Salivary Gland Lesions
1/57
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
58 Terms
what reactive salivary gland lesion is also known as mucous retention phenomenon?
mucocele
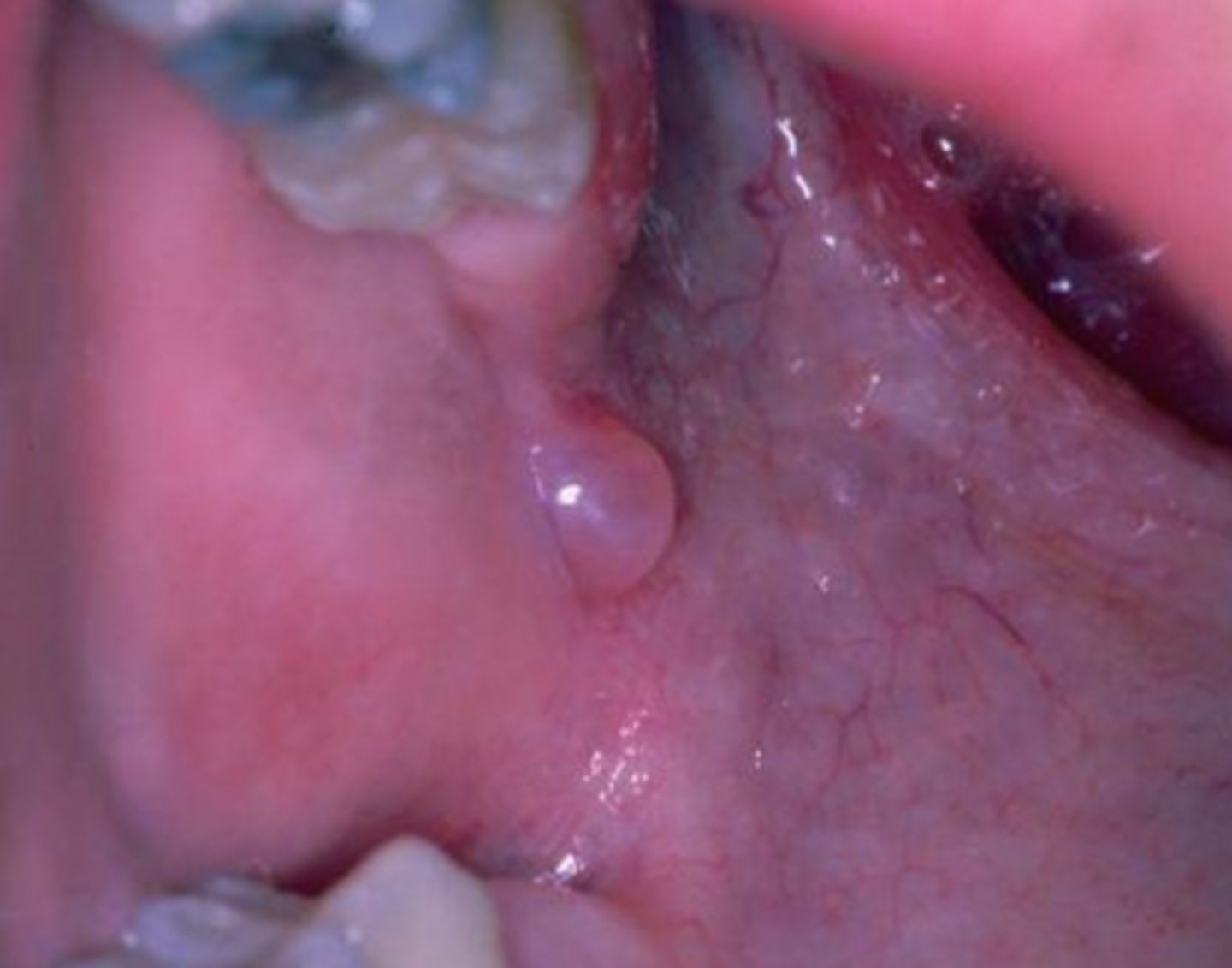
what reactive salivary gland lesion results from a rupture (not blockage) of a salivary gland duct and spillage of mucin?
mucocele
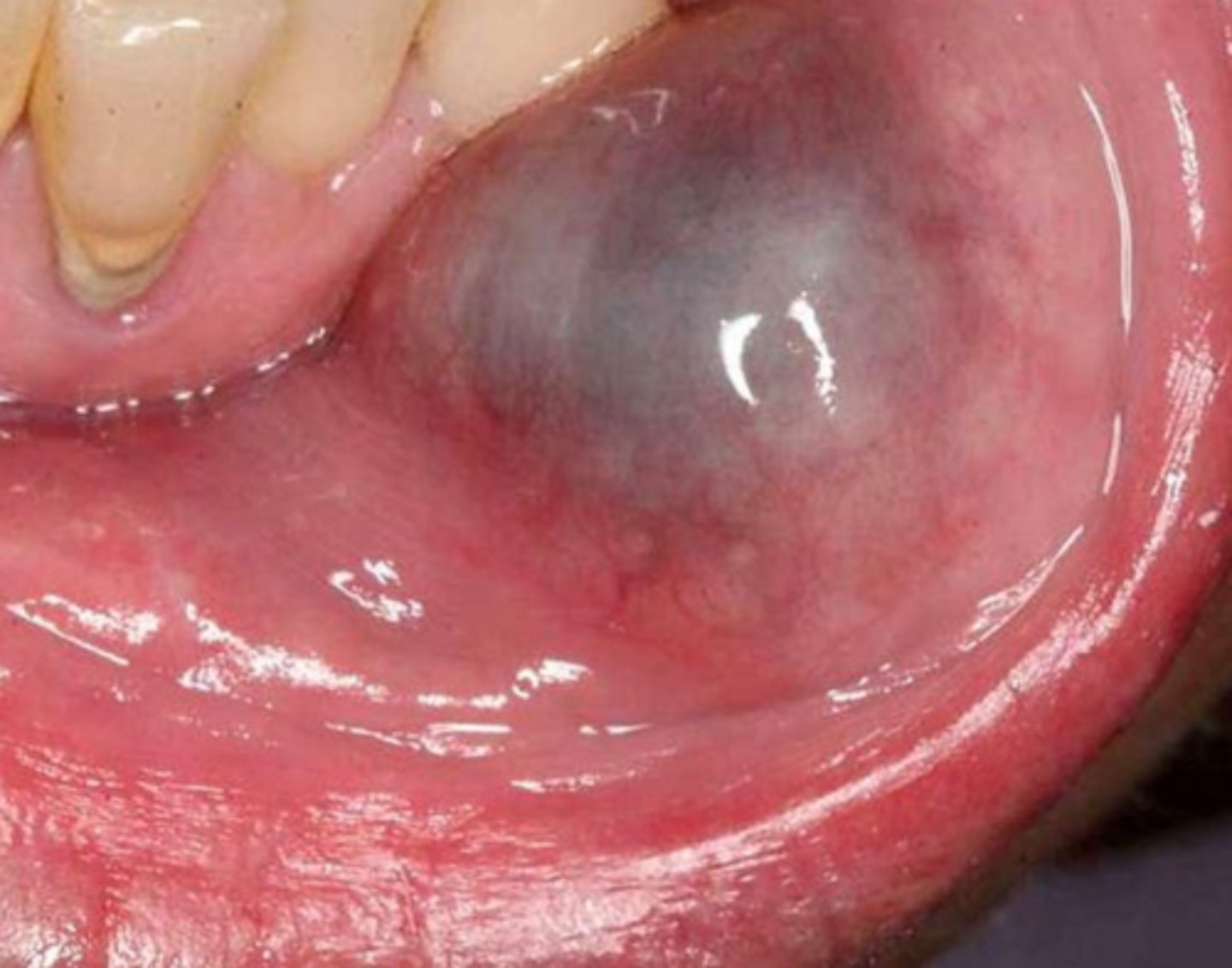
what reactive salivary gland lesion is often due to trauma (pinching/biting/hitting) seen in children and young adults, mainly found in the lower lip, and occurs in those with a history of recurrent swelling that may periodically rupture?
mucocele
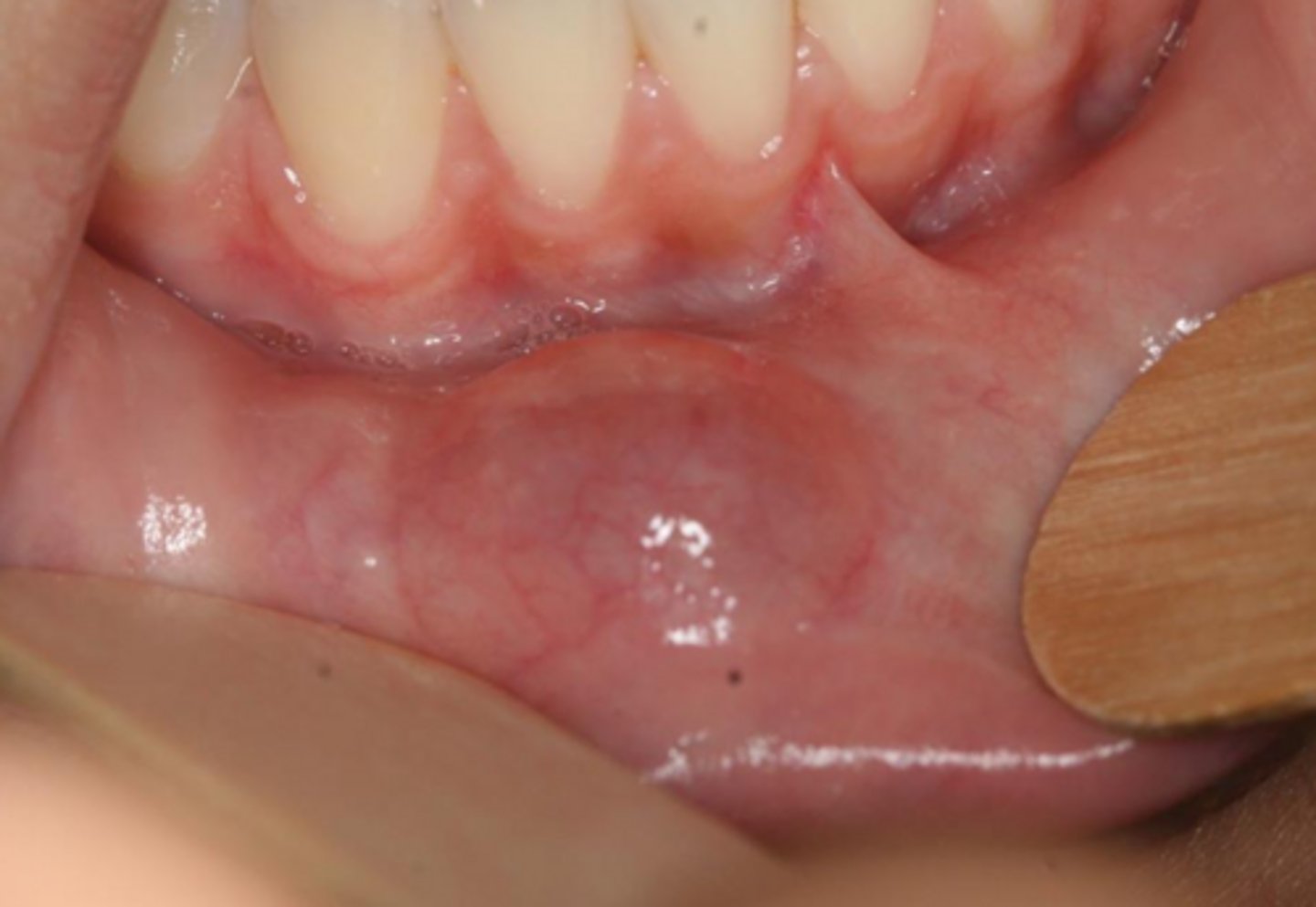
what reactive salivary gland lesion appears as a dome-shaped swelling with a bluish-translucent hue?
mucocele
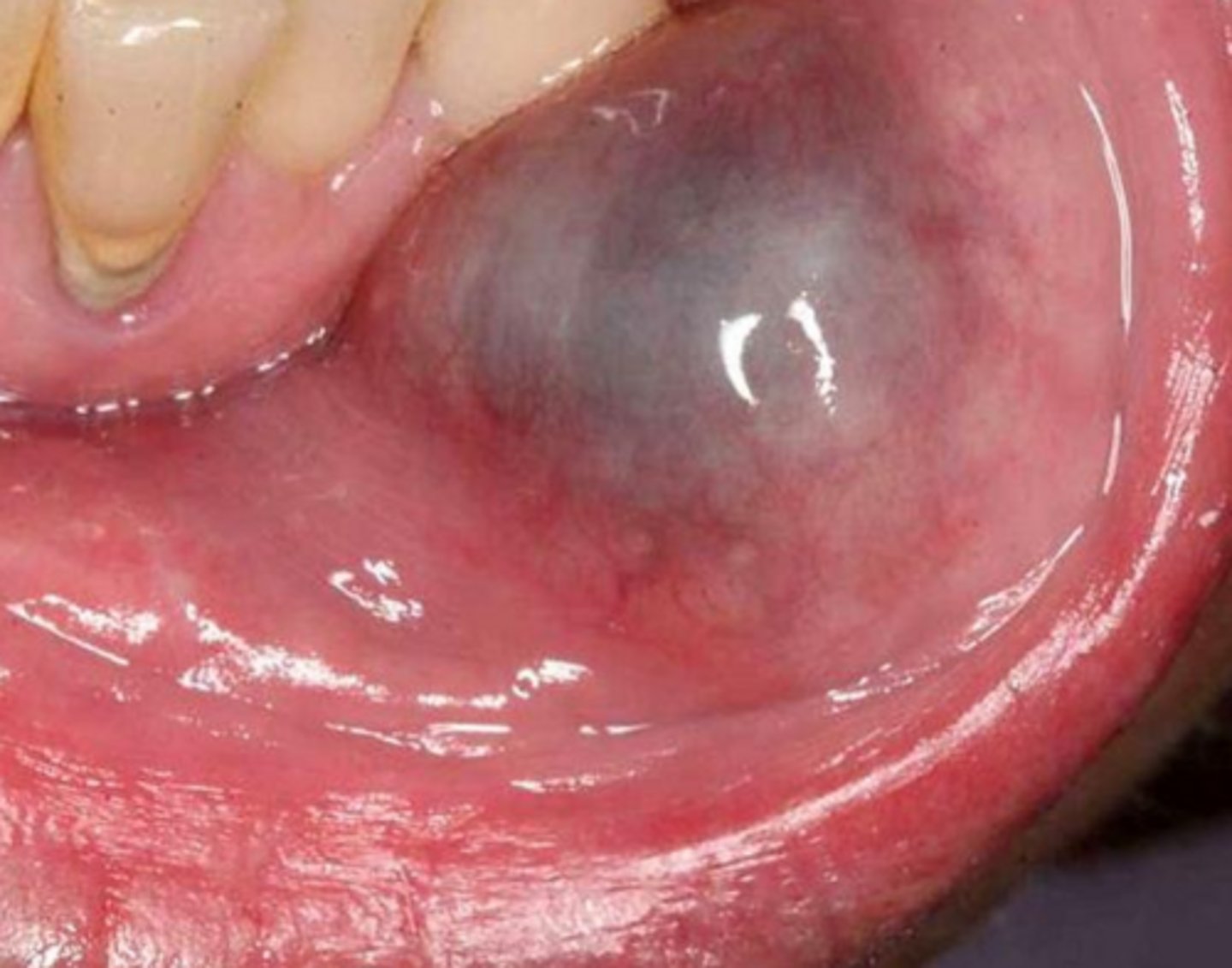
what reactive salivary gland lesion are short-lived and rupture then heal on their own, but may require surgical excisions if chronic by removing adjacent minor salivary glands?
