Fundamentals of Human Physiology Exam 3 UIOWA
1/146
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
147 Terms
skeletal muscle
A muscle that is attached to the bones of the skeleton and provides the force that moves the bones
- Striated
- Voluntary
cardiac muscle
Muscle of the heart
- Striated
- Involuntary
smooth muscle
involuntary muscle found in internal organs
- Unstriated
- Involuntary
Sarcomere
contractile unit of a muscle fiber
Myosin
thick filament
Actin
thin filament
motor neurons
neurons that carry outgoing information from the brain and spinal cord to the muscles and glands
Motor unit
A motor neuron and all of the muscle fibers it innervates
neuromuscular junction
point of contact between a motor neuron and a skeletal muscle cell
in-series sarcomeres
sarcomeres that run on top of each other (longer fiber)
in-parallel sarcomeres
sarcomeres that run parallel to one another (thicker fiber)
- greater maximum contraction
Cross-bridge cycle
repeated sequential interactions between myosin and actin filaments at cross-bridges that cause a muscle fiber to contract
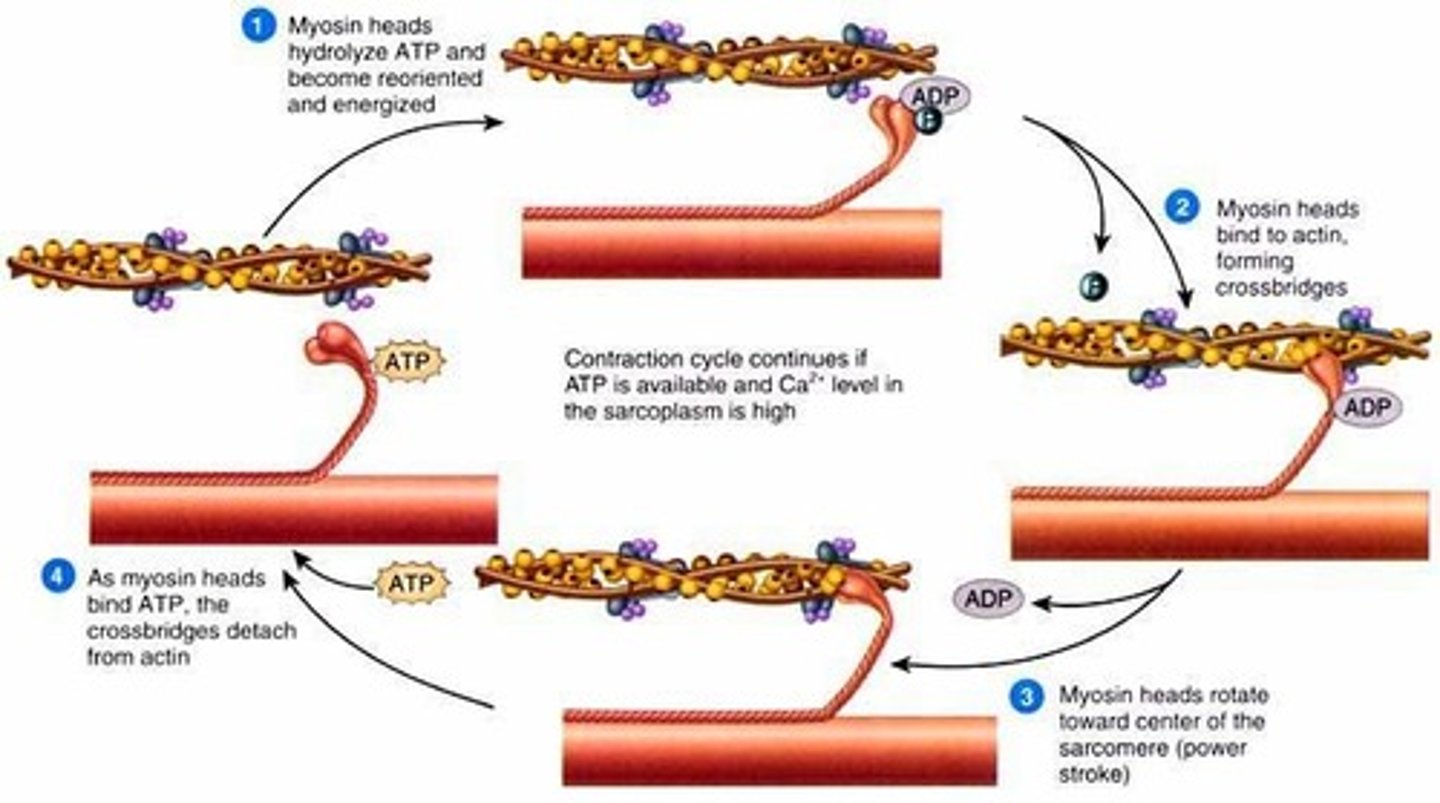
Ca+
What molecule controls the cross bridge cycle?
