Types II-IV hypersensitivity
1/57
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
58 Terms
what is type 1 hyper sensitivity
involves IgE, usually an immediate response, involves mast cells and histamine release
note: for autoimmune disease there is no type 1
what is type 2 autoimmune hypersensitivity
antibodies attacked our own cells by mistake
-IgG
what is type 3 autoimmune hypersensitivity
soluble immune complexes deposit in and clog tissues
-ex: rheumatid arthritis
what is type 4 autoimmune hypersensitivity
-cell mediated (effector T cells)
-anything with T cells!
-slower reaction
Ex: chronic transplant rejections
Q: What are autoimmune diseases?
A: Chronic diseases where the immune system attacks the body's own cells
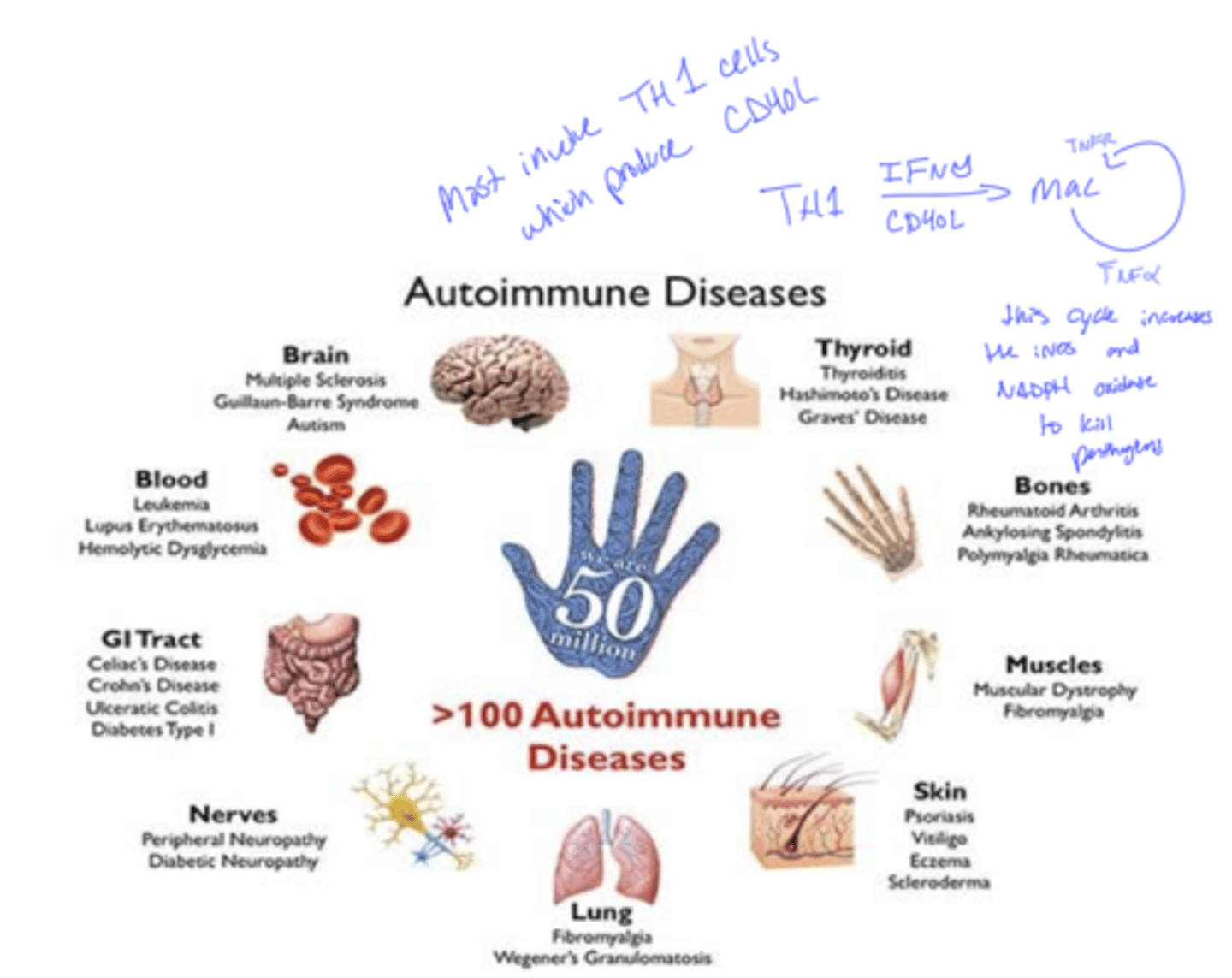
Q: Why can autoimmune diseases persist?
A: The immune system targets antigens that cannot be removed
Q: Which part of the immune system is misdirected in autoimmune diseases?
A: Adaptive immunity (antibodies or T cells attack healthy tissue)
occurs when neg selection doesn't work 100%
Q: How common are autoimmune diseases?
A: About 5% of the human population
Q: What fails in the immune system in autoimmune diseases?
A: Self-tolerance (the ability to avoid attacking the body's own cells)
Q: What antibodies are involved in autoimmune hemolytic anemia?
A: IgG and IgM
Type II: Autoimmune Hemolytic Anemia
Q: What do these antibodies bind to in autoimmune hemolytic anemia?
A: Components on the surface of red blood cells (RBCs)
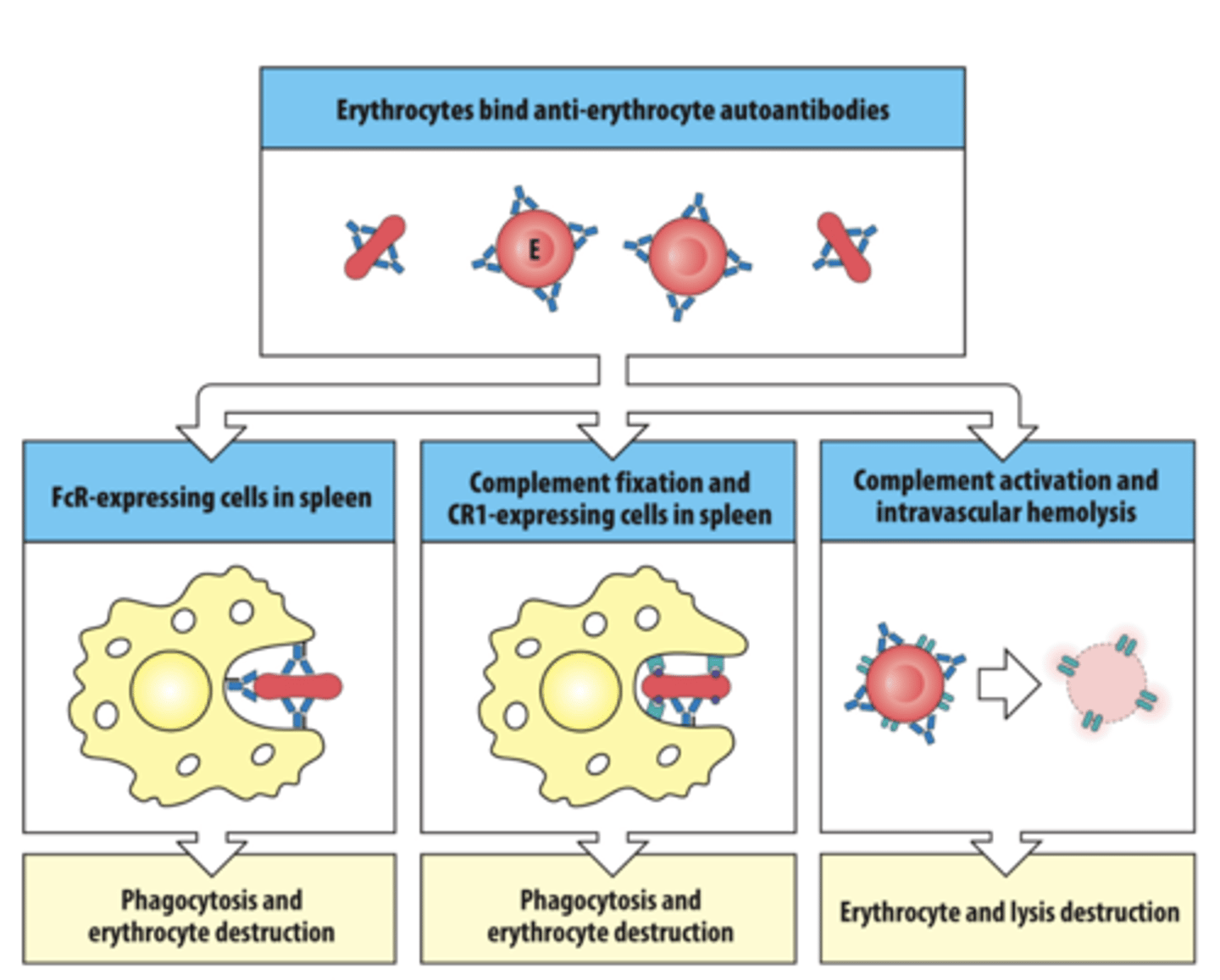
Q: What immune system process causes the RBCs to be destroyed?
