peptic ulcer drugs
1/69
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
70 Terms
what does food ingestion stimulate?
peptic cells → release pepsinogen
cholinergic neurons → release ACh
pepsinogen is produced by…
peptic cells
ACh from the cholinergic neurons activate ______ receptors
endocrine receptors
muscarinic stomach receptors
endocrine cells release….
a) pepsinogen
b) histamine
c) ACh
d) HCl
b) histamine
endocrine cells are stimulated by….
a) pepsinogen
b) histamine
c) ACh
d) HCl
c) ACh
where are H2 receptors located?
surface of parietal cells
what manufactures protons/HCl?
parietal cells
how are the synthesized protons (HCl) pumped out of the parietal cells into stomach lumen?
K+/ H+ / ATPase pump
the biological system protects the stomach walls from being digested by pepsin or corroded by the concentrated HCl by lining the stomach walls with ______
mucin
muco-polysaccharide polymer
mucin production and secretion are stimulated by _______
prostaglandins
T/F: There is no treatment for the ulcer
true
only help stop ulcer deterioration by HCl/pepsin
what helps convert pepsinogen → pepsin
HCl (makes pH = 2) which activates pepsinogen → pepsin
antacids MOA
neutralizing HCl in stomach activation of pepsinogen
what do you get when you combine HCL + NaHCO3
NaCl + H2CO3
H2CO3 → CO2 + H2O
SATA: which of the following antacids causes acid rebound?
a) sodium bicarbonate
b) calcium carbonate
c) magnesium hydroxide
d) aluminum hydroxide
a) sodium bicarbonate
b) calcium carbonate
why do some antacids cause acid rebound?
rapid effects of neutralizing HCl
release of CO2 → stomach wall → increases HCl release
how does sodium bicarbonate (or all antacids) affect basic/acidic drugs?
basic = more unionized = more reabsorbed
acidic = more ionized = more water-soluble = more excretion
which of the following antacids causes diarrhea?
a) sodium bicarbonate
b) calcium carbonate
c) magnesium hydroxide
d) aluminum hydroxide
c) magnesium hydroxide
which of the following antacids causes constipation?
a) sodium bicarbonate
b) calcium carbonate
c) magnesium hydroxide
d) aluminum hydroxide
d) aluminum hydroxide
what the benefit of mixing magnesium hydroxide and aluminum hydroxide together?
reduced constipation or diarrhea (not 100%)
T/F: NaHCO3 (Sodium bicarbonate) is water soluble and gets into circulation faster than other
true
antacids with Mg or Al ions may be detrimental for _______ function after absorption from the stomach into circulation
kidney
which of the following antacids does NOT appear as a white suspension (insoluble)?
a) sodium bicarbonate
b) calcium carbonate
c) magnesium hydroxide
d) aluminum hydroxide
a) sodium bicarbonate
what is Mylanta or Maalox
combination of AlOH and MgOH to offset each others effects
what do the anti-muscarinic agents target?
muscarinic cholinergic receptors on the endocrine cells → inhibits histamine production
what type of agent is dicyclomine
anti-muscarinic agent
T/F: Dicyclomine is used as monotherapy
false
used as adjunct therapy
can NOT be used by itself
what is the major problem with dicyclomine
needs high concentrations to be effective → causes major ADE
what is the target/MOA with H-2 antagonists
block H-2 receptors on the parietal cells = decreases HCl production
what are the 3 major components linked together in all H2 blockers?
5-membered heterocyclic ring w/ basic nitrogen
CH2-SH-CH2-CH2
guanido or amidino group with electron withdrawing group
what are the 3 electron withdrawing groups attached to guanido or the amidino group in H2 blockers? rank them by strongest → weakest
sulfonamide (SO2NH2; strongest)
nitric oxide (NO2)
cyano (CN)
what is the purpose of the electron withdrawing groups attached to the guanido or amidino group in H2 blockers?
decreases basicity
stronger electron withdrawing group = higher potency
what type of drug is Cimetidine?
H2 blocker
what type of drug is Famotidine?
H2 blocker
what type of drug is Ranitidine?
H2 blocker
what type of drug is Nizatidine?
H2 blocker
which of the following H2 blockers requires the largest dose (Least potent)?
a) famotidine
b) ranitidine
c) cimetidine
d) nizatidine
c) cimetidine
why does cimetidine have a large dose?
CN (Weak electron withdrawing group)
which of the following H2 blockers requires the smallest dose (most potent)?
a) famotidine
b) ranitidine
c) cimetidine
d) nizatidine
a) famotidine
which of the following H2 blockers is a very strong CYP inhibitor?
a) famotidine
b) ranitidine
c) cimetidine
d) nizatidine
a) famotidine
how are H2 blockers administered?
orally or injection (HCl salt)
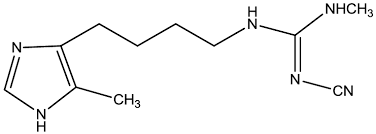
what type of drug is this?