T-tubules (transverse tubules)
Action potential travels down ________________________
sarcoplasmic reticulum
Organelle of the muscle fiber that stores calcium
- Releases and removes Ca+ from the sarcomere
- Stimulated by action potential from T-tubule
Troponin, tropomyosin
Ca binds to ________________, which changes shape and prevents ________________________ from blocking binding sites on Actin
Contraction
turning on the cross-bridge cycle so that a muscle attempts to shorten
Tension
internal force generated within a contracting muscle
Load
external force against which the muscle acts
Isotonic contraction
constant load, but muscle changing lengths
- Concentric and eccentric
concentric contraction
muscle shortens against the load (tension > load)
Eccentric contraction
muscle attempts to shorten, but is forced to lengthen by the load (load > tension)
- muscle is generating tension while lengthening
isometric contraction
Muscle contracts but there is no movement, muscle stays the same length
- Tension = load
- Immoveable load
twitch contraction
the brief contraction of all the muscle fibers in a motor unit in response to a single action potential in its motor neuron
mechanical factors affecting muscle force
length, velocity, cross-sectional area
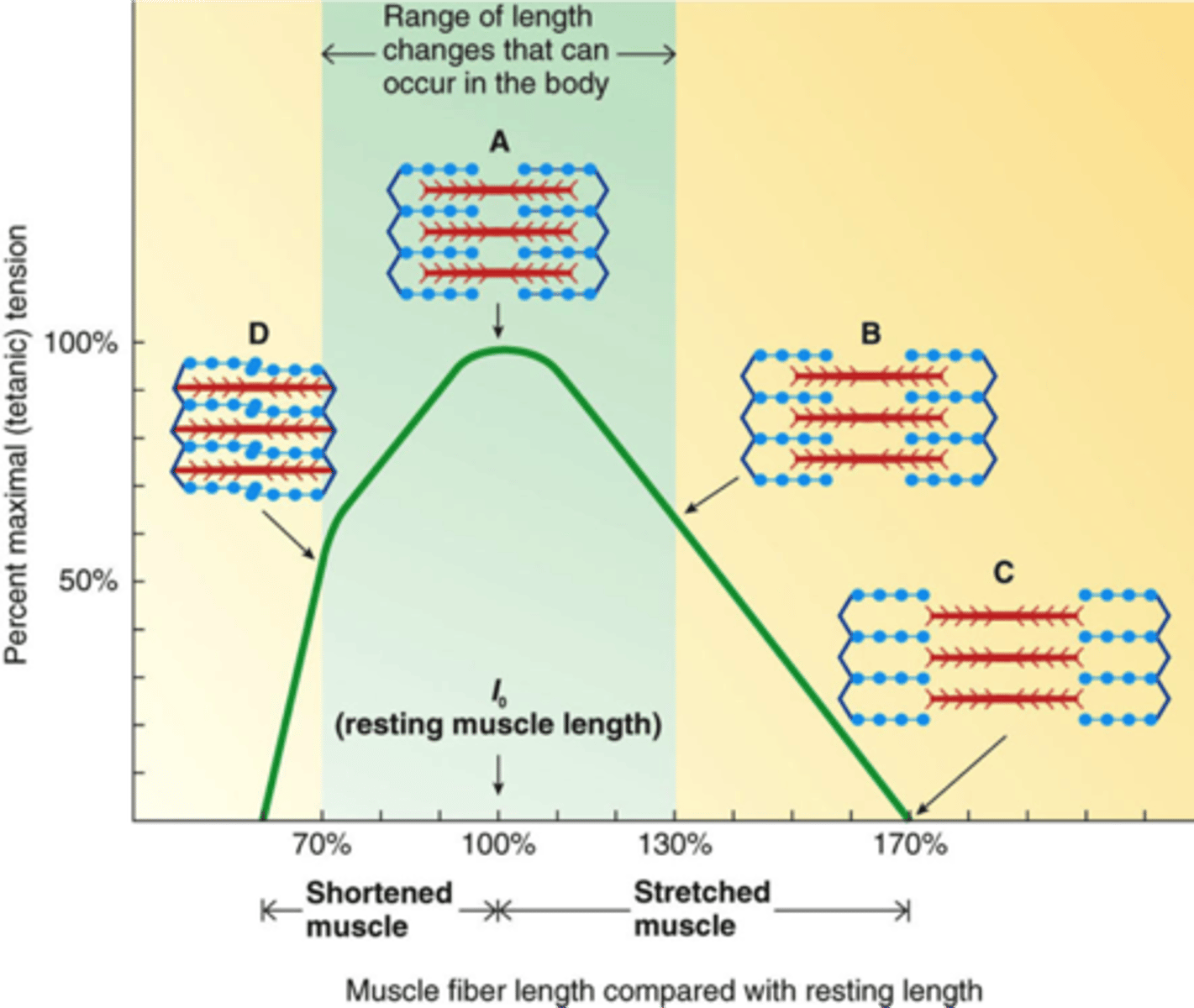
Muscle Length-Tension Relationship
maximal ability of a muscle to develop tension and exert force varies depending upon the length of the muscle during contraction
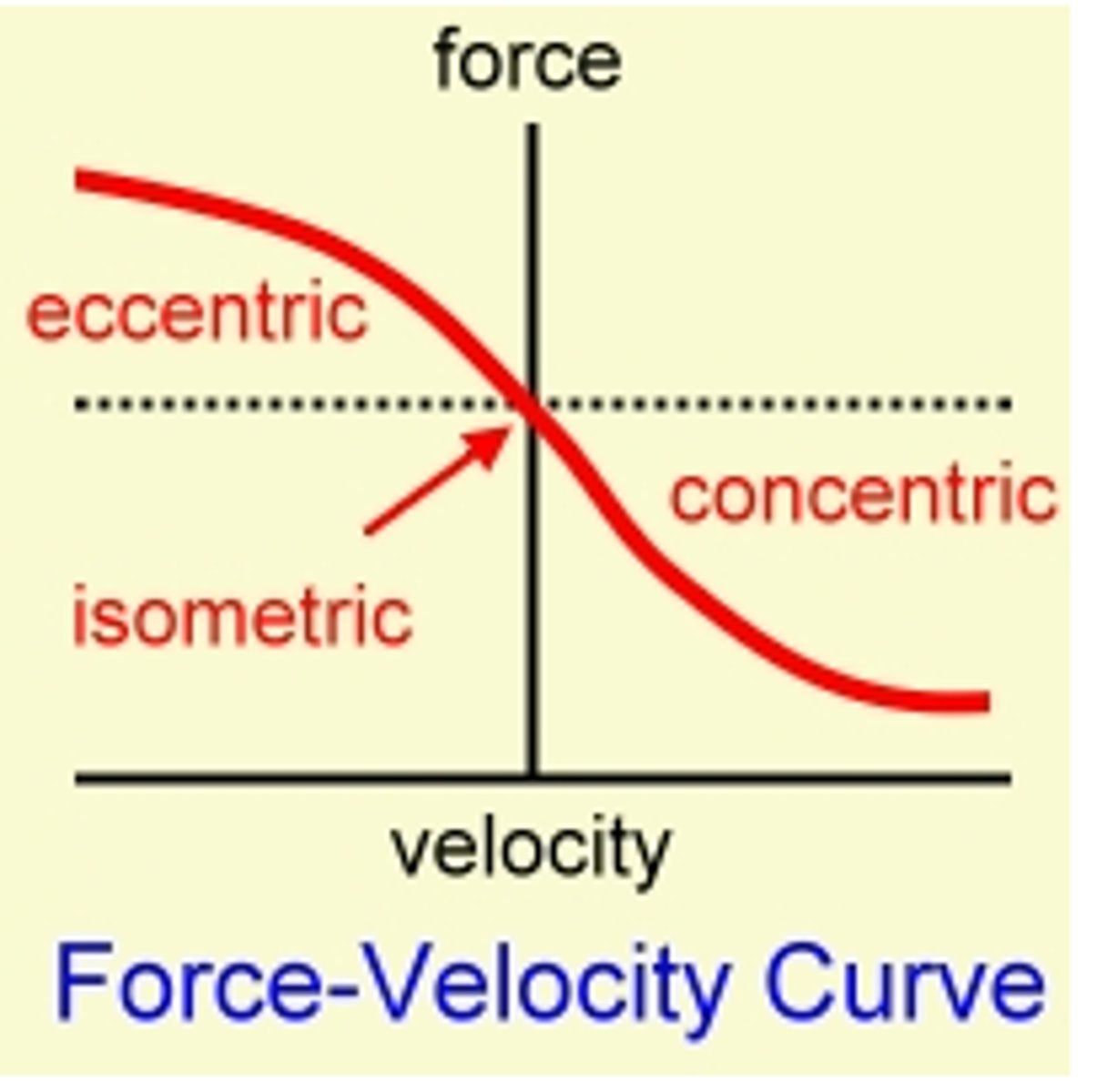
force-velocity relationship
force decreases as velocity increases
Type I fibers
Low force
Low velocity
Slow myosin ATP activity
High mitochondrial density
Type IIA Fibers (Fast Oxidative Fibers)
