Animal Transport
1/49
Earn XP
Description and Tags
Eduqas biology
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
50 Terms
Why dont single-celled organisms need a transport system?
-SA:V is high
-short distrances to travel
-low metabolic needsWhat
What is insect circulatory system?
open, with a dorsal, tube shaped heart and a fluid filled cavity
How does circulation in insects happen
Blood is pumped at low pressure into the haemocoel where it bathes the tissue directly for exchange of materials
Blood slowly returns to the heart and then is pushed forward tp the head where open circulation starts again
circulation system in earthworms
organs are not in direct contact with the blood but are bathed by tissue fluid. Respiratory gases are transported in the blood, aided by a pigment. has dorsal and ventral vessels running the length of the body, running the length of the body, connected by the 5 pseudohearts which pump the blood
single system
where blood passes through then heart once
double system
where blood passes throigh the heart twice and there re seperated systemic body and pulmonary systems
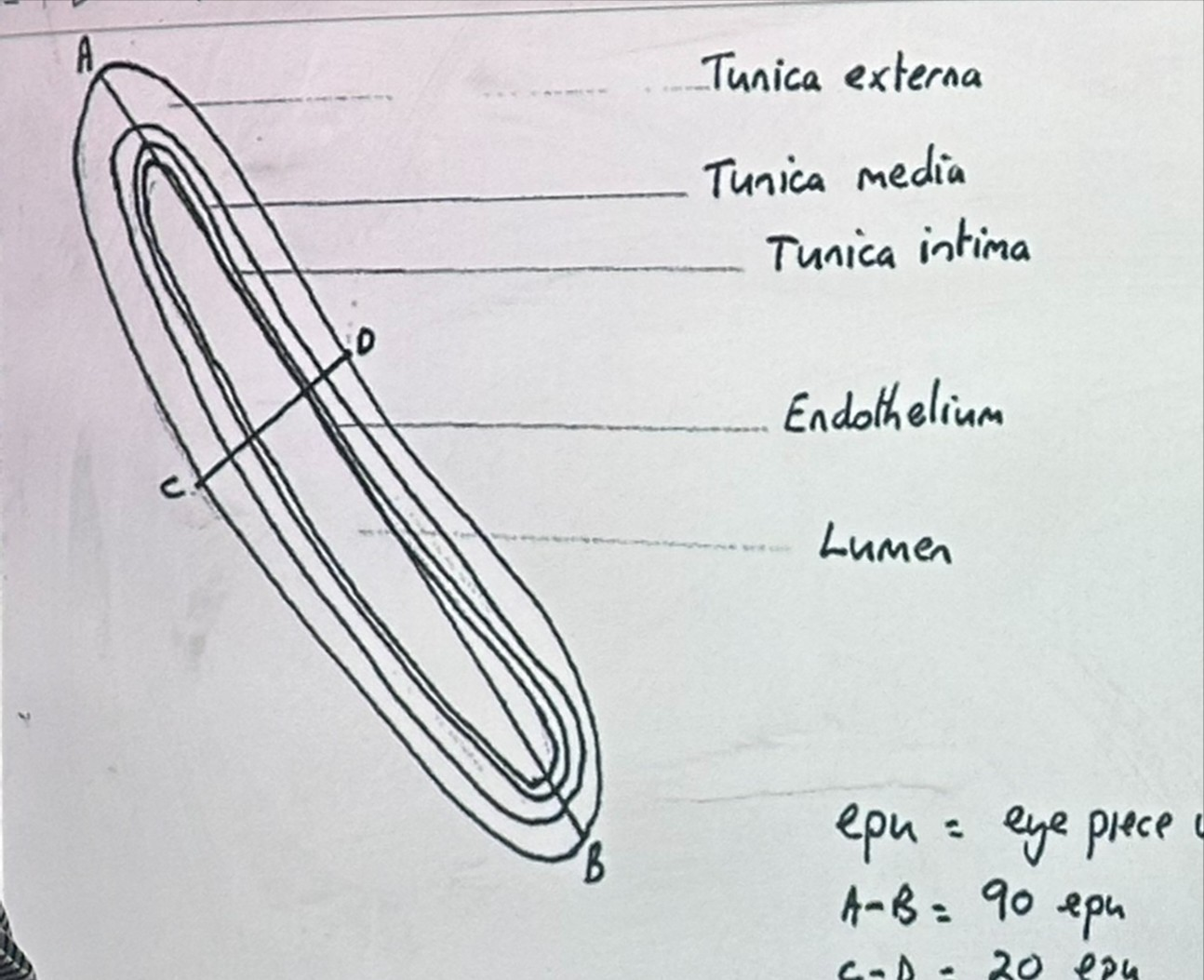
Three layers in blood vessels
-tough collagen
-elastic muscular layer to sustain pressure
-endothelium which is smooth to reduce friction
Arteries
thick walls to resist high pressure. They are able to adjust diameter to adjust blood supply and blood pressure
label artery and vein
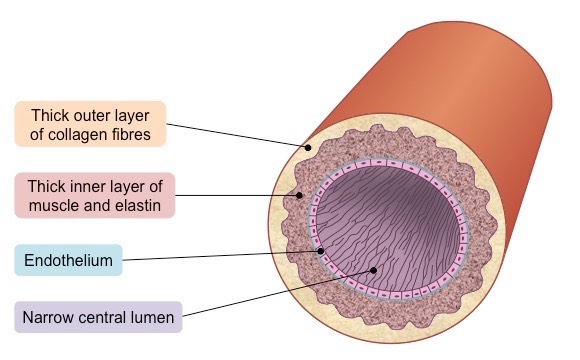
