CH15 - Antimicrobial Drugs
1/68
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
69 Terms
Antimicrobial drugs
Can be classified as antibacterial, antifungal, and antiviral agents.
antibiotic
substance produced by one microbe that can inhibit the growth or viability of another microbe.
antibiotics, synthetic
Antimicrobial drugs consist of ___ and ____ compounds
Penicillin
the first antibiotics widely used in clinic. It is produced by the fungus Penicillium and inhibits the growth of staphylococci
staphylococi
Penicillin is the first antibiotics widely used in clinic.
It is produced by the fungus Penicillium and inhibits the growth of ____
Arsphenamine, sulfonamides
_____ , and _____ are among the earliest examples of synthetic compounds for the treatment of infectious diseases.
Paul Ehrlich
____ was the discoverer of both arsphenamine and the receptor concept
syphilis
Arsphenamine: the first modern antibacterial drug
An organic arsenic compound that was dubbed “salvarsan” and clinically used to treat ____ for several decades
Sulfonamides
the first effective drugs for the treatment of systemic bacterial infection
Gerhard Domagk
_____ Discovered Prontosil
viruses, bacteria, fungi, parasites,, protozoa, metazoa
Diversity of infectious pathogens
Viruses
Bacteria
Fungi
Parasites – eukaryotes other than fungi
____ – unicellular
___ – multicellular
inactive, sulfanilamide, dihydropteroate , folate, stops
How does Prontosil work?
• Prontosil itself is ___ in vitro ( lab setting)
• In the body, it is metabolized into ____ (active form)
• This active form
○ Inhibits ____ synthase
○ Blocks ___synthesis in bacteria
→ prevents DNA synthesis → ___ bacterial growth
gram, prior, immunostaining, PCR, isothermal, unique
Identifying the infecting organism
___ staining: a rapid assessment
Cultivation of a sample taken ___ to initiating treatment for conclusive diagnosis & antibiotics susceptibility analysis
Detection of unique microbial antigens using immunostaining
Detection of unique microbial RNA or DNA using ___ or ___ nucleic acid amplification
Detection of the ___ patterns of host immune response
-cidal, -ostatic
Types of antimicrobial agents: ___ vs ____
beta lactams, penicillin, chloramphenicol
Types of antimicrobial agents: -cidal vs -ostatic
Bactericidal: killing outright (e.g., ___ , ___ )
Bacteriostatic: stalling proliferation (e.g., ___ )
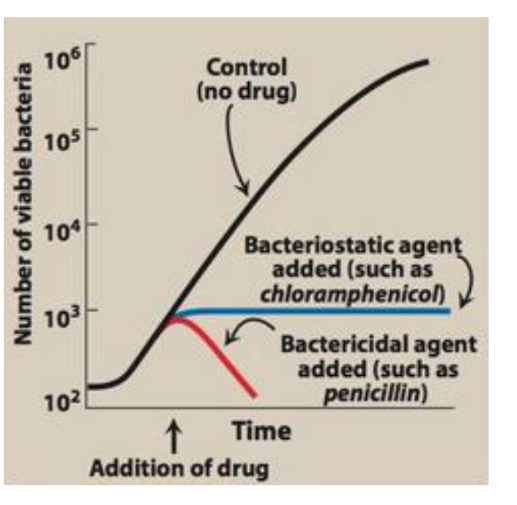
bactericidal
drugs able to effectively kill more than 99.9% bacteria within 18 to 24 hours of incubation
bacteriostatic
drugs that only arrest the growth and replication of bacteria at drug levels achievable in the patient.