mucocele; excellent prognosis
what term refers to mucoceles that occur in the floor of the mouth usually caused from the sublingual gland, usually lateral to the midline?
ranula
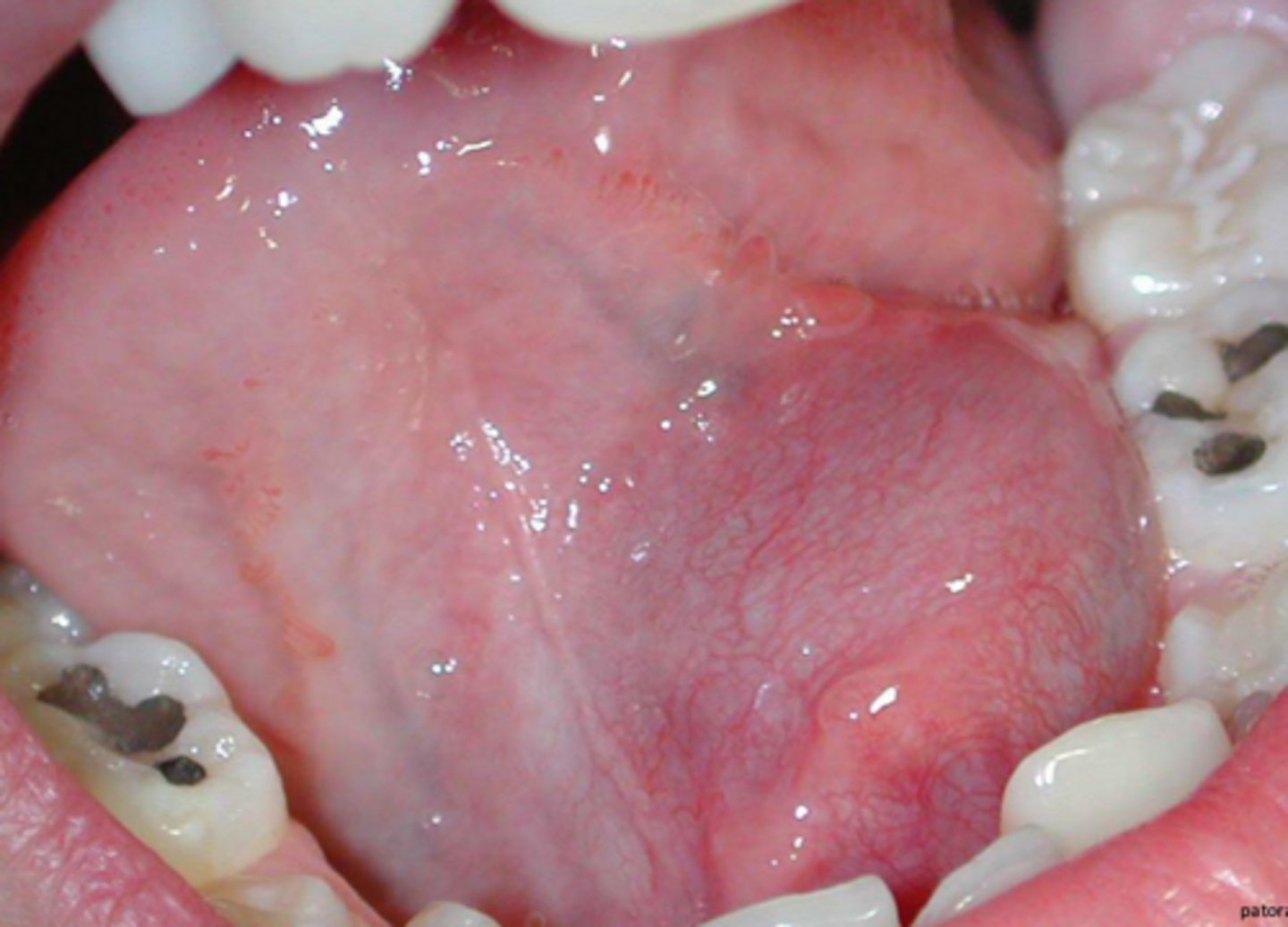
what term refers to a ranula that spills through the mylohyoid muscle and produces a swelling within the neck?
plunging/cervical ranula
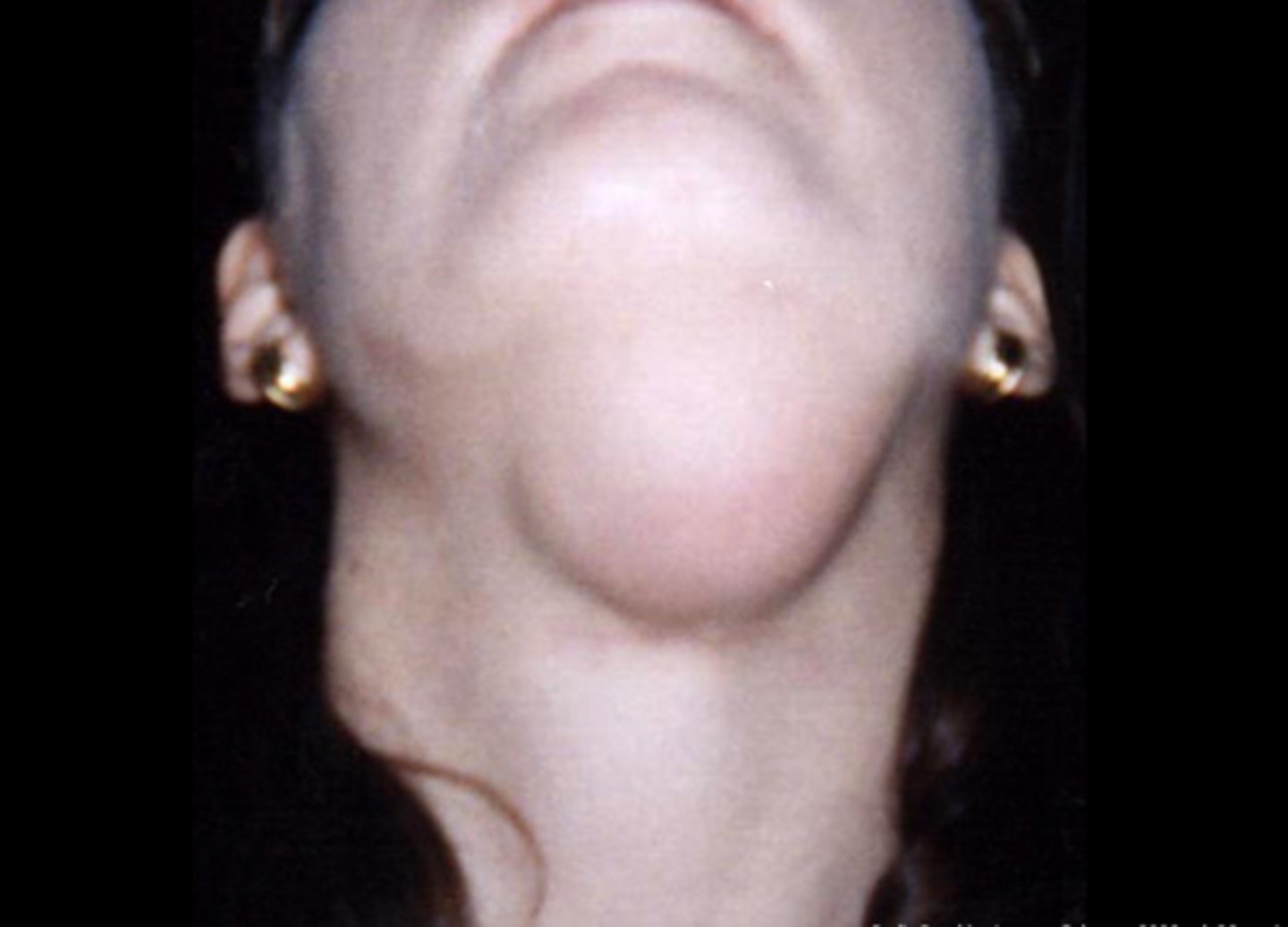
(t/f) plunging/cervical ranula are dangerous
true
(t/f) ranulas tend to be smaller than other mucoceles
false; ranulas tend to be larger than other mucoceles
how are ranulas treated?
removing the feeding gland
what is the calcified, round, yellow, hard mass structure within the salivary ductal system caused by the deposition of calcium salts around a nidus of debri within the lumen?
sialolith
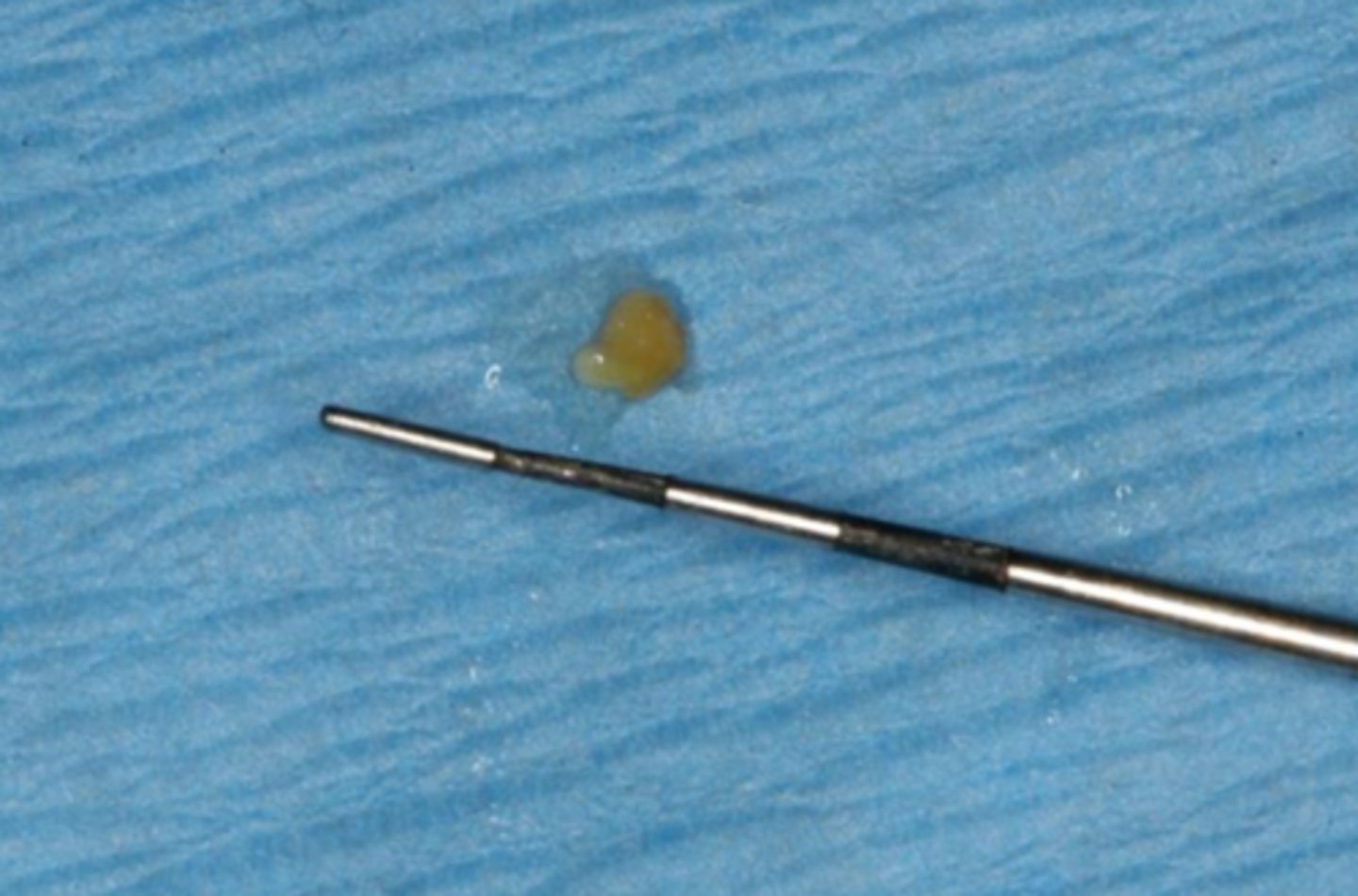
what reactive salivary gland lesion most commonly occurs in the submandibular gland/duct due to the tortuous path of Wharton's duct and may be firm/hard?
sialolithiasis
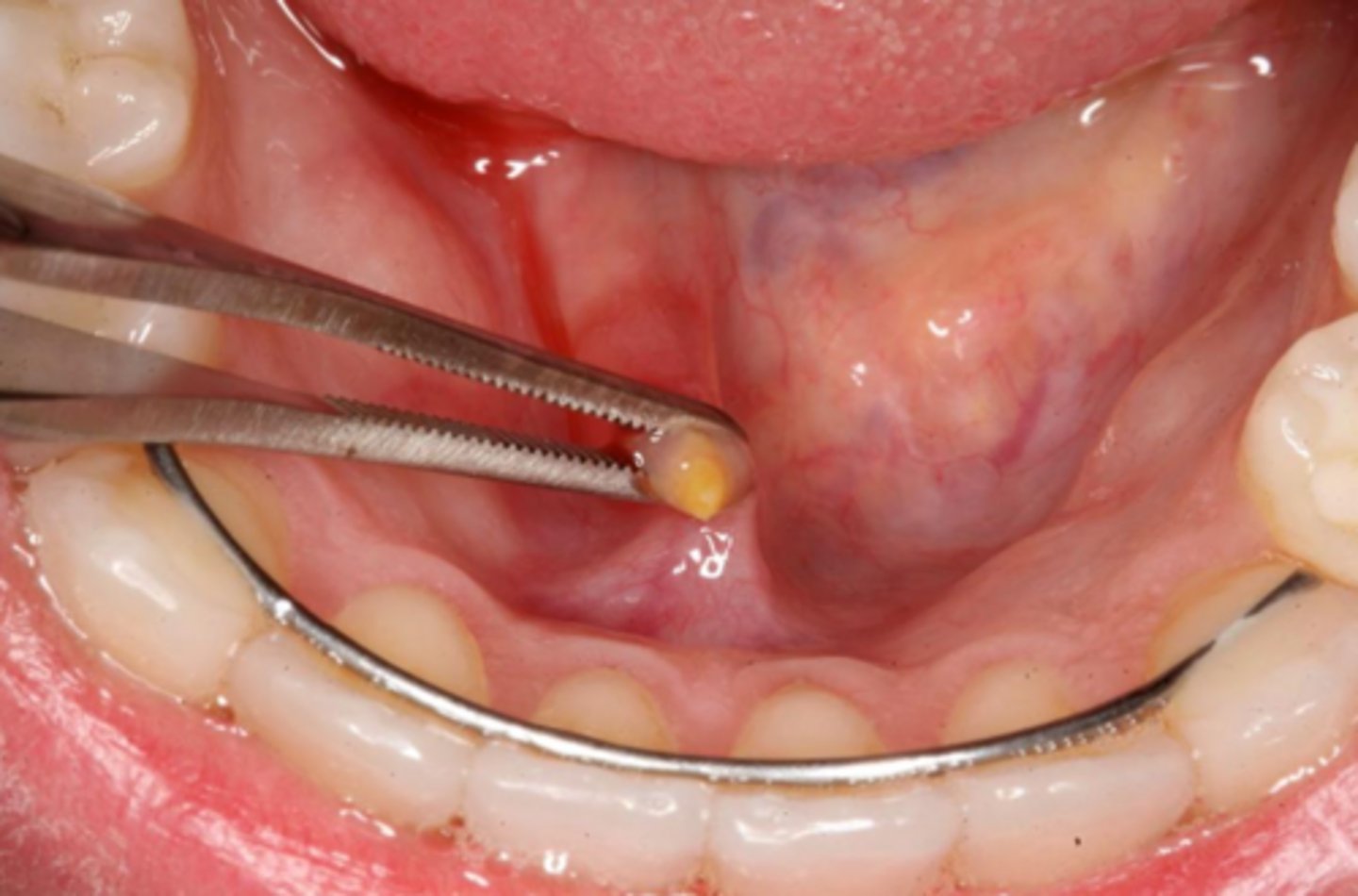
what reactive salivary gland lesion causes pain and swelling during times of increased salivation?