veins
thinner muscle layer than arteries
-larger diameter than arteries
-reduced pressure compared to arteries
valves to flow in one direction only
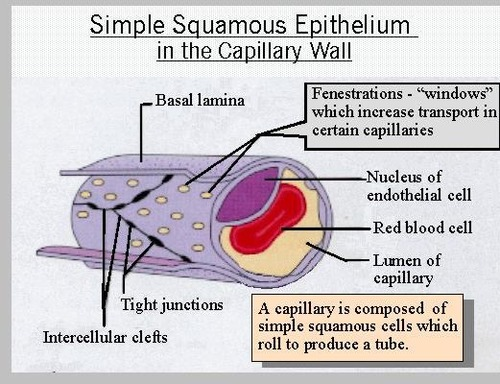
capillaries
-walls are one layer thick and permeable
-small diameter
friction in walls slow down blood flow
-many capillaries in a bed for a large total crosssectional area, which further reduces blood flow
-low velocity to enhance ability to exchnage materials with surrounding tissue
-gaps that allow exchange of material
capillary
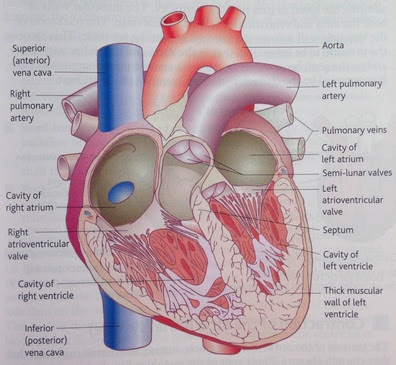
heart

cardiac muscle
intercolated discs, branched, faintly striated. MYOGENIC
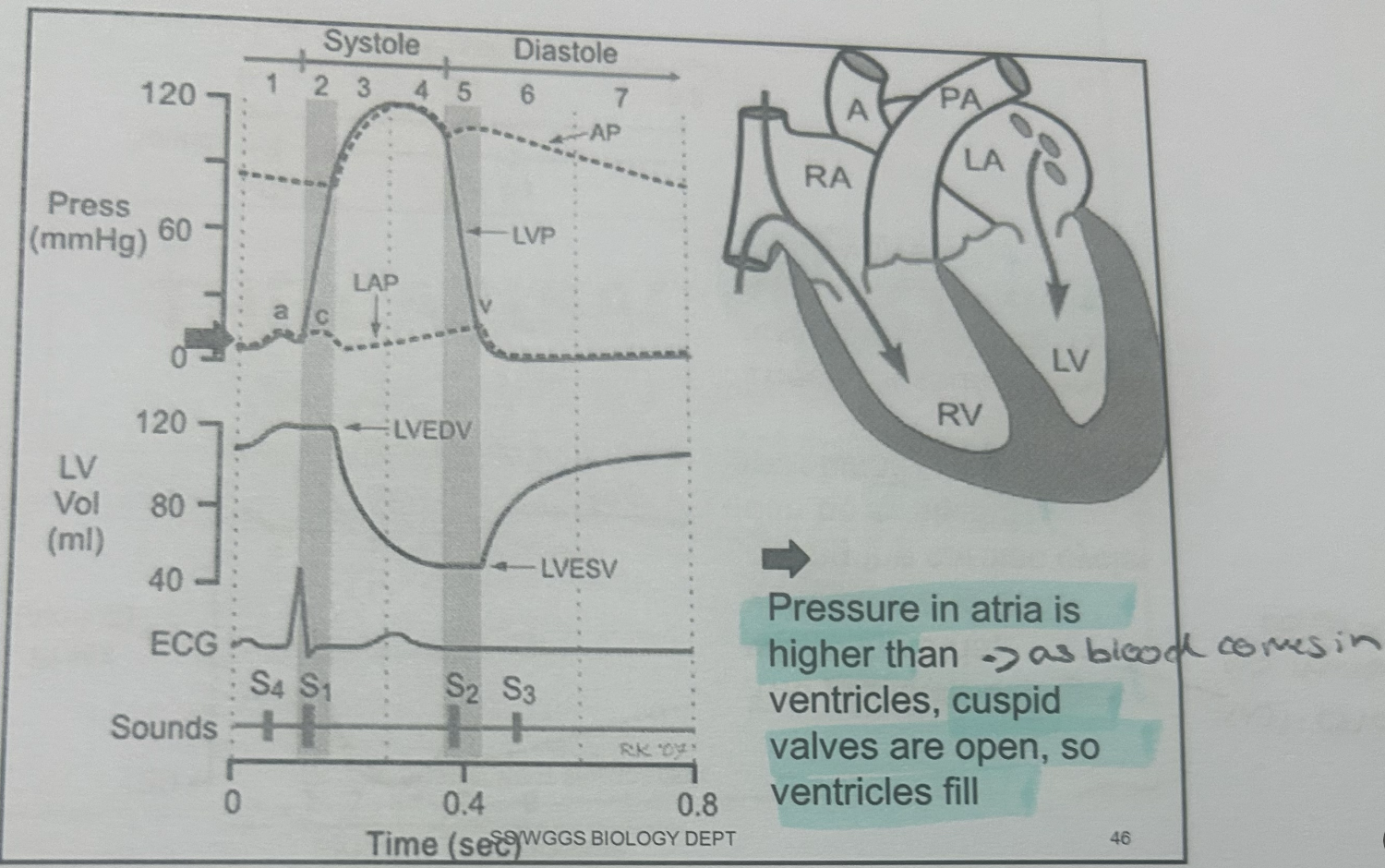
the cardiac cycle
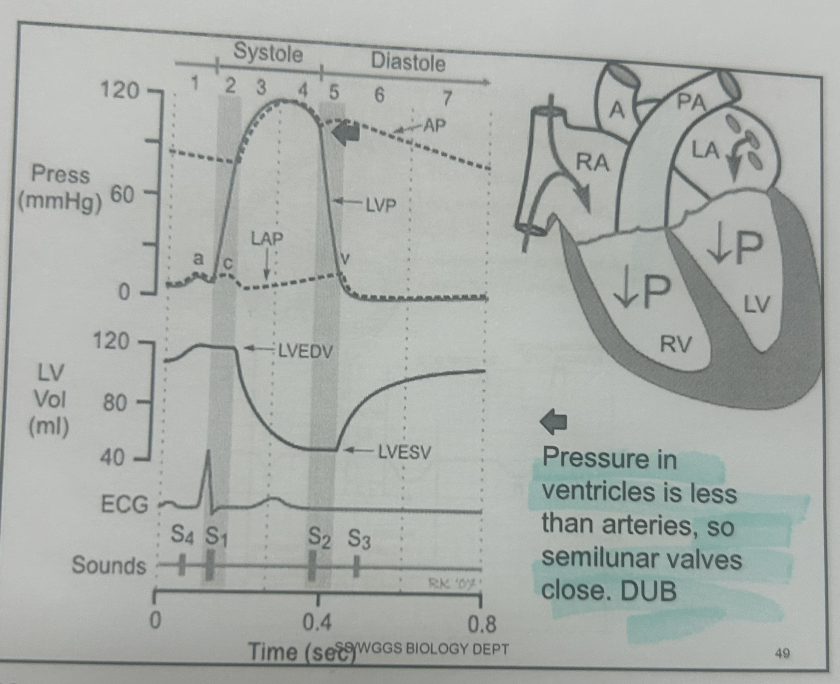
