Higher Cortical Functions
1/58
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
59 Terms
Cerebral Cortex
is “executive suite” of brain
Site of conscious mind: awareness, sensory perception, voluntary motor initiation, communication, memory, storage, understanding
Thin (2–4 mm) superficial layer of gray matter
Composed of neuron cell bodies, dendrites, glial cells, and blood vessels, but no axons
40% of total brain mass
Conscious behavior involves entire cortex in one way or another
right hemisphere receives info from…
left side of the body (contralateral)
left hemisphere receives info from…
right side of the body (contralateral)
Lateralization
certain functions only occur in only one hemisphere
i.e. speech in left
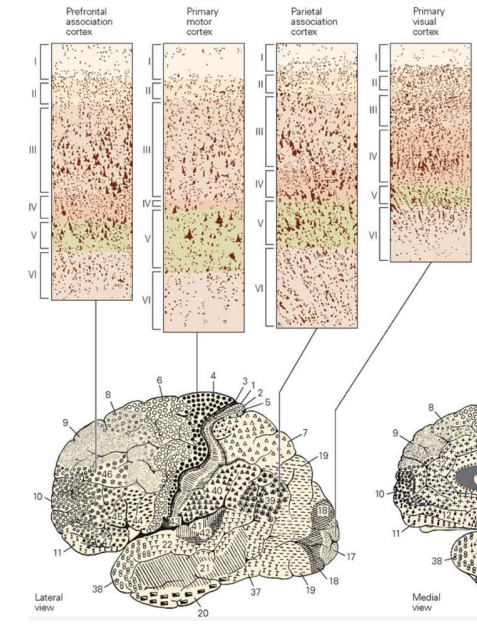
Cell layer of sensory areas of cortex
Sensory areas of cortex, such as the primary visual cortex, tend to have a very prominent internal granular cell layer (layer IV),
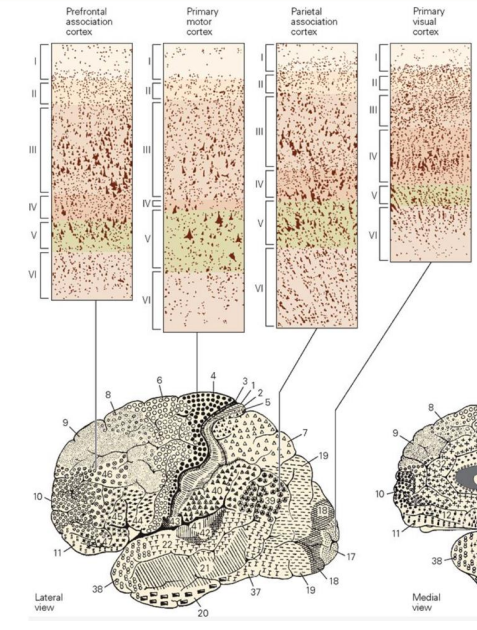
Cell layer of motor cortex
have a very meager layer IV but prominent output layers, such as layer V.