sialolithiasis
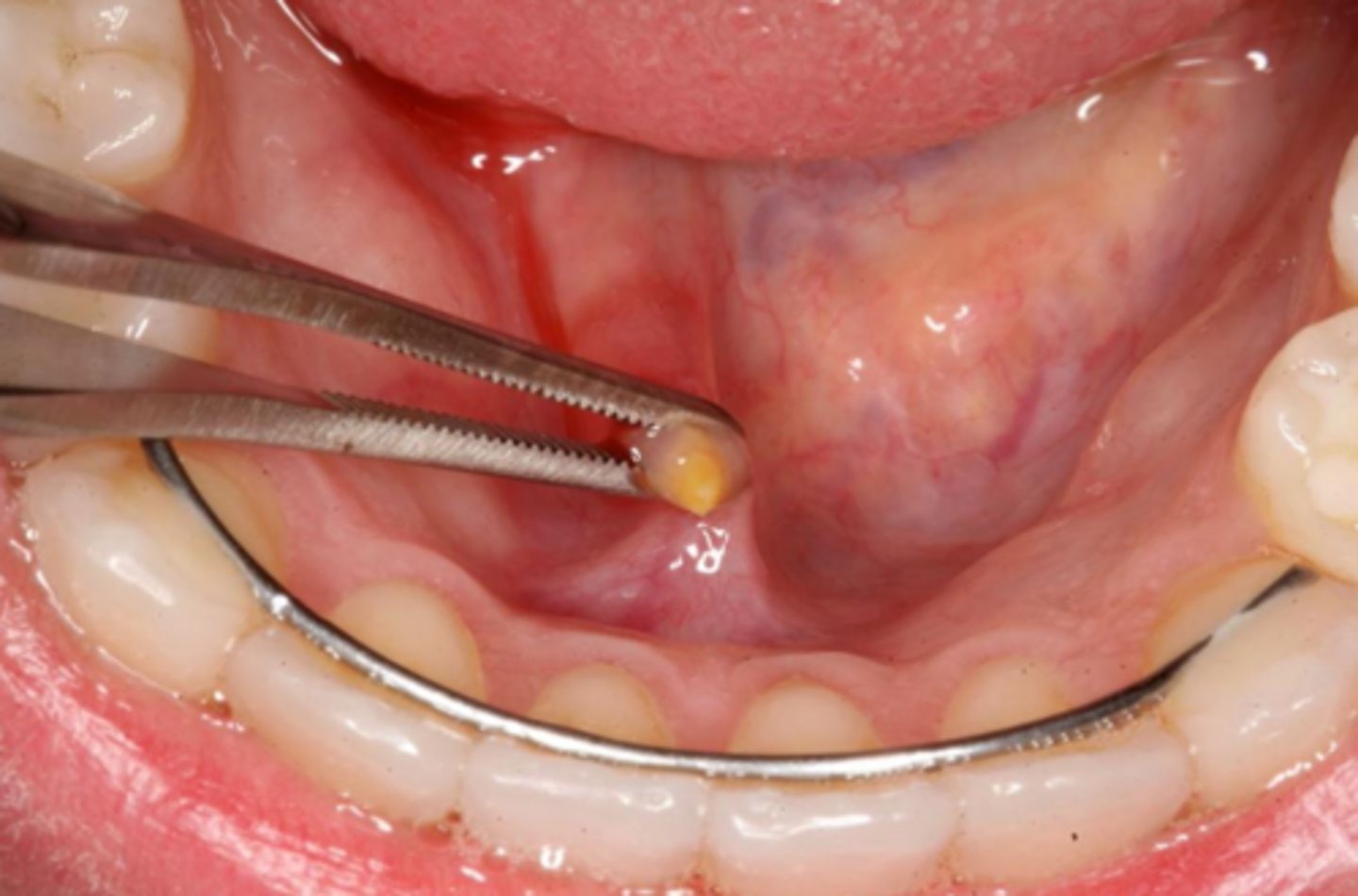
(t/f) sialoliths appear as radiolucent masses on radiographs
false; sialoliths appear as radiopaque masses on radiographs
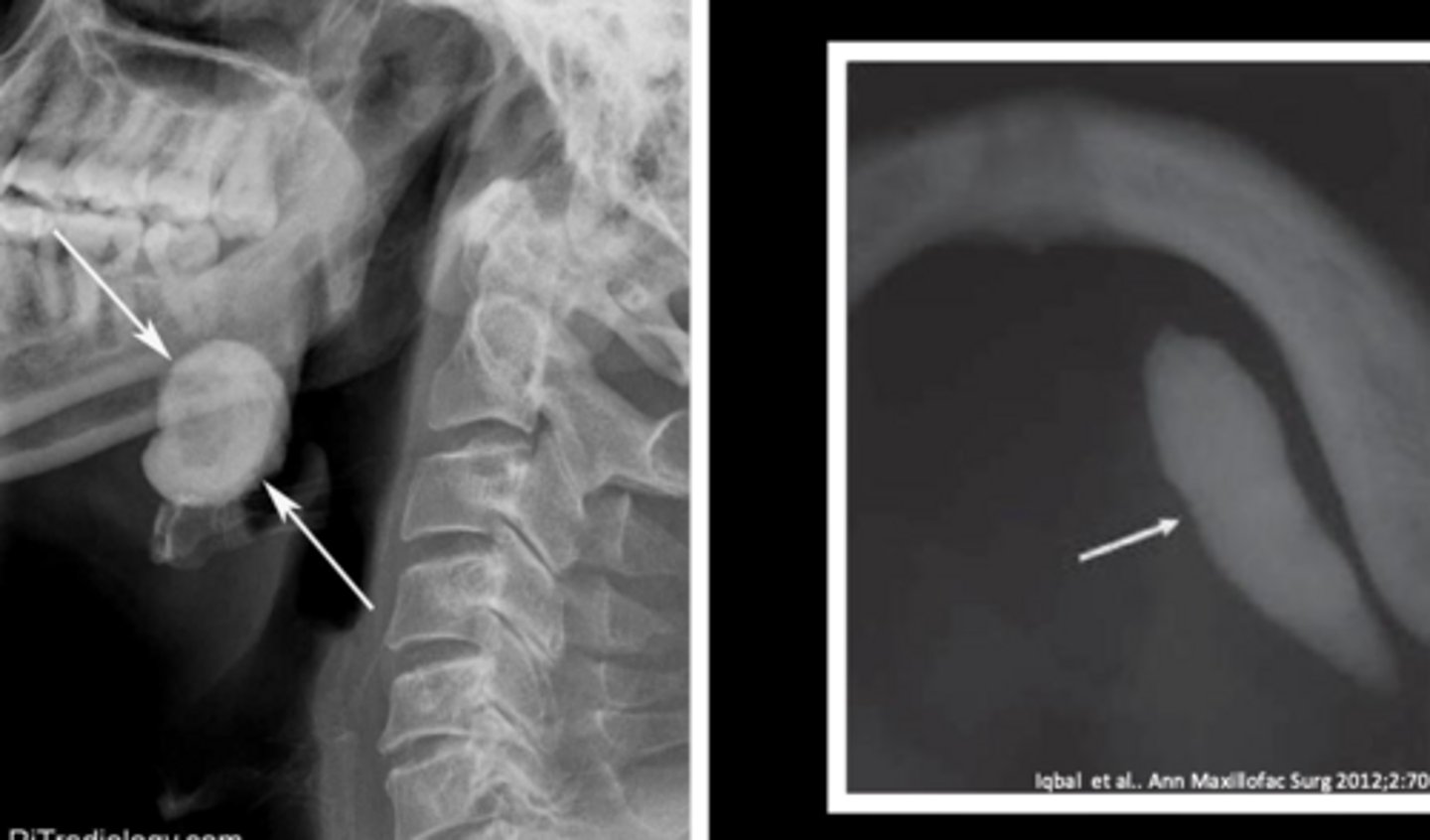
how are small sialoliths treated? how are large sialoliths treated?
milking the stone out; need surgical removal (entire gland may need to be removed)
what reactive salivary gland lesion is treated with sialagogues, moist heat, and fluid intake to promote passage?
sialolithiasis
what infectious salivary gland lesion is the inflammation of salivary glands (acute or chronic) from ductal obstruction (sialolith) or decreased saliva flow allowing the retrograde spread of bacteria?
bacterial sialadenitis
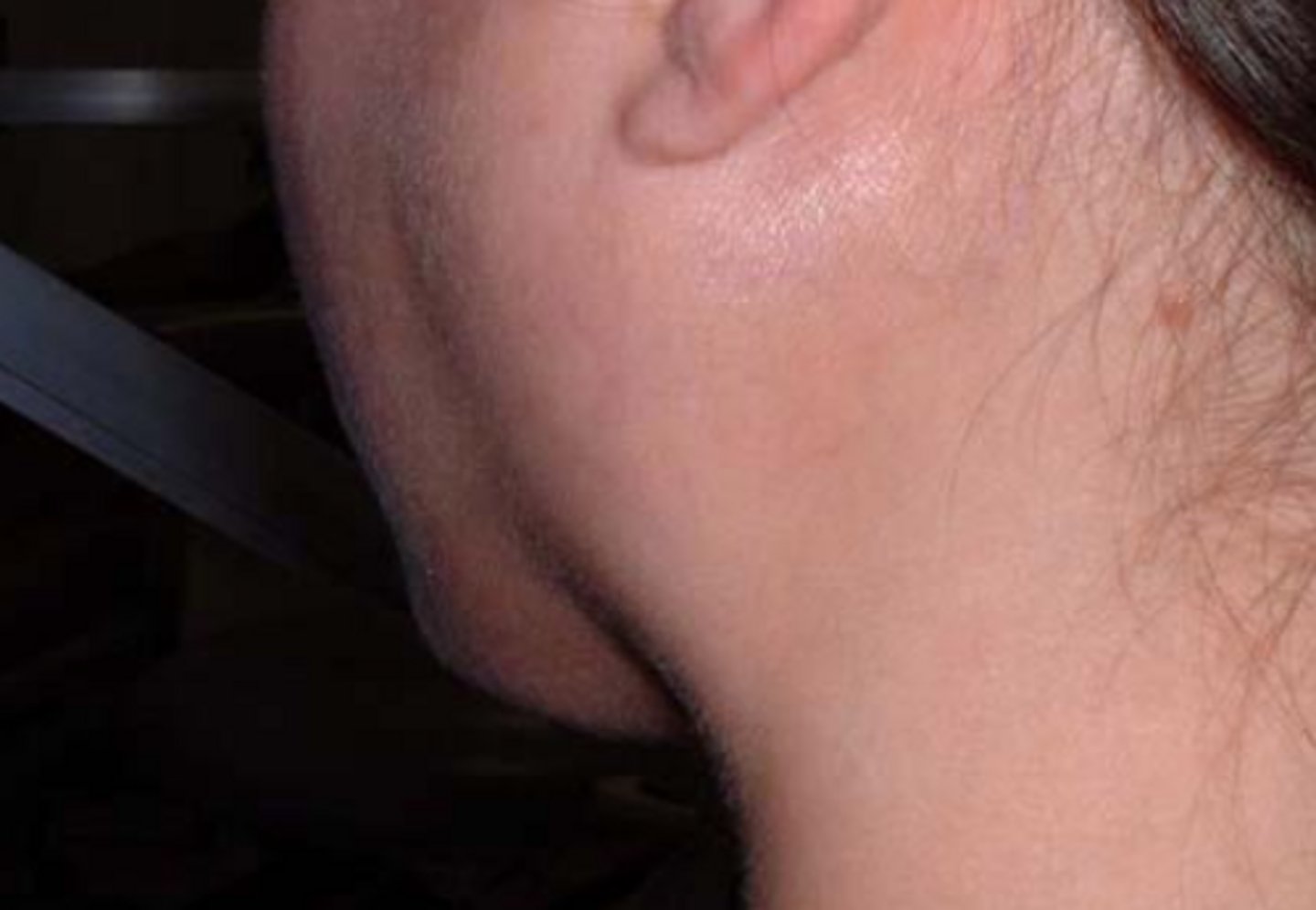
what infectious salivary gland lesion usually affects the parotid gland, can be bilateral, and causes acute pain, swelling (often at meal time), and lymphadenopathy?
bacterial sialadenitis
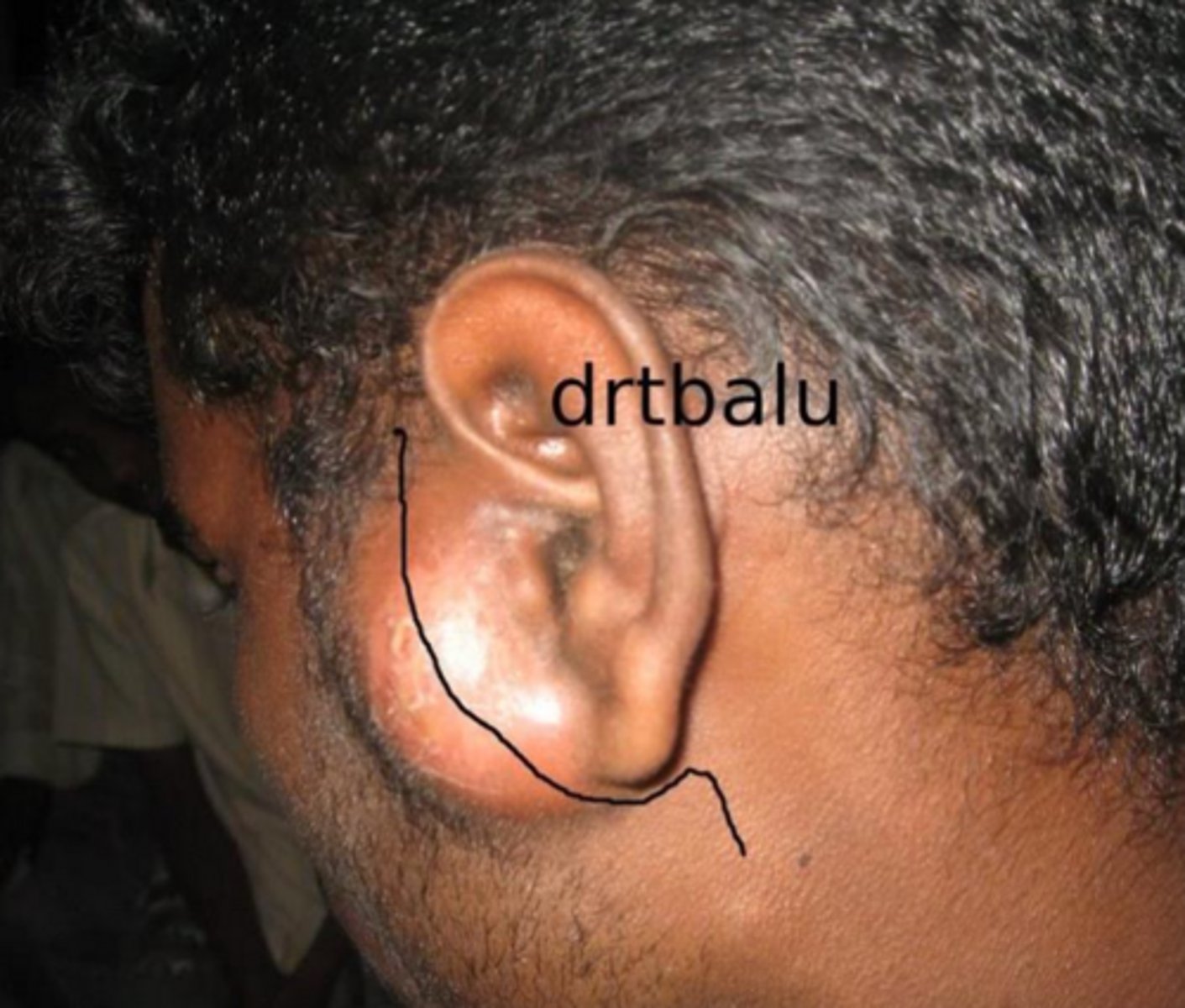
what infectious salivary gland lesion is treated with antibiotics and rehydration in acute cases or surgery in chronic cases?