- Faster myosin ATPase activity
- Higher force production
- Higher velocity
- Less fatigue resistant than type I
- Intermediate mitochondrial density, myoglobin, capillary density
Type IIX fibers (fast-glycolytic)
- Fastest myosin ATPase
- Highest force production
- Fastest velocity
- Highest lactate production
- Low mitochondrial density, myoglobin, capillary density
- Highest glycogen storage
creatine phosphate system
The energy pathway that consists of adenosine triphosphate (ATP) and phosphocreatine (PC)
- provides immediate energy (between 10 and 15 seconds) through the breakdown of these stored high-energy phosphates
- All muscle fibers use
ATP
Maximum shortening velocity is determined by how fast a fiber can hydrolyze ______ to release myosin heads (myosin ATPase)
Motor unit
All muscle fibers in a single ____________ ________ are the same type
Slower
A muscle twitch is much _________________ than an action potential
Calcium
If another action potential arrives before complete relaxation, _________________ concentration increases
- Muscle continues to contraction
size principle of recruitment
motor units fire in order from small to large
principle of orderly recruitment
motor units are generally activated on the basis of a fixed order of fiber recruitment (slow twitch --> fast twitch)
Spinal cord
Motor neurons originate in the ______________ __________
Motor neuron pool
all the motor neurons that innervate a single muscle
Abundancy of neurotransmitters released to the motor neuron pool
- Faster (hence more) fibers recruited if excitatory signal increases
How does the nervous system decide if it should modify force via frequency or via # of motor units?