3 types of functional areas of cerebral cortex
Motor areas: control voluntary movement
Sensory areas: conscious awareness of sensation
Association areas: integrate diverse information
not attached to one cortical function
CT and MRI
allow for quick identification of
tumors
intercranial lesions
plaque
or areas of infarct (dead brain tissue)
PET scans
localize brain lesions that generate seizures
based on metabolism
how much metabolic activity is occurring in each brain region
Radioactive tracer dyes
help visualize specific areas
Functional imaging (fMRI)
monitor where blood flows in the brain
does not monitor electrical signals
identify parts of brain that contribute to certain functions
fMRI of brain show specific motor and sensory functions located in discrete cortical areas called domains
Higher functions are spread over many areas
Brain waves
are patterns of neuronal electrical activity recorded
Reflect electrical activity of higher mental functions
Normal brain functions are continuous and hard to measure
EEG
Electroencephalogram (EEG) records electrical activity that accompanies brain function
Electrodes placed on scalp measure electrical potential differences between various cortical areas
Function of EEG
Used for diagnosing epilepsy and sleep disorders
Localizes lesions, tumors, infarcts, infections, abscesses
Used in research and also to determine brain death
What does EEG measure
EEG measures patterns of neuronal electrical activity generated by synaptic activity in cortex
Each person’s brain waves are unique
Patterns change with age, sensory stimuli, brain disease, and chemical state of body
Measures wave frequency in Hertz (Hz)
based on numbers of peaks per second (1 Hz = 1 peak/second)
How are brain waves classified
Can be grouped into four classes based on Hz:
Alpha, beta, theta, or delta waves
(from most active→ to least active)
Alpha waves
(8–13 Hz)—regular and rhythmic, low amplitude, synchronous waves indicating an “idling” brain
occur when someone is awake
Beta waves
(14–30 Hz)—rhythmic, less regular waves occurring when mentally alert
occur while awake and need to play close attention to something
Theta waves
(4–7 Hz)—more irregular; common in children and uncommon in awake adults
Delta waves
(4 Hz or less)—high-amplitude waves of deep sleep and when reticular activating system is suppressed, as during anesthesia; indicates brain damage in awake adult
Language
implementation system involves association cortex of left hemisphere include Broca’s area and Wernicke’s area
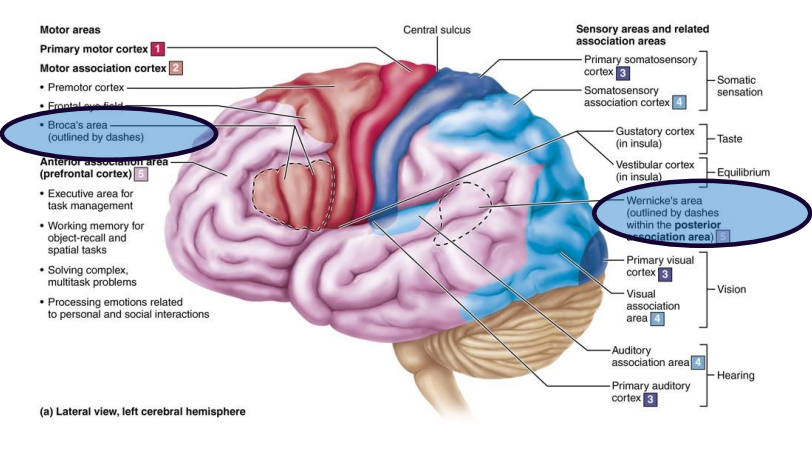
Broca’s area
involved in speech production
Patients with lesions in Broca’s understand words, but cannot speak
Wernicke’s area
involved in understanding spoken and written words
Patients with lesions in Wernicke’s can speak, but words are nonsensible
right hemisphere function
involved with nonverbal language component
Memory
production of memory + storage and retrieval of information
Different kinds of memory
Declarative (fact) memory:
(names, faces, words, dates, events)
Nondeclarative memory
Procedural (skills) memory:
(playing piano)
Motor memory:
memory of motor skills (riding a bike)
Emotional memory:
memory of experiences linked to an emotion (heart pounding when you hear rattlesnake)
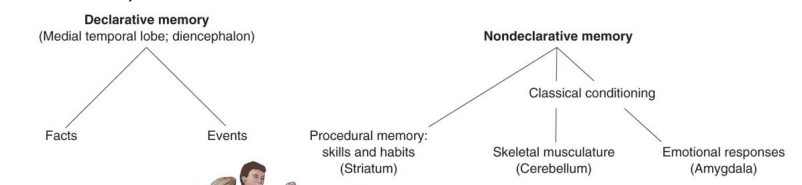
2 stages of declarative memory storage
Short-term memory (STM, or working memory): temporary holding of information
Limited to seven or eight pieces of information
Long-term memory (LTM) has limitless capacity