A: Activation of complement → membrane attack complex → hemolysis
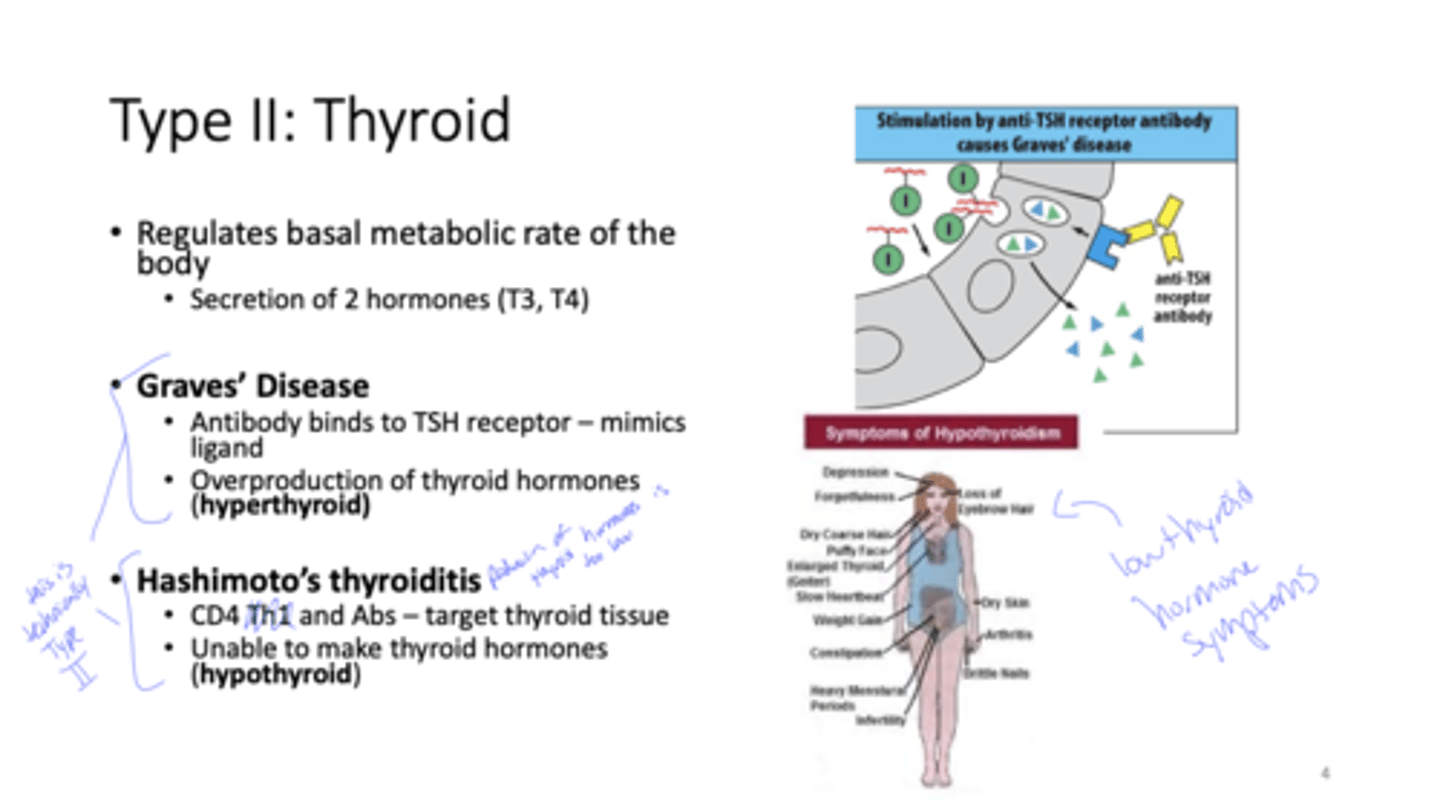
Q: What does the thyroid regulate in the body?
A: Basal metabolic rate
Q: Which two hormones are secreted by the thyroid?
A: T3 (triiodothyronine) and T4 (thyroxine)
Q: In Graves' disease, what do the antibodies target?
A: TSH receptor which mimics ligand. this causes overproduction of thyroid hormones (hyperthyroid)
technically a type 2 autoimmune disease
Q: How do antibodies in Graves' disease affect the thyroid?
A: They mimic TSH and cause overproduction of thyroid hormones (hyperthyroid)
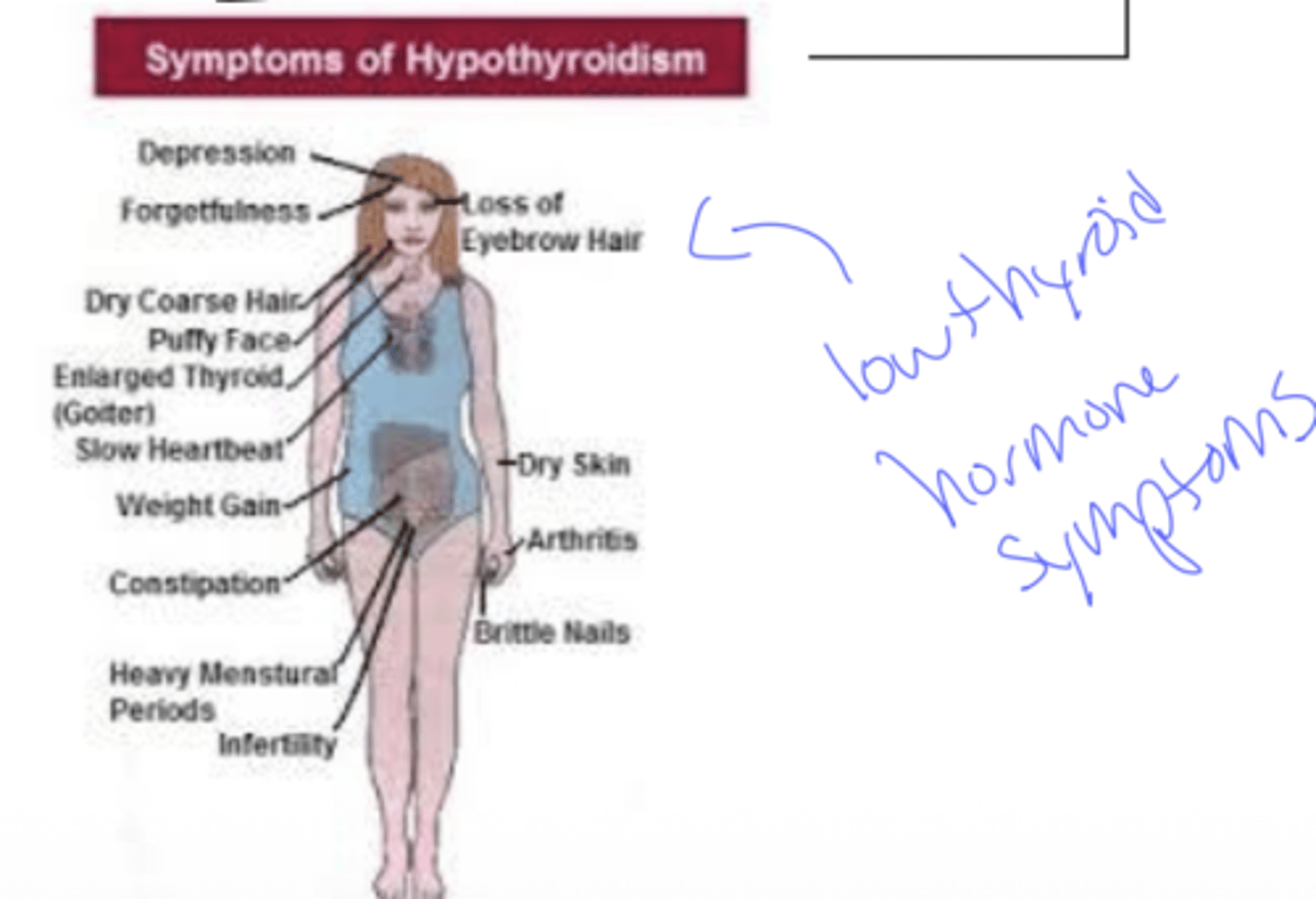
Q: In Hashimoto's thyroiditis, which immune components attack the thyroid?
