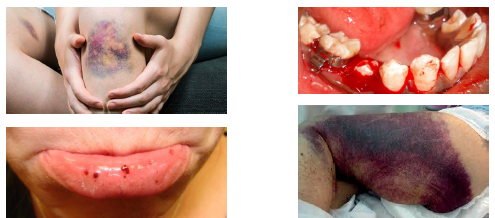
hemophilia A clinical features
•Prolonged bleeding after injury or procedures
•Spontaneous bleeding in severe cases possible
•Hemarthrosis causes joint pain and swelling
•Gingival bleeding may occur clinically
•Severity correlates with factor deficiency level