Cardiac differences similarities to skeletal muscle
- Smaller
- Un-nucleated
- Branched
Cardiac muscle fibers
Connected end-to-end via intercalated discs which contain gap junctions
- Gap junctions allow resistance free transfer of electrical current
- Optimize pumping
Myocardium
muscular, middle layer of the heart
- Atrial and ventricular are separate
Atrial
Excitation is initiated by pacemaker cells in the atrium, which excites the ______________ myocardium
ventricular
Excitation spreads from the atrial myocardium to the _________________ myocardium through conducting cells
Smooth muscle
- Found in walls of hollow organs and tubes
- Spindle-shaped cells with single nucleus
- Arranged in sheets
- Excitation-contraction coupling mechanism
myofilament arrangement of smooth muscle
No striations
- Filaments not arranged in sarcomeres or myofibrils
- Much longer thin filaments
- Dense bodies instead of z discs
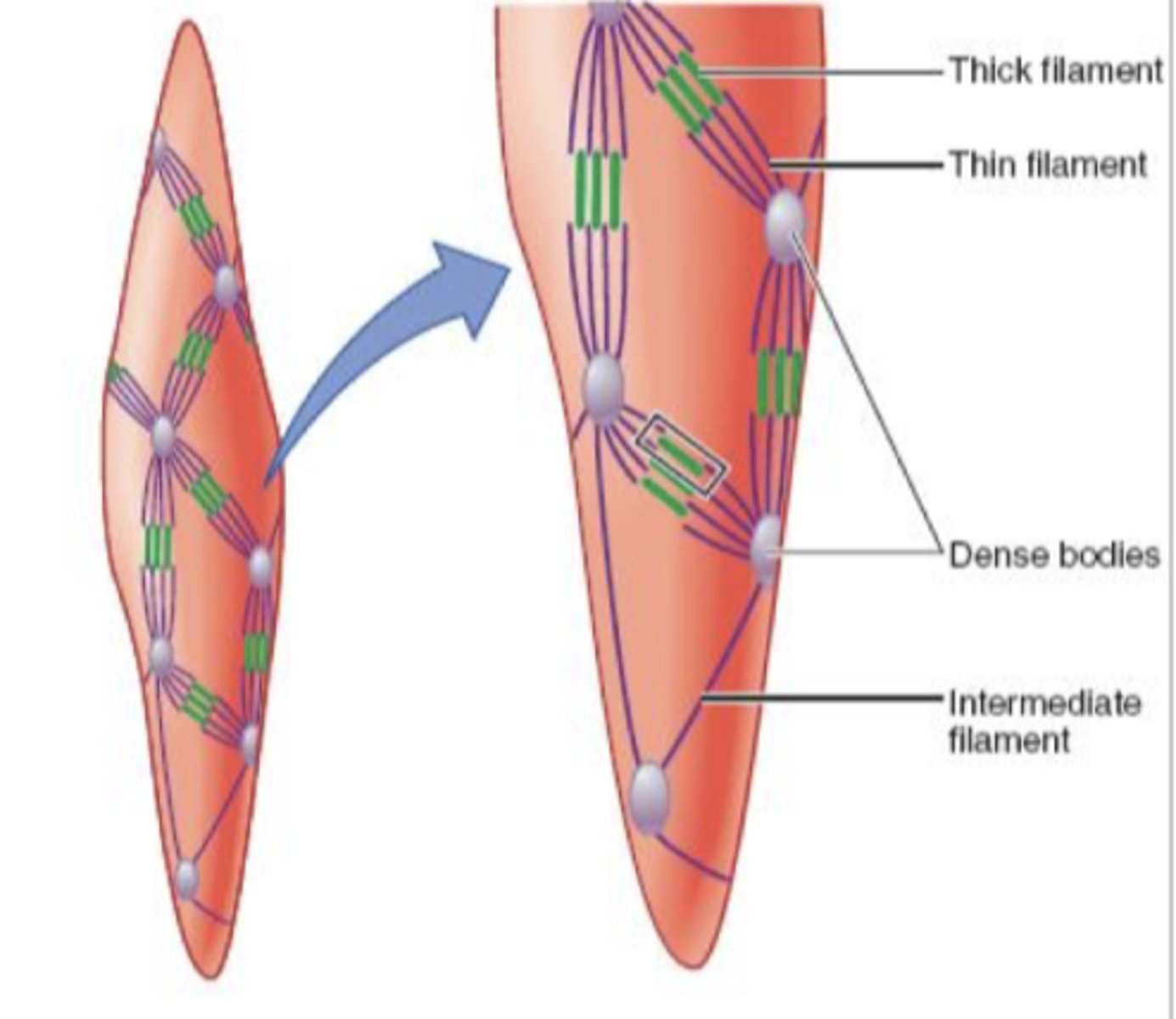
excitation inputs of smooth muscle
- ANS (SNS/PNS)
- Hormones
- Local chemical factors
- Stretch
- Pacemaker potentials
Voltage-gated channels OR Sarcoplasmic reticulum
Where does Ca+ come from in smooth muscle contraction?
excitation-contraction coupling (smooth muscle contraction)
1. Ca+ binds to calmodulin
2. Activates myosin light chain kinase
3. MLCK phosphorylates myosin heads and allows them to form cross bridges and muscle contracts
4. Myosin light chain phosphate dephosphorylates myosin heads and inactivates the cross bridges and muscle relaxes
1 gallon/5L on average
Average blood volume?