1- diastole, atria and ventricles relax and blood enters heart
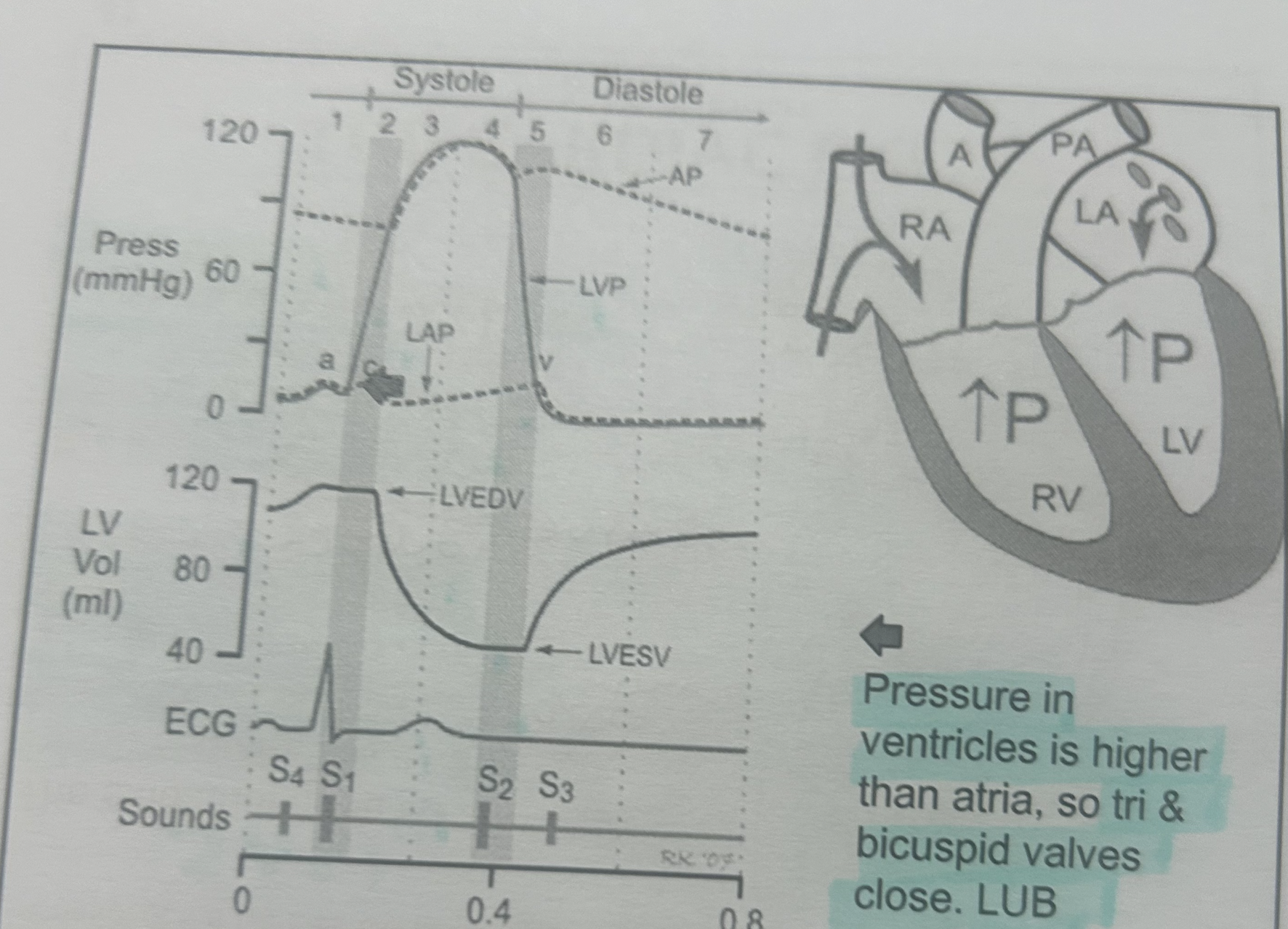
2- atrial systole, atria contract and ventricle react, blood enters ventricle
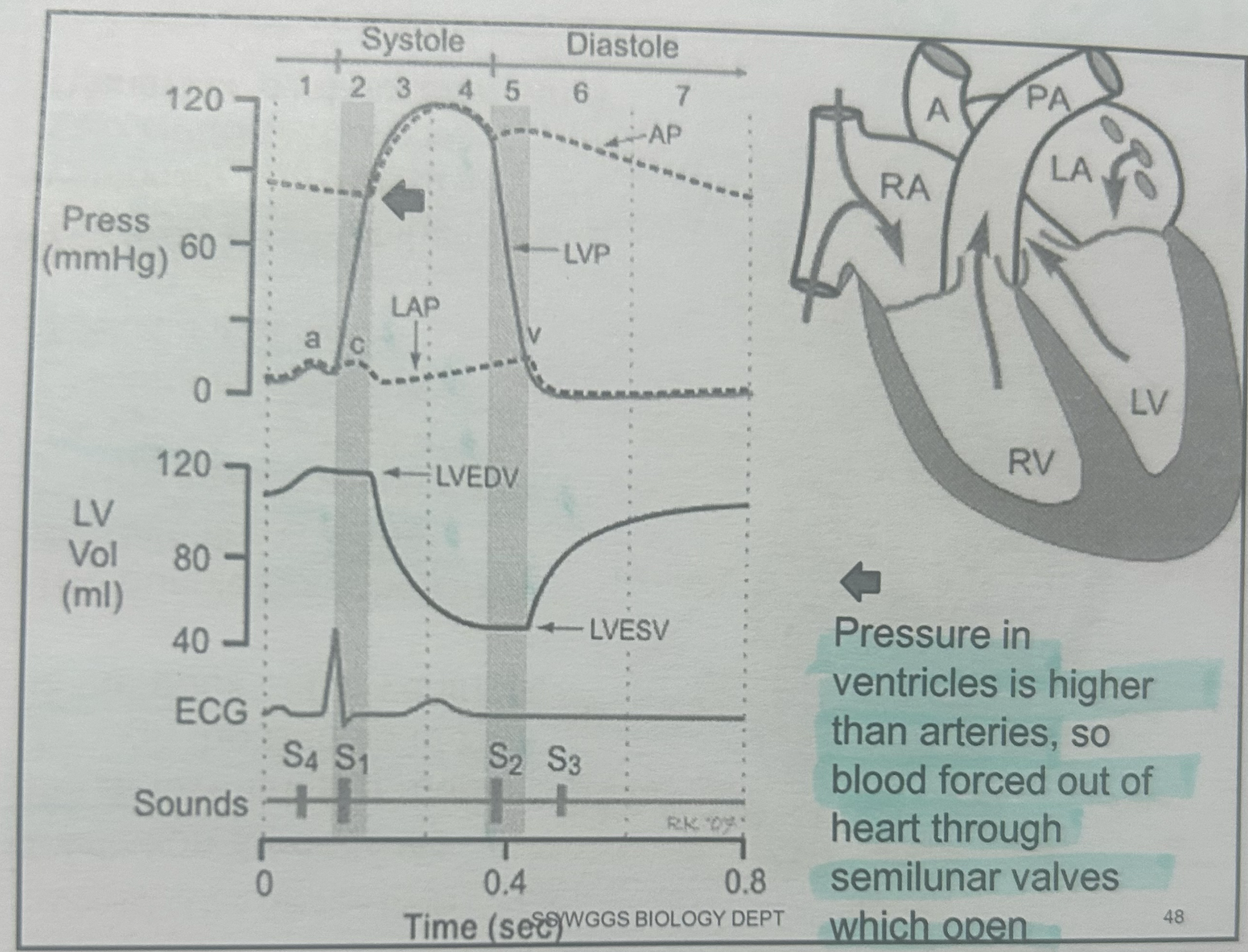
3-ventricular systole, ventricle contracts and blood is forced out of heart.
more detailed heargt
How does the heart contract
the SAN sends a wave of excitation across the atria causing them to contract at the same time
This is prevented from spreading to the ventricles by a thin layer of connective tissue
Instead it spreads via the atrioventricular node, through the bundle of His to the apex of the ventricle . This branches into the Purkinje fibres which carry the wave of excitation through the ventricle muscle .
