25- Heart catheterization. Hemodynamic evaluation. The heart cycle.
1/21
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
22 Terms
what is heart catheterisation
passage of a catheter through peripheral arteries and veins into cardiac chambers and coronary arteries
describe the catheterisation procedure
wire inserted into L or R side of heart
dye is injected → angiogram visualised via x ray imaging
number of stenosed vessels indicates what to do next
pharmacological treatment is the same after
describe left heart catheterisation
enter via femoral, radial, brachial artery → aorta/ coronaries, LV and mitral valve
useful in- coronary a., aortic BP measurement, LV pressure/ function
describe right heart catheterisation
enter via femoral, subclavian, antecubital vein → RA, tricuspid valve, pulmonary valve and artery
used in- RA/RV pulmonary artery pressures, pulmonary a. occlusion vascular resistance measurements
what does the number of stenosis indicate
>3 → CABG
1-2 → PCI angioplasty
what are the risks with PCI angioplasty
risk of stent stenosis
drug eluting stents prevent this
can have increased risk of thrombosis
what is the pharmacoological treatment
BB
ACEi
dual anti platelet therapy- aspirin + clopidogrel
high potency statins
what are the general uses for cardiac catheterisation
pressure measurements → fluid column pressure differences, gradients
flow measurements → coronary flow reserve
angiocardiography → heart chambers
coronarography → coronary arteries
PCI
biopsy
intravascular US imaging → estimation of arterial narrowing
pericardiocentesis → fluid aspiration
wha tare the indications for catheterisation
CAD investigation → detect stenosis and location of CAD
valvuloplasty
congenital HF diagnosis/ treatment
abnormal stress test
recurrent chest pain
what techniques are used
Seldinger in combination with
fluoroscopy/ digital or X ray recording → real time images
contrast dye injection- heart anatomy + vessel imaging
perform angioplasty- stenting + ballooning
valvuloplasty
cariac biopsies
what are the risks/ complications
haemorrhage/ false aneurysm → cardiac tamponade
hypersensititivty reaction to contrast material
arrhythmias, thrombosis, stroke, AMI, angina, infection
what are the relative contraindications
renal insufficiency
coagulopathy
fever/ systemic infection
uncontrolled arrhythmia
decompensated HF
radiopaque dye allergies
what is haemodynamic evaluation
blood flow and cardiac performance by measuring blood flow at different points in circulation
feel pulse → simple information about strength of circulation
how is the BP measured for evaluation
plethysmograph or cuff connected to a pressure sensor
most common clinical measure of circulation and provides peak systolic + diastolic pressure
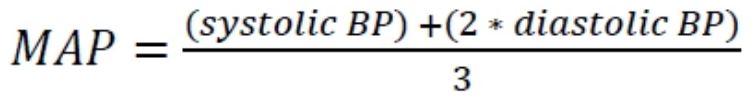
what is Doppler flow measurements
measure flow at any point in circulation including within heart
pressure gradients
pathologic flow
what is arterial pulse pressures
placing tonometer or pressure sensor on skin surface above artery → continuous pressure trace or pulse pressure waveform
reflects CV perormance
invasive → measure intraarterial PP through catheter in artery
what is CO/ SV
distinguish function of heart and vessels
allows more understanding and treatment of CV system
important regarding CO and SV is EF
EF <40%- HF
what are the phases of the heart cycle
atrial depolarisation/ contraction- diastole
isovolumetric contraction- systole
ejection systole → diastole
isovolumetric relaxation diastole
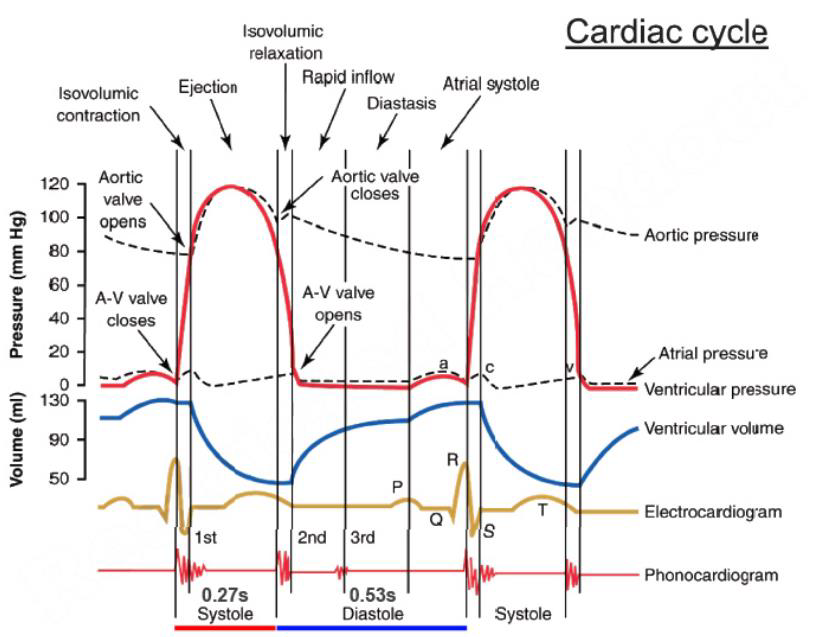
describe phase 1 of the heart cycle
SA node → depolarises atria⇒ P wave
atrial contraction → atrial P increases → ventricular filling → increased VV
atrial + ventricular pressure increases until atrial contraction is over → a P decreases
Small decrease in aortic pressure= less blood remained to flow away from aorta
describe phase 2 of the heart cycle
ventricular presure > atrial pressure = AV valve close ⇒1st heart sound
beginning of systole
ventricular depolarisation/ contraction → increased ventricular pressure
AV and semilunar valves are closed= isovolumetric contraction
describe phase 3 of the heart cycle
ventricular pressure increases → exceeds aortic pressure → semilunar valves open
blood from ventricle to aorta
V and aortic pressure decreases when ventricular repolarisation occurs
end of ejection phase when aortic pressure is > ventricular → semilunar valves close⇒ 2nd heart sound
describe phase 4 of the heart cycle
ventricular pressure decreases with no change in volume= isovolumetric relaxation
ventricular pressure a bit> atrial
atrial contraction increases slowly= increases
atrial preaaure> ventricular → AV valves open → ventricular filling
dicrotic notch= closure of semilunar valve → aortic pressure decreases slowl