55, 45
Blood is composed of ____% plasma, ____% hematocrit (everything else)
Erythrocytes
red blood cells
- carry oxygen
Leukocytes
white blood cells
- immune system
Platelets
protein cell fragments
- participate in blood clotting
Plasma
90% water
- Stuff dissolved in water: electrolytes, nutrients, gasses, plasma proteins
RBC structure
- No nucleus/organelles
- Structure: biconcave discs, flexible membrane
Helps blood flow, maximizes surface area
Why do red blood cells biconcaved?
fit through capillaries
Why do RBC's have flexible membranes?
Hemoglobin
Oxygen carrying pigment in red blood cells
- also binds CO2 and H+
Erythropoesis
production of red blood cells
Bone marrow
Where are red blood cells produced?
hematopoietic stem cells
form blood cells
Erythropoetin
Hormone produced by kidneys which stimulates red bone marrow to increase production of red blood cells
Spleen
______________ removes most of old erythrocytes
Anemia
Below normal number of hemoglobin
- Diagnosed by blood tests
Causes:
- Nutrient deficiencies (Iron, folate, B12)
- Blood loss
- Bone marrow failure
- Hemolytic anemia
Megakarocyte
Platelets come from _________________________ cells
Hemostasis
stoppage of bleeding from a broken blood vessel
3 processes:
1. Vascular spasm
2. Formation of a platelet plug
3. Blood coagulation (clotting)
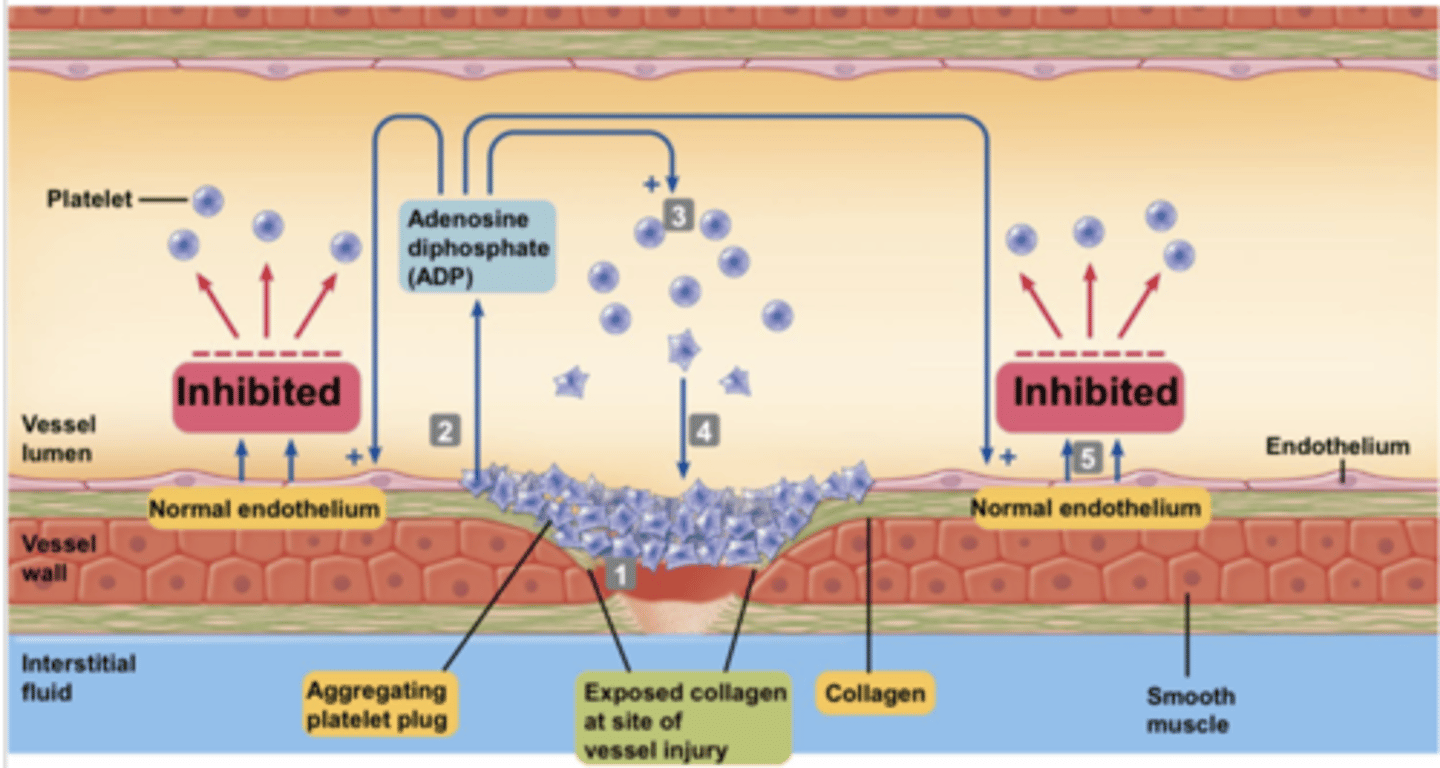
Vascular spasm
constriction of blood vessels to reduce blood flow through a damaged vessel
formation of platelet plug
- platelets aggregate on contact with exposed collagen in damaged wall of the vessel
- platelets release substances (ADP) which causes surface of nearby circulating platelets to become sticky
An undamaged endothelium constantly releases factors that prevent it
Why don't platelets aggregate on a normal endothelium?