A: CD4 T cells and antibodies
Q: What is the result of Hashimoto's thyroiditis on thyroid function?
A: Thyroid tissue is destroyed → unable to make thyroid hormones (hypothyroid)
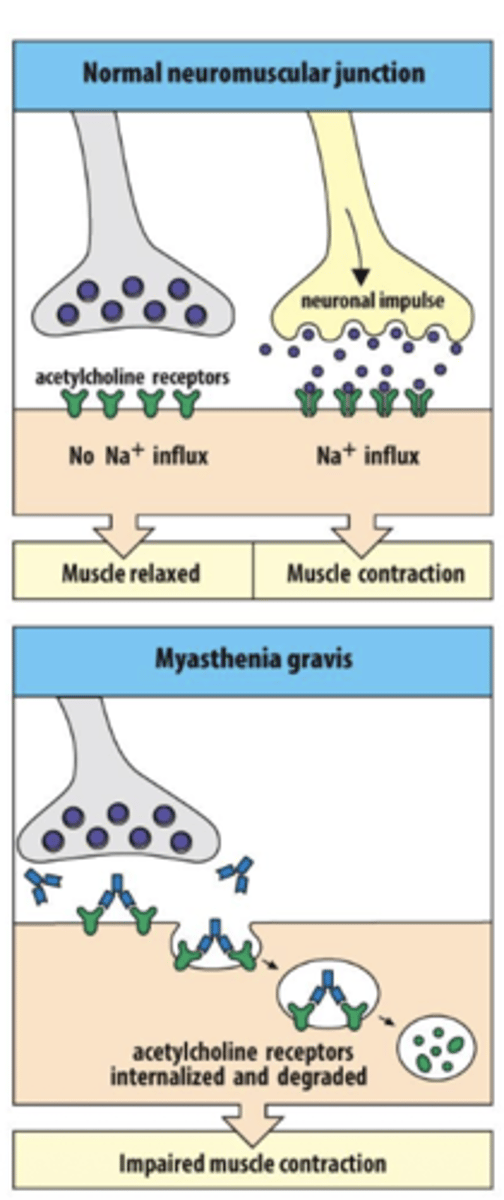
Q: What is mysathenia graves? What are the symptoms and what is it caused by? what type of autoimmune disorder is it?
A: Antibodies bind to acetylcholine receptors
on muscle cells, this will Inhibit signaling from nerve to muscle
progessive muscle weakening will lead to chest muscle weaking ythat impairs breathing
Type II: Myasthenia Gravis which is aggressive weakening of neuromuscular junction
Q: What is one treatment strategy for myasthenia gravis?
A: Prevent degradation of acetylcholine (ACh) by taking immunosupressants
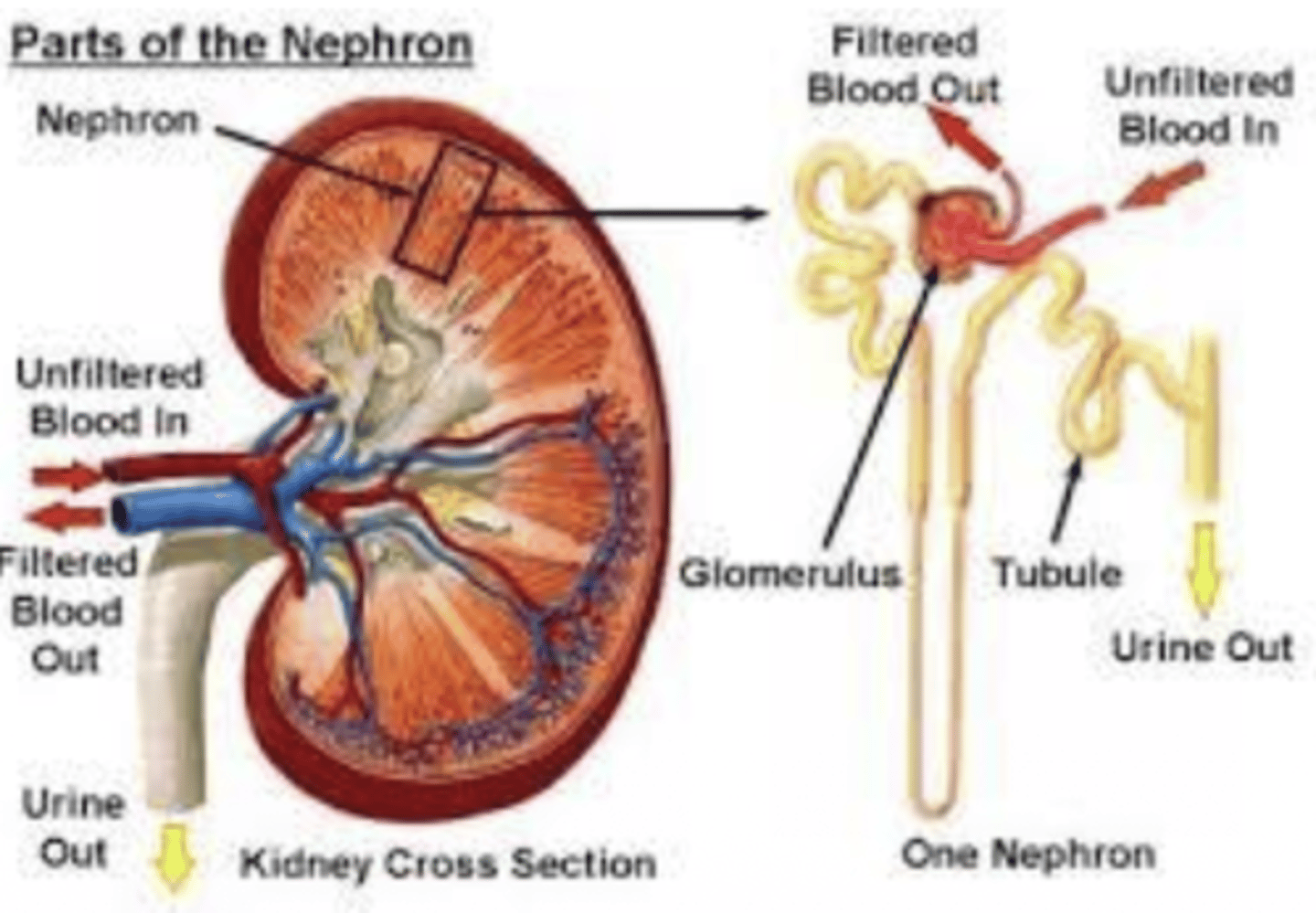
Q: What causes Type III hypersensitivity reactions in Glomerulonephritis
A: Soluble antigen-antibody immune complexes form in the bloodstream.
these protein-protein interactions accumulate in kidneys and cause kidney impairment and failure
Q: What type of hypersensitivity is Systemic Lupus Erythematosus (SLE)?