Factors affecting info transfer from STM to LTM
Emotional state: best if alert, motivated, surprised, or aroused
Rehearsal: repetition and practice
Association: connecting new information with old memories
Automatic memory: subconscious information stored in LTM
Memory consolidation
involves fitting new facts into categories already stored in cerebral cortex
Parts of brain involved in memory consolidation
Hippocampus
temporal cortical areas
thalamus
prefrontal cortex
Memory processing
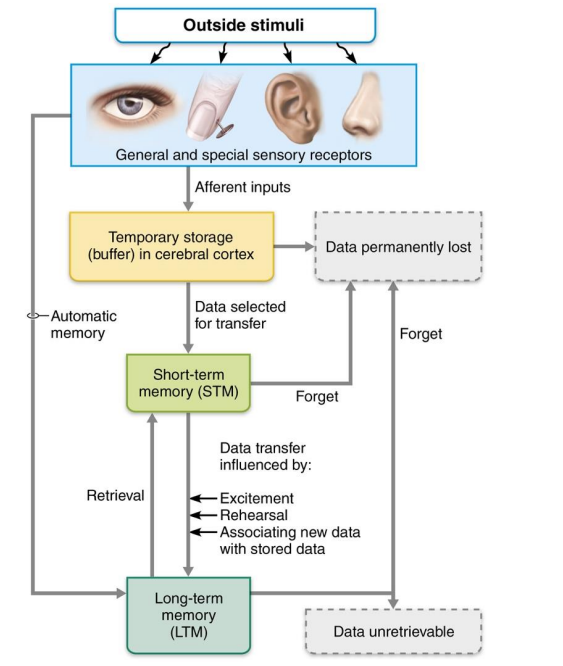
Damage to hippocampus can lead to…
Damage to hippocampus or surrounding temporal lobe structures on either side results in only slight memory loss
Bilateral(both sides) destruction causes widespread amnesia
Anterograde amnesia
consolidated memories are not lost, but new inputs are not associated with old one
Person lives in the here and now
person cannot form NEW memories
Memory of conversations from just 5 minutes before would not be remembered
Retrograde amnesia
loss of memories formed in the distant past
problem with retrieval of memories
What does consciousness involve
Perception of sensation
Voluntary initiation and control of movement
Capabilities associated with higher mental processing (memory, logic, judgment, etc.
Clinically defined on continuum that grades behavior in response to stimuli:
Alertness
Drowsiness (lethargy)
Stupor
Coma
Fainting or syncope
brief loss of consciousness
Most often due to inadequate cerebral blood flow
Due to low blood pressure or ischemia from hemorrhage or sudden, severe emotional stress
Coma
unconsciousness for extended period
Not the same as deep sleep; oxygen consumption is lowered
Brain death
irreversible coma
Ethical and legal issues surround decisions on whether person is dead or alive
Epileptic seizure
torrent of electrical discharges by groups of brain neurons
Prevent any other messages from getting through
Victim of epilepsy may lose consciousness, fall stiffly, and have uncontrollable jerking
Epilepsy occurs in 1 of 100 people
Epilepsy is not associated with intellectual impairments
Genetic factors play a role, but brain injuries, stroke, infections, or tumors can also be causes
Absence seizures
aka petit mal
Mild seizures in which expression goes blank for few seconds
Typically disappear by age 10
malfunction of Ca2+ channels in thalamus
can resolve on its own
Tonic-clonic seizures
aka grand mal
Most severe→ last few minutes
Victim loses consciousness, bones broken during intense convulsions, loss of bowel and bladder control, and severe biting of tongue are common
Aura
(sensory hallucination)
may precede seizure
constant sensory input triggers the seizures
Control of epilepsy involves…
anticonvulsive drugs
Vagus nerve stimulator or deep brain stimulator implantations deliver pulses to vagus nerve or directly to brain to stabilize brain’s electrical activity
Sleep
state of partial unconsciousness from which person can be aroused by stimulation
Cortical activity is depressed, but brain stem activity doesn’t change
2 types of sleep
Non–rapid eye movement (non-REM) sleep
Rapid eye movement (REM) sleep
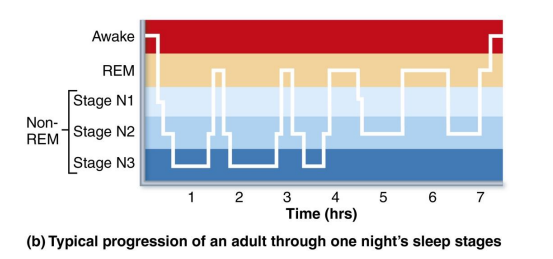
Sleep-wake cycle
During the first 30–45 minutes of the sleep cycle, pass through first two stages (N1 and N2) of non-REM, then move into stage 3 called slow-wave sleep

REM sleep
EEG, blood pressure, and heart rate decrease
About 90 minutes in the REM sleep begins abruptly
Temporary paralysis, except for rapid eye movements