blood coagulation (clotting)
transformation of blood from liquid into a solid gel (coagulation proteins)
- reinforces the platelet plug
Leukocytes function
- Defends against invading pathogens
- Identifies and destroys cancer cells
- Removes worn-out cells and debris
Pulmonary circuit
carries blood to the lungs for gas exchange and returns it to the heart
- Oxygenates blood
systemic circuit
transports blood between heart and rest of body
Atria
two upper chambers of the heart
Ventricles
the two lower chambers of the heart
atrioventricular valves
between atria and ventricles
- controls blood entering the heart
semilunar valves
controls blood flow out of the heart
- pulmonary and aortic
prevents blood from flowing in the wrong direction
- only open one way
Purpose of valves in the heart?
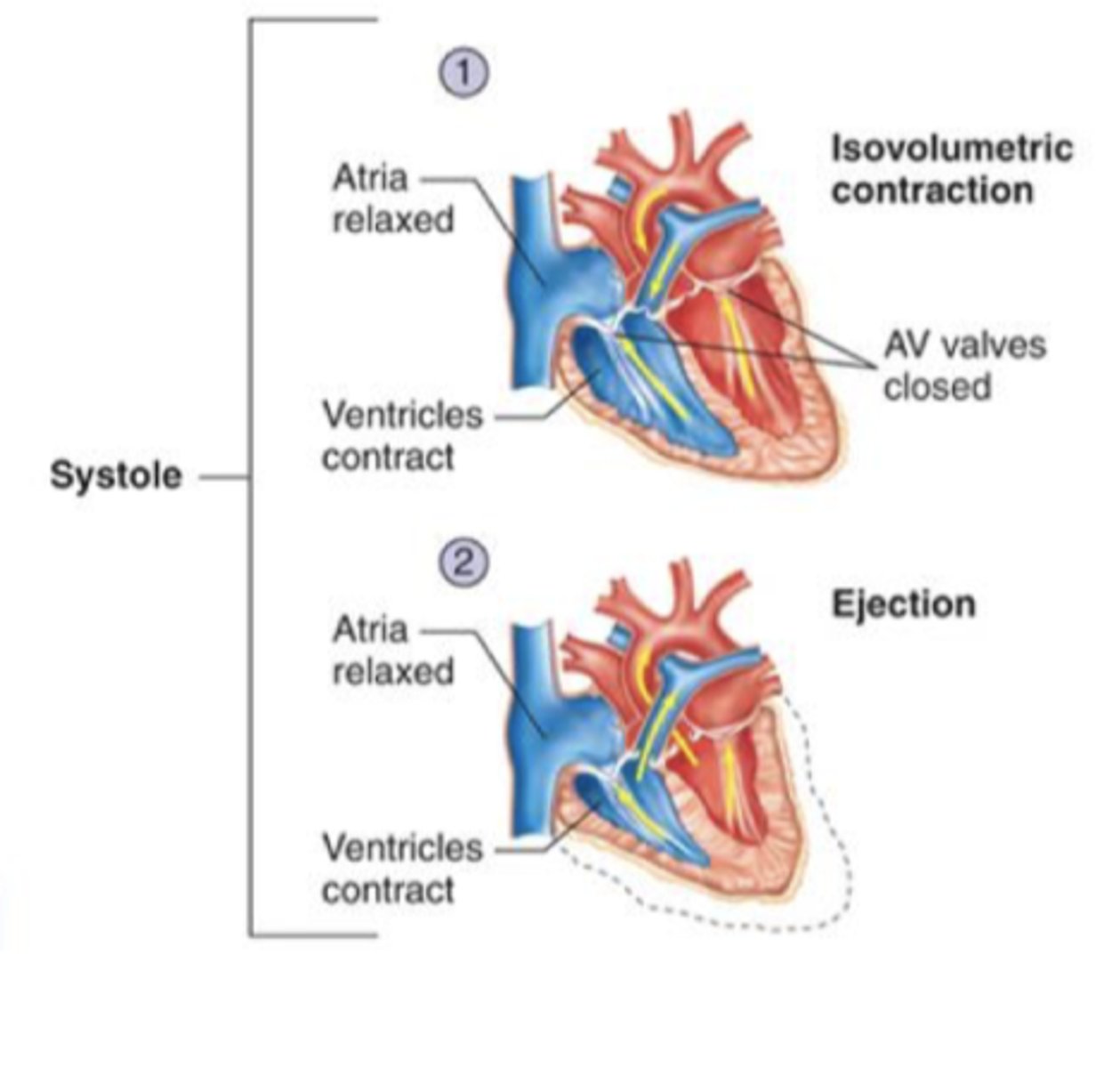
Systole
Contraction of the heart
- ejection of blood
Events:
1. Isovolumetric contraction
2. Ejection
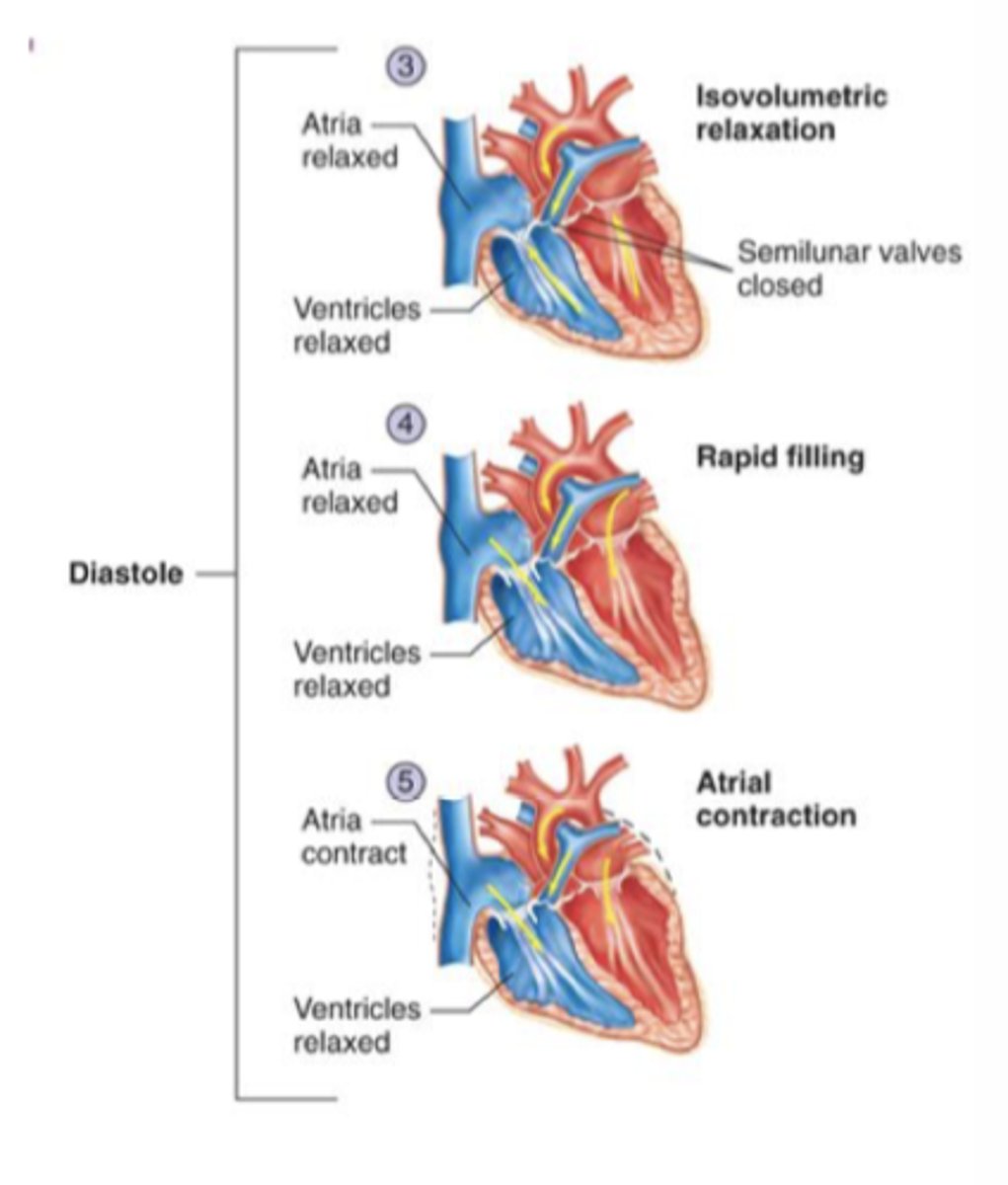
Diastole
Relaxation of the heart