A: Type III hypersensitivity.
Q: What type of hypersensitivity is Glomerulonephritis)?
A: Type III hypersensitivity.
Q: What is Systemic Lupus Erythematosus (SLE)?
A: An autoimmune disease that can affect almost every cell and tissue in the body.
Q: What antibodies are involved in SLE?
A: IgG antibodies directed against components of the cell surface, cytoplasm, and nucleus.
Q: What specific targets do antibodies attack in SLE?
A: Nucleic acids and nucleoproteins.
Q: How does tissue damage occur in SLE?
A: Cell destruction releases soluble antigens that form immune complexes.
overall effect of lupus is Widespread cell and tissue destruction due to chronic inflammation.
Q: What happens to immune complexes in SLE?
A: They deposit in tissues and organs, triggering inflammation and damage.
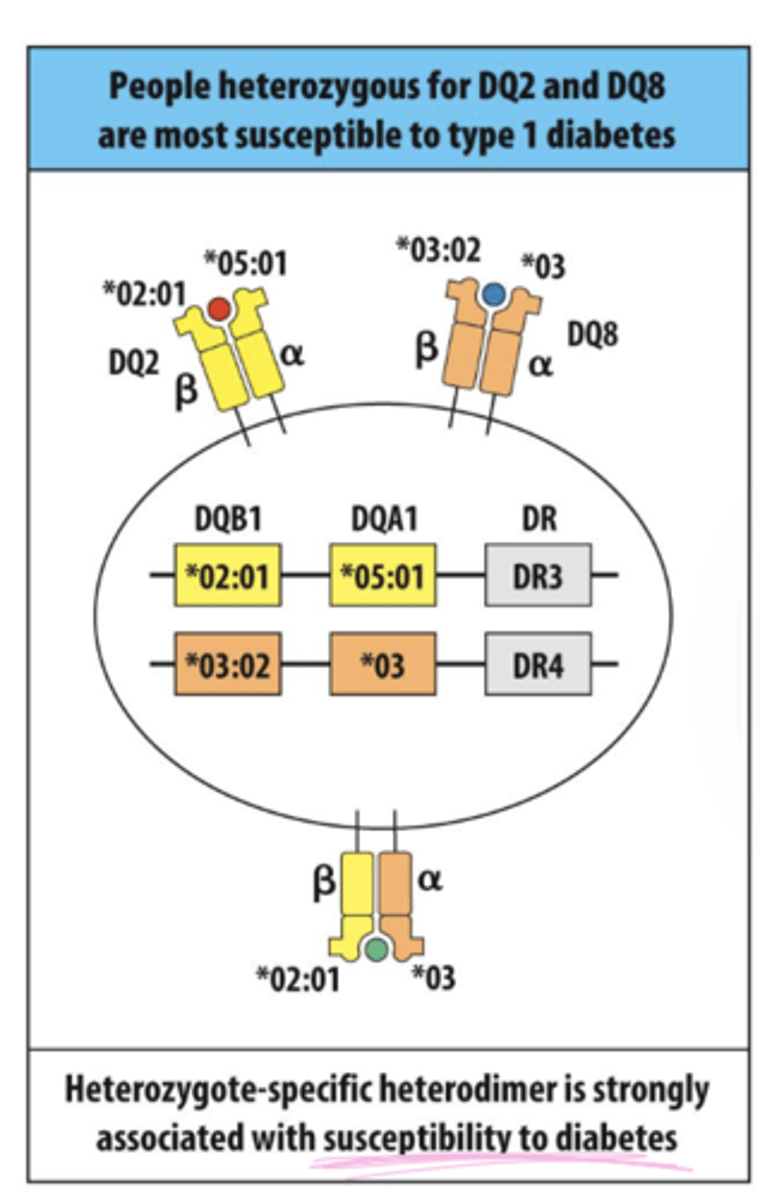
Q: What type of hypersensitivity is Type 1 Diabetes?
A: Type IV (cell-mediated) hypersensitivity., aka Insulin-dependent diabetes mellitus.
Q: What causes Type 1 Diabetes at the cellular level?
A: Immune-mediated destruction of insulin-producing β cells in the pancreas.
note: usually occurs during childhood/adolescence
moreso effects those of european origin
Q: Why are β cells important?
A: They produce insulin, which is essential for normal growth, development, and blood glucose regulation.
Q: How is Type 1 Diabetes treated?
A: Insulin therapy, insulin is purified from pigs or cattle,
Immune response (Type 1 DM): T-cell attack destroys pancreatic β cells.
Recombinant insulin: Genetically engineered insulin identical to human insulin
Q: What type of hypersensitivity is Rheumatoid Arthritis (RA)?
A: Type IV (cell-mediated) hypersensitivity.
type 4 involves t cells!!!
Q: How common is Rheumatoid Arthritis in the U.S.?
A: It affects about 1-3% of the population and is more common in women. Most often between 20-40 years old.
Q: Is Rheumatoid Arthritis a temporary or long-term condition?
A: It can be chronic or episodic(comes and goes) but is generally a long-term inflammatory disease.
Q: What immune cells are involved in Rheumatoid Arthritis?
A: CD4 T cells, CD8 T cells, B cells, neutrophils, and macrophages.
Q: What role do plasma cells play in Rheumatoid Arthritis?
A: They produce rheumatoid factor, an autoantibody that targets the Fc region of IgG.
Q: What are the main treatment approaches for Rheumatoid Arthritis?
A: Physiotherapy combined with immunosuppressant therapy.
Anti-TNFα
• Eliminates inflammation
• Reduces joint swelling and pain
• Anti-CD20
• Depletes B cells
Q: What type of hypersensitivity is Multiple Sclerosis?
A: Type IV (cell-mediated) hypersensitivity.
Q: What immune mechanism drives Multiple Sclerosis
?A: Th1 cells release IFN-γ, which activates macrophages to secrete proteases and cytokines that damage tissue. this will lead to sclerotic plaques of demyelinated tissue in the white matter of the CNS, which causes Motor weakness, impaired vision, lack of coordination, spasticity
this can lead to Severe disability or death within a few years.
Q: What is the main pathological feature of Multiple Sclerosis?
A: Loss of myelin in the central nervous system
Q: What type of hypersensitivity is Celiac Disease?
A: Type IV (cell-mediated) hypersensitivity.