Heart rate, respiratory rate, and blood pressure increase; oxygen consumption increases greater than when awake
Most dreaming occurs in REM
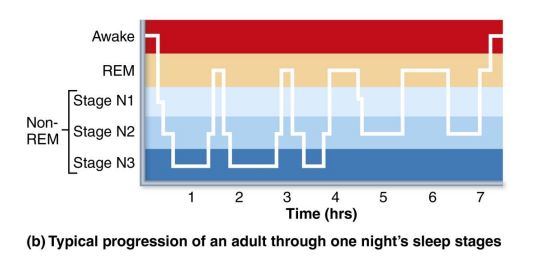
How is sleep regulated by brain
Alternating cycles of sleep and wakefulness reflect natural circadian (24-hour) rhythm
Suprachiasmatic nucleus (a biological clock) and preoptic nucleus (a sleep-inducing center) of hypothalamus regulate timing of sleep cycle
Hypothalamus releases orexins that help cortex to wake up
Why is sleep important
is the restorative stage
consolidation of new memories and discarding memories no longer accessed
During non-REM sleep pulses of cerebrospinal fluid sweep through brain, aiding in washing out of waste products, including some associated with Alzheimer’s disease
When deprived of sleep, spend more time in REM and slow-wave sleep n next sleep episode attempting to catch up
Narcolepsy
sleep disorder involving abrupt lapse into sleep from awake state
Orexins (hypothalmic “wake-up” chemicals) probably destroyed by patient’s immune system; orexin replacement possible treatment
Insonmia
Chronic inability to obtain amount or quality of sleep needed, possibly caused by depression, anxiety, overuse of caffeine, computer/cell phone use too close to bedtime
May be treated by blocking orexin action
Traumatic brain injuries
include:
Concussion: temporary alteration in function
Contusion: permanent damage
Subdural or subarachnoid hemorrhage: pressure from blood may force brain stem through foramen magnum, resulting in death
Cerebral edema: swelling of brain associated with traumatic head injury
Cerebrovascular accidents
AKA strokes
Ischemia: tissue deprived of blood supply, leading to death of brain tissue
Can be caused by blockage of cerebral artery by blood clot
Hemiplegia (paralysis on one side of body) sensory and speech deficits may result
Transient ischemic attacks (TIAs): temporary episodes of reversible cerebral ischemia
benign
Alzheimer’s disease (AD)
Progressive degenerative disease of brain that results in dementia (mental deterioration)
Memory loss of recent events, shortened attention span, disorientation, eventual language loss, irritability, moodiness, and confusion
What causes Alzheimer’s disease
Caused by misfolding of proteins that then clump together
Plaques of beta-amyloid peptides form in brain
Neurofibrillary tangles inside neurons interfere with transport mechanisms eventually killing neurons
As brain cells die, functions are lost, and brain shrinks
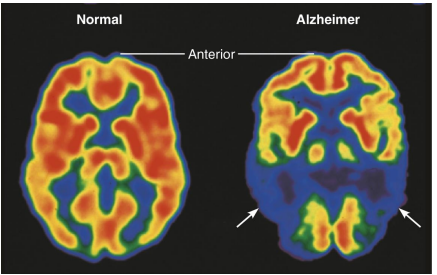
Treatment of alzheimer’s
Treatment includes
drugs to inhibit breakdown of acetylcholine
block toxic effects of excess glutamate that is released when neurons are damaged, or stimulate destruction of beta-amyloid
Parkinson’s disease
Degeneration of dopamine-releasing neurons of substantia nigra
Basal nuclei deprived of dopamine become overactive, resulting in tremors at rest
Cause unknown, but theories include mitochondrial abnormalities or protein degradation pathways
Treatment of Parkinson’s disease
Treatment includes L-dopa (dopamine precursor) to alleviate symptoms, deep brain stimulation with electrodes, and implanting stem cells
Huntington’s Disease
Fatal hereditary motor disorder
caused by accumulation of protein huntingtin in brain cells
Leads to degeneration of basal nuclei and cerebral cortex
Initial symptoms include wild, “flapping” movements called chorea
Later marked by mental deterioration
Usually fatal within 15 years of onset
Treated with drugs that block dopamine effects