bacterial sialadenitis; removal of sialolith may be beneficial
what infectious salivary gland lesion is also known as mumps?
viral sialadenitis

what infectious salivary gland lesion is caused by paramyxovirus?
viral sialadenitis

what infectious salivary gland lesion begins with low grade fever, headache, malaise, anorexia, and myalgia, then followed by swelling of the salivary glands (mainly bilateral of the parotid glands), then finally epididymo-orchitis or oophoitis?
viral sialadenitis

what infectious salivary gland lesion causes discomfort and swelling from the ear to the mandibular area with enlargement peaking within 2-3 days when pain is worse?
viral sialadenitis
what infectious salivary gland lesion rarely occurs due to vaccination?
viral sialadenitis
what reactive salivary gland lesion is a locally destructive inflammatory condition probably due to ischemia leading to infarction?
necrotizing sialometaplasia
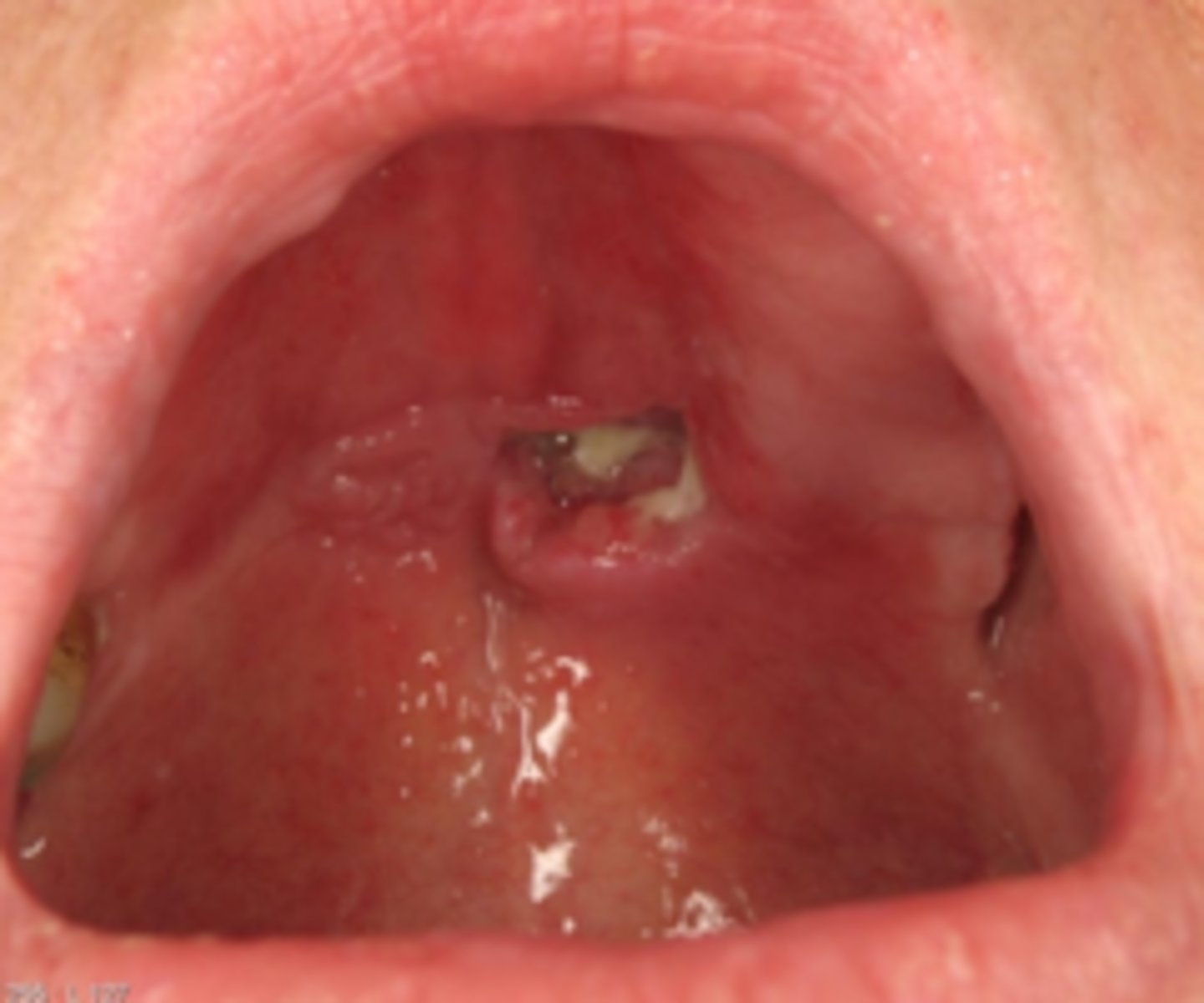
what reactive salivary gland lesion mimics a malignant process (both clinically and microscopically) and mainly occurs on the posterior palate?
necrotizing sialometaplasia
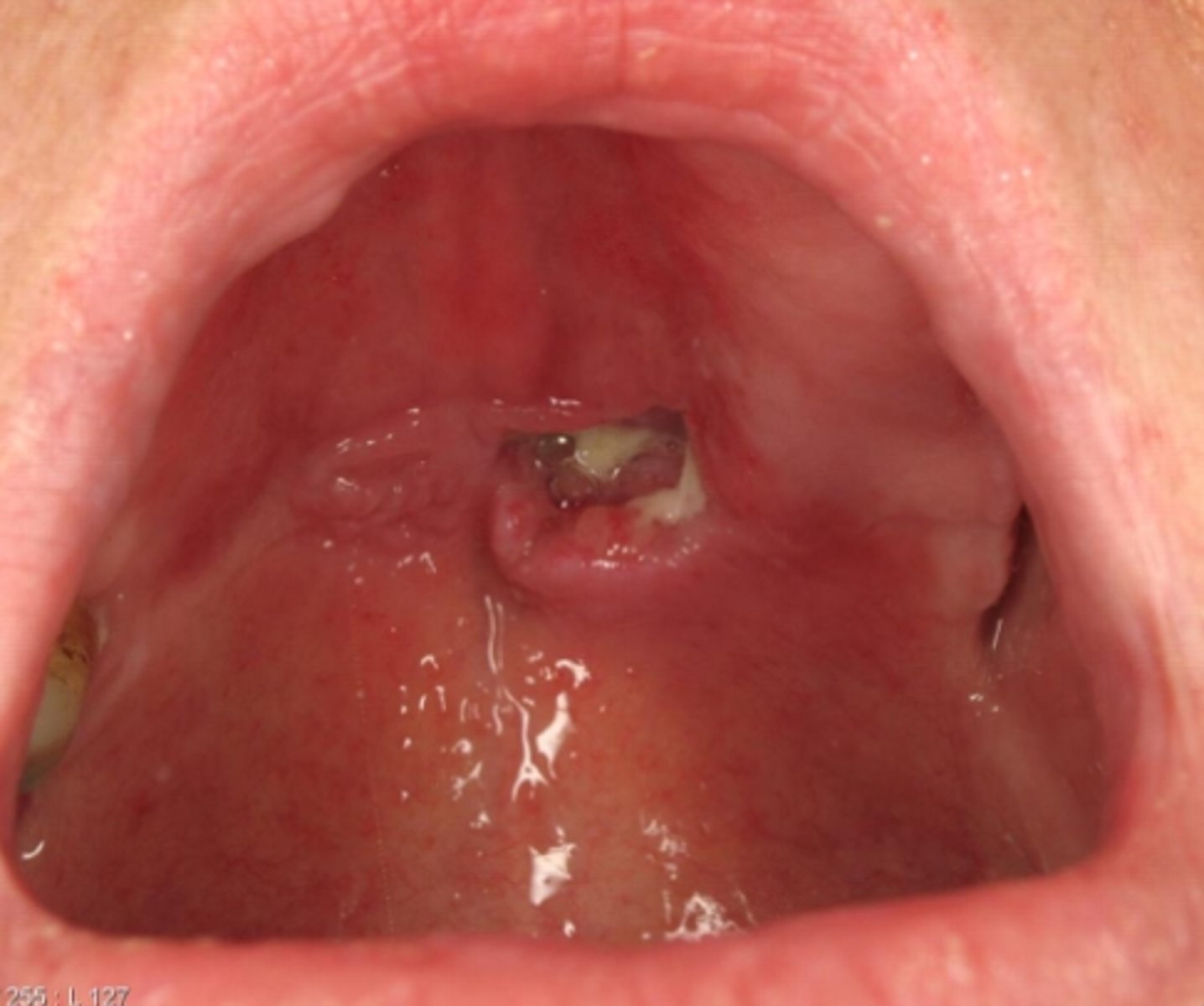
what reactive salivary gland lesion appears as a non-ulcerated swelling then a craterlike ulcer after 2-3 weeks, then finally resolves in 5-6 weeks?
necrotizing sialometaplasia
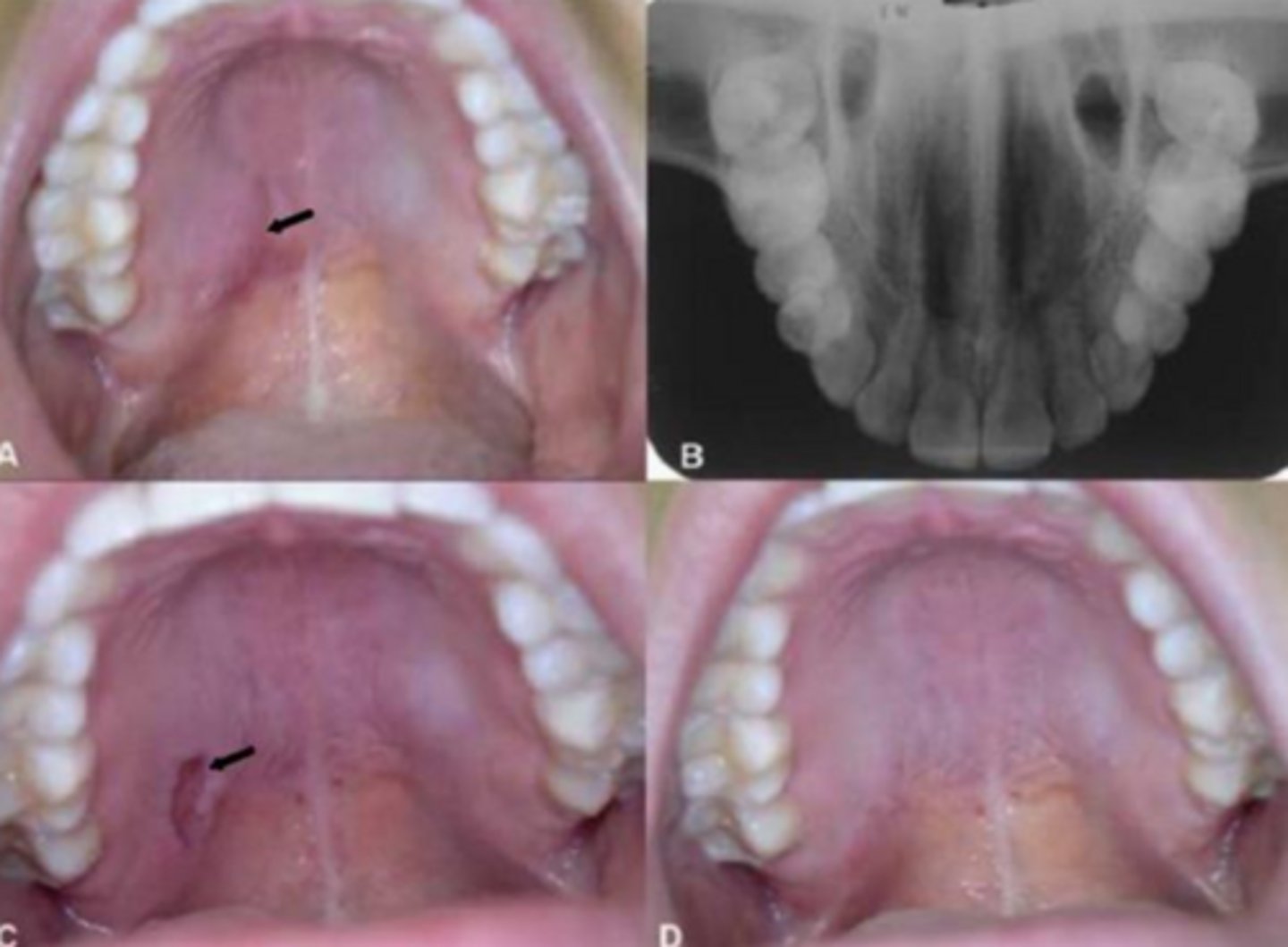
what reactive salivary gland lesion is a local ischemia that causes the infarction of salivary glands leading to squamous metaplasia and hyperplasia of epithelium (resembling SCC)?