its an autoimmune disease, but only happens when triggered by the gluten peptide
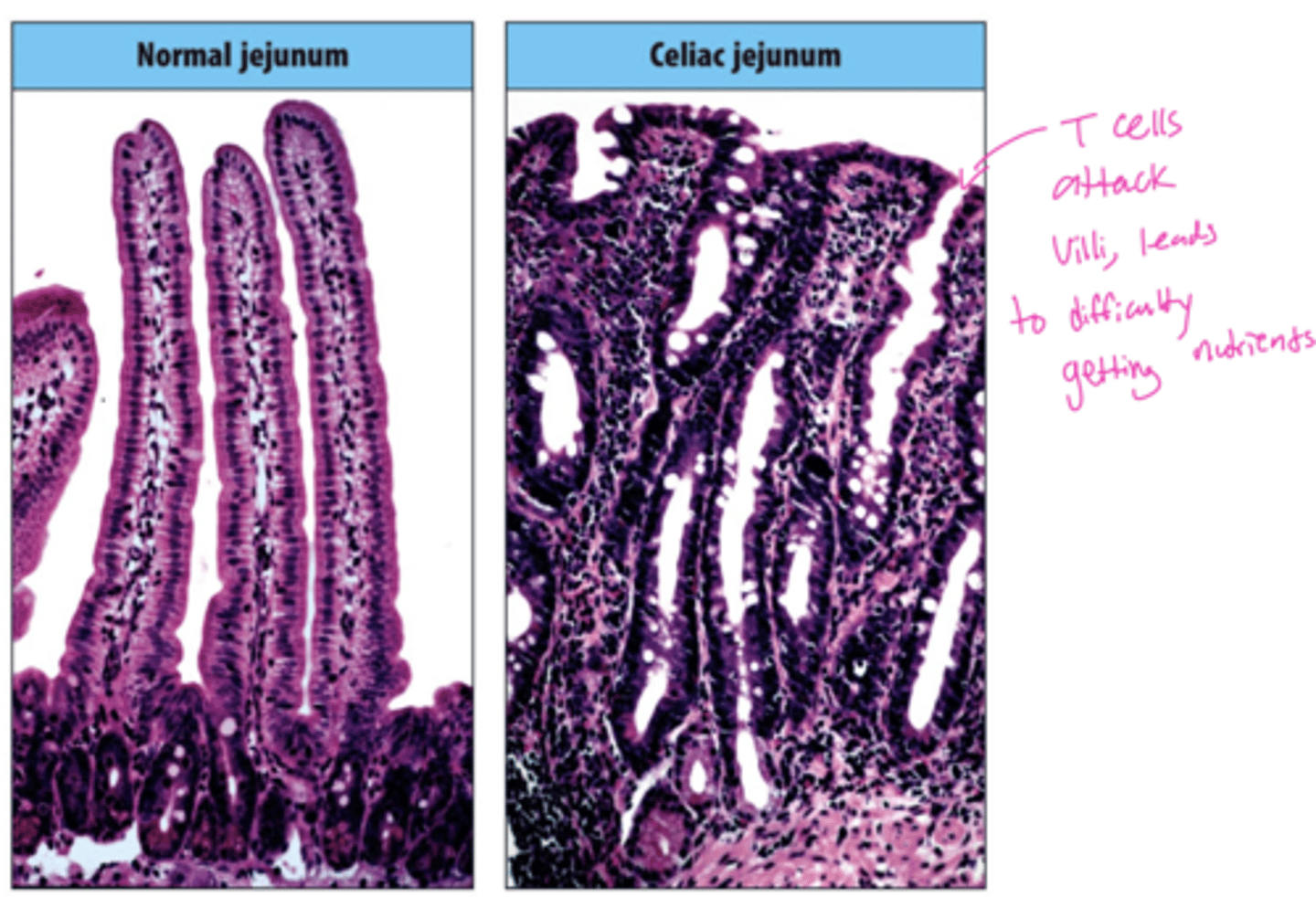
Q: What kind of disease is Celiac Disease?
A: A chronic inflammatory disease of the small intestine.
its an autoimmune disease, but only happens when triggered by the gluten peptide
Q: What immune pathway is primarily involved in Celiac Disease?
A: Th1-mediated immune response.
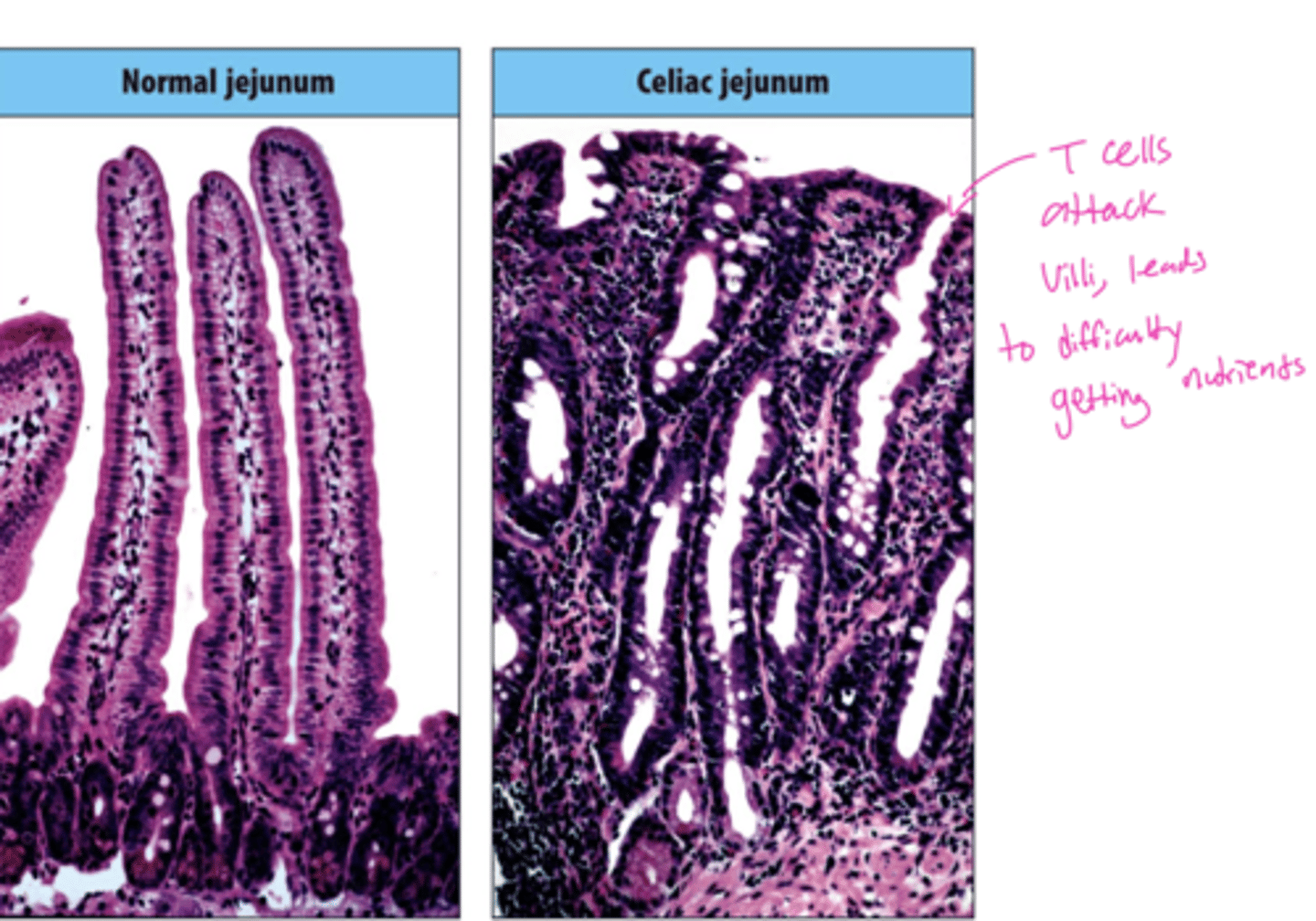
Q: Which immune cells contribute to tissue damage in Celiac Disease?
A: Macrophages activated by Th1 cells.