What does LVEDV mean
left ventricular end diastoli volume (volume of blood in the ventricle at the end of filling)
What does LVP mean
left ventricular pressure
LVESV
left ventricular end systolic volume (volume of blood in the ventricle at the end of emptying)
graphs
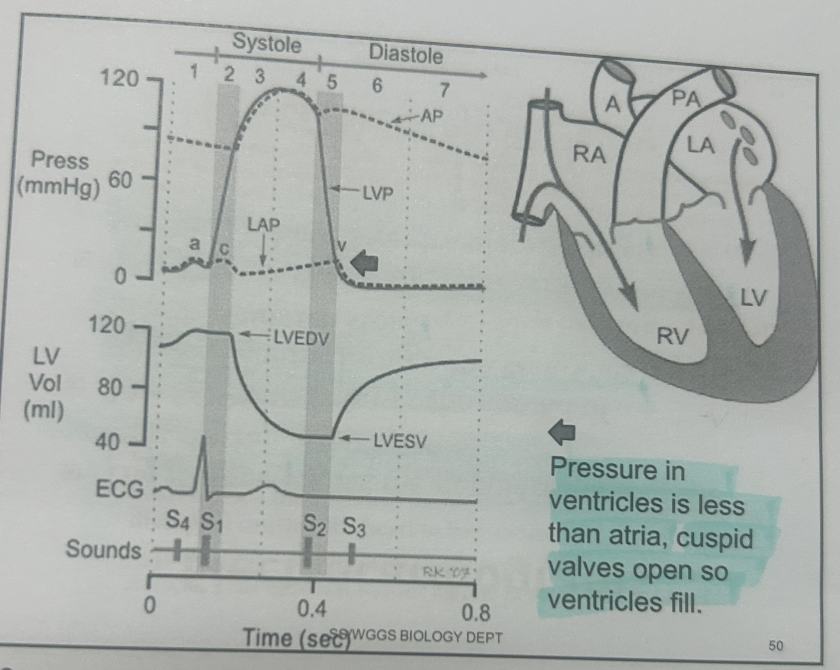
What are electrocardiograms
the electrical activity through the heart can be detected using electrodes
What does a ECT wave (healthy) look like
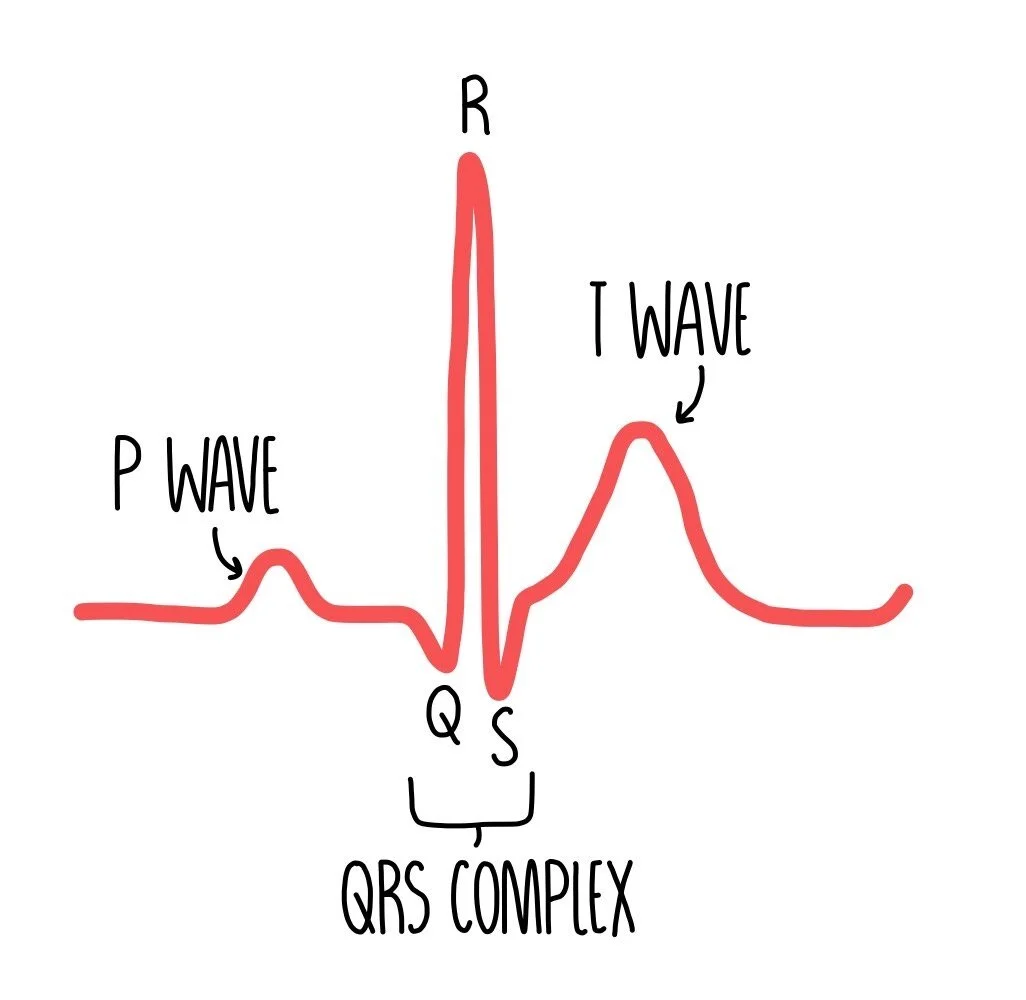
What does the P wave on an ECG show
the depolarisation of the atria during atrial systole
What does QRS wave on an ECG show
the spread of depolarisation through the ventricles resulting in ventricular systole
What does the T wave in an ECG diagram show
the repolarization of the ventricles during ventricular siastole
Where is blood pressure the highest and what does ti show
in the aorta and main arteries, showing rhythmic rise and fall corresponding to ventricukar contraction
Why does blood pressure drop as it moves away from the heart?
friction between blood cells and vessel walls as blood flows further from the heart
How do arterioles and capilleries affect blood flow?
large total surface area and narrow bore create high resistance. Lowers aortic pressur and slows down blood flow.