necrotizing sialometaplasia
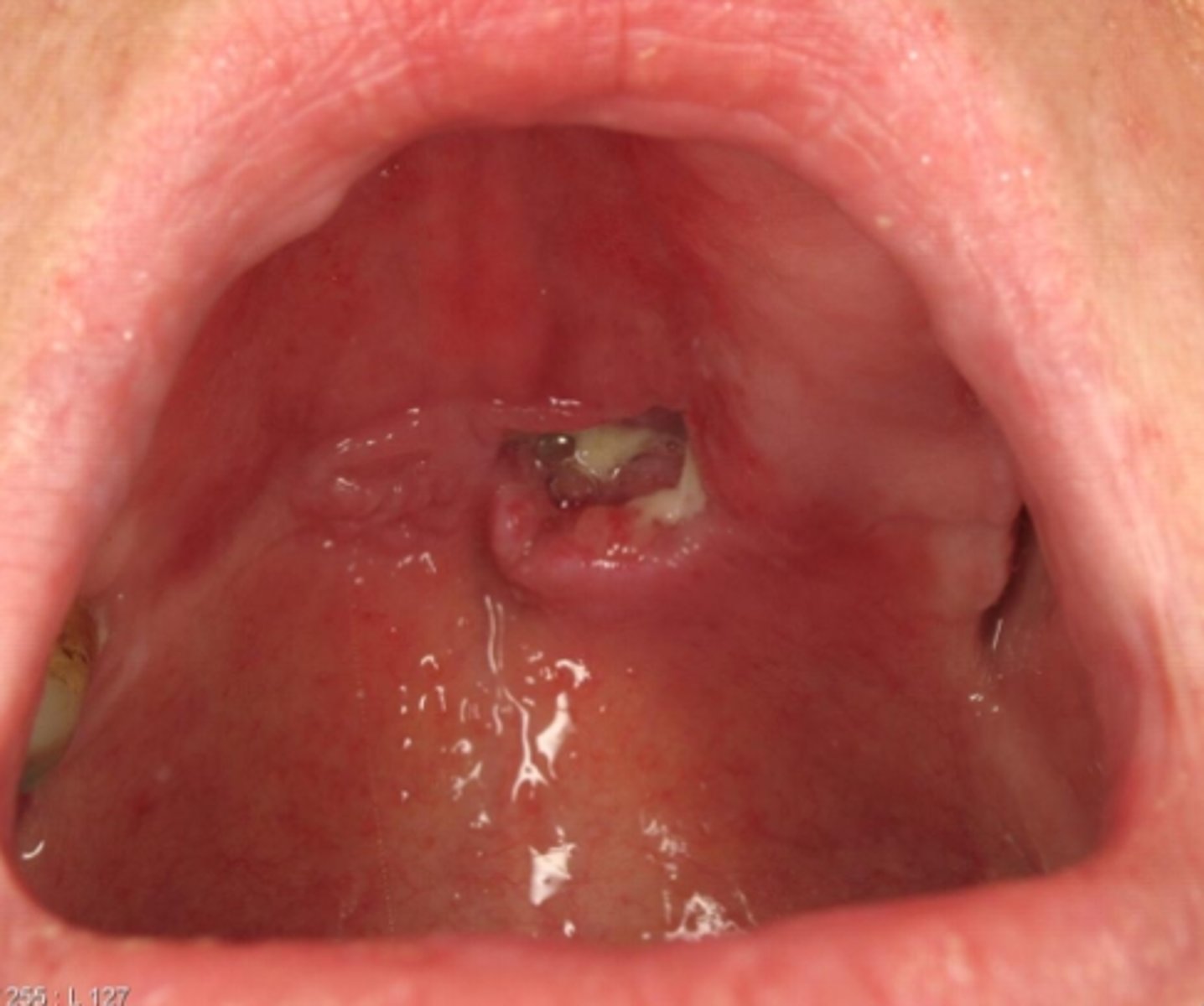
what reactive salivary gland lesion always requires biopsies to establish a diagnosis due to worrisome presentations and resolves on its own in 5-6 weeks spontaneously?
necrotizing sialometaplasia
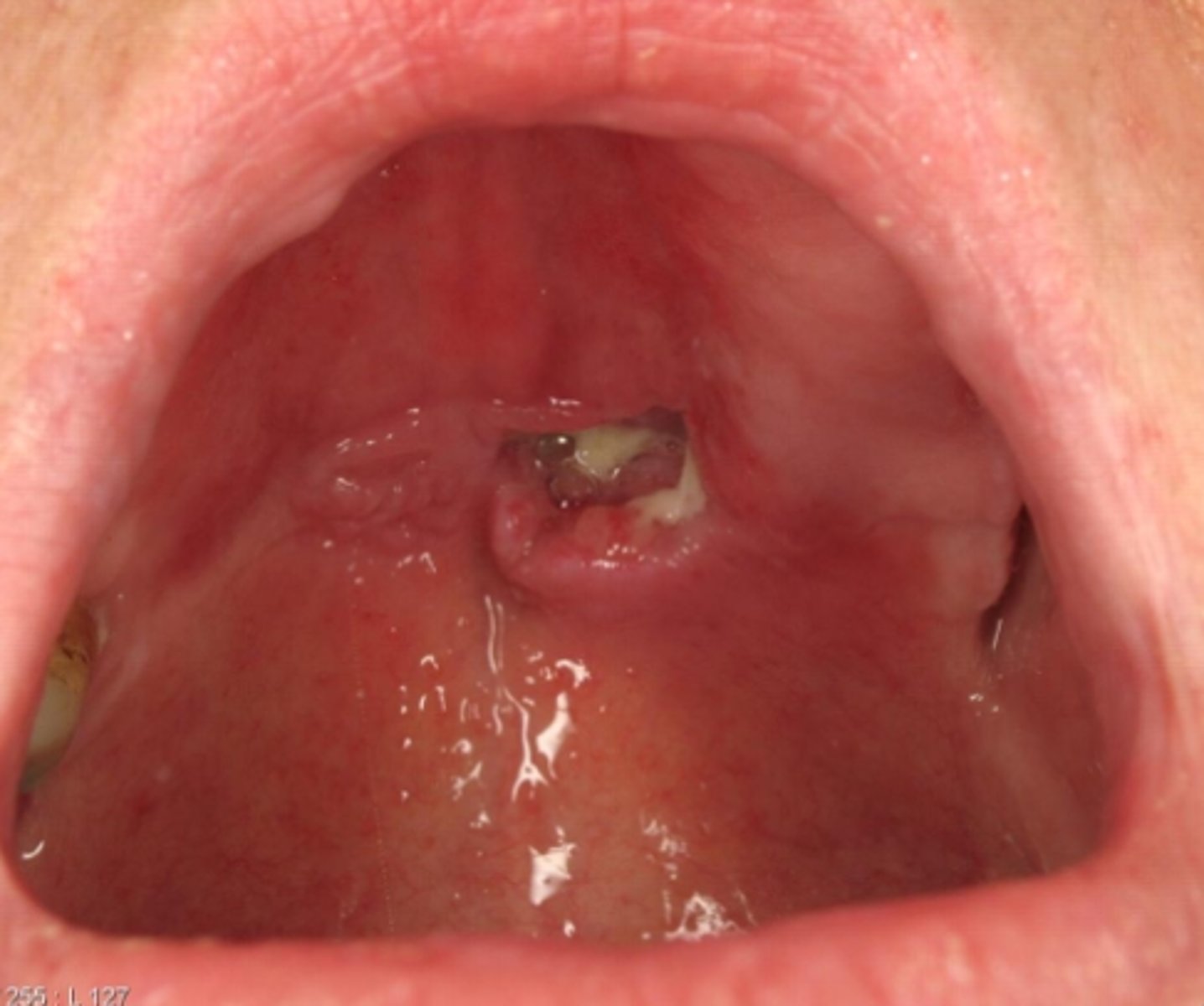
what auto-immune salivary gland lesion is a multisystem, granulomatous disorder of unknown cause?
sarcoidosis
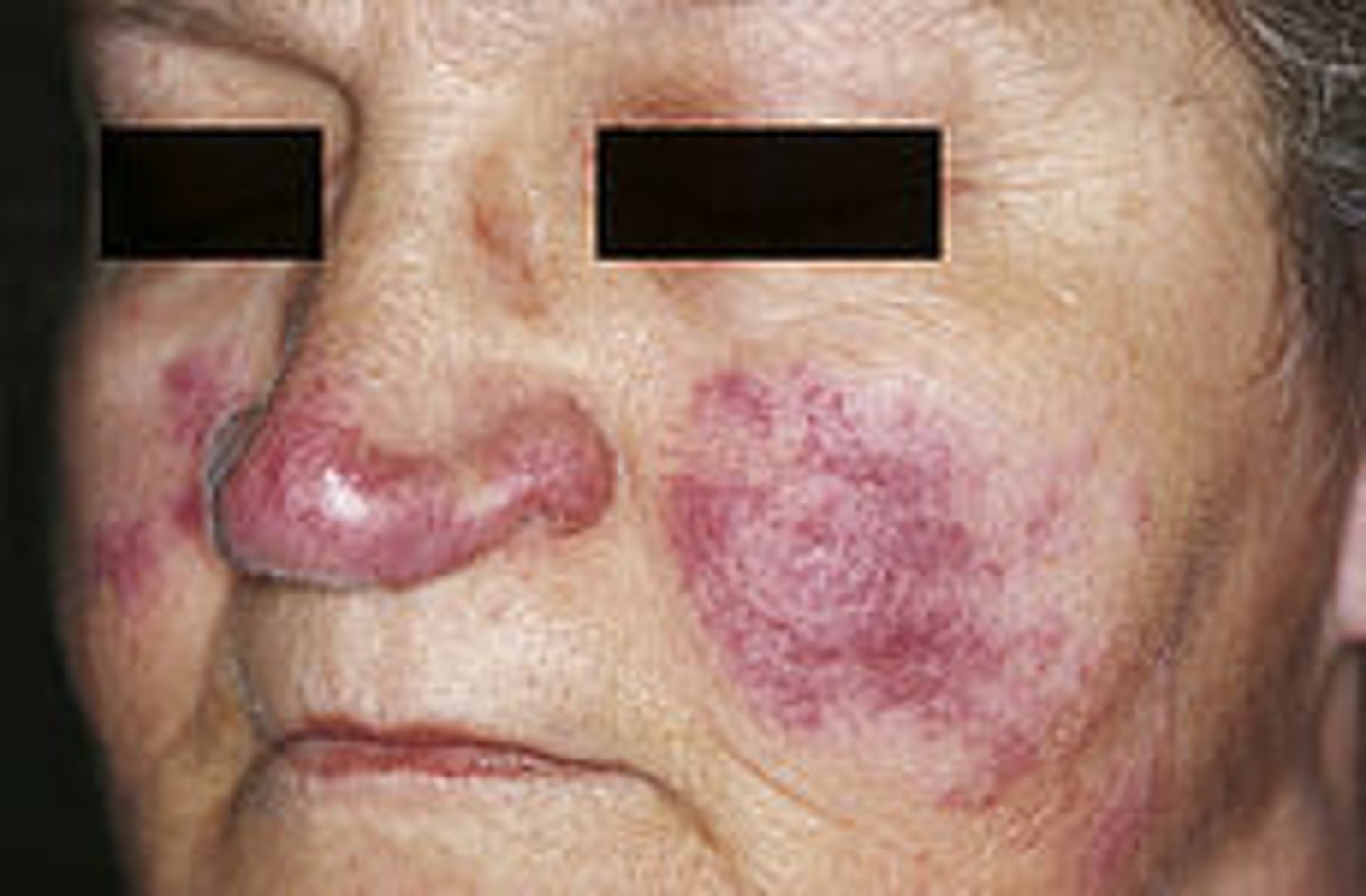
what auto-immune salivary gland lesion is caused by the improper degradation of unknown antigenic material?
sarcoidosis
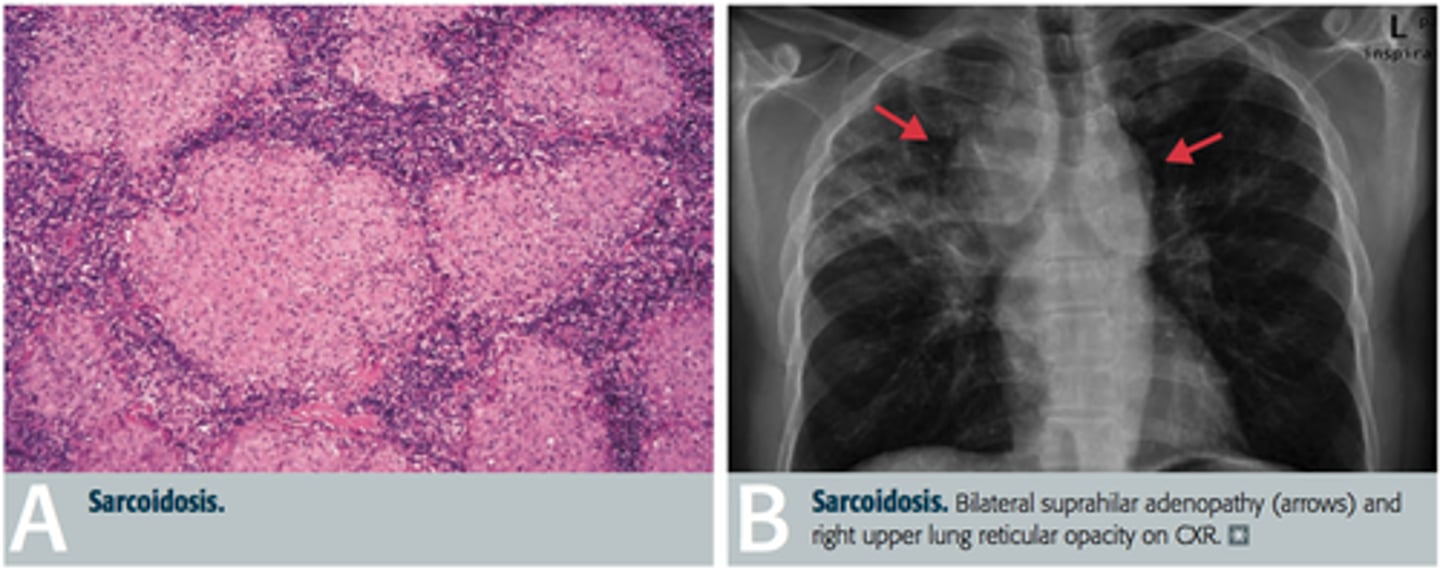
what auto-immune salivary gland lesion forms a noncaseating granulomatous inflammation in various organs of the body and is 10-17 times more common in African Americans?
sarcoidosis
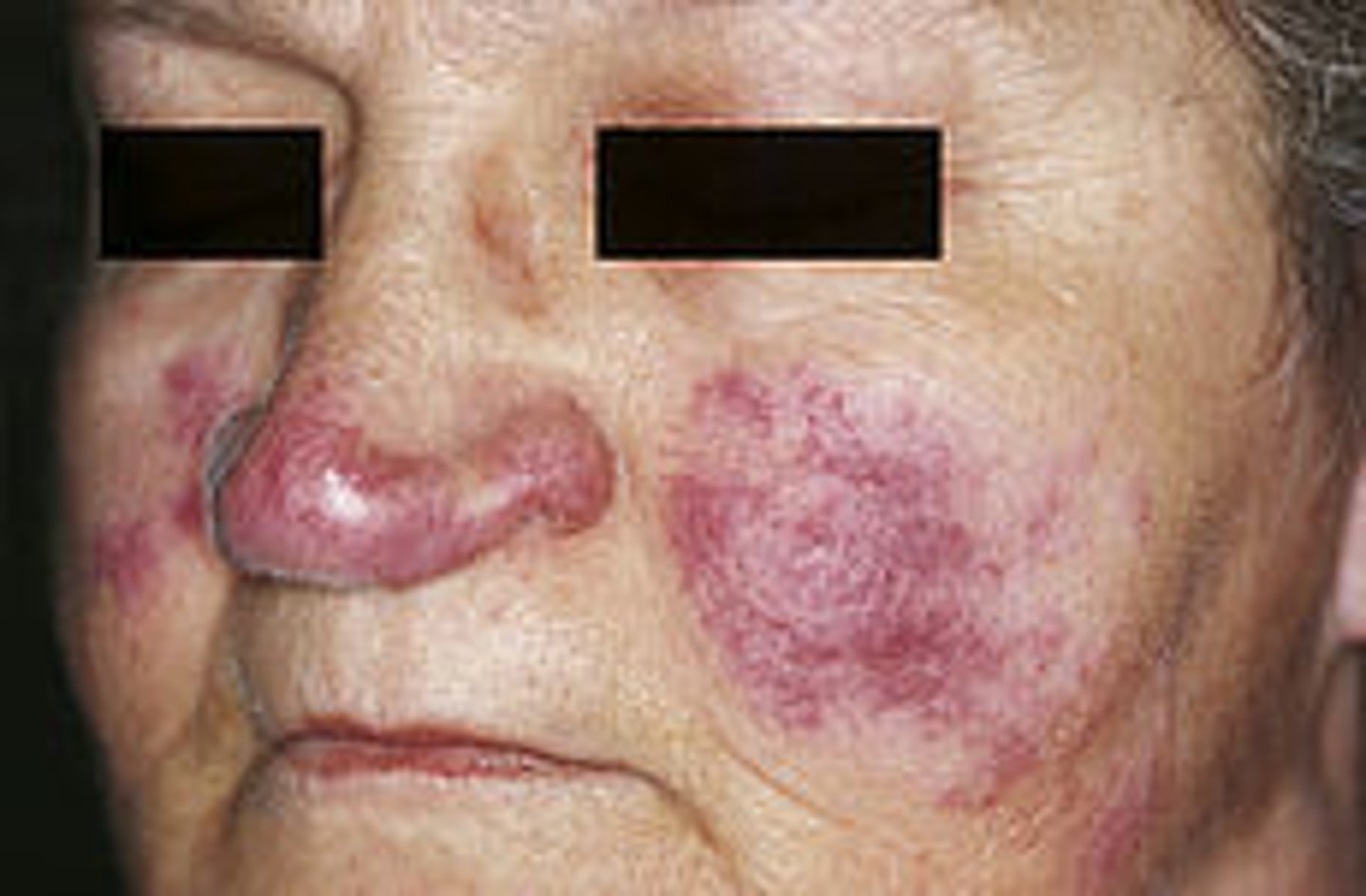
what auto-immune salivary gland lesion is associated with lupus pernio (violaceuous, indurated lesions frequent in the nose, ears, lips and face)?