H2 blocker
cimetidine
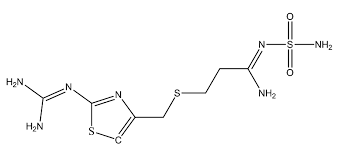
what type of drug is this?
H2 blocker
famotidine
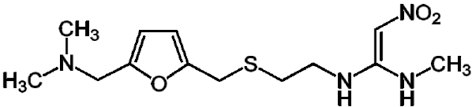
what type of drug is this?
H2 blocker
ranitidine
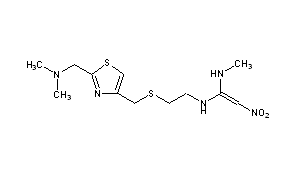
what type of drug is this?
H2 blocker
nizatidine
which of the following H2 blockers has a CN group?
a) famotidine
b) ranitidine
c) cimetidine
d) nizatidine
c) cimetidine
which of the following H2 blockers has a sulfonamide group?
a) famotidine
b) ranitidine
c) cimetidine
d) nizatidine
a) famotidine
why is FDA recalling H2 blockers? which H2 blocker was recalled first?
detection of unacceptable levels of NDMA
ranitidine = first
proton pump inhibitor target/MOA
inhibitors for K+ / H+ / ATPase pump
(parietal cells = site of action)
what is the most powerful class in decreasing HCl in stomach?
PPI (proton pump inhibitor)
PPI additional indication
Allison Zollinger Syndrome
parietal cell cancer
ALL PPIs are _____
prodrugs
naturally activated by low pH
what is the backbone for PPIs?
benzimidazole ring
sulfoxide at position 2
methylene group
pyridine at position 2
T/F: the PPIs have different potencies based on their substituents
false
all PPIs have same potency
substituents do NOT affect potency
how are PPIs activated?
become an intermediate with sulfhydryl//mercapto group (SH) → reacts covalently with an SH group on enzyme structure → S-S bond to inactivate enzyme
cyclization → decomposition
all PPI react ______ with the enzyme
covalently
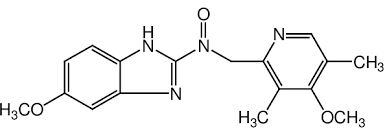
what type of drug is this?
PPI
omeprazole
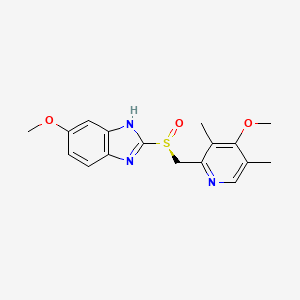
what type of drug is this?
PPI
esomeprazole
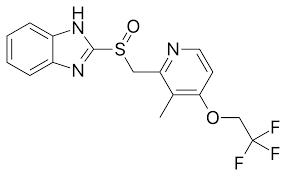
what type of drug is this?
PPI
lansoprazole
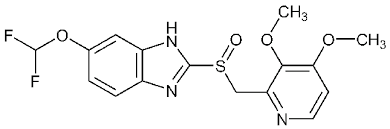
what type of drug is this?
PPI
pantoprazole
what is the purpose of adding a methoxy to PPI?
help w/ metabolism
O-demethylation
what is the purpose of cytoprotective agents?
to protect the ulcerated area of stomach wall from the corrosive HCl and/or digestive effects of pepsin
Misoprostol MOA
inducing mucin secretion + inhibits HCl secretion
PGE1 derivative
Sucralfate MOA
forms protective gel on the ulcerated area
Misoprostol CI
pregnancy
can cause uterine contraction / abortion
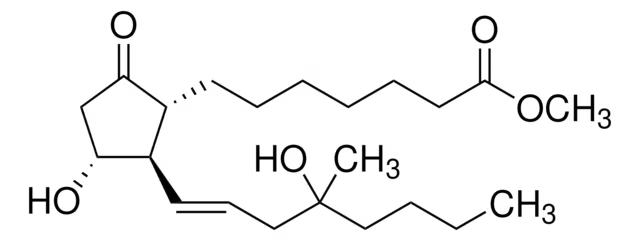
what type of drug is this?
cytoprotective agent
misoprostol
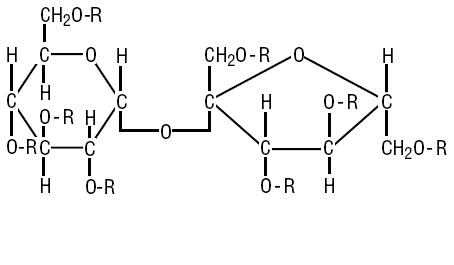
what type of drug is this?
cytoprotective agent
sucralfate
sucralfate administration
oral tablets used one hour before meal
what are the dual properties of sucralfate
non-absorbable (works locally in stomach)
Al salt → forms gel
in sucralfate, all hydroxyl groups of the sugar are making ______ with one of the sulfuric acid protons
esters