MIC
minimum inhibitory concentration
MIC
lowest antimicrobial concentration that PREVENTS the visible growth of an organism after 24 h of incubation
susceptibility, sensitivity, resistance
Based on MIC, a pathogen can be classified as:
Having ___ to the agent
Having intermediate ___ to the agent
Having ___ to the agent
4,10
The peak serum concentration of a drug should be ___ to __ times greater than the MIC in order for a pathogen to be susceptible
MBC
minimum bactericidal concentration
MBC
the lowest concentration of antimicrobial agent that results in a 99.9% decline in colony count after overnight broth dilution incubations.
varying, 24, inhibits
MIC Determination
Tubes containing ___ concentration of antibiotic are inoculated with test organism
Growth of microorganism is measured after __ hours of incubation
MIC is the lowest concentration of antibiotic that ___ bacterial growth
varying, subculture, 24, kills
MBC Determination
Tubes containing ___ concentration of antibiotic are inoculated with test organism
After 24 hours of incubation in the presence of antibiotic, ___in antibiotic-free medium, and measure growth after __ hours of incubation
MBC is the lowest concentration of antibiotic that ___ 99.9% of bacteria (equals 32 in this example)
4,64
Concentration-dependent killing
Certain antimicrobial agents show a significant increase in the rate of bacterial killing as the concentration of antibiotic increase from ___ to ___fold the MIC of the drug for the infecting organism
above
Time-dependent killing
clinical efficacy of agents can also be predicted by the % of time that blood concentrations of a drug remain ___ the MIC
Extended (generally 3 to 4 hours) or continuous (24 hours) infusions can be utilized instead of intermittent dosing to achieve prolonged time above the MIC and kill more pathogen
below, 1
Post-antibiotic effect (PAE)
This is a persistent suppression of microbial growth that occurs after levels of antibiotic have fallen below the MIC.
Agents exhibiting a LONG PAE often require only ___ dose per day
narrow, broad, extended
Based on their range of antimicrobial activity, antimicrobial drugs can be characterized as ___ spectrum, ____ spectrum, or ___ spectrum.
Narrow
____ spectrum: active against a single species or a limited group of pathogens (e.g., Gram-positive bacteria).
gram positive
Narrow spectrum: active against a single species or a limited group of pathogens (e.g., _____bacteria).
specific, without
Narrow-spectrum drugs are sometimes preferred because they target a ____ pathogen ___ disturbing the normal flora of the gut or respiratory tract.
Broad
____ spectrum: active against a wide range of pathogens
initial, not
Broad-spectrum drugs are sometimes preferred for the ___ treatment of an infection when the causative pathogen is ___ yet identified
Extended
____ spectrum: intermediate range of activities.
host, resistance
Challenges of antimicrobial drug discovery (2)
The drugs must kill the microbes but ___ the host (the principle of selective toxicity)
Microbes tend to develop ___ to drugs that are initially effective
mutation, plasmid, already
Microbes tend to develop ___ to drugs that are initially effective
From ___ and selection
From the transfer of ___ that confer drug resistance
For antibiotics: resistance genes ___ exist in the producers of antibiotics, which can spread to pathogenic bacteria by gene transfer
penicillin, sulfonamides
Drug targets for antimicrobial therapy - Macromolecules that occur in the cells of the pathogen but not within the human host.
The bacterial cell wall ( ___ )
de novo synthesis of folic acid ( ___ )
chloramphenicol, trimethoprim, ciprofloxacin
Drug targets for antimicrobial therapy - Macromolecules that occur in both humans and the pathogen but are structurally divergent.
Ribosomes ( ___ )
Dihydrofolate reductase ( ___ )
DNA topoisomerase ( ___ )
Formylmethionine deformylase
Drug targets for antimicrobial therapy -Essential pathogen genes revealed by genome
sequencing and genetic studies
____ ____
Dihydrofolate reductase:
an example of a drug target with sufficient structural difference between the host and the pathogen
wall, membrane, DNA/RNA, protein, metabolism
Drug targets for antimicrobial therapy
Cell ___ synthesis
Cell ___ function
___ synthesis
___ synthesis
Intermediate ___
acetylase, Beta-lactamase
Mechanisms of anti-microbial resistance - Inactivation of the drug by microbial enzymes
inactivation of aminoglycosides by ____;
inactivation of Beta-lactam antibiotics by ____
porin, ABC,
Mechanisms of anti-microbial resistance - Decreased accumulation of the drug by the microbe
via DEC uptake (e.g., ___ mutation)
via INC efflux ( ___ transporter P-glycoprotein)
sulfonamides, beta lactam
Mechanisms of anti-microbial resistance - Reduced affinity of the target molecule for the drug
e.g., reduced affinity of folate synthesis enzymes for ___ ;
e.g., reduced affinity of penicillin-binding proteins for ____ antibiotics
resistance, germs
Antibiotics fight germs (bacteria and fungi). But germs fight back and find new ways to survive.