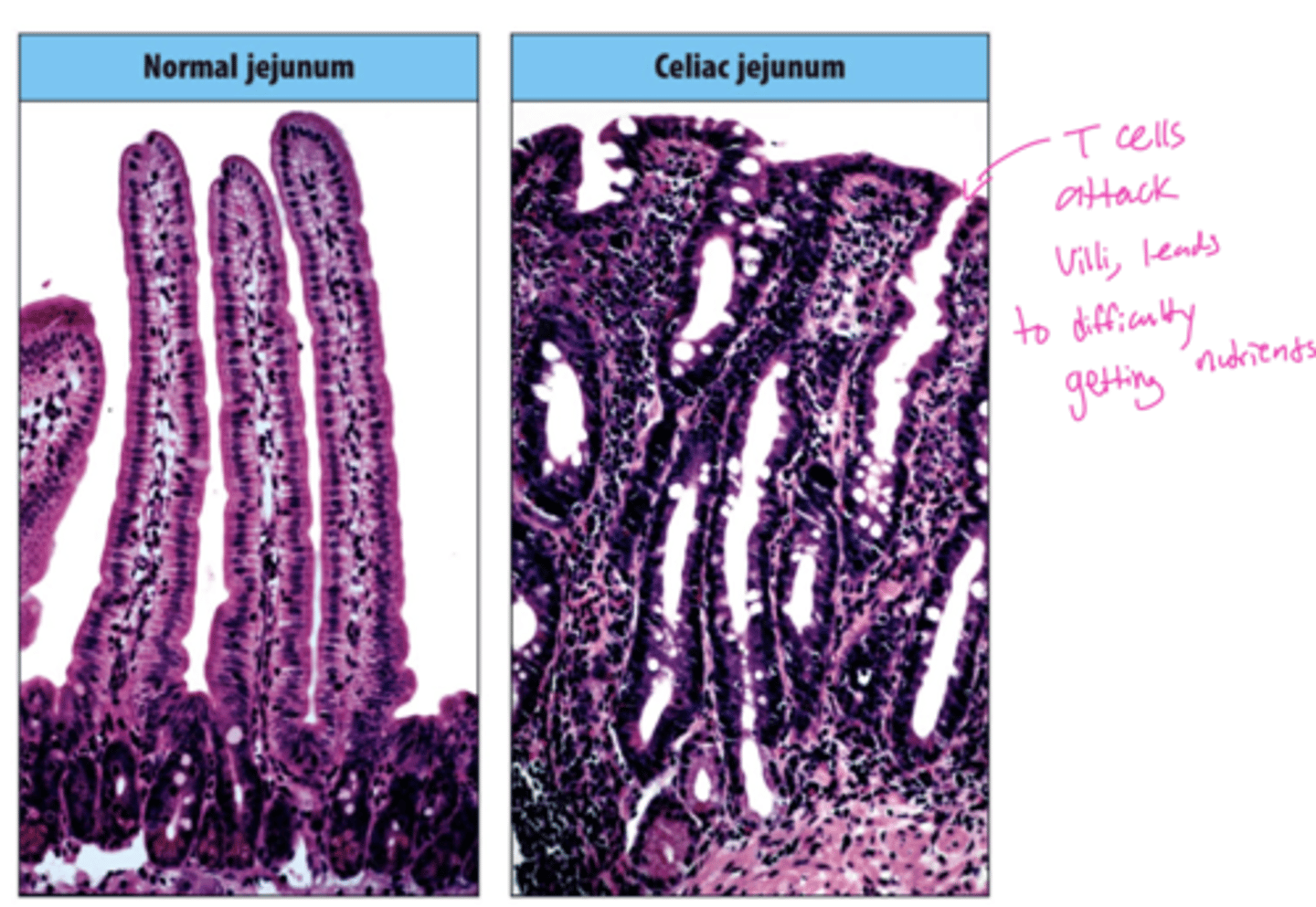
Q: What triggers the immune response in Celiac Disease?
A: Gluten proteins, usually found in rye and barley
Q: What structural change occurs in the intestine in Celiac Disease, and what does this lead to?
A: Atrophy (flattening) of the intestinal villi.
this leads to malnourishment, failure to thrive, anemia, depression and predisposition to intestinal cancer
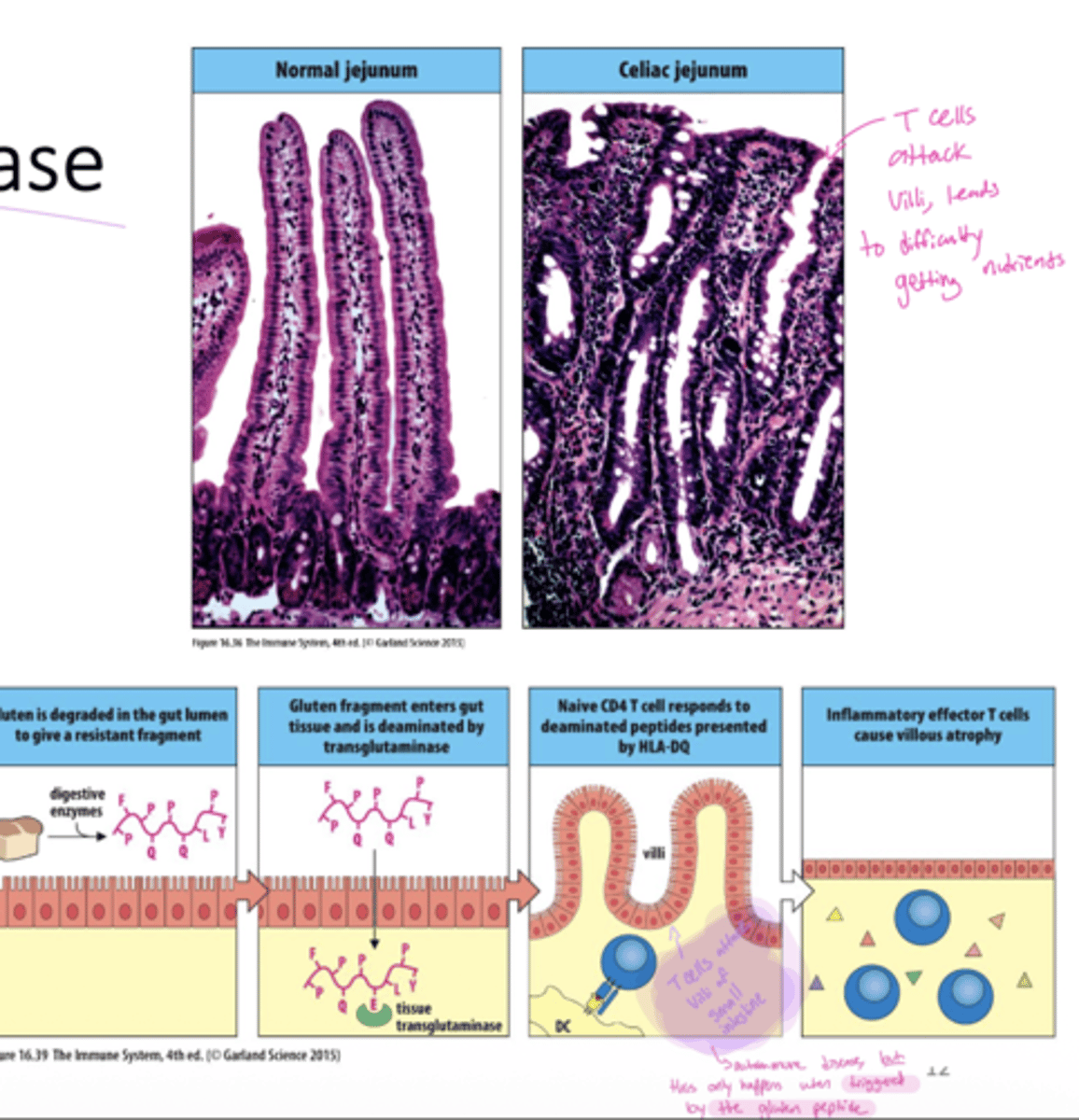
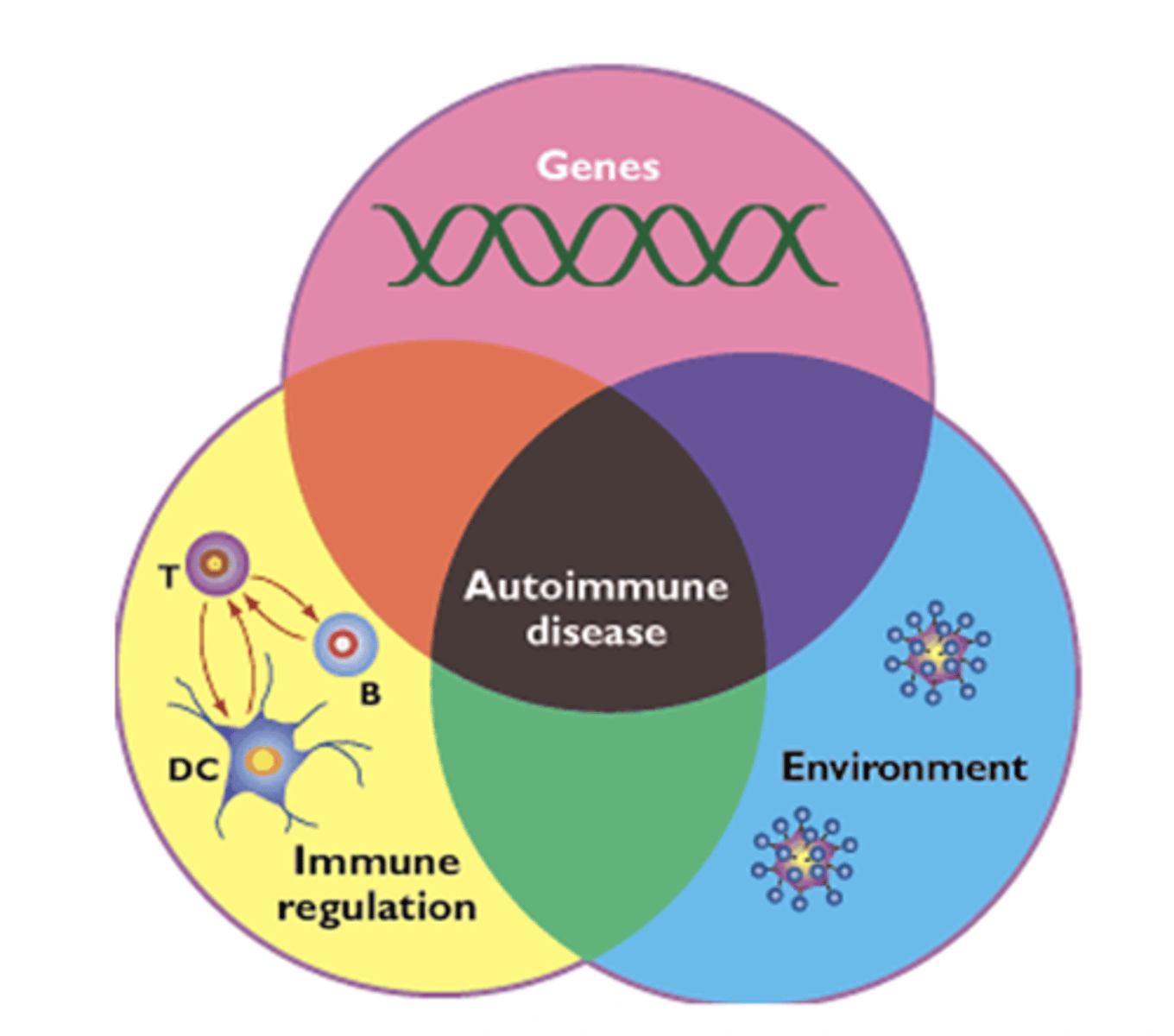
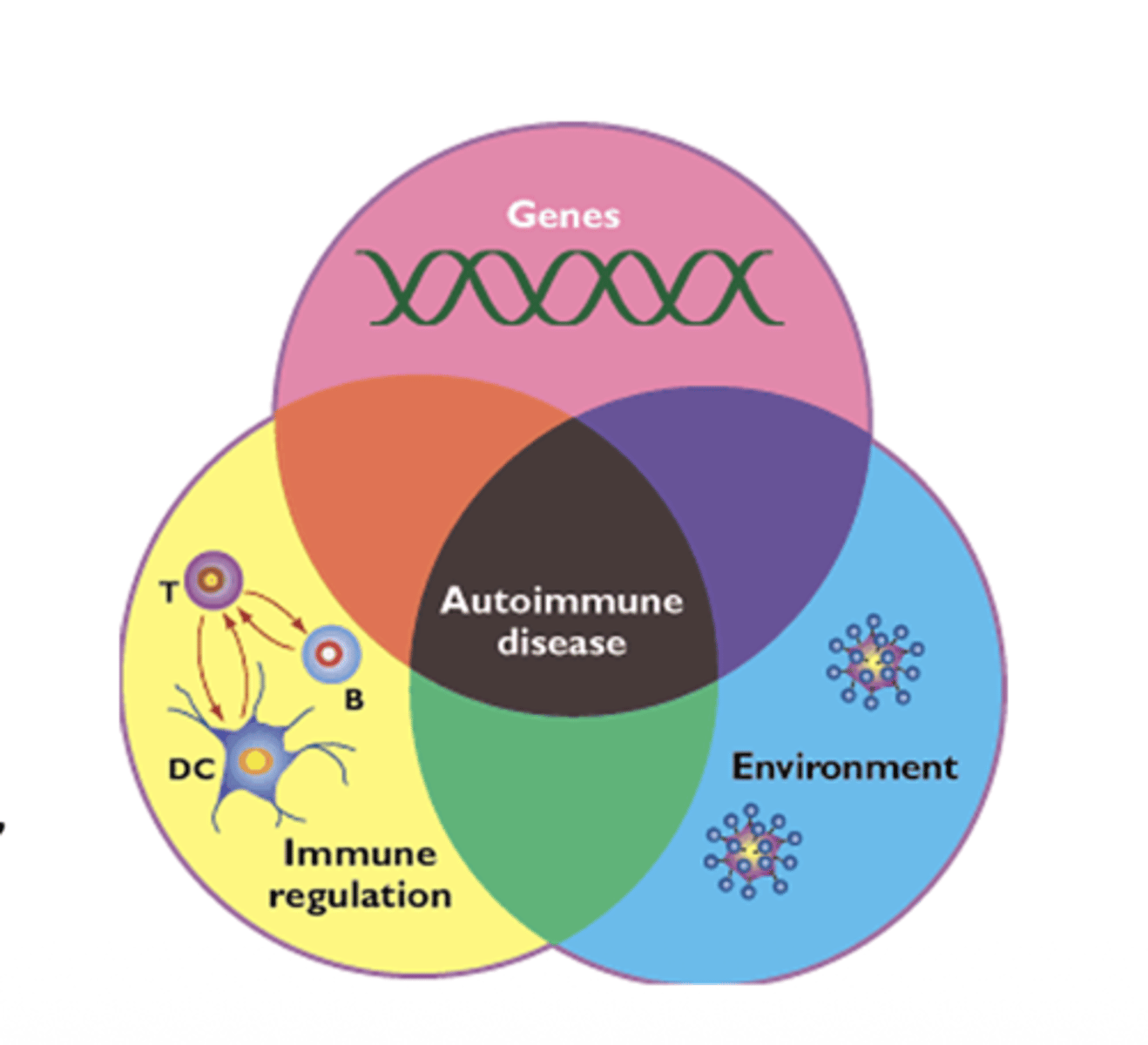
Q: What factors contribute to predisposition for autoimmune diseases?
A: Both genetic and environmental factors contribute to loss of self-tolerance (loss of self tolerance=The immune system fails to recognize the body's own tissues as self.)
Q: How do autoimmune diseases affect males and females differently?
A: They affect females more frequently than males. it may be linked to hormones, but unsure
Q: What is AIRE deficiency?
A: A genetic defect that disrupts immune self-tolerance and increases risk of autoimmune disease.
Q: What is AIRE deficiency?
A: A genetic defect that disrupts immune self-tolerance and increases risk of autoimmune disease.