sarcoidosis
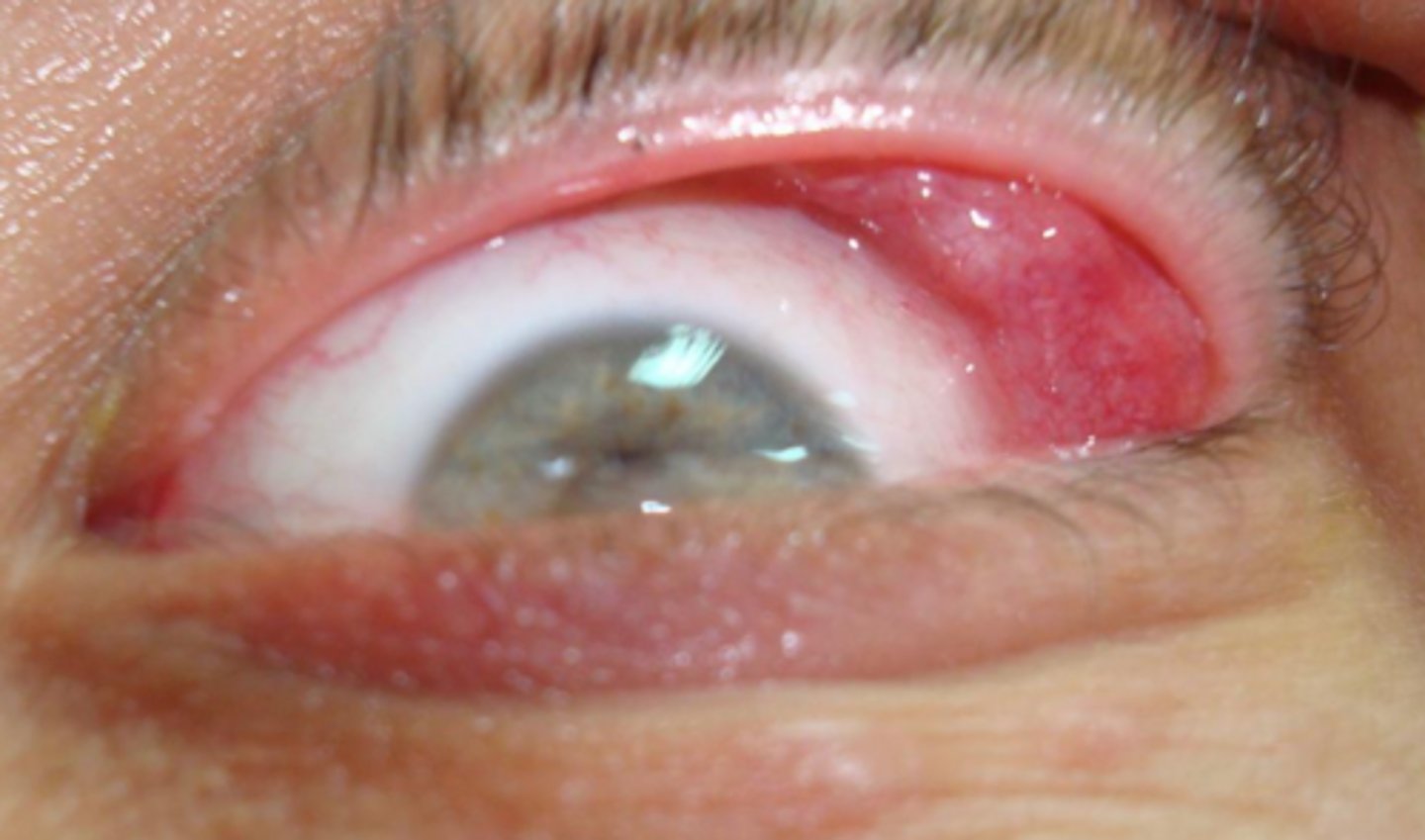
what auto-immune salivary gland lesion sometimes involves the lacrimal glands leading to xerophthalmia?
sarcoidosis
what auto-immune salivary gland lesion can cause salivary gland enlargement and leads to xerostomia (mimicking Sjogren syndrome)?
sarcoidosis
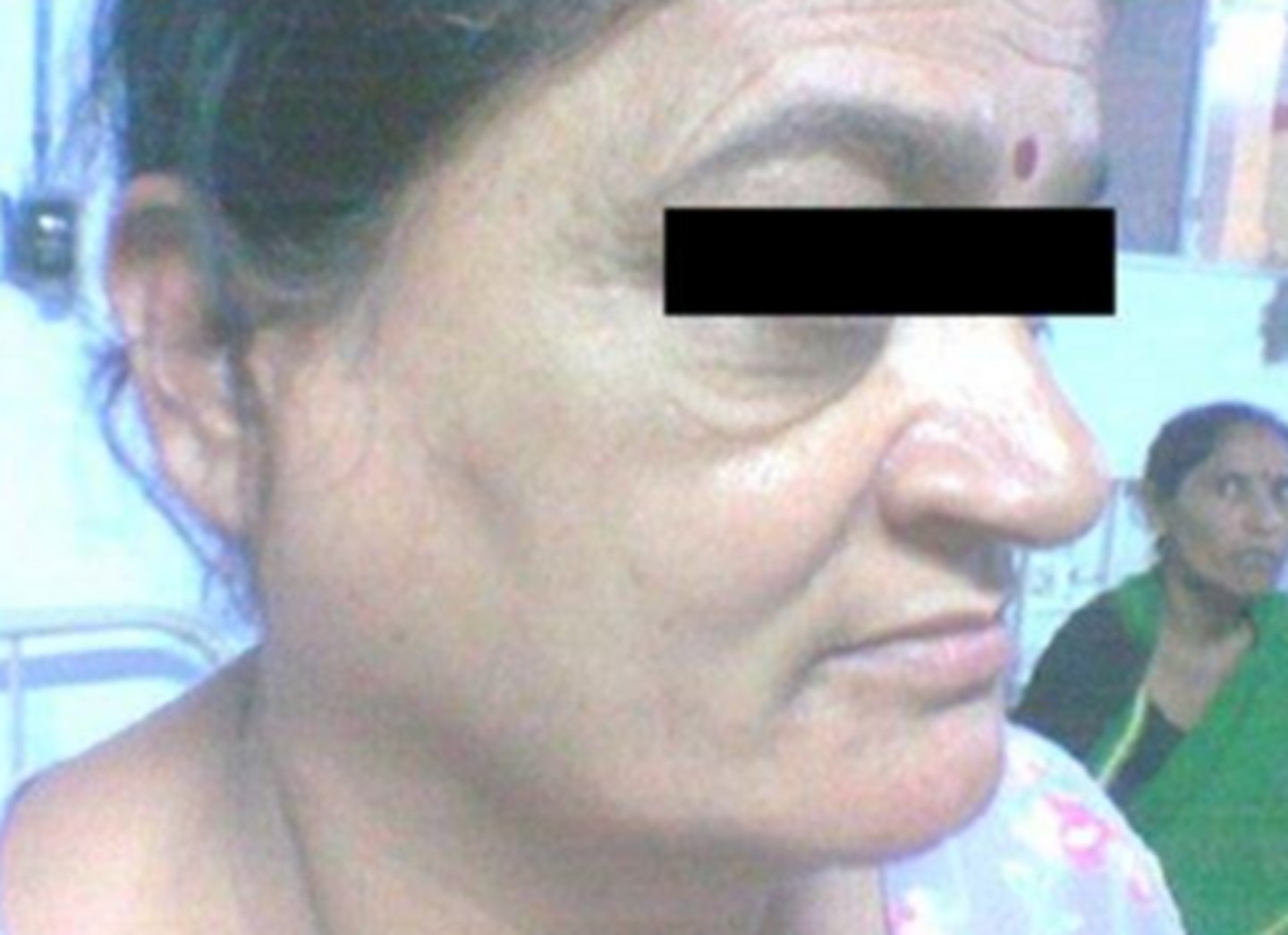
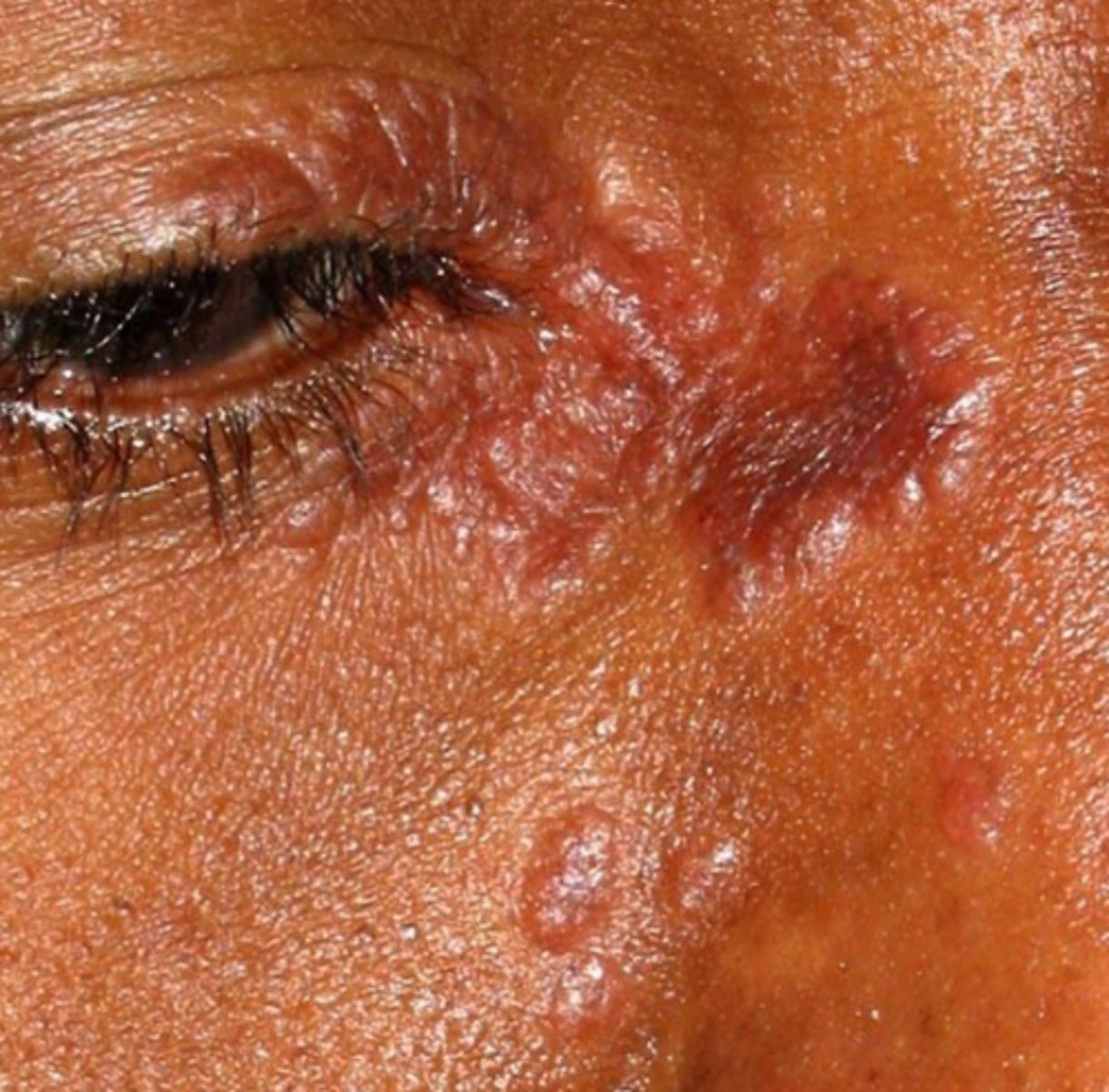
what auto-immune salivary gland lesion has oral manifestations (other than salivary gland involvement) like masses, papules, and ulcerations?
sarcoidosis
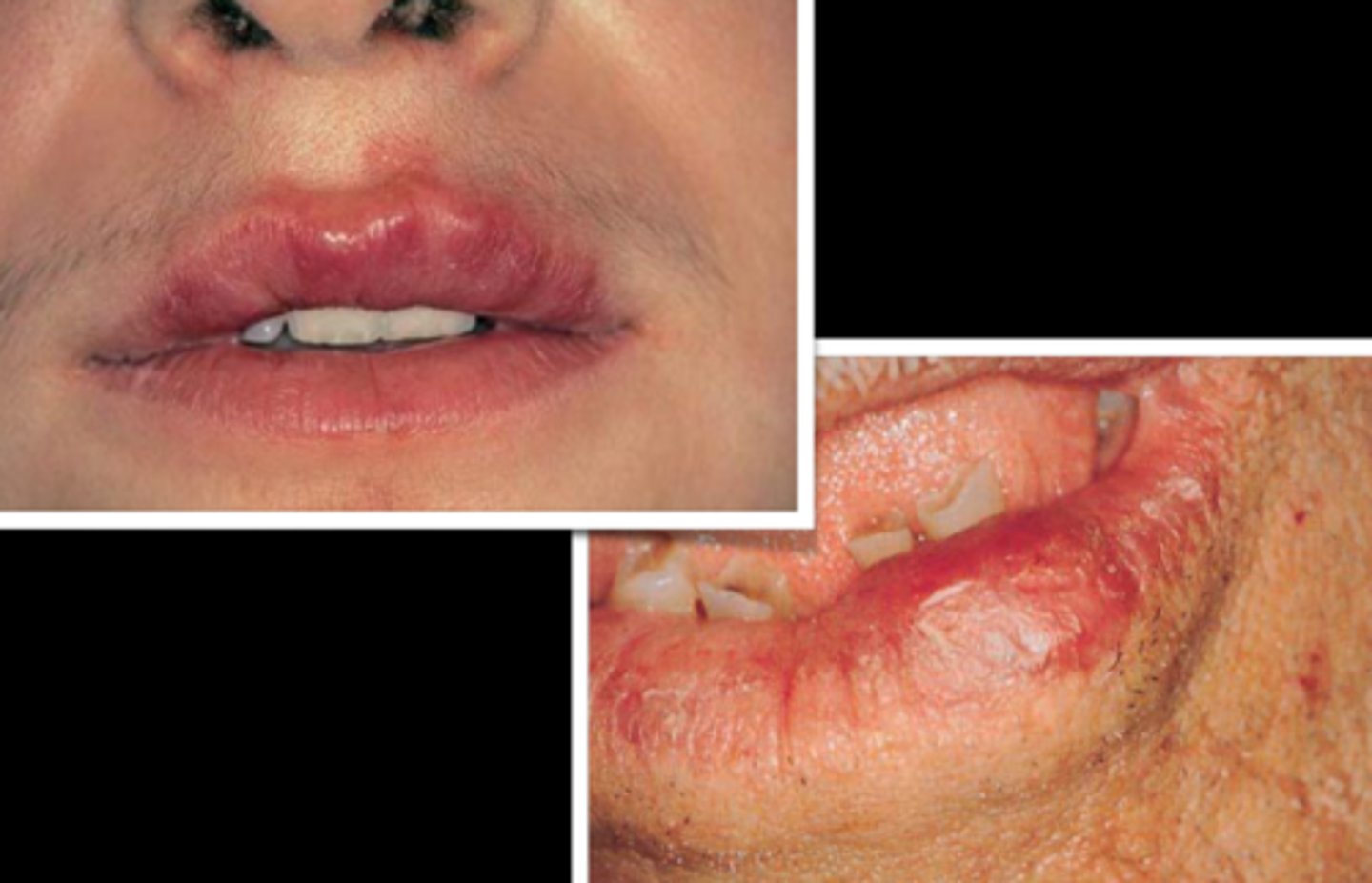
what auto-immune salivary gland lesion forms lesions that may be brown-red, violaceous (violet), or hyperkeratotic in the oral cavity?