- filling of blood
Events:
1. Isovolumetric relaxation
2. Rapid filling
3. Atrial contraction
isovolumetric contraction (systole)
- start of systole
- Ventricular pressure rises above atrial pressure resulting in closing of AV valves
- ventricles contract but no blood ejected
- both valves closed
Ejection (systole)
ventricular pressure exceeds arterial pressure resulting in semilunar valves to open
isovolumetric relaxation (diastole)
pressure in ventricles drops below arterial pressure resulting in closing of semilunar valves
- atria begin to fill
Rapid filling (diastole)
pressure in ventricles falls below atrial pressure opening the AV valves
- Begins filling of the ventricles
autorhythmicity
heart's ability to control its own contractions
autorhythmic cells
initiate action potentials and spread impulse throughout heart
- do not contract
contractile cells
produce contractions that propel blood
- 99% of myocardial cells
SA node
pacemaker of the heart
AV node
relays electrical impulses from atria into ventricles
- conduction delay because don't want atrium and ventricle to contract at same time
Bundle of His
transmits the cardiac impulse from the AV node to the ventricles causing them to contract
Purkinje fibers
fibers in the ventricles that transmit impulses to the right and left ventricles, causing them to contract
ECG
potential difference at the body surface due to electrical activity of heart
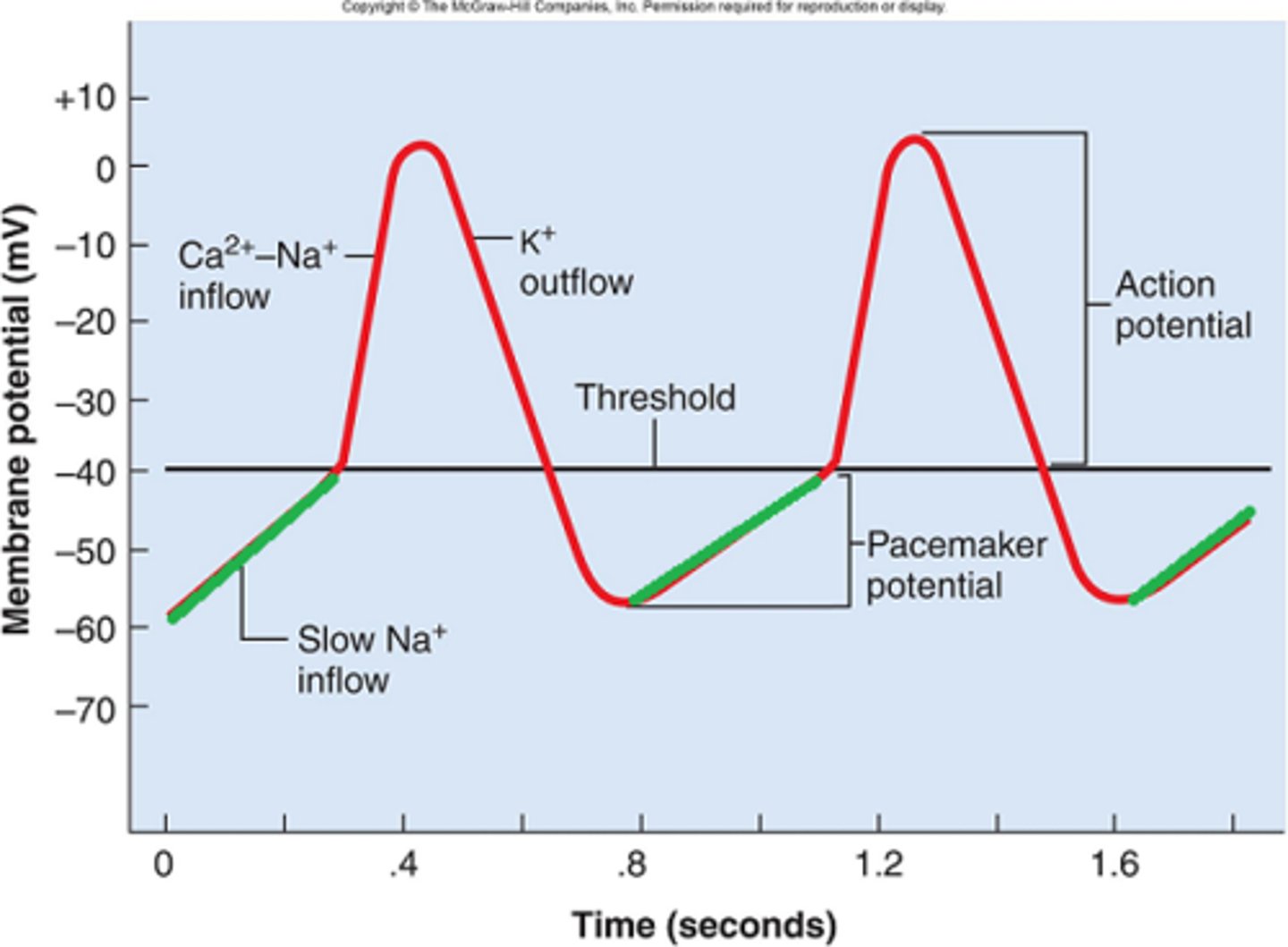
Mechanism of Autorhymicity
potential changes due to changes in permeability to various ions (K+, Na+, Ca)
- unique voltage gated channel (F type) causes pacemaker potential
- Once threshold is reached, AP due to Ca+
Hemodynamics
the science of the blood flow through the vasculature
Viscosity
A liquid's resistance to flowing
Arteries
carry blood away from the heart
Arterioles
small vessels that receive blood from the arteries
Capillaries
Microscopic vessel through which exchanges take place between the blood and cells of the body