Whats the relationship between blood velocity, pressure and capillary beds?
velocity is directly related to pressure
Return flow to the heart
non-rhythmic. Pressure in veins is low but can be increased by the massaging effect of the muscles
red blood cells
erythrocytes
white blood cells
leucocytes
1-Granulocytes- granular cytoplasm and lobved nucleis. Phagocytic
2-agranulocytes- clear cytoplasm and spherical nuclei. produce antibodies
adaptations of Erythrocytes
-biconcave discs- large SA:V, flexible to pass through capilleries
-Haemoglobin- carries 12x more oxygen
-no nuceleus- more volume for Hb
Haemoglobin structure
4 subunits of a polypeptiude chain surrounding a haem gorup
Each haem group can carry one oxygen molecule
What is Partial Pressure of oxygen
a measure of oxyge concentrations.
21 kPA (atmospheric pressure = 100kPa)
What is an oxygen dissasociation curve
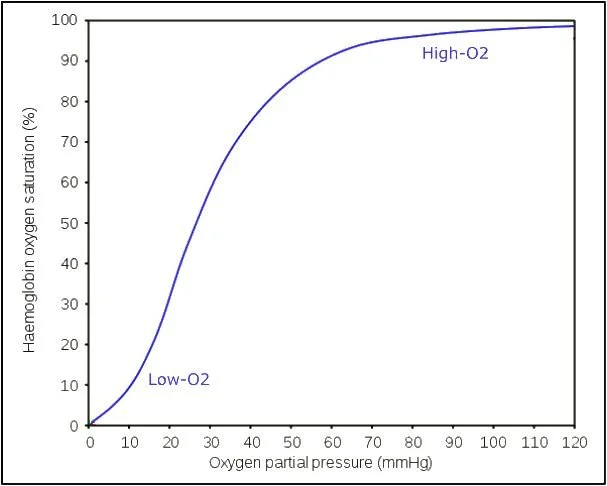
shows relationship between oxygen tension in surrounding environment and oxygen saturation in haemoglobin
Describe an oxygen dissociation graph
The curve is S-shaped. It is harder for the first o2 to join and it joins slower. When it loads/associates a conformational change in the haemoglobin shape occurs. This gives it a higher affinity for the next to oxygen to load, causing the steep section of the graph. Called positive cooperativity
It is more difficult for the last oxygen to load.
at low partial pressure haemoglobin has a low affinity for oxygen
Foetal haemoglobin