sarcoidosis
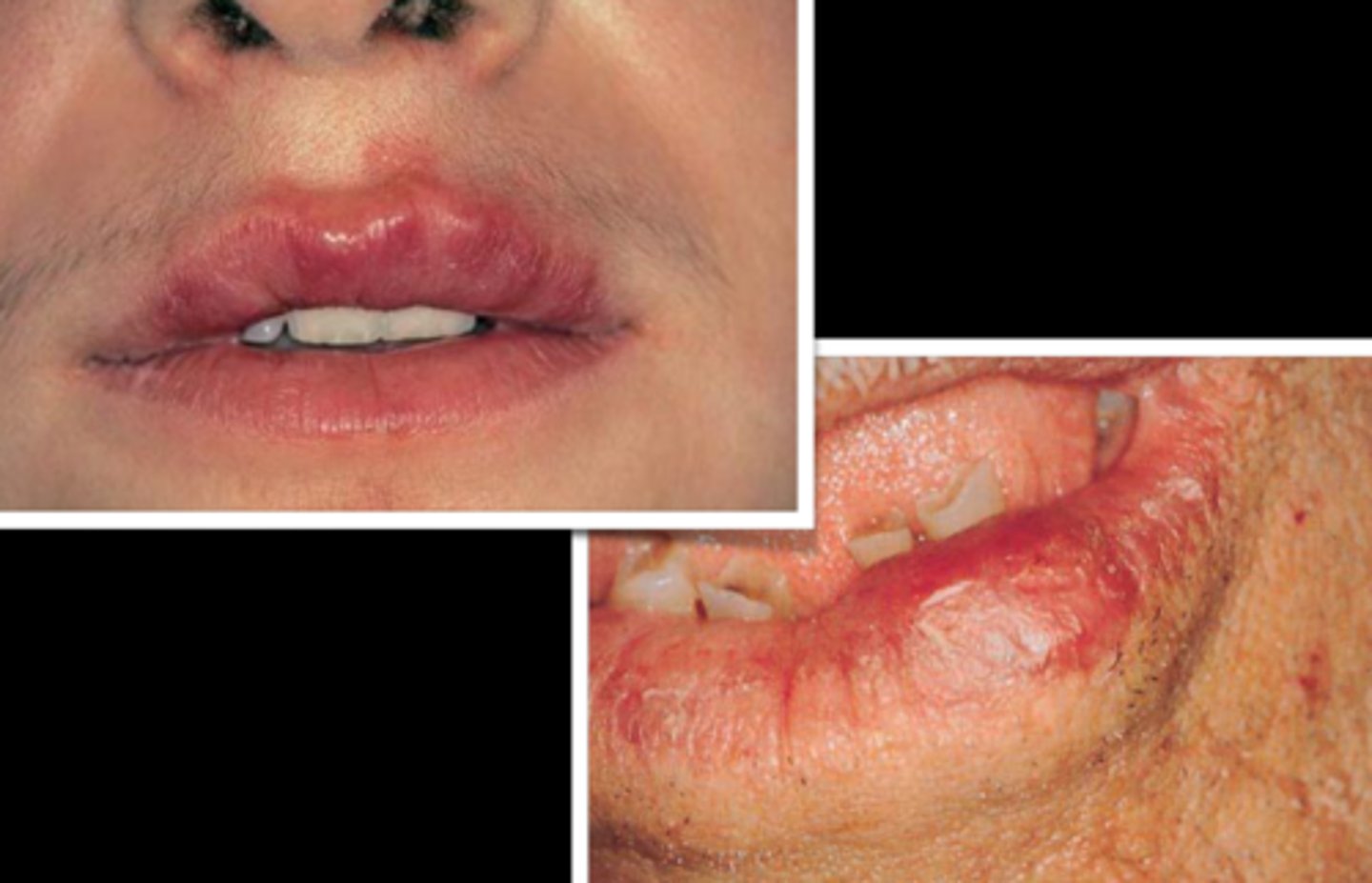
what auto-immune salivary gland lesion is diagnosed via negative findings for special stains and microorganisms, elevated ACE levels, and treated with corticosteroids?
sarcoidosis
what auto-immune salivary gland lesion is caused by antibodies to the salivary glands and other exocrine glands resulting in inflammation initially then destruction of the salivary glands?
Sjogren syndrome
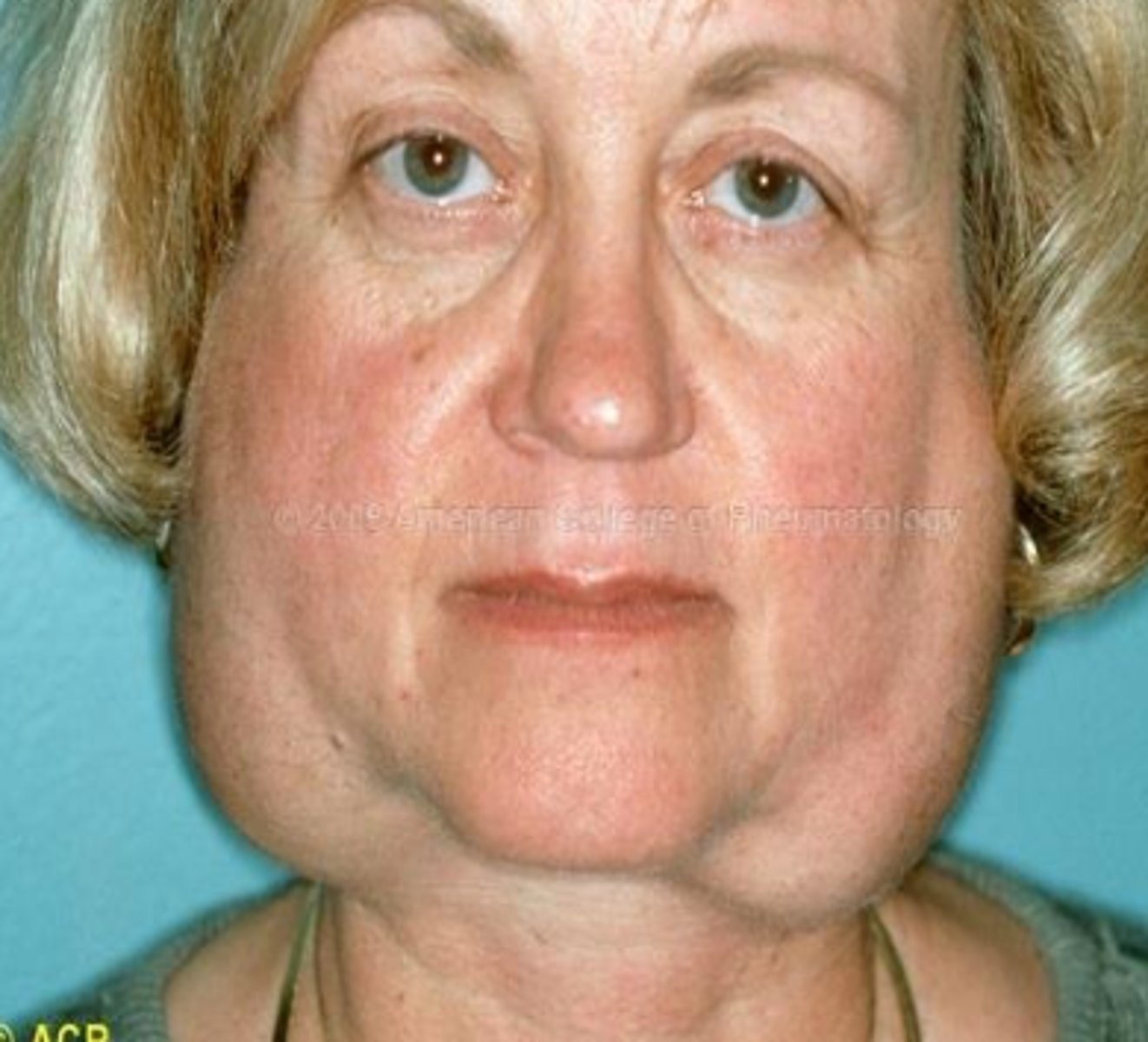
what auto-immune salivary gland lesion causes xerostomia (pain, burning, erythema) and xerophthalmia (burning and itching of eyes, blurred vision, thick secretion)?
Sjogren syndrome; for diagnosis of this syndrome, you must have both xerostomia and xerophthalmia
(primary/secondary) Sjogren syndrome is also known as sicca syndrome
primary
(primary/secondary) Sjogren syndrome involves xerostomia and xerophthalmia
primary
(primary/secondary) Sjogren syndrome involves sicca syndrome and an autoimmune disease (rheumatoid arthritis and lupus)
secondary
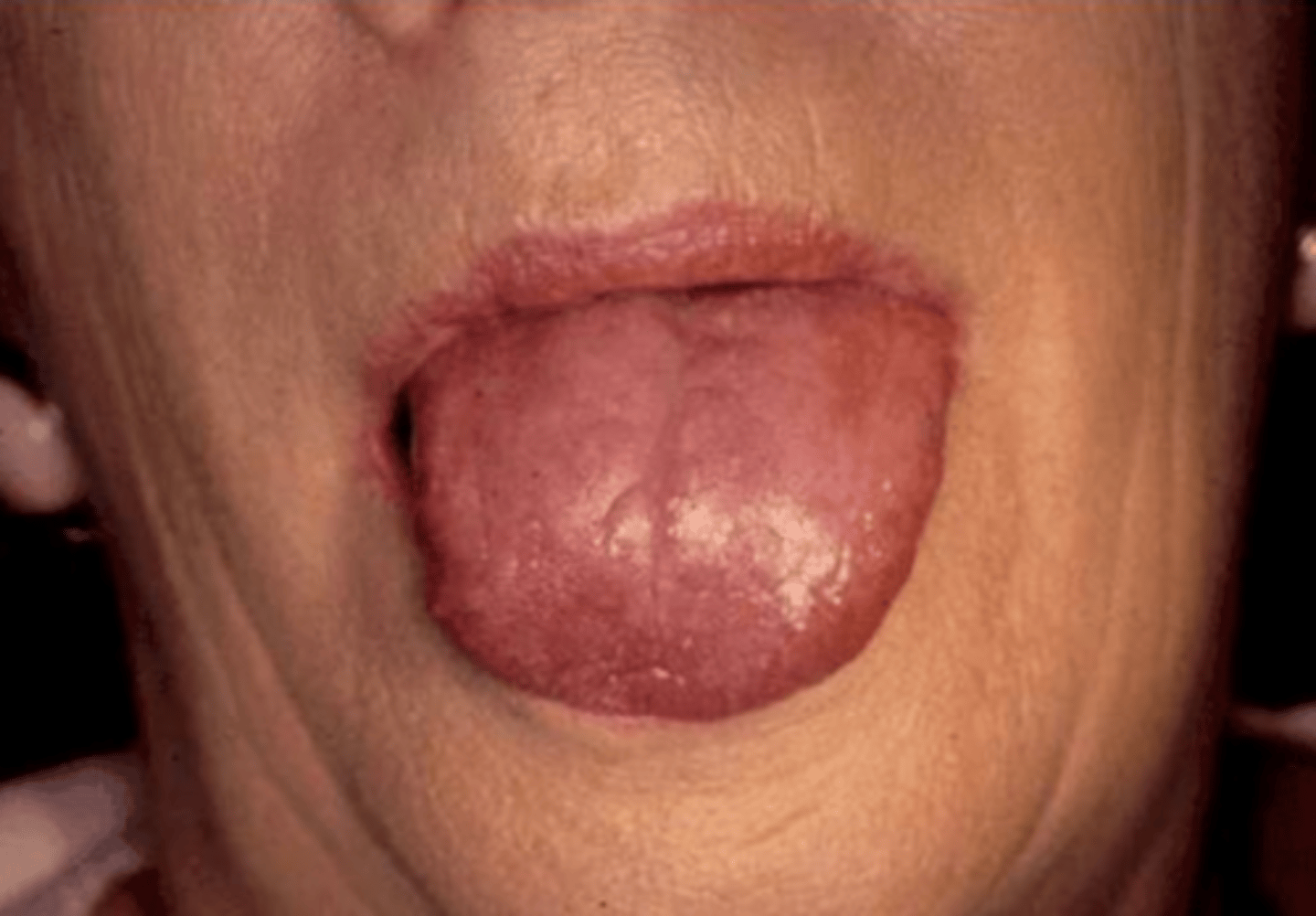
what auto-immune salivary gland lesion often results in the tongue becoming fissured and exhibits atrophy of the papillae?