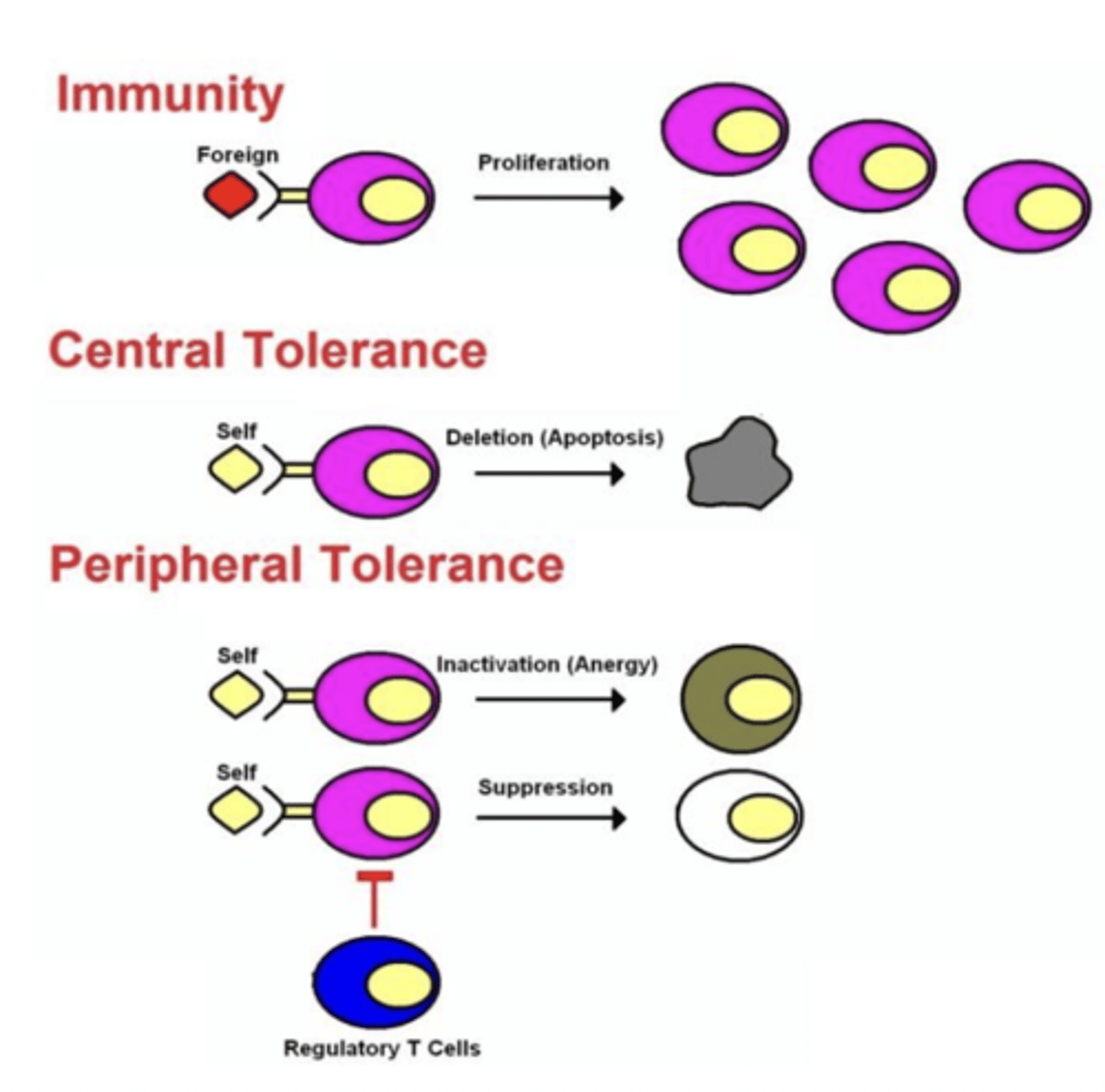
Q: What is the primary function of regulatory T cells (Tregs)?
A: They prevent activation of self-reactive T cells and help maintain immune tolerance by expressing FoxP3 which:
(Directs immature T cells to develop into regulatory T cells
Controls genes that allow Tregs to suppress other immune cells
Maintains self-tolerance, preventing the immune system from attacking the body
Keeps immune responses from becoming excessive or self-destructive)
Q: What happens when FoxP3 is deficient? (what is the disease associated w it and who does it affect)
A: Severe autoimmunity against multiple tissues occurs.
this leads to Immune dysregulation,
polyendocrinopathy, enteropathy and X-
linked syndrome
this leads to multiple autoimmune diseases, and affects boys more commonly
Q: What are Th17 cells?
A: A subset of helper CD4+ T cells involved in promoting inflammation.
Q: What is the main cytokine secreted by Th17 cells, and what is its function
A: IL-17, which Binds to receptor on fibroblasts,
epithelial cells, keratinocytes
and Stimulates release of cytokines for
inflammatory cell recruitment
Q: What happens to Th17 cells in autoimmune disease (AID)?
A: They accumulate and contribute to excessive inflammation.
AID= autoimmune diseases, we see an increase in Th17 cells in those with an autoimmune diseases
Q: How does HLA relate to autoimmune disease risk?
A: HLA is the most important genetic factor, accounting for ~50% of genetic predisposition, with susceptibility running in families and certain populations (including Caucasians)
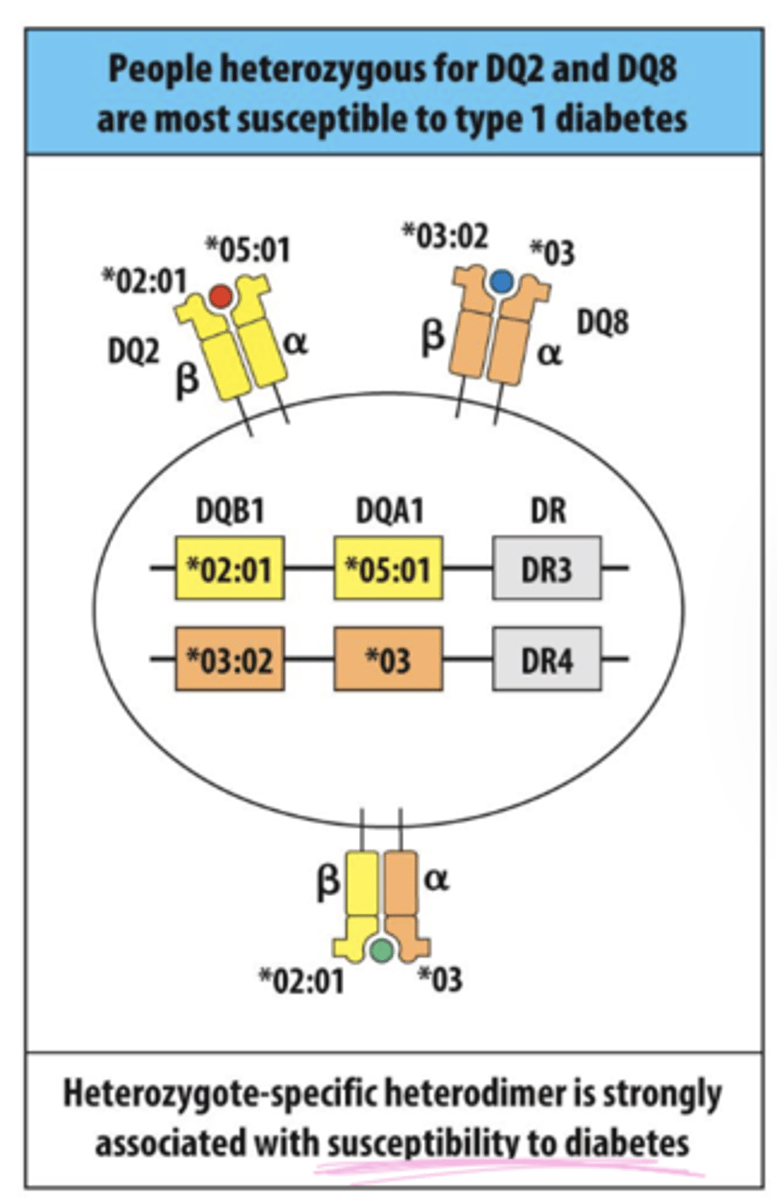
Q: What are key facts about HLA inheritance and autoimmune association?
A: Individuals have 4 HLA alleles (2 maternal, 2 paternal), autoimmune disease is most often linked to HLA class II, and only ~20% of people with AID-associated HLA actually develop disease.