Lies to the left- showing it has a greater affinity for oxygen
The Bohr effect (oxygen dissasociation curve)
in hight CO2 the curve shifts to the right so Hb more readily gives up its O2. (UNLOADsS in Low CO2 it shifts to the left, LOADING oxygen mroe readily.
In active tissues there is more respiration = more CO2 = tissues need more oxygen = more unloading
Opposite in lungs
LLAMA haemoglobin adaptation
at high altitude there is a drop in atmospheric prssure so ppO2 is less. This means the haemoglobin must have a high affinity for oxygen and curve shifts to the left
LUGWORM haemoglobin adaptations
They burrow in the sand. ppO2 in the water in the buyrrow is low so their haemoglobin has a high affinity for oxygen and have low metabolic needs
How is carbon dioxide transported
-5% in solution in plasma
-10% combines with haemoglobin to make Carbaminohaemoglobin
-85% as hydrogen carbonate
Bohr effect and chloride shift in blood
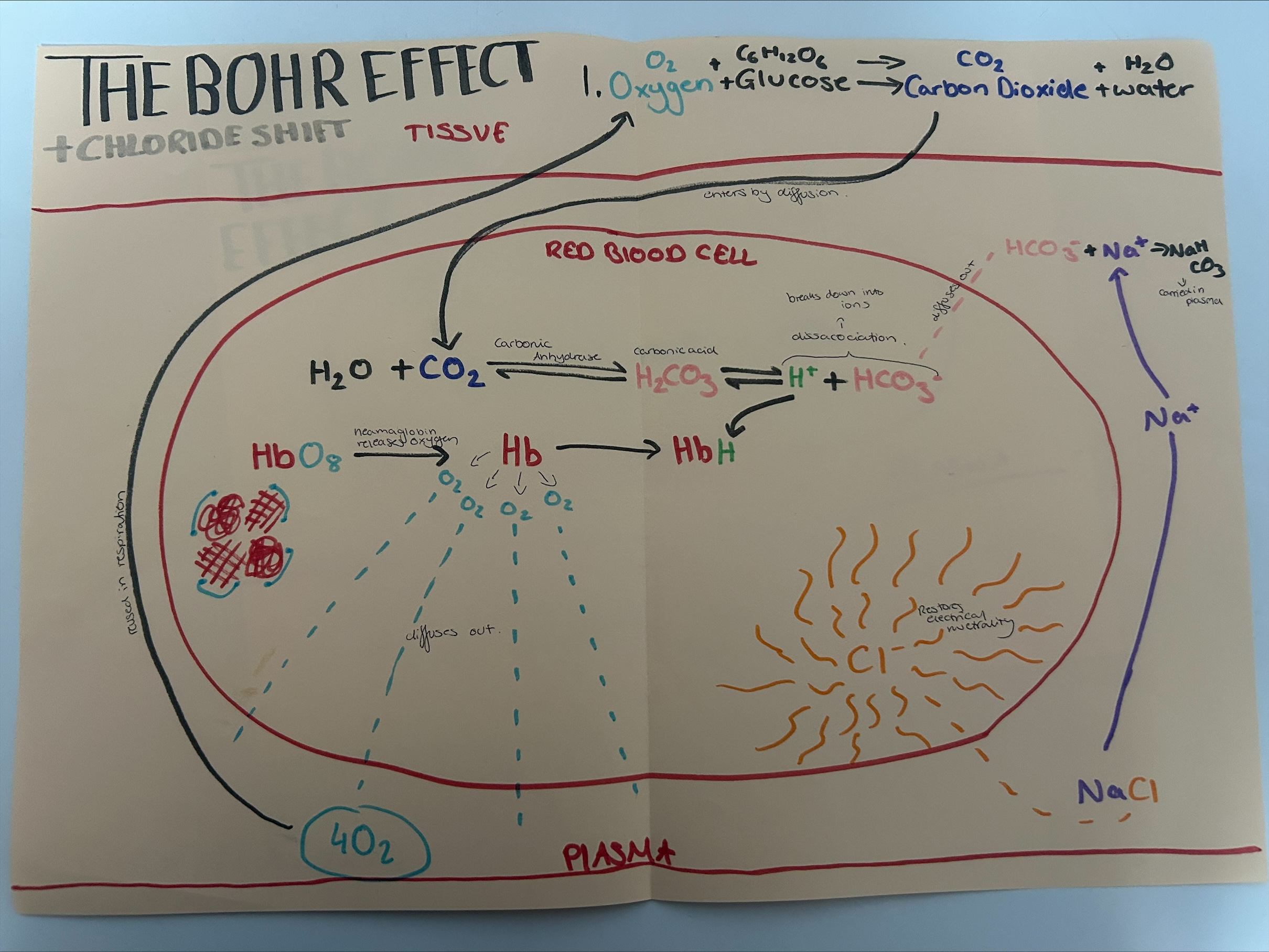
Bohr effect in lungs
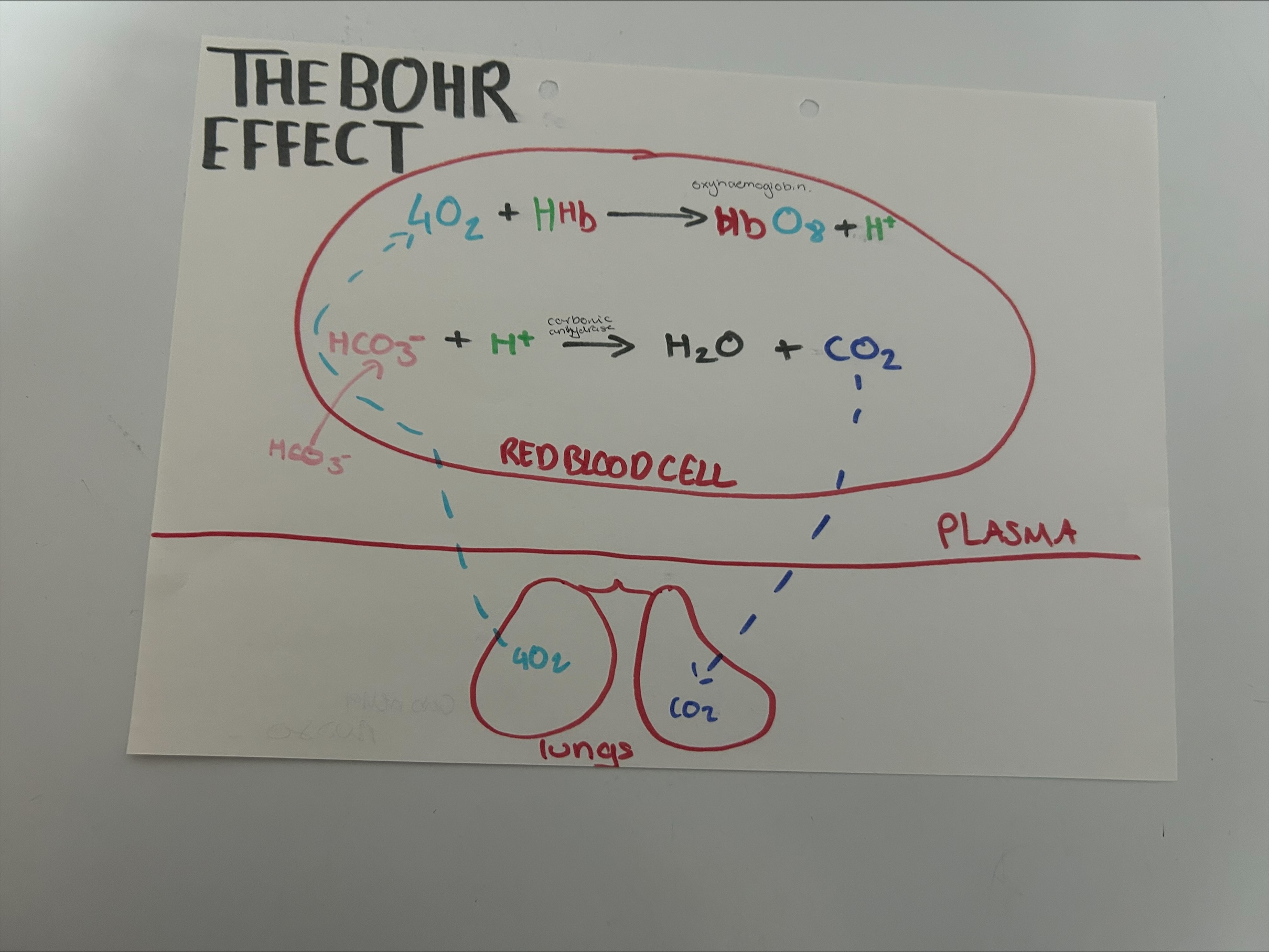
How is tissue fluid formed
ultrafiltration, formed by two pressures:
Osmotic pressure- pulling materials into capilleries
Blood pressure- forcing materials out of capilleries
has water, gluose, amino acids, fatty acids,glycerol, mineral salts, vitamins
tissue fluid journey
At the begining of the capillary beds water and small solutes pass out throuhg the endothelium. The presence of proteins means hydrostatic pressure is greater then water potential and osmotic pressure.