Sjogren syndrome
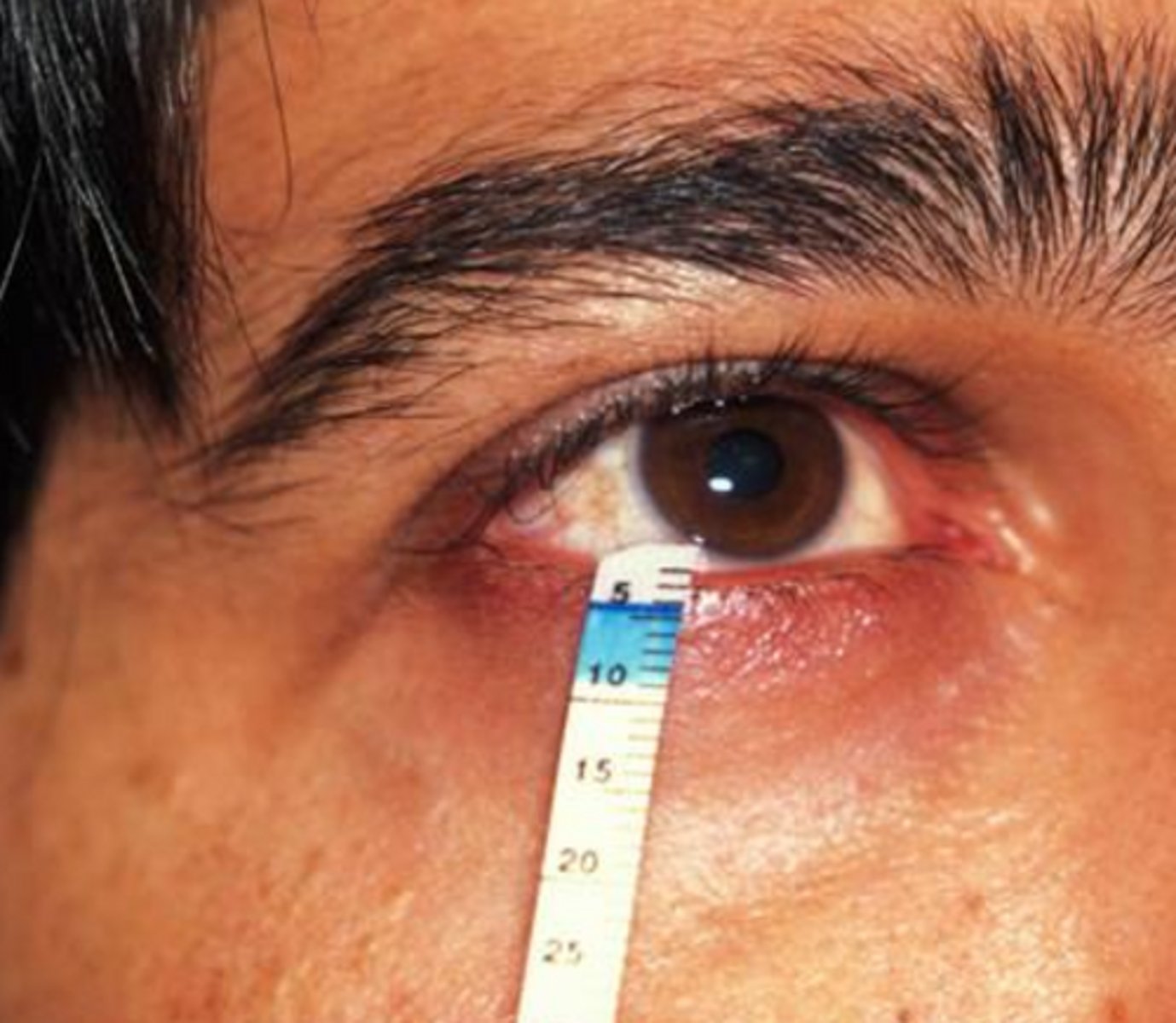
what auto-immune salivary gland lesion involves using the Schrimer test to confirm decreased tear secretion?
Sjogren syndrome
what auto-immune salivary gland lesion is caused by the lymphocytic infiltration of the salivary glands with the destruction of the acinar units?
Sjogren syndrome
what auto-immune salivary gland lesion results in laboratory abnormalities like antinuclear antibodies in the blood?
Sjogren syndrome
what auto-immune salivary gland lesion requires supportive treatment (artificial tears and saliva) and causes an increased risk of dental caries and secondary candidiasis?
Sjogren syndrome
(t/f) Sjogren syndrome is a chronic disease that is not life-threatening and has no association with malignancies
false; Sjogren syndrome is a chronic disease that is not life-threatening, but patients show a 40 times risk of developing lymphomas
what salivary gland lesion is a non-inflammatory disorder characterized by salivary gland enlargement associated with an underlying systemic problem (diabetes, malnutrition, alcoholism, bulimia)?
sialadenosis
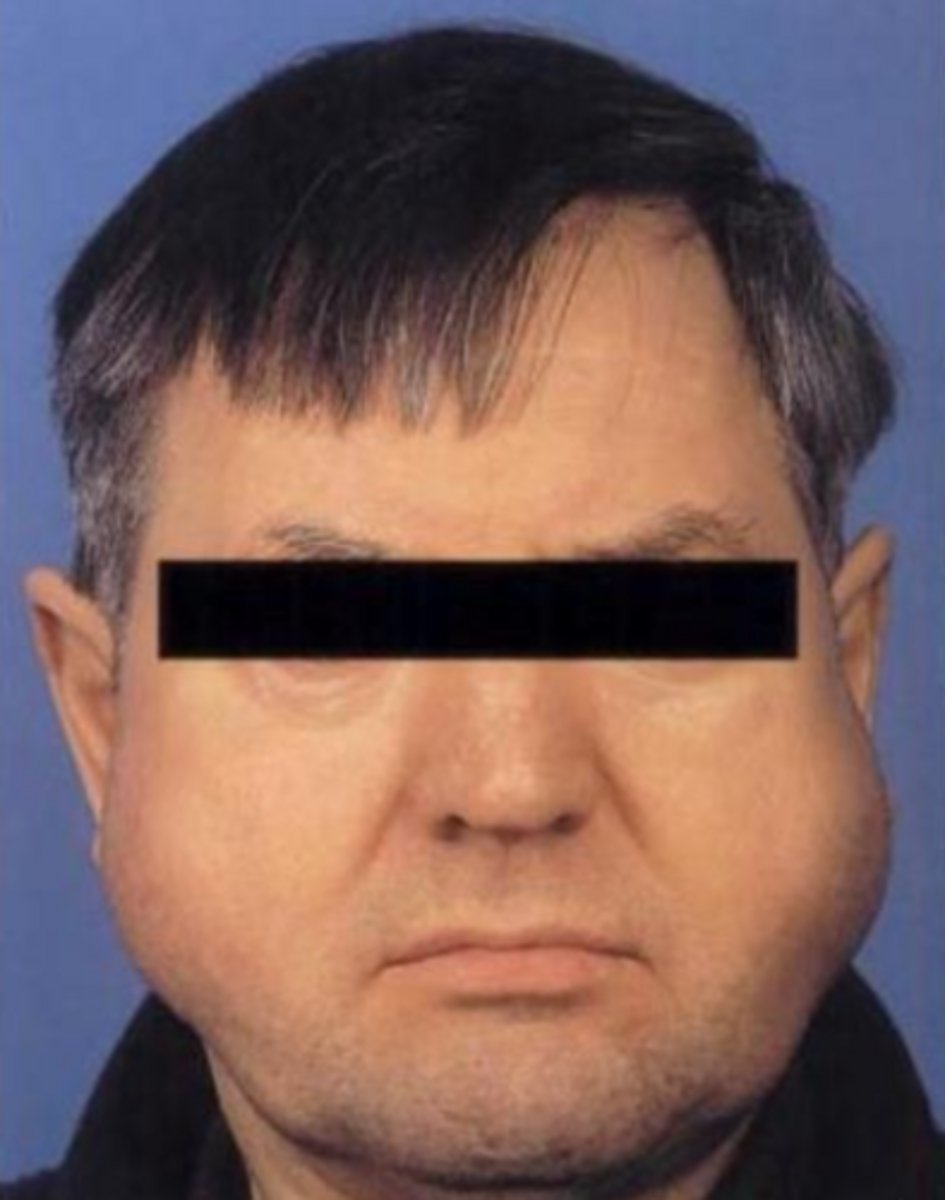
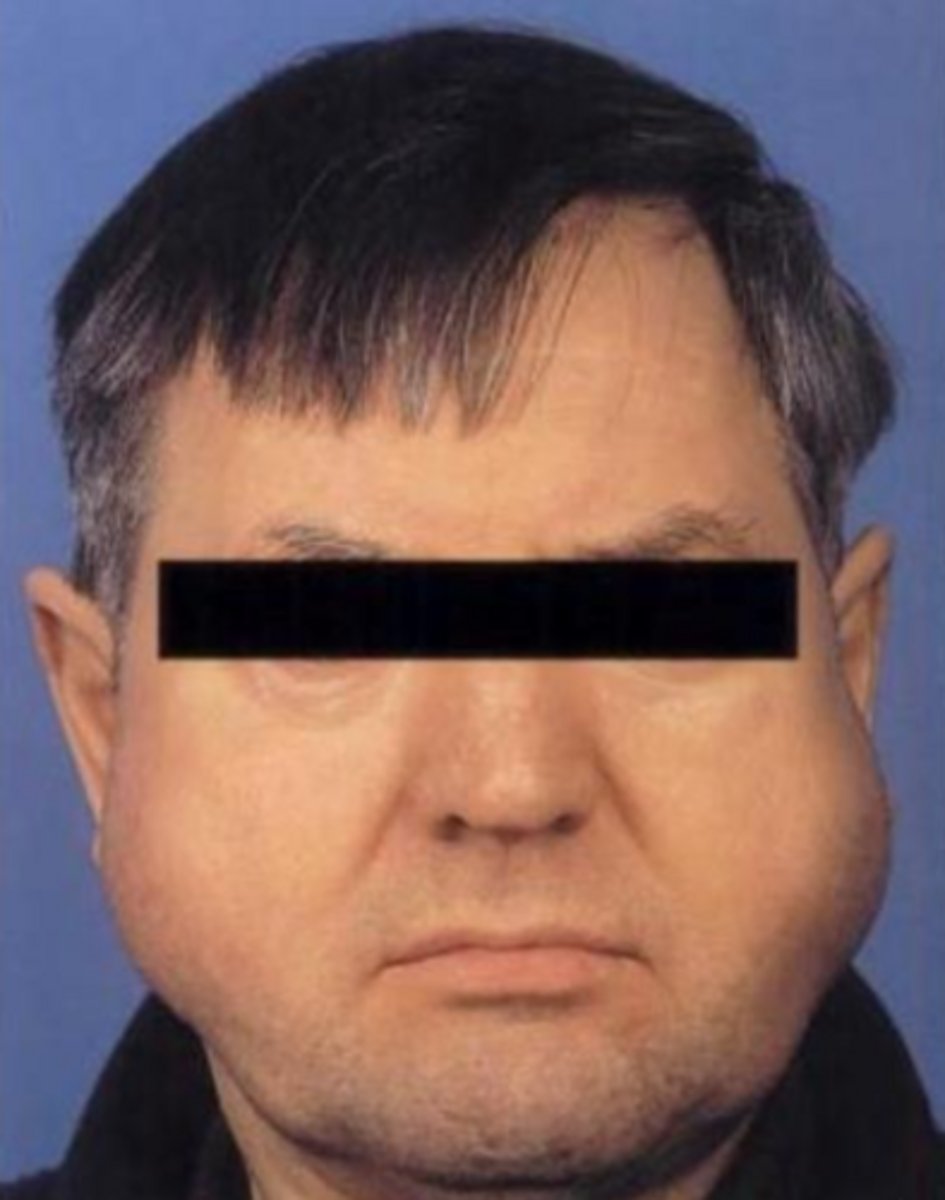
what salivary gland lesion is a slowly evolving bilateral swelling of the parotid glands from the hypertrophy of the acinar cells and managed closely relating an underlying condition?
sialadenosis
what term refers to the subjective sensation of a dry mouth most likely resulting from medication use?
xerostomia
what condition refers to foamy, thick, and ropey saliva, a dry mucosa, a fissured tongue with atrophy of the papillae, and increased prevalence of candidiasis and decay?
xerostomia
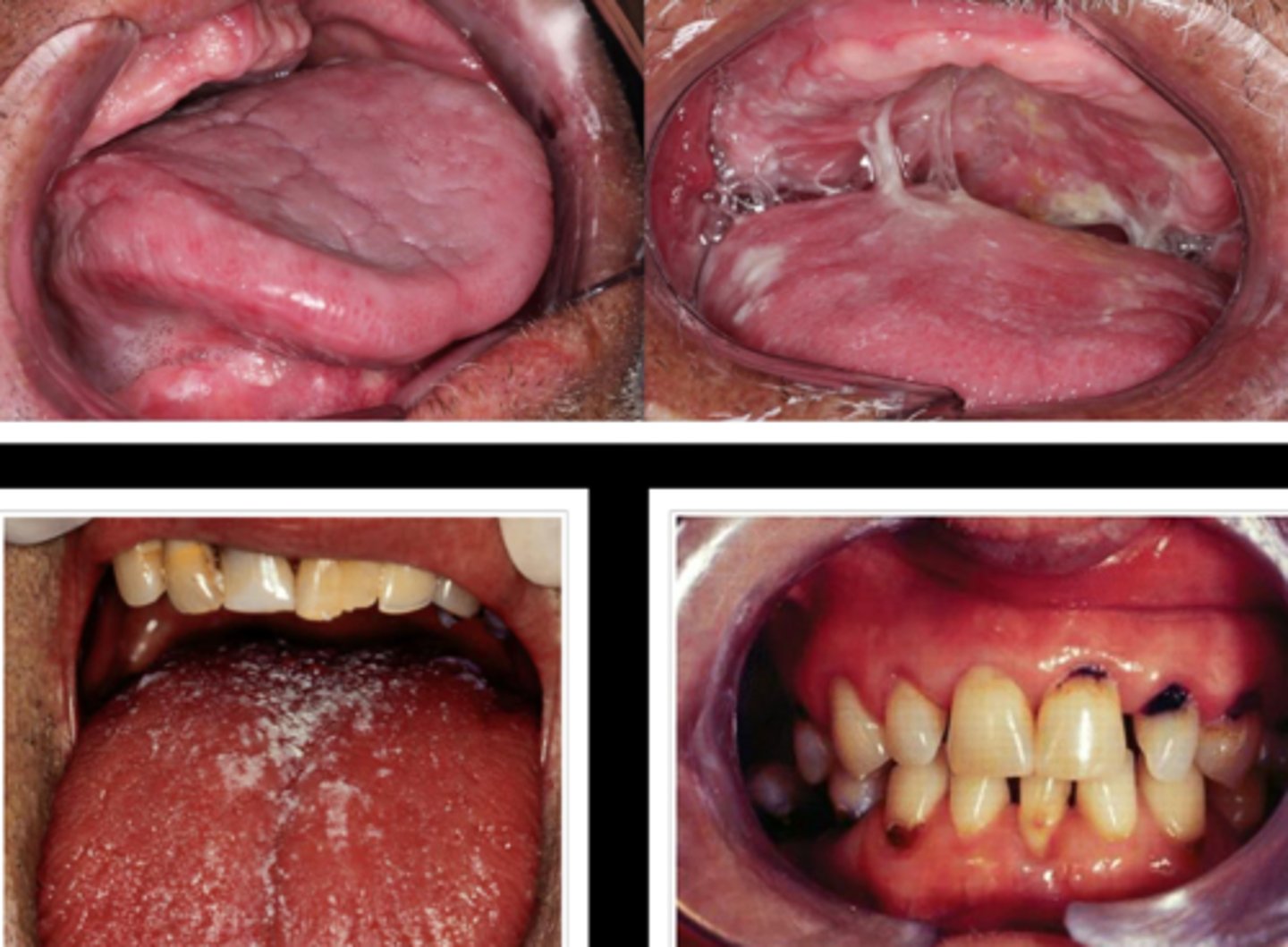
what medication is typically used to promote salivary secretion in xerostomia?
pilocarpine
what term refers to the excessive salivation that has various causes (aphthous ulcers, ill-fitting dentures, GERD, heavy metal poisoning)?
sialorrhea
(t/f) xerostomia is caused by medications used to treat Alzheimer's and myasthenia gravis
false; sialorrhea is caused by medications used to treat Alzheimer's and myasthenia gravis
what condition refers to the production of drool resulting in choking and seen in children with cerebral palsy forming sores around the mouth, chin, and neck that can become infected?
sialorrhea
(t/f) sialorrhea can be transient and require no treatment, but if persistent, requires therapeutic intervention like speech therapy, anticholinergic medication (may cause unwanted side effects), and surgery
true