Their defense strategies are called resistance mechanisms.
Only ___, not people, become resistant to antibiotics.
DNA gyrase
Alteration in the target enzyme ____ ____ resulted in resistance to fluoroquinolones
b lactamases
Enterobacter is resistant to cephalosporins by producing _____
antibiotics, transfer
Resistance genes exist in producers of ___
can spread to pathogenic bacteria by gene ___
bacteria, plasmids, transposons
Drug resistance in bacterial populations can be spread:
from person to person by ___
from bacterium to bacterium by ___
from plasmid to plasmid (or chromosome) by ___.
conjugative
The main method of transfer of resistance genes from one bacterium to another is by ___ plasmids.
The bacterium forms a connecting tube ( sex pilus) with other bacterium through which the plasmids pass.
transduction
A less common method of transfer is by ___
The transmission by a bacterial virus (phage) bearing a resistance gene into another bacterium
lipoteichoic, thick, no
Gram Positive Cell Wall
____ acids
___ peptidoglycan layer
outer membrane?
LPS, porin, MDR
Gram Negative Cell Wall
Contains ___, ___, and a ____ system
outer membrane?
mycolic, porin, yes
Mycobacteria Cell Wall
contains ___ acid and a ___
outer membrane?
isoniazid
INH is short for ___
KatG, Mycolic
Isoniazid (INH) Mechanism
INH is activated by a mycobacterial enzyme called ___
Once activated, it inhibits enzymes involved in synthesizing ___ acids ( essential components of the waxy cell wall of mycobacteria)
Weakens the cell wall → bacteria die
PEP, Fosfomycin, alanine racemase, D-alanine ligase, seromycin, removed, glycine, Lipid II, Bacitracin, Transpeptidase, penicillin G , Vancomycin
bacterial peptidoglycan synthesis pathway
NAG ( hexomeric glucose) is bound to UDP ; ___ adds a Lactose group to it
____ can inhibit this step ( used to treat UTI infections) This is cuz it’s similar to PEP structure wise
3 L-amino and 2 D-ala groups are added to it
2 L-Ala - ( alanine racemase) -> 2 D-La - (D-alanine ligase)-> D-Ala-D-Ala
____ acts as a competitive inhibitor for this rxn
UDP group is ____ and the remnants bind to Undecaprenol phosphate
Another NAG-U group is added
5 ___ molecules are added
The structure becomes ____ '
Lipid II ___ and goes to the outside of the cell
___ can inhibit this step
Leaves the undecaprenol group, and more sugars are bound together to form the peptidoglycan
___ allows the glycine of one molecule to combine with the amino acids of another molecule
___ is a suicide inhibitor of transpeptidase, making it irreversibly inhibited
negative, amide, COOH
Ampicillin and ticarcillin can pass the membrane of gram ___ bacteria
○ Ampicillin has an ___ group
○ Ticarcillin has a ___ group, which both inc the polarity ( hydrophillic) and pass the porin
methicillin
____ has INC resistance to B-lactamase
imipenem
_____ is susceptible to metallo-B-lactamase
clavulanic acid
____ inhibits b-lactamase
Vancomycin
_____ sequesters the substrate of the transpeptidase reaction
positive
Vancomycin is active against Gram ___ bacteria
positive, holes, depolarization
Daptomycin
cyclic lipopeptide antibiotic for treating infections caused by resistant gram ___ organisms.
It inserts into the cell membrane, aggregates, and creates ___ that leak ions.
This causes rapid ___ , resulting in a loss of membrane potential.
Daptomycin
A cyclic lipopeptide antibiotic for treating infections caused by resistant gram-positive organisms.
concentration
Daptomycin is a ( time / concentration) dependent bacteria
Polymyxin B:
an antibiotics that disrupts outer membrane via binding LPS
negative
Polymyxin B can be used in combination with B-lactam antibiotics to effectively kill Gram ___ bacteria