At the end of the tissue bed the hydrostatic opressure had dropped due to loss of fluid and resistance of blood flow through capilleries. Osmotic pressure causes water and solutes to flow back in
T.S of an artery
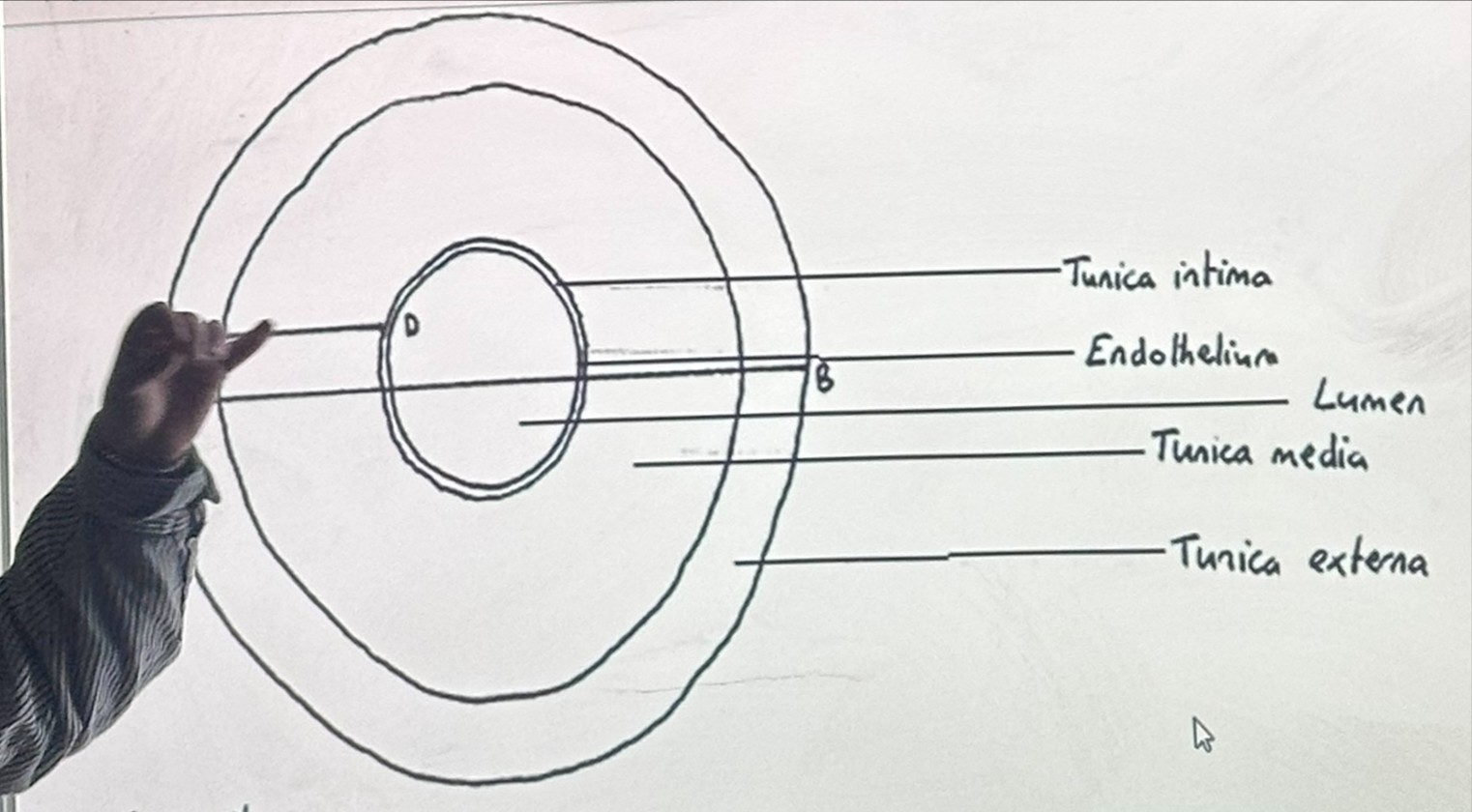
T.S of vein